Академический Документы
Профессиональный Документы
Культура Документы
Tuberculous Meningitis - A Case Report
Загружено:
yayaОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Tuberculous Meningitis - A Case Report
Загружено:
yayaАвторское право:
Доступные форматы
PRZEGL EPIDEMIOL 2013; 67: 629 - 632 Problems of infections
Katarzyna Guziejko, Piotr Czupryna, Anna Moniuszko, Sambor Grygorczuk,
Maciej Kondrusik, Joanna Zajkowska, Sławomir Pancewicz
TUBERCULOUS MENINGITIS – A CASE REPORT
Department of Infectious Diseases and Neuroinfections
Medical University in Białymstok
ABSTRACT
In this paper we present a case of a 58 years old male with a rare form of extrapulmonary tuberculosis – tuber-
culous meningitis (TBM). Tuberculous meningitis is usually caused by hematogenous spread of Mycobacterium
from lungs. The TBM is a severe disease with high mortality. The symptoms usually increase gradually and in the
course of the disease 3 clinical stages (prodromal phase, phase of neurological symptoms and phase of paresis)
may be differentiated. Cerebrospinal fluid examination, chest x-ray and sputum culture are crucial for diagnosis
of TBM. The proper diagnosis and early causative treatment significantly improve the outcome of the disease.
Key words: extrapulmonary tuberculosis, tuberculous meningitis
In Poland for many years there has been a steady (usually oculomotor) and meningeal signs.
decline in tuberculosis incidence, this is among many III. Paralysis with concomitant coma, increase in intra-
reasons mainly due to improved life conditions of Polish cranial pressure, and subsequent increase in intra-
population such as better nutrition, higher standards of cranial fluid space.
sanitation, as well as effective chemotherapy and tuber- Not typical clinical course with slowly increasing
culosis eradication programs (1). In 2009 the incidence symptoms and often mildly expressed meningeal signs,
rate of all forms of TB amounted to 21.6 per 100,000 contributes to late diagnosis, and delayed implementa-
inhabitants, which rates Poland in a group of European tion of a specific treatment, which significantly worsens
countries with average TB incidence rate (2).In 2008 the prognosis. TBM, if left untreated usually leads to
TB mortality rate in Poland amounted to 2.1/100,000 death. Despite the availability of effective and specific
population (3). Although the extrapulmonary type of TB treatment, the outcome of the disese may be fatal, which
is rare (in 2009 incidence rate amounted to 1.5/100,000 is the consequence of late or unrecognised tuberculous
population) it must be taken into consideration during process.
differential diagnosis of disorders of other organs and We present a case study of a patient with miliary
systems (2). One type of extrapulmonary tuberculosis tuberculosis, as well as TBM, who was hospitalised in
characterised by severe course of the disease and high Department of Infectious Diseases and Neuroinfections
mortality is tuberculous meningitis (TBM). The disease of Medical University in Bialystok, and in whom the di-
develops as a consequence of mycobacterium blood agnosis of TB was given at a time of symptoms appear-
borne dissemination from TB primary focus most often ance suggesting central nervous system involvement.
