Академический Документы
Профессиональный Документы
Культура Документы
Infection in Health Care Workers in Rural India: Mycobacterium Tuberculosis
Загружено:
gtzaИсходное описание:
Оригинальное название
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Infection in Health Care Workers in Rural India: Mycobacterium Tuberculosis
Загружено:
gtzaАвторское право:
Доступные форматы
ORIGINAL CONTRIBUTION
Mycobacterium tuberculosis Infection
in Health Care Workers in Rural India
Comparison of a Whole-Blood Interferon ␥ Assay
With Tuberculin Skin Testing
Madhukar Pai, MD, PhD Context Mycobacterium tuberculosis infection in health care workers has not been
Kaustubh Gokhale, MD adequately studied in developing countries using newer diagnostic tests.
Rajnish Joshi, MD Objectives To estimate latent tuberculosis infection prevalence in health care work-
Sandeep Dogra, MD ers using the tuberculin skin test (TST) and a whole-blood interferon ␥ (IFN-␥) assay;
to determine agreement between the tests; and to compare their correlation with risk
Shriprakash Kalantri, MD, MPH factors.
Deepak K. Mendiratta, MD Design, Setting, and Participants A cross-sectional comparison study of 726 health
Pratibha Narang, MD care workers aged 18 to 61 years (median age, 22 years) with no history of active
tuberculosis conducted from January to May 2004, at a rural medical school in India.
Charles L. Daley, MD A total of 493 (68%) of the health care workers had direct contact with patients with
Reuben M. Granich, MD, MPH tuberculosis and 514 (71%) had BCG vaccine scars.
Gerald H. Mazurek, MD Interventions Tuberculin skin testing was performed using 1-TU dose of purified
protein derivative RT23, and the IFN-␥ assay was performed by measuring IFN-␥ re-
Arthur L. Reingold, MD
sponse to early secreted antigenic target 6, culture filtrate protein 10, and a portion of
Lee W. Riley, MD tuberculosis antigen TB7.7.
John M. Colford, Jr, MD, PhD Main Outcome Measures Agreement between TST and the IFN-␥ assay, and
comparison of the tests with respect to their association with risk factors.
A
N ESTIMATED ONE THIRD OF
the world’s population is in- Results A large proportion of the health care workers were latently infected; 360 (50%)
fected with Mycobacterium tu- were positive by either TST or IFN-␥ assay, and 226 (31%) were positive by both tests.
berculosis,1 presenting a ma- The prevalence estimates of TST and IFN-␥ assay positivity were comparable (41%; 95%
confidence interval [CI], 38%-45% and 40%; 95% CI, 37%-43%, respectively). Agree-
jor impediment to tuberculosis control. ment between the tests was high (81.4%; =0.61; 95% CI, 0.56-0.67). Increasing age
Despite the importance of latent tuber- and years in the health profession were significant risk factors for both IFN-␥ assay and
culosis infection (LTBI), the tubercu- TST positivity. BCG vaccination had little impact on TST and IFN-␥ assay results.
lin skin test (TST) was, until recently,
Conclusions Our study showed high latent tuberculosis infection prevalence in In-
the only test available for its diagno- dian health care workers, high agreement between TST and IFN-␥ assay, and similar
sis.2-5 The TST measures hypersensitiv- association between positive test results and risk factors. Although TST and IFN-␥ as-
ity response to purified protein deriva- say appear comparable in this population, they have different performance and op-
tive (PPD), a crude mixture of antigens, erational characteristics; therefore, the decision to select one test over the other will
many of which are shared among M tu- depend on the population, purpose of testing, and resource availability.
berculosis, Mycobacterium bovis bacille JAMA. 2005;293:2746-2755 www.jama.com
Calmette-Guérin (BCG), and several
nontuberculous mycobacteria (NTM). Author Affiliations: Departments of Medicine and Mi- Mazurek); and Office of World Health Organization
The TST has limitations with respect to crobiology, Mahatma Gandhi Institute of Medical Sci- Representative to India, New Delhi (Dr Granich). Dr Da-
ences, Sevagram, India (Drs Pai, Gokhale, Joshi, Dogra, ley is now with the National Jewish Medical and Re-
accuracy and reliability.2-6 Kalantri, Mendiratta, and Narang); Divisions of Epide- search Center, Denver, Colo. Dr Granich is now with
Advances in genomics and immunol- miology and Infectious Diseases, School of Public Health, the Office of the United States Global AIDS Coordina-
University of California, Berkeley (Drs Pai, Reingold, tor, Washington, DC.
ogy have led to a promising alternative, Riley, and Colford); Department of Medicine, Univer- Corresponding Author: Madhukar Pai, MD, PhD, Di-
sity of California, San Francisco (Dr Daley); Division vision of Epidemiology, University of California, Berke-
See also pp 2756 and 2785. of Tuberculosis Elimination, Centers for Disease Con- ley, 140 Warren Hall, Berkeley, CA 94720 (madhupai
trol and Prevention, Atlanta, Ga (Drs Granich and @berkeley.edu).
2746 JAMA, June 8, 2005—Vol 293, No. 22 (Reprinted) ©2005 American Medical Association. All rights reserved.
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
the in vitro interferon ␥ (IFN-␥) as- Health care workers are at high risk ria were excluded: age younger than 18
say,6-8 based on the concept that T cells for tuberculosis.13 Despite India’s tuber- years, pregnancy, allergy to tuberculin,
of infected individuals release IFN-␥. Al- culosis burden, little is known about tu- and active tuberculosis in the past. Be-
though early IFN-␥ assays used PPD, berculosis in health care workers.14,15 The cause our goal was to recruit all health
newer assays use antigens, such as the Revised National Tuberculosis Control care workers at our institution, no for-
early secreted antigenic target 6 Programme of India is focused on ex- mal sample size determination was
(ESAT-6) and culture filtrate protein 10 panding Directly Observed Treatment, made. All participants gave written in-
(CFP-10). These proteins, encoded Short-Course services. There are cur- formed consent, and the research was
within the region of difference 1 (RD1) rently no national guidelines specific for approved by the ethics committees at the
of the M tuberculosis genome, are sig- reducing nosocomial tuberculosis risk. Mahatma Gandhi Institute of Medical
nificantly more specific to M tuberculo- Because health care workers treat large Sciences hospital and the University of
sis than PPD, as they are not shared with numbers of patients16 and isolation fa- California, Berkeley.
BCG substrains or several NTM spe- cilities are scarce and expensive, In- Each participant provided data on
cies that might cause nonspecific sen- dian hospitals do not routinely isolate age, sex, education, employment, BCG
sitization. 6 The QuantiFERON-TB patients with tuberculosis.14,15 Health vaccination, prior TST, and symp-
assay (Cellestis Limited, Carnegie, Aus- care workers often work in crowded hos- toms. We also assessed surrogate mark-
tralia) was the first commercially avail- pitals with minimal infection control ers of M tuberculosis exposure, includ-
able IFN-␥ assay. The PPD-based measures.14 The goals of our study were ing year of training, years in the health
QuantiFERON-TB test was approved by to estimate the burden of LTBI in In- care profession, job category, direct
the US Food and Drug Administration dian health care workers using the TST contact with sputum smear-positive tu-
in 2001.9 The QuantiFERON-TB Gold, and an enhanced IFN-␥ assay, deter- berculosis (defined as contact be-
an enhanced assay based on RD1 anti- mine the agreement between the tests, tween 2 people that is of sufficient dis-
gens, was approved by the Food and compare their correlation with LTBI tance to allow conversation between
and Drug Administration in December risk factors. them5), training in internal medicine,
