Академический Документы
Профессиональный Документы
Культура Документы
Cardiologia - Eletrocardiografia
Загружено:
DANIEL ALEJANDROИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Cardiologia - Eletrocardiografia
Загружено:
DANIEL ALEJANDROАвторское право:
Доступные форматы
VetGo Cardiology
January 10, 2005
CLINICAL CARDIOLOGY CONCEPTS
for the dog and cat
Michael R. O'Grady, DVM, MSc, Diplomate ACVIM (Cardiology)
M. Lynne O'Sullivan, DVM, DVSc, Diplomate ACVIM (Cardiology)
Contents Electrocardiology
General
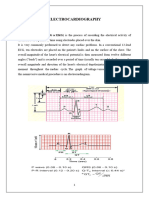
1 What is a P wave; what electrocardiographic event does this represent?
P amp = amplitude of the P wave; P dur = duration of the P wave; PR int = PR interval; R amp = amplitude of the R wave; QRS
dur = duration of the QRS complex; QT int = QT interval; T amp = amplitude of the T wave.
The P wave is the electrocardiographic representation of electrical activation of the atrial myocardium.
The amplitude measurement of the P wave depends on the calibration pulse (how many mm = 1 mv).
The duration measurement of the P wave depends on the paper speed (how many msec = 1 mm).
top Electrocardiology: General
2 What is the PR interval; what is the significance of the PR interval?
P dur = duration of the P wave; PR int = PR interval; QRS dur = duration of the QRS complex; QT int = QT interval.
The PR interval is the electrocardiographic representation of the delay in electrical activation of the ventricles after sino-atrial nodal
discharge. This interval is mainly a result of slow conduction through the atrio-ventricular node.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (1 of 40)10/1/2005 15:28:51
VetGo Cardiology
The duration measurement of the PR interval depends on the paper speed (how many msec = 1 mm).
top Electrocardiology: General
3 How are a Q, R, S, and QS different?
For a wave to be defined as a Q wave it must fullfil the following criteria:
a. It must be a negative deflection.
b. It must be the first deflection of the QRS complex.
c. It must be followed by a R wave.
Thus there can be only one Q wave per QRS complex.
For a wave to be defined as a R wave it must fullfil the following criteria:
a. It must be a positive deflection. All positive deflections are R waves and only R waves. There can be several R waves per
QRS complex.
For a wave to be defined as a S wave it must fulfil the following criteria:
a. It must be a negative deflection.
b. It must follow a R wave.
There can be several S waves per QRS complex.
For a wave to be defined as a QS wave it must fulfil the following criteria:
a. It must be a negative deflection.
b. There must be no R wave in the QRS complex.
Therefore it describes a QRS complex with only one deflection and this deflection is negative.
Comment: It should be noted that a QRS complex may thus consist of only an R wave, or only of RS waves, or only of QR waves,
etc.
top Electrocardiology: General
4 What is the significance of the QRS complex?
The QRS complex is the electrocardiographic expression of the electrical activation of the ventricular myocardium.
5. What is a T wave; what is the significance of a T wave?
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (2 of 40)10/1/2005 15:28:51
VetGo Cardiology
P amp = amplitude of the P wave; R amp = amplitude of the R wave; T amp = amplitude of the T wave.
The T wave is the electrocardiographic expression of repolarization of the ventricular myocardium.
In domestic animals patient cooperation is usually poor and therefore movement artifact is frequently encountered on the
electrocardiogram. These deflections can usually be diagnosed as artifact as opposed to a QRS complex because of the absence
of a T wave.
Therefore for any deflection on an electrocardiogram to be considered as a "beat" it must have a repolarization wave (T wave).
top Electrocardiology: General
5 What is the significance of a positive deflection in a lead; of a negative deflection in a lead?
An electrical lead used to examine the heart on the EKG can be described in terms of a negative pole and a positive pole.
As a wave of electrical depolarization moves parallel to the direction of a lead, if it moves towards the positive pole of the lead a
positive deflection occurs on the EKG, if it moves toward the negative pole of the lead a negative deflection occurs on the EKG.
top Electrocardiology: General
6 What is the frontal plane diagram?
The frontal, left sagittal, and transverse (also called horizontal) planes are illustrated in the cat. Leads I, II, III, aVR, aVL, and aVF
are frontal plane leads. Leads V1, V2, V3, V4, V5, V6, and V10 are horizontal (or transverse) plane leads.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (3 of 40)10/1/2005 15:28:51
VetGo Cardiology
In the illustration, a cross-section of the heart is superimpsed on the frontal plane diagram. The arrow
heads point toward the positive pole of each lead.
The frontal plane diagram shows the relationship of the 6 leads in the frontal plane. This diagram includes the angles in the frontal
plane and the direction of each lead with its negative and positive pole.
The frontal plane corresponds to the radiographic V/D or D/V view of the heart.
top Electrocardiology: General
7 What is the significance of the MEA of the QRS complex?
The mean electrical axis (MEA) of the QRS complex is usually determined in the frontal plane. This represents the direction
(expressed in degrees) of the net or average direction of activation of the entire ventricular myocardium.
There are three common methods of calculating the MEA in the frontal plane. All of these are merely approximations. In-dividuals
should use which ever method they feel comfortable with.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (4 of 40)10/1/2005 15:28:51
VetGo Cardiology
a. The Vector Method: Using leads I, II or III and the frontal plane diagram, calculate the algebraic sum of the QRS deflections
in any two leads (this does not include the T wave). Let us for example consider using the complexes of leads I and III. Plot
the algebraic sum of lead I on its axis on the frontal plane diagram. Similarly plot the algebraic sum of the QRS complex of
lead III on its axis on the frontal plane diagram. Draw lines perpendicular to the their respective axes at the points plotted
on the lead axes I and III. Note the point of intersection of these two perpendicular lines. A line drawn from this intersect to
the center of the diagram describes the MEA. See the example below:
b. The Isoelectric Method: Find the lead, of the 6 leads in the frontal plane, that is the most isoelectric (the algebraic sum of all
the deflections of the QRS in that lead comes closest to zero) (again omit the T wave). Next, find the lead on the frontal
plane diagram that is perpendicular to this isoelectric lead (the MEA will lie along this perpendicular lead). Note the net
polarity of the complexes in this perpendicular lead. If the net polarity of these complexes is positive, the MEA is toward the
positive pole of the perpendicular lead; if the net polarity of these complexes is negative, the MEA is toward the negative
pole of the perpendicular lead.
c. The Largest Net Deflection Method: Find the lead, of the 6 leads in the frontal plane, that contains the QRS complex with
the largest net deflection (the algebraic sum of all the deflections of the QRS in that lead is the largest value [positive or
negative]). The MEA will lie along this lead. If this largest net deflection is positive, the MEA is toward the positive pole of
this lead with the largest net deflection; if this largest net deflection is negative, the MEA is toward the negative pole of this
lead with the largest net deflection.
top Electrocardiology: General
8 Why should I bother determining the MEA?
Determining the MEA is very useful to identify right ventricular enlargement. A MEA of 100 to -75 degrees suggests right
ventricular enlargement.
The MEA also helps determine the nature of aberrant conduction disturbances (so called bundle branch block).
top Electrocardiology: General
9 What is a sinus rhythm?
A sinus rhythm is a rhythm which originates in and is controlled by the sino-atrial node. This rhythm is the normal cardiac rhythm in
all domestic animals. To determine if a rhythm is sinus or not based on the EKG requires the following criteria:
1. There is a P wave for every QRS complex.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (5 of 40)10/1/2005 15:28:51
VetGo Cardiology
2. The PR interval is relatively constant especially if the R wave to R wave interval varies.
3. The P wave is positive in lead II.
Comments: In that the P wave doesn't indicate sino-atrial activation but the result of sino-atrial activation, we can only infer the
normalcy of sino-atrial activity from the routine EKG.
top Electrocardiology: General
10 What is a sinus arrhythmia?
A sinus arrhythmia is an irregular ventricular rhythm which is of sino-atrial origin. On the EKG, the QRS to QRS interval varies and
there is a P wave for every QRS complex.
Example 1: Sinus Arrhythmia and Wandering Atrial Pacemaker in the Dog
Etiology:
● most cases of sinus arrhythmia are phasic and associated with respiration
● the rate increases with inspiration and decreases with expiration
● associated with relatively slow rates
● the sinus arrhythmia of respiratory origin occurs due to the influence of vagal tone
Individuals with respiratory disease tend to have augmented sinus arrhythmia.
Consequences:
● This is a normal finding particularly in fit individuals. An irregular cardiac rhythm may have been detected on an individual
during physical examination. The finding of sinus arrhythmia on EKG confirms the presence of an arrhythmia but also
establishes that this irregularity is non pathologic.
● It is important to distinguish this rhythm from that of atrial premature contractions.
