Академический Документы
Профессиональный Документы
Культура Документы
Diagnosis and Management of Depression in Primary Care
Загружено:
Maria Jose OcИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Diagnosis and Management of Depression in Primary Care
Загружено:
Maria Jose OcАвторское право:
Доступные форматы
Diagnosis and management
of depression in primary care:
a clinical update and review
Review
Synthèse
Ronald A. Remick
Abstract Dr. Remick is a consultant
psychiatrist with the
THERE HAS BEEN SIGNIFICANT PROGRESS in the area of mood disorders over the last 2 Department of Psychiatry,
decades, encompassing advances in our knowledge of epidemiology, diagnosis, St. Paul’s Hospital,
pathogenesis and treatment. This article presents a clinically oriented update and Vancouver, BC.
review on the diagnosis and management of major depressive disorder.
This article has been peer reviewed.
CMAJ 2002;167(11):1253-60
M
ood disorders are among the most common afflictions that bring patients
to doctors. Almost 20% of adults will have a mood disorder requiring
treatment during their lifetime, and about 8% of adults will have a major
depressive disorder during their lives.1
There are no pathognomonic markers of depression, although this is an area of
active research.2 Diagnosis both in clinical practice and in clinical research studies is
based on a set of specific signs and symptoms (Table 1). These criteria have helped
distinguish various mood disorders that may have different causes and that certainly
require different clinical management.
In this review I focus on major depressive disorders. Closely related illnesses
that are not discussed are dysthymic disorders and bipolar illnesses, which have
lifetime rates of occurrence in the North American population of 8% and 2% re-
spectively.6 As well, I do not discuss depressive syndromes induced by substance
abuse or associated with a general medical condition. Useful review articles are
available.7
Epidemiologic characteristics
As noted above, depressive disorders are common. Most clinicians will be in-
volved in the care of these patients. Depression is twice as common in women as
in men.1,8 The risk of a major depression increases 1.5 to 3.0 times if the illness is
present in a first-degree relative as compared with no such illness in a first-degree
relative.4,5
Surprisingly, for such a common disease there is little agreement on the asso-
ciation between age and onset. This is due to the fact that research is hampered
by the absence of an unambiguous and universally agreed on set of diagnostic cri-
teria and the fact that many of the studies have included patients already in the
medical care system. It is well known that many people who meet the diagnostic
criteria for depression do not seek treatment. A recent Canadian study using data
from the National Population Health Survey suggests that the highest rates of
first onset of depression (1.4%–9.1% of the population) occur among young
adults (aged 12 to 24), and lower rates (1.3%–1.8%) occur among people 65 years
of age or more.9
Depressive illnesses carry significant risks of death and disability. About 15% of
patients with a mood disorder die by their own hand,10 and at least 66% of all sui-
cides are preceded by depression. Rates of suicide in Canada are higher than those
in the United States.11
Depressive disorders are associated with poor work productivity, as indicated
by a 3-fold increase in the number of sick days in the month preceding the illness
for workers with a depressive illness compared with coworkers who did not have
such an illness.12,13 Depressive illnesses also affect family members and care-
CMAJ • NOV. 26, 2002; 167 (11) 1253
© 2002 Canadian Medical Association or its licensors
Remick
givers,14 and there is increasing evidence that children of creased heart rate variability (perhaps a consequence of im-
women with depression have increased rates of problems balance in autonomic tone), and immune system activation
in school and with behaviour, and have lower levels of so- and hypercortisolemia as stressor responses to depression.21
cial competence and self-esteem than their classmates An unhealthy lifestyle may also be more common among
with mothers who do not have depression.15 Depression is depressed people.21 Whatever the cause, the accumulating
the leading cause of disability and premature death among data strongly suggest that clinicians should be alert to de-
people aged 18 to 44 years, and it is expected to be the pression occurring in the context of other acute and
second leading cause of disability for people of all ages by chronic diseases. There is as yet no evidence that treatment
2020.16,17 of mild, clinically unapparent depressive symptoms in these
Depressive illnesses have also been shown to be associ- settings will alter the clinical course of the underlying dis-
ated with increased rates of death and disability from car- ease. Nonetheless, when depression is diagnosed in the
diovascular disease.18–21 Among 1551 study subjects with- presence of other diseases, treatment should be considered
out a history of heart disease who were followed for 13 and discussed with the patient.
years, the odds ratio for acute myocardial infarction
among the subjects who had a major depressive episode Etiology
was 4.5 times higher than among those who did not have
a depressive episode.19 Among consecutive patients admit- Depression is thought to result from disruption of the
ted to hospital with an acute myocardial infarction who normal brain neurochemistry. Work in this area has led to
had their mood measured with a standard depression rat- the development of new drugs to treat depression. These
ing scale, even those with minimal symptoms of depres- drugs appear to affect a number of central monoamine neu-
sion had evidence of higher subsequent risk of death fol- rotransmitters. Central norepinephrine neural pathways are
lowing their infarction and over the next 4 months.20 This likely involved in activities of vigilance, motivation and
risk was independent of other major risk factors, includ- general levels of energy. These pathways share a role with
ing age, ventricular ejection fraction and the presence of serotonin neural pathways in affecting anxiety and irritabil-
diabetes mellitus. ity. Serotonin neural pathways appear to control or have a
These and other findings are intriguing and are the sub- role in controlling impulsivity and share a role with the
ject of much ongoing research. Although the association dopamine pathways in appetite, sex and aggression. Our
was initially considered to be spurious, current mechanistic growing knowledge in this area helps us understand the eti-
explanations include impaired platelet functioning, de- ology and pharmacotherapy of mood disorders.
Current theories of depression are complex and beyond
the scope of this review.22–24 Fig. 1 outlines some of these
Table 1: Diagnostic criteria for major depressive disorder* theories. We are now aware that “long-term” (i.e., 30 days)
A. The patient has depressed mood (e.g., sad or empty feeling) or loss antidepressant treatment results in sustained activation of
of interest or pleasure most of the time for 2 or more weeks plus 4 cyclic adenosine 3-5-monophosphate (cAMP) in specific
or more of the following symptoms brain regions. Protein kinase A, which is stimulated by
Sleep IInsomnia or hypersomnia nearly every day cAMP, phosphorylates the cAMP regulatory element bind-
Interest IMarkedly diminished interest or pleasure in nearly ing protein. This protein then regulates and activates spe-
all activities most of the time cific target genes, including brain-derived neurotrophic
Guilt IExcessive or inappropriate feelings of guilt or factor (BDNF), a neuroprotective factor that results in hip-
worthlessness most of the time pocampal nerve growth (Fig. 1). Psychological stress, im-
Energy ILoss of energy or fatigue most of the time portant in the pathogenesis of depression, can decrease the
Concentration IDiminished ability to think or concentrate; production of BDNF and result in hippocampal neuronal
indecisiveness most of the time atrophy.23,24 Furthermore, a series of brain-imaging studies
Appetite IIncrease or decrease in appetite consistently showed reduced neuronal activity in the dorso-
Psychomotor IObserved psychomotor agitation/retardation lateral prefrontal cortex that covaried with the severity of
Suicide IRecurrent thoughts of death/suicidal ideation the depression (i.e., the more severe the depression, the
larger the prefrontal deficits).25 Thus, an updated hypothe-
B. The symptoms do not meet criteria for a mixed episode (major
depressive episode and manic episode) sis on the development of a depressive disorder might posit
that stress-induced vulnerability in genetically susceptible
C. The symptoms cause clinically significant distress or impairment in people may induce a cascade of intracellular neuronal
social, occupational, or other important areas of functioning
mechanisms that increase or decrease specific neurotrophic
D. The symptoms are not due to the direct physiological effects of a factors necessary for the survival and function of specific
substance (e.g., a drug of abuse, a medication) or a general medical
brain neurons. Furthermore, not only antidepressants but
condition
also electroconvulsive therapy26 and depression-focused
E. The symptoms are not better accounted for by bereavement psychotherapy27 can affect neuronal growth and regional
*Adapted from the Diagnostic and Statistical Manual of Mental Disorders, 4th edition.3 brain metabolism.
