Академический Документы
Профессиональный Документы
Культура Документы
Dialysis: Cresencio C. Cajigal, Jr. RN, Man
Загружено:
Mary Jane Avila Bacquial100%(7)100% нашли этот документ полезным (7 голосов)
1K просмотров32 страницыhemodialysis
Оригинальное название
Hemodialysis
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документhemodialysis
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
100%(7)100% нашли этот документ полезным (7 голосов)
1K просмотров32 страницыDialysis: Cresencio C. Cajigal, Jr. RN, Man
Загружено:
Mary Jane Avila Bacquialhemodialysis
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 32
DIALYSIS
CRESENCIO C. CAJIGAL, JR. RN, MAN
Kidney
DIALYSIS
is a procedure that
is given to people who have lost a
kidney, have kidney problems due
to birth defects, or who have
kidney failure.
A mechanical means of removing nitrogenous
waste from the blood by imitating the function
of the nephrons.
Strict aseptic care is mandatory for dialysis
clients.
TYPES OF DIALYSIS
hemodialysis
peritoneal dialysis.
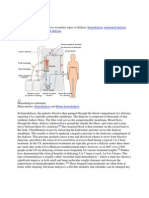
hemodialysis
A mechanical means of
removing nitrogenous waste
and excess fluid from the
blood by imitating the
function of the nephrons via
semi permeable membrane.
ACCESS FOR HEMODIALYSIS
Catheters
- jugular vein
- femoral vein
AV Fistula = anastomosis
ACCESS
HEMODIALYSIS
3x/week total of 9 to 12 hours
Dialysis orders based on body size,
renal function, dietary intake,
concurrent illness
Complications
EQUIPMENTS
Dialysis Machine
Dialysis Tubing arterial line-red
venous line-blue
IVF/IV line
Dialyzer
2 needles
2 10cc syringe
Heparin 6cc
Dialysate solution acetate, bicarbonate
Steps in Hemodialysis Process
Priming
Recirculation -15 minutes.
Dialysis process 4 hours
Termination
MOST COMMON HEMODIALYSIS
COMPLICATIONS
1. Hypotension 20 - 30%
2. Cramps 5 - 20%
3. Nausea / Vomiting 5 - 15%
4. Headache 5%
5. Chest pain 2 - 5%
6. Back pain 2 - 5%
7. Chills 1%
Definition: * Sudden drop in systolic BP to < 90 mmHg
* > 30 mmHg drop in MAP
* > 30 mmHg drop in systolic BP + symptoms
INTRADIALYTIC HYPOTENSION [IDH]
SYMPTOMS OF HYPOTENSION
1. Nausea / Vomiting
2. Cramps
3. Light headedness / dizziness
4. For some, none
INTRADIALYTIC HYPOTENSION
A. Early B. Late
1. Dialyzer volume 1. High UFR
2. Medications a. high interdialytic weight gain
3. Sepsis b. too low dry weight
4. Pericardial disease 2. Acetate dialysis
3. Autonomic neuropathy
4. Heart disease
Subgroup analysis of patients with very
frequent IDH
Co morbidities:
1. Old age
2. DM
3. Autonomic neuropathy
4. Florid uremia
5. Pericardial disease
6. Cardiac disease
a) systolic dysfxn
b) diastolic dysfxn
c) arrhythmia
VOLUME BALANCE IN HEMODIALYSIS
A. Factors decreasing intravascular
volume
1. Ultrafiltration
2. Solute removal decreased osmolality
of post dialyzer blood water moves
out into intracellular compartment
decreased plasma volume
B. Factors replenishing intravascular volume
1. Plasma refilling rate
(UF increased albumin conc. in
intravascular compartment increased
colloid oncotic pressure water moves
in from the intracellular compartment)
2. Increased cathecolamines
a. Increased vascular resistance
b. Increased HR and contractility
VOLUME BALANCE IN HEMODIALYSIS
II. Venous capacity
A. Acetate induced venodilatation
B. Dialysate temperature
C. Food ingestion
D. Dialysate sodium
DIALYSIS-RELATED IMPAIRMENT TO
COMPENSATORY RESPONSES
IV. Vascular resistance
A. Anemia
B. Acetate
C. Temperature
D. Food ingestion
E. Sodium
F. Potassium
G. Calcium
H. Dialyzer membrane
I. Drugs
DIALYSIS-RELATED IMPAIRMENT TO
COMPENSATORY RESPONSES
Strategy to help prevent hypotension during dialysis
1. Use a dialysis machine with an ultrafiltration
controller whenever possible.
