Академический Документы
Профессиональный Документы
Культура Документы
Neuromuscular Disorders
Загружено:
anibandaso0 оценок0% нашли этот документ полезным (0 голосов)
283 просмотров39 страницNeuromuscular disorders are conditions that affect muscles, nerves, the neuromuscular junction where nerves connect to muscles, or motor neurons. They can be caused by issues in the upper or lower motor neuron pathways, the neuromuscular junction, or the muscles themselves. Common causes include trauma, vascular accidents, demyelination, neuronal degeneration, transmission defects, and membrane or metabolic muscle lesions. Clinical presentation and prognosis depends on which parts of the motor system are affected and the rate of cell loss or damage. Diagnosis involves history, physical exam, laboratory tests, electrodiagnostic studies, and sometimes muscle or nerve biopsies.
Исходное описание:
neurologi
Оригинальное название
Neuromuscular Disorders.ppt
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документNeuromuscular disorders are conditions that affect muscles, nerves, the neuromuscular junction where nerves connect to muscles, or motor neurons. They can be caused by issues in the upper or lower motor neuron pathways, the neuromuscular junction, or the muscles themselves. Common causes include trauma, vascular accidents, demyelination, neuronal degeneration, transmission defects, and membrane or metabolic muscle lesions. Clinical presentation and prognosis depends on which parts of the motor system are affected and the rate of cell loss or damage. Diagnosis involves history, physical exam, laboratory tests, electrodiagnostic studies, and sometimes muscle or nerve biopsies.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
283 просмотров39 страницNeuromuscular Disorders
Загружено:
anibandasoNeuromuscular disorders are conditions that affect muscles, nerves, the neuromuscular junction where nerves connect to muscles, or motor neurons. They can be caused by issues in the upper or lower motor neuron pathways, the neuromuscular junction, or the muscles themselves. Common causes include trauma, vascular accidents, demyelination, neuronal degeneration, transmission defects, and membrane or metabolic muscle lesions. Clinical presentation and prognosis depends on which parts of the motor system are affected and the rate of cell loss or damage. Diagnosis involves history, physical exam, laboratory tests, electrodiagnostic studies, and sometimes muscle or nerve biopsies.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 39
What is a neuromuscular disorder?
A condition affecting one or more of the
following:
-Muscles
-Nerves
-Neuromuscular junction; the area where
muscle and nerve make connection
-Motor or sensory cell-body
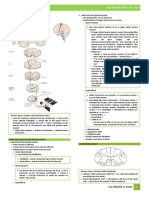
Sites of lesions producing
neuromuscular pathology
Either the upper (1,2,3)
or lower motor
neurone pathway (4,5),
N-M-J (6) or muscle (7)
may be responsible
Sites of lesions producing
neuromuscular pathology
Commonest causes trauma or vascular
accidents (1,2) or demyelination (2,3,4,5)
neuronal degeneration (4), transmission
defects (6) and membrane, fibrillary or
metabolic lesions (7).
