Академический Документы
Профессиональный Документы
Культура Документы
Case Phys Exam
Загружено:
pay tinapayОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Case Phys Exam
Загружено:
pay tinapayАвторское право:
Доступные форматы
Case Study: Physical Exam
Background
The following case study can be used with mentees to illustrate the purpose and value of
conducting a physical exam. The case is structured to include pauses in the narrative to allow
mentees to practice clinical decision-making along the way. In this way, it resembles a
structured clinical vignette (see Using Clinical Vignettes).
Case
The patient is a 50 year-old man infected with HIV who comes to a clinic for routine
follow-up.
He was diagnosed with HIV infection six months ago, with a CD4 count of 60, and
started antiretroviral therapy (ART) with nevirapine, 200 mg daily for 14 days, then
BID, i.e., twice a day. He started stavudine 30 mg BID and lamivudine 150 mg BID 3
months ago. He has tolerated this regimen well, and says he takes almost all of his
prescribed doses. He has missed several follow-up appointments with the clinic
doctors, but has come to the pharmacy to receive his medications every month. Another
clinician started him on ART, and this is the first time you have seen him. He says that
his appetite is fair, and that he is not losing weight. He denies fevers, but has some
sweats at night. He denies pain, tingling, or numbness in his extremities. The remainder
of his review of systems (ROS) is normal, by his report.
Since you do not know him, you quickly review his chart. It reveals that he had some
anemia at baseline, with hemoglobin of 10. His chemistries and liver enzymes were
normal before starting ART. He had reported some discolorations on his skin, but there
is no further mention of this in the notes.
In addition to ART he is taking cotrimoxazole, 1 double-strength tablet daily. He denies
medication allergies.
His vital signs appear normal in the triage nurse’s notes from today.
The patient would like to pick up his medications and go home.
Questions:
1. How would you like to proceed?
2. Are you done with the visit?
Case Study: Physical Exam 1
I-TECH Clinical Mentoring Toolkit
Case, continued
You explain to the patient that you would like to do a quick physical exam, since it has
been a while since he saw a clinician. Externally, his head appears normal, with no scalp
lesions or alopecia. His pupils and conjunctivae are normal. Examination of his
oropharynx reveals no thrush or leukoplakia, but there is a flat, oval, violaceous lesion
on his hard palate. The patient was unaware of this lesion. There is no cervical
adenopathy.
You ask the patient to remove his shirt.
Examination of the skin reveals 10 to 15 hyperpigmented, flat, non-tender lesions
scattered across his torso, back, and both arms. They are slightly nodular to the touch.
When you ask, the patient says that these were the skin discolorations he had when he
was first started on ART, but that they have increased in number since then. He has no
axillary adenopathy or edema of the upper extremities. His lungs are clear to
auscultation and percussion. His cardiac rate and rhythm are regular, and there are no
cardiac murmurs. His abdomen is soft and non-tender to palpation. The liver edge is
soft and non-distended, and you don’t notice any signs of splenomegaly.
You ask the patient to put his shirt back on and to remove his pants, socks, and shoes.
There is no inguinal adenopathy. There are a few hyperpigmented, flat, nodular lesions
scattered on his legs. There is no edema of either extremity.
His cranial nerves are normal. Examination of all four extremities shows intact pinprick
and light touch sensation and 5/5 strength. His biceps, patellar, and heel deep tendon
reflexes are 2+ and symmetric.
Questions
1. What is your preliminary diagnosis?
2. Do you think the patient is taking his ART?
3. What testing would you like to perform?
4. How did performing a physical exam change your management of this patient?
Comments and Questions/Discussion Points:
Case Study: Physical Exam 2
I-TECH Clinical Mentoring Toolkit
Clinically, this patient has Kaposi sarcoma (KS) in addition to AIDS. KS would have been
missed had the examiner trusted the chart and the patient’s self-report and not performed an
independent physical exam. It is likely that the patient had KS at the time ART was started, for
he complained of similar lesions at the time. These may have been misdiagnosed at the time, or
the patient may not have been thoroughly examined.
1. Why do you suppose the patient did not report progression of his skin lesions in the
review of systems?
Perhaps he was frightened, and in denial, and didn’t want the possibility of another disease
confirmed. Perhaps he didn’t think it was anything important. (Remember, KS lesions often are
painless, and his are causing him no associated symptoms, such as difficulty eating, local
swelling around the lesions, or lymphedema).
