Академический Документы
Профессиональный Документы
Культура Документы
Perioperative Nursing Lecture Notes
Загружено:
lagundaИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Perioperative Nursing Lecture Notes
Загружено:
lagundaАвторское право:
Доступные форматы
Lecture Notes on Perioperative Nursing 1
Prepared By: Mark Fredderick R Abejo R.N, MAN
According to URGENCY
Classification Indication Examples
for Surgery
Emergent – patient - severe
requires immediate Without bleeding
attention, life delay - gunshot/
threatening condition. stab wounds
MEDICAL AND SURGICAL NURSING - Fractured
skull
PERIOPERATIVE NURSING
Urgent / Imperative – Within 24 to - kidney /
patient requires prompt 30 hours ureteral
Lecturer: Mark Fredderick R. Abejo RN, MAN
attention. stones
__________________________________________
Required – patient Plan within a - cataract
needs to have surgery. few weeks or - thyroid d/o
PERIOPERATIVE Elective – patient
months
Failure to - repair of
NURSING should have surgery. have surgery scar
not - vaginal
catastrophic repair
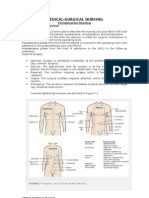
Perioperative Nursing – used to describe the nursing
care provided in the total surgical experience of the Optional – patient’s Personal - cosmetic
patient: preoperative, intraoperative and postoperative. decision. preference surgery
Preoperative Phase, extends from the time the client is According to DEGREE OF RISK
admitted in the surgical unit, to the time he/she is Major Surgery
prepared for the surgical procedure, until he is - High risk / Greater Risk for Infection
transported into the operating room. - Extensive
- Prolonged
Intraoperative Phase, extends from the time the client is - Large amount of blood loss
admitted to the OR, to the time of administration of - Vital organ may be handled or removed
anesthesia, surgical procedure is done, until he/she is Minor Surgery
transported to the RR/PACU. - Generally not prolonged
- Leads to few serious complication
Postoperative Phase, extends from the time the client is - Involves less risk
admitted to the recovery room, to the time he is
transported back into the surgical unit, discharged from Ambulatory Surgery/ Same-day Surgery / Outpatient
the hospital, until the follow-up care. Surgery
4 Major Types of Pathologic Process Requiring Advantages:
Surgical Intervention (OPET) - Reduces length of hospital stay and cuts costs
- Reduces stress for the patient
Obstruction – impairment to the flow of vital fluids - Less incidence of hospital acquired infection
(blood,urine,CSF,bile) - Less time lost from work by the patient; minimal
Perforation – rupture of an organ. disruptions on the patient’s activities and family life.
Erosion – wearing off of a surface or membrane.
Disadvantages:
Tumors – abnormal new growths.
- Less time to assess the patient and perform
preoperative teaching.
- Less time to establish rapport
Classification of Surgical Procedure
- Less opportunity to assess for late postoperative
complication.
According to PURPOSE:
Diagnostic – to establish the presence of a disease
Example of Ambulatory Surgery
condition. ( e.g biopsy )
Teeth extraction
Exploratory – to determine the extent of disease
Circumcision
condition ( e.g Ex-Lap )
Vasectomy
Curative – to treat the disease condition.
* Ablative – removal of an organ Cyst removal
* Constructive – repair of congenitally Tubal ligation
defective organ.
* Reconstructive – repair of damage organ Surgical Risks
Palliative – to relieve distressing sign and symptoms, Obesity
not necessarily to cure the disease. Poor Nutrition
Fluid and Electrolyte Imbalances
Age
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 2
Prepared By: Mark Fredderick R Abejo R.N, MAN
Presence of Disease (Cardiovascular dse., DM, Fear of Pain
Respiratory dse. ) Fear of Death
Concurrent or Prior Pharmacotherapy Fear of disturbance on Body image
other factors: Worries – loss of finances, employment, social and
- nature of condition family roles.
- loc. of the condition
- magnitude / urgency of the surgery Manifestation of Fears
- mental attitude of the patient - anxiousness
- caliber of the health care team - bewilderment
- anger
- tendency to exaggerate
- sad, evasive, tearful, clinging
PREOPERATIVE PHASE - inability to concentrate
- short attention span
Goals - failure to carry out simple directions
Assessing and correcting physiologic and - dazed
psychologic problems that may increase surgical risk.
Giving the person and significant others complete Nursing Intervention to Minimize Anxiety
learning / teaching guidelines regarding surgery. Explore client’s feeling
Instructing and demonstrating exercises that will Allow client’s to speak openly about fears/concerns
benefits the person during postop period. Give accurate information regarding surgery
Planning for discharge and any projected changes in (brief, direct to the point and in simple terms)
lifestyle due to surgery. Give empathetic support
Consider the person’s religious preference and
Physiologic Assessment of the Client Undergoing arrange for visit by a priest / minister as desired.
Surgery
Age
Presence of Pain INFORMED CONSENT
Nutritional & Fluid and Electrolyte Balance
Cardiovascular / Pulmonary Function
Renal Function Purposes:
Gastrointestinal / Liver Function To ensure that the client understand the nature of
Endocrine Function the treatment including the potential complications
Neurologic Function and disfigurement
Hematologic Function ( explained by AMD )
Use of Medication To indicate that the client’s decision was made
Presence of Trauma & Infection without pressure.
To protect the client against unauthorized
Routine Preoperative Screening Test procedure.
To protect the surgeon and hospital against legal
Test Rationale action by a client who claims that an authorized
CBC RBC,Hgb,Hct are important to the procedure was performed.
oxygen carrying capacity of blood.
WBC are indicator of immune Circumstances Requiring Consent
function. Any surgical procedure where scalpel, scissors,
Blood grouping/ Determined in case blood transfusion suture, hemostats of electrocoagulation may be
X matching is required during or after surgery. used.
Serum To evaluate fluid and electrolyte Entrance into body cavity.
Electrolyte status Radiologic procedures, particularly if a contrast
PT,PTT Measure time required for clotting to material is required.
occur. General anesthesia, local infiltration and regional
Fasting Blood High level may indicate undiagnosed block.