Treatment:
● none required
Example 2: Sinus Arrhythmia and Wandering Atrial Pacemaker in the Dog
10 fine lines vertically = 1mV; 25 fine lines horizontally = 1 sec
top Electrocardiology: General
11 What is a wandering atrial pacemaker?
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (6 of 40)10/1/2005 15:28:51
VetGo Cardiology
EKG Findings:
● variable amplitude and/or morphology of the P wave
● the change in P wave amplitude and / or morphology tends to gradually shift from normalcy
● associated with sinus arrhythmia
● the heart rate is in the mid to low normal range
Example of Wandering Atrial Pacemaker in the Dog
10 fine lines vertically = 1 mV; 25 fine lines horizontally = 1 second
Etiology:
● associated with increased respiratory effort
● usually a normal finding
● occurs due to increased vagal tone
Consequences:
● normal
● usually occurs in association with sinus arrhythmia
● in the face of a marked sinus arrhythmia, altered P wave morphology can be misinterpreted as atrial premature beats
Treatment:
● none required
Chamber Enlargement
top Electrocardiology: Chamber Enlargement
12 Approach to the EKG to determine chamber enlargement
1. Determine the ventricular rate - note paper speed.
2. Determine the atrial rate - note paper speed.
3. To assess atrial enlargement:
● measure P wave duration in lead II - note paper speed
● measure P wave amplitude in lead II - note calibration
4. To assess ventricular enlargement:
● measure QRS duration in lead II - note paper speed
● measure R wave amplitude in lead II - note calibration
● examine for S waves in leads I, II, III
● examine and measure S wave amplitude in lead V3 - note calibration
● determine MEA in frontal plane
● examine ST segment in lead II
top Electrocardiology: Chamber Enlargement
13 What is the significance of a P wave that is too tall or too wide?
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (7 of 40)10/1/2005 15:28:51
VetGo Cardiology
Normal Too Tall Too Wide
a. Electrocardiographic criteria of left atrial enlargement is a P wave that is too wide in lead II.
● dog: P > 0.04 sec
● large dog: P > 0.045 sec
● cat: P > 0.04 sec
b. Electrocardiographic criteria of right atrial enlargement is a P wave that is too high in lead II.
● dog: P > 0.4 mv
● cat: P > 0.2 mv
c. Electrocardiographic criteria of biatrial enlargement is a P wave that is too tall and too wide in lead II.
Comments:
● in the presence of a wandering pacemaker, it is inappropriate to measure P wave amplitude (just omit this measurement)
● all measurements are made in lead II, usually at 50 mm/sec paper speed
● the sensitivity and specificity of the EKG criteria for atrial enlargement are low
top Electrocardiology: Chamber Enlargement
14 What are the electrocardiographic criteria of left ventricular enlargement?
a. Dog:
Example of Left Ventricular Enlargement in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (8 of 40)10/1/2005 15:28:51
VetGo Cardiology
top Electrocardiology: Chamber Enlargement
15 What are the electrocardiographic criteria of left ventricular concentric hypertrophy?
● It is my experience that the EKG is usually completely normal in cases of left ventricular concentric hypertrophy
● Tilley and others suggest that a shift in the MEA to the left occurs in this disorder. This has not been substantiated.
● The R wave amplitude in lead II may be increased.
● The QRS duration in lead II may be increased.
top Electrocardiology: Chamber Enlargement
16 What is the electrocardiographic evidence of right ventricular enlargement?
EKG Findings:
a) Dog:
1. Presence of an S wave in leads I, II, III.
2. MEA in the frontal plane shifted to the right (pointing to the right ventricle): 100o to - 75o
3. Deep S wave in lead V3; S = 0.7 mv
4. SR in lead V3
● if all 4 criteria are present, there is strong evidence of right ventricular enlargement
● the presence of any 2 criteria is still good evidence of right ventricular enlargement
● even the presence of 1 criteria is strongly suggestive of right ventricular enlargement
Comments:
1. V3 is a horizontal plane lead. It is useful to help detect right ventricular enlargement. At times the frontal plane may show
QRS complexes that are isoelectric in all 6 leads, in such cases a V3 trace is helpful. At times the criteria for right ventricular
enlargement may only be present in V3.
2. The precordial leads are often the most useful leads to identify the presence of P waves. The identification of P waves is
the most crucial step in the identification of most dysrhythmias as will be discussed later (see diagram below).
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (9 of 40)10/1/2005 15:28:51
VetGo Cardiology
Transverse Section At The 6th Intercostal Space
Showing The Position Of The Horizontal Plane Leads
b) Cat:
1. MEA in the frontal plane shifted to the right (points to the right ventricle):
● 160° to -75°
Example of Right Ventricular Enlargement in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (10 of 40)10/1/2005 15:28:51
VetGo Cardiology
Normal ECG Parameters
top Electrocardiology: Normal ECG Parameters
17 Normal ECG Diagram
I. Diagram of Normal EKG with Location of Routine Measurements
P amp = amplitude of the P wave; P dur = duration of the P wave; PR int = PR interval; R amp = amplitude of the R wave; QRS
dur = duration of the QRS complex; QT int = QT interval; T amp = amplitude of the T wave.
top Electrocardiology: Normal ECG Parameters
18 Normal Small Animal Electrocardiographic Parameters
Normal Electrocardiographic Parameters in the Dog and Cat
Parameter Canine Feline
Adults: 70-160
Heart Rate (beats per minute) Toy Breeds: up to 180 160-240
Puppies: up to 220
Normal sinus rhythm
Normal sinus
rhythm
Rhythm Sinus arrhythmia
Sinus tachycardia
Wandering atrial pacemaker
Intervals (seconds)
P < 0.04 < 0.04
PR 0.06 to 0.13 0.05 to 0.09
< 20 kg: < 0.05
QRS > 20 kg: < 0.06 < 0.04
Giant breeds: < 0.065
QT 0.15 to 0.25 0.12 to 0.18
Amplitudes (mV) in lead II
P < 0.4 < 0.2
< 20 kg: < 2.5
R < 0.9
> 20 kg: < 3.0
SV3 0.8
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (11 of 40)10/1/2005 15:28:51
VetGo Cardiology
MEAf +40° to +100° -5° to +160°
Criteria for Chamber Enlargement: Summary
Chambers: ECG Parameter: Body Wt Canine Feline
Left Atrium PII duration >0.04 s >0.04 s
>0.4 >0.2
Right Atrium PII amplitude
mv mv
<20 kg >2.5 mv
Left Ventricle RII amplitude >3.0 >0.9 mv
>20 kg
mv
Pattern of SI, SII, & SIII Present
MEA points to Rt Vent Present Present
Right Ventricle >0.7
S in V3
mv
S in V3 > R in V3 Present
Dysrhythmias
top Electrocardiology: Dysrhythmias
19 Approach to the EKG to assess dysrhythmias.
Try the diagnostic alogrithm here (a chart form is here).
1. Determine the ventricular rate - note paper speed.
2. Determine the atrial rate.
3. Are P and QRS associated?
❍ same rate
❍ reasonable PR interval
❍ consistent PR interval
4. Determine PR interval - note paper speed
❍ does it vary?
5. Are there any P waves that are not followed by a QRS complex?
6. Are there any QRS complexes with no P waves?
7. Determine the width of the QRS complexes - note paper speed.
8. Is the rhythm regular or irregular?
9. Any premature beats? - note morphology
❍ note duration
10. Are the P waves positive in lead II?
11. Are the QRS complexes of normal morphology?
The critical feature with most dysrhythmias is to find the P waves (if present); note if the atrial rate is equal to, less than, or greater
than the ventricular rate, and is there any relationship between the P waves and the QRS complexes.
Bradycardias
top Electrocardiology: Bradycardias
20 What is bradycardia?
Bradycardia is present when the ventricular rate is too slow:
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (12 of 40)10/1/2005 15:28:51
VetGo Cardiology
● dog (< 20 kg) = < 70 bpm
● dog (> 20 kg) = < 60 bpm
● cat = < 100 bpm
top Electrocardiology: Bradycardias
21 What is sinus bradycardia?
This refers to a sinus rhythm wherein the sino-atrial rate is bradycardic.
Example of Sinus Bradycardia in the Dog
Etiology:
1. Enhanced parasympathetic tone as with:
❍ Increased inspiratory effort as with respiratory disease.
❍ Gastric irritation.
❍ Increased CSF pressure.
2. Hypothyroidism
3. Hypothermia
4. Hyperkalemia
5. Hypoglycemia
6. Drug therapy
Consequence:
1. profound bradycardia will cause weakness, hypotension, syncope
Therapy:
1. Treat the underlying cause of the bradycardia
2. Atropine will abolish the bradycardia (atropine - 0.04 mg/kg IV)
top Electrocardiology: Bradycardias
22 What is heart block?
Heart block refers to a group of disorders characterized by variable conduction from the atria to the ventricles.
Heart block can be classified as
● 1st degree Heart Block
● 2nd degree Heart Block
● 3rd degree Heart Block
top Electrocardiology: Bradycardias
23 What is 1st degree Heart Block?
EKG Findings:
1. Prolonged PR interval
❍ Dog - PR 0.13 sec
❍ Cat - PR 0.09 sec.
