Академический Документы
Профессиональный Документы
Культура Документы
Stroke Handout
Загружено:
Adebayo Tob AdeyinkaИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Stroke Handout
Загружено:
Adebayo Tob AdeyinkaАвторское право:
Доступные форматы
HANDLING A STROKE PATIENT
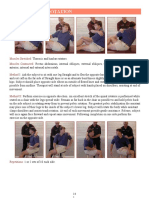
The most common type of stroke is an ischaemic stroke, which happens when a clot blocks an artery that carries blood to the brain. The second type of stroke is a bleed, when a blood vessel bursts, causing bleeding into the brain. This is called a hemorrhagic stroke. Weakness or paralysis (hemiplegia) is one of the most recognisable and most common symptoms of a stroke. It usually happens on one side of the body. Weakness or paralysis of an arm or leg is often made worse by stiffness (spasticity) of the muscles and joints. Loss of balance can be caused by damage to the cerebellum. Or it may happen because of paralysis resulting in muscle weakness and loss of coordination. Many people also experience problems with speaking and understanding, and with reading and writing. This difficulty with language is called dysphasia. All of these things have an impact on how we handle patients. Decreased muscle tone is often associated with weakness and paralysis and if patients are not handled correctly damage can be caused to joints, particularly of the upper limb. Loss of strength and balance in one side will affect the patients mobility, consequently making handling more difficult and presenting more risks. Communication difficulties also present challenges when handling a patient and trying to help them with rehabilitation. POSITIONING OF STROKE PATIENTS
Lying on the affected side
Lying on the unaffected side
University of Surrey Moving and Handling 2006
Lying on back
Sitting up in bed
Sitting up in chair In each position the patient is well supported with pillows in a good posture to avoid straining joints prevent increased muscle tone. Furniture should be positioned on the affected side of the patient to encourage them to use this side. The side that the stroke affects is often neglected and part of the rehabilitation process is to make them use that side. SHOULDER CARE Shoulder problems affect 70% of all stroke sufferers. The affected arm initially needs to be well supported on a pillow, as gravity acting on the weight of the arm can dislocate the shoulder joint. Stroke patients should never be pulled, however gently, by the arm. A physiotherapist will then work to restore normal movement and postural control. Some people can feel a gap at the shoulder joint (known as subluxation). This does not mean that the shoulder is dislocated, but it is a warning sign that the joint is not
University of Surrey Moving and Handling 2006
supported properly by the muscles. There is a risk that the soft tissue around the joint can become impinged, causing inflammation, pain
Subluxation is when the head of the humerus slips out of the glenoid socket. Cause of shoulder problems due to incorrect handling: a) Lifting distally when dressing b) Drag lift c) Pulling back in chair incorrectly d) Pulling arm as a guide when walking and supporting e) Nursing supine (on back) increased reflex activity
GOLDEN RULES FOR STROKE
1. Lie patient on their back only for short periods of time. Laying them on their side is preferable. 2. Never touch balls of the feet of toe pads as it can increase extensor tone. 3. Meals to be taken out of bed and not in a semi-recumbent position. 4. Always support affected arm in extension in chair. 5. Keep patient aware of affected side i.e. locker and chair on affected side. 6. Approach patient on affected side after the first few days. 7. Dont label patients as lazy when they forget how to do something like dressing as it could be apraxia 8. Mobilise shoulder with humerus in external rotation and scapula protracted. 9. Move the arm by supporting the whole forearm and shoulder not just the hand. 10. Early appropriate handling and positioning facilitates recovery.
REFLEXES
When we are born our bodies tend to function reflexly e.g. pretend to drop a baby and it will elicit a startle reflex; put a finger in palm of babys hand and it will grip/grasp. We soon learn to do things voluntarily and the reflex is lost i.e. it is controlled by the higher centres in the brain (cortical control is developed). After a CVA the cortical control is often lost and the reflex comes to the fore again.
University of Surrey Moving and Handling 2006
Labarinthe reflex: Brought about by changes in head position in space. if nursed supine leads to increased extensor tone in leg in prone to increased flexor tone if extensor tone ++ then appears as reduction only (relative) if sitting for long time flexed, head extended to see then increased tone in lower leg and slipping forward off chair - bent head during sitting causes reduced extension and collapse into seat Symmetrical tonic neck reflexes: To maintain balance and equilibrium. semi recumbent supine in bed/ chair causes increased tone in leg extensors and arm flexors patient has difficulty getting from lying to sitting because he has to raise his head if walks with head down then increased extensor tone in leg and flexor in arm. transferring bed to wheelchair increases extensor tone in leg and flexors in arm if he looks up increases extension in arm and flexion in leg.
