Академический Документы
Профессиональный Документы
Культура Документы
Chapter 6
Загружено:
Kate Wen GuanИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Chapter 6
Загружено:
Kate Wen GuanАвторское право:
Доступные форматы
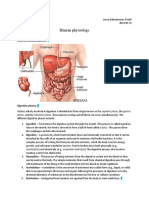
CHAPTER 6: DIGESTION AND NUTRITION
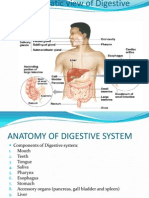
6.1 Organs and Organ Systems
o o Organs: groups of different tissues (acting together) specialized for particular functions. Example: stomach (complex organ). Outer structure epithelial tissue 3 layers of smooth muscle in different directions (to churn food with muscle contractions and relaxations) submucosa (loose connective tissue w/ blood/lymph vessels) innermost mucosa cells secreting gastric juices + mucus. Nerve cells regulate + synchronize contractions release partially digested material small intestine. Organ system: group of organs w/ related functions. Example: digestive system: esophagus, stomach, small intestine, large intestine, other organs (liver and pancreas). Interacting with each other. Example: digestive system + circulatory system (allows material transportation) + respiratory system (adequate gas exchange). Some organs classified for anatomy over function. Example: kidneys (excretory- waste removal in blood) + large intestine (digestive- concentrates + stores undigested matter, absorbs water + vitamins)
o o o
Monitoring Organs 1895: first X-ray photograph: German physicist Wilhelm Roentgen. High energy electromagnetic waves pass through soft tissue (muscle), absorbed by denser bone. 1898: first X-rays of soft tissue (viewed without surgery): Walter Cannon developed stain w/ bismuth (nontoxic mineral opaque to X rays). Patient drank it, X rays unable to penetrate stained gastrointestinal organs = white image of organs. Today barium instead of bismuth. X Ray technology + computer technology. Example: computerized axial tomography (CAT) scan: X ray machine rotates around patient 100s of pictures from different angles. Images stored in computer w/ location and angle. Pictures reassembled thin cross-sectional views, organized for 3 d imaging. Organ viewed section by section. Accuracy: can detect 1 mm abrasions. Can distinguish between gases, liquids, solid tissues can identify tumours. Useful diagnostic tool head injuries (e.g. blood clots)
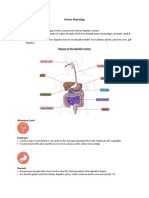
6.2 Importance of Digestion
1) INGESTION: heterotrophs take in organic compounds/nutrients 2) DIGESTION: the digestive system (coordinated, regulated by nervous and endocrine systems) breakdown of large, complex organic materials smaller components. E.g. gastrointestinal tract 3) ABSORPTION: transported by circulatory system cells supply energy, raw materials synthesis of essential chemical compounds growth, maintenance, tissue repair. E.g. oxygen + others digestive organs, absorbed foods tissues. 4) EGESTION: removal of wastes from the body. Digestive Enzymes Rate at which an enzyme functions best to break down complex molecules 2 factors: temperature, and pH -
Usually, temp + = energy + = enzyme activity + Most human enzymes: efficiency peaks at 37 degs, drops as more energy is added. * enzymes = proteins when w/ high temp, change shape denatured = no longer active Enzymes function best within certain pH ranges. E.g. Pepsin = low pH (acidic environment of stomach). Amylase = neutral pH (mouth), Trypsin = basic environments (small intestine) Digestion in Simpler Organisms Protozoa: digest meals inside food vacuoles in cells Amoeba: single celled: engulfs food w/ phagocytosis: extends pseudopods to engulf food, vacuole formed inside cell. Vacuoles fuse w/ lysosome: vesicles containing hydrolytic enzymes: use water molecules to break down food. Hydra: digestive sac (gastrovascular cavity) w/ single opening. Encloses part of external environment, allows food storage and digestion. Digestive enzymes released, break down larger food molecules. Smaller molecules engulfed by cells lining cavity. Digestion continues in cytoplasm. Wastes remain, expelled from same opening. Digestion in More Complex Organisms Digestive tracts/ alimentary canals long tubes with 2 openings (mouth, anus) Moves along 1 direction Specialized regions: breakdown + absorption: stepwise process Food ingested through mouth muscular pharynx esophagus stomach/crop (depends on species) Animals w/o teeth have muscular gizzard(designed to break down food particles) intestine hydrolytic enzymes complete chemical digestion nutrients absorbed across lining of intestine into blood circulatory system cells of the body undigested wastes removed through anus. -
6.3 Ingestion
Saliva watery fluid produced by salivary glands amylase enzymes breaks down starches (complex carbohydrates) simpler lubricates food to be swallowed, dissolves food particles, makes it possible to taste Flavour: food particles dissolved in solution penetrate cells of taste buds on tongue and cheeks. Different types of receptors: special geometry: permit I.D. of flavours. Nerve cells for tastes stimulated receptor sites filled by chemical compounds w/ complementary shape. Digestive tract of humans (6.5 m to 9 m long) stores and breaks down organic molecules simpler components.
