Академический Документы
Профессиональный Документы
Культура Документы
Pediatric Burns
Загружено:
Claudia Pamela Castro AuzaИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Pediatric Burns
Загружено:
Claudia Pamela Castro AuzaАвторское право:
Доступные форматы
The Journal of TRAUMA Injury, Infection, and Critical Care
Assessment of Adverse Events in the Demise of Pediatric Burn Patients
Dennis C. Gore, MD, Hal K. Hawkins, MD, David L. Chinkes, PhD, Dai H. Chung, MD, Arthur P. Sanford, MD, David N. Herndon, MD, and Steven E. Wolf, MD
Background: Given the contention that survival is to be expected from even the most severely burned child, then, intuitively, at least some pediatric burn victims die because of suboptimal care. The purpose of this study is to assess the impact of any adverse events that may have contributed to the death of burned children. Methods: Four surgeons with specialty training in pediatric burn care reviewed the clinical course and autopsy findings of 71 burned children who died after admission to a burn center during a 10-year interval. Reviewers were asked to
determine the predominant factor or factors contributing to each childs demise and to assess the significance of any deviations from optimal care. Results: For the 10 years under review, overall mortality for all pediatric burns was 2.4%. Of these deaths, 25% had burns encompassing less than 50% body surface area. The reviewers identified lung damage as the most frequent cause of death, which was deemed largely unpreventable. Conversely, hypovolemia related to inadequate prehospital fluid resuscitation and failure to obtain and maintain a patent airway were considered the second and third most common factors in a childs death and deemed preventable under ideal circumstances. Conclusions: This review implies that deficiencies in health care contribute to the demise of many burned children. The most notable areas for improvement are in fluid resuscitation and airway control. This suggests that quality assurance and educational initiatives to improve these aspects of care may have the greatest impact on further improving survival of burned children. Key Words: Patient safety, Quality assurance, Medical error.
J Trauma. 2007;63:814 818.
istorically the main determinants of mortality from burn injury have been age, the extent of burn, and the presence or absence of inhalation injury.13 Yet with the remarkable advances in burn care and the associated improvements in survival, the traditional determinants of skin and lung damage may no longer have a dominant influence on survival of the young.2 This contention is supported by Sheridan et al.,4 who examined the clinical course of burned children who subsequently died at the Shriners Burns Hospital in Boston. By comparing patients cared for from 1974 to 1980 with those patients seen between 1991 and 1997, and stratified by burn size, these authors concluded that the chance of survival after a burn has greatly improved for children to the extent that even the very young and severely burned child should survive. Dr. Saffle,5 a recent president of the American Burn Association, echoed this sentiment, commenting that for adolescents and young adults, almost no burn is too extensive to preclude recovery. Demonstrating that such an ambitious goal is possible, we recently reviewed
Submitted for publication February 1, 2006. Accepted for publication April 13, 2007. Copyright 2007 by Lippincott Williams & Wilkins From the Shriners Hospitals for Children (H.K.H., D.L.C., A.P.S., D.N.H.) and Department of Surgery (D.C.G., D.H.C., D.N.H.), The University of Texas Medical Branch, Galveston, and the Department of Surgery (S.E.W.), University of Texas Health Science Center, San Antonio, Texas. Address for reprints: Dennis C. Gore, MD, Department of Surgery, The University of Texas Medical Branch, 301 University Boulevard, Galveston, TX 77555-1172; email: dcgore@utmb.edu. DOI: 10.1097/TA.0b013e31811f3574
the outcome of pediatric patients with burns of greater than 80% of their body surface.6 Amazingly, more than 60% of these severely burned victims survived. Yet, regardless of these therapeutic advancements and miraculous survivals, victims of burn injury still die. At our institution alone there were 18 deaths during a past year. Because these publications imply that survival is to be expected, one must conclude that at least some pediatric burn victims die because either the correct intervention was not performed, was not performed in a timely fashion, or was not performed correctly. The purpose of this study was to appraise the major determinants of death in burned children and assess the impact of any adverse event that may have contributed to the demise of these children. It is hoped that this review and analysis may identify those factors, which are potentially correctable and thereby guide future maneuvers to improve survival.
