Академический Документы
Профессиональный Документы
Культура Документы
Floating Balls in Ovarian Cyst
Загружено:
Eduardo FerreiraИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Floating Balls in Ovarian Cyst
Загружено:
Eduardo FerreiraАвторское право:
Доступные форматы
Letters to the Editor
2. Tandon A, Agarwal R, Tandon R, et al. Multiple intracystic floating
balls: an unusual but unique sonographic pattern of mature cystic ter-
atoma. BMJ Case Rep. 2011;2011:bcr0320113962.
3. Park SB, Kim JK, Kim KR, et al. Imaging findings of complications and
unusual manifestations of ovarian teratomas. Radiographics. 2008;28:
969–83.
4. Gürel H, Gürel SA. Ovarian cystic teratoma with a pathognomonic ap-
pearance of multiple floating balls: a case report and investigation of
common characteristics of the cases in the literature. Fertil Steril.
2008;90:2008.e17–9.
5. Outwater EK, Siegelman ES, Hunt JL. Ovarian teratomas: tumor types
and imaging characteristics. Radiographics. 2001;21:475–90.
6. Tongsong T, Wanapirak C, Khunamornpong S, et al. Numerous intra-
cystic floating balls as a sonographic feature of benign cystic teratoma:
report of 5 cases. J Ultrasound Med. 2006;25:1587–91.
7. Heo SH, Kim JW, Shin SS, et al. Review of ovarian tumors in children
and adolescents: radiologic-pathologic correlation. Radiographics. 2014;
34:2039–55.
8. Salvadori PS, Bomfim LN, von Atzingen AC, et al. Spontaneous rupture
of ovarian cystadenocarcinoma: pre- and post-rupture computed tomog-
raphy evaluation. Radiol Bras. 2015:330–2.
9. Lima LLA, Parente RCM, Maestá I, et al. Clinical and radiological cor-
relations in patients with gestational trophoblastic disease. Radiol Bras.
2016;49:241–50.
10. Guerra LFA, Pessanha LB, Oliveira GA, et al. Endometrial osseous
metaplasia: sonographic, radiological and histopathological findings.
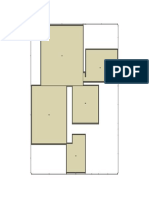
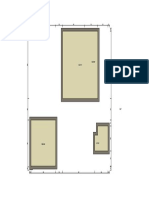
Figure 1. Ultrasound (A); sagittal T2-weighted MRI sequence (B); out-of-phase Radiol Bras. 2016;49:62–3.
T1-weighted gradient-echo MRI sequence (C); and in-phase T1-weighted gradi- 11. Queiroz RM, Costa PP, Oliveira NYF, et al. Female urethral diverticu-
ent-echo MRI sequence (D). Note the expansile cystic lesion with heterogeneous lum containing a urothelial carcinoma. Radiol Bras. 2016;49:406–7.
content, containing numerous oval formations that were hyperechoic on the ultra- 12. Manikkavasakar S, Ramachandram A, Ramalho M, et al. Malignant
sound and showed intermediate signal intensity in the T1- and T2-weighted se- uterine disease with concurrent miometrial contraction at MRI: a pos-
quences, with no evidence of signal loss in the out-of-phase T1-weighted gradi- sible source of overstaging. Radiol Bras. 2016;49:342–3.
ent-echo sequence.
