Академический Документы
Профессиональный Документы
Культура Документы
Enzalutamide in Metastatic Prostate Cancer Before Chemotherapy
Загружено:
Randa HalfianОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Enzalutamide in Metastatic Prostate Cancer Before Chemotherapy
Загружено:
Randa HalfianАвторское право:
Доступные форматы
The n e w e ng l a n d j o u r na l of m e dic i n e
original article
Enzalutamide in Metastatic Prostate Cancer
before Chemotherapy
T.M. Beer, A.J. Armstrong, D.E. Rathkopf, Y. Loriot, C.N. Sternberg, C.S. Higano,
P. Iversen, S. Bhattacharya, J. Carles, S. Chowdhury, I.D. Davis, J.S. de Bono,
C.P. Evans, K. Fizazi, A.M. Joshua, C.-S. Kim, G. Kimura, P. Mainwaring,
H. Mansbach, K. Miller, S.B. Noonberg, F. Perabo, D. Phung, F. Saad, H.I. Scher,
M.-E. Taplin, P.M. Venner, and B. Tombal, for the PREVAIL Investigators*
A BS T R AC T
Background
Enzalutamide is an oral androgen-receptor inhibitor that prolongs survival in men The authors full names, academic de-
with metastatic castration-resistant prostate cancer in whom the disease has pro- grees, and affiliations are listed in the Ap-
pendix. Address reprint requests to Dr.
gressed after chemotherapy. New treatment options are needed for patients with Beer at OHSU Knight Cancer Institute,
metastatic prostate cancer who have not received chemotherapy, in whom the dis- Oregon Health and Science University,
ease has progressed despite androgen-deprivation therapy. 3303 SW Bond Ave., CH14R, Portland,
OR 97239, or at beert@ohsu.edu.
Methods * Additional investigators in the PREVAIL
In this double-blind, phase 3 study, we randomly assigned 1717 patients to receive study are listed in the Supplementary
Appendix, available at NEJM.org.
either enzalutamide (at a dose of 160 mg) or placebo once daily. The coprimary end
points were radiographic progression-free survival and overall survival. This article was published on June 1, 2014,
at NEJM.org.
Results DOI: 10.1056/NEJMoa1405095
The study was stopped after a planned interim analysis, conducted when 540 deaths Copyright 2014 Massachusetts Medical Society.
had been reported, showed a benefit of the active treatment. The rate of radio-
graphic progression-free survival at 12 months was 65% among patients treated
with enzalutamide, as compared with 14% among patients receiving placebo (81%
risk reduction; hazard ratio in the enzalutamide group, 0.19; 95% confidence inter-
val [CI], 0.15 to 0.23; P<0.001). A total of 626 patients (72%) in the enzalutamide
group, as compared with 532 patients (63%) in the placebo group, were alive at the
data-cutoff date (29% reduction in the risk of death; hazard ratio, 0.71; 95% CI,
0.60 to 0.84; P<0.001). The benefit of enzalutamide was shown with respect to all
secondary end points, including the time until the initiation of cytotoxic chemo-
therapy (hazard ratio, 0.35), the time until the first skeletal-related event (hazard
ratio, 0.72), a complete or partial soft-tissue response (59% vs. 5%), the time until
prostate-specific antigen (PSA) progression (hazard ratio, 0.17), and a rate of de-
cline of at least 50% in PSA (78% vs. 3%) (P<0.001 for all comparisons). Fatigue and
hypertension were the most common clinically relevant adverse events associated
with enzalutamide treatment.
Conclusions
Enzalutamide significantly decreased the risk of radiographic progression and
death and delayed the initiation of chemotherapy in men with metastatic prostate
cancer. (Funded by Medivation and Astellas Pharma; PREVAIL ClinicalTrials.gov
number, NCT01212991.)
n engl j med nejm.org 1
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
P
rostate cancer is the most common- are frequently administered (i.e., those who have
ly diagnosed cancer and the sixth leading asymptomatic or mildly symptomatic metastatic
cause of cancer-related death among men disease that has progressed despite the use of
worldwide.1 Strategies to block androgen-recep- androgen-deprivation therapy) and who have not
tor signaling have formed the backbone of pros- undergone chemotherapy.
tate-cancer therapy since the first description of
the hormonal dependence of this cancer in 1941.2 Me thods
Advances in endocrine therapies have improved
survival in men with high-risk locoregional pros- Study Design and Conduct
tate cancer.3,4 However, new hormonal agents The PREVAIL study was a multinational, double-
have been shown to extend survival in men with blind, randomized, placebo-controlled, phase 3
metastatic castration-resistant disease.5-9 trial of enzalutamide. The study was approved by
In most patients who are treated for advanced the independent review board at each participat-
recurrent prostate cancer with androgen-depri- ing site and was conducted according to the pro-
vation therapy (comprising a luteinizing hormone visions of the Declaration of Helsinki and the
releasing hormone [LHRH] analogue or orchiec- Good Clinical Practice Guidelines of the Interna-
tomy with or without an antiandrogen), disease tional Conference on Harmonisation. All patients
progression occurs despite effective suppression provided written informed consent before par-
of serum testosterone. This disease state, called ticipating in the trial. An independent data and
castration-resistant prostate cancer, is almost safety monitoring committee reviewed safety data
always associated with increases in levels of se- at regular intervals and reviewed the prespecified
rum prostate-specific antigen (PSA), suggesting interim analysis conducted by an independent
that the disease continues to be driven by andro- statistical group at the contract clinical research
gen-receptor signaling. Preclinical evidence sug- organization where the study database was held.
gests that androgen-receptor overexpression is The study was designed by prostate-cancer
sufficient to confer resistance to androgen de- experts and employees of the sponsors, Mediva-
privation in prostate-cancer cell lines10,11 and tion and Astellas Pharma, which are codevelop-
that levels of intratumoral androgens are often ing enzalutamide. Investigators at the participat-
increased in patients with progressive prostate ing centers entered the data into an electronic
cancer.12 These observations have provided a data-capture system that was verified for source
clear basis for developing more effective meth- data by monitors from a separate clinical research
ods to treat prostate cancer by further suppress- organization. The data analyses reported here
ing androgen-receptor signaling.13,14 were conducted by the sponsor and were provided
Enzalutamide (formerly known as MDV3100) to all the authors, who wrote the manuscript and
is a rationally designed, targeted androgen-recep- made the decision to submit the manuscript for
tor inhibitor that competitively binds to the li- publication. These authors assume responsibility
gand-binding domain of the androgen receptor for the accuracy of the data and adherence to the
and inhibits androgen-receptor translocation to study protocol, which is available with the full
the cell nucleus, recruitment of androgen-recep- text of this article at NEJM.org. A professional
tor cofactors, and androgen-receptor binding to writer who was paid by the sponsors assisted in
DNA.15 In a phase 12 trial, enzalutamide was the preparation of the manuscript. All the authors
found to have encouraging antitumor activity in and participating institutions have agreements
men with castration-resistant prostate cancer, with with the sponsors regarding the confidentiality
data suggesting a greater benefit in men who had of the data.
