Академический Документы
Профессиональный Документы
Культура Документы
Potentially Malignant Lesions and Conditions
Загружено:
Naleena JosephИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Potentially Malignant Lesions and Conditions
Загружено:
Naleena JosephАвторское право:
Доступные форматы
POTENTIALLY CONDITIONS
MALIGNANT
LESIONS
AND
PRESENTED BY NALEENA JOSEPH CTAHBDS029 KMCT DENTAL COLLEGE
POTENTIALLY MALIGNANT LESION Definition: A morphologically altered tissue in which cancer is more likely to occur than its normal counterpart - Shafer 1) 2) 3) 4) Leukoplakia Erythroplakia Palatal Keratosis associated with reverse smoking Actinic Keratosis, Cheilitis, & Elastosis
POTENTIALLY MALIGNANT CONDITION Definition: A generalized state or condition associated with significantly increased risk of cancer development - Shafer 1) 2) 3) 4) 5) 6) 7) 8) Oral Submucous Fibrosis Oral Lichen Planus Discoid Lupus Erythematosus Dyskeratosis Congenita Sideropenic Dysphagia Syphilitic Glossitis Xeroderma Pigmentosum Epidermolysis Bullosa
LEUKOPLAKIA DEFINITION: A white patch or plaque that cannot be characterized clinically or pathologically as any other lesion -WHO A predominantly white lesion of the oral mucosa that cannot be characterized as any other definable lesion. Some oral leukoplakia will transform into cancer. -Axell 1996 A predominant white lesion of oral mucosa that cannot be characterized as any other definable lesion - Pindborg 1997
EPIDEMIOLOGY Risk of malignant transformation is 4-6% Global prevalence of 2.6% Common in patients above 50 yrs of age Common in men
ETIOLOGY TOBACCO - Smoking form - Smokeless form ALCOHOL CHRONIC IRRITATION SANGUINERIA CANDIDIASIS VIRAL INFECTION NUTRITIONAL DEFICIENCY DRUGS IDIOPATHIC CLASSIFICATION LEUKOPLAKIA 1) Mild / Thin Leukoplakia 2) Homogenous Leukoplakia 3) Non homogenous Leukoplakia HOMOGENOUS LEUKOPLAKIA Well-defined white patch, localized or extensive, that is slightly elevated and that has a fissured, wrinkled, or corrugated surface on palpation, these lesions may feel leathery to dry, or cracked mud-like NON HOMOGENOUS LEUKOPLAKIA White patches or plaque intermixed with red tissue elements. Also called Erythroleukoplakia and speckled leukoplakia NODULAR VERRUCOUS PROLIFERATIVE VERRUCOUS ULCERATED ERYTHROLEUKOPLAKIA 6
NODULAR LEUKOPLAKIA Keratotic white nodules or patches are distributed over an Erythematous background. Associated with higher rate of malignant transformation
VERRUCIFORM LEUKOPLAKIA Presence of thick white lesions with papillary surfaces in the oral cavity. These lesions are usually heavily keratinized and are most often seen in older adults in the sixth to eighth decades of life. Some of these lesions may exhibit an exophytic growth pattern. PROLIFERATIVE VERRUCOUS LEUKOPLAKIA (PVL) Extensive papillary or Verrucoid white plaques that tend to slowly involve multiple mucosal sites in the oral cavity and to inexorably transform into Squamous cell carcinomas over a period of many years. PVL has a very high risk for transformation to dysplasia, Squamous cell carcinoma or verrucous carcinoma .Verrucous Carcinomas is a slow growing and well-differentiated lesion that seldom metastasizes. CLINICAL FEATURES Asymptomatic Common sites buccal mucosa, lower lip, Gingiva Less common sites palate, retro molar area Lesions on the floor of mouth and lateral borders of tongue are high risk sites for malignant transformation
HISTOPATHOLOGY
Epithelial hyperplasia and surface hyperkeratosis Mild to moderate epithelial dysplasia Chronic inflammatory changes
DIAGNOSIS 1) 2) 3) 4) Elimination of possible causes Biopsy (gold standard test) Toluidine blue staining Exfoliative cytology (Limited value)
