Академический Документы
Профессиональный Документы
Культура Документы
cn08015 PDF
Загружено:
adhityasdewiОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
cn08015 PDF
Загружено:
adhityasdewiАвторское право:
Доступные форматы
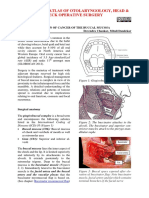
Original Cervical lymph node metastases of
Article
squamous cell carcinoma from an unknown
primary: Outcomes and patterns of failure
Mistry RC, Qureshi SS, Talole SD1, Deshmukh S
Departments of Head and Neck Services, 1Biostatistics, Tata Memorial Hospital, Ernest Borges Road,
Parel, Mumbai, India.
Correspondence to: Dr Rajesh Mistry, E-mail: musica@vsnl.com
Abstract
CONTEXT: Management of cervical lymph nodes metastases of squamous cell carcinoma (SCC) from primary of unknown
origin (PUO) is contentious and there is insignificant data from India on this subject. AIMS: To present experience of
management of these patients treated with curative intent at a single institution. SETTINGS AND DESIGN: Retrospective
study of patients treated between 1989-1994 in a tertiary referral cancer centre. MATERIALS AND METHODS: Eighty-nine
patients were evaluated in the study period and their survival compared with patients with common sites of primary in the
head and neck with comparable node stage. STATISTICAL ANALYSIS USED: Kaplan-Meier method. RESULTS: The
clinical stage of the neck nodes at presentation was N1 in 11%, N2a in 28.5%, N2b in 22.5%, N3 in 35% and Nx in 3.4%
patients. All patients underwent surgery and 70 patients received more than 40Gy postoperative radiotherapy. Twenty-
nine (32.6%) patients had relapse of which 19 (21%) were in the neck. Postoperative radiotherapy did not influence the
neck relapse (p=0.72). Primary was detected in 13 patients (14.6%) on subsequent follow up. The overall five and eight-
years survival was 55% and 51% respectively. The overall five-year survival was better compared to patients with known
primary with comparable node stage. CONCLUSIONS: Patients with cervical lymph nodes metastases of SCC from PUO
have reasonable survival and low rate of development of subsequent primary when treated with surgery and radiotherapy.
The overall survival is comparable to that of patients with known primary and hence an attempt at cure should always be
made.
Key words: Cervical metastases, head and neck, squamous cell carcinoma, unknown primary.
Introduction randomized studies involving patients managed with
various diagnostic and therapeutic procedures and
Metastases of squamous cell carcinoma (SCC) to cervical institutional policies.[2,4,5,8,9] Although sufficient data exist
lymph nodes from primary of unknown origin (PUO) in the literature on the subject, reports from India are
represent 1% to 2% of head and neck cancers.[1-3] The deficient.[10]
explanations for this unusual form of presentation are of
speculative nature: spontaneous regression of the primary The paper presents the experience at the Tata Memorial
and inability to detect a small primary particularly Hospital with treatment of patients with SCC metastatic
in the nasopharynx, which is known to metastasize to cervical lymph nodes from PUO.
to nodes at an early stage. Unlike metastatic lymph
nodes from PUO at other body sites, the prognosis in Materials and Methods
metastatic cervical nodes is not discouraging. The five-
year overall survival rates range between 40% to 60% The study included 89 patients with metastases of SCC
in recent series.[3-7] However, the optimal management to cervical lymph nodes from PUO treated with curative
of these patients remains controversial. The lack of intent between 1989 to 1994. The study excluded
randomized studies comparing treatment options has patients who received palliative therapy because of
led to therapeutic decision based on retrospective non- advanced or comorbid disease, with histology other than
54 Indian Journal of Cancer | April–June 2008 | Volume 45 | Issue 2
Mistry RC, et al.: Cervical nodes metastases of unknown origin
SCC and distant metastases at the time of diagnosis. software. Survival was computed by the Kaplan-Meier
method and compared by log-rank testing.
The median age of patients was 55 years (range 28 to
84 years). There were 78 men and 11 women. Forty-six Results
patients had involvement of right sided cervical nodes
and 43 had left sided nodes. The frequency of metastatic In six (7%) patients none of the nodes were metastatic;
lymph nodes at various neck levels were as follows: level all of them had open biopsy before neck dissection. In
1, 9 patients (10%); level 2, 67 patients (75%); level 3, six (7%) patients nodes were involved at a single level
46 patients (51.7%); level 4, 12 patients (13.5%); level and in seven (8%) patients, nodes were involved at all
5, 1 patient (1%). All patients were staged according to levels in the neck [Table 1]. Details of the level at which
the 2002 American Joint Committee on Cancer (AJCC) nodes where involved is listed in Table 2. Extra nodal
system for nodal disease in the head and neck region.[11] disease was reported in 59(66%) patients.