1254 JAMC • 26 NOV. 2002; 167 (11)
Diagnosis and management of depression
Some of the neurotransmitters that
are thought to be involved in the etiol- Mossy fibre
ogy of depression are outlined in Fig. 2, pathway Dentate
which emphasizes the interactions or Hippocampus gyrus
“cross talk” that probably occur.28 Granule
Schaffer collateral
cell
Principles of management
CA3
Recognition of the disease
CA1
Despite its high prevalence, only one-
third of all patients with depression re-
ceive adequate treatment.29 The follow- Normal Stress Antidepressants
ing are 4 common clinical errors that
lead to diagnostic or treatment failures
Glucocorticoids Serotonin and NE
associated with depressive disorders:
• Insufficient questioning. Diagnostic BDNF BDNF
failures occur when the patient is Glucocorticoids
not asked questions that may elicit Normal Atrophy
survival or death
the symptoms of a mood disorder and growth of neurons Increased survival
despite what should be a high index and growth
of suspicion based on its prevalence. Hippocampal
The mnemonic “SIGECAPS” neurons
(sleep, interest, guilt, energy, con-
centration, appetite, psychomotor,
suicide) (Table 1) may be a useful
clinical adjunct (i.e., 4 or more
SIGECAPS for major depression, 2
or 3 SIGECAPS for dysthymia).
• Failure to consult a family member. Injury or death
Owing to the cognitive distortions Genetic
Other
associated with the disease, it is not factors
neuronal insults:
Paulette Dennis
unusual for patients to minimize or •Hypoxia-ischemia •Hypoglycemia
exaggerate their symptoms. Thus, •Neurotoxins •Virusues
in patients who are relatively new
to one’s practice, it is risky at best Fig. 1: A molecular and cellular model for the action of antidepressant treatments and the
to make (or exclude) a diagnosis of pathophysiology of stress-related disorders. This model of the hippocampus shows the
depression without collateral infor- major cell types in the hippocampus and how stress and antidepressant treatments may
mation from a relative, such as a influence CA3 pyramidal cells. The 3 major subfields of the hippocampus (CA3 and CA1
spouse or parent. pyramidal cells and dentate gyrus granule cells) are connected by the mossy fibre and
• Acceptance of a diagnosis of a mood Schaffer collateral pathways. Recent studies demonstrate that chronic stress decreases
disorder despite lack of diagnostic the expression of brain-derived neurotrophic factor (BDNF) in the hippocampus. This
criteria (e.g., starting treatment for may contribute to the atrophy or death of neurons in the CA3 pyramidal cell layer of the
depression when only a “depressed hippocampus. Long-term elevation of glucocorticoid levels is also known to decrease the
survival of these neurons. Other types of neuronal insult, such as hypoxia–ischemia, hy-
mood” is present without the con-
poglycemia, neurotoxins and viral infections, may also cause atrophy or damage of neu-
comitant mental and physical symp-
rons and thereby make a person vulnerable to subsequent insults. These types of interac-
toms [i.e., SIGECAPS]). tion may underlie the observations of decreased function and volume of hippocampus in
• Exclusion of a diagnosis or failure to patients with affective disorders and may explain the selective vulnerability of certain
start treatment for depression de- people to become depressed. Long-term antidepressant treatments increase the expres-
spite the associated symptom com- sion of BDNF as well as tyrosine kinase receptor B (trkB) and prevent the down-regula-
plex (e.g., “Of course you’re de- tion of BDNF elicited by stress. This may increase the growth or survival of neurons, or
pressed. Who wouldn’t be depressed help repair or protect neurons from further damage. Increased expression of BDNF and
if these events were occurring in trkB seems to be mediated by the sustained elevation of the serotonin and norepineph-
their life?” In other words, “explain- rine (NE) systems and the cyclic adenosine monophosphate cascade. Normalization of
ing” the diagnosis rather than con- glucocorticoid levels by long-term antidepressant treatments may also contribute to the
sidering treatment options). recovery of CA3 neurons. (Adapted from Duman et al22 with permission of the publisher.)
CMAJ • NOV. 26, 2002; 167 (11) 1255
Remick
These clinical errors, coupled with the stigma associ- intent and lethality. The priority is always the patient’s
ated with psychiatric conditions,30 result in the underdiag- (and others’) safety. Detailed lethal plans, social isolation,
nosis of major mood disorders. Clinicians should keep a substance abuse, previous suicide attempts and a family
high index of suspicion for this common disorder, ques- history of suicide all increase the risk, which may increase
tion the patient about the constellation of symptoms (not the need for careful and close monitoring (frequent visits,
just a mood change) associated with depression (i.e., having the patient reside with friends or family, or hospi-
SIGECAPS), and consider obtaining collateral informa- tal care).31
tion from a relative if they do not know the patient well or
if the diagnosis is unclear. Therapeutic alliance
Do no harm Treatment requires a compassionate, nonjudgemental at-
titude on the part of the physician. Initially, physicians need
The patient’s thoughts of suicide should be taken seri- to educate patients about the illness concept of depression
ously. The clinician should broach this topic in the first and to specifically tell them of their expectations for signifi-
visit and regularly monitor for a change in the patient’s cant or full recovery (instillation of hope). Patients should
be encouraged to ask questions and to let the doctor know if
they cannot adhere to the treatment regimen rather than
stopping treatment unilaterally. Family members are essen-
tial allies in supporting the depressed patient to comply with
treatment, and their involvement is encouraged.
Biologic treatment
Antidepressant drug therapy
Therapy with an antidepressant agent is the preferred
treatment in cases of moderate to severe major depression.