2. P wave for every QRS and QRS for every P wave.
Etiology:
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (13 of 40)10/1/2005 15:28:51
VetGo Cardiology
1. This disorder is due to prolonged conduction across the atrio-ventricular node.
2. Associated with disorders that cause increase parasympathetic tone.
3. May be normal.
4. PR increases with age and lengthens with rapid HR.
5. Drug therapy (digitalis, beta blocker, calcium channel blocker, procainamide, quinidin-e).
6. Hyperkalemia.
Consequences:
● causes no hemodynamic abnormality
Treatment:
● none required
Example of First Degree Heart Block in the Dog
10 fine lines vertically = 1 mv. (1cm = 1 mv); 50 fine lines horizontally = 1 sec. (50 mm/sec).
top Electrocardiology: Bradycardias
24 What is 2nd degree Heart Block?
General Remarks:
Due to failure of the sino-atrial impulse after activating the atrial myocardium to activate the ventricular myocardium.
Depending on the location of the abnormality it may be classified as:
1. Mobitz type 1 (Wenckebach)
2. Mobitz type 2
Mobitz type 1:
This trace is of a dog; 10 fine lines vertically = 1 mv; 25 fine lines horizontally = 1 sec.
1. EKG Findings:
1.
P wave that is not followed by a QRS complex
2.
QRS complex is usually of normal duration and morphology
3.
the PR interval progressively prolongs just prior to blocked beat
4.
When comparing the PR interval of the beat immediately preceeding the blocked beat, with that of the beat
immediately following the blocked beat, the PR interval of the preceeding beat is longer than the PR interval of the
following beat.
2. Etiology:
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (14 of 40)10/1/2005 15:28:51
VetGo Cardiology
1. due to failure of the sino-atrial impulse to propagate through the atrio-ventricular node
2. excessive vagal tone can cause this abnormality
3. may be normal in some dogs
4. drug therapy (digitalis)
3. Consequences:
1. very rarely is the heart rate sufficiently reduced to cause any reduction in cardiac output.
2. this rhythm disturbance is important to distinguish from second degree heart block of the Mobitz type II variety which
is potentially much more severe.
4. Treatment:
1. none required
2. atropine responsive
Mobitz Type 2:
(10 fine lines vertically = 1 mv; 25 fine lines horizontally = 1 sec.)
1. EKG Findings:
1. P wave that is not followed by a QRS complex
2. often has a wide QRS complex
3. PR interval of constant duration
4. may have multiple P waves that are not followed by QRS complexes (ie. 2:1, 3:1, 4:1, etc. block)
2. Etiology:
1. due to failure of the sino-atrial impulse to propagate through the His bundle or bundle branches
2. associated with organic disease of the His bundle or bundle branches. This may be in the form of an ischemic area,
scar, infection with necrosis, neoplasia or granuloma
3. Consequences:
1. evidence of reduced cardiac output may occur if the ventricular rate is substantially reduced:
■ dog with HR <40
■ cat with HR <60
4. Treatment:
1. usually not responsive to atropine, glycopyrrolate
2. the ventricular rate can usually be increased with intravenous isoproterenol
3. unless the ventricular rate is slow, no treatment is required
4. permanent pacemaker implantation
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (15 of 40)10/1/2005 15:28:51
VetGo Cardiology
Comments:
1. Mobitz Type 2 2nd degree Heart Block is considered an important signal warning of the potential progression to 3rd degree
Heart Block which requires immediate treatment.
2. Therefore it is important to distinguish between Mobitz Type 1 and Type 2 because Type 1 warrants no concern but Type 2
warrants continued monitoring to detect the onset of 3rd degree Heart Block
Dosages:
1. Atropine:
❍ dog: 0.01-0.04 mg/kg (IV,IM); 0.02-0.04 mg/kg TID- QID (SQ, PO)
❍ cat: 0.02-0.04 mg/kg (IV,IM), QID (SQ)
2. Glycopyrrolate:
❍ dog: 0.005-0.01 mg/kg (IV,IM); 0.01-0.02 mg/kg BID-TID (SQ)
❍ cat: 0.005-0.01 mg/kg (IV,IM); 0.01-0.02 mg/kg (SQ)
3. Isoproterenol:
❍ dog: 0.04-0.09 ug/kg/min (CRI)
❍ cat: 0.04-0.09 ug/kg/min (CRI)
4. Terbutaline:
❍ dog: 2-5 mg BID (PO)
❍ cat: unknown
top Electrocardiology: Bradycardias
25 What is 3rd degree Heart Block?
Example of Third Degree Heart Block in the Dog
(10 fine lines vertically = 1 mv; 25 fine lines horizontally = 1 sec.)
EKG Findings:
1. An atrial rate and rhythm that occurs is independent of a much slower ventricular rhythm.
2. The atrial rate tends to be fast, and regular.
3. The ventricular rhythm is regular and much slower than the atrial rhythm.
❍ dog - ventricular rate approx. 40 - 50 bpm
❍ cat - ventricular rate approx. 90 - 110 bpm
4. The resultant ventricular activation is initiated from latent, subsidiary automatic pacemaker foci. The resultant rhythm is
referred to as an escape rhythm. If the escape ventricular activation occurs from a high ventricular focus, the QRS
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (16 of 40)10/1/2005 15:28:51
VetGo Cardiology
morphology may look relatively normal. Usually the QRS morphology tends however to be very abnormal.
Etiology:
1. Due to the same etiologies as for 2nd degree Heart Block Mobitz Type 2.
Consequences:
1. Can cause all the signs of reduced cardiac output (see #1 and#2)
Treatment:
1. Atropine is usually not effective.
2. I.V. isoproterenol may increase the ventricular rate.
3. Pacemaker therapy is usually the only effective therapy.
4. Evaluation and treatment for hypothyroidism may be rewarding.
This could be caused by hyperthyroidism.
Dosage:
1. Isoproterenol:
❍ dog: 0.04-0.09 ug/kg/min (CRI)
❍ cat: 0.04-0.09 ug/kg/min (CRI)
2. Terbutaline:
❍ dog: 2-5 mg BID (PO)
❍ cat: unknown
top Electrocardiology: Bradycardias
26 What is Sick Sinus Syndrome?
Sick Sinus Syndrome refers to a group of disorders involving the sino-atrial node usually with further involvement of the atrio-
ventricular node, His bundle and/or bundle branches. Frequently, multiple areas of the conduction system are involved.
Paroxysms of sinus and supraventricular trachycardia may be interspersed among periods of bradycardia and asystole.
Example of Sick Sinus Syndrome in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (17 of 40)10/1/2005 15:28:51
VetGo Cardiology
ECG findings (may include any of the following):
1. A slow and irregular atrial rate (impaired sino-atrial activity), severe sinus bradycardia, or long pauses of asystole with no
escape beats.
2. Evidence of impaired atrio-ventricular conduction such that 2nd degree heart block is prevalent.
3. The ventricular rate is very slow and irregular.
❍ Ventricular escape beats are common.
4. Incomplete 3rd degree heart block may be present.
5. Paroxysms of supraventricular tachycardia alternating with severe sinus bradycardia.
Etiology:
1. May have SA nodal artery disease -- ischemia.
2. Fibrosis of SA node with partial involvement of the rest of conduction system.
3. Possibly inherited in some breeds as Miniature Schnauzer.
4. Usually idiopathic.
Consequences:
1. periods of ventricular standstill are associated with syncope
2. The paroxysms of supraventricular tachycardia may also cause syncope
Treatment:
1. Atropine is usually not effective.
2. I.V. isoproterenol may accelerate the ventricular rate.
3. Myocardial pacing (permanent pacemaker) is the only definitive therapy.
Dosages:
1. Atropine:
❍ dog: 0.01-0.04 mg/kg (IV,IM); 0.02-0.04 mg/kg TID-QID (SQ,PO)
❍ cat: 0.02-0.04 mg/kg (IV,IM), QID (SQ)
2. Isoproterenol:
❍ dog: 0.04-0.09 ug/kg/min (CRI)
❍ cat: 0.04-0.09 ug/kg/min (CRI)
Comments: Certain breeds are predisposed:
Miniature Schnauzers, especially females
Tachycardias
top Electrocardiology: Tachycardias
27 What is sinus tachycardia?
Example of Sinus Tachycardia in the Dog
EKG Findings:
1. It is a sinus rhythm with an increased ventricular rate.
❍ Dog (<20 kg) with heart rate 180 bpm
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (18 of 40)10/1/2005 15:28:51
VetGo Cardiology
❍ Dog (20 kg) with heart rate 160 bpm
❍ Puppies with heart rate 220 bpm
❍ Cat with heart rate 240 bpm
Etiology:
1. Pain
2. Fever
3. Anemia
4. Reduced cardiac output
5. Hyperthyroidism
6. Excitement
Consequences:
1. as per tachycardia (see #1)
Treatment:
1. none required
2. treat the underlying process
top Electrocardiology: Tachycardias
28 What are supraventricular premature beats?
Example of Supraventricular Premature Beats in the Dog
EKG Findings:
1. Premature beats.
2. The morphology of these beats usually looks very similar to the sinus beats, see #1).
3. The duration of the QRS complexes are usually normal.
Etiology:
1. These beats may originate within ectopic foci in the atria (so called atrial premature beats) or they may originate in the peri-
A-V nodal tissue (so called junctional premature beats).