The clinical stage of the neck at presentation was N1 in
10 patients (11%), N2a in 25 patients (28.5%), N2b Fifty-one patients were alive at the time of review.
in 20 patients (22.5%), N3 in 31 patients (35%) and Ten patients died due to recurrent disease, ten died
Nx in 3 patients (3.4%). The diagnosis of SCC in neck of subsequent primary, nine patients died of distant
nodes was confirmed by FNAC in 50 patients (56%) metastases, one patient had recurrent disease and distant
and by open biopsy performed elsewhere in 39 patients metastases and in eight patients the cause of death was
(44%). not known.
The provisional diagnosis of neck node metastases with The five and eight-year overall survival for all patients
unknown primary was made after a comprehensive was 55% and 51% respectively, with median survival
clinical examination of the upper aerodigestive tract of 98 months [Figure 1]. Patient with N1 neck stage
failed to detect a primary lesion. All patients underwent at presentation showed a trend towards better survival
chest X-ray, barium swallow, X-ray of the nasopharynx as compared to N2 and N3 together at 30 months
and paranasal sinuses. Computerized Tomography (CT) [Figure 2], although this was not statistically significant
was performed as a routine in the later years of the (P=0.16). Similarly extra nodal spread also showed a
study. Subsequently patients underwent a meticulous weak evidence of having an impact on survival (P=0.07).
examination under anesthesia with panendoscopy (direct However, postoperative radiotherapy, prior open biopsy
laryngoscopy, oesophagoscopy, nasopharyngoscopy and of the node and involvement of nodes at multiple levels
bronchoscopy) and palpation of nasopharynx and base in the neck did not have any impact on the survival.
of tongue. Random biopsies and washings for cytology
from tonsil, base of tongue and/or nasopharynx was not
Table 1: Number of histologically involved nodal
performed. If these investigations failed to reveal the
levels
primary tumor, diagnosis of cervical node metastases
Number of Levels Number of patients (%)
from PUO was established.
None 6(7)
All patients underwent neck dissection and were advised 1 6(7)
postoperative RT. Ten patients did not take RT and nine
2 15(17)
patients did not complete RT for various reasons. Thus
19 patients (21%) had none or less than 40 Gy and 3 42(47)
the remaining 70 patients (79%) had 40 Gy or more 4 13(15)
of postoperative RT. The RT portals were unilateral,
5 7(8)
bilateral or antero-posterior depending on the discretion
of the treating radiotherapist.
Table 2: Topographic distribution of metastatic
Patients were followed-up at regular interval; endoscopy lymph nodes
and/or imaging were performed if patient was Level Clinical (%) Pathological (%)
symptomatic or clinical examination raised suspicion of
I 9(10) 21(23.6)
primary. Follow-up were completed by letters, telephone
calls and home visits. II 67(75) 76(85.4)
III 46(51.7) 74(83)
The survival was measured from the date of diagnosis
IV 12(13.5) 59(66.3)
to the last day of follow-up or to death. The data was
analyzed using SPSS for windows version 11.5 statistical V 1(1) 16(18)
Indian Journal of Cancer | April–June 2008 | Volume 45 | Issue 2 55
Mistry RC, et al.: Cervical nodes metastases of unknown origin
1.0 1.0
.9 .9
.8 .8
.7
.7
N1
.6
.6
.5 N2 & N3
Cum Survival
.5
Cum Survival
.4
.4
.3
.3 0 12 24 36 48 60 72 84 96
0 12 24 36 48 60 72 84 96
Months
Months
Figure 2: Overall survival according to node stage at
Figure 1: Overall survival of 89 patients presentation
Twenty-nine patients (32.6%) had relapse of disease. The in this study underwent routine blind biopsies and yet
site of relapse was neck in 19 patients (21.3%), distant the rate of detection of primary on subsequent follow-
in nine (10%) patients and neck with distant failure in up was no higher than reported in the literature, thus
one patient. Four of the 19 patients (21%) who received questioning the role of these investigations in the work
less than 40 Gy postoperative RT and 15 of 60 (25%) up for PUO. Similar conclusion can be drawn for CT
patients who received more than 40 Gy of post-operative scan. In gastrointestinal cancers CT is considered to
RT developed a neck relapse (P=0.72). Only three of be less sensitive in identifying small peritoneal deposits
the 29 patient with relapse of disease were alive. and superficial liver metastases. Hence the importance
of laparoscopy, wherein there is direct visualization of
The primary was detected in 13 patients (14.6%) on the abdominal cavity is substantial.[16] Akin to this in
follow-up. Two of these patients received less than 40 cervical metastases from PUO, the primary, if there is
Gy and 11 had more than 40 Gy of RT. The mean time one, is likely to be small the best investigation would
to detection of the primary was 24 months. In two
patients, the primary was detected in less than a year
and could represent missed primaries. The commonest Table 3: Location of the primary (n=13)
site of the primary was oropharynx; none presented Site of primary Number of patients
with primary in nasopharynx [Table 3]. All, except three Nasopharynx Nil
with primary in hypopharynx, larynx and oral cavity,
Oropharynx 6
died of disease.
