Академический Документы
Профессиональный Документы
Культура Документы
Diseases of the Aorta: Causes and Types of Aortic Aneurysms
Загружено:
Medisina101Исходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Diseases of the Aorta: Causes and Types of Aortic Aneurysms
Загружено:
Medisina101Авторское право:
Доступные форматы
adiuvante Dei gratia doctorum factionis 2014-2015
CARDIOLOGY: DISEASES OF
DR. ORLANDO DEDUYO
THE AORTA
DISEASES OF THE AORTA Causes of AA:
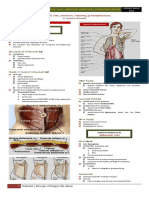
ANATOMY OF THE AORTA Degenerative diseases
Inherited or developmental diseases ( Marfan s
The aorta is the conduit through which blood ejected from the syndrome)
left ventricle is delivered to the systemic arterial bed Infections ( syphilis, TB)
diameter is approximately 3 cm at the origin Vasculitis
ascending portion- 2.5 cm Trauma
descending portion in the thorax- 2.5 cm Inflammation, proteolysis, and biomechanical wall stress
abdomen- 1.8-2 cm contribute to the degenerative processes that characterize most
Aortic wall consist of a thin intima composed of: aneurysms of the abdominal and descending thoracic aorta.
Tunica intima- composed of endothelium, These are mediated by B and T cell lymphocytes, macrophages,
subendothelial connective tissue and an internal elastic inflammatory cytokines, and matrix metalloproteinases that
lamina degrade elastin and collagen and alter the tensile strength and
Tunica media- composed of smooth muscle cells and ability of the aorta to accommodate pulsatile stretch.
extracellular matrix
Tunica adventitia- composed primarily of connective DEGENERATIVE AORTIC ANEURYSM (AA)
tissue enclosing the vasa vasorum and nervi vascularis
The viscoelastic and compliant properties of the aorta serves as a Factors associated with degenerative aortic aneurysms:
buffering function. Aging
The aorta is distended during systole to allow a portion of the Cigarette smoking
stroke volume and elastic energy to be stored, and it recoils Hypercholesterolemia
during diastole so that blood continues to flow to the periphery Male gender
Due to its continues exposure to high pulsatile pressure and Family history of aortic aneurysm
shear stress, the aorta is particularly prone to injury and disease Atherosclerosis - most common pathologic condition associated
resulting from mechanical trauma with degenerative aortic aneurysm.
Its also more prone to rupture especially with the development High risk condition such as high blood, DM age 50 and above are
of aneurysmal dilation, since its wall tension will be increased, as high risk in developing Aortic aneurysm
governed by Laplaces law (proportional to the product of Screened for AA
pressure and radius) Female > 65 years old are also high risk
Age>40 above
AORTIC ANEURYSM
CYSTIC MEDIAL NECROSIS
Aneurysm pathologic dilatation of a segment of a blood vessel.
True aneurysm involves all three layers of the vessel Cystic medial necrosis histophatologic term used to describe
wall and is distinguished from a pseudoaneurysm the degeneration of collagen and elastin fibers in the tunica
Pseudoaneurysm- intimal and medial layers are media of the aorta, as well as the loss of medial cells that are
disrupted and the dilatation is lined by adventitia only replaced by multiple clefts of mucoid material.
and, at times, by perivascular clot. Affects the proximal aorta, results in circumferential weakness
Ectasia- arterial dilatation < 150% of normal artery and dilatation, and leads to the development of fusiform
diameter aneurysms involving the ascending aorta and sinuses of Valsalva
TYPES in terms of SHAPE
o Fusiform aneurysm affects the entire This condition is particularly prevalent in patients with:
circumference of a segment of the vessel, Marfan syndrome
resulting in a diffusely dilated artery. Ehlers-Danlos syndrome type IV
o Saccular aneurysm involves only a portion of HPN
the circumference, resulting in an out pouching Congenital bicuspid aortic valves- sometimes these
of the vessel wall. patients has no symptoms and they are referred for
Aortic aneurysms are also classified according to location, i.e. presence of murmur only
abdominal vs. thoracic. Familial thoracic aortic aneurysm syndromes.
Sometimes it appears as an isolated condition in
ETIOLOGY Patient without any other apparent cause.
Aortic aneurysms result from conditions that cause degradation
or abnormal production of the aortic walls structural
components, elastin and collagen.
INFECTIOUS CAUSES THORACIC AORTIC ANEURYSM (TAA)
Infectious causes of AA: Clinical manifestations and natural history depend on their
Syphilis location
TB ( most common in the Philippines) Cystic medial necrosis is the most common cause of ascending
Other bacterial infections aortic aneurysms, whereas atherosclerosis is the condition most
frequently associated with aneurysms of the aortic arch and
Syphilis descending thoracic aorta.
relatively uncommon cause Average growth rate of thoracic aneurysms: 0.1 0.2 cm/year.
Syphilitic periaortitis and mesoaortitis damage elastic Risk of rupture is related to:
fibers, resulting in thickening and weakening of the size of the aneurysm
aortic wall. The presence of symptoms, ranging approx. from 2-
Approximately 90% of syphilitic aneurysms are 3% per year for thoracic aneurysms <4.0 cm in
located in the ascending aorta and aortic arch. diameter to 7% per year for those >6 cm in diameter.
Tuberculous aneurysms The bigger the aneurysm increase manifestation or
Typically affect the thoracic aorta and result from symptoms increase risk for rupture
direct extension of infection from hilar lymph nodes Borderline in requesting surgery for patient with
or contiguous abscesses, or from bacterial seeding. Thoracic aortic aneurysm is 5.5 cm diameter and for
Loss of aortic wall elasticity results from patient with Marfan syndrome and congenital
granulomatous destruction of the medial layer. bicuspid aortic valve the cu-off is lower 5 cm
So if you have patient with multidrug resistance Most thoracic aortic aneurysms are asymptomatic
tuberculosis and develop chest pain you have screen However, compression or erosion of adjacent tissue by
patient and you will see in the x-ray that there is aneurysms may cause symptoms such as
widened mediastinum so you will suspect aortic 1. chest pain (MOST COMMON)
aneurysm 2. shortness of breath
Mycotic aneurysm 3. cough
is a rare condition that develops as a result of 4. hoarseness
Staphylococcal, Streptococcal, Salmonella or other 5. Dysphagia.
