Академический Документы
Профессиональный Документы
Культура Документы
197
Загружено:
Husayn NgaillahИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
197
Загружено:
Husayn NgaillahАвторское право:
Доступные форматы
197
Antiphospholipid Syndrome Associated with Cytomegalovirus Infection: Case Report and Review
Jaime A. Labarca, Ricardo M. Rabaggliati, Francisco J. Radrigan, Paula P. Rojas, Carlos M. Perez, Marcela V. Ferres, Guillermo G. Acuria, and Pablo A. Bertin
From the Departments of Internal Medicine, Rheumatology, Pediatrics, and Hematology-Oncology, Escuela de Medicina, Pontificia Universidad CatOlica de Chile, Santiago, Chile
Antiphospholipid antibodies are commonly related to connective tissue disorders, the use of certain drugs, and infection. It is thought that antiphospholipid syndrome (APS) is associated primarily with connective tissue disorders. We describe a healthy young male who had an episode of APS that was associated with cytomegalovirus infection and who developed mesenteric and femoropopliteal thrombosis. He responded well to treatment with anticoagulants; 6 months after the onset of APS, IgM and IgG anticardiolipin antibody titers declined. We point out the importance of screening for infectious agents in cases of APS; if the agents are identified, APS may be transitory.
Downloaded from http://cid.oxfordjournals.org/ by guest on February 9, 2012
Available data indicate that --.50% of episodes of vascular thrombosis can be attributed to factors that clearly promote thrombosis. The hypercoagulable states that present as arterial thrombosis or venous thrombosis in one or more sites can be caused by alterations in protein C or protein S, antithrombin III deficiency, activated protein C resistance, abnormalities in the fibrinolytic system, and the presence of anticardiolipin antibodies [1]. Anticardiolipin antibodies have been reported in association with bacterial, viral, and parasitic infections [2, 3]. We describe a patient who developed vascular thrombosis in two regions; this condition was associated with the transitory presence of anticardiolipin antibodies and acute cytomegalovirus (CMV) infection.
Case Report
A healthy 35-year-old male with no history of thrombosis, thrombocytopenia, transient ischemic attacks, or livedo reticularis was in his usual good state of health until the first week of December 1994, when he developed pain in the epigastrium and in the right abdominal quadrants that was associated with weakness and anorexia. Three weeks later he developed lowgrade fever (temperature, <38C) and a nonproductive cough in association with progressive worsening of the abdominal pain; he was admitted to the hospital. Physical examination revealed a temperature of 37.8C, a pulse rate of 86, and a blood pressure of 120/70 mm Hg. His skin had a slight icteric tint, and bilateral cervical lymphadenopathy was noted. Examination of the abdomen revealed only
Received 21 February 1996; revised 31 July 1996. Reprints or correspondence: Dr. Jaime Labarca, UCLA Clinical Microbiology Laboratories, 11633 San Vicente Boulevard, 4th Floor, Los Angeles, California 90049.