Glucose DM
BUN / Evaluate renal function Essential Elements of Informed Consent
Creatinine the diagnosis and explanation of the condition.
ALT/AST/LDH Evaluate liver function a fair explanation of the procedure to be done and
and Bilirubin used and the consequences.
Serum albumin Evaluate nutritional status a description of alternative treatment or procedure.
and total CHON a description of the benefits to be expected.
Urinalysis Determine urine composition material rights if any.
Chest Xray Evaluate resp.status/ heart size the prognosis, if the recommended care, procedure
ECG Identify preexisting cardiac problem. is refused.
Psychosocial Assessment and Care Requisites for Validity of Informed Consent
Causes of Fears of the Preoperative Clients Written permission is best and legally accepted.
Fear of Unknown ( Anxiety ) Signature is obtained with the client’s complete
Fear of Anesthesia understanding of what to occur.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 3
Prepared By: Mark Fredderick R Abejo R.N, MAN
- adult sign their own operative permit Interlace his fingers and place hands over the
- obtained before sedation proposed incision site, this will act as a splint and
For minors, parents or someone standing in their will not harm the incision.
behalf, gives the consent. Lean forward slightly while sitting in bed.
Breath, using diaphragm
Note: for a married emancipated minor parental Inhale fully with the mouth slightly open.
consent is not needed anymore, spouse is accepted Let out 3-4 sharp hacks.
With mouth open, take in a deep breath and quickly
For mentally ill and unconscious patient, consent give 1-2 strong coughs.
must be taken from the parents or legal guardian
If the patient is unable to write, an “X” ia accepted Turning
if there is a witness to his mark Changing positions from back to side-lying (vice
Secured without pressure and threat versa ) stimulates circulation, encourages deeper
A witness is desirable – nurse, physician or breathing and relieve pressure areas
authorized persons. Help the patient to move onto his side if assistance is
When an emergency situation exists, no consent is needed.
necessary because inaction at such time may cause Place the uppermost leg in a more flexed position
greater injury. (permission via telephone/cellphone than that of the lower leg and place a pillow
is accepted but must be signed within 24hrs.) comfortably between the legs.
Make sure that the patient is turned from one side to
the back and onto the other side every 2 hours.
PREOPERATIVE CARE Foot and Leg Exercise
Moving the legs improves circulation and muscle
tone.
Physical Preparation Have the patient lie supine, instruct patient to bend a
knee and raise the foot – hold it a few seconds and
Before Surgery lower it to the bed.
Repeat above about 5 times with one leg and then
Correct any dietary deficiencies
with the other. Repeat the set 5 times every 3-5
Reduce an obese person’s weight
hours.
Correct fluid and electrolyte imbalances
Then have the patient lie on one side and exercise the
Restore adequate blood volume with BT legs by pretending to pedal a bicycle.
Treat chronic diseases For foot exercise, trace a complete circle with the
Halt or treat any infectious process great toe.
Treat an alcoholic person with vit. supplementation,
IVF or fluids if dehydrated Turning to the Side
Turn on your side with the uppermost leg flexed most
Preoperative Teaching and supported on a pillow.
Grasp the side rails as an aid to maneuver to the side.
Incentive Spirometry
Encouraged to use incentive spirometer about 10 to
12 times per hour.
Deep inhalations expand alveoli, which prevents
atelectasis and other pulmonary complication.
There is less pain with inspiratory concentration than
with expiratory concentration.
Diaphragmatic Breathing
Refers to a flattening of the dome of the diaphragm
during inspiration, with resultant enlargement of
upper abdomen as air rushes in. During expiration,
abdominal muscles contract.
In a semi-Fowlers position, with your hands loose-
fist, allow to rest lightly on the front of lower ribs.
Breathe out gently and fully as the ribs sink down and
inward toward midline.
Then take a deep breath through the nose and mouth,
letting the abdomen rise as the lungs fill with air.
Hold breath for a count of 5.
Exhale and let out all the air through your nose and
mouth.
Repeat this exercise 15 times with a short rest after
each group of 5.
Coughing
Promotes removal of chest secretions.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 4
Prepared By: Mark Fredderick R Abejo R.N, MAN
Preparing the Patient the Evening Before Surgery Check ID band, skin prep
Preparing the Skin Check for special orders – enema, IV line
- have a full bath to reduce microorganisms in the Check NPO
skin. Have client void before preop medication
- hair should be removed within 1-2 mm of the skin Continue to support emotionally
to avoid skin breakdown, use of electric clipper is Accomplished “preop care checklist
preferable.
Preparing the G.I tract
- NPO, cleansing enema as required
PREOPERATIVE MEDICATIONS
ASA (American Society of Anesthesiologists)
Guidelines for Preoperative Fasting Goals:
To aid in the administration of an anesthetics.
Liquid and Food Intake Minimum To minimize respiratory tract secretion and changes
Fasting Period in heart rate.
Clear Liquids 2
To relax the patient and reduce anxiety.
Breast Milk 4
Nonhuman Milk 6 Commonly used Preop Meds.
Light Meal 6 Tranquilizers & Sedatives
Regular / Heavy Meals 8 * Midazolam
* Diazepam ( Valium )
Preparing for Anesthesia * Lorazepam ( Ativan )
- Avoid alcohol and cigarette smoking for at least 24 * Diphenhydramine
hours before surgery. Analgesics
Promoting rest and sleep * Nalbuphine ( Nubain )
- Administer sedatives as ordered Anticholinergics
* Atropine Sulfate
Preparing the Person on the Day Of Surgery Proton Pump Inhibitors
* Omeprazole ( Losec )
Early A.M Care * Famotidine
Awaken 1 hour before preop medications
Morning bath, mouth wash Transporting the Patient to the OR
Provide clean gown Adhere to the principle of maintaining the comfort
Remove hairpins, braid long hair, cover hair with cap and safety of the patient.
if available. Accompany OR attendants to the patient’s bedside
Remove dentures, colored nail polish, hearing aid, for introduction and proper identification.
contact lenses, jewelries. Assist in transferring the patient from bed to
Take baseline vital sign before preop medication. stretcher.
Complete the chart and preoperative checklist.
