Академический Документы
Профессиональный Документы
Культура Документы
Harle V 2016
Загружено:
Asri Ayuning KusumaОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Harle V 2016
Загружено:
Asri Ayuning KusumaАвторское право:
Доступные форматы
Original article
Long-term outcome of neonates with suspected
Hirschsprungs disease, but normal rectal biopsy
Daniel Harleva, Oleg Kharenkoa, Jacob Waxmana, Tanya Frankela, Dan Turnera,b and Oren Leddera,b
Background and objectives Hirschsprungs disease (HD) must always be considered in very early-onset constipation.
Although HD has a well-described clinical course, little is known about those neonates in whom HD was excluded. We aimed to
describe the long-term clinical outcomes of neonates with a clinical suspicion of HD that was excluded by rectal suction biopsy.
Methods This is a single-center double-cohort comparative study. Neonates who underwent rectal mucosa biopsy for
suspected HD were age and sex matched with healthy controls. A survey on clinical outcomes, stooling patterns, and other
gastrointestinal (GI)-related conditions was sent to parents. Pathology slides were re-reported by an experienced histopathologist
blinded to the clinical data.
Results A total of 51 neonates were included [25 cases, 26 controls; 41% males, median time of follow-up 4.25 years
(interquartile range 2.76.9)]. Nine (36%) of patients in the case group required prolonged laxative use for constipation during the
rst year of life compared with 0 (0%) controls (P < 0.001). This difference was maintained at the end of follow-up, with 5 (20%)
versus 0 (0%), respectively (P = 0.02). Case neonates were signicantly more likely to be hospitalized or to be diagnosed with a
chronic GI-related condition than the controls (33 vs. 12%, P = 0.01; and 19 vs. 8%, P = 0.04, respectively).
Conclusion Neonatal constipation is associated with long-term GI-related disorders and should be considered clinically
signicant even when the diagnosis of HD is excluded. Neonates with early-onset abnormal stooling patterns should be
monitored with adequate pediatrician or pediatric gastroenterologist follow-up. Eur J Gastroenterol Hepatol 28:917922
Copyright 2016 Wolters Kluwer Health, Inc. All rights reserved.
Introduction these variant HD disorders, ganglion cells are present on
rectal suction biopsy, but may be atypical in number (e.g.
Hirschsprungs disease (HD), also known as congenital
hyperganglionosis and hypoganglionosis) or in phenotyp-
aganglionic megacolon, is a congenital disorder in which
ing (e.g. immature or small ganglion cells). Described
ganglion cells are absent in the colon, causing constipation conditions within the spectrum of variant HD include,
and, in severe cases, life-threatening toxic megacolon. The among others, intestinal neuronal dysplasia and neuronal
aganglionosis starts at the anus and progresses proximally hypoplasia [6,7].
to varying degrees [1]. Several clinical parameters have We aimed to describe the long-term clinical outcomes of
been shown to predict the diagnosis of HD, such as failure neonates with early constipation and a clinical suspicion of
to pass meconium within 2448 h and early onset of HD that was excluded by rectal suction biopsy. We further
constipation, especially if accompanied by vomiting and aimed to compare the clinical outcomes of neonates with
abdominal distension [2,3]. Diagnosis may be supported typical and atypical ganglion cells identied on their rectal
by a plain abdominal radiography, contrast enema, or biopsy.
manometry, but a denite diagnosis can only be made by
rectal biopsy showing aganglionosis and hypertrophic
Methods
nerve bers [4,5]. A biopsy showing the presence of even
one ganglion excludes the diagnosis of HD. Study design
The spectrum between HD and health has a wide range
This is a single-center double-cohort comparative study.