Pyriform sinus 2
The survival of patients with known primary site treated Larynx 2
in Tata Memorial Hospital is reported in the Hospital
Lung 2
Registry. [12] The five-year survival of patients with
common sites of primary in the head and neck area was Oral cavity 1
compared with the patients reported in this study. For
comparable node stage the overall survival was better
Table 4: Comparison of five-year survival of
for patients with unknown primary [Table 4].
patients with known and unknown primary*
Discussion Site of primary N0 N1 N2 N3
Tonsil 21 14 - 5.5
The diagnosis of cervical node metastases from PUO Oropharynx 24 4 14 6
is made after thorough assessment fails to reveal the
Pyriform sinus 30 17 8 4
presence of tumor in the upper aerodigestive tract. In
addition to the array of investigations, many reports Nasopharynx 25 21 29 19
have advocated tonsillectomy, blind biopsies and/or Unknown - 63 63 32
washings for cytology from nasopharynx, and base *Comparison based on survival of patients with known primary reported in
tongue.[1,13-15] However, none of the patients reported the Hospital Registry.[12], Figures are in percentage
56 Indian Journal of Cancer | April–June 2008 | Volume 45 | Issue 2
Mistry RC, et al.: Cervical nodes metastases of unknown origin
be thorough examination of all the mucosal areas in the whom primary was detected later did poorly as compared
upper aerodigestive tract rather than relying on CT scan to those who continued to be free of disease.[5,14]
which is not ideal for detecting small lesions.
Postoperative RT did not help in controlling the
Hence we believe that imaging of the neck, if disease in the neck for 21% patients who had less than
performed, should be to define the extent of nodal 40 Grays versus 25% in those who had 40 Grays or
disease and its resectability rather than search for a more of radiation (P=0.72). This is contrary to the
primary. However, Sinnathamby et al and other authors experience at the Memorial Sloan Kettering Hospital
recommend routine imaging so as to avoid missing an where postoperative radiation failed to influence the
occult primary and unnecessary radiation to mucosal overall survival but helped in improving the local
areas.[2] Lately newly introduced diagnostic methods control.[23] Iganej also described a similar experience
have also been endeavored. Fluorodeoxyglucose (FDG) with postoperative RT.[7]
positron emission tomography (PET) or single-photon-
emission computed tomography (SPECT) have been Numerous factors have been recognized influencing
utilized. However, limited data has suggested that they the overall survival including node stage, number of
are useful only in small subsets of patients. [1,14,15,17] histologically involved nodes, grading, presence of
Laser-induced fluorescence imaging, Epstein-Barr virus extra nodal disease and performance status.[1-4,24] In our
(EBV) evaluation in metastatic lymph nodes by in situ study presence of extra capsular disease had a minor
hybridization, Human papilloma virus (HPV) detection impact on survival and nodal stage at presentation
by polymerase chain reaction, microsatellite mutation showed a trend towards better survival although it did
analysis of metastatic nodal tissue and samples of normal not achieve statistical significance. None of the other
pharyngeal mucosa were also proposed.[18-21] factors studied (open node biopsy, presence of metastatic
nodes at multiple levels, tumor grade and postoperative
The management of patients with cervical metastases radiotherapy) had impact on the overall survival.
from PUO evokes considerable controversy and has
not been standardized. Nieder et al,[1] in their review The five-year survival of 55% is comparable to published
have suggested surgery alone in selected patients with results.[3,5,6,23-25] We compared the overall survival of these
N1 disease without extracapsular extension and with no patients with that of patients with known primary at
history of incisional or excisional biopsy based on their common sites in the head and neck region as reported
finding of an appearance rate of the primary tumor of in the hospital registry.[12] For comparable node stage,
25%, median nodal recurrence rate of 34% and overall patients with occult primary appear to fare better than
five-year survival rate of 66%. The application of RT patients with known primary [Table 5]. This observation
has ranged from RT alone to postoperative RT and the should be interpreted with caution as the comparison is
portals included spanned from ipsilateral neck nodes to with historical data. Jones et al, on similar comparison
bilateral neck nodes and the putative primary sites.[2-7,22] did not find any difference in the survival between the
There is evidence that patients receiving postoperative two groups.[26]
RT to bilateral neck nodes and potential primary sites
have higher reported control odds and survival rate than The limitation of this study is its retrospective nature.