Make sure that the patient arrive in the OR at the
proper time.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 5
Prepared By: Mark Fredderick R Abejo R.N, MAN
Patient’s Family Each procedure room should maintained with
Direct to the proper waiting room. positive pressure, which forces the old air out of
Tell the family that the surgeon will probably contact the room and prevents the air from surrounding
them immediately after the surgery. areas from entering into the procedure room
Explain reason for long interval of waiting:
anesthesia prep, skin prep, surgical procedure, RR. • Electrical Safety
Tell the family what to expect postop when they see Faulty wiring, excessive use of extension cords,
the patient poorly maintained equipment and lack of
current safety measures are just some of the
hazardous factors that must be constantly
INTRAOPERATIVE PHASE checked
All electrical equipment new or used, should be
Goal: routinely checked by qualified personnel.
Asepsis Equipment that fails to function at 100%
Homeostasis efficiency should be taken out of service
immediately.
Safe Administration of Anesthesia
Hemostasis
• Communication System
The Surgical Team
Surgical Environment
Surgeon
Unrestricted Area
• Primary responsible for the preoperative
- provides an entrance and exit from the surgical suite
medical history and physical assessment.
for personnel, equipment and patient
• Performance of the operative procedure
- street clothes are permitted in this area, and the area
according to the needs of the patients.
provides access to communication with personnel within
• The primary decision maker regarding surgical
the suite and with personnel and patient’s families
technique to use during the procedure.
outside the suit.
• May assist with positioning and prepping the
patient or may delegate this task to other
Semi-restricted Area
members of the team
- provides access to the procedure rooms and
peripheral support areas within the surgical suite.
Assistant Surgeon
- personnel entering this area must be in proper
• May be a resident, intern , physician’s assistant
operating room attire and traffic control must be
or a perioperative nurse.
designed to prevent violation of this area by
• Assists with retracting, hemostasis, suturing and
unauthorized persons
any other tasks requested by the surgeon to
- peripheral support areas consists of: storage areas
facilitate speed while maintaining quality
for clean and sterile supplies, sterilization equipment and
during the procedure.
corridors leading to procedure room
Anesthesiologist
Restricted Area
• Selects the anesthesia, administers it, intubates
- includes the procedure room where surgery is
the client if necessary, manages technical
performed and adjacent substerile areas where the scrub
problems related to the administration of
sinks and autoclaves are located
anesthetic agents, and supervises the client’s
- personnel working in this area must be in proper
condition throughout the surgical procedure.
operating room attire
• A physician who specializes in the
administration and monitoring of anesthesia
while maintaining the overall well-being of the
Environmental Safety
patient.
• The size of the procedure room
Scrub Nurse
Usually rectangular or square in shape
• May be either a nurse or a surgical technician.
20 x 20 x 10 with a minimum floor space of
• Reviews anatomy, physiology and the surgical
360 square feet
procedures.
• Assists with the preparation of the room.
• Temperature and humidity control
• Scrubs, gowns and gloves self and other
The temperature in the procedure room should
members of the surgical team.
maintained between 68 F - 75 F ( 20 - 24
• Prepares the instrument table and organizes
degrees C)
sterile equipment for functional use.
Humidity level between 50 - 55 % at all times
• Assists with the drapping procedure.
• Passes instruments to the surgeon and assistants
• Ventilation and air exchange system
by anticipating their need.
Air exchange in each procedure room should be
• Counts sponges, needles and instruments.
at least 25 air exchanges every hour, and five of
• Monitor practices of aseptic technique in self
that should be fresh air.
and others.
A high filtration particulate filter, working at
• Keeps track of irrigations used for calculations
95% efficiency is recommended.
of blood loss
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 6
Prepared By: Mark Fredderick R Abejo R.N, MAN
Circulating Nurse Surgical Incisions
• Must be a registered nurse who, after additional
education and training, specialized in Incision Site Type of Surgery
perioperative nursing practice. Butterfly For craniotomy
• Responsible and accountable for all activities Limbal For eye surgeries
occurring during a surgical procedure including Halstead / Elliptical For breast surgeries
the management of personnel equipment, Subcostal Gallbladder and biliary tract
supplies and the environment during a surgical surgery
procedure. Paramedian Right side – gallbladder, biliary
• Patient advocate, teacher, research consumer, tract
leader and a role model. Left side - splenectomy
• May be responsible for monitoring the patient Transverse Gastrectomy
during local procedures if a second Rectus Right side – small bowel
perioperative nurse is not available. resection
• Ensure all equipment is working properly. Left side – sigmoid colon
• Guarantees sterility of instruments and supplies. resection
• Assists with positioning. McBurney Appendectomy
• Monitor the room and team members for breaks
Pfannenstiel Gynecologic surgery
in the sterile technique.
Lumbotomy For kidney surgeries
• Handles specimens.
• Coordinates activities with other departments,
Position During Surgery
such as radiology and pathology.
• Documents care provided. Position Type of Surgery
• Minimizes conversation and traffic within the Dorsal Recumbent Hernia repair, mastectomy,
operating room suite. bowel resection
Trendelenburg Pelvic Surgeries
Lithotomy Vaginal repair, D&C, rectal
Principles of Surgical Asepsis surgery, APR
Prone Spinal surgery, laminectomy
Sterile object remains sterile only when touched by Lateral Kidney, chest, hip surgery
another sterile object Jack Knife Position Rectal procedures,
Only sterile objects may be placed on a sterile field sigmoidoscopy and colonosc
A sterile object or field out of range of vision or an Reverse Upper abdominal, head, neck
object held below a person’s waist is contaminated Trendelenburg and facial surgery
When a sterile surface comes in contact with a wet, Position
contaminated surface, the sterile object or field
becomes contaminated by capillary action Explain the purpose of position
Fluid flows in the direction of gravity Avoid undue exposure
The edges of a sterile field or container are Strap the person to prevent falls
considered to be contaminated (1 inch) Maintain adequate respiratory and circulatory
functions.
Medical Asepsis vs. Surgical Asepsis Maintain good body alignment
ANESTHESIA
• State of “Narcosis”
• Anesthetics can produce muscle relaxation,
block transmission of pain nerve impulses and
suppress reflexes.