of variant HD. However, controversy exists in terms of
The case group included neonates with very early-onset
the various diagnoses and outcomes in this spectrum. In
constipation who underwent rectal suction biopsy for
European Journal of Gastroenterology & Hepatology 2016, 28:917922
suspected HD and in whom the diagnosis of HD was
excluded on the basis of the presence of ganglion cells on
Keywords: chronic constipation, Hirschsprung, infant, rectal biopsy
a
histology. The control group included neonates who were
Shaare Zedek Medical Center and bThe Hebrew University of Jerusalem,
Jerusalem, Israel
matched to the observation cohort by sex and gestational
age, who were born on the same day as the cases with the
Correspondence to Oren Ledder, MD, Pediatric Gastroenterology and Nutrition
Unit, Shaare Zedek Medical Center, The Hebrew University; PO Box 3235, same gestational age, but were discharged without the
Jerusalem 91031, Israel need for rectal biopsy.
Tel: + 972 266 66482; fax: + 972 265 55756; e-mail: orenl@szmc.org.il Inclusion criteria for the case group were neonates who
Received 28 December 2015 Accepted 1 March 2016 were subjected to a rectal suction biopsy at Shaare Zedek
Supplemental digital content is available for this article. Direct URL citations appear
Medical Center between 1996 and 2013 under the age of
in the printed text and are provided in the HTML and PDF versions of this article on 3 months for suspected HD and in whom the diagnosis
the journal's website (www.eurojgh.com). was excluded. At our center, all rectal biopsies are
0954-691X Copyright 2016 Wolters Kluwer Health, Inc. All rights reserved. DOI: 10.1097/MEG.0000000000000636 917
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
918 European Journal of Gastroenterology & Hepatology August 2016 Volume 28 Number 8
referred and performed by experienced pediatric gastro- corresponding 95% condence intervals), means SD, or
enterologists or pediatric surgeons on the basis of the medians (interquartile range), as appropriate for the dis-
clinical presentation and, sometimes, imaging studies. We tribution normality. Continuous data were compared
excluded neonates who had less than 1 year of follow-up. using Students t-test or the Wilcoxon rank sum test as
Neonates with signs or symptoms suggestive of gastro- appropriate for the distribution normality. Categorical
enterological pathology by hospital discharge were exclu- variables were compared using 2 or Fisher exact tests, as
ded from the control group. appropriate. Statistical analyses were carried out using
Cases were identied from the hospitals electronic SPSS for Windows V21.0 (IBM, Armonk, New York,
database by searching ICD-9 coding. Charts of neonates USA), with P value less than 0.05 considered the sig-
found by the electronic search were screened for eligibility. nicance threshold.
Controls were randomly selected and matched from the
same electronic database. Parents of eligible children were
Results
contacted by a letter asking them to complete a short
questionnaire detailing the occurrence of constipation, A total of 55 neonates were identied in the case group
vomiting, abdominal distension, and abdominal pain. and 110 neonates were matched in the control group.
Those who did not respond by mail were followed up by a Three cases died during infancy and, of the remaining, 25
phone call with an option to complete the questionnaire consented to complete the survey. Amongst the control
orally or through an emailed electronic questionnaire. group, of the 110 surveys distributed, 26 consented to
Other relevant clinical data were obtained from the med- participate in the study.
ical chart after obtaining parental consent. The pathology The median duration of follow-up was 4.25 years
slides were retrieved and re-reported by a histopathologist (interquartile range 2.76.9; range 1.911.8).There were
with 22 years of clinical experience, blinded to the clinical no signicant differences between the two groups in
outcome. Histological ndings related to ganglion size, demographics and other background variables (Table 1).
maturity, and number were described on a standardized The case group had a signicantly shorter period of
case report form. Immature ganglia were characterized by exclusive breastfeeding and a nonsignicant trend toward
small numbers of cells per ganglion with an irregular shorter partial breastfeeding than the control group
distribution. 6.7 4.1 versus 4.2 4.8 (P = 0.05) and 11.7 5.2 versus
8.7 8.2 (P = 0.13), respectively.