13. Donnadieu AC, Deffieux X, Le Ray C, et al. Unusual fast-growing ova-
rian cystic teratoma during pregnancy presenting with intracystic fat
MRI, the fat seen within the lesion produces a hyperintense sig- “floating balls” appearance. Fertil Steril. 2006;86:1758–9.
nal on T1-weighted images and signal loss in fat-saturated se- 14. Altinbas SK, Yalvac S, Kandemir O, et al. An unusual growth of ovarian
quences(3,5,7). In rare cases, the presentation of MCT is atypical, cystic teratoma with multiple floating balls during pregnancy: a case
which can be a diagnostic challenge for radiologists(2,6). Multiple report. J Clin Ultrasound. 2010;38:325–7.
small floating spheres within a large cyst, as observed in the case 15. Rao JR, Shah Z, Patwardhan V, et al. Ovarian cystic teratoma: deter-
mined phenotypic response of keratocytes and uncommon intracystic
presented here, is one of those rare presentations, known as the
floating balls appearance on sonography and computed tomography. J
“floating ball” presentation(4,6). Histologically, the spheres are Ultrasound Med. 2002;21:687–91.
composed of keratin, fibrin, hemosiderin, sebaceous debris, hair, 16. Kawamoto S, Sato K, Matsumoto H, et al. Multiple mobile spherules in
and fat, in variable proportions(2,6,13). Although the mechanism mature cystic teratoma of the ovary. AJR Am J Roentgenol. 2001;176:
of formation of these spheres has yet to be clarified, it is specu- 1455–7.
lated that it involves aggregation of sebaceous material around a
Ana Paula Barroso Pazinatto Espindola1, Viviane
nidus(2,4,14). The mobility of the spheres is due to their low density Brandão Amorim2, Hilton Augusto Koch1, Paulo Roberto
relative to the other content of the cyst(2,4,6). A finding of multiple Valle Bahia2, Márcio V. P. Almeida2
floating spheres within a single large cyst has not been reported 1. Pontifícia Universidade Católica do Rio de Janeiro (PUC-Rio), Rio de
for other types of tumors and is therefore considered pathogno- Janeiro, RJ, Brazil. 2. Centro Estadual de Diagnóstico por Imagem do
monic of MCT(2,4,6,14–16). Rio de Janeiro (CEDI), Rio de Janeiro, RJ, Brazil. Mailing address: Dra.
Ana Paula Barroso Pazinatto Espindola. Rua Vinícius de Moraes, 71,
REFERENCES Ipanema. Rio de Janeiro, RJ, Brazil, 22411-010. E-mail: apazinatto@
1. Rha SE, Byun JY, Jung SE, et al. Atypical CT and MRI manifestations yahoo.com.br.
of mature ovarian cystic teratomas. AJR Am J Roentgenol. 2004;183:
743–50. http://dx.doi.org/10.1590/0100-3984.2015.0155
Self-limiting thoracic aortic dissection during bronchial artery tery and the left pulmonary artery. During manual-injection digi-
embolization tal subtraction angiography, enhancement and stagnation of the
contrast media were observed in a false lumen of the descending
Dear Editor, thoracic aorta (Figures 1B and 1C), consistent with iatrogenic
A 75-year-old woman presented with a 3-week history of in- aorta dissection. The iatrogenic aortic dissection extended to the
termittent hemoptysis related to a history of recurrent episodes of left bronchial artery, leading to obstruction of blood flow to the
pneumonia. Chest computed tomography (CT) showed cylindri- shunt. However, there were no signs of hemodynamic instability,
cal bronchiectasis in the lingula, and bronchoscopy showed clots and the patient therefore received conservative therapy with clini-
in the left bronchial tree. Bronchial arteriography was requested cal and radiological monitoring. A second CT scan, obtained 7
and revealed a shunt (Figure 1A) between the left bronchial ar- days later, showed that the iatrogenic aorta dissection was stable
Radiol Bras. 2017 Mai/Jun;50(3):199–208 207
Letters to the Editor
D
Figure 1. A: Left bronchial arteriography showing a shunt (arrowheads) between the left bronchial artery (LBA) and the left pulmonary artery (LPA). B,C: Stagnation of
the contrast media (arrowheads) can be seen at the false lumen of the descending thoracic aorta, indicating dissection. D: Coronal CT reconstruction at 7 days after
bronchial arteriography showing persistence of the contrast media in the false lumen of the thoracic aorta (arrows), with no increase in the extent of the dissection.