• It can also temporary decrease memory
retrieval and recall.
The effects of anesthesia are monitored by considering
the following parameters:
- Respiration
- O2 saturation / CO2 level
- HR and BP
- Urine output
Types of Anesthesia
1. General Anesthesia
reversible state consisting of complete loss of
consciousness and sensation.
protective reflexes such as cough and gag are lost
provides analgesia, muscle relaxation and sedation.
produces amnesia and hypnosis.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 7
Prepared By: Mark Fredderick R Abejo R.N, MAN
Techniques used in General Anesthesia E. Intravenous Block ( Beir block )
often used for arm,wrist and hand procedure
A. Intravenous Anesthesia an occlusion tourniquet is applied to the extremity to
prevent infiltration and absorption of the injected IV
This is being administered intravenously and agents beyond the involved extremity.
extremely rapid.
Its effect will immediately take place after thirty
minutes of introduction.
It prepares the client for smooth transition to the
surgical anesthesia.
B. Inhalation Anesthesia
This comprises of volatile liquids or gas and
oxygen.
Administered through a mask or endotracheal tube
2. Regional Anesthesia
temporary interruption of the transmission of nerve
impulses to and from specific area or region of the
body.
achieved by injecting local anesthetics in close
proximity to appropriate nerves.
reduce all painful sensation in one region of the body Indicating a site for insertion of the lumber puncture
without inducing unconsciousness. needle into the subarachnoid space of the spinal
agents used are lidocaine and bupivacaine. canal.
Techniques used in Regional Anesthesia:
A. Topical Anesthesia
applied directly to the skin and mucous membrane,
open skin surfaces, wounds and burns.
readily absorbed and act rapidly
used topical agents are lidocaine and benzocaine.
B. Spinal Anesthesia ( Subarachnoid block )
local anesthetic is injected through lumbar puncture,
between L2 and S1
anesthetic agent is injected into subarachoid space
surrounding the spinal cord. F. Caudal Anesthesia
- Low spinal, for perineal/rectal areas Is produced by injection of the local anesthetic into
- Mid spinal T10 ( below level of umbilicus) the caudal or sacral canal
for hernia repair and appendectomy.
- High spinal T4 ( nipple line ), for CS G. Field Block Anesthesia
anesthetic block conduction in spinal nerve roots and The area proximal to a planned incision can be
dorsal ganglia; paralysis and analgesia occur below injected and infiltrated with local anesthetic agents.
level of injection
agents used are procaine, tetracaine, lidocaine and Stages of Anesthesia
bupivacaine. Onset / Induction. Extends from the
administration of anesthesia to the time of loss
C. Epidural Anesthesia of consciousness.
achieved by injecting local anesthetic into epidural
space by way of a lumbar puncture. Excitement / Delirium. Extends from the time
result similar to spinal analgesia of loss of consciousness to the time of loss of
agents use are chloroprocaine, lidocaine and lid reflex. Increase in autonomic activity and
bupivacaine. irregular breathing. It may be characterized by
shouting, struggling of the client.
D. Peripheral Nerve Block Surgical. Extends from the loss of lid reflex to
achieved by injecting a local anesthetic to anesthetize the loss of most reflexes. surgical procedure is
the surgical site. started.
agents use are chloroprocaine, lidocaine and
bupivacaine. Medullary / Stage of Danger. It is
characterized by respiratory and cardiac
depression or arrest. It is due to overdose of
anesthesia. Resuscitation must be done.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 8
Prepared By: Mark Fredderick R Abejo R.N, MAN
Complication and Discomforts of Anesthesia
Hypoventilation - inadequate ventilatory support
POSTOPERATIVE PHASE
after paralysis of respiratory muscles. Goals:
Oral Trauma Maintain adequate body system functions
Malignant Hyperthermia Restore homeostasis
Hypotension - due to preoperative hypovolemia or Alleviate pain and discomfort
untoward reactions to anesthetic agents. Prevent postop complication
Cardiac Dysrhythmia - due to preexisting Ensure adequate discharge planning and teaching.
cardiovascular compromise, electrolyte imbalance or
untoward reaction to anesthesia.
Hypothermia - due to exposure to a cool ambient
OR environment and loss of thermoregulation PACU CARE
capacity from anesthesia.
Peripheral Nerve Damage - due to improper
positioning of patient or use of restraints. Transport of client from OR to RR
Nausea and Vomiting avoid exposure
Headache avoid rough handling
avoid hurried movement and rapid changes in
position.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 9
Prepared By: Mark Fredderick R Abejo R.N, MAN
Initial Nursing Assessment Use mechanical ventilation to maintain adequate
pulmonary ventilation if required.
Verify patient’s identity, operative procedure and the
surgeon who performed the procedure. Assessing Thermoregulatory Status
Evaluate the following sign and verify their level of Monitor temperature per protocol to be alert for
stability with the anesthesiologist: malignant hyperthermia or to detect hypothermia.
- Respiratory status Report a temperature over 37.8 C or under 36.1 C
- Circulatory status Monitor for postanesthesia shivering, 30-45 minutes
- Pulses after admission to the PACU.
- Temperature Provide a therapeutic environment with proper
- Oxygen Saturation level temperature and humidity.
- Hemodynamic values
Determine swallowing and gag reflex , LOC and Maintaining Adequate Fluid Volume
patients response to stimuli.
Evaluate lines, tubes, or drains, estimate blood loss, Administer I.V solutions as ordered.
condition of wound, medication used, transfusions and Monitor evidence of F&E imbalance such as N&V
output. and weakness.
Evaluate the patient’s level of comfort and safety. Evaluate mental status, skin color and turgor
Perform safety check; side rails up and restraints are Recognized signs of:
properly in placed. a. Hypovolemia
Evaluate activity status, movement of extremities. - decrease BP
- decrease urine output
Review the health care provider’s orders.
- decreased CVP
- increased pulse
Initial Nursing Interventions
b. Hypervolemia
- increase BP
Maintaining a Patent Airway
- changes in lung sounds (S3 gallop )
- increased CVP
Allow the airway ( ET tube ) to remain in place until
Monitor I&O
the patient begins to waken and is trying to eject the
airway.
