Академический Документы
Профессиональный Документы
Культура Документы
Nursing Journals
Загружено:
Shaina FukamiОригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Nursing Journals
Загружено:
Shaina FukamiАвторское право:
Доступные форматы
Heart Failure With Preserved Ejection Fraction In Perspective
https://doi.org/10.1161/CIRCRESAHA.119.313572 - 2019;124:1598–1617
Heart failure (HF) was undoubtedly a major contributor to the centuries old
edematous condition, dropsy. As HF was recognized as a leading cause of edema and
dyspnea, the pathophysiologic role of the heart also emerged as is evident from the 1933
Lewis textbook definition of HF “a condition in which the heart fails to discharge its
contents adequately.”1 With the advent of hemodynamic measurements, it became clear that
congestion, the core of the HF syndrome regardless of the cause, was because of elevated
cardiac filling pressures. The more current HF definition “an inability of the heart to pump
blood to the body at a rate commensurate with its needs, or to do so only at the cost of high
filling pressures,” prominently adds this crucial aspect.
While this definition provides a reference standard against which other definitions
can be compared, it is much less transferable to clinical bedside practice where left
ventricular (LV) end-diastolic pressure is not directly measured. Multiple approaches have
been used to clinically define the syndrome of HF based on an integration of the patient’s
history, presentation, physical examination, and laboratory supportive findings to assess
whether HF is present, each with its own advantages and disadvantages. As in many aspects
of medicine, there is a range of diagnostic certainty about the time-honored constellation of
signs and symptoms attributed to HF. Dyspnea, for example, a critical component of HF can
also be a central manifestation of pulmonary disease rather than an aspect of impaired
cardiac performance. The judgment and experience needed to integrate the information
incorporated in the term HF challenges its diagnostic precision.
Despite the ambiguities and overlaps with other chronic conditions, the
unquestionable multifold higher risk for cardiovascular death as well as subsequent repeat
exacerbations of symptoms requiring hospitalizations for HF management of those with this
clinically determined diagnosis offers firm validation that the term has important specificity
and meaning. Indeed, the linkage between this longstanding clinical usage and heightened
risks for HF-specific major adverse events underscores that despite the seemingly inexact
diagnosis, HF denotes a most grave and identifiable medical disorder.
The adverse prognostic impact of a diagnosis of HF on an individual level is greatly
amplified on a population basis because its associated risk is matched by the relatively high
prevalence of HF in older individuals. In the Medicare population, HF is among the most
frequent reason to prompt an urgent hospitalization. The mortality occurring during a
hospitalization for HF is ≈4%. Despite major advances in HF management and care,
mortality within 1 month after discharge is 10%. Because 1 in 5 men and women over 40
years of age will develop HF during their lifetime, the public health burden, and cost to
society are staggering. These sobering statistics use the bedrock clinical definition of the
treating physicians for these assessments of the morbidity-mortality and economic impact
of a diagnosis of HF. It is important to note that neither the cause nor any measure of the
extent of cardiac dysfunction is incorporated into the broad overall definition or adverse
impact of a diagnosis of HF.
Acute calculous cholecystitis: Review of current best practices
World J Gastrointest Surg. 2017 May 27; 9 (5): 118-126
Acute calculous cholecystitis (ACC) represents the second source of complicated
intra-abdominal infection (18.5%), according to the World Society of Emergency
Surgery complicated intra-abdominal infections Score study. Biliary stones are the main
etiology and are present in 6.5% of men and 10.5% of women. The risk of complications,
like ACC, gallstone pancreatitis, and choledocholithiasis is 1% to 4% per year.
Furthermore, it is recognized that patients with symptomatic cholecystolithiasis will
develop ACC more frequently than their asymptomatic counterparts; thereby, effectively
raising the risk of complications to five times higher.
ACC is the most common complication of cholecystolithiasis accounting for 14%
to 30% of cholecystectomies performed in many countries. The disease can be
diagnosed at any grade of severity including wall inflammation, local complication and
systemic organ dysfunction. Moreover, complicated grades of the disease increase with
age, with a peak between 70 and 75 years.The aim is of this manuscript is to provide a
practical and comprehensive review of the most important aspects of ACC and its
complications. In parallel, to highlight the current evidence that helps the surgeons
bedside decision making, on how best to manage the disease, to improve outcomes.