not yet received chemotherapy.16 In a previous
phase 3 study, enzalutamide, as compared with Study Participants
placebo, prolonged overall and progression-free Patients were eligible if they had histologically or
survival, improved patient-reported quality of life, cytologically confirmed adenocarcinoma of the
and delayed the development of skeletal-related prostate with documented metastases and had
complications in men with metastatic castration- PSA progression, radiographic progression, or both
resistant prostate cancer who had previously re- in bone or soft tissue, despite receiving LHRH
ceived docetaxel.7 In our study, we evaluated analogue therapy or undergoing orchiectomy,
enzalutamide in men in whom hormonal agents with a serum testosterone level of 1.73 nmol per
2 n engl j med nejm.org
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
Enzalutamide in Metastatic Prostate Cancer
liter (50 ng per deciliter) or less. Continued an- scanning. Imaging was performed at the time of
drogen-deprivation therapy was required. Previous screening, at weeks 9, 17, and 25, and every 12
antiandrogen therapy and concurrent use of glu- weeks thereafter. Radiologists at a central location
cocorticoids were permitted but not required. who were unaware of the study-group assign-
Eligible patients had not received cytotoxic che- ments determined whether there was progres-
motherapy, ketoconazole, or abiraterone acetate, sive disease on the basis of Response Evaluation
had an Eastern Cooperative Oncology Group per- Criteria in Solid Tumors (RECIST), version 1.1, for
formance status grade of 0 or 1 (no symptoms or soft tissue or on the basis of criteria adapted
ambulatory but restricted in strenuous activities), from the Prostate Cancer Clinical Trials Working
and were either asymptomatic (score of 0 to 1) or Group 217 for osseous disease (Table S1 in the
mildly symptomatic (score of 2 to 3), as measured Supplementary Appendix).
on the Brief Pain Inventory Short Form question
3 (on which scores range from 0 to 10, with high- Statistical Analysis
er scores indicating a greater severity of pain). The planned enrollment was approximately 1680
Patients with visceral disease, including lung or patients. The coprimary end points were ana-
liver metastases, were eligible, as were patients lyzed in the intention-to-treat population at a to-
with New York Heart Association class I or II tal type I error rate of 0.05, with an error rate of
heart failure. Patients with a history of seizure or 0.001 (two-sided) allocated to radiographic pro-
a condition that could confer a predisposition to gression-free survival and an error rate of 0.049
seizure were excluded, although patients taking (two-sided) allocated to overall survival. It was
medications associated with lowering the seizure planned that the final analysis of radiographic
threshold were eligible. progression-free survival would be conducted af-
From September 2010 through September 2012, ter the occurrence of at least 410 events at the
patients were enrolled at 207 sites globally. All time of the interim analysis of overall survival.
patients were randomly assigned to receive either The interim analysis of overall survival was to be
oral enzalutamide (at a dose of 160 mg) or placebo conducted after the occurrence of approximately
once daily with or without food. Randomization 516 deaths, or 67% of the 765 deaths specified
was stratified according to the study site. Treat- for the final analysis. The final analysis of radio-
ment continued until the occurrence of unaccept- graphic progression-free survival was performed
able side effects or confirmed radiographic pro- after the occurrence of 439 events (with data cut-
gression and the initiation of chemotherapy or off on May 6, 2012); the interim analysis of over-
an investigational agent. Treatment discontinua- all survival was performed after the occurrence
tion because of an increase in the PSA level alone of 540 deaths with the use of a two-sided type I
was discouraged. error rate of 0.0147. Holms step-down procedure
was applied to the analyses of the secondary end
Study End Points points to maintain a two-sided type I error of 5%.18
Coprimary end points were radiographic progres- The results presented here are based on a cutoff
sion-free survival and overall survival. Secondary date of September 16, 2013, unless otherwise
end points included the time until the initiation specified. An updated survival analysis was per-
of cytotoxic chemotherapy, the time until the first formed with a data-cutoff date of January 15, 2014.
skeletal-related event, the best overall soft-tissue
response, the time until PSA progression, and a R e sult s
decline in the PSA level of 50% or more from
baseline. Prespecified exploratory end points in- Study Patients
cluded quality of life, as measured with the use A total of 1717 patients were enrolled in the
of the Functional Assessment of Cancer Therapy study, with 872 in the enzalutamide group and
Prostate (FACT-P) scale, and a decline in the PSA 845 in the placebo group; 1715 patients received
level of 90% or more from baseline. End-point at least one dose of a study drug (Fig. S1 in the
definitions are provided in Table S1 in the Sup- Supplementary Appendix). Baseline demographic
plementary Appendix, available at NEJM.org. and disease characteristics were well balanced
Radiographic disease was evaluated with the between the two groups (Tables S2 and S3 in the
use of either computed tomography or magnetic Supplementary Appendix). The median time that
resonance imaging and with the use of bone patients received a study drug was substantially
n engl j med nejm.org 3
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
longer in the enzalutamide group than in the pla- of radiographic progression or death (hazard ra-
cebo group (16.6 months vs. 4.6 months). More tio in the enzalutamide group, 0.19; 95% confi-
patients in the enzalutamide group than in the dence interval [CI], 0.15 to 0.23; P<0.001) (Fig. 1A).
placebo group received at least 12 months of treat- Fewer patients in the enzalutamide group than
ment (68% vs. 18%) and continued to receive treat- in the placebo group had radiographic progres-
ment as of the data-cutoff date (42% vs. 7%). sion or died (118 of 832 patients [14%] vs. 321 of
801 patients [40%]). The median radiographic
Coprimary End Points progression-free survival was not reached in the
Radiographic Progression-free Survival enzalutamide group, as compared with 3.9 months
At 12 months of follow-up, the rate of radiographic in the placebo group. The treatment effect of
progression-free survival was 65% in the enzalu- enzalutamide on radiographic progression-free
tamide group and 14% in the placebo group. survival was consistent across all prespecified sub-
Treatment with enzalutamide, as compared with groups (Fig. S2 in the Supplementary Appendix).
placebo, resulted in an 81% reduction in the risk
Overall Survival
At the planned interim analysis of overall sur-
A
Hazard ratio, 0.19 (95% CI, 0.150.23)
vival, the median duration of follow-up for sur-
100
vival was approximately 22 months. Fewer deaths
Radiographic Progression-free
90 P<0.001
80 occurred in the enzalutamide group than in the
Enzalutamide
70 placebo group (241 of 872 patients [28%] vs. 299
Survival (%)
60
50
of 845 patients [35%]). Treatment with enzalu-
40 tamide, as compared with placebo, resulted in a
30 29% decrease in the risk of death (hazard ratio,
20 Placebo
0.71; 95% CI, 0.60 to 0.84; P<0.001) (Fig. 1B). The
10
0 median overall survival was estimated at 32.4
0 3 6 9 12 15 18 months in the enzalutamide group and 30.2
Months months in the placebo group. The treatment ef-
No. at Risk fect of enzalutamide on overall survival was con-
Enzalutamide 832 514 256 128 34 5 1 sistent across all prespecified subgroups (Fig. S3
Placebo 801 305 79 20 5 0 0
in the Supplementary Appendix). The risk reduc-
B tions for both coprimary end points were unaf-
100 fected by previous exposure to antiandrogens.