PATIENTS AND METHODS
Records
Of a total of 3,005 admissions to the Shriners Hospitals for Children in Galveston, TX from January 1992 through December 2001, there were 72 deaths. Except for one child whose family refused autopsy on religious edict, autopsies were performed on all (71) children. All but four of these autopsies were performed by a single pathologist (H.K.H.). Three of these autopsies were performed at the adjacent University Pathology Department of the University of Texas Medical Branch with the findings recorded in the identical format prescribed by the specialty pathologist. The single October 2007
814
Adverse Events in Burn Care
remaining autopsy was performed by the county coroner. In addition to the autopsy findings, the pathologist also reviewed each patients hospital records and reported a summary of the clinical course for each patient. These clinical case summaries were available for all 72 deaths. For all admissions to the Shriners hospital during this 10-year interval, patient characteristics and demographics were available on computerized hospital records.
Table 1 Patient Characteristics
Survivors Deaths
N Age (yr) Body weight (kg) TBSA burn (%) TBSA third burn (%) Inhalation injury (%)
2,933 6.4 2.1 27.6 3.9 26 5 14 4 16
72 5.7 1.8 26.1 5.1 66 3* 60 3* 60
Review Process
After approval from the Institutional Review Board, autopsies and clinical course records were reviewed by four surgeons, all of whom have experience in burn care; three having completed postresidency fellowships in burn care at a Shriners Hospitals for Children, the other with fellowship training in pediatric surgery and with more than 10 years experience as a physician consultant at the Shriners Hospitals for Children. Using a standardized form, each reviewer was asked to note the probable cause of death and any associated factors contributing to death. Reviewers were also asked to scale the contribution of any deficiencies in care to the cause of death, from 1 (denoting no error) to 4 (denoting a significant impact of negligence on the childs death). Also scaled from 1 to 4 by each reviewer were (1) the percent chance that a misadventure caused death and (2) the possibility of surviving to discharge had the error not occurred. For grading items 1 and 2, reviewers agreed on the following scale: 1 0% to 15%, 2 16% to 50%, 3 51% to 84%, and 4 85% to 100%. Each reviewer was screened from the decisions of the other reviewers.
Values are mean SEM. * p 0.01 comparison by Students t test. p 0.05 comparison by 2. TBSA, total body surface area.
Table 2 Deaths Stratified by Severity of Burn
Burns 50% (n 2,602) Burns 50; 80% (n 259) Burns 80% (n 72)
Number of deaths Mortality (%) Age (yr) TBSA burn (%) Inhalation injury, n (%)
19 0.7 5.4 1.4 40 3 8 (42)
31 12* 7.1 2.8 71 2* 19 (61)
22 30* 6.8 3.0 91 2* 16 (73)
Values are mean SEM. * p 0.01 comparison by Students t test. p 0.06 comparison by 2.
Table 3 Primary Causes of Death and Factors Contributing to Death
Adverse Event Primary Cause of Death ( ) Contributing Factor ( )
Statistics
Patient characteristics between survivors and deaths were compared using a Students independent t test. Differences in the incidence of inhalation injury between survivors and deaths were assessed using 2. Median values between raters were used to report the incidence of an event. Median and mean values corresponded closely for all variables, so mean values are not reported. Inter-rater agreement was assessed using simultaneous -statistics for variables that had an incidence of at least 10%. values of greater than 0.7 were considered significant and indicative of strong inter-rater agreement.
Diffuse alveolar lung damage (%) Hypovolemia/inadequate resuscitation (%) Airway loss/aspiration (%) Pneumonia (%) Burn wound sepsis (%) Anoxia (%) Drug reaction (%) Data are median values. -statistics for inter-rater significant.