MANAGEMENT 1) MEDICAL topical vitamin A / Retinoid (single and combination dosages of vitamins A, C, and E; beta carotene; analogues of vitamin A; and diets that are high in antioxidants and cell growth suppressor proteins (fruits and vegetables). 2) SURGICAL Cold knife surgical excision Laser ablation & cryosurgery - preferred because of their Precision and rapid healing MANAGEMENT OF LEUKOPLAKIA PROVISIONAL CLINICAL DIAGNOSIS Elimination of possible causes No possible causes (2-4 weeks observation) (Definitive clinical diagnosis) -------------------------------- Biopsy Good response No response (Definitive clinical diagnosis) ___________________________ Definable lesion 8
(Management accordingly)
No definable lesion (Treatment/ Observation/ Follow up)
Definable lesion (Management accordingly)
PROGNOSIS Long term follow up necessary Malignant changes occur 2-4 yrs after onset ERYTHROPLAKIA DEFINITION A fiery red patch that cannot be characterized clinically or pathologically as any other definable lesion - Pindborg 1997 Less common than Leukoplakia High frequency of pre-malignant & malignant changes Often associated with heavy smoking with or without concomitant alcohol use CLASSIFICATION ERYTHROPLAKIA - Homogenous Erythroplakia - Granular / Speckled Erythroplakia - Erythroleukoplakia CLINICAL FEATURES Seen in older men Irregular outline Common sites floor of mouth, Ventral aspect of tongue, soft palate Histopathology lack of Keratin production and Atrophic Epithelium Treatment same as Leukoplakia Recurrent rate less than 5%
PALATAL CHANGES ASSOCIATED WITH REVERSE SMOKING Peak incidence 55-64 yrs CLINICAL CHANGES Keratosis Diffuse whitening of entire Palate Patches Well defined, elevated white Plaques Excrescences 1-3mm elevated white Plaques Red areas Well defined reddening of the Palatal Mucosa Ulcerated areas Crater like areas covered by Fibrin Non pigmented areas Areas of Palatal Mucosa that are devoid of Pigmentation
HISTOLOGICAL FINDINGS Hyperorthokeratosis Epithelial Dysplasia Inflammatory cells in connective tissue Melanin deposits in Lamina Propria
Malignant changes were seen in 0.3% of the palatal lesions ACTINIC KERATOSIS Also called Solar Elastosis, Senile Elastosis or Actinic Elastosis It is Dermatological disease which is a degenerative condition of skin Also called Sailors or Farmers skin ETIOLOGY 1. Hereditary factors skin pigmentation or its absence 10
2. Exposure to elements sunlight and wind
CLINICAL FEATURES Common in elderly patients Site lips Affected skin appears wrinkled, dry, atrophic and flaccid On lips there is mild Keratosis and subtle blending of the lip vermillion with skin surface Increase in amount of elastic connective tissue fibers
HISTOPATHOLOGY TREATMENT No treatment
ORAL SUBMUCOUS FIBROSIS DEFINITION A insidious and chronic disease affecting mucosa of any part of oral cavity and occasionally extend into pharynx and esophagus ,although sometimes preceded by and / or associated with vesicle formation . It is always associated with a juxta epithelial inflammatory reaction followed by fibroelastic change of lamina propria with epithelial atrophy leading to stiffness of oral mucosa causing trismus and inability to eat. Also called Atrophica Idiopathica Mucosae Oris , idiopathic scleroderma of mouth, diffuse oral submucous fibrosis ETIOLOGY a) Areca nut chewing b) Chillies c) Genetic 11
d) Tobacco e) Autoimmune disorders
PATHOGENESIS Alkaloids like Arecolin modulate matrix metallo proteins, lysyl oxidases & collagenases which the affects collagen metabolism and leads to increased fibrosis Increased fibrosis results in decrease in water retaining proteoglycans which favor increased collagen type 1 production Polymorphism in gene coding for TNF Aberrations of TGF beta and Interferon gamma CLINICAL FEATURES Age group 4-75 yrs Common in middle & old age Female predilection 3.3% risk of malignant transformation