2. The causes of both types of supraventricular beats are identical:
❍ due to disorders that result in enlargement of the atria
❍ A-V valve insufficiency
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (19 of 40)10/1/2005 15:28:51
VetGo Cardiology
❍ due to ischemic foci in the atria
❍ drugs (digitalis, anesthetics)
Consequences:
1. Several isolated premature beats are of no hemodynamic significance.
2. However, when enough of these beats are present, a marked reduction in cardiac output may result (due to a loss of atrial
induced ventricular filling and high heart rate).
Treatment:
1. Several isolated beats do not warrant therapy. However, such individuals should be frequently monitored for exacerbation of
their rhythm disturbance. In addition, attention should be directed toward identification and management of the underlying
disorder.
2. Criteria for therapy include:
1. if the animal is symptomatic with this disorder
2. if paroxysms of sustained tachycardia develop such as a burst lasting greater than 60 sec.
3. Drugs commonly used include
1. digoxin
2. beta blocker therapy:
■ propranolol
■ metoprolol
■ atenolol
3. calcium channel blocker therapy:
■ diltiazem
Dosages:
1. Digoxin:
■ dog: 0.22 mg/m2 BID (PO)
■ cat: 1/4 of 0.125 mg (PO) q 48h - SID
2. Propranolol:
■ dog: 0.21-1.0 mg/kg TID (PO); 0.04-0.06 mg/kg (IV) slowly
■ cat: 0.21-1.0 mg/kg BID-TID (PO); 0.04 mg/kg (IV) slowly
3. Metoprolol:
■ dog: 0.5-1 mg/kg TID (PO)
■ cat: 2-15 mg TID (PO)
4. Atenolol:
■ dog: 5-12.5 mg SID (PO)
■ cat: 5-12.5 mg SID (PO)
5. Diltiazem:
■ dog: 1-2 mg/kg TID (PO)
■ cat:
■ cardizem: 1-2 mg/kg TID (PO)
■ cardizem CD: 10 mg/kg SID (PO)
Comment: Although propranolol is the best known beta blocker in veterinary medicine, it has drawbacks in its combined beta 1 and
beta 2 blocking activity. We should attempt to use beta-1 selective beta blocker such as metoprolol and atenolol. As well the Ca
channel blockers, such as diltiazem, may be particularly useful in these disorders.
Efforts to increase the parasympathetic tone and thereby reduce A-V nodal conduction and slow the ventricular response is useful
to assist in detecting atrial activity (see P waves on EKG). This assists in the differentiation of supraventricular ectopia and
ventricular ectopia. This can be accomplished by:
1. Vagal maneuvers:
❍ Ocular pressure.
❍ Carotid sinus massage.
2. Parasympathominetic agents:
❍ Edrophonium chloride.
3. Reflex induced increase in vagal tone:
❍ Phenylephrine.
top Electrocardiology: Tachycardias
29 What is supraventricular tachycardia?
Example of Supraventricular Tachycardia in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (20 of 40)10/1/2005 15:28:51
VetGo Cardiology
EKG Findings:
1. A string of at least 4 supraventricular premature beats.
2. Often occurs as paroxysms (bursts).
Etiology:
1. The same as for supraventricular premature beats (see #1).
Consequence:
1. Paroxysms of supraventricular tachycardia can result in syncope and heart failure (see #2).
Treatment:
1. As for supraventricular premature beats (see #3).
top Electrocardiology: Tachycardias
30 What is atrial fibrillation?
General Remarks:
Atrial fibrilation is a supraventricular disorder associated with many microfoci of atrial myocardium acting as ectopic foci and
activating their small adjacent atrial myocardium. Each of these ectopic microfoci are acting relatively independently. Only the
ectopic foci close to the A-V node successfully penetrate the A-V node to activate the ventricles.
There is no coordinated atrial contraction in this disorder. The ventricular myocardium is activated at a very fast rate and at irregular
intervals.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (21 of 40)10/1/2005 15:28:51
VetGo Cardiology
EKG Findings:
1. Very rapid and irregular ventricular rhythm.
2. No distinct P waves; at times the baseline may show very fine baseline undulations which are called fibrillation waves.
Frequently these fibrillation waves are not apparent.
3. The QRS complexes are supraventricular in origin thus the QRS complexes tend to look of normal morphology.
Example of Atrial Fibrillation in the Dog
Another Example of Atrial Fibrillation in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (22 of 40)10/1/2005 15:28:51
VetGo Cardiology
Comments:
The hallmark EKG findings are the presence of an irregular rhythm and absence of P waves. As the heart rate becomes very rapid,
the rhythm approaches a regular rhythm; however, a slight irregularity remains present. Although the heart rate is usually rapid it
can be slow if:
1. a giant breed of dog is involved
2. A-V nodal disease co-exists
3. digitalis, beta-blocker, or calcium channel blocker therapy is on board
In that underlying ventricular myocardial disease is usually present, the morphology of the QRS is often wide and ST segment
changes may be present (see #1, #2, and#3).
Etiology:
1. Due to a very high number of microfoci in the atria that are all firing independently. They are competing to activate the A-V
node.
2. Due to disorders associated with atrial dilation.
1. A-V valvular insufficiency
2. Cardiomyopathy
3. Congenital heart disease
3. May occur in the absence of organic heart disease (usually giant breed dogs). These individuals usually have slow to
normal ventricular rates.
Consequence:
1. The rapid ventricular rhythm results in a fall in cardiac output due to excessive heart rate.
2. Cardiac output also falls due to a loss of atrial contraction. At rapid sinus rates, the atrial component to ventricular filling can
account for up to 30% of ventricular filling. At slower rates, the atria contribute relatively little to ventricular filling.
3. The rapid heart rates also result in an increase in myocardial oxygen consumption. This can result in more myocardial
hypoxia which causes a reduction in inotropy and exacerbation of dysrhythmias.
Treatment:
Goals of therapy:
1. Convert the rhythm to a sinus rhythm.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (23 of 40)10/1/2005 15:28:51
VetGo Cardiology
❍ although DC countershock cardioversion is possible, most individuals revert immediately back to atrial fibrillation
2. Slow the rhythm.
❍ reduce the tachycardic effect on cardiac output
❍ reduce the effect of loss of atrial filling by slowing the rate:
❍ digitalis - digoxin
❍ beta blockers - propranolol, metoprolol, atenolol
❍ calcium channel blockers - preliminary evidence suggests that diltiazem is the drug of choice to slow the heart rate
in this disorder.
Comments:
● dogs with cardiomyopathy may be relatively asymptomatic until the development of atrial fibrillation
Dosages:
1. Digoxin:
❍ dog: 0.22mg/m2 BID (PO)
❍ cat: 1/4 of 0.125 mg (PO) q 48h SID
2. Propranolol:
❍ dog: 0.21-1.0 mg/kg TID (PO); 0.04-0.06 mg/kg (IV) slowly
❍ cat: 0.21-1.0 mg/kg BID - TID (PO); 0.04 mg/kg (IV) slowly
3. Metoprolol:
❍ dog: 0.5-1 mg/kg TID (PO)
❍ cat: 2-15 mg TID (PO)
4. Atenolol:
❍ dog: 5-12.5 mg SID (PO)
❍ cat: 5-12.5 mg SID-BID (PO)
5. Calcium channel blockers:
❍ Diltiazem:
❍ dog: 1.0-2.0 mg/kg TID (PO)
❍ cat:
❍ Cardizem: 1.0-2.0 mg/kg SID-BID (PO)
❍ Cardizem CD: 10 mg/kg SID (PO)
Comments:
● Although propranolol is the best known beta blocker in veterinary medicine, it has drawbacks in its combined beta 1 and
beta 2 blocking activity. We should attempt to use beta-1 selective beta blockers such as metoprolol and atenolol.
● The conventional mode of therapy for symptomatic atrial fibrillation consisted of:
❍ start on digoxin
❍ start propronolol after 24 hours of digoxin.
● The dose of propranolol is begun at about 1/4 mg/kg TID (PO) and increased daily by an increment of 10 mg TID until 1 mg/
kg TID is reached.
● Work by Dr. Robert Hamlin suggests that the use of diltiazem alone is 3 times more effective than this conventional mode of
therapy.
● Not withstanding the work of Dr. Hamlin, beta blockers may have the additional ability to retard the progression of
congestive heart failure (see #4). Calcium channel blockers do not have this trait.