localised in lungs. In approximately 40-50% of patients
with identified TBM chest x-ray shows miliary changes,
or old tuberculosis lesions (4,5). DESCRIPTION OF THE CASE
The development of the disease is insidious, fol-
lowing phases can be differentiated (6.7). A 58 year old patient (farmer) who for 6 months was
I. Prodromal symptoms such as malaise, mild fever, under care of Pulmonary clinic, because of persistent
loss of appetite, headache, which are not typical, and productive cough, loss of body weight (25kg) and weak-
their duration may extend to several weeks. ness, was admitted to the Department of Infectious Dis-
II. Neurological symptoms which include lethargy, eases and Neuroinfections on the 1/09/11 with suspected
progressive cognitive disorders, cranial nerve palsy encephalitis. On an x-ray performed a month prior, there
© National Institute of Public Health – National Institute of Hygiene
630 Katarzyna Guziejko, Piotr Czupryna et al. No 4
Table I. Results of cerebrospinal fluid examination
Odczyn
Ocena Białko Albumina Odczyn Glukoza
Doba leczenia Cytoza (kom/ul) Nonne
makroskowpowa (mg/dl) (mg/dl) Pandyego (mg/dl)
Appelta
Wodojasny, 45 (Neutrofile-81;
2 79,9 47 + ++ 23
klarowny Limfocyty-9%)
Wodo jasny, 14 (Neutrofile-7%;
20 40 24,7 - + 53
klarowny Limfocyty-66%)
Wodo jasny,
60 11 31,2 18,3 - -/+ 46
klarowny
was visible presence of a shadow in left lung -apical were used (Mannitol 20%) and glucocorticosteroids
upper lobe (suspected TB). Between 31/08/- 1/09/11 the (Dextamethasone 16mg/daily in decreasing doses for
patient was hospitalised in an Internal Disease Unit at a the entire duration of hospitalisation). In 3 consecutive
District Hospital due to worsening headaches, especially induced sputum examinations, acid resistant bacilli was
in the parietal area, motor aphasia, and difficulty with present, additionally in culture system BacT/ALERT as
movement. Because of increasing cognitive decline, well as in LJ medium elevated level of mycobacteria
and the appearance of meningitis symptoms, on the was found. Furthermore csf (sample taken within the
second day of hospitalisation the patient was referred first 48 hours) of hospitalisation, bacteria culture after
to the Neurological admission room with suspected 38 days acid resistant mycobacteria grew. During the
hemorrhagic stroke. CT examination scan revealed only hospitalisation the patients’ neurological symptoms
widening of the ventricles. The patient was referred to improved. After 19 days of antituberculotic treatment
our Department with a suspicion of encephalitis. control csf examination indicated normalisation of
On admission the patient was conscious, with psy- CSF parameters (Tab.1.). Patient was discharged home
chomotor agitation, without logical contact and with after 23 days of hospitalisation in general good health
body temperature of 38.8˚C. On GCS he scored 10 with recommendation to continue treatment in a Lung
points. Physical examination revealed : neck stiffness Diseases and Tuberculosis Unit in the District Hospital.
4cm, positive bilateral Kerning’s sign, positive right side After 7 weeks and modification of treatment with
Oppenheim’s sign, dehydration, quiet vesicular sound, two drugs (Rifampicin with Isoniazid) the patient was
palpable left supraclavicular node, as well as inguinal admitted to our Department for a check-up. During
nodes and dental decay. Laboratory tests revealed el- the admission the patient presented in general good
evated inflammatory parameters (CRP- 35.9mg/l, ESR- health, without any abnormalities in physical examina-
58/70, WBC- 10k), mild hyponatraemia (131mmol/l). In tion. Chest x-ray revealed gradual remission of miliary
the next 24 hours lumbar puncture was performed. Ce- changes (Fig. 1). Patient was discharged home in general
rebrospinal fluid (CSF) examination revealed polinucle- good condition with recommendation to continue antitu-
ar pleocytosis, elevated protein concentration and low berculotic treatment (Rifamazid 300+150) in outpatient
glucose level (Tab.1.). Due to abnormalities observed on clinic and a follow up check-up in Lung Diseases and
the chest x-ray indicating miliary tuberculosis (Fig.1.) Tuberculosis Clinic in his place of residence.
antituberculotic treatment was commenced (Rifampi-
cin 600mg/d, Pyrazinamid 1500/d, Nidrazid 300mg/d,
Streptomicin 1.0/d). In addition antioedematous drugs DISCUSSION
TBM is a rare form of extrapulmonary tuberculosis
(2). The disease develops slowly, and is difficult to
diagnose, because it does not manifest itself initially
with characteristic symptoms. In the discussed study the
disease progressed in 3 typical for TBM phases (6, 7).
The condition of the patient deteriorated significantly
with the emergence of subsequent symptoms proving
the progression of the disease, and the prognosis for
total recovery, without significant neurological deficits
depended on the time of antituberculotic treatment
implementation.
In differential diagnosis different etiological factors
were taken into consideration, which could have caused
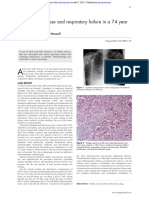
Fig. 1. Miliary tuberculosis tuberculous meningitis and encephalitis (viruses, bacte-
No 4 Tuberculous meningitis – a case report 631
results do not exclude TBM. Taking into account the
above mentioned factors, molecular tests should be
performed along with the traditional microbiological
studies (12, 13). Bacteriological infection confirmation
and thus defined time necessary to obtain tubercular my-
cobacteria growth, (depending on medium, sometimes
up to 2 months) should not delay appropriate therapy
if there is a clear clinical rationale suggestive of TBM.
