Академический Документы
Профессиональный Документы
Культура Документы
Sialodenitis
Загружено:
Alex Av CarreraАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Sialodenitis
Загружено:
Alex Av CarreraАвторское право:
Доступные форматы
The Laryngoscope
C 2018 The American Laryngological,
V
Rhinological and Otological Society, Inc.
Case Report
Acute Sialadenitis Associated With 2017–2018 Influenza A Infection:
A Case Series
John A. Stafford, MD ; Charles A. Moore, MD; Jonathan R. Mark, MD
The influenza A virus has accounted for the majority of influenza infections in the 2017 to 2018 flu season, with the typical
clinical presentation including fever, myalgias, malaise, and nonproductive cough. Notably this season, we have recognized a
cluster of influenza A cases presenting as severe neck and facial swelling, with the subsequent diagnosis of sialadenitis.
Whereas previous authors have demonstrated isolated case reports of sialadenitis associated with influenza A infection,
herein we describe the clinical history, laboratory values, and radiographic findings of four patients presenting to our institu-
tion in January 2018 with acute sialadenitis and influenza A infection.
Key Words: Sialadenitis, influenza, submandibular, salivary glands, parotid.
Laryngoscope, 00:000–000, 2018
INTRODUCTION patient was diagnosed with acute upper respiratory
Each year, influenza outbreaks generate seasonal infection, sinusitis, and asthma exacerbation, for which
epidemics of acute viral respiratory illness resulting the patient received doxycycline, benzonatate, and pred-
from influenza A or B viral infection. The typical clinical nisone. The patient did not experience improvement in
presentation of flu includes fever, myalgias, headache, the symptoms and subsequently developed severely ten-
malaise, and accompanying upper respiratory infection der and enlarged bilateral submandibular glands with
symptoms such as cough, rhinorrhea, and sore throat.1 overlying erythema of the anterior neck. Clear saliva
In 2017, Fujiwara et al. published a case report of bilat- without purulence was expressed from bilateral subman-
eral submandibular sialadenitis following influenza A dibular and parotid glands.
infection, an association not previously described.2 Dur- The patient had the following relevant vital signs
ing a month in 2018, we recognized a series of four and laboratory results: temperature 36.7 8 C; white blood
patients presenting with significant sialadenitis follow- cell count (WBC) 12,100/mL; normal electrolytes; creati-
ing influenza A infection and here aim to present this nine 0.76 mg/dL; blood glucose 115 mg/dL; influenza A-
series in an effort to better describe this association. positive; and influenza B-negative. Computed tomogra-
phy scan demonstrated significant enlargement of the
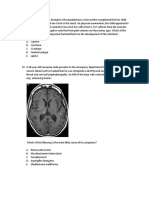
CASE REPORT bilateral submandibular glands with overlying cellulitis
and surrounding soft tissue inflammation (Fig. 1). While
Patient A in the ED, the patient received a one-time dose of ste-
A 50-year-old female with a past medical history of roids and was subsequently started on clindamycin due
asthma presented to the emergency department (ED) to a concern for deep neck space infection and also was
with a 2-day history of bilateral neck swelling, severe started on ceftriaxone and azithromycin due to a concern
neck pain, and cough. One week prior, the patient was for possible community-acquired pneumonia.
seen by the family physician for cough, headache, rhi- The patient continued the above-mentioned antibi-
norrhea, nasal congestion, and shortness of breath. The otics, along with adequate intravenous hydration, siala-
gogues, and massage of the submandibular glands. The
neck swelling significantly improved over the course of
From the Department of Otolaryngology–Head and Neck Surgery,
University of Cincinnati (J.A.S., C.A.M., J.R.M.), Cincinnati, Ohio, U.S.A. the next 24 hours, and the patient was discharged the
Editor’s Note: This Manuscript was accepted for publication on following day.
March 5, 2018.
The authors have no funding, financial relationships, or conflicts
of interest to disclose.