90 After review of the interim coprimary efficacy
80
Overall Survival (%)
Enzalutamide and safety results, the data and safety monitor-
70 Placebo
60 ing committee recommended halting the study
50 and offering enzalutamide to eligible patients re-
40 ceiving placebo. An updated analysis of overall
30
survival with 116 additional deaths showed that
20 Hazard ratio, 0.71 (95% CI, 0.600.84)
10 P<0.001
82% of patients in the enzalutamide group and
0 73% of those in the placebo group were alive at
0 3 6 9 12 15 18 21 24 27 30 33
18 months; the estimated median was not yet
Months reached in the enzalutamide group and was 31.0
No. at Risk months in the placebo group (hazard ratio, 0.73;
Enzalutamide 872 863 850 824 797 745 566 395 244 128 33 2
Placebo 845 835 781 744 701 644 484 328 213 102 27 2 95% CI, 0.63 to 0.85; P<0.001) (Table S4 in the
Supplementary Appendix).
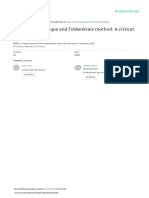
Figure 1. KaplanMeier Estimates of Radiographic Progression-free Survival
and Overall Survival. Subsequent Antineoplastic Therapy
Shown are data for the coprimary end points of radiographic progression-
Subsequent antineoplastic treatments associated
free survival (Panel A) and overall survival (Panel B). The dashed horizontal
lines indicate medians. Hazard ratios are based on unstratified Cox regres- with a demonstrated survival benefit in meta-
sion models with treatment as the only covariate, with values of less than static prostate cancer were received by 40% of
1.00 favoring enzalutamide. patients in the enzalutamide group, as compared
with 70% of those in the placebo group. The two
4 n engl j med nejm.org
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
Enzalutamide in Metastatic Prostate Cancer
most common subsequent therapies were docetax- tamide also resulted in a reduction in the risk of
el (received by 33% and 57% of patients, respec- a first skeletal-related event, which occurred in
tively) and abiraterone (received by 21% and 46%, 278 patients (32%) in the enzalutamide group
respectively) (Table S5 in the Supplementary Ap- and 309 patients (37%) in the placebo group
pendix). The use of abiraterone was more com- (hazard ratio, 0.72; P<0.001) at a median of ap-
mon in North America than in other regions. The proximately 31 months in each of the two groups
duration and efficacy of post-progression thera- (Table 1).
pies were not ascertained. Among patients with measurable soft-tissue
disease at baseline, 59% of the patients in the
Prespecified Secondary and Exploratory enzalutamide group, as compared with 5% in
End Points the placebo group, had an objective response
The superiority of enzalutamide over placebo was (P<0.001) (Table 1): complete and partial re-
shown with respect to all secondary end points. sponses were observed in 20% and 39% of the
The median time until the initiation of cytotoxic patients, respectively, in the enzalutamide group,
chemotherapy was 28.0 months in the enzalu- as compared with 1% and 4%, respectively, in
tamide group, as compared with 10.8 months in the placebo group. Enzalutamide was also supe-
the placebo group (hazard ratio, 0.35; P<0.001) rior to placebo with respect to reductions of at
(Table 1 and Fig. 2A). Treatment with enzalu- least 50% and 90% in the PSA level, the time
Table 1. Secondary and Prespecified Exploratory End Points.*
Enzalutamide Placebo Hazard Ratio
End Point (N=872) (N=845) (95% CI) P Value
Median time until initiation of cytotoxic 28.0 10.8 0.35 (0.300.40) <0.001
chemotherapy mo
Median time until decline in the FACT-P 11.3 5.6 0.63 (0.540.72) <0.001
global score mo
Median time until first skeletal-related event 31.1 31.3 0.72 (0.610.84) <0.001
mo
Median time until PSA progression mo 11.2 2.8 0.17 (0.150.20) <0.001
Confirmed change in PSA
Patients with 1 post-baseline PSA 854 (98) 777 (92)
assessment no. (%)
PSA decline of 50% from baseline 666/854 (78) 27/777 (3) <0.001
no./total no. (%)
PSA decline of 90% from baseline 400/854 (47) 9/777 (1) <0.001
no./total no. (%)
Patients with measurable soft-tissue 396 (45) 381 (45)
disease no. (%)**
Objective response 233 (59) 19 (5) <0.001
Complete response 78 (20) 4 (1)
Partial response 155 (39) 15 (4)
* A complete definition of study end points is provided in Table S1 in the Supplementary Appendix. CI denotes confi-
dence interval, and PSA prostate-specific antigen.
This category was a prespecified exploratory end point.
A decline on the Functional Assessment of Cancer TherapyProstate (FACT-P) scale was defined as decrease of 10
points or more on the global score, which ranges from 0 to 156, with higher scores indicating a better quality of life.
The hazard ratio is a more accurate measure of treatment effect than are estimates of the median time until the event
for late-occurring events in this study.
PSA progression was based on criteria of the Prostate Cancer Clinical Trials Working Group 2.
Only patients with baseline and post-baseline assessments are included.
** Only patients with measurable soft-tissue disease at baseline, as assessed on the basis of the Response Evaluation
Criteria in Solid Tumors, version 1.1, are included.
n engl j med nejm.org 5
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
in the enzalutamide group listed in the latter ta-
A ble). The median reporting period for adverse
100
events was 17.1 months in the enzalutamide
90
Patients with No Cytotoxic
80 group and 5.4 months in placebo group, which
Chemotherapy (%)
70 Enzalutamide reflected the longer exposure of patients to
60 enzalutamide. A grade 3 or higher adverse event
50
40
was reported in 43% of the patients in the enzalu-
30 Placebo tamide group, as compared with 37% in the pla-
20 Hazard ratio, 0.35 (95% CI, 0.300.40) cebo group; however, the median time until the
10 P<0.001 first event of grade 3 or higher was 22.3 months
0
0 3 6 9 12 15 18 21 24 27 30 33 in the enzalutamide group and 13.3 months in
Months the placebo group (Fig. S4 in the Supplementary
No. at Risk Appendix). The most common adverse events
Enzalutamide 872 854 799 751 665 576 389 252 158 79 21 2 leading to death were disease progression and a
Placebo 845 734 518 415 324 257 165 103 64 25 9 0
general deterioration in physical health, with
B similar incidences in the two groups.