The rate of response to an antidepressant trial is about
60% and is close to 80% if therapy with a second drug is
tried after an initial antidepressant drug failure.32,33
Patients should learn that the physiologic symptoms of
depression (disturbances of sleep, appetite, energy and mo-
tor activity) may resolve before the patient subjectively
senses improvement (hence the rationale for “objective” re-
ports from family members). Symptoms typically do not
start to resolve until the patient has received an adequate
dosage of medication for 2 to 4 weeks. Full remission (i.e.,
back to baseline and resolution of all SIGECAPS) — the
goal of treatment — may take up to 4 months. There is an
increasing risk of recurrence or chronicity, or both,34 if
residual symptoms persist.
Reminding the patient that recovery is typically a “saw-
Norepinephrine tooth curve” rather than a linear progression may reassure
Serotonin (5HT)
the patient and family when a few “bad” days occur. Pa-
tients need to be aware that side effects are typically tran-
Antidepressant drug sient and that they should not stop therapy, even if they are
Reuptake transporters feeling better, without discussing it with the doctor.
Alpha 1 receptors Choosing an antidepressant agent
Paulette Dennis
Alpha 2 receptors
Over 20 antidepressants are commercially available in
Serotonin (5-HT) receptors
Canada (Table 2), and this number will certainly increase.
Fig. 2: Schematic of the “cross talk” and purported interac- Thus, the choice can be daunting in our commercial era,
tions in the brain between norepinephrine (NE), serotonin (5- in which television advertisements, gift-laden industry rep-
HT) and the postsynaptic neurons. (Adapted from Blier28 with resentatives and distinguished professors at elegant dinners
permission of the publisher.) each extol the virtues of a different antidepressant.
1256 JAMC • 26 NOV. 2002; 167 (11)
Diagnosis and management of depression
The following are basic concepts to consider in choos- toms, the physician should consider either raising the anti-
ing an antidepressant: depressant dose if the patient can tolerate a higher dose
• If the patient has had a previous positive response to a with minimal side effects, or augmentation. The addition
specific antidepressant, it would be prudent to initiate a of a small dose of lithium,40 liothyronine sodium41 or a psy-
trial with this drug. If a family member has had a previ- chostimulant42 will quickly (i.e., within 1–2 weeks) convert a
ous good response with a certain antidepressant, the pa- partial response to a full response in 25% of patients.
tient may feel more comfortable starting treatment with
that drug. Likewise, if a family member has had an un- Switching antidepressants
toward response to a specific drug (or if the popular
press is giving a specific drug a great deal of negative at- If there is no or limited response to an adequate anti-
tention), one should consider other drug alternatives. depressant trial and increasing the dose or augmentation is
• Safety considerations should be reviewed. In suicidal either unsuccessful or not appropriate, then switching to a
patients at risk of overdose, the older-generation anti- different antidepressant is the appropriate strategy. Current
depressants (i.e., tricyclics and monoamine oxidase in- thinking is to switch to a different SSRI or a newer anti-
hibitors [MAOIs]) can be lethal, whereas the newer- depressant, or both. Most clinicians will defer a trial of a
generation selective serotonin reuptake inhibitors tricyclic antidepressant or MAOI until at least 2 trials of
(SSRIs) and others are relatively safe in overdose.36 newer medications have failed. In general, there is no need
• Side effect tolerability should be matched to the indi- to stop one antidepressant before starting a second drug
vidual patient. No antidepressant is devoid of side ef- trial, and typically the dosage of the first drug is tapered as
fects, but common class side effects, such as orthostatic
hypotension (tricyclics), sedation (trazodone, fluvox-
Table 2: Daily dose and cost of currently available
amine, paroxetine), stimulation (bupropion), weight 35
antidepressants
gain (tricyclics, phenelzine, mirtazapine) and sexual
dysfunction (SSRIs), may be more or less problematic Usual daily Cost per
for a specific patient should that side effect develop. Antidepressant dose, mg day, $*
Trindade and colleagues37 conducted a comprehensive Level I evidence and generally tolerable
systematic review and meta-analysis of side effects of side effect/safety profile
SSRIs and tricyclic antidepressants. Table 3 shows the Bupropion (Wellbutrin SR) 150–300 0.80–1.60
major class differences in the pooled analysis of 84 ran- Citalopram (Celexa) 20–40 1.31–2.32
domized controlled trials comparing SSRIs and tri- Fluoxetine (Prozac) 20–40 1.08–2.16
cyclic antidepressants. Fluvoxamine (Luvox) 100–200 0.99–1.98
• Drug interactions are possible due to induction or inhi- Mirtazapine (Remeron) 15–45 0.69–2.06
bition of liver enzymes. In patients with coexisting Moclobemide (Manerix) 450–600 1.22–2.28
medical disorders who are taking a number of other Nefazodone (Serzone-5HT2) 200–400 0.93–1.86
medications, an antidepressant with few drug–drug in- Paroxetine (Paxil) 20–40 1.59–3.18
teractions (e.g., citalopram, sertraline, venlafaxine, mir- Sertraline (Zoloft) 50–150 1.60–3.35
tazapine) would be appropriate.38 Venlafaxine (Effexor) 75–225 1.56–3.21
• Unfortunately, physicians seldom consider the cost of Level II evidence or level I evidence but
less tolerable side effect/safety profile
drugs for our patients; however, cost is often one of the
Amitriptyline (Elavil) 100–250 0.03–0.08
primary factors influencing a patient’s decision to con-
Clomipramine (Anafranil) 100–250 0.87–2.19
tinue to take a prescribed medication. Substantial cost
Desipramine (Norpramin) 100–250 0.82–2.06
differences remain between tricyclic antidepressants,
Doxepin (Sinequan) 100–250 0.63–1.57
MAOIs, the generic SSRI fluoxetine and the newer an-
Imipramine (Tofranil) 100–250 0.04–0.09
tidepressant agents (Table 2).
Maprotiline (Ludiomil) 100–250 0.78–1.96
Trazodone (Desyrel) 200–400 0.79–1.58
Monotherapy versus augmentation
Trimipramine (Surmontil) 100–250 0.34–1.00
Level III evidence or level I or II evidence
Sixty percent of patients with major depression or a dys- and significantly less tolerable side
thymic disorder will have a clinical response to an adequate effect/safety profile
trial (3–6 weeks) of an antidepressant.32,33 However, if there Amoxapine (Asendin) 150–300 0.93–1.86
is no response (i.e., no change in SIGECAPS) after 3 Nortriptyline (Aventyl) 75–150 0.91–1.82
weeks, the likelihood of a response is less than 20%,39 and a Phenelzine (Nardil) 30–75 0.60–1.50
switch to an antidepressant of a different chemical class Protriptyline (Triptil) 30–60 1.04–2.08
should be contemplated. Tranylcypromine (Parnate) 20–60 0.67–2.00
If, after 3–6 weeks, there is a partial response (i.e., some *Derived from the Ontario Drug Benefit Formulary or manufacturers’ price lists. Costs do not
change in SIGECAPS) but not full resolution of symp- include professional fees or markups.