2004. A simplified variant of the and household tuberculosis contact.
QuantiFERON-TB Gold assay, the METHODS Education and job category were used
QuantiFERON-TB Gold In-Tube test Study Design and Setting as socioeconomic status indicators. Af-
(hereafter referred to as IFN-␥ assay) has We conducted a cross-sectional com- ter the interview, BCG vaccine scar was
been recently developed. This assay uses parison study from January to May 2004, ascertained by inspection and blood was
overlapping peptides representing at the Mahatma Gandhi Institute of drawn for the IFN-␥ assay, followed by
ESAT-6, CFP-10, and a portion of tu- Medical Sciences, a rural medical school TST administration. The tests were in-
berculosis antigen TB7.7 (Rv2654), and in Sevagram, India. At this hospital, terpreted independently of each other
stimulation by this antigenic mixture oc- about 300 patients with tuberculosis are and of exposure information. Human
curs within the tube used to collect treated each year and the estimated com- immunodeficiency virus testing was not
blood. Other tests, including those us- munity prevalence of smear-positive tu- performed because of the low preva-
ing enzyme-linked immunospot, have berculosis is 200 per 100 000,17 with the lence of positive human immunodefi-
also been evaluated.6-8 annual risk of infection at 1.2% to 1.6%.18 ciency virus expected in this young,
Several studies have evaluated IFN-␥ At the Mahatma Gandhi Institute of educated population.
assays (in a review article8); however, Medical Sciences hospital, there are lim- Participants who were symptom-
very few have been conducted in tu- ited tuberculosis infection control mea- atic or positive by either test were in-
berculosis-endemic countries. In such sures in place and health care workers vestigated (using chest radiographs and
countries, high BCG vaccine cover- are constantly exposed to patients with sputum microscopy) to rule out active
age, widespread NTM exposure, and tuberculosis. Although no data were disease. Although it is not standard
high tuberculosis incidence pose chal- available on the incidence of tubercu- practice to treat LTBI in India, health
lenges for the evaluation of any LTBI losis among health care workers at the care workers diagnosed to have LTBI
test. Because of the paucity of data from time of our study, 5 (33%) of 15 inter- (n=360) in our study were offered the
endemic countries and the need for im- nal medicine residents had developed ac- option of counseling on risks and ben-
proved tuberculosis diagnostic tests, we tive tuberculosis during their training. efits of LTBI treatment. Of these, 61
evaluated an RD1-based IFN-␥ assay in (17%) health care workers (mostly stu-
a high-risk population in India, the Participants dent and staff nurses) elected to un-
country that accounts for one third of Our study was designed to recruit health dergo standard isoniazid treatment for
the global burden of tuberculosis.10,11 care workers, including trainees, nurses, 6 months.19 As of January 2005, 37
An estimated 40% of the Indian popu- laboratory workers, orderlies, and at- (61%) of 61 health care workers had
lation is infected and the annual risk of tending physicians. Health care work- completed therapy with no major ad-
infection is 1.5%.10-12 ers who met any of the following crite- verse events.
©2005 American Medical Association. All rights reserved. (Reprinted) JAMA, June 8, 2005—Vol 293, No. 22 2747
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
induration of at least 10 mm was con- assessed between continuous IFN-␥ val-
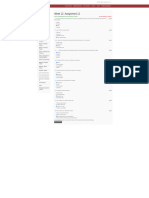
Figure 1. Study Flow Diagram
sidered positive. For comparison, 5 mm ues (IU/mL) and TST induration (mm).
1172 Total Health Care Workers and 15 mm cutpoints were also used. Factors associated with discordance were
An enhanced “in-tube” version of the explored using a logistic regression
91 Excluded (Age <18 y, IFN-␥ assay was used for this study. The model with any discordance (either posi-
Pregnancy, Tuberculin
Allergy, Past Active assay involves 2 stages: incubation of tive TST/negative IFN-␥ assay or nega-
Tuberculosis) whole blood with antigens, and mea- tive TST/positive IFN-␥ assay) as the out-
surement of IFN-␥ production in har- come, and factors such as age, sex,
1081 Eligible Health Care Workers
vested plasma by enzyme-linked immu- exposure to tuberculosis, and BCG vac-
nosorbent assay. Venous blood was cine as covariates.
355 Refused to Participate
directly collected into three 1-mL hep- Risk factors for test positivity were
726 Recruited arin-containing tubes. One tube con- evaluated using odds ratios (ORs). To
tained only heparin as negative control, adjust for multiple covariates, we used
2 Excluded another also contained the T-cell mito- a logistic regression model with TST or
1 Received TST Only
1 Received IFN-γ Assay
gen phytohemagglutinin as positive con- IFN-␥ assay results as the outcome and
Only trol, and the third tube had overlapping covariates such as markers of tubercu-
peptides representing the entire se- losis exposure. Logistic regression was
724 Received TST and IFN-γ Assay
quences of ESAT-6 and CFP-10, and an- performed using methods described
other peptide representing a portion of elsewhere24: covariates that were sig-
5 Invalid TST Results
Excluded (Late Reading) TB7.7. Within 2 to 6 hours of blood nificant in bivariate analyses were in-
draw, the tubes were incubated at 37°C. cluded in the preliminary model. In ad-
1 Indeterminate IFN-γ Assay Result; After 24 hours of incubation, the tubes dition, other covariates (such as age)
Repeat Test Valid (Negative Result)
were centrifuged and plasma was har- that were considered biologically im-
719 Valid TST and IFN-γ Assay
vested and frozen at –70°C until the en- portant were forced into the model ir-
Results zyme-linked immunosorbent assay was respective of statistical significance. In-
performed. The amount of IFN-␥ was teraction between covariates was
226 Positive 359 Negative 72 Positive 62 Negative
quantified using the enzyme-linked im- evaluated by adding interaction terms
TST/ TST/ TST/ TST/ munosorbent assay. The IFN-␥ values to the model and evaluating its statis-
Positive Negative Negative Positive
IFN-γ IFN-γ IFN-γ IFN-γ (IU/mL) for tuberculosis-specific anti- tical significance using the Wald P
Assay Assay Assay Assay gens and mitogen were corrected for value. From the initial model, covari-
background by subtracting the value ob- ates that did not contribute signifi-
TST indicates tuberculin skin test; IFN-␥, interferon ␥.
TST cutpoint is at least 10 mm; IFN-␥ assay cutpoint
tained for the respective negative con- cantly were dropped 1 at a time until
is at least 0.35 IU/mL. trol. As recommended by the manufac- the best fitting, parsimonious model
turer and based on previous studies,22,23 was identified. Model fit was evalu-
the cutoff value for a positive test was ated using the Hosmer-Lemeshow test.24
TST and IFN-␥ Testing IFN-␥ of at least 0.35 IU/mL. The en- The results of the final model are pre-
As recommended by India’s Revised Na- zyme-linked immunosorbent assay can- sented as adjusted ORs with 95% con-
tional Tuberculosis Control Pro- not accurately determine the absolute fidence intervals (CIs). Because young
gramme20 and based on previous stud- IFN-␥ values when they exceed 10 IU/ trainees in the hospital were expected
ies,3,21 we performed the TST using mL. Therefore, IFN-␥ values of more to have shorter and uncomplicated ex-
1-TU dose of PPD RT23 (Statens Se- than 10 IU/mL are shown as 10 IU/mL posure histories, and recall of expo-
rum Institut, Copenhagen, Den- in our graphs. Testing was performed at sure might be better in students, we
mark). Tuberculin skin test was ad- the study site, and all assays met quality planned a prespecified subgroup analy-
ministered by a certified technician control standards. sis to evaluate risk factors among 353
using the Mantoux method and read af- medical and nursing students.
