Академический Документы
Профессиональный Документы
Культура Документы
Joint Instability: Hendradi Khumarga SPOT. FICS
Загружено:
Joshua Obrien0 оценок0% нашли этот документ полезным (0 голосов)
53 просмотров48 страницJoint laxity, familial has been identified as tending to occur in family members. A familial cause may be from a common environmental influence or may be genetic. Treatment A dislocated joint usually can only be successfully'reduced' into its normal position by a trained medical professional.
Исходное описание:
Оригинальное название
Joint Instability.hen
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документJoint laxity, familial has been identified as tending to occur in family members. A familial cause may be from a common environmental influence or may be genetic. Treatment A dislocated joint usually can only be successfully'reduced' into its normal position by a trained medical professional.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
53 просмотров48 страницJoint Instability: Hendradi Khumarga SPOT. FICS
Загружено:
Joshua ObrienJoint laxity, familial has been identified as tending to occur in family members. A familial cause may be from a common environmental influence or may be genetic. Treatment A dislocated joint usually can only be successfully'reduced' into its normal position by a trained medical professional.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 48
Joint Instability
Hendradi Khumarga SPOT. FICS
Definition
Lack of stability of a joint or joint prosthesis.
Factors involved are intra-articular disease and integrity
of extra-articular structures such as joint capsule,
ligaments, and muscles
A very rare syndrome characterized mainly by
loose joints. Joint dislocations tend to occur
mainly in the shoulders, hips and kneecap.
Joint laxity, familial: Causes and Types
Genetic conditions
Joint conditions
Musculoskeletal conditions
Causes
Familial Cause: Joint laxity, familial
Joint laxity, familial has been identified as tending to
occur in family members. A familial cause may be from
a common environmental influence or may be genetic.
Symptoms of Joint instability syndrome (Joint
laxity, familial)
Loose joints
Dislocated joints
Dislocated kneecap
Dislocated shoulder
Dislocated hips
Dislocated joints
Joint dislocation, or luxation (Latin: luxatio) [1], occurs when
bones in a joint become displaced or misaligned.
It is often caused by a sudden impact to the joint. The ligaments
always become damaged as a result of a dislocation. A
subluxation is a partial dislocation.
Epidemiology
Although it is possible for any joint to become subluxed or
dislocated, the most common sites it is seen in the human body
are:
Shoulders
Fingers
Knees (Most likely by accompanied by a fracture)
Elbows (Most likely by accompanied by a fracture)
Joint dislocation
Classification and external resources
A traumatic dislocation of the tibiotalar joint of the ankle with distal fibular
fracture. Open arrow marks the tibia and the closed arrow marks the talus
Dislocated joints
Treatment
A dislocated joint usually can only be successfully 'reduced' into
its normal position by a trained medical professional.
Trying to reduce a joint without any training could result in
making the injury substantially worse.
X-rays are usually taken to confirm a diagnosis and detect any
fractures which may also have occurred at the time of
dislocation.
Treatment
Once a diagnosis is confirmed, the joint is usually manipulated
back into position. This can be a very painful process, therefore
this is typically done either in A&E under sedation or in an
Operating Room under a general anaesthetic.
It is important the joint is reduced as soon as possible, as in the
state of dislocation, the blood supply to the joint (or distal
anatomy) may be compromised. This is especially true in the case
of a dislocated ankle, due to the anatomy of the blood supply to
the foot.
Treatment
Shoulder injuries can also be surgically stabilized, depending on the severity,
using arthroscopic surgery.
Some joints are more at risk of becoming dislocated again after an initial
injury. This is due to the weakening of the muscles and ligaments which hold
the joint in place. The shoulder is a prime example of this. Any shoulder
dislocation should be followed up with thorough physiotherapy.
There are some medical conditions by where joint dislocations are frequent
and spontaneous, such as Ehlers-Danlos syndrome and congenital hip
dysplasia.
After care
After a dislocation, injured joints are usually held in
place by a splint (for straight joints like fingers and toes)
or a bandage (for complex joints like shoulders).
Additionally, the joint muscles, tendons and ligaments
must also be strengthened. This is usually done through
a course of physiotherapy, which will also help reduce
the chances of repeated dislocations of the same joint.
Dislocated shoulder
A dislocated shoulder occurs when the humerus separates
from the scapula at the glenohumeral joint.
The shoulder joint has the greatest range of motion of any joint
in the body and as a result is particularly susceptible to
dislocation and subluxation.