Send correspondence to Dr. Jonathan R. Mark, Assistant Profes- Patient B
sor, Otolaryngology–Head and Neck Surgery, University of Cincinnati
Medical Center, Department of Otolaryngology–Head and Neck Surgery,
A 47-year-old female with a past medical history of
University of Cincinnati College of Medicine, Medical Sciences Building type II diabetes and asthma presented to the ED with a
Room 6507, 231 Albert Sabin Way, Cincinnati, OH 45267-0528. E-mail: 2-day history of left-sided facial and neck swelling. One
jonathan.mark@uc.edu
week prior to presentation, the patient was hospitalized
DOI: 10.1002/lary.27202 elsewhere with fever, myalgias, and shortness of
Laryngoscope 00: Month 2018 Stafford et al.: Sialadenitis and Influenza A
1
5,200/mL; creatinine 1.03 mg/dL; mumps IgM-negative;
and blood glucose 92 mg/dL. Computed tomography
scan at that time demonstrated right parotid gland
hyperemia and inflammation. The patient received
intravenous fluids, pain medications, ondansetron, and a
prescription for prednisone.
On physical examination, the patient was noted to
have right-sided facial, parotid, and submandibular
swelling with clear saliva expressible from the salivary
ducts. The patient was instructed to continue the pre-
scribed course of prednisone, along with aggressive
hydration, parotid and submandibular massage, warm
compresses, and sialagogues.
Patient D
A 43-year-old female with hypothyroidism and
hypertension presented to an outside ED with bilateral
submandibular swelling and tenderness. The patient
had been diagnosed 5 days earlier with presumed bron-
chitis, for which the patient was subsequently treated
with a steroid taper and azithromycin. The patient com-
Fig. 1. Axial computed tomography neck with IV contrast demon- pleted both courses 1 day prior to secondary ED presen-
strating enlarged bilateral submandibular glands with inflammation
of the glands, thickening of the platysma, and fat-stranding of the tation. The patient reported new neck swelling that
overlying soft tissues correlated clinically with cellulitis. developed overnight and progressed to bilateral neck
pain and odynophagia with findings of significant bilat-
breath—and was found to be influenza A-positive and eral submandibular swelling, tenderness to palpation,
influenza B-negative. The patient was discharged after and overlying erythema of the anterior neck. Clear
receiving oseltamivir and encouraged to remain saliva was expressed from the patient’s salivary ducts.
hydrated. The patient subsequently developed painful The computed tomography (CT) scan demonstrated bilat-
left-sided facial and neck swelling worsening over 2 eral submandibular gland inflammation with overlying
days, prompting transfer to our institution for evalua- fat stranding and cellulitic changes. Pertinent laboratory
tion and management. findings included the following: temperature 37.4 8 C;
Computed tomography scan of the neck demonstrated WBC 5,400/mL; creatinine 0.69 mg/dL; normal electro-
inflammatory changes to the left submandibular and lytes; Monospot-negative; mumps IgM-negative; influ-
parotid glands with inflammation of the overlying soft tis- enza A-positive; and influenza B-negative.
sues of the neck. Pertinent laboratory findings included The patient received intravenous steroids;
the following: temperature 37.2 8 C; WBC 7,700/mL; normal amoxicillin-clavulanate; and conservative measures
electrolytes; blood glucose 120 mg/dL; and creatini- including use of sialagogues, salivary gland massage,
ne < 0.5 mg/dL. On examination, the patient was noted to and aggressive intravenous and oral hydration. The
have significant left-sided facial edema and erythema, patient was observed overnight and noted to signifi-
with an underlying firm, tender left submandibular gland. cantly improve prior to discharge.
Clear saliva was expressed from the salivary ducts.
