Академический Документы
Профессиональный Документы
Культура Документы
Beta Code
Загружено:
Harold Christian GarridoАвторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Beta Code
Загружено:
Harold Christian GarridoАвторское право:
Доступные форматы
Antenatal Betamethasone Compared With
Dexamethasone (Betacode Trial)
A Randomized Controlled Trial
Andrew Elimian, MD, David Garry, DO, Reinaldo Figueroa, MD Alan Spitzer, MD,
Vandy Wiencek, RN, and J. Gerald Quirk, MD, PhD
OBJECTIVE: To compare betamethasone with dexa- orrhage was 11.3 % ( 95% CI 2.7–11.9%), and the number
methasone in terms of effectiveness in reducing perinatal needed to treat was 9 (95% CI 5–37) in favor of dexa-
morbidities and mortality among preterm infants. methasone.
METHODS: We enrolled 299 women at risk for preterm CONCLUSION: Betamethasone and dexamethasone are
delivery in a double-blind, placebo-controlled, random- comparable in reducing the rate of most major neonatal
ized trial of antenatal betamethasone compared with morbidities and mortality in preterm neonates. However,
dexamethasone at Stony Brook University Hospital from dexamethasone seems to be more effective in reducing
August 2002 through July 2004. We excluded women the rate of intraventricular hemorrhage compared with
with clinical chorioamnionitis, fetal structural and chro- betamethasone.
mosomal abnormalities, prior antenatal steroid exposure, CLINICAL TRIAL REGISTRATION: ClinicalTrials.gov,
and steroid use for other indications. Statistical analysis www.clinicaltrials.gov, NCT00418353
was performed in accordance of the intention-to-treat (Obstet Gynecol 2007;110:26–30)
principle. LEVEL OF EVIDENCE: I
RESULTS: There were no significant differences between
the groups with regard to baseline characteristics. The
rate of respiratory distress syndrome, need for vasopres-
sor therapy, necrotizing enterocolitis, retinopathy of pre-
maturity, patent ductus arteriosus, neonatal sepsis, and
A dministration of a single course of antenatal steroids
results in decrease in neonatal morbidity and mor-
tality as well as substantial savings in health care costs by
neonatal mortality were not significant different between specifically reducing the risk of respiratory distress syn-
the groups. However, the rates of intraventricular hem- drome, intraventricular hemorrhage, and neonatal
orrhage (6 of 105 [5.7%] compared with 17 of 100 [17.0%], death among premature infants.1–3 The preferred corti-
relative risk [RR] 2.97, 95% confidence interval [CI] 1.22– costeroids for antenatal therapy are betamethasone ad-
7.24, Pⴝ.02) and any brain lesion (7 of 105 [6.7%] com-
ministered intramuscularly as two doses of 12 mg each
pared with 18 of 100 [18.0%], RR 2.7, 95% CI 1.18 – 6.19,
24 hours apart or dexamethasone four doses of 6 mg
Pⴝ.02 ) were significantly lower in neonates exposed to
dexamethasone compared with betamethasone. The ab- given intramuscularly every 12 hours. These agents are
solute risk reduction in the rate of intraventricular hem- favored over other forms of steroids because they are the
most widely studied, seem to have identical biologic
activity, and readily cross the placenta. In addition, they
See related editorial on page 7.
are devoid of mineralocorticoid activity, have relatively
weak immunosuppressive actions, and have longer
From the Department of Obstetrics, Gynecology and Reproductive Medicine and
Department of Pediatrics, Stony Brook University, Stony Brook, New York. duration of action in comparison with cortisol and
Corresponding author: Andrew Elimian, MD, Section of Maternal Fetal methylprednisolone.4
Medicine, Department of Obstetrics and Gynecology, University of Oklahoma, However, there continue to be reports from uncon-
Health Sciences Center, WP 2450, Oklahoma City, OK 73190; e-mail: trolled studies of differences in effectiveness between
andrew-elimian@ouhsc.edu.
betamethasone and dexamethasone. A meta-
Financial Disclosure
The authors have no potential conflicts of interest to disclose.