bacterial or fungal infections of the aorta, usually at But the manifestation is not specific because it can
an atherosclerotic plaque. mimic other diseases such as TB, emphysema,
These aneurysms are usually saccular pericarditis. So put together the history, P.E and
Tx: prolonged IV antibiotics Laboratory examination to diagnose the patient
Aneurysmal dilatation of the ascending aorta may cause
VASCULITIS Congestive Heart Failure as a consequence of aortic
regurgitation (warning sign)
Vasculitides associated with aortic aneurysm include Marked compression of the superior vena cava may
Takayasus arteritis produce congestion of the head, neck, and upper
giant cell arteritis extremities.(edematous upper extremities)
which may cause aneurysms of the aortic arch and descending Chest X-ray may be the first test to suggest the diagnosis of a
thoracic aorta. thoracic aortic aneurysm. Findings include
Spondyloarthropathies, such as ankylosing spondylitis, Widening of the mediastinal shadow
rheumatoid arthritis, psoriatic arthritis, relapsing polychondritis, Displacement or compression of the trachea or
and Reiters syndrome, are associated with dilatation of the left mainstem bronchus.
ascending aorta 2D-echo, particularly transesophageal echocardiography, can be
Behcets syndrome causes thoracic and abdominal aortic used to assess the proximal ascending aorta and descending
aneurysms. thoracic aorta.-
So for simple 2 D ECHO (surface echo) you can see
TRAUMA only up to the root of the aorta. Yung transesophageal
Echo pinapasok sa bibig and you can visualize your
Traumatic aneurysm may occur after penetrating or non- proximal ascending and descending thoracic aorta
penetrating chest trauma Contrast-enhanced computed tomography (CT), Magnetic
Most commonly affected is the descending aorta just beyond the resonance imaging (MRI), and Conventional invasive aortography
site of insertion of ligamentum arteriosum are sensitive and specific tests for assessment of aneurysms of
the thoracic aorta and involvement of branch vessels.
In asymptomatic patients whose aneurysms are too small to
justify surgery, noninvasive testing with either contrast
enhanced Ct or MRI should be performed at least every 6-12
months to monitor expansion.
Page 2 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
SURGICAL PROCEDURE FOR TAA .001) and treatment with conventional open
repair (P = .02).
Operative repair with placement of a prosthetic valve Conclusion
Indicated in patient with symptomatic thoracic aortic o An endovascular approach for the ruptured
aneurysm (non-traumatic) descending thoracic aorta
Ascending aortic diameter is > 5.5-6 cm reduces early morbidity, mortality, and duration
Aneurysm that has increased by > 1 cm per year of hospitalization, while providing equivalent
Endovascular repair is an alternative for some patients with late outcomes even in an older group largely
descending thoracic aortic aneurysm considered high risk for open repair. These data
Complication of surgery support a paradigm shift, with TEVAR emerging
Increase risk of paraplegia or stroke as the preferred therapy for all patients
- Increase risk heart attack for patient with distal presenting with descending aortic rupture.
abdominal aorta 32% o Based on the guidelines open surgery is on level
Neurologic deficit 1A evidence thats why still this is the treatment
Acute renal failure or CKD of choice while TEVAR is level 2A evidence.
- 38% mortality for patient with renal disease
- 13% mortality for patient with no renal disease RUPTURED ABDOMINAL AORTIC ANEURYSM
- 30 day mortality occur for patient with low GFR ( th
patient with stage 3A) 27% 10 leading cause of death in Men
- Stage IV- dialysis is needed 2:1-4:1 M-F predominance
Cardiac failure 50% undetected
Infection Occur more frequently in males than females
TH
Respiratory failure 13 leading cause of death
24,000 deaths/year
DESCENDING THORACIC AORTIC ANEURYSM (DTAA) Increase incidence with age- 6-7 decade of life
AAA 4.0 cm may affect men older than 50 years old
90% of all AAA > 4 cm are related to atherosclerotic disease and
Type C: 54% - extensive (MOST COMMON)
most of them are below the level of renal arteries
Type A: 33% (proximal only)
Prognosis is related to both the size of the aneurysm and the
Type B: 13% (distal part)
severity of coexisting coronary artery and cerebrovascular
disease
30d mortality:8%
The risk of rupture increases with size
Neurologic deficits: 23%
Many complications < 5 cm- 1-2%
HF, Renal failure, Infections > 5cm in diameter- 20-40%
6cm diameter: exponential increase
THORACIC ENDOVASCULAR AORTIC REPAIR ( TEVAR) 10cm diameter: 50% chance of rupture
5.5cm decide if patient undergo open surgery or
Analogous to angioplasty TEVAR
Benefits in comparison with open surgery Increase high operative mortality maybe because of
Attractive option late detection
Less invasive 50% die before they reach the hospital
40-50% die before they reach surgery
Minimal blood loss
High mortality and high operative mortality due to late
Minimal pulmonary complication
detection and diagnosis
Decrease risk of paraplegia
Quick recovery
IMAGING MODALITY
Anatomical criteria
Proximal and distal diameter- 23-37 cm
Information needed from diagnostic studies
Proximal landing zone- 2cm
Length and size of the aneurysm
Distal landing zone
Proximal extent (infra, supra, or juxtarenal)
Candidate for TEVAR
Supre/juxta-complex and extensive
dissection
A comparative analysis of open and endovascular repair for the
Obligatory renal ischemia time due to
ruptured descending thoracic aorta ( taken from journal)
clamping above the renal arteries.
Result
Distal extent, aneurysm or occlusive disease of the
o By multivariate analysis, independent predictors
iliofemoral segments.
of a composite outcome of early mortality,
Status of the suprarenal-visceral vessels
stroke, permanent spinal cord ischemia, or need
(dilatation/stenosis of coeliac, mesenteric)
for dialysis or tracheostomy included the
Presence of anatomical variant (horseshoe
presentation with hemodynamic instability (P <
kidney,retroaortic renal vain, IVC duplication)
Leak or rupture
Page 3 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
For thoracic aortic aneurysm the imaging modality of choice is
chest x-ray and for
Abdominal aneurysm if patient present with pulsatile mass on
periumbilical area you have to suspect
ABDOMINAL ULTRASOUND
Most practical screening tool readily available
Sensitivity: 88-99%; specificity: 100%
Fast and accurately defines aneurysm size within +/-
0.3 cm
Fairly defines proximal extent (infra, supra, juxta
renal) improved by DUPLEX UTZ
Fairly defines status of suprarenal/visceral segments
improved by DUPLEX UTZ
Distal extent poorly defines (dilatation/stenosis of
iliofemoral segments)
Poorly defines presence of anatomic variants
(retroaortic renal veins, IVC duplication)
Cannot identify leak or rupture.