The patient was treated with warm compress, DISCUSSION
hydration, sialagogues, gland massage, oral care, and During the 2014 to 2015 influenza season, the Cen-
clindamycin. After overnight observation in the ED, the ters for Disease Control and Prevention (CDC) report-
patient was discharged after improvement of symptoms edly received hundreds of confirmed influenza cases
and reduction in facial swelling and tenderness.
with associated parotitis, primarily occurring following
influenza A (H3N2) infection.3 Subsequent CDC influ-
Patient C enza reports have not carried similar advisories regard-
A previously healthy 20-year-old female presented ing parotitis and influenza. Our institution has
to an outside hospital ED with 3-day history of fever, recognized this recent cluster of sialadenitis cases follow-
cough, myalgias, and malaise. At that time, the patient ing influenza A infection. Notably, the CDC recently
was found to be influenza A-positive and influenza B- reported that 86.6% of documented influenza infections
negative and was discharged with instructions to remain this season have resulted from the influenza A virus,
hydrated. Two days later, the patient presented at our with 89.4% of those infection specifically resulting from
institution with complaints of right-sided face and neck the H3N2 strain.4 This series aims to highlight the asso-
swelling, as well as shortness of breath. ciation between sialadenitis and influenza A in the 2017
Pertinent laboratory results and vital signs at that to 2018 season in order to facilitate better recognition of
time include the following: temperatures 37.7 8 C; WBC such cases in the future.
Laryngoscope 00: Month 2018 Stafford et al.: Sialadenitis and Influenza A
2
The relationship between sialadenitis and influenza neck and/or facial swelling in the setting of previously
infection remains a poorly described clinical association. unrecognized Influenza A infection. This association has
Whereas the mumps virus is the classic viral cause of not been previously well characterized and represents
parotitis, the influenza virus has been recognized as a an atypical presentation for influenza A infection in the
rare cause of nonsuppurative parotitis.5 Within the pedi- 2017 to 2018 flu season. Earlier recognition of influenza
atric population, the H3N2 strain of influenza A has A infection in patients with sialadenitis this season may
been detected in the saliva of children with sialadenitis allow for reduced interpersonal spread of disease,
who were suspected to have mumps infection.6 Despite prompt initiation of treatment, and potential limitation
these associations, the majority of literature addressing of CT scans ordered for such patients.
sialadenitis in the setting of influenza A infection
remains limited to isolated case reports, such as those of
BIBLIOGRAPHY
Fujiwara et al. and Krilov et al.2,7
1. Nicholson KG. Clinical features of influenza. Semin Respir Infect 1992;7:
The cause of this association is unclear. Dehydra- 26–37.
tion secondary to preceding respiratory infection may 2. Fujiwara SA, Kobayashi T, Ikeda R, Yasuda K, Kubota I, Takeishi Y. Bilat-
predispose the patient to salivary stasis and subsequent eral submandibular sialadenitis following influenza A virus infection. ID
Cases 2017;10:49–50.
development of sialadenitis. Alternatively, the influenza 3. Centers for Disease Control and Prevention (CDC). 2016–2017 Influenza
A virus itself has been detected within the salivary Update for Health Care Providers: Parotitis and Influenza. Centers for
Disease Control and Prevention web site. Updated October 20 2016.
gland tissues after respiratory exposure in animal mod- Available at: https://www.cdc.gov/flu/about/season/health-care-providers-
els, supporting direct viral sialadenitis secondary to the parotitis.htm. Accessed January 29, 2018.
4. Centers for Disease Control and Prevention (CDC). 2017–2018 Influenza
influenza virus as a potential mechanism.8 Despite ini- Season Week 3 ending January 20, 2018. Centers for Disease Control
tially demonstrating evidence of severe neck swelling, and Prevention web site. Updated January 26, 2018. Available at:
patients within our series appear to respond to largely https://www.cdc.gov/flu/weekly/. Accessed January 29, 2018.
5. Al-dajani N, Wootton SH. Cervical lymphadenitis, suppurative parotitis,
supportive therapy, with the addition of steroids for thyroiditis, and infected cysts. Infect Dis Clin North Am 2007;21:523–
inflammation reduction and antibiotics for treatment of 541, viii.
6. Thompson CI, Ellis J, Galiano M, Ramsay M, Brown KE, Zambon M.
associated soft-tissue infections. Detection of influenza A(H3N2) virus in children with suspected mumps
during winter 2014/15 in England. Euro Surveill 2015;20. pii: 21203.