NMJ
M
Neurone Axon
Diseases of
motor neurones
Peripheral
neuropathies
Diseases of neuromuscular
transmission
Primary muscle
disease: myopathies
~ generalised wasting & fasiculation
~ Bulbar muscle involvement common
~ Associated upper motor neurone
symptoms and signs
~ No sensory symptoms
~ Steadily progressive and fatal
Clinical presentation
Selective loss of LMN from pons, medulla and
spinal cord, together with loss of UMN from the
brain
Clinical picture varies depending on whether :
a) upper or lower motor neurones are
predominantly involved
b) Which muscles are most affected
c) The rate of cell loss
Aetiology of ALS
~ cause unknown
~ 5-10% AD and in familial cases usually starts
10 years earlier than sporadic cases
~ Mutations in the Cu/Zn superoxide dismutase
gene on Ch 21q accounts for 25% of all
familial cases
~ Mutations of the neurofilament heavy
~ Tunisian ALS uncommon AR disease linked to
2q33-q35
NMJ
M
Neurone Axon
Diseases of
motor neurones
Peripheral
neuropathies
Diseases of neuromuscular
transmission
Primary muscle
disease|: myopathies
Peripheral neuropathy
~ Axonal or demyelinating
~ Neurotransmission most impaired in long
nerves because nerve impulse confronted
by a greater number of demyelinated
segments
~ Therefore symptoms distal in distribution
~ Affects legs and feet more than arm and
hand
axon
myelin
Node of ranvier
Spinal cord
Peripheral nerve
M
1. Deficiency Vit B1 alcoholic, Vit B6 in pts taking
isoniazid, Vit B12 in patients with PA and bowel
disease
2. Toxic- Alcohol, drugs isoniazid, vincristine
3. Metabolic DM, CRF
4. Post-infectious Guillain- Barre syndrome
5. Collagen vascular RA, SLE, PA
6. Hereditary Charcot- Marie Tooth disease
7. Idiopathic Perhaps up to 50% cases
Guillain-Barre syndrome
~ Rapid evolution over several days
~ Life threatening weakness
~ Affects nerve roots as well as peripheral
nerves
~ Occurs within 2 weeks of an infection usually
campylobacter, cytomegalo, EBV
~ Auto-immune response
~ Weakness and sensory symptoms which
worsen daily for 1-2 weeks
~ Demyelinating polyneuropathy and
polyradiculopathy
Myasthenia Gravis
UMN
LMN
NMJ
M
~ Muscle weakness without wasting
~ Fatiguability
~ Ocular and bulbar muscles commonly involved
~ Responds well to treatment
Muscle disease
UMN
LMN
NMJ
M
~ Muscle weakness and wasting the distribution of which depends
on the type of disease but strong tendency to involve proximal
muscles i.e trunk and limb girdles
~ Various causes
INHERITED ACQUIRED
Muscular dystrophies Endocrinopathies
Myotonic dystrophy Drug induced
Congenital myopathies Idiopathic inflammatory
myopathy
Metabolic myopathies Metabolic myopathy
Channelopathies Myasthenia Gravis
/LEMS
Muscle weakness
Difficulty climbing stairs
Difficulty holding arms above head for a long
period of time
Congenital or acquired, can have
inflammation of the muscles
Need muscle biopsy
Steroids for inflammatory muscle disease
- Weakness
- Numbness, sharp shooting pain
- Abnormal MRI scan, myelogram, EMG/NCV
- Surgical treatment
- Physical therapy
- Medicines
History & Physical Examination
Laboratory Tests
NCV/EMG
MRI Scans
Muscle biopsy
Nerve biopsy
CONCLUSIONS
UMN lesions involving the corticospinal tract
LMN lesions involving brain stem and spinal
cord
MND may present with UMN and LMN signs
Peripheral neuropathy may be axonal or
demyelinating
Muscle disease may be inherited or acquired
Вам также может понравиться
- Stroke & Hemiplegia LocalizationДокумент54 страницыStroke & Hemiplegia LocalizationVasu PottabatthiniОценок пока нет