2. Counsel patient to limit salt intake, which will result
in a lower interdialytic weight gain, ideally <1 kg / d.
3. Do not ultrafilter to below patients dry weight.
4. Keep dialysis solution sodium level at or above the
plasma level or use sodium gradient dialysis
(controversial).
5. Give daily dose of antihypertensive medications after,
not before, dialysis.
COMMENTARY: Dialysate Sodium
1. Low Dialysate Na increased generation of PGE 2
2. Warning: Never use a dialysate Na lower than the
patients Na. Risk of cerebral edema
3. Sodium profiling: linear, exponential, ramped
4. Recommendations: a) High Na (144 150)
b) Sodium profiling
6. Use bicarbonate containing dialysis solution
7. In selected patients, try lowering the dialysis
solution temperature to 34 36C.
8. Ensure the hematocrit is > 33% prior to
dialysis.
9. Do not give food or glucose orally during
dialysis to hypotension prone patients.
10. Consider use of blood volume monitor.
11. Consider use of -adrenergic agonists
(midodrine) prior to dialysis.
Strategy to help prevent hypotension during dialysis
1. Obligatory increase in splanchnic blood
flow
2. Lasts for 2 hours
3. No food intake during dialysis is
recommended only to those prone to
IDH
COMMENTARY: .Food Ingestion
MANAGEMENT OF DIALYSIS HYPOTENSION
A. Improve cardiac filling
1. Expand intravascular volume [ 0.9 NSS /colloid bolus]
2. Increase plasma refilling [ hypertonic saline / glucose ]
B. Supportive
1. Decrease UFR
2. Trendelenburg position
3. Oxygen
4. Decrease BFR *( ? )
TROUBLE SHOOTING DIALYSIS COMPLICATIONS
PROBLEM MECHANISM PREVENTION TREATMENT
1. Cramps
2.Dysequilibrium
syndrome
a. hypotension 1. correct hypotension a. 0.9 NSS
b. px below dry 2. correct dry weight b. hypertonic glucose
weight c. hypertonic saline
c. low sodium 3. sodium profilling*
dialysate 4. higher sodium
5. vitamin E 400 iu hs
6. Carnitine
7. Quinine
8. Oxazepam
a. cerebral edema 1. slow initial BFR a. supportive
b. cellular acidosis 2. limit initial UFR b. hypertonic glucose
3. mannitol c. hypertonic saline
4. sodium profiling
TROUBLE SHOOTING DIALYSIS COMPLICATIONS
PROBLEM MECHANISM PREVENTION TREATMENT
3. Dialysis
associated
hypoxemia
4. Conductivity
a. metabolic alkalosis 1. identify pxs at risk a. terminate HD
b. complement 2. higher O2 b. ventilate px
activation 3. hydrocortisone*
a. high 1. check system a. correct it
- low water
b. low 1. check system a. correct it
- empty dialysate
- defective proportioning
pump
c. wrong dialysate 1. pre HD check a. get a good
combination lawyer
TROUBLE SHOOTING DIALYSIS COMPLICATIONS
PROBLEM MECHANISM PREVENTION TREATMENT
5. Arterial
pressure
a. High 1. Insertion technique a. repositioning/
- needle/catheter 2. periodic AVF Doppler reinsertion
positioning assessment b. tourniquet
- AVF flow
(arterial)
- hypotension
b. Low 1. pre HD check a. eliminate air and
- disconnected 2. WOF air embolism reconnect
lines
TROUBLE SHOOTING DIALYSIS COMPLICATIONS
PROBLEM MECHANISM PREVENTION TREATMENT
6. Venous
pressure
a. High 1. periodic AVF Doppler a. NSS flushing
- AVF pressure assessment b. readjust BFR
- high BFR 2. reassess anticoag. (too fast vs. too slow)
- clotting in system protocols
- kinked tubings 3. target best BFR
b. Low 1. WOF air embolism a. eliminate air and
- disconnected lines reconnect
Peritoneal dialysis
Continuous ambulatory peritoneal
dialysis (CAPD)
2 liters dialysate, replaced every 4-6
hours
Continuous cyclic peritoneal dialysis
(CCPD
Peritoneal dialysis
In evaluating a client's understanding
of administration of peritoneal dialysis
which client action would require an
intervention by the nurse?
The client warms the dialysate before starting the
infusion.