Outcome measures
Outcomes over the rst year
The primary outcome was the proportion of patients with
chronic constipation, dened as children requiring laxative Most of the measured outcomes were signicantly differ-
treatment for more than a 1-month period during the rst ent between the study groups during the rst year of life
year of life. Despite the absence of formal verication of (Fig. 1). Under the primary analysis, nine (36%) neonates
this outcome measure as accurately reecting neonatal in the case group required laxatives for more than 1 month
constipation, in the absence of a better outcome measure, during the rst year of life compared with 0 (0%) in the
and within the connes of a retrospective analysis with the control group (P < 0.001). This nding was similarly
associated risk of recall bias, this easy to remember, reported by the caregivers for stool consistency as well as
objective endpoint was selected. This sought to minimize vomiting, abdominal distension, abdominal pain, use of
recall bias and is easily validated by an outpatient chart anal stimulants, effort while defecating, and general
review. Furthermore, prolonged use of laxatives (longer irritability.
than 1 month) was specied because of the relatively
widespread ad hoc use of laxatives for transient con- Long-term outcomes
stipation of doubtful clinical signicance and prolonged
Outcomes at the last follow-up remained signicantly
usage likely representing more clinically signicant con-
higher in the study group than the control group (Fig. 2),
stipation. Secondary outcomes were dened as the pro-
but were signicantly improved compared with outcomes
portion of children who had chronic constipation during
at 1 year of age. At the last follow-up, constipation (72 vs.
the rst year of life as dened by the Rome III criteria, and
32%, P = 0.02) and vomiting (52 vs. 12%, P = 0.01) were
incidence and severity of other gastrointestinal (GI) dis-
present in signicantly higher proportions in the case
orders including, but not limited to, vomiting, abdominal
cohort. There was a trend toward improved rates of
pain, and distention. These data were obtained from the
abdominal pain and reduced laxative use (Fig. 3).
questionnaire utilizing focused questions on stool fre-
A signicantly higher incidence of a subsequent diag-
quency, stool consistency (Bristol stool scale), straining
nosis of a chronic or an otherwise signicant medical or
with defecation, pain and irritability (WongBaker faces
surgical condition was identied in the study cohort
rating scale), vomiting/reux, the need for assisted stool-
compared with the control (32 vs. 8%, P = 0.04). These
ing, and other features. The secondary outcomes were
conditions largely, although not exclusively, involved the
considered exploratory in nature because of recall bias.
digestive tract, including two patients with cystic brosis
The last follow-up was characterized as the survey-derived
and one with intestinal volvulus, one patient with a limited
clinical manifestations at the time of survey completion.
bowel resection (unclear clinical details surrounding this
presentation), one patient with Noonan syndrome, one
Statistical analysis
patient with global developmental delay (not otherwise
Statistical analysis of unpaired data was carried out on specied), and another patient who developed a brain
outcomes by frequencies and proportions (with abscess. There was also a signicantly higher rate of
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
Outcomes following exclusion of HD Harlev et al. www.eurojgh.com 919
Table 1. Basic characteristics of the entire cohort
Entire cohort (N = 51) [n (%)] Control group (N = 26) [n (%)] Study group (N = 25) [n (%)] P-value
Males 21 (41) 13 (50) 8 (32) 0.19
Agea (years) 5.8 2.9 6.3 3.2 5.2 2.6 0.20
Gestational age (weeks) 36.2 3.9 36.1 3.6 36.2 4.4 0.94
Race 0.81
Ashkenazi 20 (39) 11 (42) 9 (36)
Sephardic 16 (31) 9 (35) 7 (28)
Mixed 13 (25) 6 (23) 7 (28)
Arabic 2 (4) 0 (0) 2 (8)
Family history of GI disorderb 17 (33) 9 (35) 8 (32) 0.84
Exclusive breastfeeding (months) 5.5 4.6 6.7 4.1 4.2 4.8 0.05
Exclusive and partial breastfeeding (months) 10.2 6.9 11.7 5.2 8.7 8.2 0.13
Child sequence in family 3.0 1.1 2.8 1.1 2.6 1.0 0.58
Unrelated diagnosesc 10 (19) 2 (8) 8 (32) 0.04
Hospitalizationd 17 (33) 3 (12) 14 (56) 0.01
Medians [IQR], means SD and proportions (95% CI) are presented as appropriate.