patients receiving postoperative ipsilateral RT or RT However all the patients had similar histology and
alone.[5] Nevertheless, considering the lack of comparative treatment was uniform in all patients. Based on this,
studies, the optimal radiotherapy strategy remains to it appears that routine blind biopsies from upper
be delineated. Similarly, the role of chemotherapy in aerodigestive tract may not be necessary. Nodal stage
the management of PUO with cervical metastases is at presentation and extra capsular disease has a role in
also indistinct. In fact, in the review by Nieder et al,[1] outcome of these patients.
substantial data supporting the use of chemotherapy
was deficient. In conclusion, the optimal diagnostic and therapeutic
approach still eludes us. The first randomized trial
The incidence of subsequent primary in our series (15%) proposed by the European Organization for Research
is in agreement with incidence reported by other studies on Treatment of Cancer (EORTC), Radiation Therapy
where postoperative RT was routinely administered. Oncology Group (RTOG), and other cooperative groups
[1,4-7,22]
We did not include any patient with metastases from Australia, Canada, Denmark and Germany (study
of undifferentiated carcinoma in the study. This could 24001-22005) is ongoing.[1,14] The results of this trial
explain why none of the primary was found in the will help in expounding several questions regarding
nasopharynx. As reported in the literature, patients in passable management of cervical metastases from PUO.
Indian Journal of Cancer | April–June 2008 | Volume 45 | Issue 2 57
Mistry RC, et al.: Cervical nodes metastases of unknown origin
References 14. Jereczek-Fossa BA, Jassem J, Orecchia R. Cervical lymph node
metastases of squamous cell carcinoma from an unknown primary.
Cancer Treat Rev 2004;30:153-64.
1. Nieder C, Gregoire V, Ang KK. Cervical lymph node metastases from 15. Mendenhall WM, Mancuso AA, Amdur RJ, Stringer SP, Villaret
occult squamous cell carcinoma: Cut down a tree to get an apple? DB, Cassisi NJ. Squamous cell carcinoma metastatic to the neck
Int J Radiat Oncol Biol Phys 2001;50:727-33. from an unknown head and neck primary site. Am J Otolaryngol
2. Sinnathamby K, Peters LJ, Laidlaw C, Hughes PG. The occult head 2001;22:261-7.
and neck primary: To treat or not to treat? Clin Oncol (R Coll Radiol) 16. Weickert U, Jakobs R, Riemann JF. Diagnostic laparoscopy.
1997;9:322-9. Endoscopy 2005;37:33-7.
3. Grau C, Johansen LV, Jakobsen J, Geertsen P, Andersen E, Jensen BB. 17. Greven KM, Keyes JW Jr, Williams DW 3rd, McGuirt WF, Joyce WT 3rd.
Cervical lymph node metastases from unknown primary tumours. Occult primary tumors of the head and neck: Lack of benefit from
Results from a national survey by the Danish Society for Head and positron emission tomography imaging with 2-[F-18]fluoro-2-deoxy-
Neck Oncology. Radiother Oncol 2000;55:121-9. D-glucose. Cancer 1999;86:114-8.
4. Colletier PJ, Garden AS, Morrison WH, Goepfert H, Geara F, Ang KK. 18. Kulapaditharom B, Boonkitticharoen V, Kunachak S. Flourescence-
Postoperative radiation for squamous cell carcinoma metastatic to guided biopsy in the diagnosis of an unknown primary in patients
cervical lymph nodes from an unknown primary site: Outcomes and with metastatic cervical lymph nodes. Ann Otol Rhinol Laryngol
patterns of failure. Head Neck 1998;20:674-81. 1999;108:700-4.
5. Reddy SP, Marks JE. Metastatic carcinoma in the cervical lymph 19. Lee WY, Hsiao JR, Jin YT, Tsai ST. Epstein-Barr virus detection in
nodes from an unknown primary site: Results of bilateral neck plus neck metastases by in-situ hybridization in fine needle aspiration
mucosal irradiation vs. ipsilateral neck irradiation. Int J Radiat Oncol cytologic studies: An aid differentiating the primary site. Head Neck
Biol Phys 1997;37:797-802. 2000;22:336-40.
6. Erkal HS, Mendenhall WM, Amdur RJ, Villaret DB, Stringer SP. 20. Gillison ML, Koch WM, Capone RB, Spafford M, Westra WH,
Squamous cell carcinomas metastatic to cervical lymph nodes from Wu L, et al. Evidence for a causal association between human
an unknown head-and-neck mucosal site treated with radiation papillomavirus and a subset of head and neck cancers. J Natl Cancer
therapy alone or in combination with neck dissection. Int J Radiat Inst 2000;92:709-20.
Oncol Biol Phys 2001;50:55-63. 21. Califano J, Westra WH, Koch W, Meininger G, Reed A, Yip L, et
7. Iganej S, Kagan R, Anderson P, Rao A, Tome M, Wang R, et al. al. Unknown primary head and neck squamous cell carcinoma:
Metastatic squamous cell carcinoma of the neck from an unknown molecular identification of the site of origin. J Natl Cancer Inst
primary: Management options and patterns of relapse. Head Neck 1999;91:599-604.
