Академический Документы
Профессиональный Документы
Культура Документы
Kuliah 7 PA (Dr. Al Munawir)
Загружено:
azmifalah0 оценок0% нашли этот документ полезным (0 голосов)
18 просмотров124 страницыОригинальное название
Kuliah 7 PA [Dr. Al Munawir]
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
18 просмотров124 страницыKuliah 7 PA (Dr. Al Munawir)
Загружено:
azmifalahАвторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 124
LUNGS
Blok 7 Sistem Respirasi
Al Munawir
FK Universitas Jember
The LUNG
Degenerative
Inflammatory
Neoplastic and Pleura
LAB: (Review, Cases, and/or
Virtual Microscopy)
OVERVIEW I
Normal Anatomy and Histology
Pathology
Congenital
Atalectasis
Acute Pulmonary Injury
Obstructive vs. Restrictive (infiltrative) concepts
Obstructive Pulmonary Disease (COPD)
Restrictive (Infiltrative) Pulmonary Disease
Vascular Pulmonary Diseases
OVERVIEW II
INFECTIONS
NEOPLASMS and PLEURA
(effusions, pneumothorax,
tumors)
WEIGHT
LOBES
SEGMENTS
BRONCHI
ARTERIES,
pulmonary
ARTERIES,
bronchial
VEINS
PLEURA,
visceral
PLEURA,
parietal
NERVES
Bronchi
Bronchioles
Terminal
bronchioles
Alveolar ducts
Alveoli
Type 1
pneumocytes
Type 2
pneumocytes
Macrophages
Capillaries
N
O
R
M
A
L
C
X
R
OVERVIEW
Pathology
CONGENITAL
Atalectasis
Acute Pulmonary Injury
Obstructive vs. Restrictive (infiltrative) concepts
Obstructive Pulmonary Disease (COPD)
Restrictive (Infiltrative) Pulmonary Disease
Vascular Pulmonary Diseases
CONGENITAL
Agenesis/Hypoplasia
Tracheal/bronchial anomalies, i.e.,
Tracheo-Esophageal (TE) fistula
Vascular anomalies
Congenital Emphysema (idiopathic usually)
Foregut cysts
Pulmonary Artery Malformations (CPAM)
Sequestration (no connection to airways or
pulmonary arteries, but systemic!)
OVERVIEW
Pathology
Congenital
ATALECTASIS
Acute Pulmonary Injury
Obstructive vs. Restrictive (infiltrative) concepts
Obstructive Pulmonary Disease (COPD)
Restrictive Pulmonary Disease
Vascular Pulmonary Diseases
ATALECTASIS
INCOMPLETE
EXPANSION
COLLAPSE
OVERVIEW
Pathology
Congenital
Atalectasis
ACUTE PULMONARY INJURY
Pulmonary Edema
ARDS (DiffuseAlveolarDamage)
Acute Interstitial Pneumonia
Obstructive vs. Restrictive (infiltrative) concepts
Obstructive Pulmonary Disease (COPD)
Restrictive (Infiltrative) Pulmonary Disease
Vascular Pulmonary Diseases
PULMONARY EDEMA
IN-creased
venous pressure
DE-creased
oncotic pressure
Lymphatic
obstruction
Alveolar injury
ACUTE* RESPIRATORY DISTRESS
SYNDROME (ARDS or D.A.D., i.e., Diffuse
Alveolar Damage) (aka, SHOCK lung)
NON-specific pattern of lung injury
INFECTION
PHYSICAL INJURY
TOXIC
CHEMICAL
DIC
ETC
ARDS
ACUTE INTERSTITIAL
PNEUMONIA
Think of it as ARDS with NO
known etiology!
OVERVIEW
Pathology
Congenital
Atalectasis
Acute Pulmonary Injury
OBSTRUCTION vs. RESTRICTION
Obstructive Pulmonary Disease (COPD)
Restrictive (Infiltrative) Pulmonary Disease
Vascular Pulmonary Diseases
OBSTRUCTION v. RESTRICTION
OBSTRUCTION
Air or blood?