Approximately half of major joint dislocations seen in
emergency departments are of the shoulder.
Partial dislocation of the shoulder is referred to as subluxation.
Dislocated shoulder
The left shoulder and acromioclavicular joints, and the proper ligaments of
the scapula
Anterior (forward)
Over 95% of shoulder dislocation
cases are anterior.
Most anterior dislocations are sub-
coracoid. Sub-glenoid; subclavicular;
and, very rarely, intrathoracic or
retroperitoneal dislocations may occur.
It can result in damage to the axillary
artery.
Posterior (backward)
Posterior dislocations are occasionally due to electrocution or
seizure and may be caused by strength imbalance of the rotator
cuff muscles.
Posterior dislocations often go unnoticed, especially in an elderly
patient and in the unconscious trauma patient.
An average interval of 1 year was discovered between injury and
diagnosis of posterior dislocation in a series of 40 patients.
Inferior (downward)
Inferior dislocation is the least likely form,
occurring in less than 1% of all shoulder
dislocation cases.
This condition is also called luxatio erecta
because the arm appears to be permanently
held upward or behind the head.
It is caused by a hyper abduction of the arm
that forces the humeral head against the
acromion.
Inferior dislocations have a high
complication rate as many vascular,
neurological, tendon, and ligament injuries
are likely to occur from this kind of
dislocation.
Signs
Significant pain, which can sometimes be felt past the shoulder, along the arm.
Inability to move the arm from its current position, particularly in positions
with the arm reaching away from the body and with the top of the arm
twisted toward the back.
Numbness of the arm.
Visibly displaced shoulder. Some dislocations result in the shoulder appearing
unusually square.
No bone in the side of the shoulder showing shoulder has become dislocated.
Treatment
Prompt professional medical treatment should be sought for any suspected dislocation
injury.
Usually, a dislocated shoulder is kept in its current position by use of a splint or sling
(however, see below). A pillow between the arm and torso may provide support and
increase comfort. Ice may help reduce pain.
Emergency department care is focused on returning the shoulder to its normal
position via processes known as reduction. Normally, closed reduction, in which
several methods are used to manipulate the bone and joint from the outside, is used.
A variety of techniques exist, but some are preferred due to fewer complications or
easier execution.
In cases where closed reduction is not successful, surgical open reduction may be
needed.
Treatment
Following reduction, X-Ray imaging is often used to ensure that the reduction
was successful and there are no fractures. The arm should be kept in a sling or
immobilizer for several days, preferably until orthopedic consultation.
Hippocrates' and Kocher's method are rarely used anymore. Hippocrates used
to place the heel in the axilla and reduce shoulder dislocations. Kocher's
method if performed patiently and slowly can be performed without
anesthesia and if done correctly does not cause pain.
Traction is applied on the arm and it is abducted. Then, it is externally
rotated, and the arm is adducted following which it is internally rotated and
maintained in the position with the help of a sling. A chest x-ray should be
taken to confirm whether the head of humerus has reduced back into the
glenoid cavity.
Post-reduction: immobilisation in external versus
internal rotation
For thousands of years, treatment of anterior shoulder dislocation has
included immobilisation of the patient's arm in a sling, with the arm placed in
internal rotation (across the body).
However, three studies, one in cadavers and two in patients, suggest that the
detachment of the structures in the front of the shoulder is made worse when
the shoulder is placed in internal rotation to be seen.
By contrast, the structures are realigned when the arm is placed in external
rotation. New data suggest that if the shoulder is managed non-operatively
and immobilised, it should be immobilised in a position of external rotation.
Another study found that conventional shoulder immobilisation in a sling
offered no benefit
Surgery
Some cases require non-emergency surgery to repair damage to the tissues surrounding
in the shoulder joint and restore shoulder stability.
Arthroscopic surgery techniques may be used to repair the glenoidal labrum, capsular
ligaments, biceps long head anchor or SLAP lesion and/or to tighten the shoulder
capsule.
The time-proven surgical treatment for recurrent anterior instability of the shoulder is
a Bankart repair.
When the front of the shoulder socket has been broken or worn, a bone graft may be
required to restore stability [. When the shoulder dislocates posteriorly (out the back), a
surgery to reshape the socket may be necessary .
Conversly, there are new procedures that should be investigated as a possible
alternative to open surgery.
Kneecap dislocation
Kneecap dislocation occurs when the triangle-
shaped bone covering the knee (patella) moves
or slides out of place.
The problem usually occurs toward the outside
of the leg.