Asymmetrical tonic neck reflexes: - if you turn head to the right, arm and leg on that side increase extensor tone - babies use this to fixate and grasp things - if patient turns head away from affected side it increases the tone - if standing and walking delayed, flexor tone increases in affected leg even when lying. Positive supporting reflex - exteroceptive stimulus to skin on toe pads and ball of foot stimulated increased extensor tone eg babies precursor to walking. - Never touch ball of foot leads to increased extensor tone, leg rigid, knee hyperextended, cannot put heel to floor or release hip and knee to bring leg forward and cannot swing weight forward over foot. Crossed Extensor reflex: increased extensor tone in one leg when other is flexed precursor to walking and crawling. lying supine patient unable to bridge unaided bends sound leg then affected leg has increased tone. Patient allowed to stand from sitting with weight over sound leg, then unable to weight bear because affected leg has increased flexor tone.
University of Surrey Moving and Handling 2006
University of Surrey Moving and Handling 2006
Вам также может понравиться
- Tips for Everyday Life and Sports With an Artificial Joint: Expert guidebook for dealing with a prosthesis for patients with a new hip or knee jointОт EverandTips for Everyday Life and Sports With an Artificial Joint: Expert guidebook for dealing with a prosthesis for patients with a new hip or knee jointОценок пока нет
- Exo Kinetics Explosive Performance and Training PrimerДокумент17 страницExo Kinetics Explosive Performance and Training PrimerHari SetiawanОценок пока нет
- Snapping Hip Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandSnapping Hip Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Neurology NotesДокумент3 страницыNeurology Notesdlynne23Оценок пока нет
- Lumbar Spondylolisthesis PDFДокумент6 страницLumbar Spondylolisthesis PDFghidecmaria0% (1)
- Healthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesОт EverandHealthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesРейтинг: 2 из 5 звезд2/5 (1)
- Lower Crossed SyndromeДокумент8 страницLower Crossed SyndromeThaseen75% (4)
- Anterior Shoulder Dislocation, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandAnterior Shoulder Dislocation, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- NeckДокумент6 страницNeckBéla JózsiОценок пока нет
- HemiplegiaДокумент11 страницHemiplegiaFares EL DeenОценок пока нет
- Bad Posture - A Reason For Change in SpinalДокумент58 страницBad Posture - A Reason For Change in SpinalPooja jainОценок пока нет
- Shoulder Range of Motion Exercises PDFДокумент4 страницыShoulder Range of Motion Exercises PDFGade JyОценок пока нет
- Mobility & ImmobilityДокумент85 страницMobility & Immobilityanumaria100% (5)
- SPASTIC QUADRIPLEGIA CEREBRAL PALSY OldДокумент26 страницSPASTIC QUADRIPLEGIA CEREBRAL PALSY OldsanalcrazyОценок пока нет
- Scapular Ax in NeuroДокумент6 страницScapular Ax in NeurolavanyaphdОценок пока нет
- Lower Crossed SyndromeДокумент11 страницLower Crossed SyndromeJúnior Alvacir Camargo50% (2)
- Skills 116 Finals ROM Assistive Devices PDFДокумент64 страницыSkills 116 Finals ROM Assistive Devices PDFMae Arra Gilbao Lecobu-anОценок пока нет
- LECT 8 Relieving The Discomforts of Pregnancy Part 1Документ27 страницLECT 8 Relieving The Discomforts of Pregnancy Part 1Umer RafiqОценок пока нет
- Spondylolysis SpondylolisthesisДокумент89 страницSpondylolysis SpondylolisthesisAh ZhangОценок пока нет
