Академический Документы
Профессиональный Документы
Культура Документы
02VBL Pemphigus
Загружено:
Raniya Zain0 оценок0% нашли этот документ полезным (0 голосов)
37 просмотров48 страницPemphigus is a group of rare autoimmune blistering diseases of the skin and mucous membranes. Pemphigus vulgaris is the most common type and causes blisters and sores in the mouth and throat. Histopathology shows a separation in the epithelial layers due to loss of cell junctions. Diagnosis involves direct immunofluorescence microscopy detecting antibodies between epithelial cells. Treatment is with high-dose corticosteroids and immunosuppressants to control the autoimmune response.
Исходное описание:
Оригинальное название
02VBL_Pemphigus
Авторское право
© © All Rights Reserved
Доступные форматы
PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документPemphigus is a group of rare autoimmune blistering diseases of the skin and mucous membranes. Pemphigus vulgaris is the most common type and causes blisters and sores in the mouth and throat. Histopathology shows a separation in the epithelial layers due to loss of cell junctions. Diagnosis involves direct immunofluorescence microscopy detecting antibodies between epithelial cells. Treatment is with high-dose corticosteroids and immunosuppressants to control the autoimmune response.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
37 просмотров48 страниц02VBL Pemphigus
Загружено:
Raniya ZainPemphigus is a group of rare autoimmune blistering diseases of the skin and mucous membranes. Pemphigus vulgaris is the most common type and causes blisters and sores in the mouth and throat. Histopathology shows a separation in the epithelial layers due to loss of cell junctions. Diagnosis involves direct immunofluorescence microscopy detecting antibodies between epithelial cells. Treatment is with high-dose corticosteroids and immunosuppressants to control the autoimmune response.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 48
Diseases of SKIN
Vesiculobullous Lesions
Pemphigus
Dr. Anthony George
Dept. of Oral & Maxillofacial Pathology and Oral Microbiology
Pemphigus
Variants / types of pemphigus
1. Pemphigus vulgaris.
2. Paraneoplastic pemphigus.
3. Familial benign pemphigus (Hailey-Hailey
disease).
4. Pemphigus vegetans.
5. Pemphigus foliaceus (Brazilian wildfire).
6. Pemphigus erythematous.
7. Pemphigus herpetiformis.
8. Drug-induced pemphigus.
9. IgA pemphigus.
10.Endemic pemphigus (fogo selvagem).
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris
Pemphigus Vulgaris
Vulgaris – Latin word meaning „common‟.
(Lupus vulgaris – Tuberculosis of skin).
Pemphigus Vulgaris is mucocutaneous blistering
disease, caused by circulating autoantibodies,
directed against keratinocyte transmembrane
proteins, resulting in intraepithelial split.
Of all variants only Pemphigus Vulgaris occurs in
oral cavity.
Oral lesions may appear first (before skin lesions)
Last to resolve after initiation of treatment.
Patho-physiology (Etiology)
Vesiculobullous Lesions
For unknown reasons autoantibodies are directed
against cell junctions that hold epithelial cells
together, causing damage to host tissue, resulting in
clinical appearance of vesiculo-bullous lesions.
Auto-anti-bodies – inappropriate production of
antibodies against normal constituents (self antigens) of
human body.
Adhesive Cell Junctions
Cell to cell adhesive junction – desmosomes.
Cell to matrix adhesive junction – hemidesmosomes.
Antony George Oral & Maxillofacial Pathology
Unknown reason.
Individuals with certain human lymphocyte antigen (HLA) are more prone.
IgG (G1 & G4) & C3 autoantibodies produced
against transmembrane adhesive protein of
desmosomal cell junction
E-cadherin protein – desmoglein 1 & 3.
» Desmoglein 1 is expressed more in upper layers of skin.
» Desmoglein 3 is expressed more in supra basal cell layer of
oral mucosa.
Intraepithelial supra basal cleft (blister) containing
clear fluid develop due to lack of cell adhesion.
Antony George Oral & Maxillofacial Pathology
Clinical Features
Pemphigus Vulgaris: Clinical Features
Epidemiology
Rare skin disease (1 in 1 million).
Age: 50-60 yrs (30-50 yrs in Indian population).
