Академический Документы
Профессиональный Документы
Культура Документы
Rhesus Type and Abo Incompatibility in Jaundiced Neonates
Загружено:
daniel_iosif_glОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Rhesus Type and Abo Incompatibility in Jaundiced Neonates
Загружено:
daniel_iosif_glАвторское право:
Доступные форматы
ORIGINAL ARTICLE
PREVALENCE OF RHESUS TYPE AND ABO
INCOMPATIBILITY IN JAUNDICED NEONATES
Mohammad Irshad, Ameer Mohammad, Mohammad Hussain,
Behram Khan, Nusrat Ali, Ashfaq Ahmad, Mohsin Hayat,
Rahida Karim
Department of Paediatrics and Neonatology,
Lady Reading Hospital, Peshawar - Pakistan
ABSTRACT
Objective: To determine the prevalence of Rh and ABO incompatibility in jaundiced neonates.
Methodology: This hospital based descriptive study was conducted in Pediatrics Unit, Lady Reading
Hospital Peshawar. A total of 200 neonates with clinically diagnosed jaundice were included in the study.
Results: Out of 200 neonates 70% were male and 30%female. Majority of neonates 99.5% age was ranged
from 0-10 days while only 0.5% neonate was 13 days. Out of 200 neonates, the frequency of ABO-
incompatibility and Rh-incompatibility in jaundiced neonates in this study was 22.5% and 12.5%
respectively. Out of the remaining 65.5% cases physiological jaundice was diagnosed in 40.5% neonates,
prematurity in 15% neonates and G6PD in 9.5% neonates. Among 22.5% cases of ABO incompatibility
there were 16.5% males and 6% females. Majority 15% presented on 1st day of life, followed by 3% on 2nd
and 3rd day of life respectively, 1% on 4th day, 0.5% on 5th day of life.
Conclusion: Out of 200 neonates presented with jaundice, prevalence of ABO-incompatibility was found to
be 22.5% followed by Rh-incompatibility 12.5%
Key Words: Neonatal jaundice, hyperbilirubinemia, Kernicterus ABO-incompatibility, Rh-incompatibility.
INTRODUCTION is a condition in which life span of fetal red blood
cells (RBCs) is shortened by the action of maternal
Neonatal jaundice is defined as yellowish
antibodies against the antigens present on RBCs.
discoloration of skin, sclera of eyeball, and
Anti-D is the commonest cause of mild, moderate
mucous membranes caused by deposition of bile
and severe HDN. Red cells destruction begins in
salts in these tissues. Depending upon the cause
intrauterine life and it leads to severe anemia,
the jaundice may be present at birth or any time
during the neonatal period. Jaundice due to either hydrops fetalis and death in utero3.
indirect (unconjugated) or direct (conjugated) The most common cause of jaundice in
bilirubin within the first 24 hours of life should be first 24 hours of life due to HDN is rhesus (Rh)
taken seriously1. hemolytic disease. As the mother becomes
sensitized due to fetomaternal transfusions in
Neonatal Jaundice (NNJ) is a common
previous pregnancies, anti-D IgM and IgG are
disorder worldwide. Early identification and proper
produced. Anti-D IgG is responsible for rhesus
management is needed to prevent the serious
disease in the neonate as this antibody can cross
neurological complications associated with it2.
placenta. Rhesus (Rh) incompatibility develops
Kernicterus or bilirubin encephalopathy is between an Rh-negative mother (previously
a neurological syndrome which results from the sensitized) and her Rh-positive fetus4.
deposition of unconjugated (indirect) bilirubin in
ABO incompatibility (mother usually
the basal ganglia and brain stem nuclei1.
blood group O, infant blood group A or B), is
Hemolytic disease of the newborn (HDN) the most common cause for HDN in the UK and
JPMI 2011 Vol. 25 No. 03 : 233 - 239 233
PREVALENCE OF RHESUS TYPE AND ABO INCOMPATIBILITY IN JAUNDICED NEONATES
occurs in 15% of pregnancies. IgG antibody is criteria presenting through Out-patient department
responsible for this condition also4. ABO (OPD) or accident/emergency department and
incompatibility is a common condition in a admitted in Pediatrics and Neonatology department
newborn baby and causes minimal hemolysis. It of Postgraduate Medical Institute, Lady Reading
may cause elevated levels of bilirubin and anemia Hospital, Peshawar. An informed consent was
but less severe than Rh hemolytic disease5. taken from parents or relatives of the neonates for
further evaluation. Parents were inquired about the
In a local study, HDN was diagnosed in age of presentation of jaundice in the neonates.
82 cases (20.5%) associated with blood group The skin, sclera of eyeball and mucous membrane
incompatibility. In this study ABO incompatibility was examined for jaundice. The required
was more common with 58 cases, while Rh- investigations like serum bilirubin level (total,
incompatibility was diagnosed in 19 cases6. direct and indirect), blood groups of baby and
ABO incompatibility occurs in 20% of mother were done in hospital laboratory for the
pregnancies but only 20% of these develop diagnosis of Rhesus (Rh) and ABO incompatibility
hemolytic disease. In addition to severe jaundice, in jaundiced neonates. All these information and
these infants may also develop significant anemia other demographic data like name, age, sex,
over the first several weeks of life7. address, date of admission and date of discharge
was also entered into a proforma.