ter 48 to 72 hours using a blinded cali- Statistical Analysis
per. Interreader variability was as- Statistical analyses were performed us- RESULTS
sessed using a second independent ing Stata version 8 (Stata Corp, College Participant Description
reader for a subset of the participants. Station, Tex). The outcomes included Of 1081 eligible health care workers,
The second trained reader used the agreement between the tests, factors as- 726 (67%) participated in the study
same palpation technique as the first. sociated with discordance, and com- (FIGURE 1). Participation rates were
As recommended by the Revised parison of the tests with respect to their high among students (91%) but low
National Tuberculosis Control Pro- association with risk factors. Agree- among attending physicians (10%). As
gramme20 and consistent with the stan- ment between the tests was quantified shown in TABLE 1, medical and nurs-
dard risk-stratified interpretation,19 an using the statistic. Correlation was also ing students accounted for 48% of the
2748 JAMA, June 8, 2005—Vol 293, No. 22 (Reprinted) ©2005 American Medical Association. All rights reserved.
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
cohort. The median age was 22 years Subgroup Analysis
Table 1. Participant Characteristics
(range, 18-61 years). Only 36 of the Among students, we evaluated covari- (N=726)*
health care workers (5%) had ever been ates, including age, sex, student cat- No. (%) of
tuberculin tested and 514 (71%) of 726 egory, socioeconomic status, year of Characteristics Participants
had BCG vaccine scars. A total of 493 training, direct contact with active Age, y
(68%) of the participants reported di- tuberculosis, household contact, 18-20 226 (31)
21-30 324 (45)
rect contact with patients with spu- training in internal medicine, and 31-40 75 (10)
tum smear-positive tuberculosis. Ex- BCG vaccine scar. With TST as the ⱖ41 101 (14)
Women 453 (62)
posure was particularly high among outcome, the final model had only 2 Educational level
interns, residents, physicians, and covariates: age and sex. Students aged Medical degree, master’s, 619 (85)
bachelor’s degree,
nurses. On average, these health care 21 to 23 years and older than 23 years or diploma†
workers reported at least 3 contacts with had increased ORs compared with High school or lower 107 (15)
Job category
patients with tuberculosis in the week students aged 18 to 20 years (1.45; Medical students 227 (31)
before their interviews. 95% CI, 0.8-2.6; and 4.2; 95% CI, 1.9- Interns 43 (6)
9.3; respectively). Although not statis- Residents 30 (4)
Nursing students 126 (17)
TST Results tically significant, female students had Nurses 161 (22)
Valid TST results were available in 720 higher odds of TST positivity (OR, Laboratory staff 39 (5)
Orderlies 87 (12)
(99%) of 726 individuals. FIGURE 2 1.7; 95% CI, 0.9-2.9). With IFN-␥ Attending physicians/ 13 (2)
shows a bimodal TST distribution with assay as the outcome, only age and faculty
Years served in the
the first peak centered on zero and a sex were retained in the final model. health care profession
second peak centered on 15. With a cut- The ORs for those participants aged ⱕ1 96 (13)
point of at least 10 mm, 298 (41%) of 21 to 23 years and older than 23 years 2-5 343 (47)
6-10 118 (16)
720 participants were positive (95% CI, were 1.36 (95% CI, 0.8-2.4) and 4.01 ⬎10 169 (23)
38%-45%). With a cutpoint of at least (95% CI, 1.8-8.8), respectively. Tuberculin skin tested 36 (5)
in the past
15 mm, 167 (23%) of 720 participants Female students had higher odds of Ever tested for human 22 (3)
were positive (95% CI, 20%-27%). A IFN-␥ assay positivity (OR, 1.6; 95% immunodeficiency virus
BCG vaccine scar present 514 (71)
second TST reader independently read CI, 0.9-2.8) but was not statistically Ever had direct contact 493 (68)
254 (35%) of 720 participants and the significant. with a patient with
tuberculosis‡
interrater agreement was excellent Ever lived in a household 40 (6)
(=0.91). TABLE 2 shows the risk fac- Agreement Between TST with a patient with
tors for TST positivity. On multivari- and IFN-␥ Assay Results tuberculosis
*Percentages may not add up to 100 due to rounding.
ate analysis, age (21-30 vs 18-20 years) Data on agreement between the TST and †In India, diploma is completed after high school but is 1
and number of years in the health care IFN-␥ assay results were available for 719 level less than a bachelors degree; therefore, this cat-
egory does not include high school.
profession (⬎5 vs ⱕ1 year) were sta- participants (TABLE 3). Of these, 360 ‡Direct contact was defined as contact between 2 people
that is of sufficient distance to allow conversation be-
tistically significant. Previous BCG vac- (50%) were positive by either test and tween them.
cination was not associated with TST 226 (31%) were positive by both tests.
positivity in bivariate and multivari- With a 10-mm cutpoint, the agreement
ate analyses. was 81.4% ( = 0.61; 95% CI, 0.56- years in health profession, lower edu-
0.67). Agreement was lower when 5-mm cational level, and specific job catego-
IFN-␥ Assay Results and 15-mm cutpoints were used. ries (laboratory staff, orderlies, and at-
Valid IFN-␥ assay results were avail- FIGURE 3 shows the distribution of tending physicians/faculty) were
able for 725 (99%) of 726 participants IFN-␥ assay values by TST category. A associated with greater discordance
(Figure 2). The median IFN-␥ assay level sharp increase in the IFN-␥ assay val- (either positive TST/negative IFN-␥
was 0.11 IU/mL. With a cutpoint of at ues was observed when the induration assay or negative TST/postive IFN-␥ as-
least 0.35 IU/mL, 291 (40%) of 725 par- exceeded 10 mm. FIGURE 4 shows the say) on bivariate analyses. However, on
ticipants were positive (95% CI, 37%- TST distribution by IFN-␥ assay sta- multivariate analysis, only 2 covari-
43%). Table 2 shows the risk factors for tus. The TST distributions are well- ates were important but not statisti-
IFN-␥ assay positivity. On multivariate separated, with a median of 3 mm and cally significant: job category (attend-
analysis, age (ⱖ41 vs 18-20 years), num- 15 mm in the negative IFN-␥ assay and ing physicians/faculty vs medical
ber of years in the health profession (⬎5 positive IFN-␥ assay groups, respec- students: OR, 3.9; 95% CI, 0.9-15.6)
vs ⱕ1 year), and job category (orderlies tively (P⬍.001 for difference between and increasing years in health care (OR,
vs medical students) were significant. medians, using the Wilcoxon rank sum 1.3; 95% CI, 0.6-2.8; 2.01; 95% CI, 0.8-
Previous BCG vaccination was not as- test). 5.4; and 2.1; 95% CI, 0.6-7.5; respec-
sociated with IFN-␥ assay positivity in TABLE 4 shows the agreement data tively) for those participants with 2 to
bivariate and multivariate analyses. stratified by covariates. Increasing age, 5 years, 6 to 10 years, and more than
©2005 American Medical Association. All rights reserved. (Reprinted) JAMA, June 8, 2005—Vol 293, No. 22 2749
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
10 years in the health profession com- tuberculosis-specific antigen–based workers,14,15 these studies did not test
pared with those with 1 year or less. A IFN-␥ assay was expected. The use of for LTBI.