Left knee-joint from behind, showing interior ligaments.
Capsule of right knee-joint (distended). Lateral aspect.
Patellar dislocation
Dislocation usually
occurs as a result of
sudden direction changes
while running and the
knee is under stress or it
may occur as a direct
result of injury.
Causes
A dislocated kneecap most often occurs in women. It is
usually a result of sudden direction changes while
running. This puts the knee under stress.
Dislocation may also occur as a direct result of injury.
When it is dislocated, the kneecap may slip sideways
and around to the outside of the knee.
Symptoms
Kneecap (patella) moves to the outside of the knee
Knee pain and tenderness
Knee swelling
"Sloppy" kneecap -- you can move the kneecap excessively from right to left
(hypermobile patella)
The first few times this occurs, you will feel pain and be unable to walk.
However, if dislocations continue to occur and are untreated, you may feel
less pain and have less immediate disability. This is not a reason to avoid
treatment.
Kneecap dislocation damages your knee joint.
First Aid
Stabilize (splint) the knee with the leg fully straight (extended), and get medical attention.
Your health care provider will examine the knee, which could confirm that the kneecap is
dislocated.
A knee x-ray and, sometimes, MRIs should be done to make sure that the dislocation did not
cause a bone to break or cartilage to be damaged.
If tests show that you have no such damage, your knee will be placed into an immobilizer or cast
to prevent you from moving it for several weeks (usually about 3 weeks).
After this time, physical therapy can help build back your muscle strength and improve the knee's
range of motion.
If the knee remains unstable, you may need surgery to stabilize the kneecap. This may be done
using arthroscopic or open surgery.
Prevention
Use proper techniques when exercising or playing
sports. Keep your knee strong and flexible.
Some cases of knee dislocation may not be preventable,
especially if anatomic factors make you more likely to
dislocate your knee.
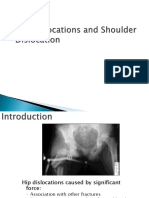
Dislocated Hip
Background
Hip dislocations can be classified into congenital and traumatic.
The annual incidence of congenital hip dislocation is approximately 2-4 cases
per 1000 births, and approximately 80-85% of the affected individuals are
girls.
Congenital hip dislocations are commonly the result of femoral head or
acetabular dysplasia.
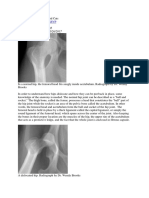
Pathophysiology
The hip is a modified ball-socket joint. The
femoral head is situated deep within the
acetabular socket, which is further enhanced
by a cartilaginous labrum.
The hip is also bolstered by a fibrous joint
capsule, the ischiofemoral ligament, and
many strong muscles of the upper thigh and
gluteal region.
Because of this anatomic configuration, the
hip is stable, subsequently, a large force is
required to dislocate the joint.
Since a high force mechanism is required,
other life-threatening injuries and fractures
are common.
Dislocated Hip
Motor vehicle crashes (MVC) account for almost two
thirds of traumatic hip dislocations.
Falls from height and sports injuries are also common
causes of hip dislocations.
The relationship of the femoral head to the acetabulum
is used to classify hip dislocations. The 3 main patterns
are posterior, anterior, and central.
Posterior dislocation
Posterior dislocations compromise
approximately 80-90% of hip
dislocations caused by MVCs.
The femoral head is situated posterior
to the acetabulum.
During a MVC, force is transmitted to
the flexed hip in one of two ways.
During rapid deceleration, the knees
strike the dashboard and transmit the
force through the femur to the hip.
If the leg is extended and the knee is
locked, force can be transmitted from
the floorboard though the entire lower
and upper leg to the hip joint.
Anterior dislocation
The femoral head is situated anterior to the acetabulum.
An anterior dislocation is most commonly caused by a
hyperextension force against an abducted leg that levers
the femoral head out of the acetabulum. Less
commonly, an anterior force against the posterior
femoral neck or head can produce this dislocation
pattern.
Central dislocation
A central dislocation is a
fracture-dislocation, the
femoral head lies medial to a
fractured acetabulum.
This is caused by a lateral
force against an adducted
femur seen in side impact
MVCs.
Clinical
A high index of suspicion for hip dislocation must be present whenever
evaluating a patient involved in a major trauma such as an MVC, significant
fall, or an athletic injury.
Patients with a hip dislocation will be in severe pain. They may complain of
pain to the lower extremities, back, or pelvic areas.
Patients will have difficulty moving the lower extremity on the affected side
and may complain of numbness or paresthesias.