7. Krilov K, Swenson P. Acute parotitis associated with influenza A infection.
CONCLUSION J Infect Dis 1985;152:853.
8. Frankova V, Rychterova V. Inhalatory infection of mice with influenza A0/
This series demonstrates a cluster of cases of acute PR8 virus. II. Detection of the virus in the blood and extrapulmonary
nonsuppurative sialadenitis presenting as new-onset organs. Acta Virol 1975;19:35–40.
Laryngoscope 00: Month 2018 Stafford et al.: Sialadenitis and Influenza A
3
Вам также может понравиться
- Anatomy 2Документ5 страницAnatomy 2Balsam TeineОценок пока нет
- Fever in Patients with Acute Stroke: Aetiology and OutcomesДокумент7 страницFever in Patients with Acute Stroke: Aetiology and OutcomesRovanОценок пока нет
- First Case of Hemorrhagic Stroke from GBS MeningitisДокумент2 страницыFirst Case of Hemorrhagic Stroke from GBS MeningitisHelen EngelinaОценок пока нет
- 691-Article Text-2643-3-10-20200709Документ5 страниц691-Article Text-2643-3-10-20200709Sharan SahotaОценок пока нет
- Chapter 10Документ4 страницыChapter 10Srinu WestОценок пока нет
- 2002 1 200Документ23 страницы2002 1 200Dhrubashis KalitaОценок пока нет
- Caso Clinico NejДокумент9 страницCaso Clinico NejSilvina MartinezОценок пока нет
- Vitamin D Supplementation in COVID-19 Patients: A Clinical Case SeriesДокумент6 страницVitamin D Supplementation in COVID-19 Patients: A Clinical Case SeriesChairul LatiefОценок пока нет
- COVID-19 and Kawasaki Disease: Novel Virus and Novel CaseДокумент6 страницCOVID-19 and Kawasaki Disease: Novel Virus and Novel CaseCarlos Alberto Hernandez TorresОценок пока нет
- Pregnancy With Dengue Haemorrhagic Fever in Zainoel Abidin General Hospital Banda Aceh: A Case ReportДокумент5 страницPregnancy With Dengue Haemorrhagic Fever in Zainoel Abidin General Hospital Banda Aceh: A Case ReportfebyolandaОценок пока нет
- Case Report: Atypical Presentation of COVID-19 Leading To ARDSДокумент4 страницыCase Report: Atypical Presentation of COVID-19 Leading To ARDSEhab MardawiОценок пока нет
- 2021JULYДокумент25 страниц2021JULYNicole VinnikОценок пока нет
- Jurnal - Ayu AndiraДокумент11 страницJurnal - Ayu AndiraAriqa AzzhraОценок пока нет
- Case 25-2020: A 47-Year-Old Woman With A Lung Mass: Case Records Massachusetts General HospitalДокумент10 страницCase 25-2020: A 47-Year-Old Woman With A Lung Mass: Case Records Massachusetts General HospitalClinica CorominasОценок пока нет
- MicroДокумент11 страницMicroSuman MahmoodОценок пока нет
- A 9-Year-Old Boy With Severe Diphtherial Infection and Cardiac ComplicationsДокумент4 страницыA 9-Year-Old Boy With Severe Diphtherial Infection and Cardiac Complicationsummu yayaОценок пока нет
- Status of Sars-Cov-2 in Cerebrospinal Fluid of Patients With Covid-19 and StrokeДокумент3 страницыStatus of Sars-Cov-2 in Cerebrospinal Fluid of Patients With Covid-19 and StrokeSanjay KumarОценок пока нет
- Krok2 - Medicine - 2005Документ25 страницKrok2 - Medicine - 2005Badriya YussufОценок пока нет
- Krok2 - Medicine - 2005Документ25 страницKrok2 - Medicine - 2005gauravОценок пока нет
- Acute Respiratory Distress Syndrome During A PandeДокумент1 страницаAcute Respiratory Distress Syndrome During A PandeRaisa Mentari MoeisОценок пока нет
