Академический Документы
Профессиональный Документы
Культура Документы
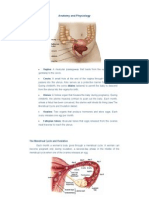
1-Obs&Gynae - Anatomy and Embryology of The Female Reproductive System
Загружено:
fadiawwad100%(3)100% нашли этот документ полезным (3 голоса)
328 просмотров52 страницыFemale Reproductive System
Оригинальное название
1-Obs&Gynae - Anatomy and Embryology of the Female Reproductive System
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документFemale Reproductive System
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
100%(3)100% нашли этот документ полезным (3 голоса)
328 просмотров52 страницы1-Obs&Gynae - Anatomy and Embryology of The Female Reproductive System
Загружено:
fadiawwadFemale Reproductive System
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 52
Anatomy and Embryology of the
Female Reproductive System
Gynaecology Lecture
September 28
th
2009
By
Abdel-Fattah Salem, M.D., F.R.C.O.G.
The Bony Pelvis
Sex differences in the pelvis
Female
Iliac blades more vertical
Iliac fossa shallower
Sacrum broader
Sub-pubic arch 80-85:
Ischiopubic rami narrower
Obturator foramen
traiangular
Greater sciatic notch wider
Greater anteroposterior
diameters
Male
Iliac crest rugged
Sub-pubic arch 50-60:
Obturator foramen ovoid
Ischial spines closer
Cavity longer and more
conical
Normal Pelvic Shape in Females
The brim is round
Sacral promontory is not prominent
The angle of inclination is about 55: to the
horizontal
The cavity is shallow with straight, non-converging
walls
The sacrum is smoothly curved
In the outlet the sacro-scieatic notches are wide
and shallow
Normal Pelvic Shape in Females(continued)
The sacrum does not project forwards
The ischial spines are not prominent
The pubic arch is wide and domed
The sub-pubic angle is about 90:
The inner tuberous diameter is wide accommodating four
knuckles of the average-sized hand with ease
Pelvic Diameters (cm)
Antero-posterior Oblique Transverse
Brim 11-11.5 12.5
Cavity 12
Outlet 12.5 11-11.5
12 12 12
12
12
12
Angle of Inclination
Uteropelvic axes
Anatomy of the female
reproductive organs
External Genitalia
Referred to collectively as the
vulva
Blood Supply: Internal pudendal artery
Nerve Supply: Pudendal nerve (sensory)
Lymphatic Drainage: via the inguinal nodes
Muscular
Canal
Extends from
cervix to
vulva
Anterior to
Rectum
Posterior to
bladder
Epithelial
Lining
Rugated,
stratified
squamous
Separated by
cervix into;
Anterior
fornix
Posterior
fornix
Lateral fornix
Vagina
Vagina (continued)
Blood Supply;
- Uterine artery
- Inferior pudendal artery
- Inferior vesical artery
- Middle rectal artery
Lymphatic Drainage;
- Lower 1/3 Vulva
- Upper 2/3 Cervix
Uterus
Muscular
Organ
Thick walled
Between bladder
and rectum
Consists
of 2
parts;
Uterine Corpus
Cervix
Blood
Supply
Uterine Corpus:
Uterine artery
Cervix: Cervical branch
of uterine artery
Uterine Support
Uterus supported by;
- Pelvic Diaphragm
- Pelvic Organs
- 4 paired sets of ligaments
Round Uterosacral Cardinal Broad
Round Ligament
Anterior surface of uterus
Labia majora
Start
End
Inginal canal
Broad Ligament
Paths
through
Keeps uterus anteverted
Function
Uterosacral Ligament
Origin Sacral Fascia
Insertion Posterior Inferior Uterus
Functions
-Mechanical Support -Contains autonomic nerves
Cardinal Ligament
Origin: Lateral pelvic wall
Insertion: Lateral cervix and vagina
Function;
- Mechanical support
- Prevent prolapse
Broad Ligament
Origin: Lateral pelvic wall
Insertion: Sides of uterus
Structures coursing through broad ligament;
- Fallopian tubes
- Round ligament
- Ovarian ligament
- Nerves, vessels, lymphatics
Fallopian Tubes
8-14 cm muscular tubes extending laterally from
uterus
Consists of 4 segments;
- Interstitial - Isthmic
- Ampullary - Infundibular
Ends with fimbriae at the ovary
Mesosalpinx is a peritoneal fold that attaches the
fallopian tubes to the broad ligament
Blood supply: Uterine and ovarian arteries
Ovaries
Consists of 2 parts;
- Cortex contains ova
- Medulla contains blood vessels
Mesovarium is a peritoneal fold that attaches the
ovary to the broad ligament