- VertigoДокумент50 страницVertigosaltoftheearthlightoftheworld506Оценок пока нет
- Optic Nerve PathologiesДокумент64 страницыOptic Nerve Pathologieshasan aslamОценок пока нет
- Cranial Nerve Exam Part1Документ9 страницCranial Nerve Exam Part1Jennifer Pisco LiracОценок пока нет
- Guillain-Barré Syndrome OtrДокумент5 страницGuillain-Barré Syndrome OtrMariam PlataОценок пока нет
- Biochemistry of VitaminsДокумент64 страницыBiochemistry of VitaminsConrado CatimbangОценок пока нет
- Spinal Cord Lesions: Jia Yan-Jie M.D PH.DДокумент170 страницSpinal Cord Lesions: Jia Yan-Jie M.D PH.Dapi-19916399Оценок пока нет
- Peripheral Nerve Injuries - Medical ApplicationsДокумент103 страницыPeripheral Nerve Injuries - Medical ApplicationsJune Epe100% (1)
- Brachial Plexus InjuriesДокумент64 страницыBrachial Plexus Injuriesprashanth naikОценок пока нет
- Approach To Movement Disorders ..Документ54 страницыApproach To Movement Disorders ..Ihda ParidahОценок пока нет
- Neurocutanous SyndromesДокумент3 страницыNeurocutanous SyndromesnicdeepОценок пока нет
- Neurology Multiple Choice Questions With Explanations: Volume IОт EverandNeurology Multiple Choice Questions With Explanations: Volume IРейтинг: 4 из 5 звезд4/5 (7)
- Acute Brain InjuryДокумент96 страницAcute Brain InjuryManjiwan GarchaОценок пока нет
- Cranial NeuropathiesДокумент74 страницыCranial NeuropathiesKevin Woodard100% (1)
- Pathology of Peripheral Nerve and Skeletal Muscle - DAДокумент46 страницPathology of Peripheral Nerve and Skeletal Muscle - DASinta Dewi AdityaniОценок пока нет
- Ascending TractsДокумент42 страницыAscending TractsJustine Nyangaresi100% (2)
- Gait Abnormalities: Albertus Johan Edy Paramestri Sekar Wikan Tamara Tyasning Mentor: Dr. Kamal Adib, SP - OT, M.KesДокумент21 страницаGait Abnormalities: Albertus Johan Edy Paramestri Sekar Wikan Tamara Tyasning Mentor: Dr. Kamal Adib, SP - OT, M.KesAlbertus Johan EdyОценок пока нет
- Motor Neuron DiseaseДокумент7 страницMotor Neuron DiseasegeraldineongОценок пока нет
- MigraineДокумент16 страницMigraineAbigail CruzОценок пока нет
- Mr. M. Shiva Nandha ReddyДокумент71 страницаMr. M. Shiva Nandha Reddyd kumarОценок пока нет
- Upper Motor Neuron PDFДокумент3 страницыUpper Motor Neuron PDFkevin_jawanОценок пока нет
- Neuropathic Myofascial PainДокумент18 страницNeuropathic Myofascial PainAngela PagliusoОценок пока нет
- Basic Overview of NeurologyДокумент45 страницBasic Overview of NeurologyDith Rivelta CallahanthОценок пока нет
- Neurological DisordersДокумент20 страницNeurological DisordersEdil M JamaОценок пока нет
- Approach To A Child With Coma by Dr. M. A. Rahim 2 Year PGT Paediatric MedicineДокумент64 страницыApproach To A Child With Coma by Dr. M. A. Rahim 2 Year PGT Paediatric MedicineRipan SahaОценок пока нет
- (PhysioB) Motor System II - Dr. Vila (Lea Pacis)Документ5 страниц(PhysioB) Motor System II - Dr. Vila (Lea Pacis)miguel cuevasОценок пока нет
- Guillain Barre SyndromeДокумент19 страницGuillain Barre SyndromeCrisMartAgullanaОценок пока нет
- Jaundice Biochemical ProfileДокумент64 страницыJaundice Biochemical ProfileGhaidaa SadeqОценок пока нет
- Motor Neuron DiseaseДокумент24 страницыMotor Neuron DiseasemanikantatssОценок пока нет
- Myopathies: Lecture ObjectivesДокумент15 страницMyopathies: Lecture ObjectivesanjelikaОценок пока нет
- Acute Flaccid ParalysisДокумент34 страницыAcute Flaccid ParalysisMentari Alisha100% (1)
- Disorders of Aromatic Amino AcidsДокумент6 страницDisorders of Aromatic Amino AcidsJohn Christopher LucesОценок пока нет