CMAJ • NOV. 26, 2002; 167 (11) 1257
Remick
the new antidepressant is started. Classic MAOIs are the In elderly people, pregnant women and breast-feeding
exception, requiring a 2-week washout period before ther- women, one should be aware of certain factors. Anti-
apy with another antidepressant can be initiated. If the pa- depressants are effective in elderly people.43 The tenant
tient has not tolerated the first drug well, then a washout “start low, go slow” applies, and the use of the newer
period may be prudent to dissipate side effects before a sec- agents, in particular those with minimal CYP450 inhibi-
ond drug trial. tion, is appropriate and safer than the use of tricyclic anti-
depressants or MAOIs. There is growing evidence that
Special considerations antidepressants are safe during pregnancy, that they do not
increase the risk of teratogenesis and that the risk of de-
There are few significant drug–drug interactions with pressive relapse may be as high as 75% in pregnant women
the newer non-tricyclic/non-MAOI antidepressants. All who stop their antidepressant therapy. 44,45 These data
antidepressants are metabolized by one or more of the should be incorporated into discussions with pregnant
cytochrome P450 (CYP450) hepatic isoenzymes. For de- women as they review the benefits and risks of ongoing an-
pressive patients taking a number of other medications, an- tidepressant chemotherapy. Data on the use of antidepres-
tidepressants that have minimal CYP450 inhibitions (e.g., sants during breast-feeding are limited, and long-term de-
citalopram, venlafaxine, mirtazapine) should be considered. velopmental effects are unknown. Preliminary safety data
do not contraindicate the use of several tricyclic anti-
Table 3: Pooled weighted differences between SSRIs and TCAs depressants and SSRIs.46
in percentages of patients reporting adverse effects*
Maintenance therapy
Pooled difference
Category and type of adverse effect relative to TCAs, %
Over 70% of patients experience a recurrence of depres-
Adverse effects for which there was no sion during their lifetime.47 Most physicians (and their pa-
statistically significant difference between any tients) stop antidepressant therapy too early, without dis-
1 of the 4 SSRIs and all TCAs
cussion as to the risk of relapse and the subsequent risk of
Headache +2
disability and death. Current guidelines suggest that, after
Tremor –1
recovery occurs, antidepressant therapy should be contin-
Urinary disturbance –1
ued at the therapeutic dosage for at least 6 months to sig-
Hypotension –5
nificantly lessen the chance of relapse.35,36 Indefinite anti-
Adverse effects that occurred statistically
significantly more often with TCAs than with at depressant maintenance therapy should be discussed with
least 1 of the SSRIs patients with additional risk factors (2 or more episodes of
Dry mouth –29* depression in 5 years, episodes after the age of 50 and diffi-
Constipation –11* cult-to-treat episodes).48 The clinician should review with
Dizziness –9* the patient the benefits (prevention of recurrence) and risks
Sweating –3* (e.g., cost, side effects, inconvenience of taking medication)
Blurred vision –3* of treatment. If antidepressant therapy is stopped, the
Palpitations –2 dosage should be tapered gradually to avoid discontinua-
Adverse effects that occurred statistically tion symptoms.49
significantly more often with at least 1 of the SSRIs
than with TCAs Electroconvulsive therapy
Nausea +10*
Anorexia +5* Electroconvulsive therapy (ECT) has been and contin-
Diarrhea +8* ues to be the most effective treatment for major
Insomnia +4* depression.50,51 Between 60% and 80% of all depressed pa-
Nervousness +4* tients who receive a course of ECT respond to this treat-
Fatigue –2 ment.50,51 A typical course of ECT is 6 to 12 treatments,
Adverse effects for which there was a statistically with 2 to 3 treatments given per week. Improvement is typ-
significant difference (occurring more often with
SSRIs than with the group of TCAs) only for ically noted after the fourth treatment. ECT should be
pooled rates considered a first-line treatment in depressed patients with
Agitation +6* psychotic features, actively suicidal patients and patients
Anxiety +5* who have not responded to or cannot tolerate antidepres-
Note: SSRI = selective serotonin reuptake inhibitor, TCA = tricyclic antidepressant. Adapted from
sant chemotherapy. Although the mechanism of efficacy of
Trindade et al.37 The entries in the final column are from meta-analyses of all of the trials of 4 SSRIs ECT remains unclear, electroencephalography typically
(fluoxetine, fluvoxamine, paroxetine and sertraline) against any TCA. Data for the individual SSRIs
are available in Table 2 of the study by Trindade et al (www.cmaj.ca/cgi/reprint/159/10/1245.pdf). shows slowing in the prefrontal cortex (which likely reflects
*Adverse event occurred statistically significantly more frequently with an SSRI (positive value)
or a TCA (negative value). Based on pooled rate difference obtained by meta-analysis of
a more fundamental neurobiologic process) in patients who
randomized controlled trials. respond to ECT.52
1258 JAMC • 26 NOV. 2002; 167 (11)
Diagnosis and management of depression
Light therapy Conclusion
Phototherapy is an established and effective treatment There has been significant progress in the area of mood
for major depression with a seasonal variation, particularly disorders over the last 2 decades, encompassing advances in
fall/winter depressions. Its efficacy in nonseasonal depres- our knowledge of epidemiology, diagnosis, pathogenesis and
sion is not established. Phototherapy is an alternative treat- treatment. As clinicians we must enhance our efforts to rec-
ment intervention to antidepressant therapy in mild to ognize this illness in our patients and ensure that the myriad
moderate seasonal depression. The reader is encouraged to of effective treatments are offered and used. Furthermore, by
refer to published Canadian guidelines.53 The usual treat- espousing a medical model of this disease, we lessen the per-
ment is at least 30 minutes per day of light therapy with a vasive stigma that is associated with all mental disorders.
standard phototherapy device (delivering 10 000 lx of full-
spectrum white light) throughout the fall/winter episode. Competing interests: None declared.
Phototherapy devices can now be purchased or rented at Acknowledgements: I thank Dr. Raymond W. Lam for his helpful and construc-
many medical supply and equipment stores. tive critiques of the manuscript.
St. John’s wort References
St. John’s wort (hypericin) is a popular alternative treat- 1. Murphy JM, Laird NM, Monson RR, Sobel AM, Leighton AH. A 40-year
ment for depression. Despite European studies demonstrat- perspective on the prevalence of depression: the Stirling County Study. Arch
Gen Psychiatry 2000;57:209-15.
ing the efficacy of St. John’s wort,54 a recent North American 2. Duffy A. Towards effective early intervention and prevention strategies for
controlled study showed the compound to be no more effec- major affective disorders: a review of antecedents and risk factors. Can J Psy-
chiatry 2000;45:340-8.
tive than placebo in major depressive disorder.55 Although pa- 3. American Psychiatric Association. Diagnostic and statistical manual of mental
tients with mild mood symptoms (i.e., not major depression) disorders. 4th ed. Washington: The Association; 1994.