analysis3showed that although the two agents reduce the
risks of respiratory distress syndrome and intraventricu-
© 2007 by The American College of Obstetricians and Gynecologists. Published
by Lippincott Williams & Wilkins. lar hemorrhage to a comparable extent, betamethasone
ISSN: 0029-7844/07 was more consistently associated with reduction in neo-
26 VOL. 110, NO. 1, JULY 2007 OBSTETRICS & GYNECOLOGY
natal death than dexamethasone. Furthermore a retro- the study. Those who elected to participate in the study
spective study5 found that betamethasone but not dexa- signed a formal consent form approved by our institu-
methasone was associated with a decreased risk of tion’s Committee on Research on Human Subjects.
periventricular leukomalacia, a major precursor of cere- Consenting women were randomly allocated to one
bral palsy. On the other hand, dexamethasone is sub- of two groups. The random allocation sequence was
stantially cheaper, more readily available and less likely carried out by the Pharmacy using computer-generated
to decrease fetal breathing movements and fetal heart random numbers, and each participant was assigned to
rate variability. In addition a recent retrospective one of two groups, ie, betamethasone or dexametha-
study6did not find any differences in effectiveness in the sone. One group received 12 mg of betamethasone
reduction of neonatal mortality and morbidity, includ- (Celestone Soluspan, Schering, Kenilworth, NJ) intra-
ing intraventricular hemorrhage and periventricular muscularly at 0 and 24 hours and similar-appearing
leukomalacia. placebo at 12 and 36 hours. The second group received
The choice of which of these agents to use is 6 mg of dexamethasone (dexamethasone sodium phos-
currently based on ease of administration, cost, availabil- phate, Baxter Healthcare Corporation Anesthesia and
ity, and results from conflicting observational studies. Critical Care, New Providence, NJ) intramuscularly at 0,
Our hypothesis was that there are no differences 12, 24, and 36 hours. Concealment was achieved by
between betamethasone and dexamethasone with re- delivering all doses in identical-looking syringes covered
gards to effectiveness when used in the clinical setting by opaque material. Both subjects and health care
of anticipated preterm delivery. Our objective was to providers were blinded as to the group to which partic-
compare betamethasone with dexamethasone in ipants belonged.
terms of effectiveness in reducing perinatal morbidi- After delivery, study personnel blinded to group
ties and mortality among preterm infants. assignment reviewed the prenatal, delivery, neonatal,
and postpartum records and documented maternal
MATERIALS AND METHODS and neonatal independent outcome variables. The
We conducted a randomized, double-blind, placebo- primary outcome variables were respiratory distress
controlled trial involving pregnant women at risk for syndrome, intraventricular hemorrhage, and neonatal
delivering preterm at Stony Brook University Hospital death. Secondary outcome variables included the
from August 1, 2002, through July 31, 2004. These need for exogenous surfactant, oxygen dependency at
included all women in preterm labor with intact mem- 28 days after birth or oxygen dependency at equiva-
branes, those with preterm premature rupture of mem- lent of 36 completed weeks gestational age, retinopa-
branes, and those anticipated to deliver for fetal and thy of prematurity, inotropic support for hypotension
maternal indications between 24 and 33 weeks 6 days initiated during the first 24 hours of life, treatment for
gestation. patent ductus arteriosus, necrotizing enterocolitis,
Preterm labor with intact membranes was diag- neonatal sepsis, and histologic chorioamnionitis.
nosed in the presence of six to eight contractions per Other variables recorded were maternal age, clinical
hour or four contractions in 20 minutes, associated diagnosis, gestational age at randomization and at
with cervical changes but with no prelabor rupture of delivery, gender, and birth weight.
membranes. Preterm PROM included cases in which Respiratory distress syndrome was diagnosed
delivery followed prelabor rupture of membranes, clinically, by the need for mechanical ventilation and
documented by pooling of fluid on sterile speculum oxygen for at least 48 hours, and the presence of
examination, ferning, and alkaline pH of fluid col- radiologic chest findings. Each neonate had transfon-
lected from the posterior vaginal fornix. Fetal and tanelle head ultrasound scans on days 3 and 7 of life.