Imagining tests (CT, MR) of CNS are helpful in as-
sessing the severity of the disease, and qualification of
the patients for life saving medical procedures (severe
hydrocephalus). In the course of TBM CT scan of the
head usually reveals in at least half of the patients widen-
Fig. 2. Miliary tuberculosis – partial regression of changes ing of ventricles, abnormalities on the base of the brain
and cerebral infarctions. Less frequently tuberculoma,
ria). CSF test plays a vital role in suspected tuberculosis or oedema of the brain are observed . MR of the head
etiology. CSF lymphocytosis, elevated concentration is more sensitive in imaging of CNS inflammation le-
of proteins, and reduced concentration of CSF glucose sions (meningeal enhancement) in the TBM compared
suggest diagnosis. In CSF examination at the beginning to CT scan (4, 14). In approximately 50% of patients
of the patients hospitalisation, in addition to typical with TB there are also tuberculous lesions in the lungs,
deviations in protein and glucose levels, polinuclear so x-ray of the chest as well as microbiological sputum
pleocytosis was found, which can occur in the initial test, remain an essential part in diagnostic process.
phase of the disease (10). Glucose concentration in CSF On a basic of the chest x-ray and patients history, it
(23mg/dl) fully met the criterion level of less than 60% was decided to commence specific therapy. The choice
of the concentration in the blood serum (94mg/dl). The of right combination of antituberculotic drugs as well
growth of Mycobacterium tuberculosis in culture of the time of TBM treatment, should cover intensive 4x drug
CSF sample is still the best standard in diagnosis of treatment (Isoniazid INH, Rifampicin RMP, Pyrzinamid
tuberculosis. Unfortunately, traditional microbiologi- PZA, and Streptomycin SM), which continuation will
cal tests have low sensitivity and long waiting period be two drug maintenance therapy (INH+RMP) for 12
for positive results, while new and faster molecular months. Administration of glucocorticoids (Dextameth-
tests (bacterial DNA amplification by PCR) remain asone) favourably influences revisable changes in CSF
expensive and inaccessible in routine hospital diagnosis. as well as greatly increases survival of patients. They
Although these tests have positive predictive value and should be administered sequentially over a period of 6-8
high specificity, their sensitivity in diagnosis of extra- weeks in decreasing doses. Glucocorticoid therapy has
pulmonary tuberculosis is hardly satisfactory. This is no effect on the incidence rate of late consequences of
most likely due to low concentration of mycobacteria neurological disorders (6, 15, 16, 17). On the third day of
in CSF, insufficient volume of test material (CSF), and the specific therapy one could observe overall improve-
the presence of inhibitory substances in the process of ment in a patient’s well being, as well as regression of
bacterial DNA amplification. Due to this, negative test neurological symptoms. Check-up examination on the
19th day of therapy showed tendency towards normalisa-
tion of parameters csf. After 2 months of treatment with
4 drugs (INH+RMP+PZA+SM), two drug therapy was
maintained (INH+RMP). Check-up chest x-rays showed
gradual remission of lung changes.
As previously mentioned, tuberculous meningitis
and encephalitis occur rarely, but it should be taken into
consideration in differential diagnosis of neuroinfection.
Early diagnosis and commencement of specific therapy
determines survival of the patient.
Fig. 3. Miliary tuberculosis – after 2 months of treatment
632 Katarzyna Guziejko, Piotr Czupryna et al. No 4
REFERENCES tuberculosis DNA in cerebrospinal fluid filtrates using
PCR. J Med Microbiol 2009;58:616-624.
12. Pai M, Ramsay A, O’Brien R Evidence-Based Tuber-
1. Korzeniewska-Koseła M. Gruźlica w Polsce – czyn-
culosis Diagnosis. PLoS Med 5(7): e156. doi:10.1371/
niki sukcesu leczenia. Pneumonol Alergol Pol
journal.pmed.
2007;75(supl.2):1-7.
13. Pai M, Flores LL, Pai N, et al. Diagnostic accuracy of
2. DOTS Expansion Plan to Stop TB in the WHO European
nucleic acid amplification tests for tuberculous meningi-
Region 2002–2006. World Health Organization. Regional
tis: a systematic review and meta-analysis. Lancet Infect
Office for Europe 2002.