2002;24:236-46. 22. Strojan P, Anicin A. Combined surgery and postoperative
8. Tong CC, Luk MY, Chow SM, Ngan KC, Lau WH. Cervical nodal radiotherapy for cervical lymph node metastases from an unknown
metastases from occult primary: Undifferentiated carcinoma versus primary tumour. Radiother Oncol 1998;49:33-40.
squamous cell carcinoma. Head Neck 2002;24:361-9. 23. Davidson BJ, Spiro RH, Patel S, Patel K, Shah JP. Cervical metastases
9. McMahon J, Hruby G, O’Brien CJ, McNeil EB, Bagia JS, Clifford AR, et of occult origin: The impact of combined modality therapy. Am J
al. Neck dissection and ipsilateral radiotherapy in the management Surg 1994;168:395-9.
of cervical metastatic carcinoma from an unknown primary. Aust N 24. Fernandez JA, Suarez C, Martinez JA, Llorente JL, Rodrigo JP,
Z J Surg 2000;70:263-8. Alvarez JC. Metastatic squamous cell carcinoma in cervical lymph
10. Shenoy AM, Hasan S, Nayak U, Anantha N, Reddy BK, Kannan V, et nodes from an unknown primary tumour: prognostic factors. Clin
al. Neck metastasis from an occult primary--the Kidwai experience. Otolaryngol Allied Sci 1998;23:158-63.
Indian J Cancer 1992;29:203-9. 25. Weir L, Keane T, Cummings B, Goodman P, O’Sullivan B, Payne D, et
11. American Joint Committee on Cancer. In: Greene FL, Page DL, al. Radiation treatment of cervical lymph node metastases from an
Fleming ID, Fritz AG, Balch CM, Haller DG, et al, editors. American unknown primary: An analysis of outcome by treatment volume and
Joint Committee on Cancer Staging Manual. Head and Neck sites. other prognostic factors. Radiother Oncol 1995;35:206-11.
6th ed. New York: Springer-Verlag; 2002. p. 17-22. 26. Jones AS, Cook JA, Phillips DE, Roland NR. Squamous carcinoma
12. Dinshaw KA, Rao DN, Shroff PD. Annual Report 1987, Hospital presenting as an enlarged cervical lymph node. Cancer
Cancer Registry. Mumbai: Tata Memorial Hospital; 1989. 1993;27:1756-61.
13. Lapeyre M, Malissard L, Peiffert D, Hoffstetter S, Toussaint B,
Renier S, et al. Cervical lymph node metastasis from an unknown
primary: Is a tonsillectomy necessary? Int J Radiat Oncol Biol Phys
Source of Support: Nil, Conflict of Interest: None declared.
1997;39:291-6.
58 Indian Journal of Cancer | April–June 2008 | Volume 45 | Issue 2
Вам также может понравиться
- Incidence of Small Lymph Node Metastases in Patients With Nasopharyngeal Carcinoma: Clinical Implications For Prognosis and TreatmentДокумент7 страницIncidence of Small Lymph Node Metastases in Patients With Nasopharyngeal Carcinoma: Clinical Implications For Prognosis and TreatmentAdelin Luthfiana FajrinОценок пока нет
- Bacciu 2013Документ10 страницBacciu 2013AshokОценок пока нет
- Metaplastic Breast Carcinoma: Case Series and Review of The LiteratureДокумент5 страницMetaplastic Breast Carcinoma: Case Series and Review of The LiteratureMariela Judith UgarteОценок пока нет
- P. Wang Et Al.2019Документ6 страницP. Wang Et Al.2019Mai M. AlshalОценок пока нет
- Rcsann 2016 0300Документ4 страницыRcsann 2016 0300Siti Ayu kamsiahОценок пока нет
- Magnetic Resonance Imaging For The Detection of Nasopharyngeal CarcinomaДокумент4 страницыMagnetic Resonance Imaging For The Detection of Nasopharyngeal CarcinomaFebri W FinisiaОценок пока нет
- Abdominoperineal Resection For Squamous Cell Anal Carcinoma: Survival and Risk Factors For RecurrenceДокумент8 страницAbdominoperineal Resection For Squamous Cell Anal Carcinoma: Survival and Risk Factors For RecurrenceWitrisyah PutriОценок пока нет
- Head and Neck Surgery: Pressure Ulcer Prevention Strategies in Prolonged SurgeryДокумент2 страницыHead and Neck Surgery: Pressure Ulcer Prevention Strategies in Prolonged SurgeryBenny KurniawanОценок пока нет