COMPUTED TOMOGRAPHY SCAN
Sufficient as a stand-alone modality for vital information
Extremely accurate in diagnosis & sizing with accuracy within +/-
0.2 cm
Provides better definition of proximal extent of aneurysm and
local anatomical relationship of the visceral & renal vessels
Provides information regarding the presence of anatomical
Example of suprarenal abdominal aneurysm
variants (horsehoe kidney, retroaortic renal vein, IVC
duplication)
MAGNETIC RESONANCE ANGIOGRAPHY (MRA)
Provides information for iliofemoral aneurysmal extension
Identifies leak or rupture
Excellent modality for monitoring changes in aneurysm size Alternative to CT scan for preoperative evaluation in elective
cases in those with incipient renal insufficiency (Px w/ CKD)
Extremely accurate for sizing
Correctly defines proximal and distal extent of disease in >80%
of cases
Defines anatomical variants
Identifies leak or rupture
Time consuming, expensive and not readily available.
AORTOGRAPHY (invasive)
Excellent in vascular roadmapping especially with suspected
concomitant renal and iliofemoral stenosis.
Leak or rupture may be seen with extravasation of contrast
medium.
Underestimates aneurysm size in the presence of non-opacified
mural thrombus lining the walls.
SPIRAL CT WITH 3D RECONSTRUCTION Cannot identify anatomical variants.
Time consuming
Provides 3D images or aorta & its branches Mobilizes many personnel
Better definition and roadmapping for surgical strategy Entails a lot of cathlab preparation
May be time-consuming for urgent or emergent AAA Invasive, potential catheter insertion related complications
(hematoma, dissection, ect.)
Largely supplanted by high-definition CT
So if patient is for TEVAR you start with CT contrast and do
aortography prior to placement of stent
Page 4 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
Analogous to coronary angiogram but the dye is injected to the CONSERVATIVE TREATMENT for LOW RISK RUPTURE
aorta from proximal carotid vessel, renal vessel, & aortic iliac
vessel No conservative tx for elimination of aneurysm
Hypertension Control
RISK FOR RUPTURE o Beta blockers (reduces expansion rate
independent of hemodynamic effects)
Estimated Rupture Risk o Target SBP of 110-120mmHg and HR of 60-
70bpm
AAA DIAMETER ( CM) RUPTURE RISK( % /YEAR) o Higher BP, higher HR higher shear stress
<4 0 o If Px is asthmatic and COPD
4-5 0.5-5 Verapamil/Diltiazem or Digoxin for HR control
5-6 3-15 o (--ra---in) New agent that controls only HR and
6-7 10-20 not BP
7-8 20-40 o The new agent should not coexist with
>8 30-50 verapamil/diltiazem beacause it will prolong QT
interval high risk for sudden cardiac death
AAA diameter best predictor of rupture risk (just like drinking coffee w/ energy drink!)
Rupture risk very low for <5 cm (1.5%), increase substantially by Smoking cessation
6 cm Cessation of steroid treatment for COPD
Current evidence 5.5 cm best threshold for repair for average Modify/treat risk factors (DM, Dyslipidemia, etc.)
patient UTZ surveillance
Independent predictors of AAA rupture in 4-5.5 cm size Recommendations for UTZ Surveillance
(Society for Vascular Surgery and the Society for Vascular Medicine
PARAMETERS RELATIVE RISK and Biology)
FEMALE GENDER (ACS higher 3X
independent risk) < 3cm No further testing
LARGER INITIAL DIAMETER 2.9X per cm 3-4 cm Annual US
CURRENT SMOKING 1.5X 4-4.5 cm US every 6 months
WORSE COPD 0.6X per L FEV1 > 4.5 cm Referral to a vascular specialist
HIGHER MAP 1.02X per mmHg
AVERAGE OR HIGH RISK RUPTURE
Observation that not all AAA rupture at the same size threshold.
Unfortunately, there is no precise formula that incorporates the Assess life expectancy
risk factors to calculate rupture risk. Risk factors used in If short, i.e. terminal malignancy, irreversible severe
combination to estimate rupture risk and categorize patients as CAD, cardiomyopathy, etc.;
low, average or high risk. If average or long, assess operative risk
Conservative management
Factors Influencing Risks of Aneurysm Rupture if Px will undergo TEVAR or Open Surgery, most likely
this patients will die
Low risk Average risk High risk (for
TEVAR)
Diameter < 5 cm 5-6 cm >6 cm
expansion < 0.3 cm/yr 0.3-0.6 cm/yr >0.6 cm/year
Smoking/COPD None, mild moderate Severe/steroids
Family history No relatives 1 relative Numerous
relatives
Hypertension Normal BP controlled Poorly
controlled
shape Fusiform saccular Very eccentric
Smoking/COPD bad predictors (longer time extubating patient
during surgery)
Page 5 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
- Example of open repair
OPERATIVE MORTALITY FOR OPEN REPAIR X
Elective= 1-3 (4-6%)
Urgent= 19%
Ruptures (massive blood loss/transfusion, intraoperative
MI, DIC, ARDS, Renal Failure, etc.) = 40-50%
Age is not an absolute contraindication for the procedure
ENDOVASCULAR ANEURYSM REPAIR X
GOOD OR MODERATE OPERATIVE MORTALITY
Emerged in the early 1990s as an alternative treatment for AAA
Open Repair (Gold standard) IA level of evidence Studies have demonstrated equivalent early safety/efficacy of
Endovascular Aneurysm Repair (EVAR) (Alternate procedure) 2A EVAR
level of evidence EVAR short term benefits of reduced ICU and hospital stays,
EVAR mortality lower mortality than open repair in RAAA reduced blood loss, fewer major complications, and more rapid
recovery.