- Medical Microbiology & Parasitology Exam Past PapersДокумент11 страницMedical Microbiology & Parasitology Exam Past PapersThanatchawan Janwaro100% (1)
- JAssocChestPhysicians5287-8058932 222309Документ2 страницыJAssocChestPhysicians5287-8058932 222309AlexОценок пока нет
- Catheter-related fungal endocarditis in a hemodialysis patientДокумент3 страницыCatheter-related fungal endocarditis in a hemodialysis patientYohanna GomesОценок пока нет
- Late Presentation of Post Diphtheritic Myocarditis in A 15-Year MaleДокумент3 страницыLate Presentation of Post Diphtheritic Myocarditis in A 15-Year MaleFaqih Alam RuqmanaОценок пока нет
- COVID-19 Cytokine Storm Syndrome: Identification and TreatmentДокумент13 страницCOVID-19 Cytokine Storm Syndrome: Identification and TreatmentIoana PelinОценок пока нет
- E02T05V1Документ29 страницE02T05V1Ali ZeeshanОценок пока нет
- Krok2 - Medicine - 2013Документ28 страницKrok2 - Medicine - 2013ashighaОценок пока нет
- PTR 9999 0Документ7 страницPTR 9999 0Annie ShineОценок пока нет
- Early hydroxychloroquine and azithromycin therapy for COVID-19Документ8 страницEarly hydroxychloroquine and azithromycin therapy for COVID-19Tasya OktavianiОценок пока нет
- Methylene Blue For The Treatment-BMJ Case Rep-2022Документ4 страницыMethylene Blue For The Treatment-BMJ Case Rep-2022Lisandro IglesiasОценок пока нет
- Journal of Clinical and Translational Endocrinology: Case ReportsДокумент5 страницJournal of Clinical and Translational Endocrinology: Case ReportsKartikaa YantiiОценок пока нет
- Imaging Spectrum of Acute Invasive Fungal Rhino-Orbital-Cerebral Sinusitis in COVID-19 PatientsДокумент6 страницImaging Spectrum of Acute Invasive Fungal Rhino-Orbital-Cerebral Sinusitis in COVID-19 PatientsNurul Aisyah PaldarОценок пока нет
- A Case of Interstitial Pneumonia, Myocarditis Caused by C.pneumoniaeДокумент2 страницыA Case of Interstitial Pneumonia, Myocarditis Caused by C.pneumoniaeamyОценок пока нет
- Explore: Shuo-Wen Hung, Yuan-Ching Liao, I-Chang Chi, Ting-Yen Lin, Yu-Chuan Lin, Hung-Jen Lin, Sheng-Teng HuangДокумент6 страницExplore: Shuo-Wen Hung, Yuan-Ching Liao, I-Chang Chi, Ting-Yen Lin, Yu-Chuan Lin, Hung-Jen Lin, Sheng-Teng HuangJOHNОценок пока нет
- Infectious Disease Questions/Critical Care Board ReviewДокумент5 страницInfectious Disease Questions/Critical Care Board ReviewAzmachamberAzmacareОценок пока нет
- 513-Article Text-2205-1-10-20220330Документ8 страниц513-Article Text-2205-1-10-20220330kornelis aribowoОценок пока нет
- Case QuestionsДокумент4 страницыCase Questionsliza tilakdhariОценок пока нет
- Cotterman2009 PDFДокумент3 страницыCotterman2009 PDFAnonymous hxXpvZdZОценок пока нет
- Information MSQ KROK 2 Medicine 2007 2021 INFECTIOUS DISEASESДокумент39 страницInformation MSQ KROK 2 Medicine 2007 2021 INFECTIOUS DISEASESReshma Shaji PnsОценок пока нет
- Penggunaan Heparin Dosis Tinggi Pada Pasien COVID-19 Dengan ARDS Dan Hipertensi Di Unit Perawatan Intensif (ICU)Документ8 страницPenggunaan Heparin Dosis Tinggi Pada Pasien COVID-19 Dengan ARDS Dan Hipertensi Di Unit Perawatan Intensif (ICU)Vicky LumalessilОценок пока нет