ACC is caused by an inflammatory/infectious process involving the gallbladder
wall, in many cases due to an impacted gallstone in the infundibulum or in the cystic
duct. The continued mucin production from epithelium and the gallbladder distention,
results in micro and macro circulatory perfusion deficits. The subsequent events are
serosa edema, mucosal sloughing, venous and lymphatic congestion, ischemia and
necrosis with regional or diffuse peritonitis. Acute inflammation may be complicated by
secondary bacterial infection, from the bile duct, via the portal lymphatic or vascular
system. The microorganisms present in the gastrointestinal tract are the most common
pathogens
Вам также может понравиться
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Seamanship ReportingДокумент19 страницSeamanship ReportingShaina FukamiОценок пока нет
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- 12 Lead Ecg PlacementsДокумент2 страницы12 Lead Ecg PlacementsShaina FukamiОценок пока нет
- Fasting Blood Sugar: ND RD THДокумент1 страницаFasting Blood Sugar: ND RD THShaina FukamiОценок пока нет
- Mechanism of LaborДокумент1 страницаMechanism of LaborShaina FukamiОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
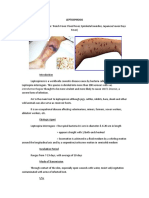
- Leptospirosis: Icterohemorrhagiae Thought To Be More Virulent and More Likely To Cause Weil's Disease, AДокумент2 страницыLeptospirosis: Icterohemorrhagiae Thought To Be More Virulent and More Likely To Cause Weil's Disease, AShaina FukamiОценок пока нет
- Types of Fetal PresentationДокумент2 страницыTypes of Fetal PresentationShaina FukamiОценок пока нет
- Acute Pain Due To Labor Process NCPДокумент1 страницаAcute Pain Due To Labor Process NCPRhod Vincent Jamolod TayongОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The Trauma of War in The Poem Dulce Et Decorum EstДокумент1 страницаThe Trauma of War in The Poem Dulce Et Decorum EstRahiem PottingerОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- SEO Price CovidДокумент275 страницSEO Price CovidMohammad AbdulhadiОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Treatment Planning FPD Lec 2Документ23 страницыTreatment Planning FPD Lec 20 0Оценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- 16pf ReportДокумент11 страниц16pf Reportipsa.khuranaОценок пока нет
- Marketing Ayurveda-Recent Trends: Currently-CONSULTANT HR & Administration, FDCM ESSELWORLD GOREWADA ZOO Pvt. LTDДокумент27 страницMarketing Ayurveda-Recent Trends: Currently-CONSULTANT HR & Administration, FDCM ESSELWORLD GOREWADA ZOO Pvt. LTDUday DokrasОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Cook Poultry and Game DishesДокумент37 страницCook Poultry and Game DishesDanica Joy Ocampo Dianzon100% (1)
- G10 Las Health Q4Документ2 страницыG10 Las Health Q4ALBERT IAN CASUGAОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- Prevention Practice For Cardiopulmonary ConditionsssДокумент38 страницPrevention Practice For Cardiopulmonary ConditionsssArham ShamsiОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Clinical Teaching ProgrammeДокумент11 страницClinical Teaching ProgrammeKrini TandelОценок пока нет
- Microbiology at A GlanceДокумент126 страницMicrobiology at A GlanceMuhammad UsmanОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- 1066UE 2023-01 RANDOX Level 3Документ92 страницы1066UE 2023-01 RANDOX Level 3Dharmesh PatelОценок пока нет
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- GP 44.0 Coshh Risk Assessment FormДокумент1 страницаGP 44.0 Coshh Risk Assessment FormLarbi BelazizОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- NHS Change ManagementДокумент20 страницNHS Change ManagementMary NjeriОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- 28,29 Management of Cardiac ArrhythmiasДокумент41 страница28,29 Management of Cardiac ArrhythmiasSL Dr ChEMiSОценок пока нет
- Thesis StatementДокумент15 страницThesis StatementJos50% (2)
- 2019 HSPD Report - WebДокумент40 страниц2019 HSPD Report - WebNevin SmithОценок пока нет
- Health-Preneurship: Why Does Public Health Need An Entrepreneur?Документ11 страницHealth-Preneurship: Why Does Public Health Need An Entrepreneur?LipatriОценок пока нет
- KSSM Science Form 4 Chapter 10Документ16 страницKSSM Science Form 4 Chapter 10Tang Lilee100% (1)
- Janson Medical Clinic: A Case Study in Quality ImprovementДокумент7 страницJanson Medical Clinic: A Case Study in Quality ImprovementAira Genille YaochingОценок пока нет
- Rad 97Документ188 страницRad 97Ahmed BadranОценок пока нет
- Respect in The Workplace: The Management of Disrespectful ConductДокумент8 страницRespect in The Workplace: The Management of Disrespectful ConductHP w1907Оценок пока нет
- Spectre CaseДокумент9 страницSpectre CaseAhmad ZaryabОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Acute Respiratory Distress Syndrome: Diagnosis and Management p730Документ9 страницAcute Respiratory Distress Syndrome: Diagnosis and Management p730Ahmed AlhalwajiОценок пока нет
- Review Jurnal Bunga Aurelia (18621005)Документ3 страницыReview Jurnal Bunga Aurelia (18621005)bungaОценок пока нет
- 761 ResearchДокумент7 страниц761 ResearchBrianna TorkelsonОценок пока нет
- Millerj Resume2021Документ1 страницаMillerj Resume2021api-546620936Оценок пока нет
- TDSB GR 9-12 Student Census, 2022Документ31 страницаTDSB GR 9-12 Student Census, 2022True NorthОценок пока нет
- Position Paper About Legalization of Marijuana in The PhilippinesДокумент2 страницыPosition Paper About Legalization of Marijuana in The PhilippinesHabibi Waishu93% (14)
- Effect of Cognitive Dissonance On The Performance of Employees in Academic JobsДокумент3 страницыEffect of Cognitive Dissonance On The Performance of Employees in Academic JobsAnonymous klP1LOCbОценок пока нет