25 (0.32) 16 (0.24) 15 (0.48) 13 (0.24) 13 (0.31) 7 1 agreement 0.7
51 (0.32) 23 (0.32) 22 (0.47) 23 (0.34) 33 (0.53) 20 (0.53)
considered
RESULTS
The overall mortality for all hospital admissions during the 10 years of review was 2.4%. Comparison of patient characteristics between survivors and deaths is shown in Table 1 with deaths having a significantly greater extent of burn and a higher incidence of inhalation injury. In Table 2, patients characteristics are stratified by their severity of burn demonstrating a significant association between a greater surface area burn to increasing mortality. Of note, there were 19 deaths (mortality rate 0.7%) of patients admitted to the hospital with burns encompassing 50% of their body surface area. Volume 63 Number 4
The reviewers determined that diffuse alveolar damage of the lungs was the most prevalent primary cause of death (Table 3). Hypovolemia and inadequate emergency resuscitation were considered the second most common cause of death. Loss of airway or aspiration, pneumonia, and burn wound sepsis were designated as the third, fourth, and fifth most common primary causes of death, respectively. Death related to anoxic brain damage occurring at the time of the fire was noted as the cause of death in five children; the sixth most frequent cause of death. One child died from an apparent anaphylactic drug reaction. For the five most frequent causes of death, there was no significant agreement between reviewers with a maximum score for airway or aspiration at 815
The Journal of TRAUMA Injury, Infection, and Critical Care
0.48. As to whether adverse events contributed to death, reviewers noted diffuse alveolar lung damage as the most common contributing factor to death (Table 3). Burn wound sepsis, pneumonia, hypovolemia or inadequate resuscitation, and airway loss or aspiration completed the five most commonly noted factors contributing to a childs demise. There was no significant inter-rater agreement in designating an adverse contributing factor with a maximum score for burn wound sepsis at 0.53. Reviewers assessment as to the significance of any error in each childs death is shown in Table 4. The cumulative score for all patients on a 1 to 4 scale was 2.4. Thus, in the aggregate opinion of the reviewers, suboptimal care contributed significantly in the demise of approximately 50% of the burn victims. Stratifying the significance of any deficiency in care by cause of death, drug reaction, airway loss or aspiration, and hypovolemia or inadequate resuscitation was considered by the reviewers to be frequently associated with negligence. In contrast, error was not deemed of much importance to either anoxic brain injury or diffuse alveolar lung damage. The impact of a medical misadventure on the demise of each child was also assessed by the reviewers determination of a percentage chance that error contributed to a childs death (Table 5). Also scaled 1 to 4, physician reviewers assessed a cumulative score for this impact of error at 2.3, translating into the reviewers perception that medical misadventure contributed to a childs demise is about 50% of all burn victims. There was, however, a wide range of disagree-
Table 6 Inter-Rater Variability for Percent Chance of Surviving had Error not Occurred
Reviewers Scores 1 2 3 4
1 2 3 4 Mean
50 (71) 21 (29) 27 (38) 31 (44) 6 (8) 23 (32) 6 (8) 21 (29) 6 (8) 13 (18) 13 (18) 4 (6) 9 (13) 14 (20) 25 (35) 15 (21) SD 1.61 1.06 2.89 1.10 2.17 1.73 2.04 1.16
Values presented as no. patients (%) for each score given by a reviewer. Cumulative score 2.0 ( 0.06).
Table 4 Significance of Medical Error to Death
Cause of Death Average Score
Diffuse alveolar lung damage Hypovolemia/inadequate resuscitation Airway loss/aspiration Pneumonia Burn wound sepsis Anoxia Drug reaction
1.7 3.0 3.5 2.3 2.5 1.5 3.9
Cumulative score 2.4 ( 0.06). Scale: 1 0%15%; 2 16%50%; 3 51% 84%; 4 85%100%. -statistics for inter-rater agreement 0.7 considered significant.
Table 5 Inter-Rater Variability for Percent Chance that Error Caused Death
Reviewers Scores 1 2 3 4
1 2 3 4 Mean
51 (72) 16 (22) 29 (41) 25 (35) 5 (7) 12 (17) 1 (1) 17 (24) 7 (10) 7 (10) 5 (7) 8 (11) 8 (11) 36 (51) 36 (51) 21 (29) SD 1.61 1.06 2.89 1.26 2.37 1.83 2.35 1.24
ment as to the impact of error with a score of only 0.06. Another determination as to the significance of medical error was assessed by the reviewers as the percentage chance that the child would have survived had the error not occurred. Again scaled 1 to 4, reviewers assigned this an overall 2.0 score, meaning approximately one-third of all deaths could have been prevented had a deficiency in care not occurred (Table 6). Again inter-rater variability was high with a score of 0.06. Although there was a wide range of disagreement concerning the incidence and severity of medical error, this disparity of opinion did not seem to arise from differences as to the seriousness of an adverse event because the range of values that raters gave for significance of error was usually relatively narrow. In general, there were only systematic differences between raters. For example, rater 3 assessed the significance of error for pneumonia as 1 (i.e. no error) whereas the other reviewers typically gave ratings of 2 or 3. Rater 3 also assessed any deficiencies in care for burn wound sepsis as 1 in about half the cases, whereas the other reviewers almost universally assigned burn wound sepsis to a rating of 2 or 3. Reviewer 4 often rated the significance of medical error for anoxia as a 3 to 4 suggesting that in his opinion something could have been performed in the initial resuscitation to preserve brain function. In contrast, the other reviewers rated the significance of error for anoxia as a 1 or 2 indicative of their opinion as to the futility of any medical intervention to forego the anoxic brain death. Opinions also varied as to the significance of error with diffuse alveolar lung damage. For example, rater 2 consistently assigned a significance of error of 3 for children dying primarily from lung injury and thereby conveying his opinion that something might have been performed to forego pulmonary failure. Other reviewers consistently gave diffuse alveolar damage an error significance score of 1.