Clinical Infectious Diseases 1997; 24:197-200 1997 by The University of Chicago. All rights reserved. 1058-4838/97/2402-0017$02.00
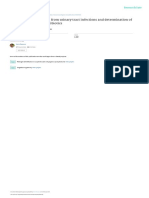
diffuse tenderness. There were no signs of peritoneal involvement. Findings of the remainder of the physical examination were unremarkable. Twenty-four hours after admission, the patient's right leg began to swell. Laboratory studies done on admission showed a WBC count of 7,600/mm 3 with 41% lymphocytes; a hematocrit of 43%; and an erythrocyte sedimentation rate of 27 mm/h. Liver function studies revealed elevated levels of aspartate aminotransferase (65 U/L; normal range, 0-37 U/L), alanine aminotransferase (89 U/L; normal range, 0-40 U/L), and bilirubin (4.72 amol/L). A contrast-enhanced CT scan of the abdomen demonstrated splenomegaly and thrombosis of the superior mesenteric vein (figure 1). A Doppler ultrasonogram of the right leg showed the presence of femoropopliteal venous thrombosis. The coagulation work-up included partial thromboplastin time; prothrombin time; serum levels of lupus anticoagulant, protein C and S, and antithrombin III; activated protein C resistance; and an assay for anticardiolipin antibodies. All results were normal except for the presence of anticardiolipin antibodies: the values were IgM, 42.6 MPL (1 MPL is the phospholipid binding activity of 1 pg/mL of an affinity-purified IgM antibody; normal value, < 10 MPL); IgG, 25.2 GPL (1 GPL is the phospholipid binding activity of 1 Ag/mL of an affinity-purified IgG antibody; normal value, < 10 GPL); and a slightly lower than normal value for protein S (0.32 U/mL; normal value, >0.58 U/mL). Cultures of blood and urine were performed to determine the cause of the febrile syndrome; both were negative. Tests were performed to detect the presence of HIV; hepatitis A virus, hepatitis B virus, and hepatitis C virus; Epstein-Barr virus; and CMV. Findings on chest radiograph were normal. Serology showed the presence of acute infection with CMV: the titer of IgM was 2.446 A450 (absorbance units), and that of IgG was 0.726 A450 during the first week (cutoff values, 0.273 A450 and 0.148 A450, respectively). During the third week, the titer of IgM was 1.387 A450 and that of IgG was
198
Labarca et al.
CID 1997;24 (February)
Figure 1. Abdominal CT scan of patient with antiphospholipid syn-
drome and cytomegalovirus infection shows occlusion of the superior mesenteric vein by a thrombus (arrow).
1.280 A450 (cutoff values, 0.296 and 0.148, respectively).
CMV was also isolated from urine. The patient was treated systematically with heparin, followed by oral acenocumarol. He remained febrile for the first 5 days after admission; the fever then remitted spontaneously. The patient was discharged in good condition after 10 days of hospitalization. Five months after discharge, titers of IgM and IgG anticardiolipin antibodies had decreased to 1.30 MPL and 12.1 GPL, respectively; therefore, anticoagulant treatment was discontinued. Twelve months after discharge, he remains asymtomatic.
cold agglutinins, rheumatoid factor, and anticomplement antibodies [6]. Antiphospholipid antibodies, anticardiolipin antibodies, and lupus anticoagulant are a group of antibodies with apparent affinity for anionic phospholipids. Their presence is associated with APS. The most specific clinical features of APS are venous or arterial thrombosis, recurrent fetal loss, and autoimmune thrombocytopenia. This syndrome is known as primary APS (PAPS) when it is not associated with systemic disease and secondary APS when it occurs in patients with underlying autoimmune disease, usually systemic lupus erythematosus (SLE) [7, 8]. Two types of antiphospholipid antibodies have been described: those that are related to PAPS or secondary APS, and have a pathogenic effect and those that are associated with infections [9] or certain drugs [10] or that are present in the 10%-20% of healthy individuals, especially the elderly [11], who do not develop this syndrome [9]. In this latter group, antiphospholipid antibody is not pathogenic and probably represents an epiphenomenon. Antiphospholipid antibodies have been associated with various infectious diseases: 75% of patients with syphilis have these antibodies [9]. Antiphospholipid antibodies have also been reported in patients with acute infections due to adenovirus, rubella virus, varicella-zoster virus, mumps virus [12],
Mycoplasma pneumoniae [12, 13], Mycobacterium tuberculosis [14], Schistosoma species [14], Borrelia burgdorferi [15], and Plasmodium species [14, 16]. The presence of these anti-
Downloaded from http://cid.oxfordjournals.org/ by guest on February 9, 2012
Discussion
Infection caused by CMV is highly prevalent in the general population. Seroprevalence studies have shown that infection ranges between 40% and 100%; the likelihood of infection increases with age [4]. The most common clinical manifestation is a mononucleosislike syndrome, but CMV infection can also present as interstitial pneumonitis, hepatitis, myocarditis, meningoencephalitis, thrombocytopenia, hemolytic anemia, retinitis, or asymptomatic subclinical infection in immunocompetent patients. Serological studies are widely used for diagnosis; an increase in IgG antibody titers confirms the presence of acute infection with CMV. The virus is not normally isolated from the pharynx or from cultures of blood or urine, so its presence indicates infection [5]. Serological abnormalities have been described in patients with CMV mononucleosis or infectious mononucleosis. These abnormalities include the presence of cryoglobulins,