Kernicterus is more likely to occur with
bilirubin levels higher than 20 mg/dl. The risk of All the qualitative variables like gender,
kernicterus is less for full term infants as blood groups of baby and mother, diagnostic
compared to pre-term infants. Phototherapy and findings, Rh-incompatibility and ABO-
exchange transfusion are the options available to incompatibility were analyzed for percentages and
avoid the risk of kernicterus7. frequencies. Mean + standard deviation was
calculated for quantitative variables like age and
All the pregnant women should be tested age at the onset of jaundice, weight and serum
for ABO/Rh type and screened for antibody during bilirubin levels (total, direct and indirect). For
the first visit to obstetrician. These initial tests will gender male to female ratio was calculated. The
help to identify women who require anti- results were presented through tables, cross
immunoglobulin (Rh IG) and further monitoring. tabulation, graphs and charts. All the data was
Rh IG administration results in greater than 90% stored and analyzed by statistical program SPSS
reduction in alloimmunization rate among treated version 12 for windows.
women8.
The purpose of the study was to determine RESULTS
the prevalence of Rh and ABO incompatibility in A total of 200 neonates with jaundice were
jaundiced neonates presenting at Department of included in the study. Out of 200 neonates 140
Pediatrics & Neonatology, Lady Reading Hospital, (70%) were male while 60 (30%) were female. The
Peshawar. overall male to female ratio was 2.33: 1 (Table 1).
In majority of neonates 199 (99.5%) age
METHODOLOGY was ranged from 0-10 days, while only 01 (0.5%)
This cross sectional study was conducted neonate was 13 days. Mean age was 3.5585 +
in Department of Pediatrics and Neonatology, Lady 2.5599 days (Table 1).
Reading Hospital, Peshawar for one year from
April 2009 to March, 2010 on 200 neonates, both Out of 200 neonates included in the study,
male and female with clinically diagnosed jaundice 45 were diagnosed as ABO-incompatibility which
makes up 22.5% of the total cases; while 25
included by consecutive (Non probability)
neonates were diagnosed as Rh-incompatibility
sampling.
accounting for 12.5% of the total cases. Therefore
Jaundiced neonates with gestational age the frequency of ABO-incompatibility and Rh-
less than 28 weeks; jaundiced neonates with incompatibility in jaundiced neonates in this study
weight of less than 500 gms; babies with history was 22.5% and 12.5% respectively (Table 1).
of drug intake like Moxalactum and Sulfisoxazole
Out of the remaining 130 (65.5%) cases
and babies whose mothers were hepatitis A IgM
physiological jaundice was diagnosed in 81
positive, HBsAg (hepatitis B surface antigen)
(40.5%) neonates, prematurity in 30 (15%)
positive, and anti-HCV (hepatitis C antibody)
neonates and G6PD in 19 (9.5%) neonates.
positive were excluded from the study.
Cross tabulation of blood grouping of
After getting approval from the hospital
babies and mothers are given in Table 2.
ethical committee to conduct the study, data was
collected of all those neonates who met inclusion Among the 45 (22.5%) cases of ABO
JPMI 2011 Vol. 25 No. 03 : 233 - 239 234
PREVALENCE OF RHESUS TYPE AND ABO INCOMPATIBILITY IN JAUNDICED NEONATES
incompatibility there were 33 (16.5%) males and Among 25 (12.5%) cases of Rh-
12 (6%) females. Majority 30 (15%) presented on incompatibility there were 18 (9%) male and 7
(3.5%) female neonates. Majority 18 (9%) cases
1st day of life, followed by 6 (3%) on 2nd and 3rd
presented on 1st day of life, followed by 3 (1.5%)
day of life respectively, 2 (1%) on 4th day, and 01 on 2nd day of life, 2 (1%) on 4th day, and 01 (0.5%)
(0.5%) on 5th day of life. on 3rd and 6th day of life respectively (Table 3).
Table 1: Demographic Distribution of Patients (n=200)
Variables No. of Cases Percentage
Gender distribution:
Male 140 70%
Female 60 30%
Age ranges
0-10 days 199 99.5%
11-29 days 01 0.5%
Frequency of rhesus and
ABO-incompatibility:
ABO-incompatibility 45 22.5%
Rhesus-incompatibility 25 12.5%
01 day 90 45%
02 days 24 12%
03 days 54 27%
04 days 15 7.5 %
05 days 07 3.5%
06 day 03 1.5%
07 days 05 2.5%
08 days 02 01%
Table 2: Cross Tabletion of Blood Groups of Neonates and Mothers
Blood Group of Mothers
Blood
Groups A+ A- AB+ AB- B+ B- O+ O- Total
A+ 37 3 2 1 22 1 66
A- 3 2 5
AB+ 3 3 2 1 9
-
Blood Group AB 1 1
of Neonates B+ 1 3 1 42 6 16 3 72
-
B 1 1 2
+
O 6 5 1 23 5 40
-
O 2 3 5
Total 49 6 8 2 50 10 63 12 200
JPMI 2011 Vol. 25 No. 03 : 233 - 239 235
PREVALENCE OF RHESUS TYPE AND ABO INCOMPATIBILITY IN JAUNDICED NEONATES
Table 3: Cross Tabulation of Sex and Age of Presentation of Jaundice in Neonates (n=200)
Sex Age of presentation of jaundice in neonates (in days) Total
Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Day 8
ABO-incompatibility Male 18 6 6 1 2 - - - 33
Female 12 - - - - - - - 12
Total 30 6 6 1 2 - - - 45
Rhesus-incompatibility Male 14 2 - 2 - - - - 18
Female 04 1 1 - - 1 - - 07
Total 18 3 1 2 - 1 - - 25
DISCUSSION Neonatal jaundice is the most common
medical problem affecting babies in the first week
Newborns with jaundice or unrecognized
of life. About 50% of term and 80% of preterm
hyperbilirubinemia are a vulnerable population. Of
babies develop jaundice, which usually appears 2-4
the 4 million infants born each year in the United
days after birth and resolves spontaneously after 1-
States, over 3.5 million are born at 35 or more 2 weeks. Jaundice is caused by bilirubin deposition
weeks of gestation. Most have benign outcomes in the skin. Most jaundice in newborn infants is a
with little or no threat of neurological compromise result of increased red cell breakdown and
from medical conditions during their first year of decreased bilirubin excretion11,12 .
