Академический Документы
Профессиональный Документы
Культура Документы
Cord Prolapse YOR LBS 001
Загружено:
Onnie WiratamaИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Cord Prolapse YOR LBS 001
Загружено:
Onnie WiratamaАвторское право:
Доступные форматы
Guideline for the Management of Umbilical cord
Prolapse
The Queen Mother’s Hospital
Introduction
Objectives of this guideline
– to manage prolapse of the umbilical cord to improve perinatal outcome
– to safely and efficiently manage umbilical cord prolapse to minimise maternal
risk
This guideline is to be used by all registered midwives and medical staff within
Yorkhill Division of NHS Greater Glasgow and is to be applied to all antenatal
patients experiencing this complication within the unit.
Definition
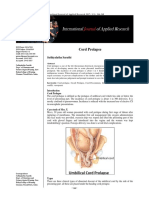
• Umbilical cord prolapse exists when a loop of cord is present below the
presenting part and the membranes are ruptured.
• Incidence is approximately 0.2% of births
• Risk of perinatal morbidity/mortality from asphyxia secondary to mechanical
compression of the cord between the presenting part and the pelvis, or spasm
of cord vessels secondary to cold or manipulation.
Risk Factors
Fetal Malpresentation Prematurity
Polyhydramnios Multiple pregnancy
Anencephaly
Maternal Contracted pelvis Pelvic tumour
Other Long cord
Sudden rupture of membranes, esp. if polyhydramnios
Obstetric Intervention
amniotomy, FSE application
expectant management of PPROM
Recommendations
Diagnosis
Vaginal examination to confirm diagnosis of prolapsed cord and to
ascertain cervical dilatation.
Cord Prolapse Version: 1.1 Page 1 of 2
Author(s): Dr J Roberts Authorised: Labour Suite Forum Issue Date: March 2005
Review Date: March 2007 Ref: YOR-LBS-001
Management
• Call for help – senior midwife, obstetric registrar, anaesthetist
• Determine that fetal heart present and monitor by CTG.
If fetus is viable -
• Discontinue Syntocinon, administer oxygen by face mask
• Make preparations for emergency Caesarean section - IV access, group and
save
• Elevation of the presenting part of the fetus above the pelvic inlet will
relieve cord compression. This can be achieved manually, in which case the
hand should remain in the vagina until delivery. Alternatively the patient may
be placed in the knee chest position, or the bladder may be filled with 500mls
saline through a Foley catheter. The catheter should be clamped, then
unclamped to allow bladder emptying when the skin incision is made at
Caesarean section.
Anaesthesia
Delivery will usually be by Caesarean section under GA. However, where the
bladder filling has been employed and there is no evidence of fetal distress,
regional anaesthesia may be considered.
Vaginal delivery
If the cervix is fully dilated then instrumental delivery may be appropriate but
should only be undertaken by experienced obstetric staff, i.e. Consultant or
experienced SpR.
If no FH auscultated – confirm intrauterine death using ultrasound and aim for
vaginal delivery.
If fetus of a non-viable gestation – discuss with senior obstetric staff and aim for
vaginal delivery
References
• MOET Course Manual, RCOG Press, 2003
This guideline has been assessed for Equality and Diversity issues.
Cord Prolapse Version: 1.1 Page 2 of 2
Author(s): Dr J Roberts Authorised: Labour Suite Forum Issue Date: March 2005
Review Date: March 2007 Ref: YOR-LBS-001
Вам также может понравиться
- Elizabeth G. Querubin BSN 3E1-9 - Group 195 A Ectopic PregnancyДокумент16 страницElizabeth G. Querubin BSN 3E1-9 - Group 195 A Ectopic PregnancyLizeth Querubin97% (38)
- Cord ProlapseДокумент4 страницыCord ProlapseCleta Escabarte Dehlin100% (1)
- Pectus Carinatum, (Pigeon Chest) A Simple Guide To The Condition, Treatment And Related ConditionsОт EverandPectus Carinatum, (Pigeon Chest) A Simple Guide To The Condition, Treatment And Related ConditionsОценок пока нет
- Cord ProlapseДокумент11 страницCord ProlapseWilliams Emmanuel AdeyeyeОценок пока нет
- Umbilical Cord ProlapseДокумент5 страницUmbilical Cord Prolapseangga hergaОценок пока нет
- Cord ProlapseДокумент16 страницCord ProlapseKarthiga RajooОценок пока нет
- Umibilical Cord ProlapseДокумент58 страницUmibilical Cord Prolapsekhadzx100% (3)
- Umbilical Cord Prolapse - StatPearls - NCBI BookshelfДокумент5 страницUmbilical Cord Prolapse - StatPearls - NCBI Bookshelfhermalina sabruОценок пока нет
- Guideline Umbilical Cord Prolapse NSH 2012Документ8 страницGuideline Umbilical Cord Prolapse NSH 2012Isikhuemen MaradonaОценок пока нет
- Benin LesionДокумент14 страницBenin Lesionsandeepv08Оценок пока нет
- Umbilical Cord ProlapseДокумент6 страницUmbilical Cord ProlapseCeth BeltranОценок пока нет
- Placenta and Placental ProblemsДокумент13 страницPlacenta and Placental ProblemsLuvita Ronteltap100% (1)
- Umbilical Cord ProlapseДокумент19 страницUmbilical Cord ProlapsedenekeОценок пока нет