- Kinesiology 3 2Документ16 страницKinesiology 3 2Marianne GasmenОценок пока нет
- Hip Flexors - The Iliopsoas - Tightness or WeaknessДокумент4 страницыHip Flexors - The Iliopsoas - Tightness or Weaknessatpicker100% (1)
- Rotator Cuff TendinitisДокумент23 страницыRotator Cuff TendinitisVrushali NikamОценок пока нет
- J. Everette Backcare Certification Mid-Term Exam 2020 KH CommentsДокумент10 страницJ. Everette Backcare Certification Mid-Term Exam 2020 KH CommentsIiam JamesОценок пока нет
- Normal Tone & Abnormal Tone - Handling TechniquesДокумент2 страницыNormal Tone & Abnormal Tone - Handling TechniquesWasemBhatОценок пока нет
- Active Isolated Stretching The Mattes Method 151 184Документ38 страницActive Isolated Stretching The Mattes Method 151 184Nazareth Varas AlonsoОценок пока нет
- Positioning 2018studentДокумент33 страницыPositioning 2018studentRay Morgan Sport and FitnessОценок пока нет
- Frozen Shoulder: By: Denise Dela CruzДокумент44 страницыFrozen Shoulder: By: Denise Dela CruzDenise De la Cruz100% (1)
- Rehab of Patients With HemiplegiaДокумент2 страницыRehab of Patients With HemiplegiaMilijana D. DelevićОценок пока нет
- Discharge Planning InstructionsДокумент3 страницыDischarge Planning Instructionsad3_aaaОценок пока нет
- Range of MotionДокумент59 страницRange of MotionIsrael Jiel Fedelicio100% (1)
- Scoliosis: Futhri Rifa Zaimsyah, S.TR - FT., M.PhysioДокумент42 страницыScoliosis: Futhri Rifa Zaimsyah, S.TR - FT., M.PhysioMaria Rosma CemaОценок пока нет
- GeriatricsДокумент14 страницGeriatricsParul ThakurОценок пока нет
- Assesment of Cerebeller Function 30-04-2020Документ9 страницAssesment of Cerebeller Function 30-04-2020Harshit SharmaОценок пока нет
- Lumbar ExaminationДокумент19 страницLumbar ExaminationGavin TessierОценок пока нет
- Neuroo 170210095341 PDFДокумент162 страницыNeuroo 170210095341 PDFmalathiОценок пока нет
- Elbow PT AssessmentДокумент31 страницаElbow PT Assessmentkrissh20Оценок пока нет
- Gait and Posture AnalysisДокумент6 страницGait and Posture Analysisapi-545717294Оценок пока нет
- Figure FaultsДокумент17 страницFigure FaultsMichael SimpsonОценок пока нет
- Pilates Pentru Spate CifoticДокумент15 страницPilates Pentru Spate Cifoticcristinaradu13Оценок пока нет
- Positioning and Its ImportanceДокумент22 страницыPositioning and Its ImportanceDeepika PatidarОценок пока нет
- Shoulder Impinge MentДокумент26 страницShoulder Impinge MentkotraeОценок пока нет
- Management of Motor Disorders in Children With Cerebral PalsyДокумент56 страницManagement of Motor Disorders in Children With Cerebral PalsyAnnie KhanОценок пока нет
- Musculoskeletal SystemДокумент160 страницMusculoskeletal SystemAirene Aquino BusaniaОценок пока нет
- Impaired Physical Mobility NCPДокумент3 страницыImpaired Physical Mobility NCPYan ReyesОценок пока нет
- Neurological History and ExaminationДокумент30 страницNeurological History and ExaminationMaria Agatha100% (1)
- PostureДокумент85 страницPostureDr.Debanjan Mondal (pt)100% (1)
- Biomechanics of SpineДокумент41 страницаBiomechanics of SpineMuhammad MustaqeemОценок пока нет
- Advanced Anatomy 2nd. Ed.: Body MovementsДокумент23 страницыAdvanced Anatomy 2nd. Ed.: Body Movementseyob yirsaw basaznewОценок пока нет
- Abero, Richervin P. Bs Architecture Ii-A 1.health Health Is "A State of Complete Physical, Mental, and Social Well-Being and Not Merely TheДокумент5 страницAbero, Richervin P. Bs Architecture Ii-A 1.health Health Is "A State of Complete Physical, Mental, and Social Well-Being and Not Merely TheluffyОценок пока нет