Teeth physical digestion incisors: 8 chisel shaped teeth at front: for cutting canine teeth: sharp, dagger-shaped, for tearing premolars: broad, flattened teeth, for grinding molars: broader, flattened cusps, for crushing wisdom teeth: 16-20 years of age. Often must be removed. 2 divisions: root and crown. Enamel crown (covers tooth w/ calcium compounds hardest substance in body). Inside Dentin (bonelike substance), part of root structure. Encases: pulp cavity (containing nerves and blood vessels) Tooth decay: bacteria living off nutrients that cling to teeth. Harmful microbes corrosive acids that erode tooths structure. Infections can spread to periodontal membrane anchors teeth to jawbone. Periodontal tissue can be destroyed, teeth loosen. Esophagus -
Food mouth stomach Bolus of food stretches walls, activates smooth muscles peristalsis (involuntary rhythmic contractions): moves food along gastrointestinal tract. Only times voluntary swallowing and egestion
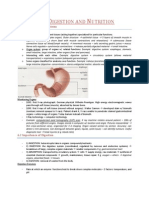
6.4 The Stomach and Digestion
Stomach: site of food storage, initial protein digestion Sphincters: constrictor muscles, surround a tubelike structure: regulate food going in and out Example: Cardiac sphincter contractions/relaxations - opening to the stomach near heart Example: Pyloric Sphincter: movement of foods and stomach acids to small intestine J-shaped stomach: numerous ridges (expansion) can store 1.5L of food. Millions of cells line inner wall, secreting stomach fluids gastric fluids/gastric juice digestion. 1) Mucus: protective coating: protein produced by layer of epithelial cells (mucus membrane) 2) Hydrochloric Acid (HCl): kills harmful substances in food, converts 3) Pepsinogen (moves through cell membrane and mucous lining) into active form Pepsin (protein digesting enzyme) breaks long amino acid chains shorter chains (polypeptides) pH range: usually 2-3, but possibly: 1.0. High acidity allows HCl to kill pathogens + pepsin to break proteins. Alkaline mucus layer protects stomach lining.
Ulcers
Peptic ulcer (lesion): from destruction of the cell membrane by HCl and pepsin after protective mucous lining breaks down. Under thin layer of cells = rich capillary network. Acids irritate cells of stomach lining = increase in blood flow and acid secretions = more tissue burned = allergic reaction stronger = eventually blood vessels breakdown. Most linked to Heliobacter pylori bacterium. Other factors: diet, stress. Dr. Barry Marshall: Australian physician changed minds. Before: believed microbes unable to live in stomach. H. pylori can survive in harsh environment, only powerful antibiotics can kill. Research in U.S.: attempting to connect it with stomach cancer. Now: simple breath test for presence of H. pylori Frontiers of Technology: Ulcers and Lasers 1960: American physicist: Theodore Maiman: 1 laser. Medical applications: remove damaged tissues (stomach ulcers). Laser beam thinner than most scalpels, can seal small blood vessels. Reduces need for surgery. Endoscope : instrument fitted with light-emitting glass fibre positioned inside patients body. Can be used to view inside body. Tiny forceps, fitted in, extracts small pieces of tissue for biopsy.