Blood supply: ovarian arteries (branch of aorta)
Left ovarian vein drains into left renal vein
Embryology
Gonadal differentiation
Ovarian differentiation
Determined by presence of
two X chromosomes
Located on short arm of X
chromosome
Absence of short arm of X
chromosome results in
ovarian agenisis
Testicular differentiation
TDF induces differentiation
Determined by presence of
cell surface antigen (H-Y)
Gene for H-Y antigen
located close to TDF gene
In Females In Males
Development of the ovary
25
th
Day
Germ cells
originate
from;
Primitive
hind gut
30
th
Day
Germ cells
migrate to;
Root of
mesentry
At birth
At puberty
Number of
follicles;
2 million
300,000
Development of the ovary (continued)
The coelomic epithelium proliferates and forms the
genital ridges
At early stages the primitive gonads consist of mesoderm
covered by coelomic epithelium
Germ cells migrate from the root of mesentry to the
genital ridge
Epithelium growing into the genital ridges forms the sex
cords
Germ cells and most of the sex cords remain in the
superficial part to form the ovarian cortex
Some of the sex cord cells form the ovarian medulla
Mullerian Duct
Also known as paramesonephric duct
The 2 mullerian ducts extend caudally until they reach
the urogenital sinus at 9 weeks gestation
The blind end projects into the posterior wall of the
sinus to become the mullerian tubercle
Lower ends of ducts fuse in the midline to form the
uterus and cervix
The thick muscular walls of the uterus and cervix
develop from proliferation of the mesenchyme
The cephalic ends of the ducts remain separated to
form the fallopian tubes
Development of the Vagina
Develops from an area of marked growth of the
mullerian tubercle also known as vaginal plate
The vaginal plate grows in all dimensions greatly
increasing the distance between the cervix and the
urogenital sinus
The upper 4/5
th
of the vagina is formed from the
Mullerian duct
The lower 1/5
th
of the vagina is formed from the
urogenital sinus
Development of external genitalia
The primitive cloaca is divided by a transverse
septum into;
- anterior urogenital portion
- posterior rectal portion
The genital folds and the genital swellings are
then formed by the proliferation of mesoderm
around the end of the urogenital sinus
The bladder and urethra form from the
vesicourethral portion of the urogenital sinus
External Genitalia
Genital tubercle enlarges
slightly Clitoris
Genital folds Libia
minora
Genital swelling
Libia majora
Genital tubercle enlarges
substantially Penis
Genital folds fuse
Penile urethra
Genital swelling
Scrotum
In Females In Males
Uterine Anomalies
Absence of Uterus Fusion Anomalies
Absence of the Uterus
Fusion anomalies of the uterus
Incidence;
-Overall; not uncommon
- Lesser degrees of defects are quite common
Minor fusion defects are asymptomatic
Possible presenting symptoms;
- Repeated abortion
- Persistent transverse lie of the fetus in late pregnancy
- Uterus didelphysis (double uterus) may lead to obstructed
labour
- Profound bleeding from rupture of rudimentary horn
consequent to implantation of the fetus
Agenesis of one Mullerian duct Unicornuate uterus
Incomplete fusion of Mullerian duct Double, arcuate or
septate uterus
Fusion anomalies of the uterus
Vaginal Anomalies
Absence of vagina Vaginal Septum
- Longitudinal
- Transverse
Absence of vagina
Generally associated with absence of uterus which
presents with 1: amenorrhea
Rarely; uterus maybe present and vagina absent
Secondary sexual characters + primary amenorrhea
ANATOMICAL DEFECTS such as;
- imperforate hymen
- absent vagina
Absence of vagina (treatment)
Meticulous search for urinary anomalies
Use of dilators in cases of absent uterus
McIndoe and Read operation; the created vagina
is then lined by either;
- split-skin graft
- amnion
Williams operation (vulvovaginoplasty)
Treatment; cruciate surgical incision
Imperforate hymen
Imperforate hymen/
Transverse vaginal septum
Called hydrocolpos
Fluid consists of cervical
and endometrial mucous
or in rare instances urine
accumulated through a
vesicovaginal fistula
proximal to the
obstruction.