maternal indications included mainly intrauterine Neurosonograms were evaluated by an experienced
growth restriction, preeclampsia, and chronic hyper- radiologist blinded to the antenatal steroid exposure
tension with superimposed preeclampsia. We ex- status of the parturient. Intraventricular hemorrhage
cluded women with clinical chorioamnionitis, known was graded as described by Papile et al7 Periventricu-
major fetal structural anomalies, known fetal chromo- lar leukomalacia was diagnosed by the presence of
somal abnormalities, prior antenatal steroid exposure, echolucent areas or persistent echogenicity in the
steroid use for other indications, and quadruplets, as periventricular areas on coronal and sagittal views.
well as women who declined enrollment. For study purposes, “any brain lesion” was defined as
Subjects meeting inclusion criteria were ap- any grade of intraventricular hemorrhage or periven-
proached by a resident or attending physician who tricular leukomalacia present exclusively or in com-
explained the study and sought consent to participate in bination.⬙ Necrotizing enterocolitis was diagnosed
VOL. 110, NO. 1, JULY 2007 Elimian et al The Betacode Trial 27
clinically and radiologically and confirmed at surgery
or autopsy. Proven neonatal sepsis included positive
blood, cerebrospinal fluid, or urine cultures.
Data analysis was performed in accordance of the
intention-to-treat principle. Sample size computations
for an equivalence study were performed according to
the work of Blackwelder.8 We assumed that approxi-
mately 80% of neonates exposed to either betametha-
sone or dexamethasone will not develop respiratory
distress syndrome. We also defined a deviation in
effectiveness of 10% or less as been essentially equiva-
lent. A sample size of 354 neonates (177 exposed to
betamethasone compared with 177 exposed to dexa-
methasone) would provide more than 80% power to
detect differences of more than 10% for a two-tailed test
of significance at a critical level of 0.05. The distribu-
tional characteristics of the variables were examined.
Continuous data were normally distributed. As such,
differences between groups defined by exposure to
antenatal steroids were examined using Student t test for
continuous variables and 2 for categorical variables.
Fisher exact test was used when expected cell frequency
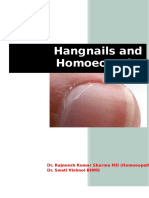
was equal to or less than five. A P value of ⬍.05 was Fig. 1. Betacode trial profile.
considered statistically significant. Elimian. The Betacode Trial. Obstet Gynecol 2007.
RESULTS
Five hundred forty-three women were screened for respiratory distress syndrome (73 of 181 [40.5%]
eligibility. One hundred sixty (29.5%) received compared with 79 of 178 [44.4%], P⫽.53), necrotizing
antenatal steroids before their transport and subse- enterocolitis (0 of 181 [0%] compared with 2 of 178
quently had completion of their course based on [1.1%], P⫽.25), retinopathy of prematurity (28 of 181
what was initiated in the transferring hospital. [15.5%] compared with 26 of 178 [14.6%], P⫽.92),
Fifty-five (10.1%) women declined participation patent ductus arteriosus (12 of 181 [6.7%] compared
and were given antenatal steroids based on the with 14 of 178 [7.9%], P⫽.81), neonatal sepsis (16 of
discretion of the treating physician and availability, 181 [8.9%] compared with 18 of 178 [10.1%], P⫽.83),
whereas 29 (5.3%) women could not be approached bronchopulmonary dysplasia (27 of 181 [15.0%] com-
because of immediate or imminent delivery. Thus, pared with 18 of 178 [10.1%], P⫽.22), need for
the study cohort consisted of 299 (55.1%) women vasopressor (14 of 181 [7.8%] compared with 6 of 178
and their 359 neonates. The profile of the study [3.4%], P⫽.07), and neonatal mortality (5 of 181
participants is shown in Figure 1. There were no [2.8%] compared with 6 of 178 [3.4%], P⫽.98) (Table
statistically significant differences between the 3). However, the rates of intraventricular hemorrhage
groups in terms of maternal age, race, body mass (6 of 105 [5.7%] compared with 17 of 100 [17.0%],
index, smoking status, gestational age at random- relative risk 2.97, 95% confidence interval [CI] 1.22–
ization, and diagnoses between women who partic- 7.24, P⫽.02) and any brain lesion (7 of 105 [6.7%]
ipated in the trial and those who did not participate. compared with 18 of 100 [18.0%], relative risk 2.7,
Similarly, the baseline characteristics of the women 95% CI 1.18 – 6.19, P⫽.02 ) were significantly lower in
and neonates randomly assigned to betamethasone neonates exposed to dexamethasone compared with
were not different from those that assigned to betamethasone (Table 3).