CI, condence interval; GI, gastrointestinal; IQR, interquartile range.
a
At the time of survey completion.
b
According to the parental survey documentation, includes irritable bowel disease, inammatory bowel disease, reux, peptic ulcer disease, chronic constipation, and celiac
disease.
c
Neonates diagnosed with other diseases during the follow-up period.
d
Neonates hospitalized during the follow-up period for any reason.
N = 25
Control N = 26 Case N = 25 80
80 P = 0.02 First year End of follow-up
P < 0.001 70
P < 0.001
P < 0.001
70 60
P < 0.001 P = 0.2
P < 0.001 P = 0.01
60 P < 0.001 50
Percentage
P < 0.001
50 40 P = 0.2
Percentage
30
40 P = 0.001
20
30
10
20 P = 0.051
0
10 Constipation Abdominal pain Laxative use Vomiting
Fig. 3. Long-term outcomes of the case cohort: 1 year versus the end of
0
follow-up.
n
ng
ng
y
ts
ti al
ea n al
n of
io
us
lit
im of
an
en min
cr pai min
iti
iti
at
bi
tio ort
Ab on
e
ss
al se
ul
ita
ip
tiv
do
do
Vo
ca ff
Po
an U
st
Irr
fe d e
xa
on
Ab
st
La
st
de se
C
neonates who had a hospital admission by the end of
di
In
follow-up in the study group than in the control group: 14
Fig. 1. Clinical manifestations during the rst year of life in controls versus (56%) versus 3 (12%) (P = 0.01). Six of these admissions
suspected Hirschsprungs disease cases. were for GI-related conditions including chronic con-
stipation or the underlying GI surgical condition as
listed above.
To assess the extent to which recall bias may have
affected the results of our study, a subanalysis was carried
out comparing recent cases with longer follow-up cases.
No signicant differences were detected between the
Control N = 26 Case N = 25
groups, suggesting that recall bias did not likely sig-
40
nicantly affect the data accuracy (Supplementary
P = 0.01 Table 2 Supplementary Appendix, Supplemental digital
35 P = 0.01 content 1, http://links.lww.com/EJGH/A93).
30
25 Atypical ganglia
Percentage
P = 0.02
20
To assess the signicance of atypical ganglion cells, the
15
P = 0.35 study cohort was subdivided into 2 groups on the basis of
10 normal histology (six cases) and atypical histology (13
5 cases), including small ganglions (n = 9) and/or immature
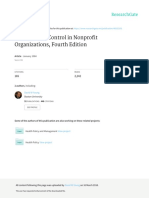
ganglions (n = 11) (Figs 47). Seven cases had both small
0
Constipation Abdominal pain Laxative use Vomiting and immature ganglions. Six cases had inadequate biopsy
Fig. 2. Clinical manifestations at the end of follow-up in controls versus preparations, in which ganglion cells were identied, but
suspected Hirschsprungs disease cases. with inadequate specimen to further categorize the
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
920 European Journal of Gastroenterology & Hepatology August 2016 Volume 28 Number 8
Fig. 4. Normal ganglion cells (arrows) (hematoxylin and eosin). Fig. 7. Immature ganglion cells (arrows) (calretinin immunohistochemistry).
ndings; however, no signicant differences were noted
between those with normal and abnormal ganglionic
phenotype in any of the clinical outcomes both by 1 year
and by the end of the follow-up (Supplementary Table 3
Supplementary Appendix, Supplemental digital content 2,
http://links.lww.com/EJGH/A94).