- Babinski and Other Pyramidal Reflexes Without VideosДокумент12 страницBabinski and Other Pyramidal Reflexes Without VideosMaurizio SeverinoОценок пока нет
- LPD - Myrin P Forte (Pakistan)Документ17 страницLPD - Myrin P Forte (Pakistan)Azeem Abbas0% (1)
- Drug-Induced Peripheral Neuropathy, A Narrative ReviewДокумент11 страницDrug-Induced Peripheral Neuropathy, A Narrative ReviewMaksum Muh MaksumОценок пока нет
- TuberculomaДокумент7 страницTuberculomaAdeleОценок пока нет
- Neuro LupusДокумент12 страницNeuro Lupusidno1008100% (2)
- 19 Neuromuscular DisordersДокумент39 страниц19 Neuromuscular DisordersSara 'Yaa SaraaОценок пока нет
- Transverse MyelitisДокумент19 страницTransverse MyelitisAnonymous YHQmN8a01100% (1)
- Okubadeja N - Epidemiology and Classification of Movement DisordersДокумент50 страницOkubadeja N - Epidemiology and Classification of Movement DisordersVictoria NatashaОценок пока нет
- Motor Neuron DiseaseДокумент8 страницMotor Neuron DiseaseyigoОценок пока нет
- Cerebellar Disorders: Dr. Mohamed Nasreldin HamdoonДокумент14 страницCerebellar Disorders: Dr. Mohamed Nasreldin HamdoonMohamed Nasreldin HamdoonОценок пока нет
- Ring Enhancing LesionsДокумент50 страницRing Enhancing LesionsVivek GuptaОценок пока нет
- Vitiligo PPT (1) .PPTX LectureДокумент35 страницVitiligo PPT (1) .PPTX LectureVinay DhranaОценок пока нет
- Meningocele & Spina BifidaДокумент21 страницаMeningocele & Spina BifidakeynechristaОценок пока нет
- Musculoskeletal Disorders Part 3 Muscular DisordersДокумент112 страницMusculoskeletal Disorders Part 3 Muscular DisordersCarmela Lacsa DomocmatОценок пока нет
- SSPEДокумент8 страницSSPEJanellah batuaan100% (1)
- Eagle's Syndrome-15-07-2015 PDFДокумент39 страницEagle's Syndrome-15-07-2015 PDFfahriitoОценок пока нет
- Approach To Ataxia: DR Jithesh R M6Документ30 страницApproach To Ataxia: DR Jithesh R M6jitheshОценок пока нет
- R.N. Kapoor Memorial Homoeopathic Hospital & Medical College, INDOREДокумент12 страницR.N. Kapoor Memorial Homoeopathic Hospital & Medical College, INDOREvinay patidar100% (1)
- Physio For Spondylolisthesis and SpondylolysisДокумент12 страницPhysio For Spondylolisthesis and SpondylolysisHasan RahmanОценок пока нет
- Rheumatoid ArthritisДокумент19 страницRheumatoid ArthritisKim GonzalesОценок пока нет
- Approach To Back PainДокумент12 страницApproach To Back PainSivaneasan KandiahОценок пока нет
- Transverse MyelitisДокумент18 страницTransverse MyelitisNaveen KumarОценок пока нет
- Approach To AtaxiaДокумент6 страницApproach To AtaxiaVivek KumarОценок пока нет
- Myopathy: By: Rey MartinoДокумент16 страницMyopathy: By: Rey Martinorey martinoОценок пока нет
- Presented By:: Ali Jaber Al-Faifi Salman NasserДокумент23 страницыPresented By:: Ali Jaber Al-Faifi Salman NasserCalvin PrasetioОценок пока нет
- ChiropracticДокумент4 страницыChiropracticYe Myint100% (1)
- Chapter 10 - Trigeminal NeuralgiaДокумент5 страницChapter 10 - Trigeminal NeuralgiaMuhammad IkbarОценок пока нет
- Carpal Tunnel SyndromeДокумент22 страницыCarpal Tunnel SyndromeAbu 'Ibby' IbrahimОценок пока нет
- Myoclonic Epilepsy With Ragged Red Fibers (MERRF)Документ32 страницыMyoclonic Epilepsy With Ragged Red Fibers (MERRF)Alok Aaron Jethanandani0% (1)
- PoliomyelitisДокумент14 страницPoliomyelitisadericky84100% (1)
- Guillain-Barré SyndromeДокумент60 страницGuillain-Barré SyndromekharaОценок пока нет
- Neuromuscular Disorders: FM Brett MD., FrcpathДокумент40 страницNeuromuscular Disorders: FM Brett MD., FrcpathNugroho HarsonoОценок пока нет