positive TST/negative IFN-␥ assay pat- 1-TU dosage of PPD in our study may The risk factors we identified have
tern of discordance was more fre- have improved TST specificity, as many been shown to be important in several
quently observed with increasing age, countries use a 2-TU dosage.21 Increas- studies.13,25-29 Age and years in health
increasing years in the health care pro- ing age and years in the health profes- care reflect cumulative exposure to
fession, and in specific subgroups sion were risk factors for both IFN-␥ M tuberculosis. Variability of risk
(nurses, laboratory staff, and attend- assay and TST positivity, and the risk across job categories may reflect varia-
ing physicians/faculty). A negative TST/ factor associations were fairly similar tions in exposure frequency and inten-
positive IFN-␥ assay pattern of discor- for both tests. To our knowledge, our sity.28,29 Although direct contact with
dance was more frequently observed in study is the largest evaluation of an patients with tuberculosis has been
those participants with household tu- IFN-␥ assay among health care work- shown to be a risk factor in previous
berculosis contact. However, none of ers in a developing country and the first studies,13,25-27 we did not find a strong
these differences were statistically sig- report of the In-Tube version of the effect. However, this is not surprising
nificant on multivariate analyses (data QuantiFERON-TB Gold assay. This ver- as nearly 70% of our health care work-
not shown). sion of the assay is easier to perform and ers reported direct contact, reducing
facilitates testing of people in remote the predictive ability of this exposure
COMMENT locations. factor. Overall, our findings highlight
Our study demonstrated the expected The high prevalence of LTBI in our the need to study tuberculosis among
high prevalence of LTBI in Indian health study is consistent with estimates from Indian health care workers. India’s
care workers. Although TST and IFN-␥ other developing countries.13,25-27 How- Revised National Tuberculosis Control
assay use different antigen combina- ever, our prevalence of approximately Programme is the largest Directly
tions, it was surprising that these tests 40% might be an underestimate be- Observed Treatment, Short-Course
had comparable prevalence estimates cause we recruited few senior physi- program in the world,16 and the safety
(41% and 40%, respectively) and a high cians who were older and, presum- and well-being of health care workers
level of agreement (81.4%, = 0.61). ably, more frequently exposed to is important for the continued expan-
The marginal bimodal TST distribu- M tuberculosis. Also, our study was not sion of this successful program. Fur-
tion appears to be composed of 2 fairly designed to determine if tuberculosis ther research is needed to document
well-separated component distribu- transmission occurred in the nosoco- the incidence of tuberculosis among
tions of negative and positive IFN-␥ as- mial setting. Although studies from Indian health care workers and deter-
say individuals. Greater discordance be- India have suggested a high rate of mine the rate of nosocomial transmis-
tween the PPD-based TST and the tuberculosis among health care sion. If such studies demonstrate a
Figure 2. Distribution of TST (n=720) and IFN-␥ Assay (n=725) Responses
TST Results IFN-γ Assay Results
12 70
Probability Density
60
10
50
8
Percentage
Percentage
40
6
30
4
20
2
10
0 0
0 5 10 15 20 25 0 2 4 6 8 ≥10
TST Induration, mm IFN-γ, IU/mL
IFN-γ Assay Cutpoint ≥0.35 IU/mL
TST indicates tuberculin skin test; IFN-␥, interferon ␥. The overlaid curve is a plot of the probability density function, a smoothed version of the histogram.
2750 JAMA, June 8, 2005—Vol 293, No. 22 (Reprinted) ©2005 American Medical Association. All rights reserved.
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
Table 2. Covariates Associated With Positive TST and IFN-␥ Assay Results
TST Cutpoint ⱖ10 mm IFN-␥ Assay Cutpoint ⱖ0.35 IU/mL
No. Positive/ OR (95% CI) No. Positive/ OR (95% CI)
Total No. Total No.
Covariate Tested (%) Unadjusted Adjusted* Tested (%) Unadjusted Adjusted*
Age, y
18-20 47/225 (21) 1.00 1.00 50/226 (22) 1.00 1.00
21-30 130/322 (40) 2.56 (1.73-3.79) 1.91 (1.12-3.25) 127/323 (39) 2.28 (1.55-3.35) 1.48 (0.88-2.48)
31-40 49/75 (65) 7.13 (4.02-12.67) 1.75 (0.63-4.80) 42/75 (56) 4.48 (2.57-7.79) 1.43 (0.54-3.80)
ⱖ41 72/98 (73) 10.48 (6.04-18.20) 2.92 (0.94-9.01) 72/101 (71) 8.73 (5.12-14.89) 3.09 (1.04-9.21)
Sex
Male 98/270 (36) 1.00 1.00 102/273 (37) 1.00 1.00
Female 200/450 (44) 1.40 (1.02-1.91) 1.49 (0.96-2.31) 189/452 (42) 1.20 (0.88-1.63) 1.22 (0.78-1.87)
Education level
Medical degree, master’s, 226/617 (37) 1.00 216/618 (35) 1.00
bachelor’s degree,
or diploma
High school or lower 72/103 (70) 4.02 (2.55-6.31) 75/107 (70) 4.36 (2.79-6.81)
Job category
Medical students 52/227 (23) 1.00 1.00 49/227 (22) 1.00 1.00
Nursing students 36/125 (29) 1.36 (0.82-2.23) 1.05 (0.60-1.83) 41/126 (33) 1.75 (1.07-2.85) 1.63 (0.94-2.83)
Interns 8/43 (19) 0.76 (0.33-1.76) 0.43 (0.18-1.06) 12/43 (28) 1.40 (0.67-2.94) 0.87 (0.39-1.91)
Residents 13/30 (43) 2.57 (1.17-5.64) 0.51 (0.19-1.32) 13/30 (43) 2.77 (1.26-6.11) 0.83 (0.32-2.14)
Nurses 104/161 (65) 6.14 (3.92-9.60) 1.55 (0.81-2.95) 88/160 (55) 4.43 (2.84-6.92) 1.56 (0.82-2.96)
Laboratory staff 23/39 (59) 4.83 (2.38-9.83) 0.93 (0.37-2.38) 21/39 (54) 4.23 (2.09-8.57) 1.07 (0.43-2.66)
Orderlies 57/83 (69) 7.37 (4.22-12.88) 1.49 (0.68-3.29) 63/87 (72) 9.53 (5.41-16.8) 2.71 (1.25-5.86)
Attending physicians/faculty 5/12 (42) 2.40 (0.73-7.89) 0.41 (0.10-1.59) 4/13 (31) 1.61 (0.47-5.46) 0.41 (0.10-1.61)
Years served in the
health care profession
ⱕ1 23/95 (24) 1.00 1.00 17/96 (18) 1.00 1.00
2-5 86/343 (25) 1.04 (0.61-1.77) 0.76 (0.42-1.37) 98/343 (29) 1.85 (1.04-3.30) 1.61 (0.86-3.02)
6-10 72/117 (62) 5.00 (2.75-9.11) 2.78 (1.23-6.25) 67/117 (57) 6.22 (3.28-11.80) 4.15 (1.81-9.50)
⬎10 117/165 (71) 7.63 (4.28-13.59) 3.20 (1.08-9.45) 109/169 (65) 8.44 (4.58-15.55) 3.34 (1.13-9.81)
BCG vaccine scar
Absent 87/209 (42) 1.00 90/212 (42) 1.00
Present 211/511 (41) 0.98 (0.71-1.36) 201/513 (39) 0.87 (0.63-1.20)
Direct contact with tuberculosis
No 84/229 (37) 1.00 84/233 (36) 1.00
Yes 214/491 (44) 1.33 (0.96-1.84) 207/492 (42) 1.28 (0.93-1.77)
Household contact
with tuberculosis
No 282/680 (42) 1.00 271/685 (40) 1.00
Yes 16/40 (40) 0.94 (0.49-1.80) 20/40 (50) 1.52 (0.80-2.89)
Abbreviations: CI, confidence interval; IFN-␥, interferon ␥; OR, odds ratio; TST, tuberculin skin test.
*From a multivariate logistic regression model with age, sex, job category, and years in health care as covariates.
problem, control strategies will be
Table 3. Agreement Between TST and IFN-␥ Assay Results (n = 719)
needed to address the issue.