Discussion
Our study showed for the rst time that neonates with
early-onset constipation in whom HD was excluded by
way of a normal rectal biopsy had an increased rate of
constipation throughout early childhood. This suggests
that clinical presentation in the rst few days is predictive
of future long-term stooling behavior even in the
absence of HD.
Fig. 5. Normal ganglion cells (arrows) (calretinin immunohistochemistry). The prevalence of childhood constipation varies sig-
nicantly between studies, ranging from 1.1 to 28.8%
[813], the vast majority of which are functional in nature.
Less frequent among the causes of constipation are
neurological disorders including HD variants. These
include intestinal neuronal dysplasia [1418], hypo-
ganglionosis [1921], immature ganglion cells, absence of
argyrophil plexus, internal anal sphincter achlasia, smooth
muscle cell abnormalities, perinuclear vacuolation, and
megacystis-microcolon-intestinal hypoperistalsis syndrome
[2226].
The clinical signicance of small and immature gang-
lions remains unclear. In our study, 13 of the rectal
biopsies had atypical ganglion cells; however, none ful-
lled the diagnostic criteria for small and immature
ganglions. Within the limitation of the small numbers
analyzed, we found no difference between the long-term
outcomes of neonates with small or immature ganglion
cells compared with those with normal ganglion cells.
These ndings should be studied further with a larger
Fig. 6. Immature ganglion cells (arrows) (hematoxylin and eosin). cohort to better assess the clinical signicance of these
histological variants.
Our observation cohort had a signicantly higher rate
phenotype, and were thus excluded from this sub-analysis. of diagnosis of a chronic medical condition at the time
No specimens fullled the classication criteria of either of survey. The majority of these neonates (six of eight)
hyperganglionosis or hypoganglionosis. The small number were diagnosed with conditions largely involving the GI
of patients in this sub-analysis limited statistical analysis of tract including cystic brosis, volvulus, and chronic
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
Outcomes following exclusion of HD Harlev et al. www.eurojgh.com 921
constipation. This nding supports the suggestion that Acknowledgements
clinical suspicion of a defecation disorder, even in neonates
This study has been carried out as part of the DG MD
in whom a rectal suction biopsy excludes HD, leads to a
degree requirements from the Hebrew University
signicantly higher risk for development of medical mor- Hadassah Medical School in Jerusalem.
bidity involving the GI system in the future. We also found Tali Bdolah-Abram assisted in designing statistical
a higher proportion of neonates who had been hospitalized analysis.
in whom many of these hospitalizations were related to GI Authors contribution: Drs Harlev and Ledder collected
conditions. The additional nding of a higher hospitali- data, carried out the initial analyses, drafted the initial
zation rate in the study group suggests the clinical burden manuscript, and approved the nal manuscript as sub-
and relevance of these medical conditions and diagnoses. mitted; Dr Turner conceptualized and designed the study,
These data indicate that the nding of constipation in critically reviewed the manuscript, and approved the nal
neonates, even with normal biopsies, is associated with a manuscript as submitted; Dr Waxman and Frankel
clinical burden that should be recognized. designed the data-collection instruments, collected data,
It is noteworthy that all of the clinical manifestations critically reviewed the manuscript, and approved the nal
assessed at the last follow-up indicated signicant manuscript as submitted; Dr Kharenko retrieved pathol-
improvements when compared with the rst year; how- ogy slides, re-reported their pathology, and approved the
ever, these were still signicantly higher than the nal manuscript as submitted.
control group.
In our study group, there was a trend to more females
(although this was not statistically signicant), whereas in Conicts of interest
HD, there is a recognized male predominance of 75% There are no conicts of interest.
[27]. Considering that the entire studied cohort did not
have HD, this sex distribution, although interesting, is of
unclear signicance.
A further interesting nding in this comparative ana- References
lysis is the signicant difference in the age until which the 1 Mattei P. Hirschsprungs disease. In: Wyllie RHJ, Kay M, editors.
neonates diet was exclusively breastmilk. The study design Pediatric gastrointestinal and liver disease. Philadelphia: Elsevier
does not allow us to answer whether this is a cause or Saunders; 2011. pp. 57682.