DISCUSSION
The overall mortality for this 10-year review was only 2.4%; far less than that reported from the national burn registry.7 As to be expected, there was a significantly greater extent of burn injury and a higher incidence of inhalation October 2007
Values presented as no. patients (%) for each score given by a reviewer. Cumulative score 2.3 ( 0.06).
816
Adverse Events in Burn Care
injury in those dying at our institution. However, the mean value for all deaths was a body surface area burn of only 66% and an incidence of inhalation injury of only 60%. Furthermore, 19 children died with burns of less than 50% body surface area of which only 8 were noted to have an inhalation injury. These values demonstrate that some deaths were the result of neither devastating skin nor lung damage. This shows that, regardless of the extent of burns, something other than the actual injury must have contributed to the demise of many of these children. One probable assumption would be that a deficit in care, either as an omission or delay in providing appropriate care or possibly inappropriate care, may be a factor in some deaths. In this review, experts in pediatric burn care identified lung damage as the most frequent cause of death in these injured children. In general, these reviewers thought that death from pulmonary failure, a consequence predominantly of either the initial smoke injury or as sequelae from sepsis, was largely not preventable. Conversely, these physician reviewers in aggregate considered hypovolemia or inadequate resuscitation as the second, and failure of airway control or aspiration as the third, most common cause of death. It was their opinion that such deaths were likely preventable. Death from infection, noted separately as pneumonia or burn wound sepsis, was also considered a frequent primary cause of death. Reviewers generally scaled these infectious deaths as potentially preventable, but with a varied opinion as to the responsibility of the medical community regarding infection control versus a feeling of pessimism for any intervention in an individual patient with severe sepsis. The main goal of this study was to categorize failures in the care of injured children and thereby provide a guide to direct future quality care initiatives and ultimately improve patient care and survival. One presumption is to focus on those failures deemed most preventable; for example, an educational initiative aimed at optimizing fluid resuscitation and airway control of a severely burned child. With the findings of this study demonstrating that hypovolemia and loss of airway, a common facet in the death of some children, such a quality assurance directive would intuitively be beneficial. However, an acutely burned child is relatively infrequent for even an experienced emergency room physician, thus any postevent education is unlikely to have much impact in the future care of burn children as a rarely repeated event.8 Likewise, pre-emptive education such as that provided by the Advanced Burn and Trauma Life Support courses designed to reduce errors in resuscitation and airway management may fail to have a prolonged impact with possibly many years preceding an occurrence. As an alternative to a traditional continuing medical education initiative, advances in information technology, such as telemedicine,9,10 may provide an avenue for improving the emergency care and transfer of burn victims by allowing closer, more timely interaction of a burn expert to the initial care of an injured child. A key aspect of any such interaction is the prompt contact from the initial Volume 63 Number 4 emergency room to the burn specialist and the ready availability of the technology. Furthermore, a concentrated effort at education and training for personnel dedicated to repeatedly providing safe transport would also likely be beneficial. Likewise, many physicians who work at a burn center are residents in training who lack experience in fluid resuscitation and airway intubation, especially for severely burned children. Emerging facilities such as the Human Patient Simulator11 may greatly aid in resident physician training by providing a manner for skills acquisition before such a physician is thrust into a life-or-death situation. In contrast to emergency resuscitation, death from pulmonary failure was generally considered nonpreventable. Yet, considering the prominent contribution of pulmonary damage to the demise of these patients, any improvements in this regard may have a substantial impact on outcome. However, considering health care negligence was not deemed to