Frequently, patients will be a victim of multiple trauma and may not pinpoint
pain to the hip as a result of altered mental status or distracting injuries.
Patients with a total hip replacement may present differently
Physical
As with any major trauma victim, assessment of the
airway, breathing, and circulation are of primary
importance. During the secondary survey, an
examination of the pelvic girdle and hip are
mandatory. Examination should consist of inspection,
palpation, active/passive range of motion, and a
neurovascular examination.
Physical
Inspection
Isolated anterior and posterior dislocations have classic appearances. In practice, these
appearances may be altered by the presence of fracture-dislocations or other bony
abnormalities along the leg.
Posterior: The hip is flexed, internally rotated, and adducted.
Anterior: The hip is minimally flexed, externally rotated and markedly
abducted
Palpation
Palpate the pelvis and lower extremity for any gross bony deformities or step-offs. In
an anterior hip dislocation, the femoral head can occasionally be palpated. Large
hematomas may signify vascular injury.
Range of motion
Patients with a hip dislocation have severely limited range of motion. Evaluate what
the patient can do comfortably. Do not forcefully perform range of motion on a
patient who cannot tolerate manipulation. Normal, painless range of motion virtually excludes hip dislocation.
Physical
Neurovascular examination
Signs of sciatic nerve injury include the following:
Loss of sensation in posterior leg and foot
Loss of dorsiflexion (peroneal branch) or plantar flexion (tibial branch)
Loss of deep tendon reflexes (DTRs) at the ankle
Signs of femoral nerve injury include the following:
Loss of sensation over the thigh
Weakness of the quadriceps
Loss of DTRs at knee
Signs of vascular injury include the following:
Hematoma
Loss of pulses
Pallor
Treatment
Prehospital Care
Patients with hip dislocation often have associated injuries that may take
precedence during stabilization, both in the field and in the ED. Attempts to
reduce the dislocation in the field are ill advised.
Establish the ABCs with appropriate spinal immobilization.
If hip dislocation is detected in the field, the patient should be placed on a
backboard and allowed to assume the leg position that is most comfortable
(ie, hip slightly flexed, leg adducted).
The patient should be transported to a level of trauma center appropriate for
his or her overall clinical status.
Treatment
Emergency Department Care
Patients with hip dislocations often have life-threatening injuries that take
precedence.
Once life-threatening injuries have been stabilized or ruled out, the hip
dislocation can be addressed. A proper neurovascular examination should be
performed. If a neurovascular deficit exists, there is even more urgency to
reduce the dislocation.
Appropriate analgesia should be provided. If hemodynamic status permits,
intravenous narcotics are usually indicated.
Radiographs to detect hip pathology should be obtained.
Reduction is greatly facilitated by the use of procedural sedation. Unless
sufficient sedation and muscle relaxation is achieved, attempts at relocation are
futile.
Treatment
Simple hip dislocations without associated fracture are within the practice scope of
most emergency physicians. Consider orthopedic consultation if it will not delay
relocation beyond a reasonable amount of time, usually within 6 hours.
Once procedural sedation has been achieved, the hip may be reduced by one of
the preceding methods.
Reducing a hip usually takes a significant amount of space and resources.
Usually, one person applies traction and one or two people supply counter traction. A
nurse or other physician provides sedation.
More than 3 attempts at closed reduction in the ED is not recommended. The
incidence of AVN increases with multiple attempts. If the dislocation cannot be
reduced, an emergent CT scan is indicated to visualize any bony or soft tissue
fragments that may hinder reduction. Closed reduction may be attempted in the
operating room under general anesthesia. However, a majority of these patients may
require open reduction.
Treatment
Fracture-dislocations or concomitant fractures of the femoral neck usually require the expertise of
an orthopedic specialist. Practice styles vary widely. Some orthopedists make an attempt at closed
reduction, whereas others immediately perform an open reduction if a fracture-dislocation exists.
After closed reduction, confirm placement with a repeat radiograph. A repeat neurovascular
examination should be performed and documented as well. A CT scan or MRI of the hip can
provide valuable information about further treatment and prognosis.
If relocation of the hip is successful, immobilize the legs in slight abduction by using a pad
between the legs to prevent adduction until skeletal traction can be instituted.
After reduction, patients with hip dislocation should be admitted to the hospital. Patients will be
nonambulatory and require a great deal of supportive care. Pain will be significant, even after
reduction, and patients may require parenteral narcotics.