life. Nearly all healthy infants have some degree
of hyperbilirubinemia and over 60% develop In this study majority of neonates 45%
jaundice during their first week of life. When presented with jaundice on day 01 of their life
unmonitored or untreated in a timely manner, followed by 27% on day 03 of their life. These
11, 12
hyperbilirubinemia can become excessive and may results are comparable with the studies in which
be unrecognized if the infant is not under medical it is also mentioned that neonatal jaundice usually
supervision.9 appears 2-4 days after birth.
Neonatal jaundice is usually harmless, this Hyperbilirubinemia is a common disorder
condition is often seen in infants around the during the neonatal period. It is associated with
second day after birth, lasting until day 8 in a variety of physiologic and pathologic conditions.
normal births, or to around day 14 in premature Isoimmune hemolytic disease has been
births. Serum bilirubin normally drops to a low identified as a pathologic cause of neonatal
level without any intervention required: the hyperbilirubinemia attributed to blood group
jaundice is presumably a consequence of metabolic incompatibility. Group A and group B newborns of
and physiological adjustments after birth. In group O mothers are defined as having ABO
extreme cases, a brain-damaging condition known incompatibility 1 3 . In our study out of 200
as kernicterus can occur, leading to significant neonates, the prevalence of ABO-incompatibility in
lifelong disability. There are concerns that this jaundiced neonates was 22.5%.
condition has been rising in recent years due to ABO incompatibility and glucose-6-
inadequate detection and treatment of neonatal phosphate dehydrogenase (G6PD) deficiency are
hyperbilirubinemia. Early treatment often consists the most common causes of hemolytic anemia. If
of exposing the baby to intensive phototherapy.10 these conditions are present, phototherapy and
JPMI 2011 Vol. 25 No. 03 : 233 - 239 236
PREVALENCE OF RHESUS TYPE AND ABO INCOMPATIBILITY IN JAUNDICED NEONATES
exchange transfusion may be considered at lower positive because the infant's red blood cells are
TSB levels because these conditions can cause coated with maternal antibodies. These cells will
predictably severe hyperbilirubinemia14. G6PD was be hemolyzed, putting the infant at risk for severe
diagnosed in 9.5% neonates out of 200 neonates hyperbilirubinemia14.
included in this study.
Majority of neonates in this study were
In this study out of 200 neonates, the having blood group B+ followed by A+ with the
frequency of ABO-incompatibility and Rh- frequencies of 37.5% and 31% respectively. The
incompatibility in jaundiced neonates was 22.5% distribution of ABO blood group varies world-
and 12.5% respectively. Our results are in wide. Blood group O was the most common blood
agreement with the studies done abroad 14,15 and group found in one local study and other
6,16
local studies . They all agree that ABO- international studies except in Nepal where A was
incompatibility was more prevalent than Rh the most common (34%) and O was 1.5% less
incompatibility in their studies. common (32.5%) than A23-26. With few exceptions
ABO blood group distribution in various ethnic
In one study factors associated with severe
groups in one local study27 was not significantly
neonatal jaundice in babies requiring exchange
different from each other. While it was compared
blood transfusion (EBT) included low birth weight
with earlier studies performed, by Majeed T et al28
(<2500 g, 44.4%), ABO incompatibility (30.0%),
on 3000 subjects in Lahore, and by Bhatti FA29 in
glucose-6-phosphate dehydrogenase deficiency
Rawalpindi, blood group B was the most frequent
(34.4%) and septicemia (26.1%). Twenty-seven
(30.0%) neonates developed features of (35.8%) blood group. In another local study27 the
kernicterus; 26 before admission while 1 during authors found blood group B was the most
admission; all except one were delivered outside frequent blood group in Arain (40.5%), and blood
group O was less common (24.7%) while it was
the hospital17.
the most frequent blood group among Awans,
Jaundice in the newborn is a problem Rajputs, miscellaneous Punjabi sub casts, Balochs,
because elevation of serum bilirubin is potentially Sindhis, and Pathans that has not been documented
toxic to infant's developing central nervous in earlier studies, however it agreed with the study
system18. performed by Bhatti R 30 in Sindh on 38,000
Neonatal jaundice is the result of an subjects, and by Mian et al31 in Multan on 1632
imbalance between bilirubin production and subjects. This difference may be due to difference
of sample sizes of these studies and requires
elimination. Bilirubin conjugation in newborns is
further comprehensive studies to confirm.
significantly impaired in the first few days; even a
small increase in the rate of production can
contribute to the development of hyperbilir-
CONCLUSIONS
ubinemia19. In our study in 200 neonates with Out of 200 neonates presented with
jaundice mean total serum bilirubin was 20.0878 + jaundice, frequency of ABO-incompatibility was
5.6424. Mean direct serum bilirubin was 2.7711 + found to be 22.5% followed by Rh-incompatibility
4.510. Mean indirect serum bilirubin was 17.9630 12.5%. Majority of neonates with jaundice
+ 4.6841. presented on their first day of life with the
frequency of 45%.