Gender: No gender predilection.
Race: More common in Jews, south Asians.
Site:
In oral cavity commonly seen in – palate, labial & buccal
mucosa, tongue, gingiva.
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris: Clinical Features
Skin Lesions
Rapid appearance of flaccid vesicles and bulla
covering large areas of skin.
Few mm to several cm in size.
Initially contain thin watery clear fluid.
Later become purulent due to pus formation – dead
cells.
Bulla rupture easily due to thin roof of bulla to form
raw eroded painful erythematous areas.
Antony George Oral & Maxillofacial Pathology
Pemphigus
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris: Clinical Features
Oral Manifestations
Oral lesions may appear first in 50% of cases.
May appear 1 yr earlier to skin lesions.
1. Intact bulla are rare in oral cavity as roof is thin &
friable – rupture easily during mastication.
Bulla rupture to form ill-defined, irregularly
shaped, superficial erosions or painful ulcers.
Patient unable to eat and drink due to painful ulcers
that are slow to heal.
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris: Clinical Features
Haphazardly distributed map-like painful ulcerated
lesions of buccal mucosa and palate.
Mucosa appear to peal away from surface.
Upper layers of mucosa can be lifted up with dental
probe.
Lesions may involve larynx leading to hoarseness of
voice.
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris: Clinical Features
2. Desquamative gingivitis.
Painful eroded erythematous
marginal and interdental gingiva.
No plaque or calculus deposits.
3. Cerebriform tongue.
Dorsum of tongue have painful
ulcers forming deep sulcus and
grooves.
Painful eroded and ulcerated
lesions on ventral surface and tip of
tongue.
Palatal mucosa may be involved.
Pemphigus Vulgaris: Clinical Features
4. Nikolsky’s sign is positive.
Diagnostic clinical skin test for vesiculobullous
lesions.
Application of oblique lateral pressure on
unaffected skin produce clear fluid filled blister.
Lateral pressure cause disruption of desmosomal cell
junctions resulting in split in epithelium.
In oral cavity air blown from 3-way syringe of dental
unit on gingiva will produce clear fluid filled blister.
Antony George Oral & Maxillofacial Pathology
Histopathological Investigation
Pemphigus Vulgaris
Special care during BIOPSY
Biopsy should be taken from peri-lesional tissue.
Obtained peri-lesional tissue is incubated in salt solution
to create blister – salt split technique
Should be submitted in Michel’s solution (fixative) or
frozen in liquid nitrogen to prevent pealing away of
epithelium.
10% formalin to be avoided as fixative.
Diagnosis cannot be made if ulcerated mucosa
without epithelium is submitted.
Epithelium should be present to identify level of split for
diagnosis.
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris: Histopathology
1. Supra basal intraepithelial cleft (separation) with
lifting of superficial epithelium.
Loss of desmosomal cell junctions.
2. Basal cells appear as ‘row of tombstones’ in floor
of bulla.
3. Stratum spinosum show acantholysis –
‘dilapidated brick wall’ appearance.
4. Tzanck Cells = clumps of loose round
degenerating swollen epithelial cells with hyper-
chromatic nucleus lying free in vesicular space.
Antony George Oral & Maxillofacial Pathology
Pemphigus Vulgaris: Histopathology
Antony George Oral & Maxillofacial Pathology
Cytological Investigation
Pemphigus Vulgaris
Tzanck Test
Cytological diagnostic test for pemphigus.
Un-ruptured intact bulla is pierced with sterile fine
needle and fluid content is obtained.
Cytological smear is prepared on clean glass slide.
Smear is stained with PAP stain.
Studied under microscope for Tzanck Cells.
Clumps of round swollen epithelial cells with hyper-
chromatic nucleus.
Special Investigations
Immuno Fluorescence
Immuno Fluorescence
Special diagnostic technique to identify specific
antibodies produced.
Fluorescence: property of some chemical
substances which when illuminated by light of certain
wavelength (UV light) will re-emit light of longer
wavelength.
Studied under Fluorescent Microscope.
Two Variants of Immunofluorescent Technique
1. Direct immunofluorescence (DIF).
2. Indirect immunofluorescence (IIF).
Antibodies directed against
human immunoglobulin's to
be studied are created by
inoculating them into goat.