The duration of traction and nonweight-bearing immobilization is controversial. Evidence
suggests that early weight bearing (eg, 2 wk after relocation) may increase the severity of aseptic
necrosis when it occurs. Early weight bearing decreases the incidence of other complications (eg,
venous thromboembolism, decubiti), and some studies have found equivalent outcomes with
early and delayed weight bearing.
Indications for open reduction
Irreducible dislocation (approximately 10% of all
dislocations)
Persistent instability of the joint following reduction (eg,
fracture-dislocation of the posterior acetabulum)
Fracture of the femoral head or shaft
Neurovascular deficits that occur after closed reduction
Medication
Administer adequate parenteral analgesia. The emergency physician,
consultant, and patient must decide on the most appropriate type and place
for reduction: open versus closed and emergency department versus operating
room.
If a closed reduction is attempted in the ED, the patient requires procedural
sedation. Procedural sedation policies should be established to define who
can administer medication, who must monitor the patient, the classes and
doses of procedural sedation medications, and the resources on hand for
resuscitation.
In addition to airway protection and rescue, the procedural sedation goals
must include pain relief, muscle relaxation, and procedure amnesia.
General anesthesia in the operating room may be required for patients with
dislocations that are irreducible by closed means as well as for those with
significant associated fractures, central dislocations, or associated
neurovascular injury.
Medication
Analgesics
Pain control is essential to good-quality patient
care. It ensures patient comfort, promotes
pulmonary toilet, and aids physical therapy
regimens. The analgesic must have a rapid onset,
predictable action, and be easily titratable.
Вам также может понравиться
- Shoulder Trauma Fractures and Dislocations-Orthoinfo - AaosДокумент6 страницShoulder Trauma Fractures and Dislocations-Orthoinfo - Aaosapi-228773845Оценок пока нет
- Hip DislocationДокумент4 страницыHip DislocationcrunkestОценок пока нет
- Shoulder DislocationДокумент28 страницShoulder DislocationQueen SofiaОценок пока нет
- Healthy Shoulder Handbook: Second Edition: 100 Exercises for Treating Common Injuries and Ending Chronic PainОт EverandHealthy Shoulder Handbook: Second Edition: 100 Exercises for Treating Common Injuries and Ending Chronic PainОценок пока нет
- Dislokasi Panggul & BahuДокумент42 страницыDislokasi Panggul & BahuAnton TrihartantoОценок пока нет
- Fracture-Dislocation of The Hip-KaizarДокумент69 страницFracture-Dislocation of The Hip-KaizarKaizar Ennis100% (1)
- Acquired DeformitiesДокумент6 страницAcquired DeformitiesAnonymous fVtDc9hОценок пока нет
- Shoulder Dislocation SubluxationДокумент4 страницыShoulder Dislocation SubluxationSisca Dwi AgustinaОценок пока нет
- William C. Cottrell, MD AbstractДокумент4 страницыWilliam C. Cottrell, MD AbstractmalaОценок пока нет
- Shoulder Dislocation Background: Shoulder Dislocations Traumatic InjuryДокумент7 страницShoulder Dislocation Background: Shoulder Dislocations Traumatic Injuryanastasiaanggita_265Оценок пока нет
- Shoulder Sports InjuryДокумент12 страницShoulder Sports InjuryfriskaОценок пока нет
- Anterior Shoulder Dislocation, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandAnterior Shoulder Dislocation, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Materi Kuliah FK ULM 2022 - Lower Extremity I - Hip & KneeДокумент61 страницаMateri Kuliah FK ULM 2022 - Lower Extremity I - Hip & Kneezaki ridhoniОценок пока нет
- Fractures and Dislocations of The Upper Limb IIДокумент90 страницFractures and Dislocations of The Upper Limb IIatikah_jamilОценок пока нет