The client uses soap and water to clean ports
before connecting to dialysis tubing.
The client weighs himself before starting process
The client wears sterile gloves when
connecting/disconnecting the tubing
Peritoneal dialysis
A client with chronic renal failure is
undergoing peritoneal dialysis. Which nursing
measure will be most helpful in promoting
outflow drainage of the dialyzing solution?
Turn the client from side to side.
Elevate the height of the dialysate bag.
Apply manual pressure to the clients lower
abdomen.
Push the peritoneal catheter in approximately one
inch further.
Вам также может понравиться
- Hemodialysis Training NotesДокумент77 страницHemodialysis Training NotesLester Dalanon94% (16)
- Chicago Review Press NCLEX-PN Practice Test and ReviewОт EverandChicago Review Press NCLEX-PN Practice Test and ReviewРейтинг: 4 из 5 звезд4/5 (4)
- DialysisДокумент157 страницDialysisKaran Dhingra100% (14)
- Kidney Dialysis ExamДокумент30 страницKidney Dialysis Examlouie roderos100% (2)
- Dialysis ExamДокумент10 страницDialysis ExamEljhae AquinoОценок пока нет
- Hemodialysis PDFДокумент880 страницHemodialysis PDFmmm777maribel100% (2)
- Dialysis Notes 1Документ3 страницыDialysis Notes 1SarahSigrid88% (24)
- HemodialysisДокумент120 страницHemodialysissigmundmaharajanОценок пока нет
- Complications of Hemodialysis and Their Management For NursingДокумент10 страницComplications of Hemodialysis and Their Management For Nursingroserem2000100% (1)
- HaemodialysisДокумент98 страницHaemodialysisKo Zin100% (1)
- Potri Hafisah B. Macadaya Group 2 BSN 3Документ26 страницPotri Hafisah B. Macadaya Group 2 BSN 3Marivic Diano100% (2)
- DIALYSISДокумент7 страницDIALYSISIvy E. LantapeОценок пока нет
- Dialysis: Dr. Frank EdwinДокумент50 страницDialysis: Dr. Frank EdwinASHRAFQOTMOSH100% (2)
- Hemodialysis and Peritoneal DialysisДокумент57 страницHemodialysis and Peritoneal Dialysisirene joy91% (11)
- Complications of DialysisДокумент26 страницComplications of DialysisrlinaoОценок пока нет
- Hemodialysis Training by RENAPДокумент1 страницаHemodialysis Training by RENAPFilipino Nurses CentralОценок пока нет
- Dialysis PresentationДокумент21 страницаDialysis PresentationRon Anderson100% (1)
- Hemodialysis Catheter InfectionДокумент38 страницHemodialysis Catheter InfectionKavidu KeshanОценок пока нет
- HemodialysisДокумент58 страницHemodialysisPamela Joy Seriosa100% (1)
- KDOQI Clinical Practice Guideline Hemodialysis Update - Public Review Draft FINAL - 20150204 PDFДокумент78 страницKDOQI Clinical Practice Guideline Hemodialysis Update - Public Review Draft FINAL - 20150204 PDFศักดิ์ชัย พูนศรีเจริญกุลОценок пока нет
- Complications of DialysisДокумент7 страницComplications of DialysisDilessandro PieroОценок пока нет
- Dialysis PrescriptionДокумент23 страницыDialysis PrescriptionMercy Juliana Jacqualine100% (1)
- HemodialysisДокумент9 страницHemodialysisKristine Artes Aguilar100% (2)
- DIALYSIS ReportingДокумент10 страницDIALYSIS ReportingGlenelyn Grace InfanteОценок пока нет
- DIALYSIS ProcedureДокумент8 страницDIALYSIS ProcedureRaman SamraoОценок пока нет
- HemodialysisДокумент28 страницHemodialysischarlenetan18100% (6)
- Complications During Hemodialysis2007Документ40 страницComplications During Hemodialysis2007Gumarbio Setiadi ZakariaОценок пока нет
- 2013 Dialysis Tech Study Guide PDFДокумент2 страницы2013 Dialysis Tech Study Guide PDFZH. omg sarОценок пока нет
- DialysisДокумент34 страницыDialysisdaisy100% (2)
- Complications Dialysis 12 09Документ47 страницComplications Dialysis 12 09irish_meg316557100% (2)