Dis 2003;3(10):633-43.
3. Wojewódzka Stacja Sanitarno–Epidemiologiczna
14. Christensen ASH, Andersen AB, Thomsen V , et al. Tu-
w Poznaniu, http://wsse-poznan.pl/wp-content/up-
berculous meningitis in Denmark: a review of 50 cases.
loads/2011/05/zapadalnosc.pdf
BMC Infect Dis 2011; 11:47.
4. Chotmongkol V, Panthavasit J, Tiamkao S, et al. Tuber-
15. Slavin RE, Walsh TJ, Pollack AD. Late generalized
culous meningitis in adults: a four-year review during
tuberculosis: a clinical pathologic analysis and compari-
1997-2000. Southeast Asian J Trop Med Public Health
son of 100 cases in the preantibiotic and antibiotic eras.
2003;34(4):869-871.
Medicine (Baltimore) 1980;59(5):352-66.
5. Thwaites GE, Bang ND, Dung NH, et al.. Dexametha-
16. Thwaites G, Chau TTH, Mai NTH, et al. Tuberculous
sone for the Treatment of Tuberculous Meningitis in
meningitis. Neurol Neurosurg Psychiatry 2000;68:289-
Adolescents and Adults. N Engl J Med 2004;351:1741-
299.
1751.
17. Simmons CP, Thwaites GE, Quyen NT et al. The Clinical
6. Coyle PK. Glucocorticoids in central nervous system
Benefit of Adjunctive Dexamethasone in Tuberculous
bacterial infections. Arch Neurl 1999;56:796-801.
Meningitis Is Not Associated with Measurable Attenu-
7. Prusiński A. Neurologia praktyczna, Wyd.2 Warszawa :
ation of Peripheral or Local Immune Responses. J Im-
Wydaw Lek PZWL; 2001: 188-189.
munol 2005; 175:579-590.
8. Wojewódzka Stacja Sanitarno–Epidemiologiczna
w Poznaniu, http://wsse-poznan.pl/wp-content/up-
Received: 18.03.2013
loads/2011/05/plik.pdf
Accepted for publication: 18.04.2013
9. Hosoglu , Geyik MF, Balik I, et al. Predictiors of outcome
in patiens with tuberculous meningitis. Int J Tuberc Lung
Address for correspondence:
Dis 2002; 6:64-70.
Lek. Katarzyna Guziejko
10. Wojewódzka Stacja Sanitarno–Epidemiologiczna
Department of Infectious Diseases and Neuroinfections
w Poznaniu, http://wsse-poznan.pl/wp-content/up-
Medical University in Białystok
loads/2011/05/PlikLeczenie.pdf
14 Żurawia Str.15-540 Białystok
11. Haldar S, Sharma N, Gupta VK, et al. Efficient diagnosis
Tel. 85 74 -09- 514, fax 85 74-09-515
of tuberculous meningitis by detection of Mycobacterium
e-mail: kguziejko@wp.pl
Вам также может понравиться
- MEningitis TBДокумент4 страницыMEningitis TBAlexander TegarОценок пока нет
- Fulltext - Ams v5 Id1040Документ4 страницыFulltext - Ams v5 Id1040yaneemayОценок пока нет
- Outcomes of Tuberculous Meningitis in ChildrenДокумент31 страницаOutcomes of Tuberculous Meningitis in ChildrenDelphine DedelОценок пока нет
- Paraneoplastic Syndrome Mimicking Adult-Onset Still 'S Disease Caused by Advanced Lung Cancer: A Case ReportДокумент4 страницыParaneoplastic Syndrome Mimicking Adult-Onset Still 'S Disease Caused by Advanced Lung Cancer: A Case Reportoralposter PIPKRA2023Оценок пока нет
- AbscessДокумент12 страницAbscesslittlecandiesОценок пока нет
- Confirmed Tuberculous Brain Miliary in An Immunocompetent Patient: A Case ReportДокумент3 страницыConfirmed Tuberculous Brain Miliary in An Immunocompetent Patient: A Case ReportInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Seronegative Myasthenia Gravis Presenting With PneumoniaДокумент4 страницыSeronegative Myasthenia Gravis Presenting With PneumoniaJ. Ruben HermannОценок пока нет
- Wegener SДокумент7 страницWegener SJeffrey Ian M. KoОценок пока нет
- Journal of Medical Case ReportsДокумент5 страницJournal of Medical Case ReportsDumitru RadulescuОценок пока нет