PRODROMAL SYMPTOMS/ EARLY OSF Burning sensation while consuming spicy food Blisters ,ulcerations ,altered salivary flow, defective gustatory sensation Appearance of vesicles, petechiae, pain ADVANCED OSF Blanching of mucosa and appearance of white fibrous vertical bands Buccal mucosa and lips are affected first Dense fibrosis of Pterygomandibular raphe results in trismus Restricted tongue movements and depappilation also seen
12
OTHER SYMPTOMS Obstruction of Eustachian tube Nasal intonation of speech TMJ pain Inability to blow
HISTOPATHOLOGY Early stage there is Epithelial Hyperplasia and later stage there is epithelial atrophy Sub-mucosal deposition of extremely dense and avascular collagenous tissue also seen Chronic inflammatory cells seen in connective tissue such as Lymphocytes and Plasma cells DIAGNOSIS Clinical examination and history of betel chewing habit At least one of the following should be present Palpable fibrous band Mucosa tough and leathery Blanching of mucosa and Histopathological features TREATMENT PREVENTION By stoppage of chewing habits EXERCISE In mouth opening MEDICAL Topical or systemic steroids - Vitamin and nutrient supplements - Placentrex - Fibrinolytic agents - Colloidal Iodine - Antioxidants SURGICAL Surgical excision of bands Surgical removal of affected followed by repair with grafts
mucosa
13
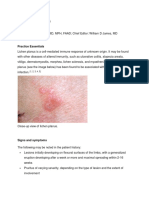
ORAL LICHEN PLANUS Oral Lichen Planus (OLP) is a common chronic immunologic inflammatory mucocutaneous disorder that varies in appearance from Keratotic (reticular or plaque like) to Erythematous and ulcerative. The skin lesions are flat violaceous papules with a fine scaling on the surface. Unlike oral lesions, skin lesions are usually self-limiting, lasting only 1 year or less. ETIOLOGY Cell mediated immune response Autoimmune disease Stress Hepatitis C Virus CLINICAL FEATURES Radiating white or grey, velvety, thread like papules in a linear, annular or retiform arrangement with Wickhams striae 0.3-3% rate of malignant transformation. Common in erosive and atrophic form The Buccal mucosa is the most common site.
TYPES OF LICHEN PLANUS a) b) c) d) e) f) RETICULAR PLAQUE ERYTHEMATOUS BULLOUS PAPULAR EROSIVE
RETICULAR -Fine white striae or lines which form a network or annular pattern with peripheral Erythematous Zoneand usually seen bilaterally in buccal mucosa. 14
PLAQUE TYPE- Homogenous well demarcated white plaque. Common in smokers ERYTHEMATOUS FORM- Homogenous red area and striae seen in periphery BULLOUS FORM Appear as bullous structures surrounded by a reticular network PAPULAR FORM- seen in initial phase of disease, small white dots are seen which intermingle with reticular form EROSIVE FORM disabling form of OLP, fibrin coated ulcers surrounded by an Erythematous zone with radiating white striae HISTOPATHOLOGY Hyperparakeratosis Saw tooth rete pegs Subepithelial band of mononuclear infiltrate Civatte bodies degenerated basal Keratinocytes Max-Joseph space
TREATMENT Topical and systemic steroids Calcineurin inhibitors (Cyclosporine & Tacrolimus) Retinoid & UV phototherapy DYSKERATOSIS CONGENITA Also called Cole Engman Syndrome Rare Genodermatosis, inherited as x-linked characterized by Cutaneous reticulated hyper-pigmentation Nail dystrophy 15
recessive
trait
Pre-malignant leukoplakia of oral mucosa Progressive pancytopenia Striking male predilection is seen ETIOLOGY Mutations in DKC1 gene