● I currently recommend using beta blockers and not calcium channel blockers to slow the heart rate as a first choice
● Carvedilol may also have a role here.
● Sotalol may have a role here.
top Electrocardiology: Tachycardias
31 What are ventricular premature contractions?
Example of Ventricular Premature Contractions
This lead II trace is of a dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (24 of 40)10/1/2005 15:28:51
VetGo Cardiology
EKG Findings:
1. These are premature beats.
2. The QRS complexes are usually wide and bizarre.
3. If several ectopic foci are present, the morphology of the QRS will vary with each focus (multi-form VPC's).
4. VPC's may occur as fusion and as interpolated beats. More commonly VPCs are accompanied with a pause that follows
VPCs.
5. A fusion beat is a QRS with a morphology that is neither identical to the sinus QRS, nor to a typical VPC. It is also a QRS
which occurs on time (i.e. it is not premature). It represents a fortuitous situation wherein part of the ventricular mass was
depolarized as a result of the sinus beat and the remainder of the ventricular mass was depolarized as a result of the
ectopic ventricular focus. Example of a fusion beat
6. An interpolated QRS is a special form of VPC wherein the presence of the VPC did not interrupt the underlying sinus
rhythm.
7. As most VPCs are accompanied by a pause or delay prior to the onset of the next sinus beat, a time measurement that
includes the pause can be used to discriminate between VPCs and SVPCs. For a representation please see diagram under
question 33.
Etiology:
1. Associated with ventricular concentric hypertrophy or eccentric hypertrophy.
2. Associated with hypoxemic states as anemia, gastric dilation volvulus, heart failure.
3. Associated with acidosis.
4. Associated with drugs as digitalis, barbiturates, antiarrhythmic agents.
Consequence:
1. If enough premature beats are present, cardiac output may fall (dysynergy of contraction).
2. May predispose to ventricular fibrillation.
Treatment:
1. Lidocaine:
❍ dog: 2-4 mg/kg slow (IV), repeat 10 min. to maximum of 8 mg/kg; 25-75 ug/kg/min (CRI)
❍ cat: 0.25-1.0 mg/kg slow (IV) over 5 minutes
2. Oral lidocaine analogs:
❍ Tocainide:
■ dog: 5-10 mg/kg TID-QID (PO); Dr. Hamlin suggests 25 mg/kg QID (PO)
■ cat: undetermined
❍ Mexiletine:
■ dog: 2-5 mg/kg BID-TID (PO)
■ cat: undetermined
3. Procainimide:
❍ dog: 6-8 mg/kg (IV) over 5 min; 25-40 ug/kg/min (CRI); 8-20 mg/kg q 4-6 hr (IM), TID (PO) slow release
❍ cat: 8-20 mg/kg TID (PO)
4. Quinidine:
❍ dog: gluconate 6-20 mg/kg QID (IM); Extentab (sulfate) 6-16 mg/kg TID (PO); Quinaglute, Cardioquin 8-20 mg/kg
TID-QID (PO)
❍ cat: Sulfate 5.5-11.0 mg/kg TID (PO)
5. Sotalol:
❍ dog: 0.5-2 mg/kg BID (PO)
❍ cat: unknown
6. Amiodarone:
❍ dog: Initial dose:10-15mg/kg BID (PO) for 7 d; then: 5-7.5mg/kg BID for 14d; then:7.5 mg/kg SID
❍ cat: unknown
Comment: Our experience with amiodarone is very limited. In people toxicities related to pulmonary pneumonitis is well
documented in at least 6% of cases. It appears that higher doses and longer duration of administration increase the likihood of this
toxicity. In addition, hypo and hyperthyroidism are described. GI and hepatic toxicity may occur.
Comment: The class 1 antiarrhythmics are known to have proarrhythmic properties. Thus my first choice drug is sotalol.
top Electrocardiology: Tachycardias
32 When should I begin therapy for premature ventricular contractions?
Therapy should be started if:
1. The patient is symptomatic due to the dysrhythmia (syncopal or weak or in heart failure due to the fast heart rate)
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (25 of 40)10/1/2005 15:28:51
VetGo Cardiology
2. You believe the patient's rhythm is in imminent danger of degenerating to ventricular fibrillation
Most of us have little difficulty determining if condition #1 is present. The most common problem is determining if condition #2 is
present. We used to believe that any of the following criteria suggested that a patient was at risk of degenerating to ventricular
fibrillation:
1. more than 20 PVC's per min.
2. presence of doublets or triplets
3. presence of multi-formed PVC's
4. presence of runs of PVC's (more than 3 in sequence)
5. presence of so-called R on T phenomenon (very early premature beats)
Recent work suggests that these old criteria are likely not indicators of patients at risk of developing ventricular fibrillation. Well
why not institute antiarrhythmic therapy any way just to be safe? This "cover your ass" approach would be useful if there were
no deleterious effects to this type of medication.
Recent work in people with slightly weakened hearts and having ventricular premature beats and treated with
antiarrhythmic drugs potentially sheds light on this issue.
In 1989 and 1991 the results of the CAST Trial (Cardiac Arrhythmia Suppression Trial) were released. (N Engl J Med 1989; 321:
406-12 and 1991; 324: 781-8)
Purpose: To compare the effect of Placebo vs Encainide vs Flecainide (both Class IC agents and the best and
safest agents available in people at the time to treat VPC's) on survival in patients with ventricular arrhythmias and
asymptomatic or minimally symptomatic with LV dysfunction
Sample: 1498 people enroled
857 assigned to receive encainide or its placebo, 641 assigned to receive flecainide or its placebo
Results: The study was prematurely aborted because the mortality rate was significantlly higher in the encainide and
flecainide patients vs placebo. Thus in asymptomatic or minimally symptomatic patients with LV dysfunction to treat
with any Class I agent is to markedly increase the risk of mortality.
This important study demonstrated that oral antiarrhythmic therapy can actually exacerbate arrhythmias and kill the patient via
sudden death (the very disorder it was intended to prevent). We now believe that drugs like the oral lidocaine analogs,
procainamide and quinidine are extremely proarrhythmic. The Class 3 antiarrhythmics sotalol and amiodarone are believed to be
the safest antiarrhythmics.
At present, only the beta blockers have been shown to reduce the risk of mortality in the setting of unsustained ventricular
tachycardia. It is likely that amiodarone and sotalol will also reduce the risk of sudden death, however, survival studies are
unavailable as yet in people.
Comment: It is my belief that heart rate may be the ultimate criteria predicting the malignancy of such dysrhythmias (in individuals
that are not hemodynamically embarrassed by this arrhythmia). If VPC's occur in the presence of an excessive heart rate, I believe
this represents a condition which has a high probability of progression to ventricular fibrillation. However, if VPC's occur in the
setting of a normal heart rate or a low heart rate, I believe this situation does not represent a threat to the dog of degenerating to
ventricular fibrillation. The definitive importance of heart rate in the presence of VPC's remains to be determined.
top Electrocardiology: Tachycardias
33 What is ventricular tachycardia?
Example of Ventricular Tachycardia in the Dog
Ventricular tachycardia (VT) refers to runs of greater than 3 PVC's in sequence. VT may markedly reduce cardiac output
(dysynergy of contraction). Etiology is as for premature ventricular contractions (see #1). VT is treated as described under
premature ventricular contractions. A number of cases of slow VT (dogs with heart rates from 80 - 120 bpm) frequently have
minimal hemodynamic consequences a result of this dysrhythmia and therefore warrant observation but not anti-arrhythmic
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (26 of 40)10/1/2005 15:28:51
VetGo Cardiology
therapy.
top Electrocardiology: Tachycardias
34 Outline criteria to assist in the differentiation of supraventricular and ventricular premature beats.
In that supraventricular premature beats may conduct with aberrancy resulting in bizarre and wide morphologic beats, the
differentiation of supraventricular premature beats from ventricular premature beats can be very difficult. In that the therapy for one
may be contraindicated in the other, it behooves us to attempt to differentiate these abnormalities. Also the prognosis for one is
different than that for the other. However "when all is said and done" at times we simply cannot separate these dysrhythmias.
A refers to the time between two normal sinus beats close to the premature beat. B refers to the time between the sinus beat just
before the premature beat to the sinus beat just after the premature beat.
If A > B (this is called a non-compensatory pause), indicates the premature beat is a supraventricular beat.
If A < B (this is called a compensatory pause), indicates the premature beat is a ventricular beat.
Example of an Interpolated Beat (VPC)
Example of Premature Beats
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (27 of 40)10/1/2005 15:28:51
VetGo Cardiology
This is a lead II trace of a dog; 5 fine lines vertically = 1 mv; 25 fine lines horizontally = 2 sec.