Some 60% of normal newborns become
clinically jaundiced sometime during the first week REFERENCES
of life. Unconjugated (indirect) hyperbilirubinemia
occurs as a result of excessive bilirubin formation 1. Kliegman RM. Digestive system disorders:
and because the neonatal liver cannot clear jaundice and hyperbilirubinemia in the
bilirubin rapidly enough from the blood. Although newborn. In: Behrman RE, Kliegman RM,
most newborns with jaundice are otherwise healthy, Jenson HB, editors. Nelson's textbook of
they need to be monitored because bilirubin is pediatrics. 18th ed. New Delhi: Saunders,
potentially toxic to the central nervous system. 2008.p.756-66.
Sufficiently elevated levels of bilirubin can lead to 2. Eneh AU, Ugwu RO. Perception of neonatal
bilirubin encephalopathy and subsequently jaundice among women attending children out
kernicterus, with devastating, permanent patient and immunization clinics of the UPTH
neurodevelopmental handicaps20-22. Port Harcourt. Niger J Clin Pract 2009;12:187-
91.
Blood type and Coombs' testing should be
performed in all infants who are receiving 3. Shaheen R, Subhan F, Tahir F. Severe Rh-D
phototherapy or whose bilirubin level is increasing alloimmunisation: a miraculous suppression of
rapidly. In infants with isoimmune hemolysis immunogenicity. Pak J Med Res 2005:44:133-
(ABO incompatibility), the Coombs' test will be 5.
JPMI 2011 Vol. 25 No. 03 : 233 - 239 237
PREVALENCE OF RHESUS TYPE AND ABO INCOMPATIBILITY IN JAUNDICED NEONATES
4. McIntosh N, Stenson B. The newborn. In: M, Izhar TS, Qureshi AW. Complications and
McIntosh N, Helms PJ, Symth RL, editors. immediate clinical outcome of exchange
Forfar & Arneil's textbook of pediatrics. 6th transfusion in Neonatal hyperbilirubinemia.
e d . E d i n b u rg h : C h u r c h i l l L i v i n g s t o n e , Pak Paed J 2005;29:3-8.
2003.p.177-391.
17. Owa JA, Ogunlesi TA. Why we are still doing
5. Drabik-Clary K, Reddy VV, Benjamin WH, so many exchange blood transfusion for
Boctor FN. Severe hemolytic disease of the neonatal jaundice in Nigeria. World J Pediatr
newborn in a group B African-American infant 2009;5:51-5.
delivered by a group O mother. Ann Clin Lab 18. Maisels MJ. Neonatal jaundice. Pediatr Rev
Sci 2006:36:205-7. 2006;27:443-54.
6. Waheed I, Chishti AL, Alvi A, Iqbal A. 19. Cakmak A, Calik M, Atas A, Hirfanoglu I,
Hemolytic disease of newborn: Can we meet Erel O. Can haptoglobin be an indicator for
this challenge? Pak Paediatr J 2005;29:129-32. the early diagnosis of neonatal jaundice? J
7. Thilo EH, Rosenburg AA. The newborn infant: Clin Lab Anal 2008;22:409-14.
common problems in the newborn infant: 20. American Academy of Pediatrics Subcomm-
neonatal jaundice. In: Hay WW, Levin MJ, ittee on Hyperbilirubinemia. Management of
Sondheimer JM, Deterding RR, (edi). Current hyperbilirubinemia in the newborn infant 35 or
pediatric diagnosis and treatment. 18th ed. more weeks of gestation. Pediatrics 2004;114
New York: Lange Medical Books/McGraw- :297-316.
Hill, 2007.p.11-7.
21. Maisels MJ, Kring EA. Does intensive
8. Eder AF. Alloimmune hemolytic disease of the phototherapy produce hemolysis in newborns
fetus and newborn. In: Greer JP, Foerster J, of 35 or more weeks gestation? J Perinatol
Lakens JN, Rodgers GM, Paraskevas F, Glader 2006;26:498-500.
B, eds. Wintrobe's clinical hematology. 11th
ed. Philadelphia: Lippincott Williams & 22. Maisels MJ, McDonagh AF. Phototherapy for
Wilkins, 2004.p.1183-1202. neonatal jaundice. N Engl J Med 2008;358:
920-8.
9. Bhutani VK, Johnson L. Prevention of severe
neonatal hyperbilirubinemia in healthy infants 23. Das PK, Nair SC, Harris VK, Rose D,
of 35 or more weeks of gestation: Mammen JJ, Bose YN, et al. Distribution of
implementation of a systems-based approach ABO and RhD blood group among blood
[Editorial]. J de Pediatria 2007;83:289-93. donors in a tertiary care center in South India.
Trop Doct 2001;31:47-8.
10. Wikipedia, the free encyclopedia. Jandice.
[Online] 2010 [Cited on 2010, April 10]. 24. Mwangi J. Blood group distribution in an
Av a i l a b l e f r o m : U R L : / / h t t p : / / w w w. e n / urban population of patient targeted blood
wikipedia.org/wiki/jandice.htm donors. East Afr Med J 1999;76:615-8.