EVAR midterm (3-6 years) result favourable with limitation of AAA
HIGH OPERATIVE MORTALITY RISK expansion 80-90%, and rupture prevention 95-98%
Has a higher reintervention rate, increases surveillance burden, and
Conservative management a small but ongoing risk of AAA rupture.
Endovascular aneurysm repair (Px w/ high income who insists Pxs preference is important (EVAR vs. Open Repair) for those with
they want to live) good or moderate operative risk.
Preferred intervention for those with high operative risk who
satisfy the EVAR anatomic criteria
Presently, there are no randomized control trials comparing EVAR
vs. Open repair
Page 6 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
Anatomic Criteria SYMPTOMATIC
1. Proximal neck length >1.5 cm
2. Proximal neck diameter <2.8 cm Steady gnawing pain in the hypogastrium or lower back that lasts
for hours or days
3. Distal cuff length >1 cm
Leak or heralds impending rupture
4. Distal cuff diameter <2.8 cm Diagnostic test: CT scan
5. Angulation/tortuosity <60 degrees Indication for surgery:
6. Iliac artery diameter >7 mm Any size especially if saccular, mycotic or inflammatory
7. Mural thrombus attachment site Timing: urgent
not present
8. Iliac site attachment common iliac RUPTURED ANEURYSM
artery
9. Associated mesenteric disease not Pathognomonic Triad
present 1. Pulsatile abdominal mass
2. Hypotension
3. Abdominal/back pain (1/3 of cases)
MANAGEMENT
Rx: no work-up needed, emergent intervention
Acute abdominal or back pain which is generally sudden in onset,
Goal of Repair
or worsening pain
Most aneurysm repairs aim to prevent rupture Often associated with light headedness or collapse (most likely
(rupture operative mortality risk 50%) stroke or involvement of carotid vessels)
Most effective if performed when rupture risk is high
compared to elective operative risk (1-5%) in patients
Known AAA Px, STABLE
who will live long enough to enjoy the longterm
benefits ECG (to r/o ACS)
Thus decision influenced primarily by estimates of: CT Scan
Aneurysm rupture risk o Ruptured: Emergent intervention (unstable &
Elective operation mortality hypotensive)
Life expectancy o Non-ruptured: Evaluate for early repair
Patient preference
Known AAA Px, UNSTABLE (Hypotension)
STENT PLACEMENT Emergent intervention
Undiagnosed AAA Px, STABLE
ECG, CT Scan (UTZ)
o Ruptured: Emergent intervention
o Non-ruptured: Evaluate for early repair
Undiagnosed AAA Px, UNSTABLE
Rx: ECG, Resuscitate
o If stabilized: CT scan (UTZ)
If not AAA: evaluate other causes
Ruptured AAA: Emergent intervention
Non-ruptured AAA: Evaluate for early
repair
o Remain unstable: Emergent intervention
***NOTE: Study this part because Doc will give cases and
necessary management will be based on this.(dati pa to hehe,
not sure if applicable to satin)
Page 7 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
Ruptured Abdominal Aneurysm
AORTIC DISSECTION
Considered emergency
Uncommon
Potentially catastrophic disease if not recognized early and treated
promptly
Diagnosis often requires clinical suspicion
th th
Peak incidence is the 6 to 7 decade of life
Has a 3:1 male preponderance
ANATOMIC CLASSIFICATION (Debakey)
hematoma
CURRENT RECOMMENDATIONS FOR AAA REPAIR X
Type I Entire length (proximal-distal)
Report of a subcommittee of the Joint Council of the American Type II Proximal
Association for Vascular Surgery and Society for Vascular Surgery
Type III thoracic
1. Single threshold diameter for elective AAA repair not applicable to
all Pxs, decision for repair must be individualized in each case SPECTRUM of AORTIC DISSECTION
2. RCTs have shown rupture risk of small (<5cm) AAA is quite low, Ascending aorta 65%
and a policy of careful surveillance up to a diameter of 5.5 cm is safe, Descending aorta 25%
unless rapid expansion (>1cm/yr) or symptoms develop. Aortic arch about 10%
Abdominal aorta 5%
However, early surgery is comparable to surveillance with later
surgery, so that Px preference is important, especially for AAA 4.5 CLINICAL MANIFESTATIONS
to 5.5 cm in diameter.
Based on the best available current evidence, 5.5 cm diameter Severe pain
appears to be an appropriate threshold for repair in an average Px.
Most common presenting symptoms of acute aortic
However, subsets of younger low-risk Pxs, with long projected life
dissection
expectancy, may prefer early repair.
In up to 96% of cases
Typically severe and of sudden onset
3. If the surgeons personal documented operative mortality rate is
tearing, ripping, sharp and stabbing
low, repair may be indicated at smaller sizes (4.5-5.5 cm) if that is the
Pxs preference. Migratory pain in 17% of cases
Mean age 63.1%
4. For women, or with AAA greater than average rupture risk, Mostly Males
elective repair at 4.5-5.0 cm is an appropriate threshold for repair. PE
5. For high-risk Pxs, delay in repair until larger diameter is warranted, Any reported pain 96%
especially if EVAR is not possible. Abrupt onset 85%
Chest pain 73%
6. In view of its uncertain long-term durability and effectiveness, as Anterior 61%
well as the increased surveillance burden, EVAR is most appropriate Posterior 36%
for Pxs at increased risk for conventional open aneurysm repair. Back pain 53%
Abdominal pain 30%
7. EVAR may be preferred treatment method for older, high risk Pxs, Hypotensive 8%
those with hostile abdomen or other clinical circumstances likely to Shock 8.4%
increase the risk of conventional open, repair, if their anatomy is Murmurs (mostly AR)
appropriate. CHF 7%
8. Use of EVAR in Pxs with unsuitable anatomy markedly increases the
risk of adverse outcomes and need for conversion to open repair.