Several studies have compared RD1- TST Cutpoint, mm
based IFN-␥ assays with TST, mostly Results* ⱖ5 ⱖ10 ⱖ15
in low-endemic populations. 8 The Positive TST/positive IFN-␥ assay 259 226 148
agreement in our high-endemic popu- Negative TST/negative IFN-␥ assay 254 359 412
lation (81.4%), interestingly, is consis- Positive TST/negative IFN-␥ assay 177 72 19
tent with those data reported by a ma- Negative TST/positive IFN-␥ assay 29 62 140
jority of the studies.22,30-33 A recent study Agreement, % 71.4 81.4 77.9
on an RD1-based IFN-␥ assay that re- (95% CI) 0.45 (0.39-0.51) 0.61 (0.56-0.67) 0.51 (0.44-0.57)
ported agreement data showed an agree- Abbreviations: CI, confidence interval; IFN-␥, interferon ␥; TST, tuberculin skin test.
*IFN-␥ assay cutpoint was at least 0.35 IU/mL.
ment of 94%, but this analysis in-
©2005 American Medical Association. All rights reserved. (Reprinted) JAMA, June 8, 2005—Vol 293, No. 22 2751
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
cluded participants who had not epidemiological estimate for India of assay uses RD1 antigens, the effect of
received BCG vaccine.22 Only 1 pub- 40%10 and the 41% TST positivity in the NTM on the test should be limited.
lished study has estimated the preva- present study. Differences in IFN-␥ as- However, ESAT-6 and CFP-10 have the
lence of LTBI in India using an IFN-␥ say methodology might explain this dif- potential to cross-react with certain
assay. Lalvani et al34 showed that 80% ference. NTM species,6,30 and it has been sug-
of healthy adults (affluent corporate ex- Although previous studies have gested that cross-reactivity may exist
ecutives) in Bombay (Mumbai) tested shown BCG vaccine to cause a posi- with Mycobacterium leprae.41 Because
enzyme-linked immunospot−positive to tive TST/negative IFN-␥ assay discor- NTM and M leprae are endemic in In-
either ESAT-6 or CFP-10. In contrast, dance,31,35 previous BCG vaccination dia, research is needed to study the
only 40% of our high-risk cohort was had little impact on TST in our study. effect of NTM on IFN-␥ assays.
positive by IFN-␥ assay, in line with the Our study largely comprised adults who Our cross-sectional data suggest that
received BCG vaccine (Danish 1331 both tests are comparable in the popu-
Figure 3. Correlation Between TST and strain) at birth. In individuals vacci- lation we studied. However, this does
IFN-␥ Assay Responses (n=719) nated in infancy, TST response due to not necessarily indicate that these tests
BCG vaccine wanes rapidly.3,5,36,37 An- are completely equivalent because they
≥10
other explanation could be misclassi- do not measure exactly the same im-
8
fication of BCG vaccine status owing to munological phenomenon.35 To put our
the use of scar as a proxy.3,36 Recent tu- findings in context, it is important to
IFN-γ, IU/mL
6 berculin surveys from India, involv- review the evidence on the perfor-
ing more than 100 000 children, have mance characteristics of these tests.
4
also shown the BCG vaccination does The TST has moderate to high sensi-
2 not influence the estimation of annual tivity and specificity, depending on the
risk of infection.36,38,39 However, BCG population screened, with specificity
0
vaccine might have an effect on TST in being more unpredictable.2-5 Several
0-4 5-9 10-14 15-19 >19 other populations, depending on vac- studies have shown a positive associa-
TST Induration, mm
cine strain, timing, frequency, and time tion between TST response and subse-
TST indicates tuberculin skin test; IFN-␥, interferon ␥. since vaccination.4,5,37 Infection with quent risk of active tuberculosis,2,4,42,43
The boxes, which indicate the distribution of IFN-␥ val- NTM, which tends to cause nonspe- and randomized trials have shown that
ues for each category of TST induration, are bordered
at the 25th and 75th percentiles of the IFN-␥ values, cific tuberculin sensitivity, is highly treatment of LTBI, diagnosed using TST,
with a median line at the 50th percentile. Outliers are prevalent in India.3,40 Therefore, NTM reduces the risk of active tuberculosis by
not displayed. IFN-␥ values of more than 10 IU/mL are
displayed as 10 IU/mL. The horizontal dotted line in- infection might have caused false- 60% to 90%.19 Furthermore, the TST is
dicates the IFN-␥ assay cutpoint of 0.35 IU/mL. positive TST results. Because the IFN-␥ a simple test with low material costs that
does not require a laboratory, but does
require skilled testers.
Figure 4. Distribution of TST Responses by IFN-␥ Assay Status (n=719)
The RD1-based IFN-␥ assays have
12
higher specificity than TST, better cor-
relation with exposure to M tuberculo-
Probability Density sis than TST, no cross-reactivity due to
Negative IFN-γ Assay Result
10 BCG vaccination, and limited cross-
Positive IFN-γ Assay Result
reactivity due to NTM infection.6-9,22,23,31,35
8 Other advantages include rapidity, the
need for only a single visit, avoidance of
Percentage
subjective measurements, and boost-
6
ing.6,7,35 There is limited evidence of an
association between IFN-␥ assay re-
4 sponse to ESAT-6 and subsequent pro-
gression to active tuberculosis among
2
contacts of patients with tuberculosis.44
To date, no trial has demonstrated the
efficacy of treatment based on IFN-␥ as-
0 say results. A limitation of IFN-␥ assays
0 5 10 15 20 25
TST Induration, mm is its higher material costs and the need
for laboratory infrastructure.8 Also, IFN-␥
TST indicates tuberculin skin test; IFN-␥, interferon ␥. The overlaid curves are plots of the probability density assays have been inadequately evalu-
functions, smoothed versions of the histograms.
ated in children, individuals with im-
2752 JAMA, June 8, 2005—Vol 293, No. 22 (Reprinted) ©2005 American Medical Association. All rights reserved.
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
munosuppressive conditions, and in population this may be difficult. Be- might have led to an underestimation
high-burden countries.8 cause of the cross-sectional design and of LTBI prevalence, it is unlikely to
Our study has several limitations. the lack of follow-up data, we were un- affect the comparisons between TST
Unlike the previous IFN-␥ assay stud- able to adequately resolve the discor- and the IFN-␥ assay. Unfortunately, due
ies in outbreak and contact investiga- dance between the 2 tests. to lack of data from nonparticipants, we
tions,22,31-33 we were unable to quan- We were also unable to measure im- could not compare their characteris-
tify duration and proximity of contact portant covariates, such as NTM and tics with those who did participate.