- 2012 - Yoon Et Al. - Contouring Guidelines of The Inguinal Lymph Nodes Using Lymphangiograms For The Delivery of Radiation Therapy in GastroДокумент1 страница2012 - Yoon Et Al. - Contouring Guidelines of The Inguinal Lymph Nodes Using Lymphangiograms For The Delivery of Radiation Therapy in GastroPoljarLijanОценок пока нет
- Nijhuis2000 Article Clinico-PathologicalDataAndProДокумент9 страницNijhuis2000 Article Clinico-PathologicalDataAndProAhmed AllamОценок пока нет
- Submandibular Salivary Gland Tumors: Clinical Course and Outcome of A 20-Year Multicenter StudyДокумент4 страницыSubmandibular Salivary Gland Tumors: Clinical Course and Outcome of A 20-Year Multicenter StudyDiornald MogiОценок пока нет
- Abdominoperineal Resection For Squamous Cell Anal Carcinoma: Survival and Risk Factors For RecurrenceДокумент8 страницAbdominoperineal Resection For Squamous Cell Anal Carcinoma: Survival and Risk Factors For RecurrenceWitrisyah PutriОценок пока нет
- Clinico-Radiological Co-Relation of Carcinoma Larynx and Hypopharynx: A Prospective StudyДокумент7 страницClinico-Radiological Co-Relation of Carcinoma Larynx and Hypopharynx: A Prospective StudyDede MarizalОценок пока нет
- Supraclavicular Lymph NodeДокумент14 страницSupraclavicular Lymph NodeNeva PadillaОценок пока нет
- Favorable Female NPCДокумент6 страницFavorable Female NPChi-lineОценок пока нет
- Cervical Metastasis From Squamous Cell Carcinoma of The Maxillary Alveolus and Hard PalateДокумент3 страницыCervical Metastasis From Squamous Cell Carcinoma of The Maxillary Alveolus and Hard PalateCarolina Silva LamusОценок пока нет
- 11 Preoperative - High - Neutrophil-Lymphocyte - Ratio - MayДокумент8 страниц11 Preoperative - High - Neutrophil-Lymphocyte - Ratio - MayBridia BogarОценок пока нет
- 1530 Jul 27Документ6 страниц1530 Jul 27kelvin amahОценок пока нет
- aijcr-2009-02-005Документ6 страницaijcr-2009-02-005Apps OmОценок пока нет
- ShearWave Elastography Thyroid NodulesДокумент8 страницShearWave Elastography Thyroid Nodulesinfo8089Оценок пока нет
- Prognostic Model For Survival of Local Recurrent Nasopharyngeal Carcinoma With Intensity-Modulated RadiotherapyДокумент7 страницPrognostic Model For Survival of Local Recurrent Nasopharyngeal Carcinoma With Intensity-Modulated Radiotherapypp kabsemarangОценок пока нет
- Clinical Significance of Micrometastases of SCCДокумент6 страницClinical Significance of Micrometastases of SCCporsanimedОценок пока нет
- 0959 80492995521 7Документ1 страница0959 80492995521 7Sayda DhaouadiОценок пока нет
- HN 04-2011 Sublingual Gland Tumors PDFДокумент6 страницHN 04-2011 Sublingual Gland Tumors PDFHafiz FatmarОценок пока нет
- 2017 Diagnostic Relevance of Metastatic Renal Cell Carcinoma in The Head and Neck An Evaluation of 22 Cases in 671 PatientsДокумент7 страниц2017 Diagnostic Relevance of Metastatic Renal Cell Carcinoma in The Head and Neck An Evaluation of 22 Cases in 671 PatientsAlfonsoSánchezОценок пока нет
- Australasian Journal of DermatologyДокумент6 страницAustralasian Journal of DermatologydentheloОценок пока нет
- Papillary Microcarcinoma of The Thyroid-Prognostic Significance of Lymph Node Metastasis and MultifocalityДокумент10 страницPapillary Microcarcinoma of The Thyroid-Prognostic Significance of Lymph Node Metastasis and MultifocalityAZ RPОценок пока нет
- Jurnal CNFДокумент36 страницJurnal CNFAndrianorMuhammadОценок пока нет
- Computed Tomography in Endometrial CarcinomaДокумент5 страницComputed Tomography in Endometrial CarcinomasuggaplumОценок пока нет
- Song 2017Документ8 страницSong 2017Patricia BezneaОценок пока нет
- Carsinoma NasopharyngealДокумент9 страницCarsinoma NasopharyngealRahma R SОценок пока нет
- Anticanres 14037Документ5 страницAnticanres 14037Shafa ShaviraОценок пока нет
- Lessismore:Minimally Invasiveandquality Surgicalmanagementof GynecologiccancerДокумент12 страницLessismore:Minimally Invasiveandquality Surgicalmanagementof GynecologiccancerNita AgarwalОценок пока нет