Page 8 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
PRACTICAL ASSESSMENT of DIAGNOSTIC RELIEF
Location of pain
Anterior involvement of ascending aorta, likewise pain in ADVANTAGES AO CT MRI TEE
the neck, throat, jaw or face (like ACS involving the L. main
Readily Fairly Quite Fairly Very
coronary high risk for sudden cardiac death)
available
Interscapular involvement of the descending thoracic
aorta (back pain) Rapid Fairly Quite Fairly Very
o Signs of AR: bounding pulse, wide pulse pressure, Performed at No No No Yes
diastolic murmur beating along the R. parasternal bedside
border, evidence of CHF Noninvasive No Yes Yes Yes
Symptoms of life-threatening complications involving dissection of
the ascending aorta No IV contrast No No Yes Yes
Congestive Heart Failure (7%)
Cost High Reasonable Moderate Reasonabble
o Almost invariably due to severe aortic regurgitation
Syncope (9%)
o May be an ominous sign suggesting a surgical
emergency due to carotid artery dissection
Cerebrovascular accident (5%)
Cardiac arrest or sudden death due to coronary artery
involvement
Signs of tamponade due to pericardial effusion
(hypotensive, very faint or no pulse)
Ischemic peripheral neuropathy
Paraplegia
THORACIC AORTIC DISSECTION
Mortality rate of untreated ascending aorta
st
80% - 1 6hrs
st
21% - 1 24hrs
st
15% - 1 2 days
Acute Severe AR
Coronary occlusion
Pericardial rupture
Arc branch lesion
VITAL INFO needed for MANAGEMENT of STRATEGY
1. Involvement of the ascending aorta
2. Dissection involving coronaries
3. Severity of AR
4. Presence of Pericardial effusion/tamponade
5. Distal extent of the dissection with occlusion
6. avulsion of visceral branches (coeliac, mesenteric, renal) /
iliofemoral vessels (ischemia/insufficiency)
Lumen that supplies the visceral organs (true or false lumen)
Dissection of Ascending Aorta
XR widened superior mediastinum w/ pleural effusion
Dissection of Descending Aorta
XR widened mediastinum w/ widened descending aorta
IMAGING TESTS
Transesophageal Echocardiography (TTE) 32%
CT Scan 62%
MRI/MRA 2%
Aortography 4%
You can see more of THROMBUS
More branch vessel involvement (also in MRI)
Page 9 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
PROTOCOL Chronic (2 weeks and above)
Formation of aneurysm from aortic dissection to a size of 6
cm and above
Rapid expansion of aneurysm 0.5 cm/6 months
TRAUMATIC AORTIC RUPTURE
BLUNT AORTIC INJURY: Epidemiology
nd
2 most common cause of death (after head injury)
Majority caused by automobile crashes
Rapid deceleration of the body (vertica or horizontal plane)
Isthmus
Most common site
Deceleration differential forces between various tissues
Strain: points of junction
This portion is mobile
MANAGEMENT PLAN
Initial management
Resuscitation
INITIAL MANAGEMENT Investigation: CXR, CTA, aortogram
Treatment of associated injuries
Elimination of pain (IV morphine) BP management
Reduction of systolic BP to 100 to 120 mmHg (mean of 60-75
mmHg) Diagnosis
Arterial dP/dt should be reduced through the use of beta-blocking CXR
agents o Wide mediastinum 85%
Serial Hgb and Hct monitoring o Indistinct aortic knob 24%
Repeat Ct scan after 5-7 days o Pleural effusion
May be adequate Rx for Stanford B (descending thoracic aorta CT-Scan
dissection)
*once stable and associated injuries are treated:
URGENT or EMERGENT SURGERY for STANFORD A involving
ASCENDING AORTA
(mas Emergency compared to B)
Acute severe AR
Presence of pericardial effusion (rupture)
Symptomatic arch branch occlusion (vessels to upper extremities
and head) Conclusion
Leak or rupture Short-term results appear favorable
st
More than 25% of all Pxs died within the 1 24 hours after Patient selection critical
the onset of dissection (more than 1% /hr) Surveillance imaging required
st
More than 50% died within the 1 week Long-term results pending
More than 75% died within 1 month Follow ups remain a challenge
More than 90% died within 1 year Future generation
AORTITIS
SURGICAL INDICATIONS for STANFORD B AORTIC DISSECTION
(DESCENDING THORACIC AORTA) Inflammatory disease of the aorta
CAUSES
(may opt for medical treatment temporarily before intervention) Large vessel vasculature
Acute (within 2 weeks) o Takayasus arteritis
Leak/rupture (hemothorax) o Giant cell arteritis
Uncontrolled HPN Rheumatic and HLA B27 associated Spondyloarthropathies
Uncontrolled or recurrent pain Behcets syndrome
Symptomatic aortic branch occlusion/avulsion (visceral, Antineutrophil cytoplasmic Antibodies (ANCA) associated
renal vessel occlusion, lower extremity ischemia) vasculitides
Page 10 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
Cogan syndrome Duplex UTZ and echocardiography
Infection
o Syphilis TREATMENT
o TB
o Salmonella Glucocorticoids
Agent of choice but complete remission in 50% of cases
TAKAYASUS ARTERITIS only
o Initial: prednisolone 4mg/KgW, dose reduction on
Granulomatous Vasculitis affecting the aorta and its branches with response
predilection for the aortic arch and its branches o Maintenance: low-dose (5mg/day)
Age <40 Methotrexate
Highest in Eastern Asia, Northern Germany Used in combination with glucocorticoids
nd rd
2 3 decade of life, 80-90% women 0.3 mg/ Kg, 1x/week + prednisolone
Cyclophosphamide
ETIOLOGY In fulminant cases
Supportive
Genetic ASA (Aspirin)
Associated with HLA Bw52 in eastern Asia, associated with BB (Beta blockers)
complement allotype C4A2 (board exam question!) Endovascular Tx, Percutaneous catheter, angiography, stent
Cellular Immune Reaction implantation (using these, conditions will just recur)
Activation of CD4 cells Vascular Surgery
Endocrine immune reactions
HISTOPATHOLOGY PROGNOSIS
Granulomatous polyarteritis 5-year survival 80-90% (high if diagnosed early)
Granuloma with multinucleic giant cells and lymphocytic Prognosis is poor f with AR, aneurysm, arterial HPN
infiltrates; fibrosis in the vessel wall; thrombi
CLASSIFICATION (ACR 1990) (no update)
CLINICAL FINDINGS
TAKE NOTE!