- G G Scholar: Pubmed CentralДокумент6 страницG G Scholar: Pubmed CentralIkhsan FebriansyahОценок пока нет
- London F, Acta Neurol Belg, 2023Документ4 страницыLondon F, Acta Neurol Belg, 2023Fabrizio Quiñonez FlorentinОценок пока нет
- Acute Meningitis Complicated by Transverse Myelitis: Case ReportДокумент2 страницыAcute Meningitis Complicated by Transverse Myelitis: Case ReportSeptian TheaОценок пока нет
- Multiple Intracranial Tuberculomas: A Rare Case of CNS TBДокумент7 страницMultiple Intracranial Tuberculomas: A Rare Case of CNS TBrisna sariОценок пока нет
- Case Report Paracoccidioidomycosis in A Liver Transplant RecipientДокумент3 страницыCase Report Paracoccidioidomycosis in A Liver Transplant RecipientCarlos AlbertoОценок пока нет
- Disseminated Multifocal Tuberculosis An Unusual Presentation With Macrophagic Activation SyndromeДокумент5 страницDisseminated Multifocal Tuberculosis An Unusual Presentation With Macrophagic Activation SyndromeInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Tuberculous Meningitis in Adults: MRI Contribution To The Diagnosis in 29 PatientsДокумент6 страницTuberculous Meningitis in Adults: MRI Contribution To The Diagnosis in 29 PatientsyayaОценок пока нет
- Landouzy Septicemia (Sepsis Tuberculosa Acutissima) Due To Mycobacterium Microti in An Immunocompetent ManДокумент4 страницыLandouzy Septicemia (Sepsis Tuberculosa Acutissima) Due To Mycobacterium Microti in An Immunocompetent Manreadyboy89Оценок пока нет
- JurnalДокумент9 страницJurnalMelita Amalia AyubaОценок пока нет
- 72 - Progressive Multifocal Leukoencephalopathy in An Immunocompetent PatientДокумент7 страниц72 - Progressive Multifocal Leukoencephalopathy in An Immunocompetent PatientFaras ArinalОценок пока нет
- s12028 018 0538 4 PDFДокумент8 страницs12028 018 0538 4 PDFMaria ZeituneОценок пока нет
- Mediastinal Tuberculous Lymphadenitis Presenting With Insidious Back Pain in A Male Adult: A Case Report and Review of The LiteratureДокумент7 страницMediastinal Tuberculous Lymphadenitis Presenting With Insidious Back Pain in A Male Adult: A Case Report and Review of The Literaturez9tpwgb5nwОценок пока нет
- Final SCRUB TYPHUS AS DIFFERENTIAL DIAGNOSIS OF COVIDДокумент6 страницFinal SCRUB TYPHUS AS DIFFERENTIAL DIAGNOSIS OF COVIDDr Gaurav SinghОценок пока нет
- Supervisor: Dr. Dr. Noni N Soeroso, M.Ked (Paru), SP.P (K) Journal Reading Thursday, 24 January 2019Документ17 страницSupervisor: Dr. Dr. Noni N Soeroso, M.Ked (Paru), SP.P (K) Journal Reading Thursday, 24 January 2019Dewi SartikaОценок пока нет
- Tuberculous Meningitis With Initial Manifestation of Isolated Oculomotor Nerve PalsyДокумент3 страницыTuberculous Meningitis With Initial Manifestation of Isolated Oculomotor Nerve PalsyRakasiwi GalihОценок пока нет
- A Patient With Hypercoagulable State Due To TuberculosisДокумент4 страницыA Patient With Hypercoagulable State Due To TuberculosisAnnisa SufiОценок пока нет
- 2 - Adult Meningitis in A Setting of High HIV and TB Prevalence - Findings From 4961 Suspected Cases 2010 (Modelo para o Trabalho)Документ6 страниц2 - Adult Meningitis in A Setting of High HIV and TB Prevalence - Findings From 4961 Suspected Cases 2010 (Modelo para o Trabalho)SERGIO LOBATO FRANÇAОценок пока нет
- Pulmonary Miliary Tuberculosis Complicated With Tuberculous Spondylitis An Extraordinary Rare Association: A Case ReportДокумент5 страницPulmonary Miliary Tuberculosis Complicated With Tuberculous Spondylitis An Extraordinary Rare Association: A Case ReportIsmail Eko SaputraОценок пока нет