(Figure 1D), and a third scan, obtained 5 months later, showed diagnostic and interventional bronchial arterial embolisation. Rofo. 2015;
total resolution. During 7 months of follow-up, the patient reported 187:248–59.
no pain or new episodes of bleeding. 4. Uflacker R, Kaemmerer A, Picon PD, et al. Bronchial artery emboliza-
tion in the management of hemoptysis: technical aspects and long-term
During endovascular procedures, iatrogenic aortic dissection results. Radiology. 1985;157:637–44.
can occur when the tip of the catheter is pushed into the vessel 5. Mal H, Rullon I, Mellot F, et al. Immediate and long-term results of
wall during catheterization, as well as when high-pressure jets of bronchial artery embolization for life-threatening hemoptysis. Chest.
contrast media are directed toward the vessel wall. Although un- 1999;115:996–1001.
common, iatrogenic aortic dissection accounts for approximately 6. Erbel R, Aboyans V, Boileau C, et al. 2014 ESC Guidelines on the diag-
5% of all thoracic aortic dissections(1,2). In a review article, Ittrich nosis and treatment of aortic diseases: document covering acute and
chronic aortic diseases of the thoracic and abdominal aorta of the adult.
et al.(3) showed rates of subintimal short segment dissection of
The Task Force for the Diagnosis and Treatment of Aortic Diseases of
the aorta during bronchial arteriography ranging from 1% to the European Society of Cardiology (ESC). Eur Heart J. 2014;35:2873–
6.3%(4,5), although there are virtually no images of such dissec- 926.
tions in the literature. There is no standard for the management 7. LeMaire SA, Russell L. Epidemiology of thoracic aortic dissection. Nat
of iatrogenic thoracic aorta dissection. Uncomplicated dissection Rev Cardiol. 2011;8:103–13.
of the descending thoracic aorta is a relatively benign process, and 8. Nienaber CA, Divchev D, Palisch H, et al. Early and late management of
complete spontaneous resolution is observed in most cases. Phar- type B aortic dissection. Heart. 2014;100:1491–7.
macological treatment to control pain and blood pressure is rec- Rafael Dahmer Rocha1, Joaquim Maurício da Motta-
ommended, as is short-term follow-up with CT(6–8). Leal-Filho1, Francisco Leonardo Galastri1, Breno Boueri
Affonso1, Humberto Bogossian1, Felipe Nasser1
REFERENCES
1. Department of Interventional Radiology and Pulmonology, Hospital
1. Nienaber CA, Fattori R, Mehta RH, et al. Gender-related differences in Israelita Albert Einstein, São Paulo, SP, Brazil. Mailing address: Dr.
acute aortic dissection. Circulation. 2004;109:3014–21. Rafael Dahmer Rocha. Avenida Albert Einstein, 627/701, Jardim Leonor.
2. Januzzi JL, Sabatine MS, Eagle KA, et al. Iatrogenic aortic dissection. São Paulo, SP, Brazil, 05652-900. E-mail: rafaeldrocha@gmail.com.
Am J Cardiol. 2002;89:623–6.