Movement dependent shoulder/arm pain (shoulder spasm) 1. Age < 40
Intermittent claudication in the arms and legs 2. Claudication in the extremities
Bilateral difference in BP up to 65% of the patients 3. Weakened pulse in one or both brachial arteries
Arterial HPN in 40-70% of cases (associated with RAS) 4. Systolic BP dfference between the arm >10 mmHg
Generalized symptoms often at the start of the disease 5. Flow murmur over the aorta or subclavian vein
Visual disturbance, amaurosis fugax w/ involvement of the carotid 6. Pathologic angiography findings
arteries
Cardiac symptoms: exertional dyspnea, angina, palpitations **3-6 criteria have to be met
Arthralgia and myalgia in 55% Sensitivity 90%
Specificity 98%
CLINICAL EXAM
OTHER TYPES
Stenotic murmurs over the large vessels especially aortic arch
branches Giant cell arteritis
Bilateral difference on BP on both arms and legs Rheumatic aortitis
Weakened pulse Idiopathic aortitis
Diastolic murmur over the aortic valve (AR) Infective aortitis
Cutaneous manifestations Chronic atherosclerotic occlusive disease
Pyoderma gangrenosum or erythema nodosum in 15% of Acute aortic Occlusion
pts
LABS & IMAGING
No specific lab
Angiography
Used to be the gold standard for the diagnosis and
assessment but does not provide info about inflammatory
activity
MRA
Demonstrate the quality of the arterial wall
Page 11 of 11 Jay and Miki
Malayo ang mararating ng ating pangarap kung sasamahan ng pagsisikap!
Вам также может понравиться
- External Abdominal Hernias GuideДокумент12 страницExternal Abdominal Hernias GuideMedisina101100% (1)
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Документ13 страницSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Оценок пока нет
- Diseases of The AortaДокумент48 страницDiseases of The AortaYibeltal AssefaОценок пока нет
- Chest Trauma Guide for CliniciansДокумент120 страницChest Trauma Guide for CliniciansRojelle LezamaОценок пока нет
- Acute Coronary SyndromesДокумент82 страницыAcute Coronary Syndromesmidras taranОценок пока нет
- CardiologyДокумент6 страницCardiologyFrancis FransОценок пока нет
- Suspecting Pulmonary Hypertension in The Dyspneic Patient: Who, When, and HowДокумент92 страницыSuspecting Pulmonary Hypertension in The Dyspneic Patient: Who, When, and HowJonathan LongОценок пока нет
- Common Histories and Red Flags Presentation Noninteractive VersionДокумент21 страницаCommon Histories and Red Flags Presentation Noninteractive VersionesmarОценок пока нет
- PericarditisДокумент29 страницPericarditisPavin KumarОценок пока нет
- SURGERY Lecture 4 - Breast (Dra. Fernandez)Документ15 страницSURGERY Lecture 4 - Breast (Dra. Fernandez)Medisina101100% (1)
- Vascular Sugergy Questions NasirДокумент19 страницVascular Sugergy Questions NasirAhmad SobihОценок пока нет
- Approach To The Cardiovascular Examination567 160120085414 PDFДокумент22 страницыApproach To The Cardiovascular Examination567 160120085414 PDFHNINОценок пока нет
- Aorta DissectionДокумент98 страницAorta DissectionDian SukaryaОценок пока нет
- ECG IMM 2020.docx.2Документ25 страницECG IMM 2020.docx.2Abdul QuyyumОценок пока нет
- 5 DISEASES OF THE CARDIOVASCULAR SYSTEMДокумент24 страницы5 DISEASES OF THE CARDIOVASCULAR SYSTEMHussein Al SaediОценок пока нет
- Cardiac Disease in Pregnancy: Management ChallengesДокумент35 страницCardiac Disease in Pregnancy: Management ChallengesMannat ZaidiОценок пока нет
- Fast F A S T: Recognizing Stroke: Ace Rms Peech ImeДокумент25 страницFast F A S T: Recognizing Stroke: Ace Rms Peech ImeIliescu DenisaОценок пока нет
- Surgical ExamДокумент302 страницыSurgical ExamHossam SabriОценок пока нет
- Raminder Nirula - High-Yield Internal Medicine (High-Yield Series) - Lippincott Williams and Wilkins (2006)Документ228 страницRaminder Nirula - High-Yield Internal Medicine (High-Yield Series) - Lippincott Williams and Wilkins (2006)Isah Mohammed100% (1)
- MEDICAL SURGICAL NURSING CARDIOVASCULAR DRILLSДокумент12 страницMEDICAL SURGICAL NURSING CARDIOVASCULAR DRILLSMaria Garcia Pimentel Vanguardia IIОценок пока нет
- Pediatric Cardiology II Lecture SummaryДокумент5 страницPediatric Cardiology II Lecture SummaryMedisina101Оценок пока нет
- Right Ventricular Myocardial InfarctionДокумент43 страницыRight Ventricular Myocardial Infarctionrudresh m g0% (2)
- Valvular Heart DiseaseДокумент27 страницValvular Heart DiseaseOwen J. WieseОценок пока нет
- Adult Congenital Heart Disease Board ReviewДокумент79 страницAdult Congenital Heart Disease Board ReviewKhajornsak Som-UnОценок пока нет
- Lower Extremity Arterial Protocol 14 1Документ2 страницыLower Extremity Arterial Protocol 14 1api-3494022400% (1)
- Mitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationДокумент33 страницыMitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationcafemedОценок пока нет
- Endovascular Surgery - BenkőДокумент33 страницыEndovascular Surgery - BenkőpampaszОценок пока нет
- 22 Ventricular Septal DefectДокумент26 страниц22 Ventricular Septal Defectdhiraj parmarОценок пока нет
- Principles of EchocardiographyДокумент3 страницыPrinciples of Echocardiographys336336anl100% (1)
- Aortic StenosisДокумент3 страницыAortic StenosisMaxine BaraquiaОценок пока нет