- Distal Clavicle Osteolysis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandDistal Clavicle Osteolysis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Dislocations: Diagnosis, Management, and Complications: Marvin H. Meyers, M.D.Документ12 страницDislocations: Diagnosis, Management, and Complications: Marvin H. Meyers, M.D.Unoscientris StupaОценок пока нет
- Elbow Dislocation Orthoinfo AaosДокумент4 страницыElbow Dislocation Orthoinfo AaosAnonymous L9D1I7DZОценок пока нет
- Acute Shoulder DislocationДокумент10 страницAcute Shoulder DislocationMalueth AnguiОценок пока нет
- 12 - Fractures & Dislocations of The Upper Limb-1Документ84 страницы12 - Fractures & Dislocations of The Upper Limb-1Ain Ul NoorОценок пока нет
- Hip Fractures-Orthoinfo - AaosДокумент9 страницHip Fractures-Orthoinfo - Aaosapi-228773845Оценок пока нет
- Elbow Pain.Документ47 страницElbow Pain.salmankhan09215Оценок пока нет
- Patient - Co.uk - Trusted Medical Information and Support: Knee Fractures and DislocationsДокумент4 страницыPatient - Co.uk - Trusted Medical Information and Support: Knee Fractures and DislocationsHayelom MichaelОценок пока нет
- The First Affiliated Hospital of Zhengzhou UniversityДокумент42 страницыThe First Affiliated Hospital of Zhengzhou Universityapi-19916399Оценок пока нет
- Shoulder Injures and Management 2Документ94 страницыShoulder Injures and Management 2Khushboo IkramОценок пока нет
- Colles Fracture & Knee DislocationДокумент38 страницColles Fracture & Knee DislocationNap91Оценок пока нет
- Joint DislocationsДокумент64 страницыJoint DislocationsSabrina Indri WardaniОценок пока нет
- Các Trường Hợp Lóc Da CLB Y KHOA TRẺ Y KHOA VINHДокумент84 страницыCác Trường Hợp Lóc Da CLB Y KHOA TRẺ Y KHOA VINHVmu ShareОценок пока нет
- Spinal SurgeryДокумент19 страницSpinal SurgerySalomeSibashviliОценок пока нет
- Congenital Hip DislocationДокумент2 страницыCongenital Hip Dislocationj-crisОценок пока нет
- Fractures of The Hip: Extraarticular Fracture Does Not Involve The Articular SurfaceДокумент6 страницFractures of The Hip: Extraarticular Fracture Does Not Involve The Articular SurfaceBella DonnaОценок пока нет
- Diseases or ConditionsДокумент3 страницыDiseases or ConditionsRao SahabОценок пока нет
- Short Arm Circular CastДокумент4 страницыShort Arm Circular CastJoy Kristine PanganОценок пока нет
- Definition: Is A Condition Resulting in Partial or Complete Separation of A Segment of Normal Hyaline Cartilage From It's Supporting BoneДокумент8 страницDefinition: Is A Condition Resulting in Partial or Complete Separation of A Segment of Normal Hyaline Cartilage From It's Supporting BoneKarla Chariz Fernandez BayagОценок пока нет
- AnatomyДокумент22 страницыAnatomygggghcОценок пока нет
- Shoulder 6 ExaminationДокумент21 страницаShoulder 6 ExaminationAnil SoodОценок пока нет
- Knee Disorders, A Simple Guide To The Condition, Diagnosis, Treatment And Improvised TreatmentsОт EverandKnee Disorders, A Simple Guide To The Condition, Diagnosis, Treatment And Improvised TreatmentsОценок пока нет
- Herniated Nucleus PulposusДокумент5 страницHerniated Nucleus PulposusNestle FolienteОценок пока нет
- Posterior Dislocation of The Hip JointДокумент25 страницPosterior Dislocation of The Hip JointadibahОценок пока нет
- Lower Limb InjuriesДокумент47 страницLower Limb InjuriesDaisyyhyОценок пока нет
- 15 - Common Shoulder DisordersДокумент70 страниц15 - Common Shoulder DisordersSyafaringga Dian oscarОценок пока нет
- Sports Injuries in UE - Shoulder - Part 3.Документ87 страницSports Injuries in UE - Shoulder - Part 3.salmankhan09215Оценок пока нет
- Gadline PrsentationДокумент12 страницGadline PrsentationsumardiОценок пока нет
- Anomalies of Skeletal System-1Документ44 страницыAnomalies of Skeletal System-1Meena KoushalОценок пока нет
- REFERAT Lumbar Compression FractureДокумент25 страницREFERAT Lumbar Compression FractureTaufik Ghockil ZlaluwОценок пока нет