3. Ittrich H, Klose H, Adam G. Radiologic management of haemoptysis: http://dx.doi.org/10.1590/0100-3984.2015.0216
208 Radiol Bras. 2017 Mai/Jun;50(3):199–208
Вам также может понравиться
- Cell Movement and Neoplasia: Proceedings of the Annual Meeting of the Cell Tissue and Organ Culture Study Group, Held at the Janssen Research Foundation, Beerse, Belgium, May 1979От EverandCell Movement and Neoplasia: Proceedings of the Annual Meeting of the Cell Tissue and Organ Culture Study Group, Held at the Janssen Research Foundation, Beerse, Belgium, May 1979M. De BrabanderРейтинг: 5 из 5 звезд5/5 (1)
- Ultrasound in Obstet Gyne - 2003 - Jantarasaengaram - Cystic Ovarian Teratoma With Intracystic Fat BallsДокумент2 страницыUltrasound in Obstet Gyne - 2003 - Jantarasaengaram - Cystic Ovarian Teratoma With Intracystic Fat BallsBrando Ellioth tayoОценок пока нет
- Letter To The Editor: Int. J. Oral Maxillofac. Surg. 2018 XXX: XXX-XXXДокумент2 страницыLetter To The Editor: Int. J. Oral Maxillofac. Surg. 2018 XXX: XXX-XXXmehak malhotraОценок пока нет
- Sacrococcygeal Teratoma in A Child: A Case Report: Yam B Roka, M Shrestha, S PandeyДокумент3 страницыSacrococcygeal Teratoma in A Child: A Case Report: Yam B Roka, M Shrestha, S PandeyM Sudha DipikaОценок пока нет
- Testicular Plasmacytoma: Appearance On Gray-Scale and Power Doppler SonographyДокумент2 страницыTesticular Plasmacytoma: Appearance On Gray-Scale and Power Doppler SonographyViktor TrajkovskiОценок пока нет
- Calvi Et Al Osteoblastic Cells Regulate The Haematopoietic Stem Cell NicheДокумент6 страницCalvi Et Al Osteoblastic Cells Regulate The Haematopoietic Stem Cell NicheNicky KellyОценок пока нет
- History of Medicine First Case of Osteosarcoma in A Dinosaur: A Multimodal DiagnosisДокумент2 страницыHistory of Medicine First Case of Osteosarcoma in A Dinosaur: A Multimodal DiagnosisJonathan SanabriaОценок пока нет
- Treatment of Distal Calvicula FractureДокумент3 страницыTreatment of Distal Calvicula FractureiglesiasowenОценок пока нет
- Kaufmann 2016 Good Study Bad TimingДокумент3 страницыKaufmann 2016 Good Study Bad TimingCamilo SotomayorОценок пока нет
- Pediatric Spinal Schwannoma Case ReportДокумент17 страницPediatric Spinal Schwannoma Case ReportrakeОценок пока нет
- Gotto 2010Документ3 страницыGotto 2010Wirda Elya SariОценок пока нет
- Metastatic Squamous Cell Carcinoma of The ButtockДокумент3 страницыMetastatic Squamous Cell Carcinoma of The ButtockApple StarОценок пока нет
- A Case of Malignant Pleural Mesothelioma With Metastasis To The OrbitДокумент3 страницыA Case of Malignant Pleural Mesothelioma With Metastasis To The OrbitjamesyuОценок пока нет
- Thyroid Nodules With U ClassificationДокумент73 страницыThyroid Nodules With U ClassificationalenОценок пока нет
- Cytologic Findings of Proliferating Trichilemmal Tumor (PTT) of ScalpДокумент4 страницыCytologic Findings of Proliferating Trichilemmal Tumor (PTT) of Scalpma hОценок пока нет
- Radio Logical Diagnosis of Horn CancerДокумент2 страницыRadio Logical Diagnosis of Horn CancereditorveterinaryworldОценок пока нет
- Distinguishing Benign Notochordal Cell Tumors From Vertebral ChordomaДокумент9 страницDistinguishing Benign Notochordal Cell Tumors From Vertebral ChordomaOM JHAОценок пока нет
- 1109 Case 2Документ4 страницы1109 Case 2willygopeОценок пока нет