Called hematocolpos
Presenting with acute
retention of urine
Primary amenorrhea
In newborns After puberty
A doctor who cannot take a good
history and a patient who cannot
give one are in danger of giving
and receiving bad treatment.
Author Unknown
Thank You
Вам также может понравиться
- INFANCY - A GUIDE TO EARLY PHYSICAL AND COGNITIVE DEVELOPMENTДокумент23 страницыINFANCY - A GUIDE TO EARLY PHYSICAL AND COGNITIVE DEVELOPMENTJayanth MamundiОценок пока нет
- Anatomy and Physiology GuideДокумент4 страницыAnatomy and Physiology GuideIanne RanchezОценок пока нет
- Female Reproductive AnatomyДокумент35 страницFemale Reproductive AnatomySasikala MohanОценок пока нет
- 01 Anatomy of Female Genital SystemДокумент63 страницы01 Anatomy of Female Genital Systemtania100% (2)
- Female Sexual Anatomy GuideДокумент50 страницFemale Sexual Anatomy GuideSitaramОценок пока нет
- Female Vulva Anatomy GuideДокумент18 страницFemale Vulva Anatomy Guidefujimeister0% (1)
- Technical Description-The Fight or Flight ResponseДокумент4 страницыTechnical Description-The Fight or Flight ResponseillyanОценок пока нет
- Understanding the Bishop's Score for a Successful Labour InductionДокумент2 страницыUnderstanding the Bishop's Score for a Successful Labour InductionAndy WijayaОценок пока нет
- Anatomy of Female Internal Genital OrganДокумент18 страницAnatomy of Female Internal Genital OrganVandana Liju Dev VasudevanОценок пока нет
- Female Reproductive System SampleДокумент15 страницFemale Reproductive System SamplemedpgnotesОценок пока нет
- Sanet - St-Ridleys The VulvaДокумент448 страницSanet - St-Ridleys The VulvaKM CorpОценок пока нет
- WHO - Labour InductionДокумент43 страницыWHO - Labour InductionDiana Yuliani AlensmeierОценок пока нет
- Clinical Anatomy of The Vulva, Vagina, Lower Pelvis, and PerineumДокумент20 страницClinical Anatomy of The Vulva, Vagina, Lower Pelvis, and PerineumJacobMsangОценок пока нет
- Bach Flowers for Emotional Eating and Weight LossДокумент3 страницыBach Flowers for Emotional Eating and Weight Lossashish PANTОценок пока нет
- Reconsidering Fetal PainДокумент4 страницыReconsidering Fetal PainFilipos ConstantinОценок пока нет
- PДокумент5 страницPmedstudОценок пока нет
- Female Reproductive System Functions and AnatomyДокумент67 страницFemale Reproductive System Functions and AnatomyPaul AndersonОценок пока нет
- Cervical incompetence diagnosis and managementДокумент40 страницCervical incompetence diagnosis and managementCristian AlbuОценок пока нет
- Anatomy of The ClitorisДокумент7 страницAnatomy of The ClitorisNongthombam NillachandОценок пока нет
- Histology of BreastДокумент6 страницHistology of BreastSusasti HasanahОценок пока нет
- "A Fun Hazily Snail Barn-Aftermaster": Neisseria Gonorrhea and Chlamydia TrachomatisДокумент3 страницы"A Fun Hazily Snail Barn-Aftermaster": Neisseria Gonorrhea and Chlamydia TrachomatisIke Rillera100% (1)
- Armand Zini, Ashok Agarwal (Eds.) - A Clinician's Guide To Sperm DNA and Chromatin Damage (2018, Springer International Publishing) PDFДокумент598 страницArmand Zini, Ashok Agarwal (Eds.) - A Clinician's Guide To Sperm DNA and Chromatin Damage (2018, Springer International Publishing) PDFMauro Porcel de PeraltaОценок пока нет
- External Ear Diseases PDFДокумент6 страницExternal Ear Diseases PDFJohn Christopher LucesОценок пока нет