Minimizing Complications of Skin Impairment
The airway keeps the passage open and prevents the
tongue from falling backward and obstructing the air
Perform handwashing before and after contact with
passages.
the patient
Aspirate excessive secretions when they are heard in
Inspect dressings routinely and reinforce them if
the nasopharynx and oropharynx.
necessary.
Record the amount and type of wound drainage.
Assessing Status of Circulatory System
Turn patient frequently and maintain good body
alignment.
Take VS per protocol, until patient is well stabilized.
Monitor intake and output closely.
Maintaining Safety
Recognized early symptoms of shock or hemorrhage:
Keep the side rails up until the patient is fully awake.
- cool extremities
Protect the extremity into which I.V fluids are
- decreased urine output ( less than 30ml/hr )
running so needle will not become accidentally
- slow capillary refill ( greater than 3 sec. )
dislodged.
- lowered BP
Avoid nerve damage and muscle strain by properly
- narrowing pulse pressure
supporting and padding pressure areas.
- increased heart rate
Recognized that the patient may not be able to
* initiate O2 therapy, to increase O2
complain of injury such as the pricking of an open
availability from the blood.
safety pin or clamp that is exerting pressure.
* place the patient in shock position with his
Check dressing for constriction
feet elevated ( unless contraindicated )
Promoting Comfort
Maintaining Adequate Respiratory Function
Assess pain by observing behavioral and physiologic
manifestations.
Place the patient in lateral position with neck
Administer analgesic and document efficacy.
extended ( if not contraindicated ) and upper arm
Position the patient to maximize comfort.
supported on a pillow.
Turn the patient every 1 to 2 hours to facilitate
breathing and ventilation.
Parameter for Discharge from PACU/RR
Encourage the patient to take deep breaths, use an
incentive spirometer.
Activity. Able to obey commands
Assess lung fields frequently by auscultation.
Periodically evaluate the patient’s orientation – Respiratory. Easy, noiseless breathing
response to name and command. Circulation. BP within 20mmHg of preop level
Note: Alterations in cerebral function may suggest Consciousness. Responsive
impaired O2 delivery. Color. Pinkish skin and mucus membrane
Administer humidified oxygen if required.
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 10
Prepared By: Mark Fredderick R Abejo R.N, MAN
Nursing Care of the Client During the Intermediate
Postop Period (RR – Unit ) Goals:
o Restore homeostasis and prevent complication.
Baseline Assessment o Maintain adequate cardiovascular and tissue
Respiratory Status perfusion.
Cardiovascular Status o Maintain adequate respiratory function.
- VS o Maintain adequate nutrition and elimination.
- Color and Temperature of Skin o Maintain adequate fluid and electrolyte balance.
Level of Consciousness o Maintain adequate renal function.
Tubes o Promote adequate rest, comfort and safety.
- Drain o Promote adequate wound healing.
- NGT o Promote and maintain activity and mobility.
- T-tube o Provide adequate psychological support.
Position
MS Perioperative Nursing Abejo
Lecture Notes on Perioperative Nursing 11
Prepared By: Mark Fredderick R Abejo R.N, MAN
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 12
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
WOUND CARE
Frequently used Dressing
Materials Common dressing Irrigating a wound
Montgomery Straps holding dressing
The strips of tape should be placed at the ends of
the dressing and must be sufficiently long and wide to
secure the dressing. The tape should adhere to intact skin.
Cleaning Surgical Site
Cleaning a wound outward
from the incision
Cleaning from top to bottom Cleaning around a
Starting at the center Penrose drain site
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 13
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
INCISION SUPPORTING
BODY PRESSURE AREAS:
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 14
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
POST OPERATIVE COMPLICATIONS
Problem Description Cause Clinical Signs Nursing Intervention
RESPIRATORY
Pneumonia Inflammation of the Infection - elevated temp. Deep breathing exercises
lung parenchyma / Toxin / irritants - cough Coughing exercise
alveoli causing - blood tinged Early ambulation
inflammatory sputum
process - dyspnea
- chest pain
Infectious Cause by
Pneumonia streptococcus
pneumoniae /
Staphylococcus
aureus
Hypostatic Immobility
Pneumonia Impaired
ventilation
Aspiration Aspiration of
Pneumonia gastric contents,
food
Atelectasis A condition in Mucous plugs - Fever ( 1st 24 Deep breathing exercises
which alveoli blocking bronchial hours) Coughing exercise
collapsed and are passageways - Dyspnea Early ambulation
not ventilated Inadequate lung - Tachycardia
expansion - Diaphoresis
Immobility - Pleural pain
- Dull or absent
lung sounds
- Dec. SaO2
Pulmonary Blood clot that has Immobility - Sudden chest Turning
Embolism moved to the lungs Use of oral pain Ambulation
and blocks a contraceptives - SOB Anti embolic stockings
pulmonary artery Coagulation - Cyanosis Compression devises
and obstruct blood problem - Tachycardia Prevent massaging the
flow to the lungs - Low BP lower extremities
CIRCULATION
Hypovolemia Inadequate Hemorrhage - Tachycardia Fluid and blood
circulating blood Fluid deficit - Dec. urine replacement
volume output
- Dec. BP
Hemorrhage Internal or external Disruption of - Cold, moist and Fluid and blood
bleeding sutures pale skin replacement
Insecure ligation of - Deep, rapid RR Vit.k and hemostat
Capillary – slow blood vessels - Low temp Ligation of bleeders
generalized oozing - Increase pain Pressure dressing
Venous – dark in - Inc. abd. girth
color and bubble out - Swelling or
Arterial – spurts, bruising around
bright red in color incision
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 15
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
Overt Bleeding
- Dressing
saturated with
bright blood
- Bright, free-
flowing blood in
drains or tubes.