have a substantive influence regarding these respiratory deaths, therapeutic advances, not educational, quality assurance initiatives, are likely to be a more viable avenue for improving outcome from this cause of death. There was no significant agreement between reviewers as to either the cause of death or the relevance of medical error in the demise of these children, despite having both autopsy records and a summary of their clinical course. Such a discrepancy between well-trained experts in a clearly defined speciality of care in a single specialized hospital setting emphasizes the difficulty and subjectivity in deciding on those factors contributing to the death of these injured children. Much of this disparity resulted from our inability to distinguish the relative contribution to a childs demise from the initial injury versus any exacerbation of that injury related to an inadequate or delayed resuscitation or damage related to sepsis. Furthermore, because children have such an extensive physiologic reserve and the vast majority have excellent cardiac function, the progression through multiple organ failure to death was often prolonged. This common scenario of prolonged, multiorgan failure often precluded a clear interpretation of the exact inciting factor in the childs death. Autopsy findings did little to relieve this uncertainty because the postmortem examination almost universally showed a combination of extensive inflammatory damage within the lung, bacterial and fungal infiltration within the lungs (i.e. pneumonia), and infection or contamination within any residual wound. Thus, autopsies were not particularly helpful in identifying either a predisposing cause of death or any associated medical error. Because autopsies are known to disagree with the clinical diagnosis as much as 40% of the time,12,13 any study with the intent of determining the nature and preventability of death would be expected to have substantial error without inclusion of the autopsy findings. Yet, this disparity between the pre- and postmortem cause of death is largely evident in review of adult patients. Furthermore, this review of injured children circumvents any variable of a natural death rate because the vast majority of these burn 817
The Journal of TRAUMA Injury, Infection, and Critical Care
victims were in good health before their injury, which negates much of the uncertainty by a reviewer as to the influence of the disease process versus error in the demise of these children. Therefore, a finding of this study suggests that, at least in regard to injured children, accurate records of a childs clinical care, and not the autopsy, are of utmost importance in assessing any medical misadventures.
6. Spies M, Herndon DN, Rosenblatt JI, et al. Prediction of mortality from catastrophic burns in children. Lancet. 2003; 361:989 994. Saffle JR, Davis B, Williams P. Recent outcomes in the treatment of burn injury in the United States: a report from the American Burn Association Patient Registry. J Burn Care Rehabil. 1995; 16:219 232. Brigham PA, McLoughlin E. Burn incidence and medical care use in the United States: estimates, trends, and data sources. J Burn Care Rehabil. 1996;17:95107. Aucar J, Granchi T, Liscum K, et al. Is regionalization of trauma care using telemedicine feasible and desirable? Am J Surg. 2000; 180:535539. Tachakra S, Jaye P, Bak J, et al. Supervising trauma life support by telemedicine. J Telemed Telecare. 2000;6(Suppl 1):S7S11. Holcomb JB, Dumire RD, Crommett JW, et al. Evaluation of trauma team performance using an advanced human patient simulator for resuscitation training. J Trauma. 2002;52:1078 1086. Goldman L, Sayson R, Robbins S, et al. The value of the autopsy in three medical eras. N Engl J Med. 1983;308:1000 1005. Mort TC, Yeston NS. The relationship of premortem diagnoses and post mortem findings in a surgical intensive care unit. Crit Care Med. 1999;27:299 303.
7.
8.
REFERENCES
1. Muller MJ, Pegg SP, Rule MR. Determinants of death following burn injury. Br J Surg. 2001;88:583587. 2. Ryan CM, Schoenfeld DA, Thorpe WP, et al. Objective estimates of the probability of death from burn injuries. N Engl J Med. 1998; 338:362366. 3. Smith DL, Cairns BA, Ramadan F, et al. Effect of inhalation injury, burn size, and age on mortality: a study of 1447 consecutive burn patients. J Trauma. 1994;37:655 659. 4. Sheridan RL, Remensnyder JP, Schnitzer JJ, et al. Current expectations for survival in pediatric burns. Arch Pediatr Adolesc Med. 2000;154:245249. 5. Saffle JR. Predicting outcomes of burns. N Engl J Med. 1998; 338:387388.
9.
10. 11.
12. 13.