with patients with tuberculosis. Such human immunodeficiency virus infec- Although consistent with the In-
exposure measures might have en- tion. Information on human immuno- dian policy, the use of 1-TU dose of PPD
abled us to evaluate whether the IFN-␥ deficiency virus status would have RT23 limits our ability to compare our
assay was better associated with in- helped to better evaluate the perfor- data with studies that have used 2-TU
creasing exposure than TST, although mance of the IFN-␥ assay. Although dosages. Our study consisted of health
in a high prevalence health care worker nonresponse among senior physicians care workers in a high prevalence coun-
Table 4. Discordance Between TST and IFN-␥ Assay Results*
%
Agreement Between No. of
TST and IFN-␥ Assay Discordant Positive TST/ Negative TST/ Positive TST/ Negative TST/
Results / Total Positive Negative Negative Positive
Covariates % (95% CI) No. Tested IFN-␥ Assay IFN-␥ Assay IFN-␥ Assay IFN-␥ Assay
Age, y
18-20 85.3 0.57 (0.43-0.70) 33/225 14 71 7 8
21-30 81.9 0.62 (0.54-0.71) 58/321 31 51 10 8
31-40 77.3 0.53 (0.34-0.72) 17/75 49 28 16 7
ⱖ41 73.5 0.34 (0.13-0.54) 26/98 59 14 14 12
Sex
Male 81.1 0.59 (0.49-0.69) 51/270 27 54 9 10
Female 81.5 0.62 (0.55-0.70) 83/449 34 48 11 8
Education level
Medical degree, master’s, 82.6 0.62 (0.56-0.69) 107/616 27 56 10 8
bachelor’s degree,
or diploma
High school or lower 73.8 0.37 (0.18-0.57) 27/103 57 17 13 14
Job category
Medical students 85.5 0.58 (0.45-0.71) 33/227 15 70 8 7
Nursing students 81.6 0.57 (0.41-0.72) 23/125 22 60 7 11
Interns 90.7 0.74 (0.51-0.97) 4/43 19 72 0 9
Residents 86.7 0.73 (0.48-0.98) 4/30 37 50 7 7
Nurses 80.0 0.59 (0.46-0.71) 32/160 50 30 15 5
Laboratory staff 69.2 0.38 (0.08-0.67) 12/39 41 28 18 13
Orderlies 75.9 0.42 (0.20-0.63) 20/83 59 17 10 14
Attending physicians/faculty 50.0 −0.09 (−0.60 to 0.42) 6/12 8 42 33 17
Years served in the
health care profession
ⱕ1 87.4 0.62 (0.43-0.81) 12/95 15 73 9 3
2-5 84.3 0.60 (0.50-0.70) 54/343 19 65 6 10
6-10 77.6 0.54 (0.38-0.69) 26/116 48 29 14 9
⬎10 74.6 0.42 (0.27-0.56) 42/165 55 19 16 10
BCG vaccine scar
Absent 84.2 0.68 (0.57-0.78) 33/209 34 50 8 8
Present 80.2 0.59 (0.52-0.66) 101/510 30 50 11 9
Direct contact with tuberculosis
No 81.7 0.60 (0.50-0.71) 42/229 27 55 10 9
Yes 81.2 0.62 (0.55-0.69) 92/490 33 48 10 9
Household contact
with tuberculosis
No 81.4 0.61 (0.55-0.67) 126/677 31 50 10 8
Yes 80.0 0.60 (0.36-0.84) 8/40 35 45 5 15
Abbreviations: CI, confidence interval; IFN-␥, interferon ␥; TST, tuberculin skin test.
*TST cutpoint was at least 10 mm and IFN-␥ assay cutpoint was at least 0.35 IU/mL.
©2005 American Medical Association. All rights reserved. (Reprinted) JAMA, June 8, 2005—Vol 293, No. 22 2753
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
try. Although this may limit our abil- other populations. To fully evaluate the REFERENCES
ity to generalize the results to settings use of IFN-␥ assays, long-term cohort 1. Dye C, Scheele S, Dolin P, Pathania V, Raviglione
with different baseline prevalences, we studies to determine the association be- MC. Consensus statement: global burden of tuber-
culosis: estimated incidence, prevalence, and mortal-
believe our data will be helpful in un- tween positive IFN-␥ assay results and ity by country: WHO Global Surveillance and Moni-
derstanding the performance of IFN-␥ the subsequent risk of active tuberculo- toring Project. JAMA. 1999;282:677-686.
2. Huebner RE, Schein MF, Bass JB Jr. The tuberculin
assays in high-burden settings for which sis are required in diverse settings.8 If skin test. Clin Infect Dis. 1993;17:968-975.
data are scarce.8 such studies demonstrate a strong con- 3. Chadha VK. Tuberculin test. Indian J Pediatr. 2001;
68:53-58.
In conclusion, our study showed a sistent association, IFN-␥ assays might 4. Menzies RI. Tuberculin skin testing. In: Reichman
high prevalence of LTBI in Indian health have the potential to replace TST. LB, Hershfield ES, eds. Tuberculosis: A Comprehen-
care workers and high agreement be- sive International Approach. New York, NY: Marcel
Author Contributions: Dr Pai had full access to all of the Dekker; 2000:279-322.
tween TST and an RD1-based IFN-␥ as- data in the study and takes responsibility for the integ- 5. Rieder HL. Epidemiologic Basis of Tuberculosis
say. Our results and the available evi- rity of the data and the accuracy of the data analysis. Control. Paris, France: International Union Against Tu-
Study concept and design: Pai, Kalantri, Narang, Daley, berculosis and Lung Disease; 1999.
dence suggest that both tests have Granich, Mazurek, Riley, Colford. 6. Andersen P, Munk ME, Pollock JM, Doherty TM.
advantages and limitations and, as of this Acquisition of data: Pai, Gokhale, Joshi, Dogra, Kalantri, Specific immune-based diagnosis of tuberculosis.
Mendiratta, Granich. Lancet. 2000;356:1099-1104.
time, both may have a useful role, de- Analysis and interpretation of data: Pai, Joshi, Kalantri, 7. Lalvani A. Spotting latent infection: the path to bet-
pending on factors unique to each set- Narang, Granich, Mazurek, Reingold, Riley, Colford. ter tuberculosis control. Thorax. 2003;58:916-918.
ting. The emergence of IFN-␥ assays is Drafting of the manuscript: Pai, Kalantri, Colford. 8. Pai M, Riley LW, Colford JM. Interferon-␥ assays
Critical revision of the manuscript for important in- in the immunodiagnosis of tuberculosis: a systematic
a welcome development that has ex- tellectual content: Pai, Gokhale, Joshi, Dogra, Kalantri, review. Lancet Infect Dis. 2004;4:761-776.
panded the armamentarium of LTBI di- Mendiratta, Narang, Daley, Granich, Mazurek, Rein- 9. Mazurek GH, Villarino ME. Guidelines for using the
gold, Riley, Colford. QuantiFERON-TB test for diagnosing latent Myco-
agnostics. The decision to select one or Statistical analysis: Pai, Colford. bacterium tuberculosis infection. Centers for Disease
the other test will depend on the popu- Obtained funding: Pai, Reingold. Control and Prevention. MMWR Recomm Rep. 2003;
Administrative, technical, or material support: Gokhale, 52(RR-2):15-18.
lation, the goal of testing, and the re- Joshi, Dogra, Mendiratta, Narang, Granich, Mazurek, 10. Chadha VK. Epidemiological situation of tubercu-
sources available. For example, for se- Reingold, Riley, Colford. losis in India. J Indian Med Assoc. 2003;101:144-147.
Study supervision: Pai, Joshi, Kalantri, Mendiratta, 11. Khatri GR, Frieden TR. Controlling tuberculosis in
rial testing of health care workers, the Daley, Granich, Reingold, Riley, Colford. India. N Engl J Med. 2002;347:1420-1425.