st
6.5 The Small Intestine and Pancreas
Most digestion small intestine: 7 m long, 2.5 cm diameter. Length related to diet. Example: meats easy to digest (carnivores short small intestines), plants longer (herbivores longer small intestines), omnivores (intermediate length) Large intestine: 1.5 m length, 7.6 cm diameter 1) Duodenum: first 25 30 cm. Majority of digestion 2) Jejunum: digestion + absorption 3) Ileum: mainly absorption Differentiated by cell shape Partially digested foods small intestine, soaked in HCl and Pepsin Acids entering chemical prosecretin secretin absorbed into bloodstream pancreas signals release of solution w/ bicarbonate ions (HCO3-) small intestine neutralize HCl in gastric fluid, raise pH 2.5 -> 9.0 Basic pH inactivates pepsin = small intestine protected. Pancreatic secretions enzymes for breakdown of 3 major component of foods
Protein Digestion protein digesting enzyme, trypsinogen from pancreas small intestine enzyme enterokinase converts trypsin breaks down long chain polypeptides shorter chain peptides. Second group, erepsins from pancreas/small intestine break bond between short chain peptides individual amino acids. Carbohydrate digestion amylase enzymes, continues digestion intermediate-size chains disaccharides. Small intestine disaccharide enzymes, disaccharidases monosaccharides Lipid digestion pancreas lipases: break down lipids. 2 types: 1) pancreatic lipase: most common, fats fatty acids + glycerol. 2) Phospholipase phospholipids Absorption: mostly in small, not large. Villi (long fingerlike tubes) increase SA (10fold increase). Cells of lining of each villus have microvilli (fine, threadlike extensions of membrane, further increase SA). Each villus capillary network, intertwining with lymph vessels lacteals (transport materials). Some nutrients absorbed diffusion, others actively transported. Carbohydrates + amino acids capillary networks. Fats lacteals.
6.6 The Liver and Gall Bladder
Liver fluid bile, containing bile salts speed up fat digestion. Empty stomach bile stored, concentrated in gall bladder. Fats in the small intestine hormone cholecystokinin (CCK) released carried in blood to gall bladder triggers gall bladder bile salts small intestine break down large flat globules into smaller droplets = physical digestion. Prepares fat for chemical digestion increasing surface area for fat-digesting enzymes (E.g. Pancreatic Lipase) Liver and Gall Bladder Problems 1) Cholesterol (insoluble component of bile, binding agent for salt crystals in bile). Crystals precipitate larger crystals = gallstones, can block bile duct, impair fat digestion, cause considerable pain. 2) Jaundice: bile contains pigments. Liver breaks down hemoglobin (red blood cells) products stored in gall bladder for removal (brown feces). Any obstruction of bile duct, accelerated destruction of red blood cells turns skins and other tissues yellow. 3) Cirrhosis: Liver stores glycogen, vitamins A, B12, C, can detoxify substances. Harmful chemicals soluble dissolved in blood urine. E.g. alcohol, broken into usable materials and wastes. Alcohol can destroy liver tissue. Damaged liver cells replaced with tissue/fat (cant carry out duties)
6.7 Absorption of Materials
Stomach absorbs some water, specific vitamins, some medicines, alcohol Food large intestine = chemical digestion complete Colon (largest segment of large intestine): stores wastes, reabsorbs water w/ some inorganic salts, minerals, vitamins. Large intestine bacteria, e.g. E. coli, essential to life, uses waste materials vitamins B and K Cellulose (long chain carbohydrate, plant cell walls) large intestine, undigested. Cannot be broken down, 1 function Bulk. Wastes build up + receptors in wall of intestine central nervous system prompts bowel movement removal of potentially toxic wastes from body. Less cellulose (roughage or fibre) wastes + toxins remain in body longer. Cancer of colon related to diet. E.g. processed, highly refined foods Fibre medical reports may reduce cholesterol levels (can be debated). Provides balanced diet. (see 6.5)
6.9 Homeostasis and Control Systems
Homeostasis: bodys ability to adjust and maintain a constant balance to a fluctuating internal and external environment. Greek words: homoiosis (similar/like) stasis (standing still).