- Acute Cardiac Failure Complicating A Case of SARS - COVID 19 in A 24-Year-Old PatientДокумент2 страницыAcute Cardiac Failure Complicating A Case of SARS - COVID 19 in A 24-Year-Old PatientMedtext PublicationsОценок пока нет
- G 3 NCM 122 Lab BSN 4 2 FinalДокумент67 страницG 3 NCM 122 Lab BSN 4 2 FinalPam RomeroОценок пока нет
- Nejmcpc 2027086Документ11 страницNejmcpc 2027086BÁCH NGUYỄN ĐẮCОценок пока нет
- A 66-Year-Old Man With Fever and ConfusionДокумент7 страницA 66-Year-Old Man With Fever and ConfusionEmmanuel HernandezОценок пока нет
- Adult Brain Hemorrhagic PRES Linked to COVIDДокумент4 страницыAdult Brain Hemorrhagic PRES Linked to COVIDAbdul AzeezОценок пока нет
- Jamadermatol 2020 0013Документ2 страницыJamadermatol 2020 0013Mostafa SalahОценок пока нет
- 319 YTPbpRДокумент10 страниц319 YTPbpRMateo MendozaОценок пока нет
- Amls Als Pretest Version 1.11Документ10 страницAmls Als Pretest Version 1.11Lancelot LeungОценок пока нет
- Case LogsДокумент4 страницыCase LogsDoaa HassanienОценок пока нет
- Sample Test Questions: Krok 2Документ29 страницSample Test Questions: Krok 2Daniel AshooriОценок пока нет
- Sample Test Questions: Krok 2Документ29 страницSample Test Questions: Krok 2Hisham aliОценок пока нет
- Valente Acosta2020Документ4 страницыValente Acosta2020Andres TameОценок пока нет
- A Case ofДокумент55 страницA Case ofYessaminОценок пока нет
- Rare Case of Bronchiolitis Obliterans in a 21-Month-OldДокумент3 страницыRare Case of Bronchiolitis Obliterans in a 21-Month-OldWelly ElvandariОценок пока нет
- Choose the Correct Diagnosis from Clinical FindingsДокумент29 страницChoose the Correct Diagnosis from Clinical Findingsanteneh67% (3)
- E92t15 2015EДокумент24 страницыE92t15 2015EDr-Mohammad AlfawazОценок пока нет
- Case 3Документ27 страницCase 3Eduard GarchitorenaОценок пока нет
- SARS CoV 2 and Influenza Virus Co Infection - 2020 - The LancetДокумент1 страницаSARS CoV 2 and Influenza Virus Co Infection - 2020 - The LancetMuhОценок пока нет
- 1 s2.0 S204908012200125X MainДокумент4 страницы1 s2.0 S204908012200125X MainAndreea CiorneaОценок пока нет
- Zakrzewska 2011Документ8 страницZakrzewska 2011Alex Av CarreraОценок пока нет
- 2D Betul Ur Rahman Sausan Al KawasДокумент6 страниц2D Betul Ur Rahman Sausan Al KawasAlex Av CarreraОценок пока нет
- Alex Carrera Enssay 1Документ1 страницаAlex Carrera Enssay 1Alex Av CarreraОценок пока нет
- Anatomical TermsДокумент12 страницAnatomical TermsAlex Av CarreraОценок пока нет
- Preboard Exam Np3 Medical Surgical NursingДокумент19 страницPreboard Exam Np3 Medical Surgical NursingDavid LopezОценок пока нет
- Dr. Noel Casumpang vs. Cortejo G.R. No. 171127, March 11, 2015Документ29 страницDr. Noel Casumpang vs. Cortejo G.R. No. 171127, March 11, 2015FD BalitaОценок пока нет
- Frequency, Severity, and Distress of Dialysis-Related Symptoms Reported by Patients On HemodialysisДокумент1 страницаFrequency, Severity, and Distress of Dialysis-Related Symptoms Reported by Patients On HemodialysisHelvia RahayuОценок пока нет
- Management of Hyperkalemia in The Acutely Ill Patient: Review Open AccessДокумент16 страницManagement of Hyperkalemia in The Acutely Ill Patient: Review Open AccessYesica Edith Aguilera ContrerasОценок пока нет