CLINICAL FEATURES First manifestation is nail changes that is Dystrophic and shedding of nails at the age of 5yrs Grayish brown pigmentation appear at same time in trunk, neck and thighs Skin becomes atrophic & teleangiectactic. Face becomes red OTHER MINOR FEATURES Frail skeleton Mental retardation Small Sella Turcica Dysphagia Transparent tympanic membrane, deafness Eyelid infections
ORAL MANIFESTATIONS Mucosal Leukoplakia buccal mucosa, tongue & oropharynx Can become verrucous or ulcerative Dysphagia and Dysuria Increased incidence of malignant neoplasms,dental caries,and tooth loss
HISTOLOGICAL FINDINGS 16
Mild hyperkeratosis Epidermal atrophy Teleangiectasia of superficial BV TREATMENT Allogenic bone marrow transplant
DISCOID LUPUS ERYTHEMATOSUS Chronic, scarring, atrophy producing, Photosensitive Dermatosis ETOLOGY Genetic predisposition PATHOGENESIS- heat shock proteins is induced in Keratinocyte following UV exposure or stress and this protein act as target for T cell mediated epidermal cell cytotoxicity CLINICAL FEATURES Third and fourth decade of life and common in women Common sites are face, oral mucous membrane,chest,back and extremities Slightly elevated red or purple macules covered by grey or yellow scales Carpet tack lesions caused by forceful removal of scales Malar rash ORAL MANIFESTATIONS Begin as Erythematous raised or depressed area, without indurations and with white spots Superficial painful ulceration with crusting or bleeding is seen Central healing result in scar formation Common site are vermillion border of lower lips
17
Malignant transformation can occur TREATMENT Corticosteroid Therapy Pulse intravenous Cyclophosphamide regimen followed by quarterly infusion for maintenance is the mainstay of modern therapy
EPIDERMOLYSIS BULLOSA Heterogenous group of inherited mucocutaneous disorders 4 broad categories * Simplex * Junctional * Dystrophic * Hemidesmosomal ETIOLOGY Mutation of gene coding for keratins 5 and 14 causes simplex type Recurrent nonsensense mutation in the LAMB3 gene causes junctional type Mutation of gene encoding for type 4 collagen COL7A1 causes dystrophic type CLINICAL FEATURES EPIDERMOLYSIS BULLOSA SIMPLEX Occurs shortly after birth. Formation of vesicles and bullae on hands and feet at sites of friction or trauma. Heals in 2-10 days 18
without scarring or pigmentation (generalized form) Localized form occur in later childhood.Bullae also seen in oral cavity JUNCTIONAL EPIDERMOLYSIS BULLOSA Onset at birth with absence of scarring or pigmentation and death occurs within 3 months of age . Oral bullae are frequent, extremely fragile and produce feeding problems. Severe disturbance in enamel and dentin formation of deciduous teeth are also seen
DYSTROPHIC EPIDERMOLYSIS BULLOSA ( DOMINANT ) Blisters develop in ankles, knees, elbows, feet and head and it heals with scarring/ keloid. Dystrophic nails, palmar plantar keratosis with hyperhidrosis and hypertrichosis are also seen. Oral bullae also present DYSTROPHIC EPIDERMOLYSIS BULLOSA ( RECESSIVE ) Classical form of the disease withonset at birth and spontaneous bullae formation at sites of trauma, friction or pressure. It also exhibits Nikolskys sign and heals by scarring. Also dystrophic nails and sparse hair. Oral bullae initiated by nursing or any simple dental operative procedure. Scar formation can obliterate sulcus and restrict tongue movements. It can also result in hoarseness and Dysphagia and dental defects like congenitally absent teeth, hypoplastic teeth and rudimentary teeth seen TREATMENT Mild form- topical and intralesional steroids Tetracycline and doxycycline to control desquamative gingivitis Dapsone therapy 19
Long term systemic steroids and immunosuppresive therapy.