2 Swenson O, Sherman JO, Fisher JH. Diagnosis of congenital
effect phenomenon. We may speculate that infants pre- megacolon: ananalysis of 501 patients. J Pediatr Surg 1973; 8:587594.
senting with chronic constipation may be suggested var- 3 Khan AR, Vujanic GM, Huddart S. The constipated child: how likely is
ious maternal dietary changes for suspected neonatal Hirschsprungs disease? Pediatr Surg Int 2003; 19:439442.
allergy that can be difcult to maintain or even be sug- 4 De Lorijn F, Reitsma JB, Voskuijl WP, Aronson DC, ten Kate FJ,
Smets AM, et al. Diagnosis of Hirschsprungs disease: a prospective,
gested on medical or neighborly advice to commence comparative accuracy study of common tests. J Pediatr Surg 2005;
formula feeds. Alternatively, this nding may suggest 146:787792.
that formula is associated with a higher rate of constipa- 5 Limousin IT, Valds JA, Jimnez MJ, Cendn RG, Fernndez Pineda I,
tion as reported previously by Van den Berg et al. [28]. Garca RC, Alonso ML. Neonatal diagnostic protocol of the
Hirschsprungs disease. Cir Pediatr 2008; 21:232234.
In any case, the retrospective nature of our analysis 6 Gath R, Goessling A, Keller K, Koletzko S, Coerdt W, Mntefering H,
cannot elucidate a cause and effect relationship of the et al. Analysis of the RET, GDNF, EDN3, and EDNRB genes in patients
association. with intestinal neuronal dysplasia and Hirschsprung disease. Gut 2001;
48:671675.
Our study is the rst to report the signicance of early
7 Gfroerer S, Rolle U. Pediatric intestinal motility disorders. World J
stooling disorder in predicting longer term defecation Gastroenterol 2015; 21:96839687.
behavior, despite the exclusion of HD, but it is not without 8 LoeningBaucke V. Prevalence rates for constipation and faecal and
limitations, most notably recall bias. We made signicant urinary incontinence. Arch Dis Child 2007; 92:486489.
9 Del Ciampo IR, Galvo LC, Del Ciampo LA, Fernandes MI. Prevalence of
efforts to minimize this bias by selecting easy to remember chronic constipation in children at a primary health care unit. J Pediatr
outcomes. Our comparative analysis of results on the basis (Rio J) 2002; 78:497502.
of length of follow-up conrmed that this potential con- 10 Liem O, Harman J, Benninga M, Kelleher K, Mousa H, Di Lorenzo C.
founder did not affect our results to any signicant level. Health utilization and cost impact of childhood constipation in the
United States. J Pediatr 2009; 154:258262.
We did nd that the rates of constipation and vomiting did 11 Lee WT, Ip KS, Chan JS, Young BW. Increased prevalence of con-
improve from 1 year to the end of follow-up, with a trend stipation in pre-school children is attributable to under-consumption of
toward improvement in abdominal pain and reduced plant foods: a community-based study. J Paediatr Child Health 2008;
laxative use; however, the presence of these features was 44:170175.
12 Iacono G, DAmico D, Merolla R, Bonci E, Cavataio F, Di Prima L, et al;
still considerably higher than that in the control group. Paediatric Study Group on Gastrointestinal Symptoms in Infancy.
Unfortunately, our subgroups were too small to enable a Gastrointestinal symptoms in infancy: a population-based
statistical analysis of the different histological abnormal- prospective study. Dig Liver Dis 2005; 37:432438.