E.g. Best internal temperature: 37 C, 0.1% blood sugar level, 7.35 blood pH. External environments change: air temperatures, foods, different demands on body from sports, etc. System of active balance has constant monitoring/feedback and special receptors sense info about blood sugar, body temperature, oxygen levels. E.g. homeostasis disrupted monitor sends signal to coordinating centre (brain) where normal limits are set info to appropriate regulator balance. E.g. Regulator adjustments: increase in heart rate during exercise, release of glucose (liver) to restore blood sugar levels. E.g. Regulation of blood sugar level. Chemical reactions ensure sugar concentration in blood appropriate level Relationship: insulin / glucagon. Increase in blood sugar level chemical receptors cause pancreas hormone insulin cells of liver and muscles (more permeable to glucose) liver excess glucose (not stored) glycogen (stored). Decrease in blood sugar level pancreas hormone glucagon conversion glycogen glucose body uses for immediate needs.
Homeostatic Control of Digestion Homeostatic controls before food is absorbed. Exerted by nervous and hormonal systems + nerves in stomach wall. Gastric secretions are produced before food in the stomach (when seeing food) + swallowing motions produce gastric juices. Hormones: e.g. secretin: released when acids small intestine with food absorbed in blood pancreas initiates release of substances raise pH of small intestine. e.g. Gastrin: (digestive hormone from stomach stimulates release of gastric juices to digest proteins): when partially digested proteins stomach. Also controlled: speed of digestive system processing food. Food stomach: nerves in stomach wall cause muscle contractions + secretion of gastric fluids. Large meal receptors more forceful stomach contractions + faster emptying. Fatty meal small intestine digestive hormone (enterogasterone) slows peristaltic movements = more time for fat digestion + absorption.
Вам также может понравиться
- Biological Systems Module 7.1Документ9 страницBiological Systems Module 7.1xara zinkОценок пока нет
- Running Head: 1: The Process of Human DigestionДокумент5 страницRunning Head: 1: The Process of Human Digestiongmelendez2Оценок пока нет
- Chapter 24 - Introduction To The Digestive SystemДокумент7 страницChapter 24 - Introduction To The Digestive Systemtomorrow.today.yesterday .yesterdayОценок пока нет
- DU - Digestive SystemДокумент6 страницDU - Digestive SystemAlexandra MatysováОценок пока нет
- The Digestive SystemДокумент23 страницыThe Digestive SystemJenderal Yohanes100% (1)
- m6 Digestive SystemДокумент23 страницыm6 Digestive Systemapi-464344582Оценок пока нет
- Digestive System Overview: Parts and FunctionsДокумент62 страницыDigestive System Overview: Parts and FunctionsKeturah IbrahimОценок пока нет
- Digestive System 258754Документ17 страницDigestive System 258754Musharaf RehmanОценок пока нет
- The Digestive System ExplainedДокумент4 страницыThe Digestive System ExplainedArash DhillonОценок пока нет
- Digest the Digestive SystemДокумент14 страницDigest the Digestive Systemrahul_onlyoneОценок пока нет
- Nutrition Quiz NotesДокумент8 страницNutrition Quiz NotesThomas AssisОценок пока нет
- Human Physiology - Lauras NotesДокумент20 страницHuman Physiology - Lauras NotesLaya ShrbagiОценок пока нет
- (GenBio2) Week 2 - Organ SystemsДокумент111 страниц(GenBio2) Week 2 - Organ SystemsmarielsolarteОценок пока нет
- Modular Handout and Worksheet For April 19-21-2023Документ5 страницModular Handout and Worksheet For April 19-21-2023ccam88743Оценок пока нет