- AJNR - Terminal Myelocystocele and SCT - A Comparison of Fetal Ultrasound Presentation & Perinatal RiskДокумент3 страницыAJNR - Terminal Myelocystocele and SCT - A Comparison of Fetal Ultrasound Presentation & Perinatal RiskManikandan PerumalОценок пока нет
- Nigerian Veterinary Journal: Mammary Gland Chondrosarcoma in A German Shepherd Bitch: A Case ReportДокумент4 страницыNigerian Veterinary Journal: Mammary Gland Chondrosarcoma in A German Shepherd Bitch: A Case ReportRichard AntiaОценок пока нет
- Decision Making for Thyroid Nodule Diagnosis and ManagementДокумент15 страницDecision Making for Thyroid Nodule Diagnosis and ManagementFadi Al HajjiОценок пока нет
- Thalmic GlomaДокумент2 страницыThalmic GlomaNazia BhatОценок пока нет
- S RL 31072018 Desmoplastic FibromaДокумент23 страницыS RL 31072018 Desmoplastic FibromaAnonymous bE4VegCcОценок пока нет
- Tumours: Xxi. of Bones and JointsДокумент18 страницTumours: Xxi. of Bones and JointsNeha PalsikarОценок пока нет
- Sonographic Diagnosis of Placental Teratoma: Case ReportДокумент4 страницыSonographic Diagnosis of Placental Teratoma: Case ReportDen JCОценок пока нет
- Weissferdt 2015Документ6 страницWeissferdt 2015gabrielnunesОценок пока нет
- Research PaperДокумент2 страницыResearch PaperMunazzah MehakОценок пока нет
- Nrneurol 2011 65Документ2 страницыNrneurol 2011 65lauravshОценок пока нет
- Mi TsuyamaДокумент8 страницMi TsuyamatnsourceОценок пока нет
- Mass-Like Extramedullary Hematopoiesis: Imaging Features: Scientific ArticleДокумент6 страницMass-Like Extramedullary Hematopoiesis: Imaging Features: Scientific ArticleVo VũОценок пока нет
- Understanding Giant Cell Tumour (OsteoclastomaДокумент22 страницыUnderstanding Giant Cell Tumour (OsteoclastomaHasyasya Furnita KosaziОценок пока нет
- ShearWave Elastography Thyroid NodulesДокумент8 страницShearWave Elastography Thyroid Nodulesinfo8089Оценок пока нет
- Condrodisplasia Tipo Telemark em Bovino MiniaturaДокумент6 страницCondrodisplasia Tipo Telemark em Bovino Miniaturaana lauraОценок пока нет
- 1009 Case 2Документ4 страницы1009 Case 2willygopeОценок пока нет
- Estudio de Medula Osea Por RMДокумент6 страницEstudio de Medula Osea Por RMAngie TapiaОценок пока нет
- Uterine Leiomyomas With An Apparently Normal Karyotype Comprise Minor Heteroploid Subpopulations Differently Represented in Vivo and in VitroДокумент9 страницUterine Leiomyomas With An Apparently Normal Karyotype Comprise Minor Heteroploid Subpopulations Differently Represented in Vivo and in VitroJORGE LUIS SANCHEZ CEDEÑOОценок пока нет
- Ameloblastoma 4Документ6 страницAmeloblastoma 4098 - SILVYARA AYU PRATIWIОценок пока нет
- Diffuse Idiopathic Skeletal Hyperostosis and Ossification of The Posterior Longitudinal Ligament in The Thoracic SpineДокумент4 страницыDiffuse Idiopathic Skeletal Hyperostosis and Ossification of The Posterior Longitudinal Ligament in The Thoracic Spinecanhtung1989Оценок пока нет
- Seminoma Metastático: Descripción Histomorfológica: Metastatic Seminoma: Histomorphologic DescriptionДокумент5 страницSeminoma Metastático: Descripción Histomorfológica: Metastatic Seminoma: Histomorphologic DescriptionEisson PitreОценок пока нет
- Classificação Kimura2012Документ10 страницClassificação Kimura2012Carlos AmaralОценок пока нет