- Adult Still's Disease and Respiratory Failure in A 74 Year Old WomanДокумент3 страницыAdult Still's Disease and Respiratory Failure in A 74 Year Old WomanEduardo Romero StéfaniОценок пока нет
- Cardiac Leptospirosis: Iralphuaborque Md14thbatch Hds DocharlabardaДокумент15 страницCardiac Leptospirosis: Iralphuaborque Md14thbatch Hds DocharlabardaJr. CesingОценок пока нет
- Meningoencephalitis of Unknown Origin in Dogs CR - 881Документ6 страницMeningoencephalitis of Unknown Origin in Dogs CR - 881Ezequiel Davi Dos SantosОценок пока нет
- Diagnostic Challenge of Tuberculosis in Systemic Lupus ErythematosusДокумент9 страницDiagnostic Challenge of Tuberculosis in Systemic Lupus ErythematosusBelinda Putri agustiaОценок пока нет
- Recurrent MeningitisДокумент14 страницRecurrent Meningitisidno1008Оценок пока нет
- Case Report - Ikmalun NatiqДокумент16 страницCase Report - Ikmalun Natiqkelompok lawangОценок пока нет
- Disseminated Miliary Cerebral Candidiasis: Candida Albicans Is The Most Common Nos-C AlbicansДокумент4 страницыDisseminated Miliary Cerebral Candidiasis: Candida Albicans Is The Most Common Nos-C Albicansdrian pamungkasОценок пока нет
- Spontaneous Pneumomediastinum. Case ReportДокумент7 страницSpontaneous Pneumomediastinum. Case ReportSebastian Felipe Sierra UmañaОценок пока нет
- Jurnal AsliДокумент8 страницJurnal AsliDwi PurwantiОценок пока нет
- Importancia de Las Imágenes y El Diagnóstico Etiológico en El Paciente Inmunocomprometido Con Afección Del SNCДокумент9 страницImportancia de Las Imágenes y El Diagnóstico Etiológico en El Paciente Inmunocomprometido Con Afección Del SNCFranciely GarridoОценок пока нет
- Acta Med Iran 2013 51 2 113 118 PDFДокумент6 страницActa Med Iran 2013 51 2 113 118 PDFbreОценок пока нет
- Studi Kasus Pasien Dengan Meningitis Tuberkulosis Dalam Pengobatan Tuberkulosis ParuДокумент9 страницStudi Kasus Pasien Dengan Meningitis Tuberkulosis Dalam Pengobatan Tuberkulosis ParuYasintha NurainiОценок пока нет
- TB MeningitisДокумент17 страницTB MeningitisSylvan LaminaОценок пока нет
- Disseminated Tuberculosis in An AIDS/HIV-Infected Patient: AbstractДокумент3 страницыDisseminated Tuberculosis in An AIDS/HIV-Infected Patient: AbstractAmelia Fitria DewiОценок пока нет
- Review: Atypical Pathogen Infection in Community-Acquired PneumoniaДокумент7 страницReview: Atypical Pathogen Infection in Community-Acquired PneumoniaDebi SusantiОценок пока нет
- Cases Journal: Tuberculosis and Venous Thromboembolism: A Case SeriesДокумент4 страницыCases Journal: Tuberculosis and Venous Thromboembolism: A Case SeriesDiana Fadly MatondangОценок пока нет
- Para-Aortic and Meningitis Tuberculosis: A Case Report: BackgroundДокумент10 страницPara-Aortic and Meningitis Tuberculosis: A Case Report: BackgroundAseta MedikaОценок пока нет
- Tuberculous Transverse Myelitis: Case Report and Review of The LiteratureДокумент7 страницTuberculous Transverse Myelitis: Case Report and Review of The LiteraturenoraОценок пока нет
- Fungi52 52.9537Документ6 страницFungi52 52.9537Reza PutradinataОценок пока нет
- Tuberculous Meningoencephalitis: 2. Case Pre-SentationДокумент2 страницыTuberculous Meningoencephalitis: 2. Case Pre-SentationAnida HasnaОценок пока нет
- Case Report Paracoccidioidomycosis in A Liver Transplant RecipientДокумент6 страницCase Report Paracoccidioidomycosis in A Liver Transplant RecipientCarlos AlbertoОценок пока нет