- Digestive NendenДокумент30 страницDigestive NendenFahmi IlyasОценок пока нет
- Digestive System: A. Def'nДокумент14 страницDigestive System: A. Def'nRahardian Gusta PatriaОценок пока нет
- Human digestion and small intestine absorptionДокумент29 страницHuman digestion and small intestine absorptionRaynaahОценок пока нет
- 4thQ Week1 PPT DigestiveДокумент49 страниц4thQ Week1 PPT DigestiveGeronimo SantiagoОценок пока нет
- Gastrointestinal System Ppt.-NewДокумент117 страницGastrointestinal System Ppt.-NewFatima Syed100% (3)
- Digestive System: From Mouth to Anus in 40 CharactersДокумент5 страницDigestive System: From Mouth to Anus in 40 CharactersKean AtonОценок пока нет
- Biopharmaceutics-01 AssignmentДокумент14 страницBiopharmaceutics-01 AssignmentRA TanvirОценок пока нет
- Digestion and AbsorptionДокумент3 страницыDigestion and AbsorptionDJ DannyОценок пока нет
- Alimentary Canal Fact FileДокумент2 страницыAlimentary Canal Fact FileAsma AbbasОценок пока нет
- Digestive System 2022-23Документ28 страницDigestive System 2022-23Fady Fady100% (1)
- Fisiology GastroenterohepatologyДокумент71 страницаFisiology GastroenterohepatologyaryopraditoОценок пока нет
- 09 DigestionДокумент85 страниц09 DigestionSumihar PasaribuОценок пока нет
- The Digestive System A Level NotesДокумент7 страницThe Digestive System A Level Noteselendria100% (1)
- Human PhysiologyДокумент26 страницHuman PhysiologyLaya ShrbagiОценок пока нет
- Maui Jullian Removed A MessageДокумент3 страницыMaui Jullian Removed A MessageGio LlanosОценок пока нет
- Fisiologi GIДокумент15 страницFisiologi GIfirda trianandaОценок пока нет
- Digestive System Grade 10-11Документ7 страницDigestive System Grade 10-11Nandana Nayana KumaraОценок пока нет
- Biology 11 - June Final Exam NotesДокумент15 страницBiology 11 - June Final Exam NotesagbavaОценок пока нет
- Homoestatic Mechanisms Regulate An Animal's Internal Environment. TheДокумент19 страницHomoestatic Mechanisms Regulate An Animal's Internal Environment. TheGabbie CruzОценок пока нет
- Name: Santos, Lore Anne Mhae T. Date: - Instructor: Giovanni D. David, Edd, RN ScoreДокумент4 страницыName: Santos, Lore Anne Mhae T. Date: - Instructor: Giovanni D. David, Edd, RN ScoreLore Anne Mhae SantosОценок пока нет
- Presentation 1Документ126 страницPresentation 1Roccie Dawn MisaОценок пока нет
- Chapter 6 - DigestionДокумент17 страницChapter 6 - DigestionTrisha100% (1)
- Cell is the smallest unit of lifeДокумент8 страницCell is the smallest unit of lifeAnsel Francis RapsingОценок пока нет
- PembahasanДокумент32 страницыPembahasanwening gbОценок пока нет
- Sci NotesДокумент4 страницыSci NotesMangoooОценок пока нет
- Digestion & AbsorptionДокумент13 страницDigestion & AbsorptionU Than HanОценок пока нет
- 6.1 Digestion and Absorption: Digestion of Food MoleculesДокумент24 страницы6.1 Digestion and Absorption: Digestion of Food MoleculesWILSON KosheyОценок пока нет
- Zoology (The Book 1)Документ48 страницZoology (The Book 1)sweetnutellaОценок пока нет
- The Anatomy of The StomachДокумент33 страницыThe Anatomy of The StomachVictor OmoloОценок пока нет
- DU - Digestive System Ivana MajovskaДокумент5 страницDU - Digestive System Ivana MajovskaivkaamajОценок пока нет
- Digestive SystemДокумент35 страницDigestive SystemAnj TrinidadОценок пока нет
- Laboratorio de La Via Digestiva BajaДокумент15 страницLaboratorio de La Via Digestiva BajaDanna Lopez RamosОценок пока нет
- The Digestive SystemДокумент3 страницыThe Digestive SystemLuz Dianne SoloriaОценок пока нет
- Caballero DigestiveДокумент5 страницCaballero DigestiveClairyssa Myn D CaballeroОценок пока нет