- 2015 Plosone Ewsr1 Pbx3Документ9 страниц2015 Plosone Ewsr1 Pbx3Ioannis PanagopoulosОценок пока нет
- PIIS0022522319345404Документ9 страницPIIS0022522319345404andryzell1987Оценок пока нет
- Bladder-Washing CytologyДокумент2 страницыBladder-Washing CytologyAleksandar VučićОценок пока нет
- Skeletal Metastasis in Carcinoma Penis Case Report With Review of LiteratureДокумент3 страницыSkeletal Metastasis in Carcinoma Penis Case Report With Review of LiteratureNunuh SulaemanОценок пока нет
- Zoo Stu 2008 SEM2Документ15 страницZoo Stu 2008 SEM2李孟芳Оценок пока нет
- Osteosarcoma of The Jaw: Report of 3 Cases (Including The Rare Epithelioid Variant) With Review of LiteratureДокумент10 страницOsteosarcoma of The Jaw: Report of 3 Cases (Including The Rare Epithelioid Variant) With Review of LiteraturesTEVENОценок пока нет
- Facial Squamous Cell Carcinoma and Abdominal Peripheral Nerve Sheath Tumour WithДокумент6 страницFacial Squamous Cell Carcinoma and Abdominal Peripheral Nerve Sheath Tumour WithJoão Pedro PiccoloОценок пока нет
- Endometrial Polyps: MR Imaging Features: Acta Med. Okayama, Vol., No., PPДокумент11 страницEndometrial Polyps: MR Imaging Features: Acta Med. Okayama, Vol., No., PPapache_sp2208465Оценок пока нет
- Lobular Adenocarcinoma of Breast Metastatic To The Mandibular CondyleДокумент4 страницыLobular Adenocarcinoma of Breast Metastatic To The Mandibular CondyleBakka BettiОценок пока нет
- Specialized Craniofacial Anatomy of A Titanosaurian Embryo From ArgentinaДокумент19 страницSpecialized Craniofacial Anatomy of A Titanosaurian Embryo From ArgentinaJorge BarОценок пока нет
- Jurnal KPDДокумент31 страницаJurnal KPDFarah F SifakОценок пока нет
- 13-Case Report - Pindborg TumorДокумент2 страницы13-Case Report - Pindborg TumorRam MohanОценок пока нет
- 2019 Article 1119Документ7 страниц2019 Article 1119elvirОценок пока нет
- Desmoplastic Small Round Cell Tumor of The Kidney: A Case ReportДокумент9 страницDesmoplastic Small Round Cell Tumor of The Kidney: A Case ReportNehemias MD GuevaraОценок пока нет
- Anatomo-Radioimaging Correlation in Atypical Ewing SarcomaДокумент5 страницAnatomo-Radioimaging Correlation in Atypical Ewing SarcomaIoana PelinОценок пока нет
- Ewings Sarcoma - DescriptionДокумент3 страницыEwings Sarcoma - DescriptionDamodara KumaranОценок пока нет
- Gender-Related Differences in The Morphology of The Lacrimal GlandДокумент6 страницGender-Related Differences in The Morphology of The Lacrimal GlandpedrojakubiakОценок пока нет
- Parthenogenesis: Accident or New LineageДокумент4 страницыParthenogenesis: Accident or New LineageAfifah ShehreyaОценок пока нет
- X BibliДокумент7 страницX BibliBJ CarminatorОценок пока нет
- New Project 200109123824Документ1 страницаNew Project 200109123824Eduardo FerreiraОценок пока нет
- New Project 200109125946Документ1 страницаNew Project 200109125946Eduardo FerreiraОценок пока нет
- New Project 200109124015Документ1 страницаNew Project 200109124015Eduardo FerreiraОценок пока нет
- New Project 200107014440Документ1 страницаNew Project 200107014440Eduardo FerreiraОценок пока нет
- New Project 200107013618Документ1 страницаNew Project 200107013618Eduardo FerreiraОценок пока нет
- Language Phylogenies PDFДокумент11 страницLanguage Phylogenies PDFEduardo FerreiraОценок пока нет
- How To Write in Plain EnglishДокумент11 страницHow To Write in Plain EnglishEduardo FerreiraОценок пока нет