KS is a vascular tumor caused by infection with Human Herpesvirus 8 (HHV8). It most
commonly affects the skin, with lesions as described in this case, but can also appear on oral
mucosae, conjunctivae, and visceral organs, including in the bronchi, lung parenchyma, and
gastrointestinal (GI) tract. Effective combination ART has revolutionized the treatment and
prognosis of KS. ART alone is often sufficient to control cutaneous disease and cause lesions to
regress, although it can take several months of ART to show an effect. Extensive cutaneous
disease and visceral disease usually require ART plus chemotherapy, which is increasingly
available in resource-limited settings. There are increasing reports of KS lesions worsening
shortly after ART is started, i.e., KS IRIS (immune reconstitution inflammatory syndrome).
This can be lethal when it involves pulmonary KS, in which case concomitant chemotherapy is
needed.
2. Why is the patient’s KS progressing despite his being on ART?
This may be a sign that the ART he is picking up every month may not actually be getting into
his system, either because he is not taking it (i.e., poor adherence) or is not absorbing it from his
GI tract. Alternatively, he may need chemotherapy in addition to ART to control his disease.
3. What tests would you consider performing at this point?
Logical next steps would be to obtain a CD4 count, which he is due for anyway, to see if he is
experiencing immunologic recovery on ART. It would also be sensible to inquire about his
adherence, inquire about symptoms of malabsorption, and obtain a chest x-ray to look for signs
of pulmonary KS (usually a nodular infiltrate). This is definitely a situation in which getting
help from a clinician highly experienced in HIV-associated KS would be helpful.
Case Study: Physical Exam 3
I-TECH Clinical Mentoring Toolkit
Вам также может понравиться
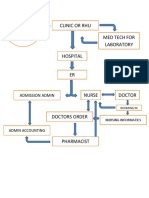
- Clinic or Rhu: Admission AdminДокумент1 страницаClinic or Rhu: Admission Adminpay tinapayОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Long Quiz Drugs For Endocrinologic DisordersДокумент4 страницыLong Quiz Drugs For Endocrinologic Disorderspay tinapayОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- Diet For Diabetic PatientsДокумент7 страницDiet For Diabetic Patientspay tinapayОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Case Study FormatДокумент15 страницCase Study Formatpay tinapayОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Rhealyn C. PojasДокумент2 страницыRhealyn C. Pojaspay tinapayОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Patient Sues Doc, Nurses, Hospital Exec: Rhealyn C. PojasДокумент2 страницыPatient Sues Doc, Nurses, Hospital Exec: Rhealyn C. Pojaspay tinapayОценок пока нет
- A Part 1 of Case Study by Angelene Tagle 09 08 2020Документ6 страницA Part 1 of Case Study by Angelene Tagle 09 08 2020pay tinapay100% (1)
- Jhezelle Nicole R. Ignacio BS Nursing Older Adult 3rd Year Reaction Paper Thursday, September 3, 2020 at 9:04 AMДокумент2 страницыJhezelle Nicole R. Ignacio BS Nursing Older Adult 3rd Year Reaction Paper Thursday, September 3, 2020 at 9:04 AMpay tinapayОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Community Health Nursing IiДокумент22 страницыCommunity Health Nursing Iipay tinapay100% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Make Sure To Feature Your Bestsellers or Signature Products or Pieces. Keep It Simple and To The Point by Listing The Name, Price and Brief Description.Документ2 страницыMake Sure To Feature Your Bestsellers or Signature Products or Pieces. Keep It Simple and To The Point by Listing The Name, Price and Brief Description.pay tinapayОценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- NCP PreeclampsiaДокумент1 страницаNCP PreeclampsiaMonica Cruz Dalida74% (23)