13 Kiefte-de Jong JC, Escher J, Arends LR, Jaddoe VW, Hofman A,
ities; thus, this comparison remains merely descriptive in Raat H, Moll HA. Infant nutritional factors and functional constipation in
nature. childhood: the Generation R study. Am J Gastroenterol 2010;
We suggest that constipation in neonates should be 105:940945.
considered clinically signicant even when HD is excluded. 14 Meier-Ruge W. Casuistic of colon disorder with symptoms of
Hirschsprungs disease (authors transl). Verh Dtsch Ges Pathol 1971;
This may be important for counseling families and for 55:506510.
planning medical follow-up in GI clinics after hospital 15 Schoeld DE, Yunis EJ. Intestinal neuronal dysplasia. J Pediatr
discharge. Gastroenterol Nutr 1991; 12:182189.
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
922 European Journal of Gastroenterology & Hepatology August 2016 Volume 28 Number 8
16 Puri P, Gosemann JH. Variant Hirschsprungs disease. Semin Pediatr 23 Melek M, Edirne Y, Beger B, Cetin M. Megacystis-microcolon-intestinal
Surg 2004; 13:293299. hypoperistalsis syndrome: a case report. Gastroenterol Res Pract 2009;
17 Montedonico S, Acevedo S, Fadda B. Clinical aspects of intestinal 2009:282753.
neuronal dysplasia. J Pediatr Surg 2002; 37:17721774. 24 Tanner MS, Smith B, Lloyd JK. Functional intestinal obstruction due to
18 Gillick J, Tazawa H, Puri P. Intestinal neuronal dysplasia: results of deciency of argyrophil neurones in the myenteric plexus. Familial syn-
treatment in 33 patients. J Pediatr Surg 2001; 36:777779. drome presenting with short small bowel, malrotation, and pyloric
19 Taguchi T, Masumoto K, Ieiri S, Nakatsuji T, Akiyoshi J. New classi- hypertrophy. Arch Dis Child 1976; 51:837841.
cation of hypoganglionosis: congenital and acquired hypoganglionosis. 25 Ciamarra P, Nurko S, Barksdale E, Fishman S, Di Lorenzo C. Internal anal
J Pediatr Surg 2006; 41:20462051. sphincter achalasia in children: clinical characteristics and treatment with
20 Schrli AF, Sossai R. Hypoganglionosis. Semin Pediatr Surg 1998; Clostridium botulinum toxin. J Pediatr Gastroenterol Nutr 2003; 37:315319.
7:187191. 26 Athow AC, Filipe MI, Drake DP. Hyperganglionosis mimicking
21 Zhang HY, Feng JX, Huang L, Wang G, Wei MF, Weng YZ. Diagnosis Hirschsprungs disease. Arch Dis Child 1991; 66:13001303.
and surgical treatment of isolated hypoganglionosis. World J Pediatr 27 Amiel J, Lyonnet S. Hirschsprung disease, associated syndromes, and
2008; 4:295300. genetics: a review. J Med Genet 2001; 38:729739.
22 Rolle U, Puri P. Structural basis of voiding dysfunction in megacystis 28 Van den Berg MM, Benninga MA, Di Lorenzo C. Epidemiology of
microcolon intestinal hypoperistalsis syndrome. J Pediatr Urol 2006; childhood constipation: a systematic review. Am J Gastroenterol 2006;
2:277284. 101:24012409.