Thrombophlebitis Inflammation of the Slowed venous - Homan’s Sign Early ambulation
veins, usually of the blood flow due to pain, discomfort in Anti embolic stocking
legs and associated immobility or calf when foot is Encourage leg exercise
with a blood clot. prolonged sitting dorsiflexed Hydrate adequately
Trauma to the vein - Aching, cramping Avoid any restricting
Increased blood pain devices that impaired
coagulability. - Swollen, red and circulation
hot to touch Avoid massage on the
- Vein feels hard calf of the leg
Initiate anticoagulant
Arterial
therapy
- Pain
- Pallor on the
affected
Blood clot attached extremities
to wall of vein or - Dec./absent of
Thrombus artery peripheral pulse
Note:
Careful maintenance of
Embolus in the
IV catheters
Foreign body or clot Broken IV catheter venous system
that has moved from Fat usually becomes a
Embolus its site of formation Amniotic fluid pulmonary
to another area of embolus
the body
URINARY
Urinary Inability to empty Depressed bladder - Larger fluid Monitor I & O
Retention the bladder, with muscle tone from intake than output Interventions to facilitate
excessive narcotics and - Inability to void voiding
accumulation of anesthetics - Bladder Urinary Catheterization
urine in the bladder Handling of tissue distention as needed
during surgery on - Suprapubic
adjacent organs discomfort
Spasm of the - Restlessness
bladder sphincter
Urinary Inability of the Loss of tone of the - 30 – 60 ml of Monitor I & O
Incontinence bladder to hold bladder sphincter urine q 15-30 mins
accumulated urine
Urinary Tract Inflammation of the Immobilization - Fever ( 48 hours Adequate fluid intake
Infection bladder, ureters or Limited fluid postop) Early ambulation
urethra intake - Burning sensation Aseptic catheterization as
when voiding needed
- Urgency Good perineal hygiene
- Cloudy urine
- Lower abdominal
pain
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 16
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
GASTRO-
INTESTINAL
Nausea and Pain - Complaints of IV fluids until peristalsis
Vomiting Abdominal feeling sick to the returns
distention stomach Progressive diet ( clear
Ingestion of fluid - Retching liquid then full fluids, soft
or food before the - Gagging then regular diet)
return of peristalsis Anti emetics as ordered
Tympanities Retention of gases Slowed motility of - Abdominal Early ambulation
within the intestines the intestines due to distention Avoid using straw
effects of anesthesia - Absence of bowel Provide ice chips
sound
Hiccups Intermittent spasms Irritation of - A sound NGT insertion as needed
of the diaphragm phrenic nerve bet. “hic” that result Hold breath while taking
the spinal cord and from the vibration a large swallow of water
terminal of closed vocal Breath in and out on a
ramifications on cords as air rushes paper bag
undersurface of the suddenly into the Anti emetics as ordered
diaphragm lungs
Abdominal
distention
Intestinal Kink loop of Due to - Intermittent NGT insertion as needed
Obstruction intestines inflammatory sharp, colicky Administered IVF as
( 3rd-5th day adhesions abdominal pains ordered
postop) - Nausea & Prepare for possible
Vomiting surgery
- Abdominal
distention
- Hiccups
- No bowel
movement
Constipation Infrequent or no Lack of dietary - Absence of stool Adequate hydration
stool passage for roughage elimination High fiber diet
abnormal length of Analgesics - Abdominal Encourage early
time Immobility distention ambulation
( within 48 hours - Abdominal
after solid diet discomfort
started )
Paralytic Ileus Lack of peristaltic Due to anesthetics - Abdominal pain Encourage early
activity Immobility - Abdominal ambulation
distention
- Constipation
- Absence of bowel
sounds
WOUND
Wound Infection Inflammation and Poor aseptic - Fever ( 72 hours Keep wound clean and
infection of incision techniques postop) dry
or drain site - Redness, swelling Surgical aseptic technique
, pain and warmth when changing dressing
- Pus or discharge Antibiotic therapy
on the wound site
- Foul smelling
discharge
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 17
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
Wound Separation of a - Increased incision
Dehiscence suture line before drainage Apply abdominal binders
the incision heals - Tissues Encourage high protein
Malnutrition underlying skin diet and Vit.C intake
emaciation/obesity become visible Keep in bed rest
Excessive strain on
suture line
Wound Extrusion of internal Poor circulation - Opening of Semi-Fowlers, bend
Evisceration organ or tissues incision and visible knees to relieve tension on
through the incision protrusion of the abdominal muscles
organs Splinting on coughing
Cover exposed organ with
sterile , moist saline
dressing
Reassure, keep him/her
quite and relaxed
Prepare for surgery and
repair of wound
PSYCHOLOGIC
Postoperative Altered Mood Weakness - Anorexia Adequate rest
Depression Surprise nature of - Tearfulness Physical activity
“E” surgery - Withdrawal Opportunity to express
News of - Rejection of anger and other negative
malignancy others feelings
Severely altered - Sleep
body image disturbances
Delirium / Acute Dehydration - Poor memory Sedatives to keep client
Confusional State Insufficient - Restlessness quite and comfortable
oxygenation - Inattentive Explain reasons for
Anemia - Inappropriate interventions
Hypotension behavior Listen and talk to the
Hormonal - Wild excitement client
Imbalances - Hallucination Provide physical comfort
Infection - Delusions