818
October 2007
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Patient Engagement: Technical Series On Safer Primary CareДокумент26 страницPatient Engagement: Technical Series On Safer Primary CareHndrОценок пока нет
- Soal Bahasa Inggris 2aДокумент19 страницSoal Bahasa Inggris 2aMegaaОценок пока нет
- 7 Steps Patient Safety PDFДокумент58 страниц7 Steps Patient Safety PDFDanissa Fidia PuteriОценок пока нет
- Executive SummaryДокумент22 страницыExecutive Summarysaleem kОценок пока нет
- HSOPSC User Comparative DatabaseДокумент80 страницHSOPSC User Comparative DatabaseBaiq KartikasariОценок пока нет
- The Risk Management of Medical Device-Related Pressure Ulcers Based On The Australian/ New Zealand StandardДокумент11 страницThe Risk Management of Medical Device-Related Pressure Ulcers Based On The Australian/ New Zealand StandardJugurtha BoutlikhetОценок пока нет
- Fran Bruscia CVДокумент5 страницFran Bruscia CVAR GameCenterОценок пока нет
- Sohn - PT - Rights To Freedom From HarmДокумент15 страницSohn - PT - Rights To Freedom From HarmEnohoj YamОценок пока нет
- Workarounds To Barcode Medication Administration Systems-Their Occurrences, Causes, and Threats To Patient SafetyДокумент16 страницWorkarounds To Barcode Medication Administration Systems-Their Occurrences, Causes, and Threats To Patient SafetyAlex PiecesОценок пока нет
- 13 ElectronicHealthRecordДокумент48 страниц13 ElectronicHealthRecordkimchi girl100% (1)
- 001 RCA FlipchartДокумент40 страниц001 RCA FlipchartAbd ZouhierОценок пока нет
- TriageДокумент95 страницTriageEduardo FriasОценок пока нет
- Gambaran Personal Higiene Dan Keadaan Sanitasi Industri Tempe Ud Andika Panguripan Di Desa Tagtag Kaja Kecamatan Denpasar Utara TAHUN 2019Документ6 страницGambaran Personal Higiene Dan Keadaan Sanitasi Industri Tempe Ud Andika Panguripan Di Desa Tagtag Kaja Kecamatan Denpasar Utara TAHUN 2019Ausi PalsuОценок пока нет
- Standardized Color-Coding Solution Labeling in The Operating RoomДокумент3 страницыStandardized Color-Coding Solution Labeling in The Operating Roomcumar cabdicazizОценок пока нет
- Leadership in NursingДокумент14 страницLeadership in NursingzainuddinОценок пока нет
- Akreditasi) - Keselamatan Pasien Tidak Hanya Diterapkan Di Rumah Sakit NamunДокумент15 страницAkreditasi) - Keselamatan Pasien Tidak Hanya Diterapkan Di Rumah Sakit Namunria kartini panjaitanОценок пока нет
- NURS FPX 6212 Assessment 1 Quality and Safety Gap AnalysisДокумент5 страницNURS FPX 6212 Assessment 1 Quality and Safety Gap Analysisfarwaamjad771Оценок пока нет
- Artificial Intelligence in Medicine: David D. LuxtonДокумент10 страницArtificial Intelligence in Medicine: David D. LuxtonGerman ArleyОценок пока нет
- 12.gittell, Jody Hoffer, and Rob Seidner. Human Resource Management in The Service SectorДокумент13 страниц12.gittell, Jody Hoffer, and Rob Seidner. Human Resource Management in The Service SectormiudorinaОценок пока нет
- Pio KoreaДокумент5 страницPio KoreaKey Nie MayrindaОценок пока нет
- Cpdprogram Nursing 81718Документ301 страницаCpdprogram Nursing 81718PRC BoardОценок пока нет
- 97084d9df084bad346c916e86a3f75abДокумент8 страниц97084d9df084bad346c916e86a3f75abDio HapyansyahОценок пока нет
- Rca KarsДокумент75 страницRca KarsAnonymous 12i1wlaALОценок пока нет
- Global Patient Safety Action Plan 2021-2030Документ108 страницGlobal Patient Safety Action Plan 2021-2030Leia MendesОценок пока нет
- Nursing LeadershipДокумент15 страницNursing LeadershipRolando PinchettiОценок пока нет
- How-To Guide: Prevent Adverse Drug Events by Implementing Medication ReconciliationДокумент40 страницHow-To Guide: Prevent Adverse Drug Events by Implementing Medication ReconciliationJorge Arturo Porras BermúdezОценок пока нет
- DR - Sumitra - Quality in Healthcare and AccreditationДокумент27 страницDR - Sumitra - Quality in Healthcare and AccreditationTejaswe Korivi67% (3)
- Clinical Nursing JudgementДокумент6 страницClinical Nursing Judgementapi-541153916Оценок пока нет
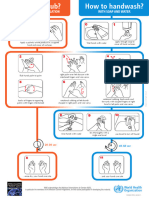
- Handwash and HandrubДокумент1 страницаHandwash and HandrubMohamed Ali RekikОценок пока нет
- Nurs FPX 4010 Assessment 1 Collaboration and Leadership Reflection VideoДокумент8 страницNurs FPX 4010 Assessment 1 Collaboration and Leadership Reflection Videozadem5266Оценок пока нет