- SURGICAL ONCOLOGY AND RECONSTRUCTION FOR CARCINOMASДокумент12 страницSURGICAL ONCOLOGY AND RECONSTRUCTION FOR CARCINOMASGisela LalitaОценок пока нет
- Radiotherapy in Phyllodes Tumour: Abst TДокумент3 страницыRadiotherapy in Phyllodes Tumour: Abst TtaufikolingОценок пока нет
- Fine Needle Aspiration Cytology of Thyroid Nodule: Diagnostic Accuracy and PitfallsДокумент4 страницыFine Needle Aspiration Cytology of Thyroid Nodule: Diagnostic Accuracy and Pitfallssalma007Оценок пока нет
- Glandula SalivarДокумент8 страницGlandula SalivarporsanimedОценок пока нет
- Ou 2016Документ8 страницOu 2016tami widiatul azahraОценок пока нет
- ANZ Journal of Surgery - 2021 - Wong - Cancer in Thyroglossal Duct CystsДокумент6 страницANZ Journal of Surgery - 2021 - Wong - Cancer in Thyroglossal Duct CystsJamesLeeОценок пока нет
- Clinicopathological Predictors of Central Compartment Lymph Node Metastases in cN0 Papillary Thyroid CarcinomaДокумент11 страницClinicopathological Predictors of Central Compartment Lymph Node Metastases in cN0 Papillary Thyroid CarcinomaYacine Tarik AizelОценок пока нет
- Ying 2016Документ7 страницYing 2016karemiaОценок пока нет
- Cancer - 2004 - Li - Treatment Outcome and Pattern of Failure in 77 Patients With Sinonasal Natural Killer T Cell or T CellДокумент10 страницCancer - 2004 - Li - Treatment Outcome and Pattern of Failure in 77 Patients With Sinonasal Natural Killer T Cell or T Cell2512505993Оценок пока нет
- Ogi2019 9465375Документ6 страницOgi2019 9465375Novi HermanОценок пока нет
- Siddiqi 2017Документ6 страницSiddiqi 2017salman khanОценок пока нет
- Reports of Practical Oncology and Radiotherapy 1 8 (2 0 1 3) S186-S197Документ2 страницыReports of Practical Oncology and Radiotherapy 1 8 (2 0 1 3) S186-S197Elisa SalakayОценок пока нет
- Clinical Impact of External Radiotherapy in Non-Metastatic Esophageal Cancer According To Histopathological SubtypeДокумент12 страницClinical Impact of External Radiotherapy in Non-Metastatic Esophageal Cancer According To Histopathological SubtypesilviailieОценок пока нет
- Management of Neck Mets in HNNДокумент9 страницManagement of Neck Mets in HNNMuhammad Azeem KhanОценок пока нет
- Original ArticleДокумент9 страницOriginal ArticlePatricia BezneaОценок пока нет
- Predictive Value of Nodal Metastases On Local Recurrence in The Management of Differentiated Thyroid Cancer. Retrospective Clinical StudyДокумент6 страницPredictive Value of Nodal Metastases On Local Recurrence in The Management of Differentiated Thyroid Cancer. Retrospective Clinical StudyuqbaОценок пока нет
- Jurnal Radiologi 2Документ21 страницаJurnal Radiologi 2Adelya Dwi AsyifaОценок пока нет
- GovindMangal IntraduralДокумент7 страницGovindMangal IntraduralAnonymous R6ex8BM0Оценок пока нет
- International Journal of Radiation Oncology Biology Physics StudyДокумент1 страницаInternational Journal of Radiation Oncology Biology Physics StudyAstie NomleniОценок пока нет
- PIIS0022522319345404Документ9 страницPIIS0022522319345404andryzell1987Оценок пока нет
- Nasopharyngeal: Undifferentiated CarcinomaДокумент4 страницыNasopharyngeal: Undifferentiated CarcinomabayuОценок пока нет
- Martha 2017Документ9 страницMartha 2017DavorIvanićОценок пока нет
- J HPB 2016 02 489Документ2 страницыJ HPB 2016 02 489hud6427Оценок пока нет
- Kevin FinalДокумент20 страницKevin Finalapi-213055674Оценок пока нет
- The Role of Stereotactic Radiosurgery For Low-Grade AstrocytomasДокумент7 страницThe Role of Stereotactic Radiosurgery For Low-Grade AstrocytomasNadia HristovaОценок пока нет
- Outcomes of Recurrent cSCCAДокумент7 страницOutcomes of Recurrent cSCCAPrincess B. MaristelaОценок пока нет
- Atlas of Parathyroid Imaging and PathologyОт EverandAtlas of Parathyroid Imaging and PathologyAlexander L. ShifrinОценок пока нет