bodies is not usually associated with APS. Investigators have focused on the relation between viral diseases and the production of antiphospholipid antibodies. These antibodies can be found in a relatively high percentage of patients with infections caused by parvovirus, Epstein-Barr virus, hepatitis A virus, hepatitis B virus, and rubella virus [17]. Thirty-nine percent of 33 patients with infectious mononucleosis were found to have positive titers of IgM anticardiolipin antibodies, and 12% had positive titers of IgG anticardiolipin antibodies; none of the controls had either antibody subtype [18]. The frequency of anticardiolipin antibodies varies between 23% and 75% among HIV-infected individuals [19-24], and the presence of these antibodies is not related to the stage of the disease [23, 25] nor, apparently, to the presence of APS. It has been shown that pathogenic anticardiolipin antibody, which is associated with APS, requires the plasma protein P 2 glycoprotein I (GPI) to bind cardiolipins. On the other hand, anticardiolipin antibodies induced by infections do not require this cofactor to bind cardiolipins and are considered nonpathogenic [26-29]. We studied anticardiolipin antibody with and without the presence of this cofactor in our patient, and we found that anticardiolipin antibody required the presence of GPI to bind cardiolipins. In contrast to what was demonstrated in the present case, previous studies suggest that antiphospholipid antibodies induced by infection have no pathogenic role. It is possible that
CID 1997;24 (February)
APS and Cytomegalovirus Infection
199
one patient can produce both types of antiphospholipid antibodies. In one study, the lymphocytes of another patient with PAPS were studied in vitro, and the results showed that it was possible to induce two lines of anticardiolipin antibody-producing cells when the lymphocytes were exposed to Epstein-Barr virus: one 'ine produced pathogenic anticardiolipin antibodies, and the other produced nonpathogenic anticardiolipin antibodies [30]. This finding suggests that the difference between pathogenic anticardiolipin antibodies in patients with PAPS or SLE and nonpathogenic anticardiolipin antibodies in patients with infections is not absolute and that an individual exposed to a particular stimulus could produce both kinds of antibodies. There is evidence that patients with anticardiolipin antibody-associated infections could have the clinical manifestation of APS. During 55 pregnancies among 46 HIV-infected patients, 11 patients with anticardiolipin antibodies showed a significant tendency to have smaller placentas than did those without these antibodies [22]. Furthermore, cases of deep vein thrombosis in patients with tuberculosis are possibly associated with the presence of anticardiolipin antibodies [31]. Moreover, Yamakazi et al. [32] reported the case of a 25-year-old patient with Epstein-Barr virus infection who developed a transient rise in titers of antiphospholipid antibodies that was associated with an episode of deep vein thrombosis of the lower extremity, similar to the case we have described. It is noteworthy that our patient was previously completely healthy. However, it is highly probable that he may have had a congenital deficit of protein S, which was of no clinical importance because he had no clinical manifestations until this episode of APS occurred. It is possible that this mild deficit could have influenced the development of the hypercoagulable state. Not only were our patient's laboratory test results abnormal, but there were also serious clinical manifestations typical of APS, consisting of thrombosis that occurred simultaneously in two independent regions. Furthermore, the anticardiolipin antibodies detected are not those usually induced by infectious agents but are the type that are present in patients with APS. Although thrombotic phenomena can cause fever, the presence of thrombosis itself cannot explain the entire clinical picture for this patient; thus, the clinical and laboratory findings prompted us to search for a possible viral infection. Finally, infection with CMV in this patient was confirmed. The temporal association between thrombosis and infection suggests a causative association rather than the coincidental occurrence of two separate phenomena. The decrease in titers of anticardiolipin antibodies indicates the transient character of APS; thus, patients with a decrease in these titers may have a more favorable prognosis than patients whose illness is produced by chronic disease (e.g., lupus). We therefore emphasize the importance of considering possible infectious agents in episodes of APS. As there are no precedents in the literature, it was difficult to decide how long to treat the patient with oral anticoagulants.