- Cardiovascular MCQsДокумент23 страницыCardiovascular MCQssb medexОценок пока нет
- SURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Документ16 страницSURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Medisina101100% (1)
- Biology IGCSE Human Circulatory SystemДокумент17 страницBiology IGCSE Human Circulatory SystemNiharika100% (1)
- EchocardiogramДокумент14 страницEchocardiogramMaria EdelОценок пока нет
- Diagnosing Chest Pain CausesДокумент8 страницDiagnosing Chest Pain CausesMedisina101Оценок пока нет
- PEDIA - Cardio (Esguerra) PDFДокумент9 страницPEDIA - Cardio (Esguerra) PDFMedisina101Оценок пока нет
- SURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Документ19 страницSURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Medisina101100% (1)
- Rheumatic Heart Disease AustrliaДокумент63 страницыRheumatic Heart Disease AustrliaMuhammad Reza100% (2)
- Diagnosis, Treatment and Follow-Up in Extracranial Carotid Stenosis, 2020Документ16 страницDiagnosis, Treatment and Follow-Up in Extracranial Carotid Stenosis, 2020CAMILO ARMANDO BENAVIDES BURBANOОценок пока нет
- Head and Neck SurgeryДокумент15 страницHead and Neck SurgeryMedisina101100% (1)
- Krok 2014 Base All 2Документ237 страницKrok 2014 Base All 2Gaurav S Batra0% (1)
- Case Summary Pediatrics03 3-Year-OДокумент10 страницCase Summary Pediatrics03 3-Year-OJeffОценок пока нет
- Acynotic Heart DiseasesДокумент13 страницAcynotic Heart DiseasesSimran JosanОценок пока нет
- Congenital Heart DiseaseДокумент45 страницCongenital Heart DiseaseBrandedlovers OnlineshopОценок пока нет
- Aortic Stenosis Symptoms and Physical Exam FindingsДокумент9 страницAortic Stenosis Symptoms and Physical Exam FindingsMedisina101Оценок пока нет
- Acquifer Case 2Документ9 страницAcquifer Case 2Emily SymesОценок пока нет
- Science 9 Worktext, Sketchnote, Face Mask Activity and Assessment L1 PRINTEDДокумент7 страницScience 9 Worktext, Sketchnote, Face Mask Activity and Assessment L1 PRINTEDClarice Jenn MaltoОценок пока нет
- Acquired Heart DiseaseДокумент44 страницыAcquired Heart DiseaseMedisina101Оценок пока нет
- Vascular Surgery Principles: Anatomy, Pathology, ManagementДокумент21 страницаVascular Surgery Principles: Anatomy, Pathology, ManagementdanebrosОценок пока нет
- Bailey & Love MCQs-EMQs in Surgery-Part - 2Документ6 страницBailey & Love MCQs-EMQs in Surgery-Part - 2JockerОценок пока нет
- Pulmonary SequestrationДокумент15 страницPulmonary SequestrationEmily EresumaОценок пока нет
- Acute Coronary SyndromeДокумент5 страницAcute Coronary SyndromeLuis OportoОценок пока нет
- Adrenaline (Child, Adult, IM, IV... ) Ya Corticosteroids Too Asthma Ya Croup o ..Документ17 страницAdrenaline (Child, Adult, IM, IV... ) Ya Corticosteroids Too Asthma Ya Croup o ..raji selvakumaranОценок пока нет
- Approach To The Diagnosis and Therapy of Lower Extremity Deep Vein ThrombosisДокумент20 страницApproach To The Diagnosis and Therapy of Lower Extremity Deep Vein ThrombosisAlina CrissОценок пока нет
- Y3 OSCE PracticeДокумент27 страницY3 OSCE PracticenamwaОценок пока нет
- End of 4 Year OSCE - SurgeryДокумент53 страницыEnd of 4 Year OSCE - SurgerySyed Irfan ArifОценок пока нет
- A Simple Guide to Abdominal Aortic Aneurysm, Diagnosis, Treatment and Related ConditionsОт EverandA Simple Guide to Abdominal Aortic Aneurysm, Diagnosis, Treatment and Related ConditionsОценок пока нет
- Fetal ArrhythmiasДокумент18 страницFetal ArrhythmiasKarin Stefanny Muñoz CastilloОценок пока нет
- CT Shows Diffuse Fatty Thickening of Interatrial SeptumДокумент13 страницCT Shows Diffuse Fatty Thickening of Interatrial SeptumHaluk AlibazogluОценок пока нет
- Tjandra MCQДокумент35 страницTjandra MCQnz chuksОценок пока нет
- Review QuizДокумент107 страницReview QuizAhmad JalladОценок пока нет
- FinalДокумент56 страницFinalvamshidhОценок пока нет
- 2018 ESC Guidelines For The Management of Cardiovascular Disease in PregnancyДокумент84 страницы2018 ESC Guidelines For The Management of Cardiovascular Disease in Pregnancyasm obginОценок пока нет
- Valvular Heart Disease 2Документ46 страницValvular Heart Disease 2Topea BogdanОценок пока нет
- ASD Atrial Septal Defect PDFДокумент9 страницASD Atrial Septal Defect PDFAco AjjahОценок пока нет
- Cardiomyopathy and MyocarditisДокумент8 страницCardiomyopathy and Myocarditisoddone_out100% (1)
- Gallstones in Pregnancy - UpToDateДокумент51 страницаGallstones in Pregnancy - UpToDateLeira BarbosaОценок пока нет
- HyphemaДокумент19 страницHyphemaLiyanti RinceОценок пока нет
- CCTGA Diagnosis, Treatment & OutcomesДокумент94 страницыCCTGA Diagnosis, Treatment & OutcomesVik SharОценок пока нет
- L-R ShuntДокумент88 страницL-R ShuntnanohaniwiekoОценок пока нет
- Clinical Profile of Patients With Acyanotic Congenital Heart Disease in Pediatric Age Group in Rural IndiaДокумент7 страницClinical Profile of Patients With Acyanotic Congenital Heart Disease in Pediatric Age Group in Rural IndiaInternational Organization of Scientific Research (IOSR)Оценок пока нет
- Cardiac Murmurs and Maneuvers GuideДокумент1 страницаCardiac Murmurs and Maneuvers GuidePkernОценок пока нет