Supraventricular Premature Beats (SVPBs) Ventricular Premature Beats (VPBs)
1. Morphology of QRS is usually similar to the sinus beats 1. Morphology of QRS is bizarre vs the sinus beats
2. QRS is usually narrow 2. QRS is usually wide
3. SVPBs can't occur as fusion beats 3. VPBs may occur as fusion beats
So if the beat in question occurs as a fusion beat it must be a VPB
4. SVPBs can't occur as interpolated beats 4. VPBs may occur as interpolated beats
So if the beat in question occurs as an interpolated beat it must be a VPB
5. Atrial (P wave) and ventricular (QRS) activation are associated 5. A-V dissociation is usually present
Often the P waves cannot be visualized in the presence of tachycardia because they are buried in the QRS or T waves.
6. Non-fully compensatory pause is present 6. Fully compensated pause is present
If the background rhythm is irregular (as with sinus arrhythmia or atrial fibrillation) we can't use this criteria because we can't
predict the duration of 2 normal R to R intervals
7.When ventricular tachycardia occurs it may be
7. When supraventricular tachycardia occurs it tends to be very regular
slightly irregular
8. A premature beat that follows a premature P is never
8. A premature beat that follows a premature P wave is always a SVPC
a VPC
The absence of a premature P does not discriminate between an SVPC and a VPC
Miscellaneous
top Electrocardiology: Miscellaneous
35 What are the electrocardiographic signs of hyperkalemia?
General remarks:
Hyperkalemia results in:
1. Inhibition of atrial myocardial depolarization.
2. Slowing of heart rate.
3. Prolonging QRS duration; complexes may become bizarre.
4. Also known as atrial standstill.
5. Rhythm called sinoventricular rhythm.
6. The EKG is a poor substitute for serum potassium levels to determine the degree of abnormality.
EKG Findings:
1. From reduction of P wave amplitude and prolongation of PR interval to absence of P waves altogether.
2. Increase of QRS duration.
3. Increase of QT duration.
4. Slowing of heart rate.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (28 of 40)10/1/2005 15:28:51
VetGo Cardiology
5. T waves become tall and spiked.
6. Decreased R wave amplitude.
Example of Hyperkalemia in the Dog
Etiology:
1. Addisons Disease.
2. Obstructive urinary disease.
3. Oliguric, anuric renal disease.
4. Acidosis.
5. Uncontrolled diabetic ketoacidosis.
Treatment:
1. Sodium bicarbonate.
2. Treat the underlying disease.
3. If use fluids use NaCl
4. Ca gluconate antagonizes the cardiotoxic effects of potassium.
Dosages:
1. NaHCO3:
❍ dog: 1-2 mEq/kg (IV) slowly
❍ cat: same
❍ Ca gluconate:
❍ dog: 0.5 mg/kg (IV) slowly
❍ cat: same
Prognosis:
1. Excellent response to therapy.
Comment:
● This disorder must be distinguished from "silent atrium". Silent atrium is a diffuse atrial myocardial disorder wherein the
atrial tissue is neither capable of initiating an impulse nor being activated. This disorder will not respond to potassium
reductive therapy.
● The most specific EKG feature is the absence of P waves. At times these may be difficult to identify in the frontal plane
leads. The V leads are usually the best leads to illustrate P waves.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (29 of 40)10/1/2005 15:28:51
VetGo Cardiology
top Electrocardiology: Miscellaneous
36 What are the electrocardiographic signs of myocardial hypoxemia/ischemia?
General Comments:
1. There are no specific EKG findings typical of hypoxemia.
2. Some vague findings may be noted and these may include:
❍ wide QRS complexes
❍ ST segment depression or elevation
❍ tall T waves (<1/4 total QRS excursion)
❍ notching of the R wave of the QRS complex (Microscopic Intramural Myocardial Infarctions or MIMI)
❍ low amplitude QRS complexes
❍ conduction disturbances with aberrant conduction leading to bizarre QRS complex morphology
Example of ST Segment Depression in the Dog
Example of Microscopic Intramural Myocardial Infarctions (MIMI) in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (30 of 40)10/1/2005 15:28:51
VetGo Cardiology
top Electrocardiology: Miscellaneous
37 What is the significance of low amplitude QRS complexes in the dog?
EKG Findings:
1. Total excursion of the QRS complex is reduced
❍ <20 kg dog: <1 mv
❍ <20 kg dog: <1.5 mv
2. Other rhythm disorders may be present
Example of Low Amplitude QRS in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (31 of 40)10/1/2005 15:28:51
VetGo Cardiology
Etiologies:
1. Pleural effusion
2. Pericardial effusion
3. Obesity
4. Hypothyroidism
5. Pneumothorax
6. Diffuse myocardial disease
7. Normal variation
Consequences:
● There is no hemodynamic signficance associated with low amplitude QRS complexes. The underlying problem may have
significant hemodynamic impact.
Treatment:
● none required for this EKG
● the underlying disorder should be sought out and treated
top Electrocardiology: Miscellaneous
38 What is the significance of wide QRS complexes?
EKG Findings:
● Dog: 0.065 seconds
● Cat: 0.04 seconds
● Rhythm is sinus
Example of Wide QRS Complexes in the Dog
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (32 of 40)10/1/2005 15:28:51
VetGo Cardiology
10 fine lines vertically = 1 mv; 50 fine lines horizontally = 1 sec. Note the presence of MIMI.
Etiologies:
1. Aberrant conduction (so-called Bundle Branch Block)
2. Myocardial hypoxemia/ischemia
3. Left ventricular enlargement
Consequences:
● As per the underlying etiology. With aberrant conduction this may be an early sign to underlying myocardial disease or
impending complete heart block.
Treatment:
● No specific treatment. Address the underlying etiology
top Electrocardiology: Miscellaneous
39 Aberrancy
What is aberancy?
Aberrancy refers to the abnormal coordination of activation of the two ventricles that occurs from an impulse originating from a
source above the bifurcation of the bundle branches (as opposed to impulses that arise below the bifurcation of the bundle
branches such as escape beats or PVCs). Aberrancy is often referred to as bundle branch block In the normal situation, the
activation of the entire ventricular myocardium occurs in a coordinated fashion such that the left ventricle and right ventricle are
activated simultaneously. In the case of aberrancy one of the ventricles is activated before the other. Bundle branch block can be
described as complete or incomplete.
What is complete bundle branch block?
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (33 of 40)10/1/2005 15:28:51
VetGo Cardiology
This refers to that situation when the activation one ventricles begins and is completed prior to activation of the other ventricle.
Normal conduction through the heart
ECG characteristics
● Supraventricular origin
● Narrow QRS complexes
● Normal MEA
Right bundle branch block
ECG characteristics
● Supraventricular origin
● Wide QRS complexes
● MEA points to RV
Left bundle branch block
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (34 of 40)10/1/2005 15:28:51
VetGo Cardiology
ECG characteristics
● Supraventricular origin
● Wide QRS complexes
● MEA points to LV
What is incomplete bundle branch block?
This refers to that situation when the activation of one ventricle begins prior to the activation of the other ventricle however the
activation of the ventricle that is activated first does finish before the activation of the other ventricle begins.
Note that a continuum of scenarios exist such that the degree of prematurity of activation of one ventricle prior to the other may
occur in the setting of incomplete aberrancy.
How does aberrancy manifest electrocardiographically?
Aberrancy results in altering the morphology and duration of the QRS.
● Morphology: can vary from a left ventricular originating PVC morphology to that of a right ventricular originating PVC morphology.
● Duration: the duration in dogs can vary from as short as 60 to 65 msec with incomplete bundle branch block to up to 120 msec
with complete bundle branch block.
Right bundle branch block
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (35 of 40)10/1/2005 15:28:51
VetGo Cardiology
Left bundle branch block
What are the causes of aberrancy?
Disorders of the bundle branches:
● These may result in complete blockage of transmission down the bundle branch or merely a slowing of the speed of transmission
down one of the branches.
Physiological:
● Any supraventricular premature beat that occurs that is markedly premature can result in aberrancy. Usually a beat must be less
than 300 msec after the preceding beat to result in aberrancy. The absolute degree of prematurity required to induce aberrancy is
variable and depends on prevailing autonomic nervous system tone and the cycle length that preceeds the premature beat. The
longer the preceeding cycle length, the less premature the premature beat must be to induce aberrancy.
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (36 of 40)10/1/2005 15:28:51
VetGo Cardiology
● The more premature the premature beat the greater the degree of aberrancy
● Supraventriclar tachycardia.
● Merely driving the heart rate fast in some individuals will induce aberrancy. This usually results in a slower conduction in the
right bundle branch compared with the left bundle branch.
top Electrocardiology: Miscellaneous
40 Differentials for Abnormalities on the ECG
If I find an abnormality on the ECG, what does it mean?
The common approach to ECG texts dealing with interpretation is to provide a list of ECG disorders with a description of the ECG
findings for each. Therefore the practitioner is faced with attempting to match his/her test ECG with one of the members of the long
list of potential ECG disorders in the text. Although this is fine, I would like to add a different approach which is based on the ECG
abnormality as a starting point. In this approach which is provided below, the practitioner notes any abnormalites present on the test
ECG and is provided a differential list of possible disorders for each. Hence a shortened list of potential disorders is provided.