- Effects of A StrokeДокумент13 страницEffects of A Strokeاحمد ناصرОценок пока нет
- Impaired Physical MobilityДокумент3 страницыImpaired Physical MobilityCalimlim Kim100% (1)
- Spastic Quadriplegia Cerebral PalsyДокумент25 страницSpastic Quadriplegia Cerebral PalsysanalcrazyОценок пока нет
- GALS Screen: G Gait A Arms L Legs S SpineДокумент6 страницGALS Screen: G Gait A Arms L Legs S SpineJoseph FreerОценок пока нет
- Transfer and AmbulationДокумент108 страницTransfer and AmbulationGladys YaresОценок пока нет
- AthetoidДокумент3 страницыAthetoidNamrah AfzalОценок пока нет
- Shoulder Dislocation Background: Shoulder Dislocations Traumatic InjuryДокумент7 страницShoulder Dislocation Background: Shoulder Dislocations Traumatic Injuryanastasiaanggita_265Оценок пока нет
- What You Should Know About Shoulder InstabilityДокумент4 страницыWhat You Should Know About Shoulder InstabilityWoo Guan Lee100% (1)
- Brunnstrom ApproachДокумент9 страницBrunnstrom ApproachavtordajОценок пока нет
- Yoga For Posture - IntrotalkДокумент5 страницYoga For Posture - IntrotalkRavi OnkariОценок пока нет
- Islamic Meditation (Full) PDFДокумент10 страницIslamic Meditation (Full) PDFIslamicfaith Introspection0% (1)
- SUBSET-026-7 v230 - 060224Документ62 страницыSUBSET-026-7 v230 - 060224David WoodhouseОценок пока нет
- Maths Lowersixth ExamsДокумент2 страницыMaths Lowersixth ExamsAlphonsius WongОценок пока нет
- Kurukku PadaiДокумент4 страницыKurukku PadaisimranОценок пока нет
- 011 - Descriptive Writing - UpdatedДокумент39 страниц011 - Descriptive Writing - UpdatedLeroy ChengОценок пока нет
- STAFFINGДокумент6 страницSTAFFINGSaloni AgrawalОценок пока нет
- Module 3 - Lesson 3.1Документ2 страницыModule 3 - Lesson 3.1Cj RomoОценок пока нет
- The New Definition and Classification of Seizures and EpilepsyДокумент16 страницThe New Definition and Classification of Seizures and EpilepsynadiafyОценок пока нет
- Dispersion Compensation FibreДокумент16 страницDispersion Compensation FibreGyana Ranjan MatiОценок пока нет
- Spiritual Transcendence in Transhumanism PDFДокумент10 страницSpiritual Transcendence in Transhumanism PDFZeljko SaricОценок пока нет
- Rem - Manila Bankers Vs NG Kok Wei - Noel DomingoДокумент3 страницыRem - Manila Bankers Vs NG Kok Wei - Noel DomingoNoel DomingoОценок пока нет
- Why Do Firms Do Basic Research With Their Own Money - 1989 - StudentsДокумент10 страницWhy Do Firms Do Basic Research With Their Own Money - 1989 - StudentsAlvaro Rodríguez RojasОценок пока нет
- MAT2355 Final 2002Документ8 страницMAT2355 Final 2002bojie_97965Оценок пока нет
- Thesis FulltextДокумент281 страницаThesis FulltextEvgenia MakantasiОценок пока нет
- 2009 Annual Report - NSCBДокумент54 страницы2009 Annual Report - NSCBgracegganaОценок пока нет
- Druze ScriptureДокумент15 страницDruze ScriptureChristopher DeMott100% (2)
- Annexure 8: Medical Certificate (To Be Issued by A Registered Medical Practitioner) General ExpectationsДокумент1 страницаAnnexure 8: Medical Certificate (To Be Issued by A Registered Medical Practitioner) General ExpectationsMannepalli RamakrishnaОценок пока нет
- A Teacher Must Choose Five Monitors From A Class of 12 Students. How Many Different Ways Can The Teacher Choose The Monitors?Документ11 страницA Teacher Must Choose Five Monitors From A Class of 12 Students. How Many Different Ways Can The Teacher Choose The Monitors?Syed Ali HaiderОценок пока нет
- ID2b8b72671-2013 Apush Exam Answer KeyДокумент2 страницыID2b8b72671-2013 Apush Exam Answer KeyAnonymous ajlhvocОценок пока нет