- Chapter IIДокумент34 страницыChapter IINycoОценок пока нет
- Atypical Renal Presentation in Severe LeptospirosisДокумент3 страницыAtypical Renal Presentation in Severe LeptospirosisADIОценок пока нет
- Pulmonary Pseudotumoral Tuberculosis in An Old Man: A Rare PresentationДокумент3 страницыPulmonary Pseudotumoral Tuberculosis in An Old Man: A Rare PresentationNurhasanahОценок пока нет
- Paroxysmal Sympathetic Hyperactivity Syndrome in Tuberculous MeningitisДокумент5 страницParoxysmal Sympathetic Hyperactivity Syndrome in Tuberculous MeningitisBelinda Putri agustiaОценок пока нет
- Artigo de Revisão TuberculomaДокумент6 страницArtigo de Revisão TuberculomaOFF14Оценок пока нет
- Lee 2007Документ6 страницLee 2007Luis PerezОценок пока нет
- GM 04015Документ6 страницGM 04015Ikhsan FebriansyahОценок пока нет
- Small Lung CarcinomaДокумент4 страницыSmall Lung CarcinomaFawzia Haznah Nurul ImaniОценок пока нет
- DR Batum PDFДокумент5 страницDR Batum PDFdenisОценок пока нет
- Tuberculous Meningitis: Basal Cistern Enhancement Pattern On CT ImagingДокумент9 страницTuberculous Meningitis: Basal Cistern Enhancement Pattern On CT ImagingDeei RizalОценок пока нет
- 2020 Article 479Документ5 страниц2020 Article 479Anida HasnaОценок пока нет
- 594: Central Nervous System Infection. United States of America: Elsevier Science, 2004: 2039Документ3 страницы594: Central Nervous System Infection. United States of America: Elsevier Science, 2004: 2039yayaОценок пока нет
- Chapter 594: Central Nervous System Infection. United States of America: Elsevier ScienceДокумент3 страницыChapter 594: Central Nervous System Infection. United States of America: Elsevier ScienceyayaОценок пока нет
- Tropicalmed 04 00042 PDFДокумент20 страницTropicalmed 04 00042 PDFyayaОценок пока нет
- Activated CharcoalДокумент7 страницActivated CharcoalyayaОценок пока нет
- Tuberculous Meningitis in Adults: MRI Contribution To The Diagnosis in 29 PatientsДокумент6 страницTuberculous Meningitis in Adults: MRI Contribution To The Diagnosis in 29 PatientsyayaОценок пока нет
- Cerebral Dysgenesis: Child Neurology 2017 September 6, 2017Документ35 страницCerebral Dysgenesis: Child Neurology 2017 September 6, 2017yayaОценок пока нет
- Case 2 ThalasemiaДокумент74 страницыCase 2 ThalasemiayayaОценок пока нет
- Ratna Sitompul AHS UI 2017 AAHC RegionalДокумент68 страницRatna Sitompul AHS UI 2017 AAHC RegionalyayaОценок пока нет
- Prevalence and Causes of Congenital Microcephaly in The Absence of A Zika Virus Outbreak in Southern BrazilДокумент7 страницPrevalence and Causes of Congenital Microcephaly in The Absence of A Zika Virus Outbreak in Southern BrazilyayaОценок пока нет
- 10 Things You'Ll Relate To If You'Re An INFP - Psychology JunkieДокумент19 страниц10 Things You'Ll Relate To If You'Re An INFP - Psychology JunkieyayaОценок пока нет
- Jadwal UIM 2017 Term IДокумент52 страницыJadwal UIM 2017 Term IyayaОценок пока нет
- The Urgency of Redifining Minimum Monitoring Standards in AnesthesiaДокумент3 страницыThe Urgency of Redifining Minimum Monitoring Standards in AnesthesiayayaОценок пока нет
- Intestinal Obstruction: Etiology, Correlation Between Pre-Operative and Operative DiagnosisДокумент9 страницIntestinal Obstruction: Etiology, Correlation Between Pre-Operative and Operative DiagnosisyayaОценок пока нет
- Intestinal Obstruction: By: Dr. Wasfi M SalaytaДокумент16 страницIntestinal Obstruction: By: Dr. Wasfi M SalaytayayaОценок пока нет