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
Вам также может понравиться
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- CircCircuit Protection in Health Care Facilitiesuit Protection in Health Care FacilitiesДокумент43 страницыCircCircuit Protection in Health Care Facilitiesuit Protection in Health Care FacilitiesMenaОценок пока нет
- Sex Differences of Brain and Their Implications For Personalized TherapyДокумент14 страницSex Differences of Brain and Their Implications For Personalized TherapyMaria Isabel Montañez RestrepoОценок пока нет
- Oet ReadingДокумент118 страницOet ReadingSamia FarooqОценок пока нет
- Alprazolam: Why Is This Medicine Prescribed To You?Документ1 страницаAlprazolam: Why Is This Medicine Prescribed To You?Jerome GeronimoОценок пока нет
- Settle Plate SamplingДокумент3 страницыSettle Plate SamplingFilipa PereiraОценок пока нет
- Forensic Aspects of Dissociative Identity DisorderДокумент240 страницForensic Aspects of Dissociative Identity DisorderDeath Tiscat100% (1)
- English Teacher's NotesДокумент24 страницыEnglish Teacher's NotesPrincess KimОценок пока нет
- 60 Substance Abuse Group Therapy ActivitiesДокумент7 страниц60 Substance Abuse Group Therapy ActivitiesHanes Labajos100% (1)
- MODULE 8: Settings, Processes, Methods, and Tools in Social WorkДокумент4 страницыMODULE 8: Settings, Processes, Methods, and Tools in Social WorkAlexandra Nicole RugaОценок пока нет
- NCM 103 Lecture - COMMUNICATIONДокумент46 страницNCM 103 Lecture - COMMUNICATIONAngelyn SalimbajonОценок пока нет
- NURS FPX 6030 Assessment 6 Final Project SubmissionДокумент11 страницNURS FPX 6030 Assessment 6 Final Project Submissionzadem5266Оценок пока нет
- Department of ICT Technology - DBMS Section: Level - IVДокумент125 страницDepartment of ICT Technology - DBMS Section: Level - IVEsubalewОценок пока нет
- Combat StressДокумент94 страницыCombat StressClaudia Maria Ivan100% (1)
- Drugs and DosagesДокумент40 страницDrugs and DosagesGeraldine Marie Salvo100% (1)
- ETW-2013 Amma PDFДокумент100 страницETW-2013 Amma PDFRosalete LimaОценок пока нет
- Brain Tumors - KY Cancer RegistryДокумент45 страницBrain Tumors - KY Cancer RegistryMohammad Galih PratamaОценок пока нет
- TSS 30 - Application Form - SOДокумент4 страницыTSS 30 - Application Form - SOkemvanОценок пока нет
- Chinese Medicine Eng BrochureДокумент12 страницChinese Medicine Eng BrochuretanasedanielaОценок пока нет
- 10 1007@s00068-mfjrbtДокумент14 страниц10 1007@s00068-mfjrbtJGunar VasquezОценок пока нет
- Assisting For Endotracheal IntubationДокумент16 страницAssisting For Endotracheal IntubationSREEDEVI T SURESH100% (1)
- Management Control in Nonprofit Organizations, Fourth EditionДокумент74 страницыManagement Control in Nonprofit Organizations, Fourth EditionSUHAIRI19084488100% (1)
- NARQ40007-PROCESS - Beauty Parlor ManagementДокумент3 страницыNARQ40007-PROCESS - Beauty Parlor ManagementYogesh ThakurОценок пока нет
- Ded-9 - 16692 Pasta Brazare Amdry 100cДокумент16 страницDed-9 - 16692 Pasta Brazare Amdry 100cAndreea GrecuОценок пока нет
- Physical Fitness Test Individual Score CardДокумент12 страницPhysical Fitness Test Individual Score CardJunessa TadinaОценок пока нет
- Nah Incarcerated HerniaДокумент4 страницыNah Incarcerated Herniafelix_the_meowОценок пока нет
- Development of A Taste-Masked Orodispersible FilmДокумент12 страницDevelopment of A Taste-Masked Orodispersible FilmKhoa DuyОценок пока нет
- Chapter One The History of BreathingДокумент5 страницChapter One The History of Breathingoiliver2011Оценок пока нет
- Chapter I Related Literature Teenage PreДокумент12 страницChapter I Related Literature Teenage PreWilkenn Tuazon100% (3)
- Assignment Strategic Human Resource Management: SUBMITTED TO: Ms. Asvir NaveedДокумент6 страницAssignment Strategic Human Resource Management: SUBMITTED TO: Ms. Asvir NaveedMuniza UsmanОценок пока нет
- MSDS PDFДокумент5 страницMSDS PDFdang2172014Оценок пока нет