Harvested goat antihuman
antibody are tagged or
conjugated with
fluorochromes.
Antibodies directed against
human immunoglobulin's to
be studied are created by
inoculating them into goat.
Harvested goat antihuman
antibody are tagged or
conjugated with
fluorochromes.
Pemphigus vulgaris
Direct immunofluorescence microscopy (DIF)
Immunoreactants deposited throughout epithelium –
‘chicken wire’ or ‘fish net’ appearance.
Demonstrates IgG (G4 & G1) in intercellular spaces of
epithelial cells in 90-100% of patients.
C3, IgM, IgA deposition seen less commonly –
commonly found in clinically normal adjacent
epithelium.
Antony George Oral & Maxillofacial Pathology
Pemphigus vulgaris
Indirect immunofluorescence microscopy (IIF)
Circulating IgG autoantibodies to squamous
intracellular substance seen in 80-90% of cases.
C3, IgM, IgA may also show positivity.
Titers of circulating autoantibodies can be measured
– helps in treatment planning.
Antony George Oral & Maxillofacial Pathology
Treatment
Pemphigus vulgaris
Initial high dose of systemic corticosteroids
followed by low dose if required.
Long term therapy avoided due to side effects.
Immuno-suppression, glaucoma, osteoporosis,
hyperglycemia, hypertension, peptic ulcer, weight gain.
Prednisone – 5 mg OD for 2 weeks.
Dose to be tapered before drug stoppage.
Antiseptic and analgesic dressing to relive pain.
Topical corticosteroids for prevention of relapse.
15 g for 2-4 weeks.
Combined with topical candidal cream to avoid
candida albicans infection (candidiasis).
Antony George Oral & Maxillofacial Pathology
Pemphigus vulgaris
Immuno suppressive drugs
Cyclophosphamide.
Azathioprine.
Methotrexate.
Combination of systemic corticosteroids & immuno
suppressive drugs are presently used.
Alternate days of prednisone & methotrexate.
Immunophoresis – IV administration of 8-methoxy
psoralen, followed by exposure of peripheral blood
to UV radiation.
Antony George Oral & Maxillofacial Pathology
Paraneoplastic Pemphigus
(Neoplasia induced pemphigus)
Antony George Oral & Maxillofacial Pathology
Paraneoplastic Pemphigus
Rare autoimmune mucocutaneous vesiculobullous
disorder that affects patients with underlying
neoplasm, especially
Non Hodgkin Lymphoma.
Chronic Lymphocytic Leukemia.
Poorly Differentiated Sarcomas.
Mucocutaneous lesions may develop even before
malignancy is diagnosed.
Characterized by intra-epithelial and sub-epithelial
blister formation.
Antony George Oral & Maxillofacial Pathology
Pathophyiology
Paraneoplastic Pemphigus
Lymphocytes produce cytokines and interleukin (IL) 6 due to
host response to underlying neoplasm evoking auto-immune
response.
Abnormal antibody formed cause cross reactivity with
desmosomal junction and basement membrane.
Desmoglein 1 & 3.
Desmoplakin 1 & 2.
Major bullous pemphigoid antigen 1 (BP230).
Envoplakin.
Periplakin.
Intra-epithelial & sub-epithelial blister formation.
Clinical Features
Paraneoplastic Pemphigus
Age: 60-70 yrs.
Gender: No gender predilection.
History of underlying malignant neoplasm.
Multiple polymorphous papular and pruritic
mucocutaneous lesions of sudden onset.
May resemble Lichen Planus.
Palmar and plantar bulla.
Rarely seen in pemphigus or other vesiculobullous
lesions.
Antony George Oral & Maxillofacial Pathology
Paraneoplastic Pemphigus
Multiple erythematous diffuse irregular painful
ulceration of any oral mucosal surface.
Mucosal lesion may appear earlier to skin lesions.
Hemorrhagic crusting of lips.
Similar to erythema multiforme.
70% show conjunctivitis and ocular involvement that
heal with scaring.
Vaginal & respiratory mucosa maybe involved.
Epistaxis maybe seen if nasal mucosa affected.