dexamethasone, as depicted in Tables 1 and 2. No The rate of grades III and IV intraventricular
adverse effect or side effects were reported in either hemorrhage was 7% (7 of 100) in neonates exposed to
group. betamethasone compared with 1.9% (2 of 105) in
There were no significant differences between neonates exposed to dexamethasone, P⫽.09 (Table
neonates exposed to betamethasone and those ex- 3). Furthermore, the rate of periventricular leukoma-
posed to dexamethasone with regard to the rates of lacia was 4.0% (4 of 100) in neonates exposed to
28 Elimian et al The Betacode Trial OBSTETRICS & GYNECOLOGY
Table 1. Baseline Characteristics of Mothers in the Betamethasone and Dexamethasone Groups
Maternal Characteristics Betamethasone (nⴝ150) Dexamethasone (nⴝ149) P
Maternal age (y) 30.6⫾6.1 29.9⫾6.2 .37
Race
White 105 (70.0) 105 (70.5) .97
African American 21 (14.0) 14 (9.4) .29
Hispanic 12 (8.0) 19 (12.7) .25
Other 12 (8.0) 11 (7.4) .99
GA presentation 29.3⫾2.9 29.5⫾2.9 .82
BMI 30.0⫾6.7 29.4⫾5.0 .41
Singleton gestation 124 (82.7) 125 (83.9) .90
Smoking 26 (17.3) 32 (21.5) .45
PTL 80 (53.3) 76 (51.0) .77
Preterm PROM 21 (14.0) 29 (19.5) .27
Medically indicated 49 (32.7) 44 (29.5) .64
HCA 27 (18.0) 30 (20.1) .75
GA, gestational age; BMI, body mass index; PTL, preterm labor; PROM, premature rupture of membranes; HCA, histologic chorioamnionitis.
Data are mean⫾standard deviation or n (%).
Table 2. Baseline Characteristics of Neonates in the Betamethasone and Dexamethasone Groups
Neonatal Characteristics Betamethasone (nⴝ181) Dexamethasone (nⴝ178) P
Mode of delivery .64
Vaginal 80 (44.2) 84 (47.2)
Cesarean 101 (55.8) 94 (52.8)
Sex .96
Male 90 (49.7) 89 (50)
Female 91 (50.3) 89 (50)
Birth weight 1983⫾814 2036⫾825 .56
Surfactant use 52 (28.7) 53 (29.8) .92
Data are mean⫾standard deviation or n (%).