- Disoriented
Trauma
- Sleep
disturbances
MS Perioperative Nursing Abejo
STI Global City College of Nursing / QMMC Surgery Ward Exposure
Lecture Notes on Perioperative Nursing 18
Prepared By: Mark Fredderick R Abejo R.N
Clinical Instructor
STUDY HARD
GOD BLESS YOU
THANKS
Mark Fredderick R. Abejo R.N, M.A.N
Clinical Instructor
MS Perioperative Nursing Abejo
Вам также может понравиться
- Perioperative NursingДокумент253 страницыPerioperative NursingCherr May Olesco - Nalasa100% (4)
- Perioperative NursingДокумент41 страницаPerioperative Nursingbajaoc100% (8)
- Perioperative Nursing 1Документ2 страницыPerioperative Nursing 1Rosie Cuasito100% (2)
- Perioperative Nursing Phases and ResponsibilitiesДокумент12 страницPerioperative Nursing Phases and ResponsibilitiesIrish Jane Gallo100% (11)
- FUNDAMENTALS OF NURSING: Passbooks Study GuideОт EverandFUNDAMENTALS OF NURSING: Passbooks Study GuideРейтинг: 5 из 5 звезд5/5 (1)
- Perioperative Nursing LectureДокумент125 страницPerioperative Nursing LectureHazel Von S. Bravo88% (24)
- 2020 NCLEX-PN Test Prep. Questions and Answers with Explanations: Study Guide to Pass the License Exam Effortlessly - Exam Review for Practical NursesОт Everand2020 NCLEX-PN Test Prep. Questions and Answers with Explanations: Study Guide to Pass the License Exam Effortlessly - Exam Review for Practical NursesРейтинг: 1 из 5 звезд1/5 (1)
- Perioperative Nursing Phases and PrinciplesДокумент5 страницPerioperative Nursing Phases and PrinciplesLester Aliser Labra100% (4)
- Emergency and Disaster NursingДокумент20 страницEmergency and Disaster NursingNeil Cuasito89% (9)
- Fundamentals of NursingДокумент8 страницFundamentals of NursingFreeNursingNotes92% (13)
- Perioperative NursingДокумент8 страницPerioperative NursingGil Platon Soriano100% (3)
- Emergency Nursing Exam and RatioДокумент5 страницEmergency Nursing Exam and RatioCharisse TaylanОценок пока нет
- NCLEX: Pharmacology for Nurses: 100 Practice Questions with Rationales to help you Pass the NCLEX!От EverandNCLEX: Pharmacology for Nurses: 100 Practice Questions with Rationales to help you Pass the NCLEX!Рейтинг: 5 из 5 звезд5/5 (4)
- Perioperative NursingДокумент12 страницPerioperative Nursingtheglobalnursing100% (12)
- Guide to the Code of Ethics for Nurses: Interpretation and ApplicationОт EverandGuide to the Code of Ethics for Nurses: Interpretation and ApplicationОценок пока нет
- Perioperative NSG Care MGTДокумент56 страницPerioperative NSG Care MGTinchack100% (1)
- Schaum's Outline of Critical Care Nursing: 250 Review QuestionsОт EverandSchaum's Outline of Critical Care Nursing: 250 Review QuestionsРейтинг: 5 из 5 звезд5/5 (1)
- Code of Ethics for Nurses with Interpretive StatementsОт EverandCode of Ethics for Nurses with Interpretive StatementsРейтинг: 5 из 5 звезд5/5 (2)
- Setting Up An IV InfusionДокумент6 страницSetting Up An IV InfusionNoel97% (31)
- NLN PAX Practice: PAX-RN Practice Test QuestionsОт EverandNLN PAX Practice: PAX-RN Practice Test QuestionsОценок пока нет
- 2018 NCLEX-PN Test Prep. Questions and Answers with Explanations: Study Guide to Pass the License Exam Effortlessly - Exam Review for Practical NursesОт Everand2018 NCLEX-PN Test Prep. Questions and Answers with Explanations: Study Guide to Pass the License Exam Effortlessly - Exam Review for Practical NursesРейтинг: 4.5 из 5 звезд4.5/5 (2)
- Emergency NursingДокумент13 страницEmergency NursingPhilip Jay Braga100% (5)
- Peri Operative NursingДокумент22 страницыPeri Operative NursingIvyBanez100% (1)
- Handout Medical-Surgical Nursing Fluid and ElectrolyteДокумент13 страницHandout Medical-Surgical Nursing Fluid and ElectrolytePaul Christian P. Santos, RN100% (10)
- Perioperative Nursing - 50 ItemsДокумент6 страницPerioperative Nursing - 50 Itemsapi-371817496% (26)
- Fundamentals of NursingДокумент21 страницаFundamentals of Nursingstuffednurse82% (22)
- Fluid and Electrolytes for Nursing StudentsОт EverandFluid and Electrolytes for Nursing StudentsРейтинг: 5 из 5 звезд5/5 (12)
- MEDICAL SURGICAL NURSING: Passbooks Study GuideОт EverandMEDICAL SURGICAL NURSING: Passbooks Study GuideОценок пока нет
- Perioperative NursingДокумент32 страницыPerioperative NursingMaria Garcia Pimentel Vanguardia II100% (2)
- Emergency NursingДокумент41 страницаEmergency NursingDr. Jayesh Patidar100% (2)
- Perioperative Nursing ConceptДокумент21 страницаPerioperative Nursing ConceptArgee Alonsabe100% (8)
- A Handbook for Student Nurses, 201617 edition: Introducing key issues relevant for practiceОт EverandA Handbook for Student Nurses, 201617 edition: Introducing key issues relevant for practiceРейтинг: 4 из 5 звезд4/5 (1)
- Test Bank CardioДокумент16 страницTest Bank CardioLudwigJayBarayuga86% (7)
- Emergency Nursing Notes 2Документ14 страницEmergency Nursing Notes 2pauchanmnl100% (3)
- Perioperative Nursing SkillsДокумент278 страницPerioperative Nursing SkillsNacel Celeste100% (3)
- Perioperative NursingДокумент271 страницаPerioperative NursingCodered Review100% (3)
- Fundamentals of Nursing Chapter ExamДокумент13 страницFundamentals of Nursing Chapter ExamAlfred Benjamin Cajita100% (4)
- Perioperative Nursing Quiz: Cardiovascular, Anesthesia & Post-Op CareДокумент4 страницыPerioperative Nursing Quiz: Cardiovascular, Anesthesia & Post-Op Caregladz25100% (1)
- Medical-Surgical Nursing 1Документ332 страницыMedical-Surgical Nursing 1KoRnflakes93% (15)
- Intra - Operative NursingДокумент8 страницIntra - Operative NursingClaire SoletaОценок пока нет