- Clavicle FractureДокумент33 страницыClavicle FractureNitin AggarwalОценок пока нет
- Healthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesОт EverandHealthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesРейтинг: 2 из 5 звезд2/5 (1)
- Orthopedic Surgery: Fracture and DislocationДокумент8 страницOrthopedic Surgery: Fracture and DislocationAhmad Samim AfsharОценок пока нет
- A Simple Guide to The Posture, Spine Diseases and Use in Disease DiagnosisОт EverandA Simple Guide to The Posture, Spine Diseases and Use in Disease DiagnosisОценок пока нет
- Shoulder Dislocations: Prepared By: Jalil AhmadДокумент14 страницShoulder Dislocations: Prepared By: Jalil AhmadJalil AhmadОценок пока нет
- Knee Dislocation, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandKnee Dislocation, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Pelvis and HipДокумент90 страницPelvis and Hipalsead798Оценок пока нет
- Snapping Hip Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandSnapping Hip Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Ankle Fractures: Winda Alviranisa/20204010293 Pembimbing: Dr. Muhammad Pandu Nugraha, SP - OTДокумент28 страницAnkle Fractures: Winda Alviranisa/20204010293 Pembimbing: Dr. Muhammad Pandu Nugraha, SP - OTwinda alviraОценок пока нет
- Fractures and Dislocations of The Upper LimbДокумент57 страницFractures and Dislocations of The Upper Limbمعتز فرعون100% (2)
- Hip DislocationДокумент39 страницHip DislocationSHAMENI VINODОценок пока нет
- Hip Joint DislocationДокумент19 страницHip Joint Dislocationshaoib.grandyОценок пока нет
- Applied Anatomy of Joints BY DR Iram Iqbal, PG Trainee, M Phill, AnatomyДокумент89 страницApplied Anatomy of Joints BY DR Iram Iqbal, PG Trainee, M Phill, Anatomyimmmi100% (3)
- Dislocation of Hip Joint: DR - PonnilavanДокумент38 страницDislocation of Hip Joint: DR - PonnilavanPankaj VatsaОценок пока нет
- Oxygen Carrying System: Physiology ofДокумент22 страницыOxygen Carrying System: Physiology ofJoshua Obrien100% (1)
- Sports Injury and Clinical Problem of JointsДокумент25 страницSports Injury and Clinical Problem of JointsJoshua ObrienОценок пока нет
- FMS II DEv of LimbДокумент47 страницFMS II DEv of LimbJoshua ObrienОценок пока нет
- Fisio Log I Jan TungДокумент32 страницыFisio Log I Jan TungJoshua ObrienОценок пока нет
- Excitable Tissue (Muscle) : V. Sutarmo SetiadjiДокумент40 страницExcitable Tissue (Muscle) : V. Sutarmo SetiadjiJoshua ObrienОценок пока нет
- Protein Targetting: Septelia Inawati WanandiДокумент11 страницProtein Targetting: Septelia Inawati WanandiJoshua ObrienОценок пока нет
- Suicide-ICM II 2012Документ11 страницSuicide-ICM II 2012Joshua ObrienОценок пока нет
- Antiaritmia: Frans D. Suyatna Modified by Sulistia 1010 Departemen Farmakologi & Terapeutik FKUIДокумент56 страницAntiaritmia: Frans D. Suyatna Modified by Sulistia 1010 Departemen Farmakologi & Terapeutik FKUIJoshua ObrienОценок пока нет
- The Upper Limb: Musculoskeletal System BlockДокумент50 страницThe Upper Limb: Musculoskeletal System BlockJoshua ObrienОценок пока нет
- Arrhythmia Overview: Antonia Anna LukitoДокумент45 страницArrhythmia Overview: Antonia Anna LukitoJoshua ObrienОценок пока нет
- Electrical Activity of The Heart: V. Sutarmo SetiadjiДокумент16 страницElectrical Activity of The Heart: V. Sutarmo SetiadjiJoshua ObrienОценок пока нет
- Connective Tissue: Dr. Jan Tambayong, PHK Histologi FK-UPHДокумент51 страницаConnective Tissue: Dr. Jan Tambayong, PHK Histologi FK-UPHJoshua ObrienОценок пока нет
- Pathophysiology of Heart FailureДокумент51 страницаPathophysiology of Heart FailureJoshua ObrienОценок пока нет
- Extrinsic Cardiomyopathies: CardiomyopathyДокумент3 страницыExtrinsic Cardiomyopathies: CardiomyopathyJoshua ObrienОценок пока нет