Table 3. Neonatal Outcomes in the Betamethasone and Dexamethasone Groups
Outcome Betamethasone (nⴝ181) Dexamethasone (nⴝ178) RR 95% CI P
RDS 73 (40.5) 79 (44.4) 0.91 0.72–1.16 .53
IVH
Any grade 17/100 (17.0) 6/105 (5.7) 2.97 1.22–7.24 .02
Grade III/IV 7/100 (7.0) 2/105 (1.9) 3.67 0.78–17.27 .09
PVL 4/100 (4.0) 2/105 (1.9) 2.10 0.39–11.21 .44
Any brain lesion 18/100 (18) 7/105 (6.7) 2.7 1.18–6.19 .02
Neonatal death 5 (2.8) 6 (3.4) 0.82 0.26–2.65 .98
NEC 0 (0) 2 (1.1) 0.00 0.00–4.0 .25
ROP 28 (15.5) 26 (14.6) 1.06 0.65–1.74 .92
PDA 12 (6.7) 14 (7.9) 0.85 0.40–1.78 .81
Sepsis 16 (8.9) 18 (10.1) 0.88 0.46–1.67 .83
BPD 27 (15.0) 18 (10.1) 1.48 0.85–2.59 .22
Vasopressor use 14 (7.8) 6 (3.4) 2.31 0.91–5.87 .07
RR, relative risk; CI, confidence interval; RDS, respiratory distress syndrome; IVH, intraventricular hemorrhage; PVL, periventricular leukomalacia;
NEC, necrotizing enterocolitis; ROP, retinopathy of prematurity; PDA, patent ductus arteriosus; BPD, bronchopulmonary dysplasia.
Data are n (%) or n/N (%) unless otherwise specified.
betamethasone compared with 1.9% (2 of 105) in DISCUSSION
neonates exposed to dexamethasone, P⫽.44 (Table A single course of antenatal steroids before preterm
3). The absolute risk reduction in the rate of intraven- delivery results in a significant decrease in neonatal
tricular hemorrhage was 11.3% (95% CI 2.7–11.9%), morbidity and mortality as well as substantial savings in
and the number needed to treat was 9 (95% CI 5–37) health care costs. Betamethasone and dexamethasone
in favor of dexamethasone. continue to be the preferred steroids because of their
VOL. 110, NO. 1, JULY 2007 Elimian et al The Betacode Trial 29
unique biologic properties, ability to readily cross the we found dexamethasone to be superior to betametha-
placenta, and because of their weak immunosuppressive sone in reducing the rate of intraventricular hemor-
and mineralocorticoid activities. The choice between rhage. Other potential advantages of dexamethasone
betamethasone and dexamethasone is currently based include lower cost, widespread availability, and less
on ease of administration, cost, availability, and results effect on fetal biophysical variables that might lead to
from conflicting observational studies. premature intervention or delivery. On the other hand,
Our study found that both betamethasone and betamethasone requires two injections as opposed to the
dexamethasone are largely comparable in reducing four injections of dexamethasone.
most morbidities and mortality among preterm neo-
nates. This finding is consistent with the reports of Baud
REFERENCES
et al5 and Bar-lev and colleaques,6 who did not demon-
1. National Institutes of Health. Report of the Consensus Develop-
strate any differences in the rate of respiratory distress ment Conference on the Effect of Corticosteroids for Fetal
syndrome, bronchopulmonary dysplasia, intraventricu- Maturation on Perinatal Outcomes (NIH Publication No.
lar hemorrhage, neonatal mortality, and other compli- 95–3784). Bethesda (MD): National Institutes of Health, National
Institute of Child Health and Human Development; 1994
cations of prematurity among neonates exposed to
2. Liggins GC, Howie RN. A controlled trial of antepartum
betamethasone and dexamethasone. However, contrary glucocorticoid treatment for prevention of distress syndrome in
to the finding of a higher rate of periventricular leu- premature infants. Pediatrics 1972;50:515–25.
komalacia among neonates exposed to dexamethasone 3. Crowley PA. Antenatal corticosteroid therapy: a meta-analysis
compared with betamethasone reported by Baud et al,5 of the randomized trials, 1972 to 1994. Am J Obstet Gynecol
our study did not find any differences in the rate 1995;173:322–35.
periventricular leukomalacia between the groups. In 4. Ballard PL, Ballard RA. Scientific basis and therapeutic regi-
mens for use of antenatal glucocorticoids. Am J Obstet
fact, the rate of periventricular leukomalacia in the Gynecol 1995;173:254–62.
dexamethasone-exposed neonates was lower among 5. Baud O, Foix-L’Helias L, Kaminski M, Audibert F, Jarreau
neonates exposed to betamethasone, although our study PH, Papiernik E, et al Antenatal glucocorticoid treatment and
was underpowered to detect differences in periventricu- cystic periventricular leukomalacia in very premature infants.