Paraneoplastic Pemphigus
Antony George Oral & Maxillofacial Pathology
Histopathology
Paraneoplastic Pemphigus
Intraepithelial and subepithelial clefting (split).
Acantholysis of supra basal layer.
Dyskeratosis
Deposition of keratin in stratum spinosum.
Keratin seen within bulla – diagnostic feature for
paraneoplastic pemphigus.
Spongiosis – „basket weave‟ appearance.
Vesicular nucleus.
Connective tissue show lymphocytic infiltrate and
peri-vascular inflammation.
Antony George Oral & Maxillofacial Pathology
Paraneoplastic Pemphigus
Antony George Oral & Maxillofacial Pathology
Special Investigations:
Immunofluorescence studies
Paraneoplastic Pemphigus
Direct immunofluorescence microscopy (DIF)
Weakly positive for IgG & C3 in intraepithelial region.
Linear granular deposition of immunoreactants at
basement membrane.
Indirect immunofluorescence microscopy (IIF)
Specific pattern of antibody localization to intercellular
spaces of rat urinary bladder mucosa.
Desmoglein 1 & 3.
Desmoplakin 1 & 2.
BP 230.
Envoplakin & Periplakin.
Treatment
Paraneoplastic Pemphigus
Surgical removal of malignant tumor usually
cause regression of vesiculobullous lesions.
Systemic corticosteroids in combination with
immunosuppressive drugs.
Immunophoresis – IV administration of 8-methoxy
psoralen followed by exposure of peripheral blood to
UV radiation.
Antony George Oral & Maxillofacial Pathology
Prognosis
Paraneoplastic Pemphigus
Skin lesions react faster to medication than oral
lesions – “oral lesions are 1st to show & last to go”.
Poor prognosis with 90% mortality.
Complication: dehydration, electrolyte imbalance,
malnutrition, secondary infections.
Complication of immunosuppressive therapy.
Progression of malignant disease.
Antony George Oral & Maxillofacial Pathology
Histopathological Terminology
Hyperkeratosis – increased thickness of stratum corneum.
Acanthosis – increased thickness of stratum spinosum.
Acantholysis – destruction of desmosomal cell junctions
and separation of epithelial cells from one another.
Spongiosis – intercellular edema.
Cytolysis – destruction of cells (viral infections).
Hyperkeratosis & Acanthosis Acantholysis & Spongiosis Cytolysis
Вам также может понравиться
- Bullos DiseaseДокумент4 страницыBullos DiseaseFiras HamidehОценок пока нет
- Desquamative GingivitisДокумент52 страницыDesquamative GingivitisPrathik RaiОценок пока нет
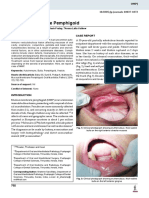
- Mucous Membrane Pemphigoid: by Student Dunya Adnan Khaled Supervision by Dr. LanaДокумент13 страницMucous Membrane Pemphigoid: by Student Dunya Adnan Khaled Supervision by Dr. LanaQueen LiveОценок пока нет
- 20 Lecture Oral Mucosa Vesiculo-Bullous DiseaseДокумент10 страниц20 Lecture Oral Mucosa Vesiculo-Bullous Diseaseمازن كريم حمودОценок пока нет
- Oral Pemphigus Vulgaris: A Case Report With Review of The LiteratureДокумент4 страницыOral Pemphigus Vulgaris: A Case Report With Review of The LiteratureDhilah Harfadhilah FakhirahОценок пока нет
- Ulcerated Lesions 5555555Документ11 страницUlcerated Lesions 5555555ربيد احمد مثنى يحيى كلية طب الاسنان - جامعة عدنОценок пока нет
- Ve Siculo Bull Ous DiseasesДокумент73 страницыVe Siculo Bull Ous DiseasesAARYAОценок пока нет
- PV 1Документ4 страницыPV 1Aing ScribdОценок пока нет
- Bacterial Infections of The Oral CavityДокумент212 страницBacterial Infections of The Oral CavitydrrakbdsОценок пока нет