4. Bland RC. Epidemiology of affective disorders: a review. Can J Psychiatry
may receive some benefit from hypericin, and the herb is rel- 1997;42(4):367-77.
atively benign in terms of side effects and drug–drug interac- 5. Sadovnick AD, Remick RA, Lam RW, Zis AP, Yee IM, Huggins NJ, et al.
Mood Disorder Service Genetic Database: morbidity risks for mood disorders
tions, physicians should encourage more standardized treat- in 3,942 first-degree relatives of 671 index cases with single depression, recur-
ments in patients with moderate to severe mood disorders. rent depression, bipolar I, or bipolar II. Am J Med Genet 1994;54:132-40.
6. Kessler RC, McGonagle KA, Zhao S, Nelson CB, Hughes M, Eshleman S, et
al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in
Other interventions the United States. Results from the National Comorbidity Survey. Arch Gen
Psychiatry 1994;51:8-19.
7. Enns MW, Swenson JR, McIntyre RS, Swinson RP, Kennedy SH, and the
Although current data are limited, potential new or CANMAT Depression Work Group. Clinical guidelines for the treatment of
novel interventions for the treatment of mood disorders depressive disorders. VII. Comorbidity. Can J Psychiatry 2001;46(Suppl
1):77S-90S.
may include exercise regimens,56 sleep deprivation,57 psy- 8. Weissman MM, Bland RC, Canino GJ, Faravelli C, Greenwald S, Hwu HG,
chosurgery,58 vagus nerve stimulation59 and transcranial et al. Cross-national epidemiology of major depression and bipolar disorder.
JAMA 1996;276:293-9.
magnetic stimulation.60 9. Patten SB. Incidence of major depression in Canada. CMAJ 2000;163:714-5.
10. Bostwick JM, Pankratz VS. Affective disorders and suicide risk: a re-examina-
Psychological treatment tion. Am J Psychiatry 2000;157:1925-32.
11. Sakinofsky I, Leenaars AA. Suicide in Canada with special reference to the
difference between Canada and the United States. Suicide Life Threat Behav
In addition to supportive and psychoeducational tech- 1997;27:112-26.
12. Parikh SV, Wasylenki D, Goerung P, Wong J. Mood disorders: rural/urban
niques, specific psychotherapeutic interventions are as ef- differences in prevalence, health care utilization, and disability in Ontario. J
fective as antidepressant therapy in mild to moderate major Affect Disord 1996;38:57-65.
13. Kessler RC, Barber C, Birnbaum HG, Frank RG, Greenberg PE, Rose RM,
depression and dysthymic disorders.61–63 et al. Depression in the workplace: effects on short-term disability. Health Aff
Cognitive behavioural therapy64,65 and interpersonal (Millwood) 1999;18:163-71.
14. Denihan A, Bruce I, Coakley D, Lawlor BA. Psychiatry morbidity in cohabitants
therapy66 are the treatment interventions with documented of community-dwelling elderly depressives. Int J Geriatr Psychiatry 1998;13:691-4.
efficacy. Both therapies require specialized training, can be 15. Goodman SH, Gotlib IH. Risk for psychopathology in the children of de-
pressed mothers: a developmental model for understanding mechanisms of
administered individually or in a group setting, and typi- transmission. Psychol Rev 1999;106:458-90.
cally require 8 to 16 weekly sessions for efficacy. 16. Murray CJ, Lopez AD. Alternative projections of mortality and disability by
The choice of psychotherapy or chemotherapy should cause 1990–2020: global burden of disease study. Lancet 1997;349:1498-504.
17. Gredon JF. The burden of disease in treatment-resistant depression. J Clin
be based on patient preference, clinician judgement and Psychiatry 2001;62:26-31.
cost as well as the practical issue of availability of psy- 18. Frasure-Smith N, Lesperance F, Talajic M. Depression and 18 month prog-
nosis after myocardial infarction. Circulation 1995;91:999-1005.
chotherapy. Furthermore, patients who have not responded 19. Pratt LA, Ford DE, Crum RM, Armenian HK, Gallo JJ, Eaton WW. De-
to their preferred treatment modality should be encour- pression, psychotropic medication, and risk of myocardial infarction. Prospec-
tive data from the Baltimore ECA follow-up. Circulation 1996;94:3123-9.
aged to try other interventions. 20. Bush DE, Ziegelstein RC, Tayback M, Richter D, Stevens S, Zahalsky H, et
Although combined pharmacotherapy–psychotherapy is al. Even minimal symptoms of depression increase mortality risk after acute
myocardial infarction. Am J Cardiol 2001;88:337-41.
widely practised in the psychiatric community, the evidence 21. Musselman DL, Evans DL, Nemeroff CB. The relationship of depression to
of additive effects remains limited.67 cardiovascular disease. Arch Gen Psychiatry 1998;55:580-92.
CMAJ • NOV. 26, 2002; 167 (11) 1259
Remick
22. Duman RS, Heninger GR, Nestler EJ. A molecular and cellular theory of de- 47. Mueller TI, Leon AC, Keller MB, Solomon DA, Endicott J, Coryell W, et al.
pression. Arch Gen Psychiatry 1997;54:597-608. Recurrence after recovery from major depressive disorder during 15 years of
23. Stahl SM. Essential psychopharmacology of depression and bipolar disorder. New observational follow-up. Am J Psychiatry 1999;156(7):1000-6.
York: Cambridge University Press; 2000. p. 20-63. 48. Remick RA. Long term pharmacological treatment of mood disorders. In:
24. Manji HK, Moore GJ, Rajkowska G, Chen G. Neuroplasticity and cellular Ancill R, Lader M, Tindall B, editors. Pharmacological management of chronic
resilience in mood disorders. Mol Psychiatry 2000;5:578-93. psychiatric disorders. London: Balliere Tindall; 1995. p. 553-63.
25. Drevets WC. Functioning neuroimaging studies of depression: the anatomy 49. Haddad P. The SSRI discontinuation syndrome. J Psychopharmacol 1998;12:
of melancholia. Annu Rev Med 1998;49:341-61. 305-13.
26. Vaidya VA, Sivciak JA, Du F, Dumnan RS. Hippocampal mossy fiber sprout- 50. Potter WZ, Rudorfer MV. Electroconvulsive therapy — a modern medical
ing induced by chronic electroconvulsive seizures. Neuroscience 1999;89:157-66. procedure [editorial]. N Engl J Med 1993;328:882-3.
27. Thase ME. Neuroimaging profiles and the differential therapies of depres- 51. Kraus RP, Chandarana P. “Say, are you psychiatrists still using ECT?” CMAJ
sion. Arch Gen Psychiatry 2001;58:651-2. 1997;157:1375-7.