- Medicine: CardiorespiratoryДокумент56 страницMedicine: CardiorespiratoryWalaa abo foolОценок пока нет
- Definition, Classification, Etiology, and Pathophysiology of Shock in Adults - UpToDateДокумент16 страницDefinition, Classification, Etiology, and Pathophysiology of Shock in Adults - UpToDatevara prasadОценок пока нет
- Infective Endocarditis - Dr. Payawal PDFДокумент6 страницInfective Endocarditis - Dr. Payawal PDFMedisina101Оценок пока нет
- Acute Coronary Syndrome - Dra. Deduyo PDFДокумент6 страницAcute Coronary Syndrome - Dra. Deduyo PDFMedisina101Оценок пока нет
- Coronary Artery Disease - Dra. Deduyo PDFДокумент7 страницCoronary Artery Disease - Dra. Deduyo PDFMedisina101Оценок пока нет
- Congestive Heart Failure - Dra. DeduyoДокумент10 страницCongestive Heart Failure - Dra. DeduyoMedisina101Оценок пока нет
- ECG Part 1 - Dr. Payawal PDFДокумент10 страницECG Part 1 - Dr. Payawal PDFMedisina101Оценок пока нет
- Arrythmia Part 2 - Dr. Payawal PDFДокумент8 страницArrythmia Part 2 - Dr. Payawal PDFMedisina101Оценок пока нет
- ECG Part 2 - Dr. Payawal PDFДокумент4 страницыECG Part 2 - Dr. Payawal PDFMedisina101Оценок пока нет
- Valvular Heart Diseases Part 1 - Dr. BartolomeДокумент18 страницValvular Heart Diseases Part 1 - Dr. BartolomeMedisina101Оценок пока нет
- Detecting Abnormal Cardiac RhythmsДокумент10 страницDetecting Abnormal Cardiac RhythmsMedisina101100% (1)
- Peripheral Vascular Medicine - Dr. Deduyo PDFДокумент14 страницPeripheral Vascular Medicine - Dr. Deduyo PDFMedisina101Оценок пока нет
- Deep Vein Thrombosis - Dr. Deduyo PDFДокумент17 страницDeep Vein Thrombosis - Dr. Deduyo PDFMedisina101Оценок пока нет
- Congenital Heart Diseases - Dr. BartolomeДокумент12 страницCongenital Heart Diseases - Dr. BartolomeMedisina101Оценок пока нет
- Cardiac Tumors - Dr. BartolomeДокумент12 страницCardiac Tumors - Dr. BartolomeMedisina101Оценок пока нет
- Cardiac Tumors Slides - Dr. BartolomeДокумент81 страницаCardiac Tumors Slides - Dr. BartolomeMedisina101Оценок пока нет
- Pedia Pulmo 3 11.03.16Документ49 страницPedia Pulmo 3 11.03.16Medisina101Оценок пока нет
- Pedia Pulmo I 10.4.16Документ129 страницPedia Pulmo I 10.4.16Medisina101Оценок пока нет
- Pedia Pulmo 2 10.18.16Документ73 страницыPedia Pulmo 2 10.18.16Medisina101Оценок пока нет
- Surgery II - Pancreas 2014Документ20 страницSurgery II - Pancreas 2014Medisina101Оценок пока нет
- Quick Study Guide To The Cardiovascular SystemДокумент9 страницQuick Study Guide To The Cardiovascular SystemMc Luis Glen AserdanoОценок пока нет
- Vascular Access in Neonates and Children: Daniele G. Biasucci Nicola Massimo Disma Mauro PittirutiДокумент405 страницVascular Access in Neonates and Children: Daniele G. Biasucci Nicola Massimo Disma Mauro PittirutiErick HernandezОценок пока нет
- Anatomi CardioRespiДокумент27 страницAnatomi CardioRespiheta aprianaОценок пока нет
- Avant Review Lesson 1-8 ECG Rhythm Strip InterpretationДокумент28 страницAvant Review Lesson 1-8 ECG Rhythm Strip InterpretationphoebjaetanОценок пока нет
- Coronary ArteriesДокумент28 страницCoronary ArteriesMihaela IonescuОценок пока нет
- Manual Cardiovascular SystemДокумент5 страницManual Cardiovascular SystemVynz Morales CosepОценок пока нет
- Basic Ecg Interpretation For NursesДокумент4 страницыBasic Ecg Interpretation For Nurseskimberly dobleОценок пока нет
- Science 9: LessonДокумент9 страницScience 9: LessonJellyn Rose Panganiban RamosОценок пока нет
- 856 t2sv87Документ6 страниц856 t2sv87AntonisОценок пока нет
- Cardiac Cath Procedure ExplainedДокумент25 страницCardiac Cath Procedure ExplainedReyna Mee AhiyasОценок пока нет
- 87EOLT49DДокумент6 страниц87EOLT49DGlecy AdrianoОценок пока нет
- ABPI-Ankle Brachial Pressure IndexДокумент23 страницыABPI-Ankle Brachial Pressure IndexTamsi MahiОценок пока нет
- Coronary Heart Disease Leaflet and Drugs Used To Treat CHDДокумент4 страницыCoronary Heart Disease Leaflet and Drugs Used To Treat CHDsigit_riyantonoОценок пока нет
- 22 Lecture PresentationДокумент88 страниц22 Lecture PresentationLeilaОценок пока нет
- Coronary Heart Disease in the Framingham StudyДокумент21 страницаCoronary Heart Disease in the Framingham StudyYunlong LiuОценок пока нет
- SECTION 1 CHAPTER 1 Vital Signs MeasurementДокумент15 страницSECTION 1 CHAPTER 1 Vital Signs MeasurementRhea Andrea UyОценок пока нет
- Introduction of Angiology and HeartДокумент58 страницIntroduction of Angiology and Heart9999999999999-567421Оценок пока нет
- Venous Ulcer Causes, Exam, and Treatment (VULEXAMTREATДокумент40 страницVenous Ulcer Causes, Exam, and Treatment (VULEXAMTREATAlexander EnnesОценок пока нет
- Cyanotic Congenital Heart DiseaseДокумент58 страницCyanotic Congenital Heart Diseasegolden37Оценок пока нет
- CHD Lecture for C-I StudentsДокумент89 страницCHD Lecture for C-I StudentsGomathi ShankarОценок пока нет
- SECTION 6: Spleen: and OverviewДокумент38 страницSECTION 6: Spleen: and Overviewtudoranluciana1Оценок пока нет
- Ischaemic Cardiogenic ShockДокумент7 страницIschaemic Cardiogenic ShockHerbert Baquerizo VargasОценок пока нет
- CathLab Webinar Series Foto dr. TaufikДокумент2 страницыCathLab Webinar Series Foto dr. TaufikzulmynurОценок пока нет