To our knowledge, this is the first reported case of a patient with acute CMV infection who developed thrombosis due to a transient rise in titers of anticardiolipin antibodies (confirmed by the decrease in titers of these antibodies). Although these antibodies are frequently present during infections, APS with thrombosis is a rare complication.
Acknowledgments
The authors thank Dr. Sergio Jacobelli for his assistance and suggestions in preparing the manuscript and Mrs. Ximena Soza for her technical support at the Immunology Laboratory, Department of Rheumatology, Pontificia Universidad CatOlica de Chile.
Downloaded from http://cid.oxfordjournals.org/ by guest on February 9, 2012
References
1. Bick RL. Hypercoagulability and thrombosis. Med Clin North Am 1994; 78:635-65. 2. Bick RL, Baker WF Jr. The antiphospholipid and thrombosis syndromes. Med Clin North Am 1994; 78:667-84. 3. Lockshin MD. Antiphospholipid antibody syndrome. Rheum Dis Clin North Am 1994;20:45-59. 4. Ho M. Epidemiology of cytomegalovirus infections. Rev Infect Dis 1990; 12(suppl 7):S701 -10. 5. Sunwen C. Newer methods for diagnosis of cytomegalovirus infection. Rev Infect Dis 1990; 12(suppl 7):S727-36. 6. Ho M. Cytomegalovirus. In: Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas and Bennett's principles and practice of infectious diseases. 4th ed. Vol 2. New York: Churchill Livingstone, 1995:1351-64. 7. Hughes GRV, Harris NN, Gharavi AE. The anticardiolipin syndrome. J Rheumatol 1986;13:486-9. 8. Roubey RAS. Update on the antiphospholipid antibody syndrome. Cliniguide to Rheumatology 1994;4:1-8. 9. Love PE, Santoro SA. Antiphospholipid antibodies: anticardiolipin and the lupus anticoagulant in systemic lupus erythematosus (SLE) and in non-SLE disorders. Prevalence and clinical significance. Ann Intern Med 1990;112:682-98. 10. Canoso RT, Sise HS. Chlorpromazine-induced lupus anticoagulant and associated immunologic abnormalities. Am J Hematol 1982;13:121-9. 11. Manoussakis MN, Tzioufas AG, Silis MP, Pange PJ, Goudevenos J, Moutsopoulos HM. High prelevance of anti-cardiolipin and other autoantibodies in a healthy elderly population. Clin Exp Immunol 1987; 69: 557-65. 12. Vaarala 0, Palosuo T, Kleemola M, Aho K. Anticardiolipin response in acute infections. Clin Immunol Immunopathol 1986;41:8-15. 13. Snowden N, Wilson PB, Longson M, Pumphrey RS. Antiphospholipid antibodies and Mycoplasma pneumoniae infection. Post Grad Med J 1990; 66:356-62. 14. Adebajo AO, Charles P, Maini RN, Hazleman BL. Autoantibodies in malaria, tuberculosis and hepatitis B in a West African population. Clin Exp Immunol 1993;92:73-6. 15. Macworth-Young CG, Harris EN, Steere AC, et al. Anticardiolipin antibodies in Lyme disease. Arthritis Rheum 1988;31:1052-6. 16. Soni PN, De Bruyn CC, Duursma J, Sharpe BL, Pudifin DJ. Are anticardiolipin antibodies responsible for some complications of severe Plasmodium falciparum malaria? S Afr Med J 1993; 83:660-2. 17. Colaco CB, Mackie IJ, Irving W, Machin SJ. Anticardiolipin antibodies in viral infection [letter]. Lancet 1989; 333:622. 18. Misra R, Venables PJV, Watkins RP, Maini RN. Autoimmunity to cardiolipin in infectious mononucleosis [letter]. Lancet 1987;2:629.
200
Labarca et al.