Large or small?
Inspiration or Expiration?
Obstruction is
SMALL AIRWAY
EXPIRATION
obstruction, i.e., wheezing
HYPEREXPANSION on CXR
RESTRICTION
Compliance
Infiltrative
REDUCED lung VOLUME,
DYSPNEA, CYANOSIS
REDUCED GAS
TRANSFER
GROUND GLASS on CXR
OVERVIEW
Pathology
Congenital
Atalectasis
Acute Pulmonary Injury
Obstruction vs. Restriction
OBSTRUCTIVE Pulmonary
Diseases (COPD)
Restrictive (Infiltrative) Pulmonary Disease
Vascular Pulmonary Diseases
OBSTRUCTION (cOPD)
EMPHYSEMA (almost always
chronic)
CHRONIC BRONCHITIS
emphysema
ASTHMA
BRONCHIECTASIS
EMPHYSEMA
COPD, or END-STAGE lung disease
Centri-acinar, Pan-acinar, Paraseptal, Irregular
(PROGRESSIVE) EXPIRATORY AIR TRAPPING,
i.e., WHEEZING
Like cirrhosis, thought of as END-STAGE of
multiple chronic small airway obstructive
etiologies
NON-specific
IN-creased crepitance, BULLAE (BLEBS)
Clinically likely to produce recurrent pneumonias,
and progressive failure
CENTRO-acinar PAN-acinar
ACINUS vs. ALVEOLUS
1) HYPER-expansion 2) flattened diaphragms (blunted),
3) bullae 4) increased lucency* (why?)
CHRONIC BRONCHITIS
INHALANTS, POLLUTION, CIGARETTES
CHRONIC COUGH
CAN OFTEN PROGRESS TO EMPHYSEMA
MUCUS hypersecretion, early, i.e. goblet cell
increase
CHRONIC bronchial inflammatory infiltrate
ASTHMA
Similar to chronic bronchitis but:
Wheezing is hallmark (bronchospasm, i.e.
wheezing)
STRONG allergic role, i.e., eosinophils, IgE,
allergens
Often starting in CHILDHOOD
ATOPIC (allergic) or NON-ATOPIC (infection)
Chronic small airway obstruction and infection
1) Mucus hypersecretion with plugging, 2)
lymphocytes/eosinophils, 3) lumen narrowing,
4) smooth muscle hypertrophy
What are the 4 classical histologic findings in bronchial asthma?
BRONCHIECTASIS
DILATATION of the BRONCHUS, associated
with, often, necrotizing inflammation
CONGENITAL
TB, other bacteria, many viruses
BRONCHIAL OBSTRUCTION (i.e., LARGE
AIRWAY, NOT SMALL AIRWAY)
Rheumatoid Arthritis, SLE, IBD (Inflammatory
Bowel Disease)
BRONCHIECTASIS
OVERVIEW
Pathology
Congenital
Atalectasis
Acute Pulmonary Injury
Obstruction vs. Restriction
Obstructive Pulmonary Diseases (COPD)
RESTRICTIVE (INFILTRATIVE)
PULMONARY DISEASES
Vascular Pulmonary Diseases
RESTRICTIVE
(INFILTRATIVE)
REDUCED COMPLIANCE, reduced gas exchange)
Are also DIFFUSE, density, crepitance
HETEROGENEOUS ETIOLOGIES
FIBROSING
GRANULOMATOUS
EOSINOPHILIC
SMOKING RELATED
PAP (Pulmonary Alveolar
Proteinosis
FIBROSING
IDIOPATHIC PULMONARY FIBROSIS (IPF)
NONSPECIFIC INTERSTITIAL FIBROSIS
CRYPTOGENIC ORGANIZING
PNEUMONIA
COLLAGEN VASCULAR DISEASES
PNEUMOCONIOSES
DRUG REACTIONS
RADIATION CHANGES
IPF (UIP)
IDIOPATHIC, i.e., not from any usual
caused, like lupus, scleroderma
FIBROSIS
NON-SPECIFIC INTERSTITIAL
PNEUMONIA
WASTEBASKET
DIAGNOSIS, of ANY
pneumonia
(pneumonitis) of
any known or
unknown etiology
FIBROSIS
CELLULAR
INFILTRATE
(LYMPHS &
PLASMA CELLS)
CRYPTOGENIC ORGANIZING
PNEUMONIA (COP)
IDIOPATHIC
BRONCHIOLITIS OBLITERANS
COLLAGEN VASCULAR
DISEASES
Rheumatoid
Arthritis
SLE (Lupus)
Progressive
Systemic Sclerosis
(Scleroderma)
PNEUMOCONIOSES
OCCUPATIONAL
COAL MINERS LUNG
DUST OR CHEMICALS OR ORGANIC
MATERIALS
Coal (anthracosis)
Silica
Asbestos
Be, FeO, BaSO4, CHEMO
HAY, FLAX, BAGASSE, INSECTICIDES, etc.