- Temporomandibular Joint DisordersДокумент46 страницTemporomandibular Joint DisordersTony LeeОценок пока нет
- A Comparison Between 2 Absorbable Hemostatic AgentДокумент5 страницA Comparison Between 2 Absorbable Hemostatic AgentadhityasdewiОценок пока нет
- ID Distribusi Keganasan Nasofaring BerdasarДокумент7 страницID Distribusi Keganasan Nasofaring BerdasaradhityasdewiОценок пока нет
- BookletДокумент6 страницBookletVania IkaОценок пока нет
- 329 Full PDFДокумент7 страниц329 Full PDFadhityasdewiОценок пока нет
- CAP Protocol-2016 Thyroid - HighlightedДокумент8 страницCAP Protocol-2016 Thyroid - Highlightedpath2016Оценок пока нет
- Untitled 1Документ17 страницUntitled 1Tiberiu CttОценок пока нет
- Definition of Lymph Node Groups Neck DissectonДокумент22 страницыDefinition of Lymph Node Groups Neck DissectonSundeep Sharma100% (3)
- Surgical Resection of Cancer of The Buccal MucosaДокумент21 страницаSurgical Resection of Cancer of The Buccal MucosapradeepОценок пока нет
- Commando Surgery PDFДокумент1 страницаCommando Surgery PDFOlga0% (1)
- Buccal Mucosa Cancer Final PDF 9.6.14 PDFДокумент36 страницBuccal Mucosa Cancer Final PDF 9.6.14 PDFTaufiqurrahman Abdul DjabbarОценок пока нет
- Papillary Thyroid CancerДокумент7 страницPapillary Thyroid CancerLalaine RomeroОценок пока нет
- TIROIDECTOMIIДокумент66 страницTIROIDECTOMIIThoreEОценок пока нет
- SEER Lymph Node FieldsДокумент9 страницSEER Lymph Node FieldsNetradeep Narayansa DagduОценок пока нет
- List of Surgeries: AbdomenДокумент35 страницList of Surgeries: AbdomenSaurav SaikiaОценок пока нет
- Neckdissections 130421031843 Phpapp02Документ62 страницыNeckdissections 130421031843 Phpapp02azizОценок пока нет
- Metastasis in Head and Neck Jochen A.werner, R. Kim DavisДокумент237 страницMetastasis in Head and Neck Jochen A.werner, R. Kim DavisChandramohan SettyОценок пока нет
- Tumors of The Head and NeckДокумент5 страницTumors of The Head and NeckMiguel CuevasОценок пока нет
- Radical Neck DissectionДокумент11 страницRadical Neck DissectionHendry Johannes100% (1)
- Pearls and Pitfalls in Head and Neck Surgery - Claudio CerneaДокумент225 страницPearls and Pitfalls in Head and Neck Surgery - Claudio CerneaAlvaro rivero calleОценок пока нет
- Lymph Node DissectionДокумент17 страницLymph Node Dissectionperdhana kusumaОценок пока нет
- Ooi 150050Документ7 страницOoi 150050MelaNia Elonk ZamroniОценок пока нет
- COSTAR Outlining GuidelinesДокумент33 страницыCOSTAR Outlining GuidelinesYizhouZhaoОценок пока нет
- Management of Patients With Oral and Esophageal Disorders PDFДокумент85 страницManagement of Patients With Oral and Esophageal Disorders PDFNixi Mbuthia100% (1)
- MBBS SEQ Surgery Questions and AnswersДокумент46 страницMBBS SEQ Surgery Questions and AnswersMuntaha Javed100% (3)
- Elective Neck Dissection in Tongue CancerДокумент6 страницElective Neck Dissection in Tongue CancerDiah HayustiningsihОценок пока нет
- Parotid MassДокумент9 страницParotid MassAndre Eka Putra PrakosaОценок пока нет
- Head and NeckДокумент21 страницаHead and NeckUday PrabhuОценок пока нет
- Cancer of Oral CavityДокумент27 страницCancer of Oral CavityMihai AlexandruОценок пока нет
- Neck Dissection PPs PresentationДокумент139 страницNeck Dissection PPs PresentationDrMohmd ZidaanОценок пока нет
- Carcinoma Buccal Mucosa: Dr. Abhilash G JR-3Документ47 страницCarcinoma Buccal Mucosa: Dr. Abhilash G JR-3LingeshОценок пока нет
- Head and Neck Cancer GuidelinesДокумент96 страницHead and Neck Cancer GuidelinesTri KurniawanОценок пока нет
- Neck DissectionДокумент51 страницаNeck DissectionRakshith12Оценок пока нет
- Examination Methods in Plastic Surgery PDFДокумент69 страницExamination Methods in Plastic Surgery PDFSanОценок пока нет
- Icd 9 10 THTДокумент34 страницыIcd 9 10 THTlistianiayuОценок пока нет