100
Adverse events that occurred in 20% or more
90 Hazard ratio, 0.17 (95% CI, 0.150.20) of patients receiving enzalutamide at a rate that
P<0.001
was at least 2 percentage points higher than that
Patients with No PSA
80
Progression (%)
70
in the placebo group were fatigue (Table S6 in
60
50 the Supplementary Appendix), back pain, consti-
40 pation, and arthralgia. After adjustment for the
Enzalutamide
30 length of exposure, events with a higher rate in
20
the enzalutamide group than in the placebo
10 Placebo
0 group were hot flush (14 vs. 12 events per 100
0 3 6 9 12 15 18 21 24 27 30 33 patient-years), hypertension (11 vs. 7 events per
Months 100 patient-years), and falls (11 vs. 9 events per
No. at Risk 100 patient-years). The most common event of
Enzalutamide 872 802 590 456 351 275 168 110 65 27 6 1 grade 3 or higher in the enzalutamide group was
Placebo 845 228 61 28 17 10 6 4 2 1 0 0
hypertension, which was reported in 7% of the
Figure 2. KaplanMeier Estimates for the Times until the Initiation of patients. The most common cardiac event was
Cytotoxic Chemotherapy and an Increased Level of Prostate-Specific atrial fibrillation, which was reported in 2% of
Antigen. the patients in the enzalutamide group and in
Shown are secondary efficacy end points that include the time until the 1% of those in the placebo group. One patient in
initiation of cytotoxic chemotherapy (Panel A) and the time until an in- each study group had a seizure. No evidence of
creased level of prostate-specific antigen (PSA) (Panel B). The horizontal
dashed lines indicate medians. Hazard ratios are based on unstratified Cox
hepatotoxicity, as measured by adverse events or
regression models with treatment as the only covariate, with values of less laboratory assessments, was observed in the
than 1.00 favoring enzalutamide. The full definition of PSA progression is enzalutamide group.
provided in Table S1 in the Supplementary Appendix.
Discussion
until PSA progression, and the time until a de- In our study involving men with metastatic pros-
cline in the quality of life (Table 1 and Fig. 2B).tate cancer who had not received previous che-
The median time until a quality-of-life deteriora- motherapy, enzalutamide extended the time until
tion, as measured on the FACT-P scale, was 11.3 radiographic progression or death, improved
months in the enzalutamide group and 5.6 overall survival, and delayed the initiation of che-
months in the placebo group (hazard ratio, 0.63; motherapy by a median of 17 months. The ben-
P<0.001). efit of enzalutamide on radiographic progres-
sion-free survival was observed from the first
Safety assessment 2 months after randomization and
Adverse events are summarized in Tables 2 and 3 conferred a relative reduction of 81% in the risk
(with events occurring in at least 10% of patients of progression or death. Consistent benefit was
6 n engl j med nejm.org
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
Enzalutamide in Metastatic Prostate Cancer
Table 2. Summary of Adverse Events.
Enzalutamide Placebo
Variable (N=871) (N=844)
Median safety reporting period mo 17.1 5.4
Any adverse event no. (%) 844 (97) 787 (93)
Any grade 3 adverse event no. (%) 374 (43) 313 (37)
Median time until first grade 3 adverse event mo 22.3 13.3
Any serious adverse event no. (%) 279 (32) 226 (27)
Any adverse event leading to treatment discontinuation no. (%) 49 (6) 51 (6)
Any adverse event leading to death no. (%) 37 (4) 32 (4)
observed in all prespecified subgroups, including tamide-treated patients than in placebo-treated
patients with visceral disease, a population with patients (43% vs. 37%), a finding that was prob-
a poorer prognosis that has been excluded from ably influenced by the fact that the safety-report-
other trials involving men with metastatic pros- ing period for the enzalutamide group was ap-
tate cancer who have not received previous che- proximately 1 year longer than that for the
motherapy.8,19 placebo group. The safety profile is further il-
Enzalutamide significantly reduced the risk lustrated by the 9-month delay in the median
of death by 29% over placebo, even though pa- time until the first adverse event of grade 3 or
tients in the placebo group had received effective higher in the enzalutamide group. A similar
post-progression therapy more frequently and proportion of patients in each group (6%) dis-
earlier than those in the enzalutamide group. continued treatment because of an adverse event.
The benefit of enzalutamide was observed as The safety profile was generally consistent
early as 4 months after randomization and was with that previously reported for enzalutamide
maintained throughout the study, as depicted by in patients who had received previous chemo-
the separation in the KaplanMeier survival therapy, with a few exceptions.7 Seizure, which
curves (Fig. 1B). At the time the trial was halted, was previously observed in the enzalutamide
following the interim analysis, the median fol- group among patients who had received chemo-
low-up for survival was 22 months, approxi- therapy, occurred in a single patient (0.1%) in
mately 8 to 10 months shorter than the esti- each group in our study. Both patients had a
mated survival medians. Because less than 5% history of seizure that was unknown to investi-
of the patients were at risk when the estimated gators at the time of enrollment. Hypertension
medians were reached, the hazard ratio, which was more commonly observed in the enzalu-
analyzes the differences in outcome across the tamide group than in the placebo group (13%
entire follow-up period, is a more accurate char- vs. 4%) and occurred more often in patients with
acterization of the survival benefit and other a medical history of hypertension. These events
late-occurring end points than is the estimate of were not associated with symptoms of mineralo-
the median time until the event. corticoid excess or an increased risk of cardio-
Health-related quality-of-life assessments can vascular or renal sequelae and generally were
reinforce and augment objective measures such managed with the use of standard therapies. In
as overall survival and radiographic progression. contrast to other antiandrogens, enzalutamide
In this population of men with metastatic pros- was not associated with hepatotoxicity. Other
tate cancer, deterioration in the quality of life adverse events that were reported more frequent-
was delayed by enzalutamide, a result suggest- ly in the enzalutamide group than in the placebo
ing that the treatment effects translated into group included fatigue or asthenia, back pain,
patient-perceived benefits. hot flush, and falls.
The benefit of enzalutamide was achieved Although chemotherapy has been shown to
with a favorable safety profile. Grade 3 or higher improve overall and progression-free survival in
adverse events were more common in enzalu- men with metastatic prostate cancer,20,21 many
n engl j med nejm.org 7
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
Table 3. Most Common Adverse Events and Events of Special Interest.