- Operating Room ExamДокумент20 страницOperating Room ExamDoyTan100% (1)
- Basic Surgical InstrumentsДокумент37 страницBasic Surgical Instrumentsapi-2658787991% (33)
- Peri Operative NursingДокумент214 страницPeri Operative NursingJohn Ervin Agena100% (2)
- Skin PreparationДокумент2 страницыSkin Preparationoxidalaj100% (24)
- Manual in Operating Room Nursing 2011Документ205 страницManual in Operating Room Nursing 2011komite100% (9)
- Oncology Nursing (Word) Bulleted For NSG RevieweesДокумент8 страницOncology Nursing (Word) Bulleted For NSG Revieweesswitlipz100% (1)
- Perioperative Nursing CareДокумент17 страницPerioperative Nursing CareMisikir Eyob100% (1)
- PhilGEPS Buyers Training Certificate July 2012Документ1 страницаPhilGEPS Buyers Training Certificate July 2012lagundaОценок пока нет
- The Republic of The Philippines and U.S. Interests: Thomas LumДокумент26 страницThe Republic of The Philippines and U.S. Interests: Thomas LumToni ChanОценок пока нет
- Resume JennieДокумент3 страницыResume JennielagundaОценок пока нет
- Nursing Care Plan AppendicitisДокумент2 страницыNursing Care Plan Appendicitisderic95% (57)
- Disadvantages of Using MOBILE PHONES in The Lives-1Документ7 страницDisadvantages of Using MOBILE PHONES in The Lives-1lagundaОценок пока нет
- Ext Ventricular DrainДокумент2 страницыExt Ventricular DrainlagundaОценок пока нет
- Metastatic Breast Cancer Treatment OptionsДокумент30 страницMetastatic Breast Cancer Treatment OptionslagundaОценок пока нет
- Nursing Care Plan Chronic Obstructive Pulmonary Disease (COPD)Документ2 страницыNursing Care Plan Chronic Obstructive Pulmonary Disease (COPD)deric95% (41)
- Head Injury Is A Broad Classification That IncludesДокумент5 страницHead Injury Is A Broad Classification That IncludeslagundaОценок пока нет
- Local Anesthetics VeterinaryДокумент32 страницыLocal Anesthetics VeterinaryEssi Rehc100% (1)
- Continuous Peripheral Nerve Block For PoДокумент5 страницContinuous Peripheral Nerve Block For PoBinОценок пока нет
- Ultrasound-Guided Quadratus Lumborum Block An Updated Review of Anatomy and TechniquesДокумент7 страницUltrasound-Guided Quadratus Lumborum Block An Updated Review of Anatomy and TechniquesWilmer Yanquen VillarrealОценок пока нет
- Manual of Regional Anesthesia PDFДокумент119 страницManual of Regional Anesthesia PDFxyrosОценок пока нет
- Anestesi - Jenis & Obat AnestesiДокумент37 страницAnestesi - Jenis & Obat AnestesiIrene Regina ArdisОценок пока нет
- Sd. Compartimental y AR A CL 2022Документ19 страницSd. Compartimental y AR A CL 2022Alejandra SanchezОценок пока нет
- OSCE Checklist ABG SamplingДокумент2 страницыOSCE Checklist ABG SamplingPiyali SahaОценок пока нет
- An Unusual Laryngeal Complication Following Inferior Alveolar Nerve BlockДокумент2 страницыAn Unusual Laryngeal Complication Following Inferior Alveolar Nerve BlockJaime Ruiz Jr.Оценок пока нет
- Topical AnaesthesiaДокумент7 страницTopical Anaesthesiapaul WongОценок пока нет
- Maxillary Anesthetic TechniquesДокумент55 страницMaxillary Anesthetic TechniquesMera Emad100% (4)
- S2 Nail Surgery Whilst Pregnant or Breastfeeding V2Документ2 страницыS2 Nail Surgery Whilst Pregnant or Breastfeeding V2Aswathy KumaranОценок пока нет
- 2020 Mcqs Pain ControlДокумент29 страниц2020 Mcqs Pain Controlareej alblowi100% (1)
- Core MGMT PDFДокумент517 страницCore MGMT PDFCristianFranceschiОценок пока нет
- BJAS - Volume 5 - Issue Issue 1 Part (2) - Pages 275-281Документ7 страницBJAS - Volume 5 - Issue Issue 1 Part (2) - Pages 275-281Vengky UtamiОценок пока нет
- Thoracic Epidural Anaesthesia and AnalgesiaДокумент8 страницThoracic Epidural Anaesthesia and AnalgesiamishelОценок пока нет
- Part 6 Anesthesiology: Anesthesiology and Its DevelopmentДокумент24 страницыPart 6 Anesthesiology: Anesthesiology and Its DevelopmentburhaninhoОценок пока нет
- Pain Treatment 14 I TaeДокумент329 страницPain Treatment 14 I TaejfarcoОценок пока нет
- Nursing Journal PACUДокумент11 страницNursing Journal PACUJet BautistaОценок пока нет
- Anaesthetic and Muscle Relaxant Agents: DR David N.MusyokaДокумент43 страницыAnaesthetic and Muscle Relaxant Agents: DR David N.MusyokaIrene Zae MwandotoОценок пока нет
- Docshare - Tips - DNB Question Paper System Wise DNB Anaesthesia PDFДокумент88 страницDocshare - Tips - DNB Question Paper System Wise DNB Anaesthesia PDFMuthuОценок пока нет
- Spinal Anesthesia: Monica M. Mordecai and Sorin J. BrullДокумент7 страницSpinal Anesthesia: Monica M. Mordecai and Sorin J. Brulljaka purna yudhaОценок пока нет
- Epidural Information CardДокумент2 страницыEpidural Information Cardheba abuhelwaОценок пока нет
- On The Concept of Third Occipital HeadacДокумент7 страницOn The Concept of Third Occipital HeadacVladislav KotovОценок пока нет
- Blocking The Pathway of Painful ImpulsesДокумент9 страницBlocking The Pathway of Painful Impulsesرامي الوافيОценок пока нет
- Akukwata SeminarДокумент22 страницыAkukwata SeminarjenniferОценок пока нет
- EXPAREL Prescribing InformationДокумент17 страницEXPAREL Prescribing InformationcignalОценок пока нет
- Analgesia For Iliac Crest Bone GraftДокумент9 страницAnalgesia For Iliac Crest Bone GraftDominik Chirito PastorОценок пока нет
- Local AnesthesiaДокумент25 страницLocal Anesthesiaapi-19916399Оценок пока нет
- LocalanestheticsДокумент51 страницаLocalanestheticskingkb4uОценок пока нет
- Regional Anesthesia for Hand Surgery: Bier Block LectureДокумент28 страницRegional Anesthesia for Hand Surgery: Bier Block LectureJessica CОценок пока нет