- Pemphigus VulgarisДокумент3 страницыPemphigus VulgarisAdib MuntasirОценок пока нет
- Pemphigus Vulgaris: Keywords: Autoimmune Disease, Bullae, Mucous Membrane, Pemphigus VulgarisДокумент4 страницыPemphigus Vulgaris: Keywords: Autoimmune Disease, Bullae, Mucous Membrane, Pemphigus VulgarisDwiKamaswariОценок пока нет
- JCDP 23 755Документ5 страницJCDP 23 755Queen LiveОценок пока нет
- Enfermedades InmunologicasДокумент14 страницEnfermedades InmunologicasKarina OjedaОценок пока нет
- Case Report: Oral Lesions: The Clue To Diagnosis of Pemphigus VulgarisДокумент4 страницыCase Report: Oral Lesions: The Clue To Diagnosis of Pemphigus Vulgarisgilang_8899Оценок пока нет
- DR - REVATI - IMMUNE MEDIATED DISEASES OF OROFACIAL REGION - RevatiДокумент72 страницыDR - REVATI - IMMUNE MEDIATED DISEASES OF OROFACIAL REGION - RevatiNanik AndianiОценок пока нет
- Case Report: Journal of Chitwan Medical College 2020 10 (31) :91-93Документ3 страницыCase Report: Journal of Chitwan Medical College 2020 10 (31) :91-93Yeni PuspitasariОценок пока нет
- A Case Study On Pemphigus VulgarisДокумент3 страницыA Case Study On Pemphigus VulgarisAdib MuntasirОценок пока нет
- Bullous-2018 TPДокумент136 страницBullous-2018 TPMary Dominique RomoОценок пока нет
- Mucous Membrane Pemphigoid: 10.5005/jp-Journals-10037-1072Документ4 страницыMucous Membrane Pemphigoid: 10.5005/jp-Journals-10037-1072SunilОценок пока нет
- Autoimmune Mucocutaneous Blistering Diseases: Devaraju D. Vijeev Vasudevan Yashoda Devi B.K. Manjunath VДокумент7 страницAutoimmune Mucocutaneous Blistering Diseases: Devaraju D. Vijeev Vasudevan Yashoda Devi B.K. Manjunath VgadispinanditaОценок пока нет
- Pemphigus Vulgaris Confined To The Gingiva: A Case ReportДокумент16 страницPemphigus Vulgaris Confined To The Gingiva: A Case ReportAlmasulah Al-akmaliyahОценок пока нет
- Case Report Pemphigus Vulgaris As Oral Mucosal Ulcer Progressive To Skin LesionДокумент5 страницCase Report Pemphigus Vulgaris As Oral Mucosal Ulcer Progressive To Skin LesionAninda Wulan PradaniОценок пока нет
- Pemphigus Vulgaris: Keywords: Autoimmune Disease, Bullae, Mucous Membrane, Pemphigus VulgarisДокумент4 страницыPemphigus Vulgaris: Keywords: Autoimmune Disease, Bullae, Mucous Membrane, Pemphigus VulgarisSetiari DewiОценок пока нет
- PemfigusДокумент5 страницPemfigusSherlyОценок пока нет
- Vesiculobullous DiseasesДокумент48 страницVesiculobullous DiseasesAprilian PratamaОценок пока нет
- Pemphigus VulgarisДокумент21 страницаPemphigus VulgarisGina Kissey100% (1)
- Pemfigus VulgarisДокумент5 страницPemfigus VulgarisAgus LarobuОценок пока нет
- Lec 3 RD BДокумент35 страницLec 3 RD BAhmet BayraktarОценок пока нет
- Pemphigus vulgarisPPTДокумент23 страницыPemphigus vulgarisPPTSiti HanisaОценок пока нет
- Microbial Diseases of The Different Organ System SKINДокумент102 страницыMicrobial Diseases of The Different Organ System SKINBea Bianca CruzОценок пока нет
- Vesiculobullous DiseasesДокумент40 страницVesiculobullous Diseasessgoeldoc_550661200100% (1)
- Paper 1 PDFДокумент54 страницыPaper 1 PDFAliyyahОценок пока нет
- Lom Mer 2013Документ17 страницLom Mer 2013M ElmanavieanОценок пока нет
- Infections of The SkinlllДокумент7 страницInfections of The SkinlllDanessa AlavataОценок пока нет
- RKDF Dental College Bhopal: Department of PeriodonticsДокумент40 страницRKDF Dental College Bhopal: Department of Periodonticsananya saxenaОценок пока нет