- Language, Culture and LearningДокумент22 страницыLanguage, Culture and LearningCao Thuy Hong100% (2)
- The 50 Most Common Phrasal Verbs B T Stoakley PDFДокумент6 страницThe 50 Most Common Phrasal Verbs B T Stoakley PDFJaime AntonioОценок пока нет
- The importance of learning English for communication and understanding other culturesДокумент0 страницThe importance of learning English for communication and understanding other culturesDanu Angga VebriyantoОценок пока нет
- Sunny Gavran PDFДокумент103 страницыSunny Gavran PDFwidieandriyaniОценок пока нет
- Aplastic Anemia InfoДокумент5 страницAplastic Anemia InfoSareno PJhēaОценок пока нет
- Applied Veterinary Gynaecology and Obste1 PDFДокумент377 страницApplied Veterinary Gynaecology and Obste1 PDFHamza AlviОценок пока нет
- BreastДокумент8 страницBreastNada MuchОценок пока нет
- Common Oral and Dental Manifestations of HIV InfectionДокумент7 страницCommon Oral and Dental Manifestations of HIV InfectionGhaniyyatul KhudriОценок пока нет
- My Courses: Dashboard RMC Cap 2 Prelim Medical Surgical Nursing 4 Post Test 2Документ9 страницMy Courses: Dashboard RMC Cap 2 Prelim Medical Surgical Nursing 4 Post Test 2Fraylle AbongОценок пока нет
- Science of The Total EnvironmentДокумент11 страницScience of The Total EnvironmentUsman AliОценок пока нет
- Msds Al2o3 PDFДокумент6 страницMsds Al2o3 PDFNazuah Ushwatun HassanahОценок пока нет
- Diagnostic Pediatric Hematopathology - 2011Документ588 страницDiagnostic Pediatric Hematopathology - 2011Omar SarvelОценок пока нет
- Nutrition During The Life CycleДокумент335 страницNutrition During The Life Cycleapi-19916399100% (2)
- 5-Aminolevulinic Acid Photodynamic Therapy For Condyloma Acuminatum of Urethral MeatusДокумент19 страниц5-Aminolevulinic Acid Photodynamic Therapy For Condyloma Acuminatum of Urethral MeatusRiefka Ananda ZulfaОценок пока нет
- Thrombo PhiliaДокумент226 страницThrombo PhiliawalkerbestОценок пока нет
- Colour BlindnessДокумент4 страницыColour BlindnessDanial HazimОценок пока нет
- Bladder Substitution and Urinary DiversionДокумент58 страницBladder Substitution and Urinary DiversionlifespotОценок пока нет
- RESEARCH PROPOSAL - 3 Nov 2013 PDFДокумент27 страницRESEARCH PROPOSAL - 3 Nov 2013 PDFWestley AbluyenОценок пока нет
- Taxotere Docetaxel 80 mg/4 ML Concentrate For Solution For InfusionДокумент52 страницыTaxotere Docetaxel 80 mg/4 ML Concentrate For Solution For InfusionArbiati Rahman100% (1)
- Tumor Marker Tests - CancerДокумент4 страницыTumor Marker Tests - CancerMonna Medani LysabellaОценок пока нет
- Kjjhhgfdsasdf HJKLKJHGFDSSDFG HJKLДокумент4 страницыKjjhhgfdsasdf HJKLKJHGFDSSDFG HJKLbubble_inОценок пока нет
- Msds Control KimiaДокумент16 страницMsds Control KimiaEny Sucitrayati SucitrayatiОценок пока нет
- Kenya Medical Training College - Nyamira End of Year Three Semester One Examination March 2015 KRCHN Class (Pre-Service)Документ4 страницыKenya Medical Training College - Nyamira End of Year Three Semester One Examination March 2015 KRCHN Class (Pre-Service)Mursal RashidОценок пока нет
- Syllabus of KU MBBS PDFДокумент147 страницSyllabus of KU MBBS PDFAnshu Thapa69% (13)
- 2.High-Resolution CT of The Lung EDITIA A-3-A.Документ736 страниц2.High-Resolution CT of The Lung EDITIA A-3-A.RamonataleОценок пока нет