28. Blier P. Crosstalk between the norepinephrine and serotonin systems and its 52. Sackeim HA, Luber B, Katzman GP, Moeller JR, Prudic J, Devanand DP, et
role in the antidepressant response. J Psychiatry Neurosci 2001;26(Suppl):S3-10. al. The effects of electroconvulsive therapy on quantitative electroencephalo-
29. Judd LL, Paulus MP, Wells KB, Rapaport MH. Socioeconomic burden of grams. Relationship to clinical outcome. Arch Gen Psychiatry 1996;53:814-24.
subsyndromal depressive symptoms and major depression in a sample of the 53. Lam RW, Levitt AJ. Canadian consensus guidelines for the treatment of seasonal
general population. Am J Psychiatry 1996;153:1411-7. affective disorder. Vancouver: Clinical & Academic Publishing; 1999.
30. Sirey JA, Bruce ML, Alexopoulos GS, Perlick DA, Friedman SJ, Meyers BS. 54. Linde K, Ramirez G, Mulrow CD, Pauls A, Weidenhammer W, Melchart D.
Stigma as a barrier to recovery. Perceived stigma and patient-rated severity of St. John’s wort for depression — an overview and meta-analysis of ran-
illness as predictors of antidepressant drug adherence. Psychiatr Serv 2001; domised clinical trials. BMJ 1996;313:253-8.
52:1615-20. 55. Shelton RC, Keller MB, Gelenberg A, Dunner DL, Hirschfeld R, Thase ME,
31. Nemeroff CB, Compton MT, Berger J. The depressed suicidal patient. As- et al. Effectiveness of St John’s wort in major depression: a randomized con-
sessment and treatment. Ann N Y Acad Sci 2001;932:1-23. trolled trial. JAMA 2001;285:1978-86.
32. Joffe R, Sokolov S, Streiner D. Antidepressant treatment of depression: a 56. Lawlor DA, Hopker SW. The effectiveness of exercise as an intervention in
meta-analysis. Can J Psychiatry 1996;41:613-6. the management of depression: systematic review and meta-regression analy-
33. Moller HJ, Fuger J, Kasper S. Efficacy of new generation antidepressant: sis of randomised controlled trials. BMJ 2001;322:763-7.
meta-analysis of imipramine-controlled studies. Pharmacopsychiatry 1994;27: 57. Wirz-Justice A, van den Hoofdakker RH. Sleep deprivation in depression:
215-23. What do we know, where do we go? Biol Psychiatry 1999;46:445-53.
34. Judd LL, Paulus MJ, Schettler PJ, Akiskal HS, Endicott J, Leon AC, et al. 58. Bridges PK, Bartlett JR, Hale AS, Poynton AM, Malizia AL, Hodgkiss AD.
Does incomplete recovery from first lifetime major depressive episode herald Psychosurgery: stereotactic subcaudate tractomy. An indispensable treatment.
a chronic course of illness? Am J Psychiatry 2000;157:1501-4. Br J Psychiatry 1994;165:599-611.
35. Kennedy SH, Lam RW, Cohen NL, Ravindran AV, and the CANMAT De- 59. George MS, Sackeim HA, Marangell LB, Husain MM, Nahas Z, Lisanby SH,
pression Work Group. Clinical guidelines for the treatment of depressive dis- et al. Vagus nerve stimulation. A potential therapy for resistant depression?
orders. IV. Medications and other biological treatments. Can J Psychiatry Psychiatr Clin North Am 2000;23:757-83.
2001;46(Suppl 1):38S-58S. 60. Hasey G, Joffe R, Ivanski C. Managing neuropsychiatic disease with transcra-
36. American Psychiatric Association. Practice guideline for the treatment of pa- nial magnetic stimulation. CMAJ 2000;162:78-80.
tients with major depressive disorder (revision). Am J Psychiatry 2000;157(4 61. Keller MB, McCullough JP, Klein DN, Arrow B, Dunner DL, Gelenberg AJ,
Suppl):1-45. et al. A comparison of nefazodone, the cognitive behavioral-analysis system of
37. Trindade E, Menon D, Topfer LA, Coloma C. Adverse effects associated psychotherapy, and their combination for the treatment of chronic depres-
with selective serotonin reuptake inhibitors and tricyclic antidepressents: a sion. N Engl J Med 2000;342:1462-70.
meta-analysis. CMAJ 1998;159(10):1245-52. 62. Ravindran AV, Anisman H, Merali Z, Charbonneau Y, Telner J, Bialik RJ, et
38. Jefferson JW. Drug interactions — Friend or foe? J Clin Psychiatry 1998;59 al. Treatment of primary dysthymia with group cognitive therapy and phar-
(Suppl 4):37-47. macotherapy: clinical symptoms and functional impairments. Am J Psychiatry
39. Nierenberg AA, McLean NE, Alpert JG, Worthington JJ, Rosenbaum JF, 1999;156:1608-17.
Fava M. Early non-response to fluoxetine as a predictor of poor 8 week out- 63. Frank E, Grochocinski VJ, Spanier CA, Buysse DJ, Cherry CR, Houck PR, et
come. Am J Psychiatry 1995;152:1500-3. al. Interpersonal psychotherapy and antidepressant medication: evaluation of
40. Bauer M, Dopfiner S. Lithium augmentation in treatment-resistant depres- a sequential treatment strategy in women with recurrent major depression. J
sion: meta-analysis of placebo-controlled studies. J Clin Psychopharmacol 1999; Clin Psychiatry 2000;61:51-7.
19:427-34. 64. Beck AT, Rush AJ, Shaw BF, Emery G. Cognitive therapy of depression. New
41. Altshuler LL, Bauer M, Frye MA, Gitlin MJ, Mintz J, Szuba MP, et al. Does York: Guilford Press; 1979.
thyroid supplementation accelerate tricyclic antidepressant response? A re- 65. Greenberg D, Padesky CA. Mind over mood. New York: Guilford Press; 1995.
view and meta-analysis of the literature. Am J Psychiatry 2001;158:1617-22. 66. Weissman MM, Markowitz JC, Klerman GL. A comprehensive guide to inter-
42. Warneke L. Psychostimulants in psychiatry. Can J Psychiatry 1990;35:3-10. personal psychotherapy. New York: Basic Books; 2000.
43. Gerson S, Belin TR, Kaufman A, Mintz J, Jarvik L. Pharmacological and psy- 67. Segal ZV, Kennedy SH, Cohen NL, and the CANMAT Depression Work
chological treatments for depressed older patients: a meta-analysis and Group. Clinical guidelines for the treatment of depressive disorders. V. Com-
overview of recent findings. Harv Rev Psychiatry 1999;7(1):1-28. bining psychotherapy and pharmacotherapy. Can J Psychiatry 2001;46(Suppl
44. Stewart DE. Antidepressant drugs during pregnancy and lactation. Int Clin 1):59S-62S.
Psychopharmacol 2000;15(Suppl 3):S19-24.
45. Cohen LS, Rosenbaum JF. Psychotropic drug use during pregnancy: weigh-
ing the risks. J Clin Psychiatry 1998;59(Suppl 2):18-28.