1. What if there is no P wave?
Several situations must be differentiated if "absence of P waves" is the abnormality.
❍ Is the P wave totally absent throughout the rhythm?
❍ Is the P wave obscured or intermittently present?
❍ Is the P wave absent for only one beat?
2. What if the P wave is totally absent throughout the rhythm?
Rule outs include:
1. Atrial fibrillation (note the QRS to QRS interval must be irregular; the heart rate is usually high normal or elevated).
Baseline undulations or f waves can be misinterpreted as P waves. If there is no consistent P morphology (usually
there are too many possible P morphologies to select from due to the undulating baseline) and it/these are at
variable distances before the QRS, then I suggest there are no P waves.
2. Hyperkalemia (also called persistent atrial standstill) (note the QRS to QRS interval tends to be regular; the heart
rate tends to be low normal or slow)
3. Silent atrium (a disorder wherein the atrial myocardium is replaced by fibrous tissue) (note the QRS to QRS interval
tends to be regular; the heart rate tends to be slow, the rhythm is called an escape rhythm)
4. Supraventricular tachycardia (in fact there is always a P wave associated with the QRS here but in many cases
the P wave is completely buried in the QRS or T wave such that we can't visualize it)
5. An idioventricular rhythm (looks like ventricular tachycardia but the rate is slow; looks like an escape rhythm but is
too fast). No P waves are present.
3. What if the P wave is obscured or intermittently present?
Rule outs include:
1. A very small P wave. The P wave can be difficult to see or find in some dogs and many cats because it is very
small. The chest leads tend to give the biggest P waves, so always check here carefully.
2. A buried P wave. When the heart rate is fast the P wave can be buried in the preceding T wave. Look for pauses in
the rhythm (such as after a PVC) to check for P waves, or try to slow the heart rate and look for P waves.
3. Ventricular tachycardia. Several P waves are usually observed intermittently in most cases; the other P waves are
buried in the QRS or T wave of the PVC.
4. Sick sinus syndrome. Intermittent periods of pause with no P or QRS, or just no P waves with an escape rhythm.
4. What if the P wave is absent for only one beat?
Rule outs include:
1. A premature ventricular contraction if the QRS occurs early (the QRS must meet the criteria for PVC)
2. A supraventricular premature contraction if the QRS occurs early (the QRS must meet the criteria for a
supraventricular premature contraction)
3. A ventricular escape beat if the QRS occurs late (>1.2 sec) (the QRS must be wide and bizarre in morphology)
Example of a ventricular escape beat
4. A supraventricular escape beat if the QRS occurs late (>1.2 sec) (the QRS must be narrow and similar to the
sinus beats)
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (37 of 40)10/1/2005 15:28:51
VetGo Cardiology
5. What if there is no QRS complex following the P wave?
Rule outs include:
1. 2nd degree heart block or 3rd degree heart block (P waves that are not followed by a QRS)
2. Sick sinus syndrome (often there are periord of absent P waves and QRS in addition to absent QRSs following a
P)
6. What if there is no T wave
Rule outs include:
1. Artifact. If a deflection looks like it might be a QRS, although perhaps somewhat bizarre, and there is no T wave,
then that deflection is not a QRS, it is an artifact. All depolarizations must have a repolarization wave.
7. What if there is an unusual shaped P wave?
Several situations must be differentiated if the P wave is of an unusual shape:
❍ Is there just one isolated P wave that is of an unusual shape?
❍ Is the P wave of variable shapes and occurring in a pattern?
❍ Is the P wave of a consistent unusual shape?
8. What if there is just one isolated P wave that is of an unusual shape?
Rule outs include:
1. A premature (ectopic) P wave (usually this occurs as an early P wave). This P wave may or may not be followed
by a QRS complex (the latter is an APC with block).
9. What if the P wave is of variable shapes and occurs in a pattern?
Rule outs include:
1. Wandering atrial pacemaker (there is usually a pattern, for example: the P wave might be tall (in lead II) on the
short cycles and absent, isoelectric or negative on the long cycles; usually occurs in the setting or sinus arrhythmia)
10. What if the P wave is of a consistent unusual shape?
Rule outs include:
1. An ectopic atrial rhythm (a normal P wave must be positive in lead II)
11. What if the QRS is of an unusual shape?
Several situations must be differentiated if the QRS is of an unusual shape:.
❍ Is there just one isolated QRS that is of an unusual shape?
❍ Is the QRS is of a consistent unusual shape?
12. What if there is just one isolated QRS that is of an unusual shape?
Rule outs include:
1. A fusion beat if there is a typical P wave with a normal or near normal PR interval (usually occurs in the company of
other examples elsewhere of PVCs)
2. A premature ventricular contraction if the QRS is early (the QRS must meet the criteria for PVC)
3. A supraventricular premature contraction if the QRS occurs early (the QRS must meet the criteria for a
supraventricular premature contraction) conducting with a slight (or more) degree of aberration.
4. A ventricular escape beat if the QRS occurs late (>1.2 sec) (the QRS must be wide and bizarre in morphology) and
it is not preceded by a P wave.
5. A supraventricular escape beat if the QRS occurs late (>1.2 sec) (the QRS must be meet the criteria for a
supraventricular beat) conducting with a slight (or more) degree of aberration.
6. A sinus beat that conducts with aberration (as bundle branch block). A normal P wave must be present and
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (38 of 40)10/1/2005 15:28:51
VetGo Cardiology
associated with this QRS complex.
7. Artifact. Artifact may be present as any of the following: if it occurs between the end of the preceding QRS and the
first half of the T wave of that QRS (no real beat [normal or ectopic] can occur at this time because the heart is
refractory); if it fails to alter the underlying rhythm (however interpolated PVCs can do this as well); or if it fails to be
followed by a repolarization wave, this should usually be a deflection in the opposite direction of the artifact wave (if
a real T wave were to be present).
13. What if the QRS is of a consistent unusual shape?
Rule outs include:
1. Bundle branch block if the rhythm is sinus or of supraventricular origin (the QRS meets the criteria for right or left
bundle branch block)
2. Ventricular tachycardia (the QRS meets the criteria for ventricular tachycardia)
3. Right ventricular enlargement (a supraventricular rhythm and the QRS is negative in lead two; meets the criteria
for right ventricular enlargement)
4. An escape rhythm. It could be supraventricular conducting with aberration or ventricular in origin.
5. An idioventricular rhythm. A form of slow ventricular tachycardia.
14. What if the QRS has a notch in it?
Rule outs include:
1. A MIMI is present (refers to microscopic intramural myocardial infarct) (the beats must be sinus in origin or
supraventricular origin)
2. Not significant if present on a PVC or a ventricular escape beat
3. Not significant if bundle branch block is present
15. What if the QRS is wide? see #1
Rule outs for a persistently wide QRS include:
1. Left ventricular enlargement (if the R wave is tall then yes left ventricular enlargement is present; if the R wave is
not tall then left ventricular enlargement may not be present) (with left ventricular enlargement the QRS is only
slightly widened)
2. A sick myocardium (dilated cardiomyopathy or heart failure can be associated with a wide QRS associated with
slow myocyte to myocyte conduction)
3. Bundle branch block (the rhythm meets the criteria for bundle branch block and the rhythm is sinus or
supraventricular) (the QRS is markedly widened)
4. Right ventricular enlargement (the QRS is only slightly widened or normal width)
5. Ventricular tachycardia (meets the criteria for PVC)
6. A ventricular escape rhythm
7. A pre-excited beat (meets the criteria for pre-excitation)
16. What if the QRS is small? see #2
Rule outs include:
1. Thoracic effusions (pleural or pericardial)
2. A sick myocardium (dilated cardiomyopathy or heart failure can be associated with a low amplitude QRS)
3. Obesity
4. Hypothyroid (probably related to obesity with hypothyroid)
5. Pnuemothorax
6. A normal variant
7. A fusion beat; occurs as a single beat (meets the criteria for a fusion beat)
17. What if the R wave is tall in lead II?
Rule outs include:
1. Left ventricular enlargement (if the rhythm is supraventricular in origin)
18. What if the ST segment is depressed?
Rule outs include:
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (39 of 40)10/1/2005 15:28:51
VetGo Cardiology
1. Left ventricular enlargement (if the left ventricular enlargement criteria are met; all by itself this is probably not
enough to suggest left ventricular enlargement)
2. A sick myocardium (dilated cardiomyopathy or heart failure can be associated with this)
3. Not of significance if not associated with a supraventricular beat (such as in a PVC)
4. Not of significance if associated with bundle branch block
19. What if the ST segment is elevated?
Rule outs include:
1. Pericardial disease
2. A sick myocardium (dilated cardiomyopathy or heart failure can be associated with this)
3. Not of significance if not associated with a supraventricular beat (such as in a PVC)
4. Not of significance if associated with bundle branch block
20. What is there is coving of the ST segment?
Rule outs include:
1. A sick myocardium (dilated cardiomyopathy or heart failure can be associated with this)
2. This may be normal (many ECG units tend to produce some degree of coving)
21. What if the P wave is wide?
Rule outs include:
1. Left atrial enlargement
22. What if the P wave is tall?
Rule outs include:
1. Right atrial enlargement
2. Pulmonary artery hypertension
23. What if the P wave is notched?
Rule outs include:
1. Left atrial enlargement (only if the P wave is also too wide)
2. Normal variant (if the P wave is not too wide)
24. What if the P wave is not associated with the QRS?
Rule outs include:
1. 3rd degree heart block (the ventricular rate is slower than the atrial rate)
2. Ventricular tachycardia (the P waves are often difficult to observe as they are buried in the QRS or T wave)
3. Non paroxysmal supraventricular (or junctional) tachycardia
4. Idioventricular rhythm
[ Concepts ] [ Quarterly Cases ] [ Radiographs ] [ Heart Sounds ]
[ Databases ] [ Formulary ] [ Contact ] [ About ]
Copyright (c) 2001-2004 Fluid Intelligence
http://www.vetgo.com/cardio/concepts/concsect.php?sectionkey=5§ion=Electrocardiology (40 of 40)10/1/2005 15:28:51
Вам также может понравиться
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookОт EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookОценок пока нет
- EKGДокумент31 страницаEKGJay JiangОценок пока нет
- EkgДокумент26 страницEkgMuhammad Zubair ZainalОценок пока нет
- ECG - Module - Printable Analysis and Interpretation of ECGДокумент37 страницECG - Module - Printable Analysis and Interpretation of ECGPankaj PatilОценок пока нет
- EcgДокумент18 страницEcgmyla adapОценок пока нет
- ECG Rhythm InterpretationДокумент16 страницECG Rhythm InterpretationJanettОценок пока нет
- ECG Module PrintableДокумент39 страницECG Module PrintableAbu HibbaanОценок пока нет
- Ecg FileДокумент29 страницEcg Fileneha miriОценок пока нет
- Electrocardiogram (ECG/EKG) : Jovel Balaba Tangonan InstructorДокумент77 страницElectrocardiogram (ECG/EKG) : Jovel Balaba Tangonan InstructorNecky AlbaciteОценок пока нет
- CardioДокумент261 страницаCardioAli Aborges Jr.Оценок пока нет
- Dissertation EkgДокумент6 страницDissertation EkgBuyACollegePaperOnlineMilwaukee100% (1)
- ECG Interpretation (WSAVA 2007, Boswood)Документ5 страницECG Interpretation (WSAVA 2007, Boswood)Kevin ChoyОценок пока нет
- Conquering The ECGДокумент25 страницConquering The ECGPankaj PatilОценок пока нет
- ECG PracticalДокумент48 страницECG PracticalbvkjtzrvnyОценок пока нет
- ECG Made Easy by Mallareddy SripujaДокумент46 страницECG Made Easy by Mallareddy Sripujagrreddy836100% (3)
- Basics of EKG InterpretationДокумент132 страницыBasics of EKG InterpretationSiddhant GautamОценок пока нет
- 4ECG ProceedingsAAДокумент12 страниц4ECG ProceedingsAATiamiyu OlayemiОценок пока нет
- Ecg Reading Made EasyДокумент59 страницEcg Reading Made EasyAngealyn GaviolaОценок пока нет
- Ecg (Ekg) : Dr. Jamal Dabbas Interventional Cardiologist & InternistДокумент87 страницEcg (Ekg) : Dr. Jamal Dabbas Interventional Cardiologist & Internistsara rababahОценок пока нет
- ECG InterpretationДокумент1 страницаECG InterpretationCecil-An DalanonОценок пока нет
- Raza's ECGДокумент45 страницRaza's ECGcozmoxxxОценок пока нет
- Electrocardiography: The ECG: A.D. John, MD, Lee A. Fleisher, MDДокумент19 страницElectrocardiography: The ECG: A.D. John, MD, Lee A. Fleisher, MDCésar Vásquez AguilarОценок пока нет
- How Procedure Is Performed: ElectrocardiogramДокумент10 страницHow Procedure Is Performed: ElectrocardiogramJonathan AlvarezОценок пока нет
- Auskultation. ECG - LastДокумент5 страницAuskultation. ECG - LastAndreyОценок пока нет
- EcgДокумент57 страницEcgenii_ta100% (9)
- Basics of EKG InterpretationДокумент132 страницыBasics of EKG InterpretationArif Imam HidayatОценок пока нет
- Clinical Demonstration: Topic: Electrocardiogram (ECG)Документ24 страницыClinical Demonstration: Topic: Electrocardiogram (ECG)soniya josephОценок пока нет
- ECG Interpretation UnismaДокумент178 страницECG Interpretation UnismadefinaОценок пока нет
- INTERPRETASI EKG MahasiswaДокумент43 страницыINTERPRETASI EKG MahasiswaMartin Susanto, MDОценок пока нет
- ECG WorldДокумент139 страницECG WorldsatyaОценок пока нет
- Belajar Ekg YukДокумент35 страницBelajar Ekg Yukannisamuti10Оценок пока нет
- EKG Self Study GuideДокумент40 страницEKG Self Study GuideArgee AlonsabeОценок пока нет
- Electrocardiography: An Introduction To The ECGДокумент76 страницElectrocardiography: An Introduction To The ECGInnocent Clifford MaranduОценок пока нет
- Lab Exercise 5 PDFДокумент50 страницLab Exercise 5 PDFE1- Villapaz, Aiemarie R. (Aie)Оценок пока нет
- ECG Waves and Intervals Spatial Orientation of The 12 Lead ECGДокумент31 страницаECG Waves and Intervals Spatial Orientation of The 12 Lead ECGiah_18Оценок пока нет
- ECG EKG InterpretationДокумент11 страницECG EKG InterpretationGunma AkagiОценок пока нет
- The ElectrocardiogramДокумент53 страницыThe ElectrocardiogramJEM93Оценок пока нет
- Basic ECG InterpretationДокумент8 страницBasic ECG Interpretationamesb100% (1)
- How To Read An ECGДокумент21 страницаHow To Read An ECGSlychenkoОценок пока нет
- EKG Basics - LongДокумент40 страницEKG Basics - Longمحمد خالدОценок пока нет
- ECG A Methodical Approach - Leaflet Print - Patient UKДокумент7 страницECG A Methodical Approach - Leaflet Print - Patient UKBen MpanzuОценок пока нет
- Anatomi 1Документ54 страницыAnatomi 1Fany LainamaОценок пока нет
- EcgДокумент11 страницEcgRajneesh TiwariОценок пока нет
- Ecg in DogsДокумент107 страницEcg in DogsPLABITA GOSWAMI100% (2)
- Basics of EKG InterpretationДокумент53 страницыBasics of EKG InterpretationHala BahaaОценок пока нет
- Electrocardiography: DR Uwanuruochi KelechukwuДокумент50 страницElectrocardiography: DR Uwanuruochi KelechukwuJake MillerОценок пока нет
- Basics of ECG: DR Subroto Mandal, MD, DM, DC Associate Professor, CardiologyДокумент206 страницBasics of ECG: DR Subroto Mandal, MD, DM, DC Associate Professor, CardiologyRavi SharmaОценок пока нет
- Basic ECG InterpretationДокумент62 страницыBasic ECG Interpretationmohannadalkwiese3Оценок пока нет
- ECG InterpretationДокумент11 страницECG InterpretationAndrea AndradaОценок пока нет
- 2012 ECG HandoutДокумент40 страниц2012 ECG Handoutlizzy596Оценок пока нет
- Hypertrophy and Enlargement of The HeartДокумент23 страницыHypertrophy and Enlargement of The HeartZion_MilgemОценок пока нет
- The 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsОт EverandThe 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsОценок пока нет
- ECG/EKG Interpretation: An Easy Approach to Read a 12-Lead ECG and How to Diagnose and Treat ArrhythmiasОт EverandECG/EKG Interpretation: An Easy Approach to Read a 12-Lead ECG and How to Diagnose and Treat ArrhythmiasРейтинг: 5 из 5 звезд5/5 (2)
- Anatomia - Diagnostica (PPTshare)Документ70 страницAnatomia - Diagnostica (PPTshare)DANIEL ALEJANDRO100% (1)
- Sindrome Del Corazon RotoДокумент6 страницSindrome Del Corazon RotoDANIEL ALEJANDROОценок пока нет
- 1.1 Trauma RaquimedularДокумент55 страниц1.1 Trauma RaquimedularDANIEL ALEJANDROОценок пока нет
- Cardiologia - EletrocardiografiaДокумент40 страницCardiologia - EletrocardiografiaDANIEL ALEJANDROОценок пока нет
- GertsmanДокумент6 страницGertsmandantevalerОценок пока нет