- MEDICINAL DIVERSITY AND ETHNOBOTANICAL USAGE OF ASTERACIOUS PLANTS OF GORAKHPUR DISTRICT, UTTAR PRADESH Srivastava C, Pande S* Department of Botany, Mahatma Gandhi P.G. College, Gorakhpur-273001, U.P., India Corresponding author: - Dr. Shail Pande, Associate Professor, Head, Dept. of Botany, Mahatma Gandhi P.G. College, Gorakhpur, U.P., India ABSTRACT The Asteraceae family is the largest family of flowering plants, with over 1600 genera and 23000 species are distributed throughout the world and occupy a wide range of habitat. In India, this family is represented by 900 species under 167 genera. Present study deals with an account of 17 medicinally important species of Asteracious plants found within present political boundaries of Gorakhpur District. The study highlights the botanical names, common names, habit, flowering and fruiting period and medicinal uses of Asteracious plants. Some important medicinal plants of this family are Ageratum conyzoides, Blumea lacera, CalenДокумент8 страницMEDICINAL DIVERSITY AND ETHNOBOTANICAL USAGE OF ASTERACIOUS PLANTS OF GORAKHPUR DISTRICT, UTTAR PRADESH Srivastava C, Pande S* Department of Botany, Mahatma Gandhi P.G. College, Gorakhpur-273001, U.P., India Corresponding author: - Dr. Shail Pande, Associate Professor, Head, Dept. of Botany, Mahatma Gandhi P.G. College, Gorakhpur, U.P., India ABSTRACT The Asteraceae family is the largest family of flowering plants, with over 1600 genera and 23000 species are distributed throughout the world and occupy a wide range of habitat. In India, this family is represented by 900 species under 167 genera. Present study deals with an account of 17 medicinally important species of Asteracious plants found within present political boundaries of Gorakhpur District. The study highlights the botanical names, common names, habit, flowering and fruiting period and medicinal uses of Asteracious plants. Some important medicinal plants of this family are Ageratum conyzoides, Blumea lacera, CalenEarthjournal PublisherОценок пока нет
- Chemical Resistance Chart GlovesДокумент8 страницChemical Resistance Chart Glovesjitendertalwar1603Оценок пока нет
- Gastrointestinal Endoscopy Volume 71 Issue 7 2010 (Doi 10.1016/j.gie.2009.12.029) Lisette G. Capelle Annemarie C. de Vries Jelle Haringsma Fran - The Staging of Gastritis With The OLGA System by PDFДокумент9 страницGastrointestinal Endoscopy Volume 71 Issue 7 2010 (Doi 10.1016/j.gie.2009.12.029) Lisette G. Capelle Annemarie C. de Vries Jelle Haringsma Fran - The Staging of Gastritis With The OLGA System by PDFAleida VivalloОценок пока нет
- Gebhard Mathis - Chest Sonography-Springer (2022)Документ248 страницGebhard Mathis - Chest Sonography-Springer (2022)Juan Francisco Antonio VázquezОценок пока нет
- Dr. Nugroho Sigit SpRad PDFДокумент20 страницDr. Nugroho Sigit SpRad PDFMira HandayaniОценок пока нет
- Pattern of Occurrence of Severe Preeclampsia Among Pregnant Women in South-West Nigeria. - Stamped PDFДокумент6 страницPattern of Occurrence of Severe Preeclampsia Among Pregnant Women in South-West Nigeria. - Stamped PDFGiovanni AtaídeОценок пока нет
- ChoeДокумент116 страницChoeJihad AnadОценок пока нет
- Horace Joules: Early Life and EducationДокумент8 страницHorace Joules: Early Life and Educationadh30aОценок пока нет