46. Misri S, Kostaras D, Kostaras X. The use of selective serotonin reuptake in-
Correspondence to: Dr. Ronald A. Remick, Department of
hibitors during pregnancy and lactation: current knowledge. Can J Psychiatry Psychiatry, St. Paul’s Hospital, 1081 Burrard St., Vancouver BC
2000;45(3):285-7. V6Z 1Y6; rremick@shaw.ca
1260 JAMC • 26 NOV. 2002; 167 (11)
Вам также может понравиться
- Apeg Handbook FinalДокумент315 страницApeg Handbook FinalkkkssbbОценок пока нет
- Chapter 5.2 - Routes of AdministrationДокумент17 страницChapter 5.2 - Routes of Administrationfahima purniОценок пока нет
- 8 Drug ExcretionДокумент61 страница8 Drug ExcretionAhmed YTОценок пока нет
- Brochure HVAC A4 PDFДокумент8 страницBrochure HVAC A4 PDFSathiaram RamОценок пока нет
- Installation and Maintenance Manual: MR - Mre - Mra MRD - Mrde - Mrda MRV - Mrve - Mrva MRT - Mrte - MRTF - MrtaДокумент50 страницInstallation and Maintenance Manual: MR - Mre - Mra MRD - Mrde - Mrda MRV - Mrve - Mrva MRT - Mrte - MRTF - MrtaAshley DeanОценок пока нет
- Atc CodeДокумент128 страницAtc Codecupidvishu123100% (1)
- Excipients InteractionsДокумент6 страницExcipients InteractionsAgatharia BudiyanaОценок пока нет
- Section EДокумент110 страницSection Ebaracuss323iОценок пока нет
- 7CH4Q45 (M) 7CH4Q90 (M) : - User'S GuideДокумент7 страниц7CH4Q45 (M) 7CH4Q90 (M) : - User'S GuideЕвгенийОценок пока нет
- Magic Wave 3000Документ140 страницMagic Wave 3000bob jacksonОценок пока нет
- Plataforma Manitou 78SEC Servicio Ingles EjesДокумент6 страницPlataforma Manitou 78SEC Servicio Ingles EjesJose LunaОценок пока нет
- Biljax 3632 TДокумент238 страницBiljax 3632 TRichard BroadwayОценок пока нет
- RT240 Technical BrochureДокумент6 страницRT240 Technical BrochureThinkDefenceОценок пока нет
- بيДокумент48 страницبيMojied AmeerОценок пока нет
- Maflosh 02 IngДокумент44 страницыMaflosh 02 IngNicoleta CosteaОценок пока нет
- 060378en - General Reachstacker Forklift - SCANIA ENGINE DC13 (74A AND 76A)Документ11 страниц060378en - General Reachstacker Forklift - SCANIA ENGINE DC13 (74A AND 76A)MohamedSalahОценок пока нет
- ENTAM+recogs - 05.217 Caffini - Starter 3300 24 BL AirДокумент9 страницENTAM+recogs - 05.217 Caffini - Starter 3300 24 BL AirPaul DanОценок пока нет
- HDF 2.5 Owners Manual PDFДокумент57 страницHDF 2.5 Owners Manual PDFLara BarradoОценок пока нет
- MAN TGE Crafter 2017 Fuse Holder Locations & Descriptions A4 VersionДокумент4 страницыMAN TGE Crafter 2017 Fuse Holder Locations & Descriptions A4 VersionChristiaan de KerpelОценок пока нет
- NR 18 - Self-Propelled Scissor PlatformДокумент67 страницNR 18 - Self-Propelled Scissor PlatformCPSSTОценок пока нет
- Imi023 David Brown Technical Service Bulletins & Parts Bulletins Part 2Документ76 страницImi023 David Brown Technical Service Bulletins & Parts Bulletins Part 2Mauro SantanaОценок пока нет
- STILL RX 70 Technical Data FREEДокумент22 страницыSTILL RX 70 Technical Data FREEErblin BlineraОценок пока нет
- Perkins Diesel Engines: MaintenanceДокумент130 страницPerkins Diesel Engines: Maintenancefrancisco barreraОценок пока нет
- Nomogram PDFДокумент2 страницыNomogram PDFAbdul ShakoorОценок пока нет
- 4 Power TransmissionДокумент131 страница4 Power TransmissionAdrian MotocОценок пока нет
- Magnum 340 CalibrationДокумент7 страницMagnum 340 CalibrationTavonga AbsОценок пока нет
- 74584TL - EN - User Manual 200116Документ72 страницы74584TL - EN - User Manual 200116Juan Jose Medero FeriaОценок пока нет
- F330B 23Документ110 страницF330B 23ניקולאי איןОценок пока нет
- Recommendation List of Concession'S Spare Parts: MLT-X 735 T LsuДокумент4 страницыRecommendation List of Concession'S Spare Parts: MLT-X 735 T LsuViacheslav BurmistrОценок пока нет
- JCB436Документ14 страницJCB436David SolisОценок пока нет
- Electric PC LS160 LS170 6 EUДокумент62 страницыElectric PC LS160 LS170 6 EUsassine khouryОценок пока нет
- Power Steering EngДокумент56 страницPower Steering EngSasko DimitrovОценок пока нет
- Control Electronico Del Motor GM 1Документ100 страницControl Electronico Del Motor GM 1adelmomouraОценок пока нет
- CN and CX200 Maintenance 91549 MHДокумент130 страницCN and CX200 Maintenance 91549 MHdozer_kamil100% (2)
- Assembly / Operators Manual: #95400 F.GB - 09.2003Документ60 страницAssembly / Operators Manual: #95400 F.GB - 09.2003wolfovic3932Оценок пока нет
- Service Manual Parts Manual Hyster N30XMDR3, N45XMR3 (G138) (Preview)Документ6 страницService Manual Parts Manual Hyster N30XMDR3, N45XMR3 (G138) (Preview)Amip FolkОценок пока нет
- HIAB14000XGДокумент267 страницHIAB14000XGMigueОценок пока нет
- Ingersoll RandДокумент22 страницыIngersoll RandezeizabarrenaОценок пока нет
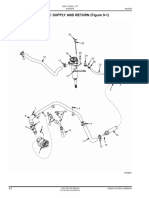
- Hydraulic Supply and Return (Figure 9-1) : Unit Code L177 Europe 06/2005Документ42 страницыHydraulic Supply and Return (Figure 9-1) : Unit Code L177 Europe 06/2005Melwyn FernandesОценок пока нет
- Evrard Alpha 2500Документ89 страницEvrard Alpha 2500Petro ServisasОценок пока нет
- Linked PDFДокумент43 страницыLinked PDFMarcelo AguirreОценок пока нет
- 3f110 03 Electrical SystemДокумент68 страниц3f110 03 Electrical SystemMaz Ariez EkaОценок пока нет
- S12u16 User ManualДокумент41 страницаS12u16 User Manualelrond.projects0% (1)
- BC-2800Vet Operator's Manual 12.0 EN H-2810-20-47202 ECM12.0 PDFДокумент246 страницBC-2800Vet Operator's Manual 12.0 EN H-2810-20-47202 ECM12.0 PDFEr Nitin SinghОценок пока нет
- Section 55 Electrical System Diagnostic H Routines Part2Документ9 страницSection 55 Electrical System Diagnostic H Routines Part2Dra MiОценок пока нет