11. Skae MS, Moise J, Clarke P. Is current 25. Omotade OO, Adeyemo AA, Kayode CM,
management of neonatal jaundice evidence Falade SL, Ikpeme S. Gene frequencies of
based? Arch Dis Child Fetal Neonatal Ed ABO and Rh (D) blood group alleles in a
2005;90:F540. healthy infant population in Ibadan, Nigeria.
West Afr J Med 1999;18:294-7.
12. Evans D. Neonatal jaundice. Clin Evid
(Online) 2007;pii:0319. 26. Pramanik T, Pramanik S. Distribution of ABO
and Rh blood groups in Nepalese medical
13. Weng YH, Chiu YW. Spectrum and outcome students: a report. East Mediterr Health J
analysis of marked neonatal hyperbiliru- 2000;6:156-8.
binemia with blood group incompatibility.
Chang Gung Med J 2009;32: 400-7. 27. Ali N, Anwar M, Bhatti FA, Nadeem M,
Nadeem A, Ali AM. Frequency of ABO and
14. Moerschel SK, Cianciaruso LB, Tracy LR. A Rh blood groups major ethnic groups and casts
practical approach to neonatal jaundice. Am of Pakistan. Pak J Med Sci 2005;21:26-9.
Fam Physician 2008;77:1255-62.
28. Majeed T, Hayee A. Prevalence of ABO blood
15. Khattak ID, Khan TM, Khan P, Shah SMA, groups and subgroups in a population of
Khattak ST, Ali A. Frequency of ABO and Lahore. Biomedica 2002;18:11-5.
rhesus blood groups in district Swat,
29. Bhatti FA, Amin M. Spectrum of ABO and D
Pakistan. J Ayub Med Coll 2008;20:127-9.
blood groups of donors at Rawalpindi/
16. Masood MK, Afridi IUK, Rizwan M, Yaqoob Islamabad. Pak J Pathol 1996;7:26-8.
JPMI 2011 Vol. 25 No. 03 : 233 - 239 238
PREVALENCE OF RHESUS TYPE AND ABO INCOMPATIBILITY IN JAUNDICED NEONATES
30. Bhatti R. Frequency of ABO and Rh (D) 31. Mian A, Farooq A. Distribution of ABO and
Blood Groups in human population of RH blood group alleles in different
southern Sindh (Pakistan). Ann King Edward populations of southern Punjab, Pakistan.
Med Coll 1998;4:32-3. Anthropol ANZ 1999;57:33-9.
Address for Correspondence:
Dr. Mohammad Irshad
Senior Registrar
Department of Paediatrics and Neonatology,
Lady Reading Hospital, Peshawar - Pakistan
JPMI 2011 Vol. 25 No. 03 : 233 - 239 239
Вам также может понравиться
- Hemolitic AutoimunДокумент3 страницыHemolitic Autoimun08- Ridho Nur CahyoОценок пока нет
- Geme 1Документ9 страницGeme 1นีล ไบรอันОценок пока нет
- Inkompatibilitas DarahДокумент3 страницыInkompatibilitas DarahIntan PermataОценок пока нет
- Association of ABO and RH Incompatibility With NeonatalДокумент8 страницAssociation of ABO and RH Incompatibility With NeonatalMer RodriguezОценок пока нет
- BB OriginalДокумент14 страницBB Originalstone siehОценок пока нет
- NeamtuSimonaDaniela RJME 63 1 2022Документ7 страницNeamtuSimonaDaniela RJME 63 1 2022Boldeanu MVОценок пока нет
- Identi Fication and Management of Fetal Anaemia: A Practical GuideДокумент10 страницIdenti Fication and Management of Fetal Anaemia: A Practical GuideSaeed HasanОценок пока нет
- Aetiology, Diagnosis and Treatment of Hydrops FoetalisДокумент10 страницAetiology, Diagnosis and Treatment of Hydrops FoetalisMargareta OktavianiОценок пока нет
- Anemia FetalДокумент9 страницAnemia FetalCarolina Cabrera CernaОценок пока нет
- Haemolytic Disease of The Fetus and Newborn: ReviewДокумент15 страницHaemolytic Disease of The Fetus and Newborn: ReviewBEREKETОценок пока нет
- Hemolytic Disease Newborn PDFДокумент6 страницHemolytic Disease Newborn PDFlokita_opdОценок пока нет
- Ijph 45 558 PDFДокумент11 страницIjph 45 558 PDFArifah Azizah ArifinОценок пока нет
- Rhalloimmunization 180317110948Документ57 страницRhalloimmunization 180317110948BIRHANE TESFAYОценок пока нет
- Knowledge Level and Determinants of Neonatal Jaundice A Cross-Sectional Study in The Effutu Municipality of GhanaДокумент10 страницKnowledge Level and Determinants of Neonatal Jaundice A Cross-Sectional Study in The Effutu Municipality of GhananicloverОценок пока нет
- Role of Intravenous ImmunoglobulinДокумент4 страницыRole of Intravenous ImmunoglobulinZamir Eid Paez MojicaОценок пока нет
- Abo IncompatabilityДокумент3 страницыAbo Incompatabilityx483xDОценок пока нет
- Jurnal Reading 1Документ16 страницJurnal Reading 1Hana NabilaОценок пока нет
- Causes of Indirect Hyperbilirubinemia in NeonatesДокумент4 страницыCauses of Indirect Hyperbilirubinemia in NeonatesRahmah WantiОценок пока нет