XERODERMA PIGMENTOSUM Genetically determined disorder Defective DNA repair mechanism due to excessive chronic UV damage leads to subsequent development of sun related skin tumors including melanoma
CLINICAL FEATURES Increased tendency to sunburn and skin changes like atrophy and freckled pigmentation Development of Actinic keratosis which progress to squamous cell or basal cell carcinoma. Melanoma also develops Oral manifestation squamous cell carcinoma of lower lip and tip of tongue TREATMENT Avoid sun exposure and use protective clothing Topical chemotherapeutic agents like 5 -Flurouracil to treat actinic keratosis Nonmelanoma skin cancers excised conservatively Genetic counselling SIDEROPENIC DYSPHAGIA Also called Plummer Vinson syndrome or Patterson Kelly syndrome Characterized by iron deficiency anemia, glossitis and dysphagia
20
CLINICAL FEATURES Seen in Scandinavian women between 30-50 yrs of age Burning sensation of tongue and oral mucosa Severe angular chelitis Abnormal bands of tissue in esophagus- esophageal web Koilonychia
TREATMENT Dietary iron supplements Esophageal dilation
SYPHILLITIC GLOSSITIS Seen in tertiary stage Surface of tongue gets broken up by fissures due to atrophy and fibrosis of tongue musculature and hyperkeratosis Exclusively seen in males High rate malignant transformation Treatment by intensive antibiotic treatment using Penicillin or Erythromycin or Tetracycline
21
22
23
REFERENCE
BURKETS ORAL MEDICINE 11TH EDITIONGREENBERG,GLICK,SHIP TEXTBOOK OF ORAL PATHOLOGY 6TH EDITION- SHAFER ORAL AND MAXILLOFACIAL PATHOLOGY 3RD EDITION NEVILLE, DAMM, ALLEN, BOUQUOT
24
Вам также может понравиться
- Oral Pre Cancerous LesionsДокумент49 страницOral Pre Cancerous LesionsAmit MishraОценок пока нет
- Precancerous Conditions of Oral CavityДокумент80 страницPrecancerous Conditions of Oral Cavitylarisabrinza12Оценок пока нет
- Oral Leukoplakia: A ReviewДокумент60 страницOral Leukoplakia: A ReviewdimasahadiantoОценок пока нет
- Oral Pathology Hereditary Conditions: Group IДокумент74 страницыOral Pathology Hereditary Conditions: Group IFatima CarlosОценок пока нет
- ORAL PRECURSOR LESION DIAGNOSIS AND MANAGEMENTДокумент51 страницаORAL PRECURSOR LESION DIAGNOSIS AND MANAGEMENTberolyan06Оценок пока нет
- Pre Malignant Conditions of Oral CavityДокумент20 страницPre Malignant Conditions of Oral CavityAsma sultanaОценок пока нет
- Oral Cavity Tumours Including The LipДокумент18 страницOral Cavity Tumours Including The LipBkas GrgОценок пока нет
- Presentation 2Документ32 страницыPresentation 2Dr. Bashir MehrОценок пока нет
- KERATOSIS AND RELATED DISORDERS OF ORAL MUCOSA (2) Edited JsmuДокумент126 страницKERATOSIS AND RELATED DISORDERS OF ORAL MUCOSA (2) Edited JsmuMINI DHABAОценок пока нет
- By:-Surbhi Jaiswal Bds 4 Year. ROLL N0. - 90Документ45 страницBy:-Surbhi Jaiswal Bds 4 Year. ROLL N0. - 90Ranjit BarОценок пока нет
- Potentially Malignant Disorders MADE EASYДокумент11 страницPotentially Malignant Disorders MADE EASYMohammedОценок пока нет
- Premalignant Lesions and Conditions: Submitted by-BALJEET KAUR B.D.S.-3 Year Roll No.15Документ60 страницPremalignant Lesions and Conditions: Submitted by-BALJEET KAUR B.D.S.-3 Year Roll No.15Rajat NangiaОценок пока нет