- War Thesis StatementsДокумент8 страницWar Thesis StatementsHelpPaperRochester100% (2)
- WO 2021/158698 Al: (10) International Publication NumberДокумент234 страницыWO 2021/158698 Al: (10) International Publication Numberyoganayagi209Оценок пока нет
- Ideal Weight ChartДокумент4 страницыIdeal Weight ChartMarvin Osmar Estrada JuarezОценок пока нет
- Lesson Plan Pumpkin Moon SandДокумент3 страницыLesson Plan Pumpkin Moon Sandapi-273177086Оценок пока нет
- Concentrating Partial Entanglement by Local OperationsДокумент21 страницаConcentrating Partial Entanglement by Local OperationsbhpliaoОценок пока нет
- Applied Nutrition: Nutritional Consideration in The Prevention and Management of Renal Disease - VIIДокумент28 страницApplied Nutrition: Nutritional Consideration in The Prevention and Management of Renal Disease - VIIHira KhanОценок пока нет
- SHS11Q4DLP 21st CentFinalДокумент33 страницыSHS11Q4DLP 21st CentFinalNOEMI DE CASTROОценок пока нет
- Espinosa - 2016 - Martín Ramírez at The Menil CollectionДокумент3 страницыEspinosa - 2016 - Martín Ramírez at The Menil CollectionVíctor M. EspinosaОценок пока нет
- 01ESS - Introducing Siebel ApplicationsДокумент24 страницы01ESS - Introducing Siebel ApplicationsRajaОценок пока нет
- Goal Ball Lesson PlanДокумент4 страницыGoal Ball Lesson Planapi-378557749100% (1)
- Predictive Tools For AccuracyДокумент19 страницPredictive Tools For AccuracyVinod Kumar Choudhry93% (15)
- Peak: The New Science of Athletic Performance That is Revolutionizing SportsОт EverandPeak: The New Science of Athletic Performance That is Revolutionizing SportsРейтинг: 5 из 5 звезд5/5 (97)
- Power of 10: The Once-A-Week Slow Motion Fitness RevolutionОт EverandPower of 10: The Once-A-Week Slow Motion Fitness RevolutionРейтинг: 3.5 из 5 звезд3.5/5 (11)
- The Yogi Code: Seven Universal Laws of Infinite SuccessОт EverandThe Yogi Code: Seven Universal Laws of Infinite SuccessРейтинг: 4.5 из 5 звезд4.5/5 (104)
- Chair Yoga: Sit, Stretch, and Strengthen Your Way to a Happier, Healthier YouОт EverandChair Yoga: Sit, Stretch, and Strengthen Your Way to a Happier, Healthier YouРейтинг: 3.5 из 5 звезд3.5/5 (5)
- Aging Backwards: Reverse the Aging Process and Look 10 Years Younger in 30 Minutes a DayОт EverandAging Backwards: Reverse the Aging Process and Look 10 Years Younger in 30 Minutes a DayОценок пока нет
- Functional Training and Beyond: Building the Ultimate Superfunctional Body and MindОт EverandFunctional Training and Beyond: Building the Ultimate Superfunctional Body and MindРейтинг: 4.5 из 5 звезд4.5/5 (1)
- Muscle for Life: Get Lean, Strong, and Healthy at Any Age!От EverandMuscle for Life: Get Lean, Strong, and Healthy at Any Age!Рейтинг: 4.5 из 5 звезд4.5/5 (22)
- Strength Training Over 40: The Only Weight Training Workout Book You Will Need to Maintain or Build Your Strength, Muscle Mass, Energy, Overall Fitness and Stay Healthy Without Living in the GymОт EverandStrength Training Over 40: The Only Weight Training Workout Book You Will Need to Maintain or Build Your Strength, Muscle Mass, Energy, Overall Fitness and Stay Healthy Without Living in the GymРейтинг: 4 из 5 звезд4/5 (6)
- Which Comes First, Cardio or Weights?: Fitness Myths, Training Truths, and Other Surprising Discoveries from the Science of ExerciseОт EverandWhich Comes First, Cardio or Weights?: Fitness Myths, Training Truths, and Other Surprising Discoveries from the Science of ExerciseРейтинг: 4 из 5 звезд4/5 (47)