N Engl J Med 1999;341:1190–6.
lar leukomalacia. Three other groups of investigators6,9,10
have reported no differences in the rates of periventricu- 6. Bar-Lev MR, Maayan-Metzger A, Matok I, Heyman Z, Sivan
E, Kuint J. Short-term outcomes in low birth weight infants
lar leukomalacia among neonates exposed to beta- following antenatal exposure to betamethasone versus dexa-
methasone and dexamethasone. methasone. Obstet Gynecol 2004;104:484–8.
The differences in intraventricular hemorrhage 7. Papile LA, Burstein J, Koffler H. Incidence and evolution of
after steroid exposure seen in our study may be subependymal and intraventricular hemorrhage: a study of
infants with birth weights less than 1,500 gm. J Pediatr 1978;
related to potency, duration of exposure, and fetal 92:529–34.
response after exposure. Dexamethasone is five times 8. Blackwelder WC. “Proving the null hypothesis” in clinical
more potent than betamethasone in nongenomic ef- trials. Control Clin Trials 1982;3:345–53.
fects in addition to the stereoisomer difference of a 9. LeFlore JL, Salhab WA, Broyles RS, Engle WD. Association of
methyl group at position 16 of ring D in their antenatal and postnatal dexamethasone exposure with out-
comes in extremely low birth weight neonates. Pediatrics
molecular structure.11,12 Derks et al12 described a more 2002;110:275–9.
rapid fall in fetal sheep progesterone levels and a 10. Lee BH, Stoll BJ, McDonald SA, Higgins RD, National
sharper rise in serum cortisol levels after betametha- Institute of Child Health and Human Development Neonatal
sone administration compared with dexamethasone, Research Network. Adverse neonatal outcomes associated
with antenatal dexamethasone versus antenatal betametha-
and the cortisol levels continued to rise at 72 hours sone. Pediatrics 2006;117:1503–10.
postexposure in the dexamethasone-treated fetal 11. Derks JB, Giussani DA, Van Dam LM, Jenkins SL, Winter JA,
sheep. Ballard and Liggins13,14 showed umbilical cord Zhao XF, et al. Differential effects of betamethasone and
cortisol levels increased more rapidly and with a dexamethasone fetal administration of parturition in sheep.
J Soc Gynecol Investig 1996;3:336–41.
higher zenith after each 12 mg of betamethasone
compared with 6 mg of betamethasone, with no 12. Buttgereit F, Brand MD, Burmester GR. Equivalent doses and
relative drug potencies for non-genomic glucocorticoid effects:
reported increased benefit to 24 mg betamethasone a novel glucocorticoid hierarchy. Biochem Pharmacol 1999;
dosing. The exact difference in physiologic responses 58:363–8.
of these stereoisomer molecules is not known and 13. Ballard PL, Liggins GC. Glucocorticoid activity in cord serum:
requires further investigation. comparison of hydrocortisone and betamethasone regimens.
J Pediatr 1982;101:468–70.
Our study largely supports the continuing use of
14. Ballard PL. Scientific rationale for the use of antenatal glu-
both betamethasone and dexamethasone in the treat- cocorticoids to promote fetal development. Pediatr Rev
ment of women at risk of preterm delivery. However, 2000;1:E83–90.