- Myths of DialysisДокумент26 страницMyths of DialysisSijo Muthukad M100% (1)
- Post Dialysis Nursing CareДокумент2 страницыPost Dialysis Nursing CareEugene Noscal Jr.100% (4)
- DIALYSISДокумент30 страницDIALYSISHecel Olita75% (4)
- Complication of Hemodialysis and Their ManagementДокумент52 страницыComplication of Hemodialysis and Their ManagementRetno SumaraОценок пока нет
- HemodialysisДокумент19 страницHemodialysisK.R.Raguram88% (26)
- Hemodialysis 1Документ25 страницHemodialysis 1Jasmine KaurОценок пока нет
- Dialysis Notes 1Документ3 страницыDialysis Notes 1Kavidu KeshanОценок пока нет
- DialysisДокумент19 страницDialysisSachin Singh100% (2)
- Dialysis DocumentДокумент3 страницыDialysis DocumentLucelle ArellanoОценок пока нет
- Management of Extracorporeal Passage of The Patient'S Blood Through A DialyzerДокумент18 страницManagement of Extracorporeal Passage of The Patient'S Blood Through A DialyzerRhonaJadeОценок пока нет
- HemodialysisДокумент22 страницыHemodialysisAlyssa Agravante100% (3)
- Hemodialysi S: Ariane Jake C. Fernandez, RN, MSNДокумент37 страницHemodialysi S: Ariane Jake C. Fernandez, RN, MSNMicah Alexis Candelario100% (3)
- Hemodialysis: Navigation SearchДокумент14 страницHemodialysis: Navigation SearchepingОценок пока нет
- DialysisДокумент32 страницыDialysisRalph Asura UchihaОценок пока нет
- Dialysis (Hemodialysis and Peritoneal)Документ63 страницыDialysis (Hemodialysis and Peritoneal)Qeely100% (2)
- Care For Dialysis PatientsДокумент18 страницCare For Dialysis PatientsHemanth PrakashОценок пока нет
- 2018 - ICRU 83 - BaliДокумент86 страниц2018 - ICRU 83 - BalisanggamОценок пока нет
- HemodialysisДокумент13 страницHemodialysisEthel Gretchen Casalla100% (2)
- Clinical Presentation On HemodialysisДокумент37 страницClinical Presentation On HemodialysisSanvar Mal SoniОценок пока нет
- Peritoneal DialysisДокумент31 страницаPeritoneal Dialysisapi-372245489% (9)
- Core Curriculum For The Dialysis Nurse - Module 1Документ7 страницCore Curriculum For The Dialysis Nurse - Module 1green_archerОценок пока нет
- Hemodialysis Training ProgramДокумент5 страницHemodialysis Training Programsakuraleeshaoran100% (1)
- Dialysis: Acute Dialysis Is Indicated When There Is A High and Rising Level of SerumДокумент19 страницDialysis: Acute Dialysis Is Indicated When There Is A High and Rising Level of SerumMJ Amarillo100% (1)
- Renal NursinglДокумент36 страницRenal NursinglgireeshsachinОценок пока нет
- Hemodialysis, Phosphorus and Calcium, Peritoneal DialysisДокумент29 страницHemodialysis, Phosphorus and Calcium, Peritoneal DialysisTrizha MaeОценок пока нет
- How Does Hemodialysis WorkДокумент19 страницHow Does Hemodialysis WorkMaxence KouessiОценок пока нет
- TypesДокумент3 страницыTypesProser Faith TabaculdeОценок пока нет
- Peritoneal DialysisДокумент23 страницыPeritoneal Dialysismakyofrancis20Оценок пока нет
- NCM 118 - Lesson 15 (Chronic Renal Failure and Dialysis)Документ7 страницNCM 118 - Lesson 15 (Chronic Renal Failure and Dialysis)Bobby Christian DuronОценок пока нет
- Nursing Care of Patient On Dialysis 10Документ17 страницNursing Care of Patient On Dialysis 10Suji MerlineОценок пока нет
- Pnemonia and Cancer of The LarynxДокумент34 страницыPnemonia and Cancer of The LarynxMary Jane Avila BacquialОценок пока нет
- BIPOLAR 1 PsychopathophysiologyДокумент1 страницаBIPOLAR 1 PsychopathophysiologyMary Jane Avila BacquialОценок пока нет
- DolfenalДокумент1 страницаDolfenalMary Jane Avila BacquialОценок пока нет
- Actual NCPДокумент2 страницыActual NCPbaki0146Оценок пока нет