CID 1997;24 (February)
19. Taillan B, Roul C, Fuzibet JG, et al. Antiphospholipid antibodies associated with human immunodeficiency virus infection [letter]. Arch Intern Med 1990; 150:1975. 20. Lafeuillade A, Delbeke E, Chaffanjon P, et al. Value of anticardiolipin antibody assay in human immunodeficiency virus infection. Presse Med
1990;19:1225-7.
21. Viscarello RR, Williams CJ, DeGennaro NJ, Hobbins JC. Prevalence and prognostic significance of anticardiolipin antibodies in pregnancies complicated by human immunodeficiency virus-1 infection. AM J Obstet Gynecol 1992; 167:1080-5. 22. Johnstone FD, Kilpatrick DC, Burns SM. Anticardiolipin antibodies and pregnancy outcome in women with human immunodeficiency virus infection. Obstet Gynecol 1992; 80:92-6. 23. Coll-Daroca J, Gutierrez-Cebollada J, Yazbeck H, Berges A, Rubies-Prat J. Anticardiolipin antibodies and acquired immunodeficiency syndrome: prognostic marker or association with HIV infection? Infection 1992; 20:140-2. 24. Matsuda J, Saitoh N, Tsukamoto M, Gohchi K, Asami K, Hashimoto M. Measurement of beta 2-glycoprotein I (apolipoprotein H)independent anticardiolipin antibody in human immunodeficiency virus-l-positive and negative hemophiliacs. Am J Hematol 1993;43:146-8. 25. Llorente MR, Carton JA, Carcaba V, et al. Antiphospholipid antibodies in human immunodeficiency virus infection. Med Clin (Barc) 1994; 103:10-3.
26. Matsuura E, Igarashi Y, Fujimoto M, et al. Anticardiolipin cofactors and differential diagnosis of autoimmune disease. Lancet 1990; 336: 177 8. 27. Gharavi AE, Sammaritano LR, Wen J, et al. Characteristics of human immunodeficiency virus and chlorpromazine induced antiphospholipid antibodies: effect of beta 2 glycoprotein I on binding to phospholipid. J Rheumatol 1994;21:94-9. 28. Hunt J, McNeil P, Morgan G, Crameri R, Krilis S. A phospholipid-02glycoprotein I complex is an antigen for anticardiolipin antibodies occurring in autoimmune disease but not with infection. Lupus 1992;1: 75 81. 29. Shoenfeld Y, Meroni PL. The beta-2-glycoprotein I and the antiphospholipid antibodies. Clin Exp Rheumatol 1992;10:205-9. 30. Hasegawa Y, Suzuki T, Ishii S, Takakuwa K, Tanaka K. Establishment of two distinct anticardiolipin antibodyproducing cell lines from the same individual by Epstein Barr virus transformation. Thromb Res
1993; 74:77-84.
31. Suarez Ortega S, Artiles Vizcaino J, Balda Aguirre Y, et al. Tuberculosis as risk factor for venous thrombosis. An Med Interna 1993;10: 398-400. 32. Yamazaki M, Asakura H, Kawamura Y, Okha T, Endo M, Matsuda T. Transient lupus anticoagulant induced by Epstein-Barr virus infection. Blood Coagul Fibrinolysis 1991;2:771-4.