- Boundless: Upgrade Your Brain, Optimize Your Body & Defy AgingОт EverandBoundless: Upgrade Your Brain, Optimize Your Body & Defy AgingРейтинг: 4.5 из 5 звезд4.5/5 (67)
- Strong Is the New Beautiful: Embrace Your Natural Beauty, Eat Clean, and Harness Your PowerОт EverandStrong Is the New Beautiful: Embrace Your Natural Beauty, Eat Clean, and Harness Your PowerРейтинг: 4 из 5 звезд4/5 (5)
- True Yoga: Practicing With the Yoga Sutras for Happiness & Spiritual FulfillmentОт EverandTrue Yoga: Practicing With the Yoga Sutras for Happiness & Spiritual FulfillmentРейтинг: 4.5 из 5 звезд4.5/5 (22)
- Music For Healing: With Nature Sounds For Natural Healing Powers: Sounds Of Nature, Deep Sleep Music, Meditation, Relaxation, Healing MusicОт EverandMusic For Healing: With Nature Sounds For Natural Healing Powers: Sounds Of Nature, Deep Sleep Music, Meditation, Relaxation, Healing MusicРейтинг: 5 из 5 звезд5/5 (1)
- Wheels of Life: A User's Guide to the Chakra SystemОт EverandWheels of Life: A User's Guide to the Chakra SystemРейтинг: 4.5 из 5 звезд4.5/5 (34)
- Yin Yoga: How to Enhance Your Modern Yoga Practice With Yin Yoga to Achieve an Optimal Mind-Body Connection: Yoga Mastery SeriesОт EverandYin Yoga: How to Enhance Your Modern Yoga Practice With Yin Yoga to Achieve an Optimal Mind-Body Connection: Yoga Mastery SeriesОценок пока нет
- Fascial Training: With Easy Exercises To More Mobility And Less Pain (10 Minutes Fascia Workout For Home)От EverandFascial Training: With Easy Exercises To More Mobility And Less Pain (10 Minutes Fascia Workout For Home)Рейтинг: 5 из 5 звезд5/5 (3)
- The Power of Fastercise: Using the New Science of Signaling Exercise to Get Surprisingly Fit in Just a Few Minutes a DayОт EverandThe Power of Fastercise: Using the New Science of Signaling Exercise to Get Surprisingly Fit in Just a Few Minutes a DayРейтинг: 4 из 5 звезд4/5 (4)
- Not a Diet Book: Take Control. Gain Confidence. Change Your Life.От EverandNot a Diet Book: Take Control. Gain Confidence. Change Your Life.Рейтинг: 4.5 из 5 звезд4.5/5 (128)
- 5-Minute Yoga: A More Energetic, Focused, and Balanced You in Just 5 Minutes a DayОт Everand5-Minute Yoga: A More Energetic, Focused, and Balanced You in Just 5 Minutes a DayРейтинг: 5 из 5 звезд5/5 (2)
- Not a Diet Book: Take Control. Gain Confidence. Change Your Life.От EverandNot a Diet Book: Take Control. Gain Confidence. Change Your Life.Рейтинг: 3.5 из 5 звезд3.5/5 (7)
- Tibetan Yoga: Magical Movements of Body, Breath, and MindОт EverandTibetan Yoga: Magical Movements of Body, Breath, and MindРейтинг: 5 из 5 звезд5/5 (1)
- Enter The Kettlebell!: Strength Secret of the Soviet SupermenОт EverandEnter The Kettlebell!: Strength Secret of the Soviet SupermenРейтинг: 4 из 5 звезд4/5 (29)
- Mind Your Body: 4 Weeks to a Leaner, Healthier LifeОт EverandMind Your Body: 4 Weeks to a Leaner, Healthier LifeРейтинг: 4.5 из 5 звезд4.5/5 (5)
- Somatic Exercises for Beginners: Transform Your Life in 30 Days with Personalized Exercises for Body and MindОт EverandSomatic Exercises for Beginners: Transform Your Life in 30 Days with Personalized Exercises for Body and MindОценок пока нет
- Roxane Gay & Everand Originals: Built for This: The Quiet Strength of PowerliftingОт EverandRoxane Gay & Everand Originals: Built for This: The Quiet Strength of PowerliftingРейтинг: 4.5 из 5 звезд4.5/5 (133)
- Super Joints: Russian Longevity Secrets for Pain-Free Movement,От EverandSuper Joints: Russian Longevity Secrets for Pain-Free Movement,Рейтинг: 4.5 из 5 звезд4.5/5 (13)