- Actual NCPДокумент2 страницыActual NCPbaki0146Оценок пока нет
- Bionette - SyrolightДокумент1 страницаBionette - SyrolightIsrael Exporter100% (1)
- Wolf PresentationДокумент35 страницWolf PresentationTahir Bin AbdullahОценок пока нет
- Inheritance and Selective Breeding QsДокумент27 страницInheritance and Selective Breeding QspartinpoutsamouОценок пока нет
- Paper - B Written Test Paper For Selection of Teachers: CSB 2013 English (PGT) : Subject Code: P11Документ4 страницыPaper - B Written Test Paper For Selection of Teachers: CSB 2013 English (PGT) : Subject Code: P11Amrit SinhaОценок пока нет
- Chaturvedi 2004Документ2 страницыChaturvedi 2004Umer HussainОценок пока нет
- PERIDA EMMALYN T. - BSci103-Lesson 4.2-Learning TaskДокумент5 страницPERIDA EMMALYN T. - BSci103-Lesson 4.2-Learning TaskEmmalyn PeridaОценок пока нет
- Medico Legal Aspect of DeathДокумент32 страницыMedico Legal Aspect of DeathKU RU RUОценок пока нет
- A Review On Herbal Drugs Used in The Treatment of COVID-19.Документ15 страницA Review On Herbal Drugs Used in The Treatment of COVID-19.Samiksha SarafОценок пока нет
- Homeostasis Case StudyДокумент3 страницыHomeostasis Case Studyapi-332887331Оценок пока нет
- Study Guide STH Edition: Clinical LaboratoryДокумент30 страницStudy Guide STH Edition: Clinical LaboratoryMendoza, Richelle A.Оценок пока нет
- Clinico-Microbiological Spectrum of Hemodialysis Catheter-Related Blood Stream Infections: A Concise ReviewДокумент7 страницClinico-Microbiological Spectrum of Hemodialysis Catheter-Related Blood Stream Infections: A Concise ReviewIJAR JOURNALОценок пока нет
- Dosage Chapter 1 PDFДокумент4 страницыDosage Chapter 1 PDFLena EmataОценок пока нет
- Wa0003Документ4 страницыWa0003YegaОценок пока нет
- ENERPEEL SA - Rev - 0 - 2011Документ48 страницENERPEEL SA - Rev - 0 - 2011CHONG WEI SHENGОценок пока нет
- Giardia M.SC PDFДокумент18 страницGiardia M.SC PDFRahul ChaudharyОценок пока нет
- Lab 1C PAR-Q and Health History QuestionnaireДокумент4 страницыLab 1C PAR-Q and Health History Questionnaireskyward23Оценок пока нет
- Bio Chapter 14 NotesДокумент3 страницыBio Chapter 14 NotesAvehiОценок пока нет
- A Review of Fluid and Hydration in Competitive TennisДокумент11 страницA Review of Fluid and Hydration in Competitive TennisSilvio DantasОценок пока нет
- Personal Trainer Magazine ISSUE 13Документ45 страницPersonal Trainer Magazine ISSUE 13Jesmin AraОценок пока нет
- Lal Suryakanta ManiДокумент4 страницыLal Suryakanta ManiGautam SikalwarОценок пока нет
- Msds ChosunДокумент6 страницMsds ChosunDheeraj E MohananОценок пока нет
- Neurological Complications in Lumbar Spine SurgeryДокумент9 страницNeurological Complications in Lumbar Spine SurgeryMimi SyakilaОценок пока нет
- Chapter 39: Plant Responses To Internal and External SignalsДокумент9 страницChapter 39: Plant Responses To Internal and External SignalsdarthОценок пока нет
- Cognosco, Brain Care Centre Newsletter: Summer 2013 IssueДокумент28 страницCognosco, Brain Care Centre Newsletter: Summer 2013 IssueBrain Care CentreОценок пока нет
- DAX2018790204 SpainДокумент64 страницыDAX2018790204 SpainHarsh BhattОценок пока нет
- CLD FinalДокумент17 страницCLD FinalHervis FantiniОценок пока нет
- Bivalirudin Anticoagulant1Документ6 страницBivalirudin Anticoagulant1walid hassanОценок пока нет
- Free Class Asclepio Metabolic SyndromeДокумент6 страницFree Class Asclepio Metabolic SyndromeJames BudiantoОценок пока нет
- Nuggets Combined - Indexed + Searchable PDFДокумент478 страницNuggets Combined - Indexed + Searchable PDFjasleenОценок пока нет