- Granulomatous Lesions of Oral CavityДокумент120 страницGranulomatous Lesions of Oral CavityMadhura ShekatkarОценок пока нет
- Vesicubullous Diseases & Mucocutaneous DisordersДокумент23 страницыVesicubullous Diseases & Mucocutaneous Disordersshahlaraib001Оценок пока нет
- Mycotic Diseases and PeriodontiumДокумент43 страницыMycotic Diseases and PeriodontiumAhmed Tawfig GamalОценок пока нет
- Unit 4 BacteriologyДокумент51 страницаUnit 4 BacteriologySharmila LamisharОценок пока нет
- By:-Surbhi Jaiswal Bds 4 Year. ROLL N0. - 90Документ45 страницBy:-Surbhi Jaiswal Bds 4 Year. ROLL N0. - 90Ranjit BarОценок пока нет
- My CologyДокумент76 страницMy CologyMarielle Anne TuazonОценок пока нет
- Erythema MultiformeДокумент5 страницErythema MultiformeNicco MarantsonОценок пока нет
- Aspergilloma of The Maxillary Sinus Complicating OACДокумент3 страницыAspergilloma of The Maxillary Sinus Complicating OACabeer alrofaeyОценок пока нет
- Specific OsteomyelitisДокумент14 страницSpecific OsteomyelitisOmnia SamiОценок пока нет
- Self - Limiting Cutaneous Pemphigus Preceding The Oral Lesions - A Case Report PDFДокумент5 страницSelf - Limiting Cutaneous Pemphigus Preceding The Oral Lesions - A Case Report PDFLing Pei ChengОценок пока нет
- Eosinophilic Ulcer Wiley 2020Документ4 страницыEosinophilic Ulcer Wiley 2020Ghea AlmadeaОценок пока нет
- Precancerous Conditions of Oral CavityДокумент80 страницPrecancerous Conditions of Oral Cavitylarisabrinza12Оценок пока нет
- Endodontic MicrobiologyДокумент9 страницEndodontic MicrobiologySarah KahilОценок пока нет
- Autoimmune DiseasesДокумент43 страницыAutoimmune DiseasesAhmed NajmОценок пока нет
- PemphigusДокумент8 страницPemphiguszuqiri ChanelОценок пока нет
- Oral Pemphigus Vulgaris: A Case Report With Direct Immunofluorescence StudyДокумент4 страницыOral Pemphigus Vulgaris: A Case Report With Direct Immunofluorescence StudyYeni PuspitasariОценок пока нет
- Lec 19 DISEASES OF THE SALIVARY GLANDДокумент17 страницLec 19 DISEASES OF THE SALIVARY GLANDpxb8dhqgs9Оценок пока нет
- Bacterial InfectionsДокумент41 страницаBacterial InfectionsoladunniОценок пока нет
- Pemphigoid Vegetans in Childhood: A Case Report and Short Review of LiteratureДокумент11 страницPemphigoid Vegetans in Childhood: A Case Report and Short Review of LiteratureCata santaОценок пока нет
- Orofacial Infections in Children PedoДокумент40 страницOrofacial Infections in Children PedoFourthMolar.comОценок пока нет
- AggressiveДокумент55 страницAggressiveSaima KhanОценок пока нет
- Jurnal 1Документ5 страницJurnal 1Dzaenap UlfahОценок пока нет
- Jcedv 10 I 5 P 495Документ4 страницыJcedv 10 I 5 P 495Yohana SimanjuntakОценок пока нет
- Epstein Barr Virus (EBV) PDFДокумент33 страницыEpstein Barr Virus (EBV) PDFahmad mohammadОценок пока нет
- Break The Cycle Activity GuidesДокумент19 страницBreak The Cycle Activity GuidesJuanmiguel Ocampo Dion SchpОценок пока нет
- Advancements in The Bbutilization of Azolla Anabaena System in RelationДокумент17 страницAdvancements in The Bbutilization of Azolla Anabaena System in Relationryana_soesantieОценок пока нет
- Nitroimidazole Wps OfficeДокумент10 страницNitroimidazole Wps OfficeCamelle DiniayОценок пока нет
- How God Changes Your Brain: The Big IdeasДокумент6 страницHow God Changes Your Brain: The Big Ideasmatache vali100% (1)