- Yaws UphДокумент44 страницыYaws UphJoshua ObrienОценок пока нет
- Drugs Uses For Heart FailureДокумент45 страницDrugs Uses For Heart FailureJoshua ObrienОценок пока нет
- Drugs Uses For Heart FailureДокумент45 страницDrugs Uses For Heart FailureJoshua ObrienОценок пока нет
- Leptospirosis UPH 2Документ33 страницыLeptospirosis UPH 2Joshua ObrienОценок пока нет
- TQ Q2 Hope1Документ6 страницTQ Q2 Hope1PrudevenoОценок пока нет
- Bandaging NewДокумент26 страницBandaging Newmalyn1218100% (7)
- Basic First Aid QuizДокумент33 страницыBasic First Aid QuizIamJmlingconОценок пока нет
- Review Questions: The Journal of Bone & Joint Surgery Continuing Medical EducationДокумент8 страницReview Questions: The Journal of Bone & Joint Surgery Continuing Medical EducationРоман ТерещенкоОценок пока нет
- Science4 - Q2 - Mod2 - Causes and Treatment of Diseases of The Major Organs - ABRIDGEDДокумент8 страницScience4 - Q2 - Mod2 - Causes and Treatment of Diseases of The Major Organs - ABRIDGEDRonie PadlanОценок пока нет
- Hip Dislocation in Dogs and Cats (Wendy Brooks, DVM)Документ8 страницHip Dislocation in Dogs and Cats (Wendy Brooks, DVM)Muhammad KholifhОценок пока нет
- HOPE12 q1 Mod5 ObservesPersonalSafetyProtocol PDFДокумент21 страницаHOPE12 q1 Mod5 ObservesPersonalSafetyProtocol PDFRuben James Jamora67% (9)
- First Aid BookletДокумент37 страницFirst Aid BookletLeОценок пока нет
- Final Year Orthopedics-Dr Imran ManzoorДокумент5 страницFinal Year Orthopedics-Dr Imran ManzoorTalmeez Fatima Talmeez FatimaОценок пока нет
- Las Mapeh 9 q1 w6 PeДокумент9 страницLas Mapeh 9 q1 w6 PeJemalyn Hibaya LasacaОценок пока нет
- Legg ReductionДокумент3 страницыLegg Reductionc_r22Оценок пока нет
- Me and Science WorktextДокумент170 страницMe and Science WorktextArimJhoOlubmaraОценок пока нет
- Medical Surgical Nursing Orthopedic NursingДокумент141 страницаMedical Surgical Nursing Orthopedic Nursingroger92% (12)
- What's More: Let's Try . Sport Injury. Injury Type Causes of Injury Sprain WДокумент7 страницWhat's More: Let's Try . Sport Injury. Injury Type Causes of Injury Sprain Wjaypee sarmientoОценок пока нет
- Practical Orthopedic Examination Made Easy JP Medi 5a053bc81723dd0336da5c77Документ13 страницPractical Orthopedic Examination Made Easy JP Medi 5a053bc81723dd0336da5c77Zed HarrisОценок пока нет
- Science Grade 4 Bone InjuriesДокумент8 страницScience Grade 4 Bone InjuriesKC CerdeñaОценок пока нет
- Penanganan FrakturДокумент78 страницPenanganan FrakturelizabethmargarethОценок пока нет
- First AidДокумент15 страницFirst AidEden Martirez-VillalonОценок пока нет
- First Aid A NecessityДокумент41 страницаFirst Aid A NecessityAlfred Melvin SolivaОценок пока нет
- Toe and Foot ConditionsДокумент14 страницToe and Foot ConditionsNur InsyirahОценок пока нет
- Disorders of The Musculoskeletal SystemДокумент245 страницDisorders of The Musculoskeletal SystemFirifan DiribaОценок пока нет
- Physiology and Injuries in Sports: Unit - 7Документ33 страницыPhysiology and Injuries in Sports: Unit - 7Vansh GoyalОценок пока нет
- Performance Task in Pe 9 ReportingДокумент3 страницыPerformance Task in Pe 9 ReportingSage MonchelleОценок пока нет
- Extremity TraumaДокумент31 страницаExtremity TraumaPap Pip100% (1)
- Treatment of Instability ShoulderДокумент7 страницTreatment of Instability ShoulderMahardiniОценок пока нет
- KSM Orthopedi New1Документ20 страницKSM Orthopedi New1rspku mayongОценок пока нет
- Trauma CompleteДокумент128 страницTrauma Completeashvin_7Оценок пока нет
- PDF Da REVdoSOCCERFINALДокумент108 страницPDF Da REVdoSOCCERFINALСергей МочаловОценок пока нет
- 12 Physical Education - Physiology & Injuries in Sports - NotesДокумент10 страниц12 Physical Education - Physiology & Injuries in Sports - NotesRahul YadavОценок пока нет
- Cachero Vs ManilaДокумент6 страницCachero Vs ManilaWEDDANEVER CORNELОценок пока нет