- White Lesions of The Oral MucosaДокумент213 страницWhite Lesions of The Oral MucosaJunaid Ramzan100% (1)
- Oral Lichen PlanusДокумент28 страницOral Lichen PlanusParul SinghОценок пока нет
- Leukoplakia and HomoeopathyДокумент8 страницLeukoplakia and HomoeopathyDr. Rajneesh Kumar Sharma MD Hom100% (1)
- Diseases of SkinДокумент12 страницDiseases of SkinpayalpachiОценок пока нет
- Actinic Cheilitis: Primary Care Diagnostic InstituteДокумент1 страницаActinic Cheilitis: Primary Care Diagnostic InstituteMuhammad Alief FahrenОценок пока нет
- Module 3-VMED 5335Документ16 страницModule 3-VMED 5335PETJSNVEОценок пока нет
- Idiopathic Non Neoplastic Salivary Gland DiseasesДокумент33 страницыIdiopathic Non Neoplastic Salivary Gland Diseasesgud4nothingОценок пока нет
- Comprehensive Patient Management: Name: Abdulhadi Al Ali ID # 2111050026Документ13 страницComprehensive Patient Management: Name: Abdulhadi Al Ali ID # 2111050026rajtanniruОценок пока нет
- Skin Disorders Affecting Oral Cavity: DR. Parul Khare Iii Mds Sarsawati Dental CollegeДокумент204 страницыSkin Disorders Affecting Oral Cavity: DR. Parul Khare Iii Mds Sarsawati Dental CollegeAMIT GUPTAОценок пока нет
- White & Red Lesion 33333 Lecture (1)Документ16 страницWhite & Red Lesion 33333 Lecture (1)ربيد احمد مثنى يحيى كلية طب الاسنان - جامعة عدنОценок пока нет
- Oral white and red lesions guideДокумент71 страницаOral white and red lesions guideHanin AbukhiaraОценок пока нет
- Drg. Rina Kartika SariДокумент109 страницDrg. Rina Kartika SarimufiОценок пока нет
- Metabolic and Deposition Disorders: Protein Energy Malnutrition, Amyloidosis, Porphyria, and Langerhans Cell HistiocytosisДокумент55 страницMetabolic and Deposition Disorders: Protein Energy Malnutrition, Amyloidosis, Porphyria, and Langerhans Cell HistiocytosisMAHMUDОценок пока нет
- Leukoplakia 170519204224Документ27 страницLeukoplakia 170519204224Mihai SemeniucОценок пока нет
- Australian Dental Journal - 2010 - Schifter - Oral Mucosal Diseases The Inflammatory DermatosesДокумент16 страницAustralian Dental Journal - 2010 - Schifter - Oral Mucosal Diseases The Inflammatory Dermatosesneetika guptaОценок пока нет
- The Small Intestine and Colon Account For The Majority of GIДокумент13 страницThe Small Intestine and Colon Account For The Majority of GIMohammed Yousif AbdualjabbarОценок пока нет
- Report OncoДокумент23 страницыReport Oncoabdallahtarek2000Оценок пока нет
- Oral Lichen Planus: Clinical Presentation and Management: Paul C. Edwards, BSC, MSC, Dds Robert Kelsch, DMDДокумент6 страницOral Lichen Planus: Clinical Presentation and Management: Paul C. Edwards, BSC, MSC, Dds Robert Kelsch, DMDPieter JohnyОценок пока нет
- Lec. 13 &14 Epithelial DisordersДокумент10 страницLec. 13 &14 Epithelial DisordersZainab AlshamaryОценок пока нет
- Pre-Cancerous Lesions: Recognizing Risk and Managing TreatmentДокумент59 страницPre-Cancerous Lesions: Recognizing Risk and Managing TreatmentSowmiya N.MОценок пока нет
- Oral Patho Lecture Shlav BДокумент65 страницOral Patho Lecture Shlav Bشبيبةالروم الملكيين الكاثوليكОценок пока нет
- Oral Potentially Malignant Lesions GuideДокумент9 страницOral Potentially Malignant Lesions GuideAbd RahmanОценок пока нет