- Motrec T-236-O.K1Документ60 страницMotrec T-236-O.K1edrei solorioОценок пока нет
- CL 74C Winch Motor: Operation ManualДокумент29 страницCL 74C Winch Motor: Operation Manualionut2007Оценок пока нет
- TorqlinkДокумент112 страницTorqlinkLaércio FerreiraОценок пока нет
- x20 System-Eng v3.60Документ3 830 страницx20 System-Eng v3.60Sem FadeyОценок пока нет
- NSC ManualДокумент263 страницыNSC ManualshutekiОценок пока нет
- RoD and BioavailibilityДокумент37 страницRoD and BioavailibilityDzil FikriОценок пока нет
- F240a 22Документ93 страницыF240a 22ניקולאי איןОценок пока нет
- Problems Facing The Pharmaceutical Industry and Approaches To Ensure Long Term ViabilityДокумент68 страницProblems Facing The Pharmaceutical Industry and Approaches To Ensure Long Term ViabilityAniruddh JainОценок пока нет
- T 220Документ54 страницыT 220Claudio RussoОценок пока нет
- Declarations of Conformity - Danfoss NRVAДокумент1 страницаDeclarations of Conformity - Danfoss NRVARoger RamosОценок пока нет
- Manejo Depresion 1Документ10 страницManejo Depresion 1Luis HaroОценок пока нет
- Park, 2019 - NEJM - DepressionДокумент10 страницPark, 2019 - NEJM - DepressionFabian WelchОценок пока нет
- The Medical Management of Depression: Review ArticleДокумент16 страницThe Medical Management of Depression: Review Articleklysmanu93Оценок пока нет
- Depression in The Elderly: Clinical PracticeДокумент9 страницDepression in The Elderly: Clinical PracticejpenasotoОценок пока нет
- True Health Fitness Center: Marketing Plan Team 4Документ17 страницTrue Health Fitness Center: Marketing Plan Team 4BassantMohamadОценок пока нет
- Cognitive Behavioral Guided Self Help For The Treatment Od Recurrent Binge EatingДокумент19 страницCognitive Behavioral Guided Self Help For The Treatment Od Recurrent Binge EatingIsmael RodriguezОценок пока нет
- Diet Analysis ProjectДокумент6 страницDiet Analysis Projectapi-254081103100% (1)
- Effect of Probiotics As A Complement To Non Surgical Periodontal Therapy in Chronic Periodontitis A Systematic RevieДокумент7 страницEffect of Probiotics As A Complement To Non Surgical Periodontal Therapy in Chronic Periodontitis A Systematic RevieMohammedОценок пока нет
- RCHДокумент25 страницRCHgauravОценок пока нет
- Qatar Cancer Society in WordsДокумент2 страницыQatar Cancer Society in WordsQatarcancersociety QcsОценок пока нет
- Gubra DIO Mouse Data FlyerДокумент2 страницыGubra DIO Mouse Data FlyerGabrielaMirelaAlexeОценок пока нет
- Some Info On Australian Medical Schools For CanadiansДокумент5 страницSome Info On Australian Medical Schools For Canadiansstargaze_night_42Оценок пока нет
- Phenol - Medical Management Guidelines - Toxic Substance Portal - ATSDR. (N.D.) - Agency ForДокумент2 страницыPhenol - Medical Management Guidelines - Toxic Substance Portal - ATSDR. (N.D.) - Agency ForREBEKAH EQUIZОценок пока нет
- Assessing Change in Women's Lives: A Conceptual Framework: Marty Chen Simeen MahmudДокумент47 страницAssessing Change in Women's Lives: A Conceptual Framework: Marty Chen Simeen MahmudmustafaОценок пока нет
- Opt WorkshopДокумент15 страницOpt WorkshopMhel Daz BabaysonОценок пока нет
- KodefДокумент45 страницKodefWann FarhannaОценок пока нет
- Caesarean Section at Full Dilatation: Incidence, Impact and Current ManagementДокумент20 страницCaesarean Section at Full Dilatation: Incidence, Impact and Current ManagementAbdur RaheemОценок пока нет
- An Overview of The Role of Nurses and Midwives in Leadership and Management in EuropeДокумент44 страницыAn Overview of The Role of Nurses and Midwives in Leadership and Management in EuropeTCОценок пока нет
- OTPeopleParkinsons PDFДокумент84 страницыOTPeopleParkinsons PDFNovoОценок пока нет
- How To Read A CTG: What Is Cardiotocography?Документ11 страницHow To Read A CTG: What Is Cardiotocography?Rinothja RajaratnamОценок пока нет
- RRL ScriptДокумент1 страницаRRL Scriptjeron encaboОценок пока нет
- A Client With Cushing's Syndrome: Nursing Care PlanДокумент1 страницаA Client With Cushing's Syndrome: Nursing Care PlanJulius Caesar ColladoОценок пока нет
- Intradermal Delivery Vaccines Report 2009 SeptДокумент94 страницыIntradermal Delivery Vaccines Report 2009 SeptSantoso CokroОценок пока нет
- SexДокумент4 страницыSexQuotes&Anecdotes100% (1)
- Park SoftДокумент942 страницыPark Softnaresh chauhanОценок пока нет
- NEBOSH IG1 Open Book Mock Examination For Sept. 2022Документ5 страницNEBOSH IG1 Open Book Mock Examination For Sept. 2022m.naОценок пока нет
- Nutrition For Liver Gallbladder and Pancreas DiseasesДокумент39 страницNutrition For Liver Gallbladder and Pancreas DiseasesMaricar Car CartallaОценок пока нет
- 5 Minute Anxiety Relief TechniquesДокумент1 страница5 Minute Anxiety Relief TechniquesBhettoh OrtizОценок пока нет
- Behavior Technician Cover Letter No ExperienceДокумент5 страницBehavior Technician Cover Letter No Experiencef5b2q8e3100% (2)
- The Gullah People of Souhth Carolina (Draft) (012914)Документ20 страницThe Gullah People of Souhth Carolina (Draft) (012914)Grissett Tony100% (2)
- Q2 Grade 7 HEALTH DLL Week 1Документ10 страницQ2 Grade 7 HEALTH DLL Week 1Jet Arcangel Laroco LarocoОценок пока нет
- Human Factor QuizДокумент5 страницHuman Factor QuizSherif AL-KammashОценок пока нет
- Integrative Cell Therapy Program EBrochureДокумент16 страницIntegrative Cell Therapy Program EBrochureAnonymous 5X7ELhpE100% (1)
- Animal Testing: Pros and ConsДокумент11 страницAnimal Testing: Pros and ConsabhishekjainitОценок пока нет