- Chapter 24: Nursing Care of A Family During A Surgical Intervention For BirthДокумент22 страницыChapter 24: Nursing Care of A Family During A Surgical Intervention For BirthAlyssaGrandeMontimorОценок пока нет
- Obstetrical EmergenciesДокумент61 страницаObstetrical EmergenciesKavya S Mohan100% (2)
- Cervical IncompetenceДокумент30 страницCervical IncompetenceSignor ArasОценок пока нет
- Wirausaha Bab 345Документ6 страницWirausaha Bab 345Bebby Siskiyawati GentiОценок пока нет
- Transverse and Unstable LieДокумент31 страницаTransverse and Unstable LieRose Ann GonzalesОценок пока нет
- Cord Prolapse: Presented ToДокумент14 страницCord Prolapse: Presented ToNirajan MaharaОценок пока нет
- Umbilical Cord AccidentsДокумент16 страницUmbilical Cord Accidentschebetnaomi945Оценок пока нет
- Umbilical Cord ProlapseДокумент3 страницыUmbilical Cord ProlapseMae Christelle HamoyОценок пока нет
- Umibilical Cord - ProlapsДокумент22 страницыUmibilical Cord - ProlapsYosuaH.KumambongОценок пока нет
- Breech BabyДокумент11 страницBreech BabyscribbОценок пока нет
- Cord Prolapse and Cord PresentationДокумент21 страницаCord Prolapse and Cord PresentationKwizera virgileОценок пока нет
- Obstructed Labour FДокумент53 страницыObstructed Labour FMax ZealОценок пока нет
- Umibilical Cord - ProlapsДокумент22 страницыUmibilical Cord - ProlapsAtikah PurnamasariОценок пока нет
- Obestetric HemorrhageДокумент56 страницObestetric HemorrhageTiblets MirutsОценок пока нет
- Estabilizacion de PotrillosДокумент6 страницEstabilizacion de PotrillosCarlos Pedro VillaОценок пока нет
- Midwifery 102 Module 2aДокумент18 страницMidwifery 102 Module 2aWynjoy NebresОценок пока нет
- Nursing Care of The Client With High Risk Labor and Her FamilyДокумент37 страницNursing Care of The Client With High Risk Labor and Her Familyanne_088Оценок пока нет
- The Role of Transabdominal Cervical Cerclage Techniques in MaternityДокумент9 страницThe Role of Transabdominal Cervical Cerclage Techniques in MaternityI Tech Services KamranОценок пока нет
- Cord ProlapseДокумент18 страницCord ProlapseHomeground entertainmentОценок пока нет
- Define Transverse LieДокумент3 страницыDefine Transverse LiemimycuteyОценок пока нет
- Obstetric EmergenciesДокумент76 страницObstetric EmergenciesN. Siva100% (1)
- Cord Prolapse Final (Dr. P Garai)Документ33 страницыCord Prolapse Final (Dr. P Garai)Akash ChakrabortyОценок пока нет
- Umbilical Cord Accidents-1Документ16 страницUmbilical Cord Accidents-1chebetnaomi945Оценок пока нет
- Anesthesia For Foetal Surgery: Dr. Athira S MadhuДокумент98 страницAnesthesia For Foetal Surgery: Dr. Athira S MadhuAthira S MadhuОценок пока нет
- Umbilical Cord ProlapseДокумент26 страницUmbilical Cord Prolapsesulekhaanoob100% (2)
- High Risk Labor and DeliveryДокумент110 страницHigh Risk Labor and DeliveryWilbert CabanbanОценок пока нет
- Ectopic Pregnancy - PowerpointДокумент60 страницEctopic Pregnancy - PowerpointAndrada Doţa100% (1)
- Umbilical Cord ProlapseДокумент4 страницыUmbilical Cord ProlapseYwagar Ywagar100% (1)
- Unit 13Документ15 страницUnit 13Manjuari GhartiОценок пока нет
- Uterine Rupture: Labor LaborДокумент6 страницUterine Rupture: Labor LaborFerreze AnnОценок пока нет
- Proceedings of The 16th Italian Association of Equine Veterinarians CongressДокумент8 страницProceedings of The 16th Italian Association of Equine Veterinarians CongressCabinet VeterinarОценок пока нет
- FIGO Second Stage of LaborДокумент10 страницFIGO Second Stage of LaborAlmira Dyah PuspitariniОценок пока нет
- Definition: Related Diagnostic TestsДокумент8 страницDefinition: Related Diagnostic TestsQuinn Xylon VillanuevaОценок пока нет
- Pregnancy Trauma NotesДокумент8 страницPregnancy Trauma NotesHisham FahadОценок пока нет
- Fetal Malpresentation: Face PresentationДокумент10 страницFetal Malpresentation: Face PresentationuouoОценок пока нет
- Cord Prolapse: Sathiyalatha SarathiДокумент3 страницыCord Prolapse: Sathiyalatha Sarathidiah komalaОценок пока нет
- Anomalies of The Placenta and Cord 1Документ52 страницыAnomalies of The Placenta and Cord 1Daniel Andre S. Somoray100% (1)
- Placenta Accreta: Rose May Formoso BSN 2Документ4 страницыPlacenta Accreta: Rose May Formoso BSN 2MayMay AscadoFОценок пока нет
- Umbilical Cord ProlapseДокумент4 страницыUmbilical Cord ProlapseAJ TaoataoОценок пока нет
- Early Pregnancy Complications: Ectopic Pregnancy Gestational Trophoblastic Disease Ji Aggasid, JanniecelДокумент60 страницEarly Pregnancy Complications: Ectopic Pregnancy Gestational Trophoblastic Disease Ji Aggasid, JanniecelmedicoОценок пока нет
- Placenta Previa: Case DiscussionДокумент4 страницыPlacenta Previa: Case DiscussionTin SumangaОценок пока нет
- Cordprolapse 190701165943Документ28 страницCordprolapse 190701165943DrPreeti Thakur ChouhanОценок пока нет
- Laparoscopic Sleeve GastrectomyОт EverandLaparoscopic Sleeve GastrectomySalman Al-SabahОценок пока нет