- Female Reproductive System ExplainedДокумент17 страницFemale Reproductive System ExplainedJasmaine RivoОценок пока нет
- Anatomy For The Gynecologic OncologistДокумент70 страницAnatomy For The Gynecologic OncologistjroshsperlingОценок пока нет
- The contents of the ovarian pedicle in torsion are:1. Infundibulopelvic ligament with ovarian vessels 2. Ovarian ligament3. Mesoovarium4. Part of fallopian tube5. Utero-ovarian anastomosisДокумент65 страницThe contents of the ovarian pedicle in torsion are:1. Infundibulopelvic ligament with ovarian vessels 2. Ovarian ligament3. Mesoovarium4. Part of fallopian tube5. Utero-ovarian anastomosisashwiniОценок пока нет
- Anatomy of Female Genital TractДокумент37 страницAnatomy of Female Genital TractSemon YohannesОценок пока нет
- Perineum and Reproductive SystemДокумент36 страницPerineum and Reproductive SystemHesbon MomanyiОценок пока нет
- 3 The Male and Female Internal GenitaliaДокумент39 страниц3 The Male and Female Internal GenitaliaOmotosho DavidОценок пока нет
- Female Reproductive System LectureДокумент33 страницыFemale Reproductive System LectureJessy OnahОценок пока нет
- Female Reproductive Organs ExplainedДокумент45 страницFemale Reproductive Organs ExplainedsahrОценок пока нет
- Female Reproductive System Functions and OrgansДокумент59 страницFemale Reproductive System Functions and Organszenith parmarОценок пока нет
- Ovaries and Fallopian TubesДокумент39 страницOvaries and Fallopian TubessureshmanguttiОценок пока нет
- 07 - Uterus, Uterine Tubes, OvariesДокумент52 страницы07 - Uterus, Uterine Tubes, Ovariesck4realОценок пока нет
- Female Genital System - Internal Structures (CU-PA-2020)Документ63 страницыFemale Genital System - Internal Structures (CU-PA-2020)karenadjei44Оценок пока нет
- L6 - Anatomy of Female Reproductive SystemДокумент60 страницL6 - Anatomy of Female Reproductive SystemJIA YUET NGОценок пока нет
- Congenital Abnormalities of The Female Reproductive TractДокумент39 страницCongenital Abnormalities of The Female Reproductive TractBTK 150% (2)
- Development of The Urinary SystemДокумент32 страницыDevelopment of The Urinary SystemPaulin AmanОценок пока нет
- Anatomy of The Female Genital OrganДокумент19 страницAnatomy of The Female Genital Organaachal dhitalОценок пока нет
- Abdomen 2Документ41 страницаAbdomen 2Cristina-Alexandra ConstantinОценок пока нет
- Femalerprdctive 100423100153 Phpapp01Документ29 страницFemalerprdctive 100423100153 Phpapp01johairah merphaОценок пока нет
- 01 Anatomy of Female Genital System DR - OsmaДокумент69 страниц01 Anatomy of Female Genital System DR - OsmaAyalewОценок пока нет
- Pelvic Cavity (Reproductive System) : Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistДокумент49 страницPelvic Cavity (Reproductive System) : Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDОценок пока нет
- Male Repro 2019Документ79 страницMale Repro 2019yasrulОценок пока нет
- Dev of Reproductive SystemДокумент75 страницDev of Reproductive SystemAravindkumar ManivannanОценок пока нет
- 2.pelvic Viscera-1Документ32 страницы2.pelvic Viscera-1GeoffreyОценок пока нет
- Human ReproductionДокумент94 страницыHuman ReproductionDivya AgarawalОценок пока нет
- Male Reproductive Organs 2018Документ80 страницMale Reproductive Organs 2018yasrul izad100% (1)