- Best Supplements For ADHD and Focus Support For Kids - GNC IndiaДокумент3 страницыBest Supplements For ADHD and Focus Support For Kids - GNC IndiaTrần Thị UyênОценок пока нет
- 5AB 783651 CompleteBook R39 Jan12Документ146 страниц5AB 783651 CompleteBook R39 Jan12Gdb HasseneОценок пока нет
- Assisting For Endotracheal IntubationДокумент16 страницAssisting For Endotracheal IntubationSREEDEVI T SURESH100% (1)
- Handout On The Concept of Health and Health EducationДокумент5 страницHandout On The Concept of Health and Health Educationmomo connorОценок пока нет
- Book of Best Practices Trauma and The Role of Mental Health in Post-Conflict RecoveryДокумент383 страницыBook of Best Practices Trauma and The Role of Mental Health in Post-Conflict RecoveryDiego Salcedo AvilaОценок пока нет
- Concurrent Visit Report 7-12Документ14 страницConcurrent Visit Report 7-12Tizita ChakaОценок пока нет
- Presentation of Neurogenic Shock Within The Emergency Department - TaylorДокумент6 страницPresentation of Neurogenic Shock Within The Emergency Department - TaylorAnprtma kaunangОценок пока нет
- Sample Massage Therapy Business Plan TemplateДокумент8 страницSample Massage Therapy Business Plan Templatewealth nwaiwuОценок пока нет
- Oet ReadingДокумент118 страницOet ReadingSamia FarooqОценок пока нет
- Union Civil Protection Mechanism: More Effective, Efficient and Coherent Disaster ManagementДокумент23 страницыUnion Civil Protection Mechanism: More Effective, Efficient and Coherent Disaster ManagementCătălin Marian IvanОценок пока нет
- An Electromyographical Analysis of Sumo and Conventional Style DeadliftsДокумент8 страницAn Electromyographical Analysis of Sumo and Conventional Style DeadliftsRafael EscamillaОценок пока нет
- Tetanus - AnatomyДокумент7 страницTetanus - AnatomyJoro27Оценок пока нет
- Free Psa PDFДокумент4 страницыFree Psa PDFJimboreanu György PaulaОценок пока нет
- Management Control in Nonprofit Organizations, Fourth EditionДокумент74 страницыManagement Control in Nonprofit Organizations, Fourth EditionSUHAIRI19084488100% (1)
- Prevention and Control of Infectious Disease Act 1988Документ16 страницPrevention and Control of Infectious Disease Act 1988smuf_2Оценок пока нет
- Extended and Expanded Roles of Nurses 2Документ1 страницаExtended and Expanded Roles of Nurses 2Sivaprasad SОценок пока нет
- BMI W HFA Validated (3!24!2017)Документ151 страницаBMI W HFA Validated (3!24!2017)jeffordillasОценок пока нет
- National Library of Medicine (NLM) FY2011 Annual ReportДокумент116 страницNational Library of Medicine (NLM) FY2011 Annual ReportLJ's infoDOCKETОценок пока нет
- OpdscheduleДокумент14 страницOpdscheduleSrinidhi ChandraguthiОценок пока нет
- Chinese Medicine Eng BrochureДокумент12 страницChinese Medicine Eng BrochuretanasedanielaОценок пока нет
- Estimation of Uric Acid Levels in SerumДокумент6 страницEstimation of Uric Acid Levels in Serumvicky_law_275% (4)
- SPS and TBT MeasuresДокумент4 страницыSPS and TBT MeasuresValentina Vasquez CasallasОценок пока нет
- African National Congress: Department of Information and PublicityДокумент9 страницAfrican National Congress: Department of Information and PublicityeNCA.com100% (2)
- Aquatics AssignmentДокумент12 страницAquatics AssignmentTyrone WewpOgzОценок пока нет
- Development of A Taste-Masked Orodispersible FilmДокумент12 страницDevelopment of A Taste-Masked Orodispersible FilmKhoa DuyОценок пока нет