Enzalutamide Placebo
Adverse Events (N=871) (N=844)
All Grades Grade 3 All Grades Grade 3
number of patients (percent)
Most common adverse events*
Fatigue 310 (36) 16 (2) 218 (26) 16 (2)
Back pain 235 (27) 22 (3) 187 (22) 25 (3)
Constipation 193 (22) 4 (<1) 145 (17) 3 (<1)
Arthralgia 177 (20) 12 (1) 135 (16) 9 (1)
Decreased appetite 158 (18) 2 (<1) 136 (16) 6 (1)
Hot flush 157 (18) 1 (<1) 65 (8) 0
Diarrhea 142 (16) 2 (<1) 119 (14) 3 (<1)
Hypertension 117 (13) 59 (7) 35 (4) 19 (2)
Asthenia 113 (13) 11 (1) 67 (8) 8 (1)
Fall 101 (12) 12 (1) 45 (5) 6 (1)
Weight loss 100 (11) 5 (1) 71 (8) 2 (<1)
Edema peripheral 92 (11) 2 (<1) 69 (8) 3 (<1)
Headache 91 (10) 2 (<1) 59 (7) 3 (<1)
Specific adverse events
Any cardiac adverse event 88 (10) 24 (3) 66 (8) 18 (2)
Atrial fibrillation 16 (2) 3 (<1) 12 (1) 5 (1)
Acute coronary syndromes 7 (1) 7 (1) 4 (<1) 2 (<1)
Acute renal failure 32 (4) 12 (1) 38 (5) 12 (1)
Ischemic or hemorrhagic cerebrovascular event 12 (1) 6 (1) 9 (1) 3 (<1)
Elevation in alanine aminotransferase level 8 (1) 2 (<1) 5 (1) 1 (<1)
Seizure 1 (<1) 1 (<1) 1 (<1) 0
* Included in this category are adverse events that were reported in at least 10% of patients in the enzalutamide group at
a rate that was at least 2 percentage points higher than that in the placebo group.
This seizure occurred after the data-cutoff date.
patients do not receive such therapy primarily tients with metastatic prostate cancer8 who had
because of preexisting medical conditions or as- not received chemotherapy, improved progres-
sociated toxic effects.22-24 Thus, there is a need sion-free survival, lengthened the time until a
for effective, convenient, and less toxic thera- quality-of-life deterioration, delayed chemother-
pies. Sipuleucel-T showed an overall survival apy use, and was associated with a trend in favor
advantage in asymptomatic or mildly symptom- of an overall survival benefit that did not reach
atic men, most of whom had not received che- statistical significance. Treatment with abi-
motherapy, but did not induce tumor responses raterone requires concomitant use of prednisone
or delay disease progression or deterioration in to ameliorate symptoms of mineralocorticoid
quality of life.19 Radium-223 was recently shown excess, including fluid overload, hypokalemia,
to extend survival in men with symptomatic and hypertension.8,9
castration-resistant prostate cancer and bone Multiple agents are now reported to improve
metastases.25 Abiraterone plus prednisone, which survival for patients with metastatic prostate can-
was recently compared with prednisone in pa- cer that has progressed after androgen-depriva-
8 n engl j med nejm.org
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
Enzalutamide in Metastatic Prostate Cancer
tion therapy. The most effective use of these tion in quality of life and significantly improved
therapies (order of administration, duration of overall survival.
treatment, and efficacy of combinations) has not
yet been defined. Presented in part at the American Society of Clinical Oncology
In conclusion, in men with minimally symp- Genitourinary Cancers Symposium, San Francisco, January 31
tomatic or asymptomatic metastatic prostate February 4, 2014.
Supported by Medivation and Astellas Pharma, which also
cancer who had not received chemotherapy, funded editorial support.
enzalutamide, an oral therapy with an excellent Disclosure forms provided by the authors are available with
side-effect profile, significantly delayed radio- the full text of this article at NEJM.org.
We thank the patients who volunteered to participate in this
graphic disease progression or death, the need study for their dedication and the study-site staff who cared
for cytotoxic chemotherapy, and the deteriora- for them.
Appendix
The authors are as follows: Tomasz M. Beer, M.D., Andrew J. Armstrong, M.D., Sc.M., Dana E. Rathkopf, M.D., Yohann Loriot, M.D.,
Cora N. Sternberg, M.D., Celestia S. Higano, M.D., Peter Iversen, M.D., Suman Bhattacharya, Ph.D., Joan Carles, M.D., Ph.D., Simon
Chowdhury, M.D., Ph.D., Ian D. Davis, M.B., B.S., Ph.D., Johann S. de Bono, M.B., Ch.B., Ph.D., Christopher P. Evans, M.D., Karim
Fizazi, M.D., Ph.D., Anthony M. Joshua, M.B., B.S., Ph.D., Choung-Soo Kim, M.D., Ph.D., Go Kimura, M.D., Ph.D., Paul Mainwaring,
M.B., B.S., M.D., Harry Mansbach, M.D., Kurt Miller, M.D., Sarah B. Noonberg, M.D., Ph.D., Frank Perabo, M.D., Ph.D., De Phung,
B.S., Fred Saad, M.D., Howard I. Scher, M.D., Mary-Ellen Taplin, M.D., Peter M. Venner, M.D., and Bertrand Tombal, M.D., Ph.D.
The authors affiliations are as follows: OHSU Knight Cancer Institute, Oregon Health and Science University, Portland (T.M.B.);
Duke Cancer Institute Divisions of Medical Oncology and Urology, Duke University, Durham, NC (A.J.A.); Memorial Sloan-Kettering
Cancer Center and Weill Cornell Medical College, New York (D.E.R., H.I.S.); Institut Gustave Roussy, University of Paris Sud, Villejuif,
France (Y.L., K.F.); San Camillo and Forlanini Hospitals, Rome (C.N.S.); Seattle Cancer Care Alliance, University of Washington, Seattle
(C.S.H.); Rigshospitalet at the University of Copenhagen, Copenhagen (P.I.); Medivation, San Francisco (S.B., H.M., S.B.N.); Depart-
ment of Medical Oncology, Vall dHebron University Hospital, and Vall dHebron Institute of Oncology, Barcelona (J.C.); Guys Hospi-
tal (S.C.) and Royal Marsden Hospital and Institute of Cancer Research (J.S.B.) both in London; Monash University and Eastern
Health, Clayton, VIC (I.D.D.), and Icon Cancer Care, South Brisbane, QLD (P.M.) both in Australia; University of California, Davis,
Comprehensive Cancer Center, Sacramento (C.P.E.); Princess Margaret Cancer Centre, Toronto (A.M.J.), Centre Hospitalier de
lUniversit de Montral, Montreal (F.S.), and Cross Cancer Institute and University of Alberta, Edmonton, AB (P.M.V.) all in Canada;
Asan Medical Center, Seoul, South Korea (C.-S.K.); Nippon Medical School, Tokyo (G.K.); CharitUniversittsmedizin Berlin, Berlin
(K.M.); Astellas Pharma Global Development, Northbrook, IL (F.P., D.P.); DanaFarber Cancer Institute, Boston (M.-E.T.); and Cli-
niques Universitaires Saint-Luc, Brussels (B.T.).