- Cleft Lip and Cleft PalateДокумент27 страницCleft Lip and Cleft Palatenamah odatОценок пока нет
- Aneroxia Research PaperДокумент34 страницыAneroxia Research PaperDuaa HammadОценок пока нет
- Association Between Mir Let-7g Gene Expression and The Risk of Cervical Cancer in Human Papilloma Virus-Infected PatientsДокумент8 страницAssociation Between Mir Let-7g Gene Expression and The Risk of Cervical Cancer in Human Papilloma Virus-Infected PatientsGICELAОценок пока нет
- DAFTAR PUSTAKA Serologi Dan ImunologiДокумент2 страницыDAFTAR PUSTAKA Serologi Dan ImunologiSari Anggun NОценок пока нет
- 9503 Duodenal AtresiaДокумент2 страницы9503 Duodenal Atresiamudasir61Оценок пока нет
- Ayurved TerminologiesДокумент30 страницAyurved TerminologiesVipul RaichuraОценок пока нет
- Free Journal List For PublicationДокумент11 страницFree Journal List For PublicationSyed Saad AliОценок пока нет
- Bill Receipt for Super Extn Health Male TestДокумент1 страницаBill Receipt for Super Extn Health Male TestSiddhant choudharyОценок пока нет
- Opsonin Pharma ListДокумент14 страницOpsonin Pharma ListDelegate Tech100% (1)
- The New Reconstructive Ladder - Modifications To The Traditional ModelДокумент8 страницThe New Reconstructive Ladder - Modifications To The Traditional ModelLovely PoppyОценок пока нет
- DNB QUESTION PAPER-Topic Wise (Author DR - Sirisha)Документ92 страницыDNB QUESTION PAPER-Topic Wise (Author DR - Sirisha)Sirisha CkvОценок пока нет
- Starting Injectable RCN PDFДокумент40 страницStarting Injectable RCN PDFPhilip HartleyОценок пока нет
- Arthrogryposis Multiplex Congenita (AMC) in Siblings - Case Report. First DCMS Annual Research Day, April 7, 2018Документ8 страницArthrogryposis Multiplex Congenita (AMC) in Siblings - Case Report. First DCMS Annual Research Day, April 7, 2018Razi MohdОценок пока нет
- Pediatric Anesthesiology PDFДокумент309 страницPediatric Anesthesiology PDFAviv Pasa100% (1)
- PVC Unido ConDuplicadosДокумент1 181 страницаPVC Unido ConDuplicadosJorge Chachaima MarОценок пока нет
- TTTTДокумент26 страницTTTTMoataz TrabehОценок пока нет
- Health DLP STAGES OF INFECTIONДокумент9 страницHealth DLP STAGES OF INFECTIONmarielabianaОценок пока нет
- PharmacovigilanceДокумент45 страницPharmacovigilancepavani valluriОценок пока нет
- Pe 1 Module 1Документ11 страницPe 1 Module 1Joanna Valerie A. IboñaОценок пока нет
- Staff Health PDFДокумент1 страницаStaff Health PDFJorgeОценок пока нет
- Daftar Obat Klinik MPHДокумент3 страницыDaftar Obat Klinik MPHxballzОценок пока нет
- Human Sexuality and Sexual DisordersДокумент42 страницыHuman Sexuality and Sexual DisordersAbdul Gafoor FahmyОценок пока нет
- Daftar PustakaДокумент3 страницыDaftar PustakamemeeeyyyОценок пока нет
- Anti-Allergy Drug GuidelinesДокумент8 страницAnti-Allergy Drug GuidelinesYojna PatilОценок пока нет
- 2015 Case Studies in Pain ManagementДокумент545 страниц2015 Case Studies in Pain ManagementJose Lavoisier moreiraОценок пока нет
- P.E. 1 Module 1 - First Semprelim-MidtermДокумент16 страницP.E. 1 Module 1 - First Semprelim-MidtermLalaine AdtoonОценок пока нет