- 1.female Reproductive SystemДокумент52 страницы1.female Reproductive SystemKhairul HananОценок пока нет
- Surgery-GynecologyДокумент101 страницаSurgery-GynecologyAman Singh Rao100% (1)
- Abdominal Wall: DR Ssebuufu Robinson Butale University Teaching HospitalДокумент29 страницAbdominal Wall: DR Ssebuufu Robinson Butale University Teaching HospitalIrakiza jean jacquesОценок пока нет
- Anatomy of Female Genital TractДокумент30 страницAnatomy of Female Genital TractHerman FiraОценок пока нет
- UntitledДокумент65 страницUntitledAbiola NerdОценок пока нет
- 2anatomy of The Inguinal RegionДокумент47 страниц2anatomy of The Inguinal Regionthowell3Оценок пока нет
- CMG: Congenital Malformations of the Genital TractДокумент54 страницыCMG: Congenital Malformations of the Genital Tractapule geraldhumbleОценок пока нет
- Revisit of Male & Female Genital Tracts Semester VIIДокумент50 страницRevisit of Male & Female Genital Tracts Semester VIIDr. AyshaОценок пока нет
- 4 The Female and Male External Genitalia DiyaДокумент48 страниц4 The Female and Male External Genitalia DiyaOmotosho DavidОценок пока нет
- Mammary Gland Additional NotesДокумент36 страницMammary Gland Additional NotesjdfОценок пока нет
- Word Salad 00Документ182 страницыWord Salad 00fadiawwadОценок пока нет
- Answer SaladДокумент7 021 страницаAnswer SaladfadiawwadОценок пока нет
- Victor Lopez - Latin RhythmsДокумент29 страницVictor Lopez - Latin RhythmsXanthus Ching100% (4)
- Seminars - 6th Yr GP AДокумент4 страницыSeminars - 6th Yr GP AfadiawwadОценок пока нет
- White ChristopherДокумент96 страницWhite ChristopherOlly StevensonОценок пока нет
- Two States For Two Peoples On Two Sides of The JordanДокумент18 страницTwo States For Two Peoples On Two Sides of The JordanfadiawwadОценок пока нет
- White ChristopherДокумент96 страницWhite ChristopherOlly StevensonОценок пока нет
- OSCE GynecologyДокумент55 страницOSCE GynecologySyahmi Yahya88% (8)
- Music - A Handbook For Composition and AnalysisДокумент217 страницMusic - A Handbook For Composition and AnalysismoonaboveОценок пока нет
- 100 Chords For GuitarДокумент32 страницы100 Chords For GuitarfadiawwadОценок пока нет
- Secret of The Mastering Engineer (Bob Katz) PDFДокумент17 страницSecret of The Mastering Engineer (Bob Katz) PDFRafaelCosta100% (1)
- MCQs in Pathology: Key ConceptsДокумент69 страницMCQs in Pathology: Key Conceptsfadiawwad100% (4)
- Apologetics Fact SheetДокумент2 страницыApologetics Fact SheetfadiawwadОценок пока нет
- Agile Process ModelsДокумент15 страницAgile Process ModelsShadrack KimutaiОценок пока нет
- JSP - How To Edit Table of Data Displayed Using JSP When Clicked On Edit ButtonДокумент8 страницJSP - How To Edit Table of Data Displayed Using JSP When Clicked On Edit Buttonrithuik1598Оценок пока нет
- Land Securities Group (A)Документ13 страницLand Securities Group (A)Piyush SamalОценок пока нет
- Journal of Electronic MaterialsДокумент10 страницJournal of Electronic MaterialsSanjib BaglariОценок пока нет
- Maheshwar Handlooms Cluster Diagnostic StudyДокумент15 страницMaheshwar Handlooms Cluster Diagnostic Studyumang31390100% (3)
- Chapter 3 - The Role of Multimedia in EducationДокумент37 страницChapter 3 - The Role of Multimedia in EducationGellie Ann Silvestre RapinОценок пока нет
- Final Project On Employee EngagementДокумент48 страницFinal Project On Employee Engagementanuja_solanki8903100% (1)