References
1. Jemal A, Bray F, Center MM, Ferlay J, gression do not predict for cancer-specif- 12. Montgomery RB, Mostaghel EA, Ves-
Ward E, Forman D. Global cancer statis- ic survival in patients receiving immedi- sella R, et al. Maintenance of intratumor-
tics. CA Cancer J Clin 2011;61:69-90. [Er- ate or deferred androgen-deprivation al androgens in metastatic prostate can-
ratum, CA Cancer J Clin 2011;61:134.] therapy for prostate cancer: final results cer: a mechanism for castration-resistant
2. Huggins C, Hodges CV. Studies on of EORTC randomized trial 30891 with 12 tumor growth. Cancer Res 2008;68:4447-
prostatic cancer. I. The effect of castra- years of follow-up. Eur Urol 2013 July 24 54.
tion, of estrogen and of androgen injec- (Epub ahead of print). 13. Attard G, de Bono JS. Translating sci-
tion on serum phosphatases in metastatic 7. Scher HI, Fizazi K, Saad F, et al. In- entific advancement into clinical benefit
carcinoma of the prostate. Cancer Res creased survival with enzalutamide in for castration-resistant prostate cancer
1941;1:293-7. prostate cancer after chemotherapy. N Engl patients. Clin Cancer Res 2011;17:3867-
3. Bolla M, Gonzalez D, Warde P, et al. J Med 2012;367:1187-97. 75.
Improved survival in patients with locally 8. Ryan CJ, Smith MR, de Bono JS, et al. 14. Massard C, Fizazi K. Targeting con-
advanced prostate cancer treated with ra- Abiraterone in metastatic prostate cancer tinued androgen receptor signaling in
diotherapy and goserelin. N Engl J Med without previous chemotherapy. N Engl J prostate cancer. Clin Cancer Res 2011;
1997;337:295-300. Med 2013;368:138-48. [Erratum, N Engl J 17:3876-83.
4. Messing EM, Manola J, Yao J, et al. Med 2013;368:584.] 15. Tran C, Ouk S, Clegg NJ, et al. Devel-
Immediate versus deferred androgen de- 9. de Bono JS, Logothetis CJ, Molina A, opment of a second-generation antian-
privation treatment in patients with node- et al. Abiraterone and increased survival drogen for treatment of advanced prostate
positive prostate cancer after radical in metastatic prostate cancer. N Engl J cancer. Science 2009;324:787-90.
prostatectomy and pelvic lymphadenec- Med 2011;364:1995-2005. 16. Scher HI, Beer TM, Higano CS, et al.
tomy. Lancet Oncol 2006;7:472-9. 10. Chen CD, Welsbie DS, Tran C, et al. Antitumour activity of MDV3100 in cas-
5. Nair B, Wilt T, MacDonald R, Rutks I. Molecular determinants of resistance to tration-resistant prostate cancer: a phase
Early versus deferred androgen suppres- antiandrogen therapy. Nat Med 2004;10: 1-2 study. Lancet 2010;375:1437-46.
sion in the treatment of advanced pros- 33-9. 17. Scher HI, Halabi S, Tannock I, et al.
tatic cancer. Cochrane Database Syst Rev 11. Knudsen KE, Scher HI. Starving the Design and end points of clinical trials
2002;1:CD003506. addiction: new opportunities for durable for patients with progressive prostate
6. Studer UE, Whelan P, Wimpissinger F, suppression of AR signaling in prostate cancer and castrate levels of testosterone:
et al. Differences in time to disease pro- cancer. Clin Cancer Res 2009;15:4792-8. recommendations of the Prostate Cancer
n engl j med nejm.org 9
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
Clinical Trials Working Group. J Clin On- 21. de Bono JS, Oudard S, Ozguroglu M, cologists versus urologists in a US man-
col 2008;26:1148-59. et al. Prednisone plus cabazitaxel or mito- aged care population. Cancer Manag Res
18. Holm S. A simple sequentially rejec- xantrone for metastatic castration-resis- 2011;3:233-45.
tive multiple test procedure. Scand J Stat tant prostate cancer progressing after 24. Lissbrant IF, Garmo H, Widmark A,
1979;6:65-70. docetaxel treatment: a randomised open- Stattin P. Population-based study on use
19. Kantoff PW, Higano CS, Shore ND, et label trial. Lancet 2010;376:1147-54. of chemotherapy in men with castration
al. Sipuleucel-T immunotherapy for cas- 22. Harris V, Lloyd K, Forsey S, Rogers P, resistant prostate cancer. Acta Oncol
tration-resistant prostate cancer. N Engl J Roche M, Parker C. A population-based 2013;52:1593-601.
Med 2010;363:411-22. study of prostate cancer chemotherapy. 25. Parker C, Nilsson S, Heinrich D, et al.
20. Tannock IF, de Wit R, Berry WR, et al. Clin Oncol (R Coll Radiol) 2011;23:706-8. Alpha emitter radium-223 and survival in
Docetaxel plus prednisone or mitoxan- 23. Engel-Nitz NM, Alemayehu B, Parry metastatic prostate cancer. N Engl J Med
trone plus prednisone for advanced pros- D, Nathan F. Differences in treatment 2013;369:213-23.
tate cancer. N Engl J Med 2004;351:1502- patterns among patients with castration- Copyright 2014 Massachusetts Medical Society.
12. resistant prostate cancer treated by on-
10 n engl j med nejm.org
The New England Journal of Medicine
Downloaded from nejm.org on July 5, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
Вам также может понравиться
- Hussain2018 PROSPERДокумент10 страницHussain2018 PROSPERjghcl.221Оценок пока нет
- Nejmoa 1606220Документ10 страницNejmoa 1606220Jay TiwariОценок пока нет
- Estudio CarmenaДокумент11 страницEstudio CarmenaAlfredo BalcázarОценок пока нет
- Enzalutamida arches-JCO.19.00799Документ15 страницEnzalutamida arches-JCO.19.00799Raul BarcellonaОценок пока нет
- Jco 19 00799Документ15 страницJco 19 00799Residentes urologiaОценок пока нет
- AsianJAndrol212107-1644782 043407Документ2 страницыAsianJAndrol212107-1644782 043407FM BujangОценок пока нет
- Prostata Terrain Trial Enzalutamida Vs BicalutamidaДокумент11 страницProstata Terrain Trial Enzalutamida Vs BicalutamidaPaulo Nunes FilhoОценок пока нет
- Kartika Erma Sundari AB212073 - CompressedДокумент33 страницыKartika Erma Sundari AB212073 - Compressedrizky ardikaОценок пока нет
- Nejmoa 2104162Документ11 страницNejmoa 2104162GwasuОценок пока нет
- The Role of Free PSA in The Detection of Prostate Cancer: Your Lab FocusДокумент5 страницThe Role of Free PSA in The Detection of Prostate Cancer: Your Lab FocusSubhasis PandaОценок пока нет