- FLC-L-BM-T2 - Alice JacksonДокумент10 страницFLC-L-BM-T2 - Alice Jacksonvoldemort killerОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- 2 Infez Med 1 2020 01 Rodriguez 003-005-2019nCoV-FINALДокумент3 страницы2 Infez Med 1 2020 01 Rodriguez 003-005-2019nCoV-FINALNataliaRiosОценок пока нет
- MCQs and Viva in Public Health Dentistry PDFДокумент235 страницMCQs and Viva in Public Health Dentistry PDFRitika90% (10)
- Chapter 6 of Modern Epidemiology 3e - Quiz Set 1Документ1 страницаChapter 6 of Modern Epidemiology 3e - Quiz Set 1Genevieve Magpayo NangitОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Pediatrics Mcqs Part 2: (Correct Answer)Документ1 страницаPediatrics Mcqs Part 2: (Correct Answer)maai33Оценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- dm2021 0327 Surge Response Plan For HFДокумент11 страницdm2021 0327 Surge Response Plan For HFMonica Lowinski100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- DR Vernon Coleman Proof That Masks Do More Harm Than GoodДокумент4 страницыDR Vernon Coleman Proof That Masks Do More Harm Than GoodGeorge KourisОценок пока нет
- Oumme Rushaa Sairally FINAL5PAGEДокумент6 страницOumme Rushaa Sairally FINAL5PAGERushaa SairallyОценок пока нет
- 200-Article Text-1119-1-10-20200603Документ6 страниц200-Article Text-1119-1-10-20200603miaОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Askep Diabetes MelitusДокумент13 страницAskep Diabetes MelitusfahrulОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1091)
- MCU 2019 Human Diseases 5th EditionДокумент626 страницMCU 2019 Human Diseases 5th EditionMoon Edits100% (1)
- An Experience On COVID-19Документ2 страницыAn Experience On COVID-19Avinash BashОценок пока нет
- Management TTPДокумент14 страницManagement TTPSutirtho MukherjiОценок пока нет
- First Aid ROLДокумент20 страницFirst Aid ROLAnitha NoronhaОценок пока нет
- ColisepicemiaДокумент8 страницColisepicemiajazz100% (1)
- Genital Herpe2Документ5 страницGenital Herpe2Blood Heart <3Оценок пока нет
- Robert R. Rich, Thomas A. Fleisher, Harry W. Schroeder JR., Cornelia M. Weyand, David B. Corry, Jennifer M. Puck - Clinical Immunology - Principles and Practice-Elsevier (2022)Документ1 259 страницRobert R. Rich, Thomas A. Fleisher, Harry W. Schroeder JR., Cornelia M. Weyand, David B. Corry, Jennifer M. Puck - Clinical Immunology - Principles and Practice-Elsevier (2022)Lina GaouarОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- ADC Part 1 - TG Keynotes II v1.0 PDFДокумент17 страницADC Part 1 - TG Keynotes II v1.0 PDFDrSaif Ullah KhanОценок пока нет
- Obstructive Sleep Apnoea (OSA) Definition of Obstructive Sleep Apnoea (OSA)Документ4 страницыObstructive Sleep Apnoea (OSA) Definition of Obstructive Sleep Apnoea (OSA)Abdul JalilОценок пока нет
- Dua Kasus Multipel Sklerosis Dengan Tipe Yang Berbeda Di Rsup M. Djamil, PadangДокумент7 страницDua Kasus Multipel Sklerosis Dengan Tipe Yang Berbeda Di Rsup M. Djamil, PadangNurul Fitriana IbrahimОценок пока нет
- Sexually Transmitted DiseaseДокумент38 страницSexually Transmitted Diseaserana arslanОценок пока нет
- Explanation Text Covid-19Документ2 страницыExplanation Text Covid-19Mr ClawОценок пока нет
- OncologyДокумент3 страницыOncologyMichtropolisОценок пока нет
- EASL Clinical Practice Guidelines: Autoimmune HepatitisДокумент34 страницыEASL Clinical Practice Guidelines: Autoimmune HepatitisBety Puma PauccaraОценок пока нет
- COVID-19 Survival Guide McMaster 2020 07 01Документ29 страницCOVID-19 Survival Guide McMaster 2020 07 01MUHAMMAD09Оценок пока нет
- CPC Case 1Документ9 страницCPC Case 1Astarte DimasalangОценок пока нет
- Kansas College Immunization WaiverДокумент1 страницаKansas College Immunization WaiverDonnaОценок пока нет
- Treatment of Cutaneous Larva Migrans: Eric CaumesДокумент4 страницыTreatment of Cutaneous Larva Migrans: Eric CaumesElva PatabangОценок пока нет
- PODCAST #67 DR.B The Vet Show - Drh. Syavira EkdhiasmaraДокумент26 страницPODCAST #67 DR.B The Vet Show - Drh. Syavira EkdhiasmaraLailatun NafisahОценок пока нет