30 Elimian et al The Betacode Trial OBSTETRICS & GYNECOLOGY
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Physioex Lab Report: Pre-Lab Quiz ResultsДокумент4 страницыPhysioex Lab Report: Pre-Lab Quiz ResultsNovanza RayhanОценок пока нет
- Hangnails and HomoeopathyДокумент7 страницHangnails and HomoeopathyDr. Rajneesh Kumar Sharma MD HomОценок пока нет
- Interpretting ABG SuccessfullyДокумент15 страницInterpretting ABG Successfullyanimathz100% (1)
- Understanding-Ocd 2016 v2Документ27 страницUnderstanding-Ocd 2016 v2Samanjit Sen Gupta100% (1)
- What is BronchoscopyДокумент19 страницWhat is BronchoscopyMARIANN JEAN ANDREA CULANAG MATALINESОценок пока нет
- Typhoid Fever NCPДокумент46 страницTyphoid Fever NCPLyra Lustre RN67% (3)
- Microbiology ReviewerДокумент3 страницыMicrobiology ReviewerWendy Escalante100% (6)
- Pathophysiology of Deep Vein Thrombosis (Thrombophlebitis)Документ7 страницPathophysiology of Deep Vein Thrombosis (Thrombophlebitis)resty tacataОценок пока нет
- A Descriptive Study To Assess The Knowledge Regarding Management of Hyperemesis Gravidarum Among PostДокумент6 страницA Descriptive Study To Assess The Knowledge Regarding Management of Hyperemesis Gravidarum Among PostIJRASETPublicationsОценок пока нет
- ACTIVIDAD INGLES Reading ComprehensionДокумент3 страницыACTIVIDAD INGLES Reading Comprehensionyulis mesaОценок пока нет
- A Review of Subdural Empyema and Its Management.6Документ5 страницA Review of Subdural Empyema and Its Management.6PatriciaChRistianiОценок пока нет
- Stanford Letter Criticizes Trump COVID-19 AppointeeДокумент11 страницStanford Letter Criticizes Trump COVID-19 AppointeeBayAreaNewsGroup100% (2)
- Leaflet YTiG Plus Tablet For CHCДокумент1 страницаLeaflet YTiG Plus Tablet For CHCDesi Health Tips UpdateОценок пока нет
- Chronic Suppurative Otitis Media PDFДокумент3 страницыChronic Suppurative Otitis Media PDFsarahОценок пока нет
- COVID-19 Patient Report SummaryДокумент2 страницыCOVID-19 Patient Report Summarymuhammad imranОценок пока нет
- NSAID's QuestionsДокумент3 страницыNSAID's QuestionsManikanta Guptha100% (2)
- HematologyДокумент100 страницHematologyerzaraptorОценок пока нет
- Rapid Pathogen Detection by Metagenomic Next-Generation Sequencing of Infected Body FluidsДокумент26 страницRapid Pathogen Detection by Metagenomic Next-Generation Sequencing of Infected Body FluidsLuisОценок пока нет
- CLUSTERS LIST - (CHNCS) GO-209Документ45 страницCLUSTERS LIST - (CHNCS) GO-209Gadde Srinivasarao67% (3)
- Transverse Dimension Diagnosis and Relevance to Functional OcclusionДокумент6 страницTransverse Dimension Diagnosis and Relevance to Functional OcclusionDino MainoОценок пока нет
- Complications of 3rd TrimesterДокумент49 страницComplications of 3rd TrimesterMA. JYRELL BONITOОценок пока нет
- Sleep and The Risk of Chronic Kidney Disease: A Cohort StudyДокумент8 страницSleep and The Risk of Chronic Kidney Disease: A Cohort StudyEtaursaeОценок пока нет
- CDN 1 PDFДокумент22 страницыCDN 1 PDFJohn Mark100% (1)
- Morpho - Pathology Final Summary: Chapter 1: Cellular Reactions To AggressionДокумент21 страницаMorpho - Pathology Final Summary: Chapter 1: Cellular Reactions To Aggressiondjxela89Оценок пока нет
- Safe SexДокумент11 страницSafe SexnathanОценок пока нет
- Health Check Template FormДокумент2 страницыHealth Check Template Form백만호Оценок пока нет
- ICU Accomplishment Report and Improvement PlanДокумент5 страницICU Accomplishment Report and Improvement PlanMikhaelEarlSantosTacordaОценок пока нет
- Ayurvedic Dosha TheoryДокумент72 страницыAyurvedic Dosha Theoryyogiraj mishraОценок пока нет
- Body's Battles (gnv64) PDFДокумент96 страницBody's Battles (gnv64) PDFameyparanjape100% (1)
- IV To PO Poster VersionДокумент1 страницаIV To PO Poster VersionJohn Benedict Sta AnaОценок пока нет