- Lutetium 177-PSMA 617 For MetastaticДокумент13 страницLutetium 177-PSMA 617 For MetastaticpaulobriosОценок пока нет
- Short-Term Metronidazole Not Linked To CancerДокумент1 страницаShort-Term Metronidazole Not Linked To CancerTika Ayu andaniОценок пока нет
- Adjuvant Pertuzumab and Trastuzumab in Early HER2-Positive Breast CancerДокумент10 страницAdjuvant Pertuzumab and Trastuzumab in Early HER2-Positive Breast Cancerfaris nagibОценок пока нет
- Afifah FixedДокумент25 страницAfifah FixedAfifah Nur KartikasariОценок пока нет
- Mrna Vaccine cv9103 and cv9104 For The Treatment of Prostate CancerДокумент8 страницMrna Vaccine cv9103 and cv9104 For The Treatment of Prostate Cancerapi-675909478Оценок пока нет
- Goserelinversuscyclophosphamide, Methotrexate, and Fluorouracilasadjuvanttherapyinpremenopausalpatients Withnode-Positivebreastcancer:Thezoladexearlybreast CancerresearchassociationstudyДокумент11 страницGoserelinversuscyclophosphamide, Methotrexate, and Fluorouracilasadjuvanttherapyinpremenopausalpatients Withnode-Positivebreastcancer:Thezoladexearlybreast CancerresearchassociationstudyRaksha MoghariyaОценок пока нет
- Jurnal LeoДокумент7 страницJurnal LeoyunielsyaОценок пока нет
- Apalutamide For Metastatic, Castration-Sensitive Prostate Cancer TITANДокумент12 страницApalutamide For Metastatic, Castration-Sensitive Prostate Cancer TITANOrlando SotoОценок пока нет
- Ahmed 2011Документ10 страницAhmed 2011skribekbenjaminОценок пока нет
- Jonat 2002Документ8 страницJonat 2002KunalОценок пока нет
- Atezolizumab and Nab-Paclitaxel in Advanced Triple-Negative Breast CancerДокумент14 страницAtezolizumab and Nab-Paclitaxel in Advanced Triple-Negative Breast CancerRodrigoSachiFreitasОценок пока нет
- Ca Mama 2Документ10 страницCa Mama 2MarisolCamposОценок пока нет
- 1 s2.0 S1078143923000893 MainДокумент9 страниц1 s2.0 S1078143923000893 MainJulio MineraОценок пока нет
- J Juro 2018 07 040Документ7 страницJ Juro 2018 07 040wanggaОценок пока нет
- Milta 4Документ14 страницMilta 4Victor RoticivОценок пока нет
- Desktop IiiДокумент9 страницDesktop IiihenryОценок пока нет
- 2014 Article 1491Документ5 страниц2014 Article 1491Glauce L TrevisanОценок пока нет
- The Addition of Pelvic Lymph Node Treatment To Pro - 9Документ2 страницыThe Addition of Pelvic Lymph Node Treatment To Pro - 9gascarteziniОценок пока нет
- Tucatinib, Trastuzumab, and Capecitabine For HER2-Positive Metastatic Breast CancerДокумент13 страницTucatinib, Trastuzumab, and Capecitabine For HER2-Positive Metastatic Breast Cancertpatel0986Оценок пока нет
- Oncology CareДокумент1 страницаOncology CareQuennie Abellon QuimanОценок пока нет
- Inotozumab OzogamicinДокумент14 страницInotozumab OzogamicinTaraОценок пока нет
- Livsey 2003Документ6 страницLivsey 2003Migue PerezОценок пока нет
- New England Journal Medicine: The ofДокумент11 страницNew England Journal Medicine: The ofAlvin JulianОценок пока нет
- Blana 2004Документ4 страницыBlana 2004skribekbenjaminОценок пока нет
- ARA II y Cancer EditorialДокумент2 страницыARA II y Cancer EditorialFabiana MuriasОценок пока нет
- Nejmoa 1406281Документ8 страницNejmoa 1406281zainabativeОценок пока нет
- Swog 8794Документ7 страницSwog 8794yingming zhuОценок пока нет
- Paper 1Документ11 страницPaper 1บอส เลิศเกียรติรัชตะОценок пока нет
- Perez Et Al 2014 Trastuzumab Plus Adjuvant Chemotherapy For Human Epidermal Growth Factor Receptor 2 Positive BreastДокумент10 страницPerez Et Al 2014 Trastuzumab Plus Adjuvant Chemotherapy For Human Epidermal Growth Factor Receptor 2 Positive BreastDaniel Del RíoОценок пока нет
- Aspirine Vs LMWH Nejm2023Документ11 страницAspirine Vs LMWH Nejm2023Esteban DavidОценок пока нет
- Provenge 2Документ12 страницProvenge 2api-675909478Оценок пока нет
- Artículo EpidemiologíaДокумент8 страницArtículo EpidemiologíaSANTIAGO ANDRES PLAZAS MARTINEZОценок пока нет
- Abstracts: Annals of OncologyДокумент1 страницаAbstracts: Annals of OncologyAsaikkutti AnnamalaiОценок пока нет
- NcologistДокумент7 страницNcologistNafia TurariezaОценок пока нет
- CNCR 21619Документ7 страницCNCR 21619Syed Shah MuhammadОценок пока нет
- 03 ON 2020 Prostate WBДокумент43 страницы03 ON 2020 Prostate WBabdullahОценок пока нет
- Ardengh Et Al - 2013 - Accuracy of Endoscopic Ultrasound-Guided Fine-Needle Aspiration in TheДокумент7 страницArdengh Et Al - 2013 - Accuracy of Endoscopic Ultrasound-Guided Fine-Needle Aspiration in TheMaria ChenОценок пока нет
- New England Journal Medicine: The ofДокумент10 страницNew England Journal Medicine: The ofmayracppОценок пока нет
- Aro 96-02auo Ap 0995Документ8 страницAro 96-02auo Ap 0995yingming zhuОценок пока нет
- PHD Thesis On Prostate CancerДокумент5 страницPHD Thesis On Prostate Cancermandyfroemmingfargo100% (2)
- Dna 2Документ8 страницDna 2api-675909478Оценок пока нет
- Management of Prostate CancerДокумент5 страницManagement of Prostate CancerDiego Fernando Alzate GomezОценок пока нет
- Prostate InternationalДокумент5 страницProstate InternationalayuОценок пока нет
- Serum PSA Concentration Is Powerfull Predictor of Acute Urinary Retension and Need For Surgery in Men With BPHДокумент8 страницSerum PSA Concentration Is Powerfull Predictor of Acute Urinary Retension and Need For Surgery in Men With BPHArga Putra PradanaОценок пока нет
- Giant Prolactinomas: Multi-Modal Approach To Achieve Tumor ControlДокумент2 страницыGiant Prolactinomas: Multi-Modal Approach To Achieve Tumor Controlaya PermatasariОценок пока нет
- 1 s2.0 S0302283818300198 MainДокумент7 страниц1 s2.0 S0302283818300198 MainM Rizqi FiryalОценок пока нет
- Nej Mo A 1201637Документ11 страницNej Mo A 1201637GianОценок пока нет
- JurnalДокумент6 страницJurnalNur AnindyaОценок пока нет
- Is Post Operative Radiotherapy Justified For Completely Resected Locally Advanced Renal Cell Cancers? PDFДокумент6 страницIs Post Operative Radiotherapy Justified For Completely Resected Locally Advanced Renal Cell Cancers? PDFRanda HalfianОценок пока нет