- Module6 All CompressedДокумент58 страницModule6 All CompressedAryanaОценок пока нет
- The Digestive System: S.Kep, NS., M.KepДокумент10 страницThe Digestive System: S.Kep, NS., M.KepAuliya AlfaОценок пока нет
- BIO Ninja - Human PhysiologyДокумент33 страницыBIO Ninja - Human PhysiologyLaya ShrbagiОценок пока нет
- 10 BiologyДокумент3 страницы10 BiologyNaveen NОценок пока нет
- Digestive SystemДокумент9 страницDigestive SystemhlorenoОценок пока нет
- BIO 1133 Exercise 9 (Digestive Sytem of The Frog)Документ6 страницBIO 1133 Exercise 9 (Digestive Sytem of The Frog)Tonet LapeОценок пока нет
- Tema 3 Bio y GeoДокумент4 страницыTema 3 Bio y GeoLaura CamposОценок пока нет
- The 4 Stages of Food Processing in the Digestive SystemДокумент30 страницThe 4 Stages of Food Processing in the Digestive SystemUniversal DiscoveringОценок пока нет
- AnaPhy Reporting ScriptДокумент5 страницAnaPhy Reporting ScriptAlliah Angela Soldevilla BasadreОценок пока нет
- MLM10 Life Processes2Документ18 страницMLM10 Life Processes2anshuman2683Оценок пока нет
- Chapter 14Документ7 страницChapter 14Kate Wen GuanОценок пока нет
- GAAPДокумент2 страницыGAAPKate Wen GuanОценок пока нет
- Chapter 13Документ7 страницChapter 13Kate Wen GuanОценок пока нет
- Chapter 5Документ5 страницChapter 5Kate Wen GuanОценок пока нет
- Chapter 9Документ4 страницыChapter 9Kate Wen GuanОценок пока нет
- Chapter 10Документ6 страницChapter 10Kate Wen GuanОценок пока нет
- Chapter 12Документ2 страницыChapter 12Kate Wen GuanОценок пока нет
- Chapter 6Документ5 страницChapter 6Kate Wen GuanОценок пока нет
- Chapter 13Документ11 страницChapter 13Kate Wen GuanОценок пока нет
- Chapter 1 QuestionsДокумент2 страницыChapter 1 QuestionsKate Wen GuanОценок пока нет
- Chapter 3Документ3 страницыChapter 3Kate Wen GuanОценок пока нет
- Chapter 14Документ3 страницыChapter 14Kate Wen Guan100% (1)
- Chapter 2Документ2 страницыChapter 2Kate Wen GuanОценок пока нет
- Accounting Chapter 5 BEДокумент1 страницаAccounting Chapter 5 BEKate Wen GuanОценок пока нет
- Chapter 11Документ2 страницыChapter 11Kate Wen GuanОценок пока нет
- Chapter 10Документ9 страницChapter 10Kate Wen GuanОценок пока нет
- Chapter 4Документ6 страницChapter 4Kate Wen GuanОценок пока нет
- Chapter 2Документ8 страницChapter 2Kate Wen GuanОценок пока нет
- Chapter 8 ReviewДокумент3 страницыChapter 8 ReviewKate Wen GuanОценок пока нет
- Chapter 7Документ4 страницыChapter 7Kate Wen GuanОценок пока нет
- Biology Exam ReviewДокумент8 страницBiology Exam ReviewKate Wen Guan100% (2)
- Chapter 7 QuestionsДокумент7 страницChapter 7 QuestionsKate Wen GuanОценок пока нет
- Hapter Igestion and Utrition: 6.1 Organs and Organ SystemsДокумент5 страницHapter Igestion and Utrition: 6.1 Organs and Organ SystemsKate Wen GuanОценок пока нет
- Chapter 9Документ10 страницChapter 9Kate Wen GuanОценок пока нет
- Chapter 5Документ6 страницChapter 5Kate Wen GuanОценок пока нет
- Chapter 3Документ9 страницChapter 3Kate Wen GuanОценок пока нет
- Chapter 1Документ3 страницыChapter 1Kate Wen Guan50% (2)
- Basic Safety TrainingДокумент70 страницBasic Safety TrainingMehryl Amponin-Viernes100% (3)
- Ealth AND Hysical Ducation: A Teachers' Guide For Class VIДокумент176 страницEalth AND Hysical Ducation: A Teachers' Guide For Class VIManoj AryanОценок пока нет
- Grade 7 Respiratory System LessonsДокумент19 страницGrade 7 Respiratory System LessonsclaireОценок пока нет
- Nutritional Status. Summary - BaselineДокумент2 страницыNutritional Status. Summary - BaselinePotato ManiacОценок пока нет
- AP-2 Lab Report - Lab 01 The Endrocine SystemДокумент15 страницAP-2 Lab Report - Lab 01 The Endrocine Systemrcdunfee86% (7)