IFN-␥ assay will be appropriate. It will Financial Disclosures: None of the investigators have 12. Chadha VK, Kumar P, Jagannatha PS, Vaidya-
eliminate the need for repeat visits, avoid any financial interest in or a financial conflict with the nathan PS, Unnikrishnan KP. Average annual risk of
subject matter or materials discussed in this manu- tuberculous infection in India. Int J Tuberc Lung Dis.
boosting, and minimize interpreta- script. Patent protection for incubation of whole blood 2005;9:116-118.
tional difficulties. Because of its high and antigens within the collection tube that contains 13. World Health Organization. Guidelines for the Pre-
a gel plug for subsequent plasma separation and stor- vention of Tuberculosis in Health Care Facilities in
specificity, RD1-based assays will be age may be requested by the US Centers for Disease Resource-Limited Settings. Geneva, Switzerland: World
helpful in populations where cross- Control and Prevention, listing Gerald Mazurek, MD, Health Organization; 1999.
as one of the inventors. 14. Rao KG, Aggarwal AN, Behera D. Tuberculosis
reactivity due to BCG vaccine and NTM Funding/Support: Dr Pai was supported by a doctoral among physicians in training. Int J Tuberc Lung Dis.
pose problems in TST interpretation training fellowship from the Fogarty AIDS International 2004;8:1392-1394.
and/or where true tuberculosis infec- Training and Research Program (grant 1-D43-TW00003- 15. Gopinath KG, Siddique S, Kirubakaran H, Shan-
16). QuantiFERON-TB Gold diagnostic kits were pro- mugam A, Mathai E, Chandy GM. Tuberculosis among
tion rate is relatively low. Furthermore, vided by Cellestis Limited, Carnegie, Australia. healthcare workers in a tertiary-care hospital in South
the IFN-␥ assay may be helpful in screen- Role of the Sponsor: The Fogarty AIDS International India. J Hosp Infect. 2004;57:339-342.
Training and Research Program had no role in the study 16. Granich R, Chauhan LS. Status report of the Re-
ing populations in which low return rates design, conduct, collection, management, analysis, or vised National Tuberculosis Control Programme: Janu-
for TST reading are a concern. interpretation of the data, or preparation, review, or ary 2003. J Indian Med Assoc. 2003;101:150-151, 156.
approval of the manuscript. The Cellestis Limited Chief 17. Narang P, Tyagi NK, Mendiratta DK, Jajoo UN,
On the other hand, in high-burden, re- Scientific Officer provided input in study design and Bharambhe MS, Nayar S. Prevalence of sputum-
source-limited settings, the TST might laboratory aspects of the QuantiFERON-TB Gold as- positive pulmonary tuberculosis in tribal and non-
serve a useful purpose. In India, the TST say. This company did not provide funding for this tribal populations of the Ashti and Karanja tahsils in
study and had no role in the conduct, collection, man- Wardha district, Maharashtra State, India. Int J Tu-
is widely used in diagnosing childhood agement, analysis, or interpretation of the data, or berc Lung Dis. 1999;3:478-482.
tuberculosis,3,20 and in epidemiological preparation, review, or approval of the manuscript. 18. Chadha VK, Jagannatha PS, Narang P, Savanur
Previous Presentation: Presented in part at the An- SJ, Mendiratta DK, Lakshminarayana . Annual risk of
studies on annual risk of infection in nual International Conference of the American Tho- tuberculous infection in three districts of Maharashtra.
which blood testing will be diffi- racic Society, San Diego, Calif, May 22, 2005. Indian J Tuberc. 2003;50:125-132.
Acknowledgment: We thank all the health care work- 19. American Thoracic Society. Targeted tuberculin
cult.3,10,12,18,21,36 In India, a 15-year fol- ers at Mahatma Gandhi Institute of Medical Sciences testing and treatment of latent tuberculosis infection.
low-up of 280 000 individuals showed hospital, Sevagram, India, for their participation; Pad- Am J Respir Crit Care Med. 2000;161:S221-S247.
makar Dhone, BSc, Santosh Chavhan, BSW, Prashant 20. Revised National Tuberculosis Control Programme.
that TST response is significantly asso- Raut, BA, Vaishali Naik, BSc, Sandeep Taksande, DMLT, Technical Guidelines for Tuberculosis Control. New
ciated with development of active tuber- and Varsha Taksande, Dip Radio, for working on this Delhi, India: Central TB Division, Directorate General
culosis.42 Our findings and evidence from project; James Rothel, PhD, Vineet Chadha, MD, and of Health Services; 1997.
Hajib Madhavan, MD, for technical assistance and help- 21. Chadha VK, Jagannatha PS, Vaidyanathan PS,
Indian studies3,10,18,21,36 suggest that the ful discussions; and Robert Jasmer, MD, Vineet Chadha, Jagota P. PPD RT23 for tuberculin surveys in India.
TST remains a useful test, particularly be- MD, Jacqueline Tulsky, MD, Dick Menzies, MD, and Int J Tuberc Lung Dis. 2003;7:172-179.
Marcel Behr, MD, for reviewing the manuscript. We 22. Brock I, Weldingh K, Lillebaek T, Follmann F,
cause of the low cost and since BCG vac- are also grateful to colleagues at the US Centers for Dis- Andersen P. Comparison of tuberculin skin test and
cine has a limited effect on TST.36,38,39 The ease Control and Prevention, for reviewing the manu- new specific blood test in tuberculosis contacts. Am J
script: Kenneth Castro, MD, Michael Iademarco, MD, Respir Crit Care Med. 2004;170:65-69.
relationship between BCG vaccine and Charles Wells, MD, Kayla Laserson, ScD, Andrew Ver- 23. Mori T, Sakatani M, Yamagishi F, et al. Specific
subsequent TST response may vary in non, MD, and Jose Becerra, MD. detection of tuberculosis infection: an interferon-
2754 JAMA, June 8, 2005—Vol 293, No. 22 (Reprinted) ©2005 American Medical Association. All rights reserved.
Downloaded from jama.ama-assn.org by guest on March 23, 2011
TUBERCULOSIS AMONG INDIAN HEALTH CARE WORKERS
gamma-based assay using new antigens. Am J Respir 31. Ewer K, Deeks J, Alvarez L, et al. Comparison of sitivity among children vaccinated with BCG under uni-
Crit Care Med. 2004;170:59-64. T-cell-based assay with tuberculin skin test for diagno- versal immunization programme. Indian J Pediatr.
24. Hosmer D, Lemeshow S. Applied Logistic sis of Mycobacterium tuberculosis infection in a school 2004;71:1063-1068.
Regression. New York, NY: John Wiley & Sons; 2000. tuberculosis outbreak. Lancet. 2003;361:1168-1173. 39. Chadha VK, Jagannatha PS, Kumar P. Can
25. Alonso-Echanove J, Granich RM, Laszlo A, et al. 32. Hill PC, Brookes RH, Fox A, et al. Large-scale evalu- BCG-vaccinated children be included in tuberculin
Occupational transmission of Mycobacterium tuber- ation of enzyme-linked immunospot assay and skin surveys to estimate the annual risk of tuberculous
culosis to health care workers in a university hospital test for diagnosis of Mycobacterium tuberculosis in- infection in India? Int J Tuberc Lung Dis. 2004;8:
in Lima, Peru. Clin Infect Dis. 2001;33:589-596. fection against a gradient of exposure in The Gambia. 1437-1442.
26. Do AN, Limpakarnjarat K, Uthaivoravit W, et al. Clin Infect Dis. 2004;38:966-973. 40. Chakraborty AK, Ganapathy KT, Nair SS, Bhus-
Increased risk of Mycobacterium tuberculosis infec- 33. Richeldi L, Ewer K, Losi M, et al. T cell-based track- han K. Prevalence of non-specific sensitivity of tuber-
tion related to the occupational exposures of health ing of multidrug resistant tuberculosis infection after culin in a South Indian rural population. Indian J Med
care workers in Chiang Rai, Thailand. Int J Tuberc Lung brief exposure. Am J Respir Crit Care Med. 2004;170: Res. 1976;64:639-651.
Dis. 1999;3:377-381. 288-295. 41. Geluk A, van Meijgaarden KE, Franken KL, et al.