- AUA2014 Highlights CRPCДокумент20 страницAUA2014 Highlights CRPCRanda HalfianОценок пока нет
- Management of Macroscopic Haematuria in The Emergency DepartmentДокумент6 страницManagement of Macroscopic Haematuria in The Emergency DepartmentRanda HalfianОценок пока нет
- Toward A Better Understanding of Kidney Stone Disease - Platinum PrioritiesДокумент2 страницыToward A Better Understanding of Kidney Stone Disease - Platinum PrioritiesRanda HalfianОценок пока нет
- Management of Macroscopic Haematuria in The Emergency DepartmentДокумент6 страницManagement of Macroscopic Haematuria in The Emergency DepartmentRanda HalfianОценок пока нет
- Association Between Metabolic Syndrome and The Presence of Kidney Stones in A Screened PopulationДокумент6 страницAssociation Between Metabolic Syndrome and The Presence of Kidney Stones in A Screened PopulationRanda HalfianОценок пока нет
- Bph. Ihushaufihasuifhuiashfashfuias. Ufusufasuifhuiashfisahfuias. UfuasufhasuihfuiashfДокумент8 страницBph. Ihushaufihasuifhuiashfashfuias. Ufusufasuifhuiashfisahfuias. UfuasufhasuihfuiashfBayu SunaryoОценок пока нет
- Prostate Biopsy - The Transperineal ApproachДокумент9 страницProstate Biopsy - The Transperineal ApproachRanda HalfianОценок пока нет
- ASMIUA Presentation Registration FormДокумент1 страницаASMIUA Presentation Registration FormRanda HalfianОценок пока нет
- Collard2001 - Ischemia and ReperfusionДокумент6 страницCollard2001 - Ischemia and ReperfusionRanda HalfianОценок пока нет
- 1 s2.0 030636239400310J MainДокумент7 страниц1 s2.0 030636239400310J MainRanda HalfianОценок пока нет
- Male LUTS 2012 PocketДокумент22 страницыMale LUTS 2012 PocketRanda HalfianОценок пока нет
- How to resize your SIM or microSIM card to nanoSIM format in 4 easy stepsДокумент5 страницHow to resize your SIM or microSIM card to nanoSIM format in 4 easy stepsRanda HalfianОценок пока нет
- Acute ScrotumДокумент9 страницAcute ScrotumIsabel ReyОценок пока нет
- Higher Algebra - Hall & KnightДокумент593 страницыHigher Algebra - Hall & KnightRam Gollamudi100% (2)
- Grandjean 2000Документ13 страницGrandjean 2000Ivan VeriswanОценок пока нет
- Diagnostic Exam TrendsДокумент3 страницыDiagnostic Exam TrendsLee Dumalaga Carinan100% (2)
- 2012 Mirror Therapy For Improving Motor Function After StrokeДокумент68 страниц2012 Mirror Therapy For Improving Motor Function After StrokeMarcelo Ortiz Valenzuela100% (1)
- C1.2 Practice Test - June 2021Документ4 страницыC1.2 Practice Test - June 2021friophotographyОценок пока нет
- Critique PaperДокумент2 страницыCritique PaperQuercusОценок пока нет
- AMDM Unit 3-Study Types (DHS 2020-2021)Документ3 страницыAMDM Unit 3-Study Types (DHS 2020-2021)Stanice LouisОценок пока нет
- EFIC2015 Poster AbstractsДокумент1 066 страницEFIC2015 Poster AbstractsszscribdОценок пока нет
- Hierbas MedicinalesДокумент11 страницHierbas MedicinalesJonathan David Yepes YepezОценок пока нет
- The Ethics of Placebo-Controlled Randomized Clinical TrialsДокумент28 страницThe Ethics of Placebo-Controlled Randomized Clinical TrialsHoney HoneyОценок пока нет
- Clinical Nutrition The Interface Between Metabolism, Diet, and DiseaseДокумент438 страницClinical Nutrition The Interface Between Metabolism, Diet, and DiseaseCris Portillo100% (5)
- Management of TMDДокумент22 страницыManagement of TMDWallisson SoaresОценок пока нет
- Statistics Concepts and Controversies 9th Edition Moore Test Bank DownloadДокумент11 страницStatistics Concepts and Controversies 9th Edition Moore Test Bank DownloadKirk Neri100% (20)
- Acute Alcoholic HepatitisДокумент11 страницAcute Alcoholic HepatitisDoc_NethoОценок пока нет
- Alexander Technique and Feldenkrais Method: A CriticalДокумент16 страницAlexander Technique and Feldenkrais Method: A CriticalAna Carolina PetrusОценок пока нет
- Obesity in Adults: Drug TherapyДокумент36 страницObesity in Adults: Drug TherapyGerman Barrientos CabreraОценок пока нет
- Homeopathic Remedies For The Treatment of Osteoarthritis: A Systematic ReviewДокумент7 страницHomeopathic Remedies For The Treatment of Osteoarthritis: A Systematic ReviewAbdulRahman OmarОценок пока нет
- Ethical Issues of Placebo TreatmentДокумент14 страницEthical Issues of Placebo Treatmentmehrasa nikandishОценок пока нет
- Melatonin as Effective as Amitriptyline for Migraine PreventionДокумент7 страницMelatonin as Effective as Amitriptyline for Migraine PreventionannisaОценок пока нет
- Pharmacology PDFДокумент109 страницPharmacology PDFRanjit TharuОценок пока нет
- Why Is Double-Blind Experiment Scientifically Valuable?: CCHU9021 Critical Thinking in Contemporary SocietyДокумент27 страницWhy Is Double-Blind Experiment Scientifically Valuable?: CCHU9021 Critical Thinking in Contemporary SocietyKaren TseОценок пока нет
- Snel Lorist 2011 CaffeineДокумент13 страницSnel Lorist 2011 Caffeinezrombie7Оценок пока нет
- Panss ScoreДокумент8 страницPanss ScoretriaclaresiaОценок пока нет
- Hydro-, Balneo-, and Spa Treatment in Pain Management PDFДокумент5 страницHydro-, Balneo-, and Spa Treatment in Pain Management PDFfriend717100% (1)
- Short Cases in International Business EthicsДокумент13 страницShort Cases in International Business Ethicsgeeta100% (1)
- Lyman Residents To Vote On Government Form: Storm The Cause of Apartment Building BlazeДокумент20 страницLyman Residents To Vote On Government Form: Storm The Cause of Apartment Building BlazegreercitizenОценок пока нет
- Lyme NeurotoxinsДокумент46 страницLyme NeurotoxinsJohnny Atman100% (1)
- Effectiveness of NonpharmacologicalДокумент13 страницEffectiveness of NonpharmacologicalzumantaraОценок пока нет
- EF Set Aswers 2024Документ12 страницEF Set Aswers 2024Sergio OrdoñezОценок пока нет
- Nano Biofusion GelДокумент8 страницNano Biofusion GelChandra SekharОценок пока нет
- Tocilizumab Giant Cell ArteritisДокумент30 страницTocilizumab Giant Cell ArteritisAnonymous akDD0qОценок пока нет