- AIESEC - Exchange Participant (EP) GuidebookДокумент24 страницыAIESEC - Exchange Participant (EP) GuidebookAnonymous aoQ8gc1Оценок пока нет
- APEC ArchitectДокумент6 страницAPEC Architectsarah joy CastromayorОценок пока нет
- College Management System Micro-ProjectДокумент27 страницCollege Management System Micro-ProjectNatashaОценок пока нет
- 04 - JTC Template On Project ProposalДокумент10 страниц04 - JTC Template On Project Proposalbakelm alqamisОценок пока нет
- Assessment of Hygiene Status and Environmental Conditions Among Street Food Vendors in South-Delhi, IndiaДокумент6 страницAssessment of Hygiene Status and Environmental Conditions Among Street Food Vendors in South-Delhi, IndiaAdvanced Research Publications100% (1)
- PCC ConfigДокумент345 страницPCC ConfigVamsi SuriОценок пока нет
- Homologation Form Number 5714 Group 1Документ28 страницHomologation Form Number 5714 Group 1ImadОценок пока нет
- Emilia Perroni-Play - Psychoanalytic Perspectives, Survival and Human Development-Routledge (2013) PDFДокумент262 страницыEmilia Perroni-Play - Psychoanalytic Perspectives, Survival and Human Development-Routledge (2013) PDFMihaela Ioana MoldovanОценок пока нет
- Epitalon, An Anti-Aging Serum Proven To WorkДокумент39 страницEpitalon, An Anti-Aging Serum Proven To Workonæss100% (1)
- Introduction To ResearchДокумент5 страницIntroduction To Researchapi-385504653Оценок пока нет
- Marcos & Sumulong Highway, Rizal Applicant'S Information Sheet (Non-Academic)Документ2 страницыMarcos & Sumulong Highway, Rizal Applicant'S Information Sheet (Non-Academic)dummy testerОценок пока нет
- OutliningДокумент17 страницOutliningJohn Mark TabbadОценок пока нет
- Fitting A Logistic Curve To DataДокумент12 страницFitting A Logistic Curve To DataXiaoyan ZouОценок пока нет
- RQQДокумент3 страницыRQQRazerrdooОценок пока нет
- Practice Questionnaire For New Omani QAQC Staff - DLQ DeptДокумент7 страницPractice Questionnaire For New Omani QAQC Staff - DLQ DeptSuliman Al RuheiliОценок пока нет
- Polystylism in The Context of Postmodern Music. Alfred Schnittke's Concerti GrossiДокумент17 страницPolystylism in The Context of Postmodern Music. Alfred Schnittke's Concerti Grossiwei wuОценок пока нет
- Vmware Vsphere Professional 8 Exam Dumps PDF (VCP DCV)Документ158 страницVmware Vsphere Professional 8 Exam Dumps PDF (VCP DCV)romal ghulamОценок пока нет
- Strategies in Various Speech SituationsДокумент6 страницStrategies in Various Speech SituationsSky NayytОценок пока нет
- TOTAL Income: POSSTORE JERTEH - Account For 2021 Start Date 8/1/2021 End Date 8/31/2021Документ9 страницTOTAL Income: POSSTORE JERTEH - Account For 2021 Start Date 8/1/2021 End Date 8/31/2021Alice NguОценок пока нет
- Training Plan JDVP 2020 - BPP (40days)Документ36 страницTraining Plan JDVP 2020 - BPP (40days)Shallimar Alcarion100% (1)
- Krittika Takiar PDFДокумент2 страницыKrittika Takiar PDFSudhakar TomarОценок пока нет
- Grimoire of Baphomet A-Z EditionДокумент18 страницGrimoire of Baphomet A-Z EditionTheK1nGp1N100% (1)
- 6 Lesson Writing Unit: Personal Recount For Grade 3 SEI, WIDA Level 2 Writing Kelsie Drown Boston CollegeДокумент17 страниц6 Lesson Writing Unit: Personal Recount For Grade 3 SEI, WIDA Level 2 Writing Kelsie Drown Boston Collegeapi-498419042Оценок пока нет