27. Kassim S, Zuber P, Wiktor SZ, et al. Tuberculin 34. Lalvani A, Nagvenkar P, Udwadia Z, et al. Enu- Identification and characterization of the ESAT-6 ho-
skin testing to assess the occupational risk of Myco- meration of T cells specific for RD1-encoded anti- mologue of Mycobacterium leprae and T-cell cross-
bacterium tuberculosis infection among health care gens suggests a high prevalence of latent Mycobac- reactivity with Mycobacterium tuberculosis. Infect
workers in Abidjan, Cote d’Ivoire. Int J Tuberc Lung terium tuberculosis infection in healthy urban Indians. Immun. 2002;70:2544-2548.
Dis. 2000;4:321-326. J Infect Dis. 2001;183:469-477. 42. Radhakrishna S, Frieden TR, Subramani R. Asso-
28. Menzies D, Fanning A, Yuan L, FitzGerald JM. Fac- 35. Mazurek GH, LoBue PA, Daley CL, et al. Compari- ciation of initial tuberculin sensitivity, age and sex with
tors associated with tuberculin conversion in Cana- son of a whole-blood interferon-␥ assay with tubercu- the incidence of tuberculosis in south India: a 15-
dian microbiology and pathology workers. Am J Respir lin skin testing for detecting latent Mycobacterium tu- year follow-up. Int J Tuberc Lung Dis. 2003;7:1083-
Crit Care Med. 2003;167:599-602. berculosis infection. JAMA. 2001;286:1740-1747. 1091.
29. Sepkowitz KA. Tuberculin skin testing and the 36. Chadha VK, Jagannatha PS, HV S. Tuberculin sen- 43. Watkins RE, Brennan R, Plant AJ. Tuberculin re-
health care worker: lessons of the Prophit Survey. Tu- sitivity in BCG vaccinated children and its implication activity and the risk of tuberculosis: a review. Int J Tu-
ber Lung Dis. 1996;77:81-85. for ARI estimation. Indian J Tuberc. 2000;47:139-146. berc Lung Dis. 2000;4:895-903.
30. Arend SM, van Meijgaarden KE, de Boer K, et al. 37. Wang L, Turner MO, Elwood RK, Schulzer M, 44. Doherty TM, Demissie A, Olobo J, et al. Immune
Tuberculin skin testing and in vitro T cell responses to FitzGerald JM. A meta-analysis of the effect of Bacille responses to the Mycobacterium tuberculosis-
ESAT-6 and culture filtrate protein 10 after infection Calmette Guerin vaccination on tuberculin skin test specific antigen ESAT-6 signal subclinical infection
with Mycobacterium marinum or M kansasii. J In- measurements. Thorax. 2002;57:804-809. among contacts of tuberculosis patients. J Clin
fect Dis. 2002;186:1797-1807. 38. Chadha VK, Jaganath PS, Kumar P. Tuberculin sen- Microbiol. 2002;40:704-706.
There is an art of reading, as well as an art of think-
ing, and an art of writing.
—Isaac D’Israeli (1766-1848)
©2005 American Medical Association. All rights reserved. (Reprinted) JAMA, June 8, 2005—Vol 293, No. 22 2755
Downloaded from jama.ama-assn.org by guest on March 23, 2011
Вам также может понравиться
- Paper - Iii Law of Torts (Paper Code: K-103) : Books RecommendedДокумент1 страницаPaper - Iii Law of Torts (Paper Code: K-103) : Books Recommendedvivek6593Оценок пока нет
- Fundamentals of Human Neuropsychology 7th Edition Kolb Test BankДокумент26 страницFundamentals of Human Neuropsychology 7th Edition Kolb Test BankDanielYoungabrn100% (60)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (894)
- Ethics Lecture Notes For Academic Year - Situation 1 Your Family Is An Exclusive Vacation On A - StuDocuДокумент1 страницаEthics Lecture Notes For Academic Year - Situation 1 Your Family Is An Exclusive Vacation On A - StuDocuRaveine JabatОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- SSC 146G Summer 2016 Human Sexuality SyllabusДокумент1 страницаSSC 146G Summer 2016 Human Sexuality SyllabusJames SmithОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- Commercial Bank of Africa Market ResearchДокумент27 страницCommercial Bank of Africa Market Researchprince185Оценок пока нет
- Draft Resolution 1.1 SPECPOL LUMUN 2013Документ8 страницDraft Resolution 1.1 SPECPOL LUMUN 2013Hamza Hashim100% (1)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- COOKERY Grade 9 (Q1-W1)Документ2 страницыCOOKERY Grade 9 (Q1-W1)Xian James G. YapОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Learning Disabilities in The ClassroomДокумент5 страницLearning Disabilities in The ClassroomekielaszekОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- NOGALES Math Files for Elementary SchoolДокумент3 страницыNOGALES Math Files for Elementary SchoolMl Phil100% (6)
- Court Document SummaryДокумент15 страницCourt Document SummaryAkAsh prAkhAr vErmA100% (1)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- CS201 Midterm Solved MCQs With ReferenceДокумент4 страницыCS201 Midterm Solved MCQs With Referencegenome companyОценок пока нет
- Wildlife Ecology - Unit 14 - Week (12) - RevisionДокумент1 страницаWildlife Ecology - Unit 14 - Week (12) - RevisionAdityaОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- CSEC English B June 2013 P2Документ7 страницCSEC English B June 2013 P2Jhanett RobinsonОценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- José Rizal: The Life of The National HeroДокумент9 страницJosé Rizal: The Life of The National HeroMark Harry Olivier P. VanguardiaОценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2219)
- SRDF S LabДокумент9 страницSRDF S LabUma SekharОценок пока нет
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- 1 Unpacking The SelfДокумент13 страниц1 Unpacking The SelfJEMABEL SIDAYENОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Tanada, Et Al. Vs Angara, Et Al., 272 SCRA 18, GR 118295 (May 2, 1997)Документ3 страницыTanada, Et Al. Vs Angara, Et Al., 272 SCRA 18, GR 118295 (May 2, 1997)Lu CasОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (265)
- Daily Aspirin Therapy Understand The Benefits and RisksДокумент5 страницDaily Aspirin Therapy Understand The Benefits and RisksNicholas OwensОценок пока нет
- Unit 8Документ2 страницыUnit 8The Four QueensОценок пока нет
- College Resume TemplateДокумент7 страницCollege Resume Templatevofysyv1z1v3100% (1)
- Lesson PlanДокумент8 страницLesson PlanNunette SenilloОценок пока нет
- Laertes' Temper: Definition of DiacopeДокумент27 страницLaertes' Temper: Definition of DiacopeAhmad Abdellah ElsheemiОценок пока нет
- Holy Trinity University: Puerto Princesa City Basic Education DepartmentДокумент2 страницыHoly Trinity University: Puerto Princesa City Basic Education DepartmentBrian Reyes GangcaОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Affidavit of DesistanceДокумент6 страницAffidavit of Desistancesalasvictor319Оценок пока нет
- Accenture 2014 Celent Claims ABCD Acn Duck Creek Dec14Документ28 страницAccenture 2014 Celent Claims ABCD Acn Duck Creek Dec14Ainia Putri Ayu KusumaОценок пока нет
- ISO/IEC 20000 Lead Implementer Course (5 Days)Документ3 страницыISO/IEC 20000 Lead Implementer Course (5 Days)rohitbanerjeeОценок пока нет
- 1201 CCP Literature ReviewДокумент5 страниц1201 CCP Literature Reviewapi-548148057Оценок пока нет
- Significance of Research in Education - Research ArticleДокумент18 страницSignificance of Research in Education - Research ArticleSalex E. AliboghaОценок пока нет
- Factors Affecting Customer Loyalty to Indosat OoredooДокумент13 страницFactors Affecting Customer Loyalty to Indosat OoredooDede BhubaraОценок пока нет
- Seduction As A Manipulation TacticДокумент6 страницSeduction As A Manipulation TacticByrlyne Van DykeDowersОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (119)