- O.patho Lec16Документ12 страницO.patho Lec16Joker KillerОценок пока нет
- A Clinical Approach White LesionДокумент5 страницA Clinical Approach White LesionTirta KusumaОценок пока нет
- Desquamative GingivitisДокумент6 страницDesquamative Gingivitissidra malikОценок пока нет
- Lichen Planus Guide: Causes, Symptoms and TreatmentДокумент37 страницLichen Planus Guide: Causes, Symptoms and TreatmentSaroash SadruddinОценок пока нет
- Common Oral Mucosal Diseases Chapter 1Документ8 страницCommon Oral Mucosal Diseases Chapter 1Nidya PutriОценок пока нет
- Cowden S Disease A Rare Cause of Oral Sis 2002 Journal of Laryngology and OtologyДокумент3 страницыCowden S Disease A Rare Cause of Oral Sis 2002 Journal of Laryngology and Otologydasea01Оценок пока нет
- Pathology of The Oral Cavity and Salivary GlandsДокумент10 страницPathology of The Oral Cavity and Salivary GlandsAbdul hadiОценок пока нет
- Learning Objectives in Gastrointestinal PathologyДокумент15 страницLearning Objectives in Gastrointestinal PathologyZul Azim AnuarОценок пока нет
- Preutz-Jegher SyndromeДокумент13 страницPreutz-Jegher SyndromeYong EnОценок пока нет
- Pediatric Oral MedicineДокумент17 страницPediatric Oral MedicinebanyubiruОценок пока нет
- Orallichenplanus 170929075918Документ40 страницOrallichenplanus 170929075918Aymen MouradОценок пока нет
- Vitiligo: Refer ATДокумент18 страницVitiligo: Refer ATAndhika FrabesОценок пока нет
- Lichen Planus Guide: Symptoms, Diagnosis and TreatmentДокумент17 страницLichen Planus Guide: Symptoms, Diagnosis and TreatmentRahma Tya Anwar0% (1)
- Commonrashes in Neonates201205suДокумент6 страницCommonrashes in Neonates201205suDanielcc LeeОценок пока нет
- 494 PDFДокумент6 страниц494 PDFranz ibonkОценок пока нет
- Dent 355-10 Keratoses and Related Disorders of Oral MucosaДокумент23 страницыDent 355-10 Keratoses and Related Disorders of Oral MucosaHamna FitriahОценок пока нет
- Oral Precancerous Lesions: Leukoplakia and ErythroplakiaДокумент76 страницOral Precancerous Lesions: Leukoplakia and ErythroplakiaPrima D Andri100% (1)
- Physical and Chemical Injuries: Oral Complications of H and N Radiation TherapyДокумент5 страницPhysical and Chemical Injuries: Oral Complications of H and N Radiation TherapynewmexicoomfsОценок пока нет
- Premalignant LesionsДокумент76 страницPremalignant LesionsGowri RaguОценок пока нет
- Differential Diagnosis 1. Atopic Dermatitis History TakingДокумент13 страницDifferential Diagnosis 1. Atopic Dermatitis History TakingCocoi MellaОценок пока нет
- MedicinДокумент40 страницMedicinAymen MouradОценок пока нет
- Leukoplakia 201119144109Документ24 страницыLeukoplakia 201119144109saldy meirisandyОценок пока нет
- Oral Submucous FibrosisДокумент18 страницOral Submucous FibrosisDrVaibhav ShrivastavaОценок пока нет
- Complete HolmesДокумент989 страницComplete HolmesDeepeshKediaОценок пока нет
- Green Engine Seminar Report PDFДокумент22 страницыGreen Engine Seminar Report PDFJitendra Panwar100% (1)
- Ch04oral MedicineДокумент35 страницCh04oral MedicineNaleena JosephОценок пока нет
- Potentially Malignant Lesions and ConditionsДокумент24 страницыPotentially Malignant Lesions and ConditionsNaleena JosephОценок пока нет