- Inflammatory Diseases of The CNSДокумент21 страницаInflammatory Diseases of The CNSMalueth AnguiОценок пока нет
- Neurology, NeuromuscularDisorders-MRyanДокумент82 страницыNeurology, NeuromuscularDisorders-MRyanFiras SawanОценок пока нет
- Diseases of Peripheral NervesДокумент46 страницDiseases of Peripheral NervesAkaОценок пока нет
- Sample # 1 of Latest CK UW Notes-2022Документ167 страницSample # 1 of Latest CK UW Notes-2022Fareena KhanОценок пока нет
- Clinical Paper Orthognathic Surgery: Int. J. Oral Maxillofac. Surg. 2015 XXX: XXX-XXXДокумент8 страницClinical Paper Orthognathic Surgery: Int. J. Oral Maxillofac. Surg. 2015 XXX: XXX-XXXRicardo BarcoОценок пока нет
- Bells Palsy Nelsons TextBook of Pediatrics 20th EditionДокумент3 страницыBells Palsy Nelsons TextBook of Pediatrics 20th EditionKRIZIA CORRINE CAINGCOY SAN PEDROОценок пока нет
- Central Post-Stroke Pain - Clinical Characteristics, Pathophysiology, and ManagementДокумент12 страницCentral Post-Stroke Pain - Clinical Characteristics, Pathophysiology, and ManagementKarimah Ihda Husna YainОценок пока нет
- Krok2 - Medicine - 2010Документ27 страницKrok2 - Medicine - 2010Badriya YussufОценок пока нет
- Indian Journal of Applied Basic Medical Science July 2011Документ79 страницIndian Journal of Applied Basic Medical Science July 2011jjvbhattinОценок пока нет
- Type of GaitsДокумент4 страницыType of GaitsSyimah UmarОценок пока нет
- Case ReportДокумент4 страницыCase ReportAnirudh AnilkumarОценок пока нет
- Steroid Dysregulation and Stomatodynia (Burning Mouth Syndrome)Документ9 страницSteroid Dysregulation and Stomatodynia (Burning Mouth Syndrome)EnzoОценок пока нет
- 10 1002@msc 1498Документ13 страниц10 1002@msc 1498Ricardo PietrobonОценок пока нет
- MDT World Press Newsletter Full PDF Vol2No3Документ19 страницMDT World Press Newsletter Full PDF Vol2No3Alexandra NadinneОценок пока нет
- Anemias (1) by DR - Hydi 3rd MBBS-2016Документ63 страницыAnemias (1) by DR - Hydi 3rd MBBS-2016Suban GouseОценок пока нет
- Module 2 - Acute Non Traumatic WeaknessДокумент55 страницModule 2 - Acute Non Traumatic WeaknessRick RanitОценок пока нет
- Guillain-Barre Syndrome Fact SheetДокумент7 страницGuillain-Barre Syndrome Fact SheetsohriaameroldimaporoОценок пока нет
- Complex Regional Pain Syndromes Differential DiagnosesДокумент11 страницComplex Regional Pain Syndromes Differential DiagnosesroboОценок пока нет
- Penodynia/Scrotodynia: Libby Edwards, MDДокумент2 страницыPenodynia/Scrotodynia: Libby Edwards, MDMarius CiobotaruОценок пока нет
- Management Discussion & Analysis For The Third Quarter of FY 2020-21Документ15 страницManagement Discussion & Analysis For The Third Quarter of FY 2020-21Echo WackoОценок пока нет
- Von Frey HairДокумент9 страницVon Frey Hair王文伶Оценок пока нет
- IDF's Diabetes AtlasДокумент160 страницIDF's Diabetes AtlasAdrian Arizmendi100% (1)
- 30 - Toronto Notes 2011 - Common Unit Conversions - Commonly Measured Laboratory Values - Abbreviations - IndexДокумент28 страниц30 - Toronto Notes 2011 - Common Unit Conversions - Commonly Measured Laboratory Values - Abbreviations - IndexRazrin RazakОценок пока нет
- Effect of Roods Approach in Diabetic PolyneuropathyДокумент6 страницEffect of Roods Approach in Diabetic Polyneuropathynandhini ragu100% (1)
- Chemotherapy Induced Peripheral Neuropathy Risk ... 2010Документ9 страницChemotherapy Induced Peripheral Neuropathy Risk ... 2010gemita aldeaОценок пока нет
- Diabetes Meet 2024 TP-Rome Italy March 11-12, 2024Документ59 страницDiabetes Meet 2024 TP-Rome Italy March 11-12, 2024David RichardОценок пока нет