Downloaded from http://cid.oxfordjournals.org/ by guest on February 9, 2012
Вам также может понравиться
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- NCP JourrnallldsdДокумент17 страницNCP JourrnallldsdCHRISTINE JOY. MOLINAОценок пока нет
- PhobiaДокумент4 страницыPhobiaZeba QuadiriОценок пока нет
- Treating Canine Distemper VirusДокумент23 страницыTreating Canine Distemper VirusJack HollandОценок пока нет
- Standard Coding Guideline ICD-10-TM 2006Документ192 страницыStandard Coding Guideline ICD-10-TM 2006api-3835927100% (1)
- Essential Questions in Paediatrics For MRCPCH v2 PDFДокумент208 страницEssential Questions in Paediatrics For MRCPCH v2 PDFa4aboo100% (11)
- Energy Drinks Are Bad RealДокумент4 страницыEnergy Drinks Are Bad RealMadihi NorhadiОценок пока нет
- Chronic Kidney DiseaseДокумент22 страницыChronic Kidney DiseaseAchmad ZainudinОценок пока нет
- Nurse Shift PDFДокумент11 страницNurse Shift PDFWisnu YogaОценок пока нет
- Clinical Features and Diagnosis of Abdominal Aortic Aneurysm - UpToDateДокумент53 страницыClinical Features and Diagnosis of Abdominal Aortic Aneurysm - UpToDateALVARO ARIASОценок пока нет
- Axa Group Corporate PresentationДокумент35 страницAxa Group Corporate PresentationRajneesh VermaОценок пока нет
- WES Ablasi SVT AVRT - Travilla Bastian A. PangestutiДокумент1 страницаWES Ablasi SVT AVRT - Travilla Bastian A. PangestutiHervin RamadhaniОценок пока нет
- Campylobacter Jejuni-Mediated Guillain-Barre Syndrome, An Overview of The Molecular Mimicry and Vaccine Development ApproachesДокумент9 страницCampylobacter Jejuni-Mediated Guillain-Barre Syndrome, An Overview of The Molecular Mimicry and Vaccine Development ApproachesInternational Medical Publisher0% (1)
- Counseling TechniquesДокумент60 страницCounseling Techniquesdinalen0% (1)
- Pe 11 Quarter 3 Lesson 1Документ17 страницPe 11 Quarter 3 Lesson 1Donah Kate AlbaОценок пока нет
- WellCat Veterinary HandbookДокумент36 страницWellCat Veterinary HandbookKatSiebrecht100% (5)
- The Conceptual Evolution of DSM 5Документ391 страницаThe Conceptual Evolution of DSM 5monkey85222100% (3)
- Diabetic Nephropathy BaruДокумент24 страницыDiabetic Nephropathy BaruRobiyanti Nur Chalifah HattaОценок пока нет
- McWilliams Center For Counseling, Inc. Community Support Office - 438Документ2 страницыMcWilliams Center For Counseling, Inc. Community Support Office - 438James BennettОценок пока нет
- Job DescriptionsДокумент139 страницJob DescriptionsAbdullah Bin SaeedОценок пока нет
- PNC Checklist AfricanДокумент2 страницыPNC Checklist AfricanAudrey Andini0% (1)
- Emergency Department Triage Prediction Ofclinical Outcomes Using Machine Learning Models PDFДокумент13 страницEmergency Department Triage Prediction Ofclinical Outcomes Using Machine Learning Models PDFOscar Julian Perdomo CharryОценок пока нет
- Treatment Modalities Applicable To The Psychiatric ClientДокумент53 страницыTreatment Modalities Applicable To The Psychiatric Clientnickybore100% (1)
- The Aao "At-A-Glance" Guide To CDT 2021 Orthodontic Codes: DentitionДокумент2 страницыThe Aao "At-A-Glance" Guide To CDT 2021 Orthodontic Codes: DentitionSweet ToothОценок пока нет
- University of Zimbabwe Dissertation TopicsДокумент4 страницыUniversity of Zimbabwe Dissertation TopicsCustomWritingPaperServiceCanada100% (1)
- Infusion PumpДокумент14 страницInfusion PumpSREEDEVI T SURESHОценок пока нет
- Bacteria Found in UrineДокумент7 страницBacteria Found in UrineAria DomingoОценок пока нет
- McGrath Video Laryngoscope Rev 0.1Документ6 страницMcGrath Video Laryngoscope Rev 0.1adevasenОценок пока нет
- Physical Abuse Teaching SlidesДокумент19 страницPhysical Abuse Teaching SlidesbentoeОценок пока нет
- Avian Influenza in ChickensДокумент19 страницAvian Influenza in ChickensShah NawazОценок пока нет
- The Apolinario Mabini Syphilis Rumors and Late 19th Century Philippine Power PlayДокумент15 страницThe Apolinario Mabini Syphilis Rumors and Late 19th Century Philippine Power PlayHaneul KImОценок пока нет