- Jurnal Internasional 3Документ4 страницыJurnal Internasional 3P17312215223 LINDA ANISAОценок пока нет
- Jemc V5i2 23384Документ6 страницJemc V5i2 23384Students CBUОценок пока нет
- Red Cell AlloimmunizationДокумент54 страницыRed Cell Alloimmunizationበአምላክ ጋሻዬ በዛОценок пока нет
- Risk Factors For Neonatal Hyperbilirubinemia: A Case Control StudyДокумент5 страницRisk Factors For Neonatal Hyperbilirubinemia: A Case Control StudyRajba NazalahОценок пока нет
- Haemolytic Disease of The Fetus andДокумент16 страницHaemolytic Disease of The Fetus andkallaliОценок пока нет
- RH IncompatibilityДокумент4 страницыRH IncompatibilityMADULI, Marlone G.Оценок пока нет
- Seminars in Fetal & Neonatal Medicine: Ross M. FasanoДокумент7 страницSeminars in Fetal & Neonatal Medicine: Ross M. FasanoRenzo Donato Sairitupa RamirezОценок пока нет
- Risk Factors For Kernicterus in Neonatal JaundiceДокумент4 страницыRisk Factors For Kernicterus in Neonatal JaundicePusparasmi Mas Ayu SuprabhaОценок пока нет
- Scifed: PublishersДокумент6 страницScifed: PublishersNadiarosmaliaОценок пока нет
- Gomella's Neonatology, 8th Edition 2020, EdithДокумент62 страницыGomella's Neonatology, 8th Edition 2020, Edithmaryano 0015Оценок пока нет
- A Comparative Clinical Investigation of Hyper Bilirubinemia in Babies With Low and Normal Birth WeightsДокумент14 страницA Comparative Clinical Investigation of Hyper Bilirubinemia in Babies With Low and Normal Birth WeightsInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- 1008-Main Article Text (Blinded Article File) - 2118-3-10-20200715Документ3 страницы1008-Main Article Text (Blinded Article File) - 2118-3-10-20200715putrinrainiОценок пока нет
- Share 'RH Neg Final - 23.6Документ80 страницShare 'RH Neg Final - 23.6AppuОценок пока нет
- The Prevalence and Risk Factors For Hyperbilirubinemia in NeonatesДокумент4 страницыThe Prevalence and Risk Factors For Hyperbilirubinemia in NeonatesIJAR JOURNALОценок пока нет
- Maternal antibodies attack fetal red blood cells in HDNДокумент7 страницMaternal antibodies attack fetal red blood cells in HDNLara CarisaОценок пока нет
- Recurrent Non-Immune Fetal Hydrops: A Case ReportДокумент3 страницыRecurrent Non-Immune Fetal Hydrops: A Case ReportHervi LaksariОценок пока нет
- Prenatal Imaging Features Suggestive of Liver Gestational Allo Immune DiseaseДокумент4 страницыPrenatal Imaging Features Suggestive of Liver Gestational Allo Immune DiseaseEuis NoorhayatyОценок пока нет
- Nonimmune Hydrops: Presenting Signs and SymptomsДокумент9 страницNonimmune Hydrops: Presenting Signs and Symptomsdian_067Оценок пока нет
- Pone 0197855Документ10 страницPone 0197855priyaОценок пока нет
- Care of Mothers with Post-term Pregnancy, Pseudocyesis and RH IncompatibilityДокумент3 страницыCare of Mothers with Post-term Pregnancy, Pseudocyesis and RH IncompatibilityCatherine PradoОценок пока нет
- Peptic UlcerДокумент3 страницыPeptic UlcerzikraalfaОценок пока нет
- Hyperbilirubinemia PaperДокумент7 страницHyperbilirubinemia Paperapi-641541726Оценок пока нет
- Hemolytic Disease of The Newborn A ReviewДокумент11 страницHemolytic Disease of The Newborn A ReviewririlibertiОценок пока нет
- E925 FullДокумент7 страницE925 FullDaeng Fahryanzi AzhariОценок пока нет
- Neonatal Anemia (About 162 Cases)Документ4 страницыNeonatal Anemia (About 162 Cases)IJAR JOURNALОценок пока нет
- Acute Respiratory Distress Syndrome Among Premature Neonates: Prevalence, Mortality Rate and Risk Factors of MortalityДокумент5 страницAcute Respiratory Distress Syndrome Among Premature Neonates: Prevalence, Mortality Rate and Risk Factors of MortalityInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Prevalence and Causes of Neonatal Jaundice in Nepali HospitalДокумент4 страницыPrevalence and Causes of Neonatal Jaundice in Nepali HospitalkattysarkОценок пока нет
- Fped 09 801955Документ9 страницFped 09 801955YandiОценок пока нет
- Impact of Rhesus Disease On The Global Problem of Bilirubin-Induced Neurologic DysfunctionДокумент4 страницыImpact of Rhesus Disease On The Global Problem of Bilirubin-Induced Neurologic DysfunctionRahmayani IsmaОценок пока нет
- Journal ABOДокумент4 страницыJournal ABORIta KameliaОценок пока нет
- Kern IcterusДокумент4 страницыKern IcterusAlwin SoetandarОценок пока нет