- Components of BloodДокумент13 страницComponents of BloodMichael LiongОценок пока нет
- Project From Vertical Knee Raise Chin Dip Station Plan Page 1 of 29Документ29 страницProject From Vertical Knee Raise Chin Dip Station Plan Page 1 of 29fokerОценок пока нет
- Dr. Sebi Nutritional GuideДокумент15 страницDr. Sebi Nutritional GuideDonnaveo Sherman90% (52)
- Bantu, Meaning and A Small Glossary. (Read 3902 Times) : Frank Jose AmayaДокумент4 страницыBantu, Meaning and A Small Glossary. (Read 3902 Times) : Frank Jose AmayaJames DavisОценок пока нет
- Chapter 1 The Human Body An OrientationДокумент18 страницChapter 1 The Human Body An OrientationHannah Lee LumosbogОценок пока нет
- Review in Science Circulatory System PulmonaryДокумент3 страницыReview in Science Circulatory System PulmonaryElvie Jane P. MolatoОценок пока нет
- BMI AssignmentДокумент1 страницаBMI AssignmentcherylasaroОценок пока нет
- DRESSMAKING-10 Q4 Mod3 USLeM-RTPДокумент10 страницDRESSMAKING-10 Q4 Mod3 USLeM-RTPApsimachiaОценок пока нет
- BSC 103 Course Outline BSPSYCH 1 - B & CДокумент3 страницыBSC 103 Course Outline BSPSYCH 1 - B & CpentojochaunceyОценок пока нет
- Does Hand Grip Strength Correlate With Shoulder Rotator Cuff FunctionДокумент6 страницDoes Hand Grip Strength Correlate With Shoulder Rotator Cuff FunctionsoylahijadeunvampiroОценок пока нет
- Feb13 TB12 High Intensity Interval Training Plan PDFДокумент16 страницFeb13 TB12 High Intensity Interval Training Plan PDFShivam Gadhia100% (4)
- Test Bank For Understanding Anatomy Physiology 3rd Edition Gale Sloan ThompsonДокумент8 страницTest Bank For Understanding Anatomy Physiology 3rd Edition Gale Sloan ThompsonBecky Ramirez100% (27)
- How Long Does It Take For The Human Body To Replace A Pint of Donated Blood - QuoraДокумент5 страницHow Long Does It Take For The Human Body To Replace A Pint of Donated Blood - Quorawdc cdwОценок пока нет
- Caplan, Michael J-Reference Module in Biomedical Research-Elsevier (2014)Документ17 страницCaplan, Michael J-Reference Module in Biomedical Research-Elsevier (2014)Muhammad IkbarОценок пока нет
- Grade 4 Muscles and Skin LessonsДокумент24 страницыGrade 4 Muscles and Skin LessonsSavion Sander AlinaОценок пока нет
- Brain & Organ FunctionsДокумент5 страницBrain & Organ FunctionsaysiiОценок пока нет
- SCIENCE ExamДокумент4 страницыSCIENCE ExamLesley AntojadoОценок пока нет
- Taliban Press Swift Advance As U.S. Mobilizes To Evacuate: Diversity Rises Fastest in The MidwestДокумент52 страницыTaliban Press Swift Advance As U.S. Mobilizes To Evacuate: Diversity Rises Fastest in The MidwestTetê BragaОценок пока нет
- B.E - I Yr 2018-19 FR ClassesДокумент220 страницB.E - I Yr 2018-19 FR ClassesMatam PrasadОценок пока нет
- Department of Education School Form 8 Learner's Basic Health and Nutrition Report (SF8)Документ8 страницDepartment of Education School Form 8 Learner's Basic Health and Nutrition Report (SF8)Ada V. TabajenОценок пока нет
- MFA - Course Outline and Training SyllabusДокумент4 страницыMFA - Course Outline and Training SyllabusFaizal ENRAОценок пока нет
- Levi Strauss Co Factory List September 2017Документ7 страницLevi Strauss Co Factory List September 2017Nischal GautamОценок пока нет
- Anatomi Wajah Untuk Filler 220815Документ71 страницаAnatomi Wajah Untuk Filler 220815feilicia75% (4)
- Fashion VocabularyДокумент2 страницыFashion VocabularySempredijous100% (2)
- Describing People Greyscale Key Picture Description Exercises 14721Документ3 страницыDescribing People Greyscale Key Picture Description Exercises 14721Gulderay IklassovaОценок пока нет