- Algorithm For Management of Acute Pulmonary OedemaДокумент1 страницаAlgorithm For Management of Acute Pulmonary OedemayayaОценок пока нет
- Increases Plasma During Acute Cardiogenic Pulmonary: in Oncotic Pressure EdemaДокумент6 страницIncreases Plasma During Acute Cardiogenic Pulmonary: in Oncotic Pressure EdemayayaОценок пока нет
- Toxoplasmosis BrochureДокумент2 страницыToxoplasmosis Brochurethecatisgay100% (1)
- CombinepdfДокумент177 страницCombinepdfPrincess RonsableОценок пока нет
- Ganser SyndromeДокумент3 страницыGanser Syndromesomebody_maОценок пока нет
- Measles (Case Presentation)Документ19 страницMeasles (Case Presentation)Zam Pamate100% (3)
- 7 CRP Glycemic ControlДокумент5 страниц7 CRP Glycemic ControlBismha NayyerОценок пока нет
- Cherry Eye: Prolapse of Third Eyelid Gland in Dog-A Case ReportДокумент4 страницыCherry Eye: Prolapse of Third Eyelid Gland in Dog-A Case ReportRocioОценок пока нет
- RSSДокумент19 страницRSSUsamah El-habib100% (1)
- Adime For DiabetesДокумент2 страницыAdime For Diabetesapi-383891195Оценок пока нет
- Nursing Care Plan For Type1 DiabetesДокумент1 страницаNursing Care Plan For Type1 DiabetesBushra AlkhdourОценок пока нет
- Assignment 7 Seegundo IntentoДокумент7 страницAssignment 7 Seegundo IntentoYeimmy Julieth Cardenas Millan0% (1)
- Activities-Specific Balance Confidence (Abc) ScaleДокумент16 страницActivities-Specific Balance Confidence (Abc) ScaleMochammad Syarif HidayatОценок пока нет
- The Preparation of The True Sulphur of AntimonyДокумент20 страницThe Preparation of The True Sulphur of AntimonyAlex BellОценок пока нет
- Underground Clinical Vignettes - Pathophysiology I PDFДокумент124 страницыUnderground Clinical Vignettes - Pathophysiology I PDFtwinkle000100% (2)
- Ramadan and Diabetes MCB DiabetesUK LeafletДокумент4 страницыRamadan and Diabetes MCB DiabetesUK LeafletChris MulyoОценок пока нет
- NCPДокумент7 страницNCPJulianne Jeamer FabroaОценок пока нет
- BДокумент118 страницBbeautifulme031690Оценок пока нет
- TigecyclineДокумент2 страницыTigecyclineVanessa Egao100% (1)
- Case PresentationДокумент14 страницCase PresentationFatema RavatОценок пока нет
- Algoritma CKD PDFДокумент2 страницыAlgoritma CKD PDFDesla Citra100% (1)
- Harrisons Lecture Notes Part14 Section3Документ14 страницHarrisons Lecture Notes Part14 Section3Arash SamieiОценок пока нет
- Healing For All (Raymond T. Richey (Richey, Raymond T.) ) (Z-Library)Документ3 страницыHealing For All (Raymond T. Richey (Richey, Raymond T.) ) (Z-Library)Delcide Teixeira100% (1)
- Ndebreleasedquestions 2019 1 PDFДокумент383 страницыNdebreleasedquestions 2019 1 PDFManish JunejaОценок пока нет
- Name: Kelvin Martinez Background Information:: Part 1: PBS Nova-Making VaccinesДокумент3 страницыName: Kelvin Martinez Background Information:: Part 1: PBS Nova-Making VaccinesNoelОценок пока нет
- Paragraph DevelopmentДокумент7 страницParagraph DevelopmentJacqueline Gregorio RamosОценок пока нет
- Sexual HealthДокумент11 страницSexual Healthapi-236516264Оценок пока нет
- Cure For All DiseasesДокумент4 страницыCure For All DiseasesNiquezОценок пока нет
- Care Plan For Schizoaffective Disorder Bipolar TypeДокумент4 страницыCare Plan For Schizoaffective Disorder Bipolar TypeAlrick Asentista100% (2)
- Tugas Bahasa Inggris (Health)Документ17 страницTugas Bahasa Inggris (Health)Weni nuraeniОценок пока нет
- 2002 July Plab EmqДокумент12 страниц2002 July Plab EmqsunjaehОценок пока нет