- Hemolytic DiseaseДокумент10 страницHemolytic DiseaseChino Paolo SamsonОценок пока нет
- HEMOLYTIC DISEASE OF THE NEWBORN - Docx PrintДокумент6 страницHEMOLYTIC DISEASE OF THE NEWBORN - Docx PrintJudy HandlyОценок пока нет
- Effect of Pregnancy Induced Hypertension on Mothers and Babies Hematological ProfilesДокумент3 страницыEffect of Pregnancy Induced Hypertension on Mothers and Babies Hematological ProfilesAbdifatah AhmedОценок пока нет
- Haemolytic Disease of The NewbornДокумент46 страницHaemolytic Disease of The Newborntan_kit_1100% (1)
- What Is Hemolytic Disease of The Newborn?Документ6 страницWhat Is Hemolytic Disease of The Newborn?Loreth Aurea OjastroОценок пока нет
- 33 59 1 SMДокумент5 страниц33 59 1 SMQobert KEeОценок пока нет
- Neonatal Jaundice - StatPearls - NCBI BookshelfДокумент14 страницNeonatal Jaundice - StatPearls - NCBI BookshelfDhany karubuyОценок пока нет
- Rh-INCOMPATIBILITYДокумент14 страницRh-INCOMPATIBILITYNithiya NadesanОценок пока нет
- Prognostic Factors and Clinical Features in Liveborn Neonates With Hydrops FetalisДокумент6 страницPrognostic Factors and Clinical Features in Liveborn Neonates With Hydrops FetalisWulan CerankОценок пока нет
- Pediatric Immunology: A Case-Based Collection with MCQs, Volume 2От EverandPediatric Immunology: A Case-Based Collection with MCQs, Volume 2Оценок пока нет
- Essential Gas Pipe Network Data Management in Arcgis: April 2019Документ22 страницыEssential Gas Pipe Network Data Management in Arcgis: April 2019daniel_iosif_glОценок пока нет
- Ac DTC CheckДокумент8 страницAc DTC Checkdaniel_iosif_glОценок пока нет
- Ac DTC CheckДокумент8 страницAc DTC Checkdaniel_iosif_glОценок пока нет
- Specification For Safe Working in The Vicinity of CadentДокумент15 страницSpecification For Safe Working in The Vicinity of Cadentdaniel_iosif_glОценок пока нет
- Optimization of Biodiesel Production From Sunflower OilДокумент5 страницOptimization of Biodiesel Production From Sunflower Oildaniel_iosif_glОценок пока нет
- ServiceOperationsGuide 062608 PDFДокумент62 страницыServiceOperationsGuide 062608 PDFdaniel_iosif_glОценок пока нет
- BGT Cloud Computing ExtractДокумент34 страницыBGT Cloud Computing ExtractAnuj SharmaОценок пока нет
- Ac DTC CheckДокумент8 страницAc DTC Checkdaniel_iosif_glОценок пока нет
- D815 Metric Section2 Belt and Chain Drives PDFДокумент245 страницD815 Metric Section2 Belt and Chain Drives PDFdaniel_iosif_glОценок пока нет
- ReadmeДокумент1 страницаReadmedaniel_iosif_glОценок пока нет
- Divi Snippets BookДокумент51 страницаDivi Snippets Bookdaniel_iosif_glОценок пока нет
- Emerging-Risks Medical MalpracticeДокумент1 страницаEmerging-Risks Medical Malpracticedaniel_iosif_glОценок пока нет
- Forbes Saudi ArabiaДокумент14 страницForbes Saudi Arabiadaniel_iosif_glОценок пока нет
- BiodieselДокумент36 страницBiodieselda8d8ash8Оценок пока нет
- Jurnal Biodiesel SunflowerДокумент6 страницJurnal Biodiesel SunflowerTaufik HidayatОценок пока нет
- Us 4459731Документ7 страницUs 4459731daniel_iosif_glОценок пока нет
- 151 D00004 PDFДокумент4 страницы151 D00004 PDFdaniel_iosif_glОценок пока нет
- Clean Cities Fact Sheet Straight Vegetable Oil As A Diesel Fuel PDFДокумент2 страницыClean Cities Fact Sheet Straight Vegetable Oil As A Diesel Fuel PDFdaniel_iosif_glОценок пока нет
- Recommended Practice For Occupational Safety For Onshore Oil and Gas Production OperationsДокумент36 страницRecommended Practice For Occupational Safety For Onshore Oil and Gas Production Operationsdaniel_iosif_glОценок пока нет
- GrantPrideco Drill Pipe Data TablesДокумент24 страницыGrantPrideco Drill Pipe Data TablesMaximo Biarrieta RodriguezОценок пока нет
- Make Your Own BiofuelДокумент6 страницMake Your Own Biofueldaniel_iosif_glОценок пока нет
- Pedia Nr-4 2008 Art-6 PDFДокумент11 страницPedia Nr-4 2008 Art-6 PDFdaniel_iosif_glОценок пока нет
- Concentric Tubing Completion System for Communicating Fluids Between a Surface Structure and Subsea WellboreДокумент21 страницаConcentric Tubing Completion System for Communicating Fluids Between a Surface Structure and Subsea Wellboredaniel_iosif_glОценок пока нет
- Oilfield Acronym Update Aug 2015Документ37 страницOilfield Acronym Update Aug 2015Eswar PrasadОценок пока нет
- Uhlted States Patent (19) (11) Patent Number: 4,579,373: Neal Et Al. (45) Date of Patent: Apr. 1, 1986Документ5 страницUhlted States Patent (19) (11) Patent Number: 4,579,373: Neal Et Al. (45) Date of Patent: Apr. 1, 1986daniel_iosif_glОценок пока нет
- MuseScore enДокумент227 страницMuseScore endaniel_iosif_glОценок пока нет
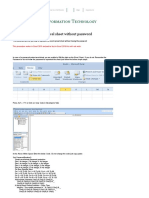
- How To Unprotect An Excel Sheet Without PasswordДокумент3 страницыHow To Unprotect An Excel Sheet Without Passworddaniel_iosif_glОценок пока нет
- Drilling ProblemsДокумент59 страницDrilling ProblemsRaghav Kiran100% (3)
- The Pathophysiology of AmenorrheaДокумент6 страницThe Pathophysiology of AmenorrheaTri Suci UtamiОценок пока нет
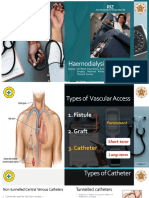
- Haemodialysis CatheterДокумент10 страницHaemodialysis CatheterRizqi AhmadОценок пока нет
- Understanding 1st, 2nd and 3rd Degree Heart BlocksДокумент3 страницыUnderstanding 1st, 2nd and 3rd Degree Heart BlockslhenОценок пока нет
- Leading Causes of Mortality - Department of Health WebsiteДокумент14 страницLeading Causes of Mortality - Department of Health WebsiteRippie RifdahОценок пока нет
- DecongestantsДокумент3 страницыDecongestantskОценок пока нет
- The New Biology and Pharmacology of GlucagonДокумент46 страницThe New Biology and Pharmacology of GlucagonAntonio SalemeОценок пока нет
- Ebook PDF Developmental Biology 12th Edition PDFДокумент41 страницаEbook PDF Developmental Biology 12th Edition PDFjanet.dicks248100% (36)
- Analgesia AvesДокумент16 страницAnalgesia AvesJESSICA ZAPATAОценок пока нет
- Ppe4 Reflection AssignmentДокумент11 страницPpe4 Reflection Assignmentapi-318846856100% (1)
- Dirty Genes Course Copy 1Документ181 страницаDirty Genes Course Copy 1Rachel Bruce50% (4)
- HXX N3ur0anat0myyДокумент29 страницHXX N3ur0anat0myyLINDSLEY GOОценок пока нет
- Enteral NutritionДокумент11 страницEnteral NutritionEso Soso0% (1)
- Figure 1 Human Nervous System Source:courses - Lumenlearning.c Om/microbiology/chapter/anato My-Of-The-Nervous-SystemДокумент14 страницFigure 1 Human Nervous System Source:courses - Lumenlearning.c Om/microbiology/chapter/anato My-Of-The-Nervous-SystemShekaina Faith Cuizon LozadaОценок пока нет
- MicronutrientsДокумент21 страницаMicronutrientsJohn Paolo OcampoОценок пока нет
- Osmosis Diffusion Active - Transport+studentДокумент35 страницOsmosis Diffusion Active - Transport+studentMetaknight360 LiveОценок пока нет
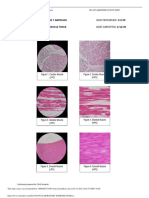
- The Tongue of Leopard Gecko (Eublepharis Macularius) LMДокумент9 страницThe Tongue of Leopard Gecko (Eublepharis Macularius) LMSandra Clavero ClopèsОценок пока нет
- Ch.12 Getting the measure of hormones講義Документ7 страницCh.12 Getting the measure of hormones講義邱小瀧Оценок пока нет
- NCP-Case Presentation (CHF)Документ4 страницыNCP-Case Presentation (CHF)Jessamine EnriquezОценок пока нет
- 8 Curious Meridians Exercises for LongevityДокумент6 страниц8 Curious Meridians Exercises for Longevitypeter911x100% (2)
- Nursing Care Plans for Acute Pain, Hyperthermia, Activity Intolerance, and Infection RiskДокумент20 страницNursing Care Plans for Acute Pain, Hyperthermia, Activity Intolerance, and Infection RiskNursidar Pascual Mukattil80% (5)
- Xylazine HCLДокумент7 страницXylazine HCLGPrime RОценок пока нет
- Structure of BacteriaДокумент13 страницStructure of BacteriaRirin UtariОценок пока нет
- HBCJ Npev Vedw T60B PDFДокумент20 страницHBCJ Npev Vedw T60B PDFAnonymous fPQaCe8Оценок пока нет
- Peripheral Testosterone MetabolismДокумент8 страницPeripheral Testosterone MetabolismAgung SentosaОценок пока нет
- Vol IДокумент273 страницыVol IReza ParkerОценок пока нет
- % Chapter 3: Regulation of Gas Content in BloodДокумент33 страницы% Chapter 3: Regulation of Gas Content in BloodK CОценок пока нет
- Blueprint of LifeДокумент42 страницыBlueprint of Lifesophiehee1234Оценок пока нет
- Laboratory Exercise No.8Документ3 страницыLaboratory Exercise No.8yumi castroОценок пока нет
- A Presentation On Pantothenic Acid or b5Документ28 страницA Presentation On Pantothenic Acid or b5jainsaketОценок пока нет
- Effects of Social Media On The Psychology of PeopleДокумент6 страницEffects of Social Media On The Psychology of PeopleIJAFRCОценок пока нет