GRANULOMATOUS
SARCOIDOSIS, i.e., NON-caseating
granulomas (IDIOPATHIC)
HYPERSENSITIVITY (DUSTS,
bacteria, fungi, Farmers Lung,
Pigeon Breeders Lung)
SARCOIDOSIS
Mainly LUNG, but eye, skin or
ANYWHERE
UNKNOWN ETIOLOGY
IMMUNE, GENETIC factors
F>>M
B>>W
YOUNG ADULT BLACK WOMEN
NON-Caseating Granulomas are the RULE
Asteroid bodies within these granulomas
are virtually diagnostic, but hard to find
SMOKING RELATED
DIP
(Desquamative
Interstitial
Pneumonia)
M>>F
CIGARETTES
100% Survival
Alveolar
Macrophages
PAP (Pulmonary Alveolar
Proteinosis)
Very RARE, usually acquired
Proteinaceous Material in Alveoli
MINIMAL cellular inflammatory infiltrate
Like Pulmonary Edema, but MUCH Protein
OVERVIEW
Pathology
Congenital
Atalectasis
Acute Pulmonary Injury
Obstruction vs. Restriction
Obstructive Pulmonary Diseases (COPD)
Restrictive (Infiltrative) Pulmonary Diseases
VASCULAR PULMONARY
DISEASES
VASCULAR PULMONARY DISEASES
PULMONARY EMBOLISM (with or usually
WITHOUT infarction)
PULMONARY HYPERTENSION, leading to cor
pulmonale
HEMORRHAGIC SYNDROMES
GOODPASTURE SYNDROME
HEMOSIDEROSIS, idiopathic
WEGENER GRANULOMATOSIS
P.E.
Usually secondary to debilitated states with
immobilization, or following surgery
Usually deep leg and deep pelvic veins (DVT), NOT
superficial veins
Follows Virchows triad, i.e., 1) flow problems, 2)
endothelial disruption, 3) hypercoagulabilty
Usually do NOT infarct, usually ventilate
When they DO infarct, the infarct is hemorrhagic
Decreased PO2, acute chest pain, V/Q MIS-match
DX: Chest CT, V/Q scan, angiogram
RX: short term heparin, then long term coumadin
VQ scan
CT
CXR
GROSS
saddle
embolism
PULMONARY HYPERTENSION
COPD, CIPD (vicious cycle)
CHD (Congenital HD, increased
left atrial pressure)
Recurrent PEs
Autoimmune, e.g., PSS
(Scleroderma), i.e., fibrotic
pulmonary vasculature
VERY thickened
arteriole in pulmonary
hypertension
NORMAL pulmonary
arteriole
Narrowing causes HTN, and HTN causes narrowing! (vicious cycle)
HEMORRHAGIC SYNDROMES
GOODPASTURE Syndrome: Abs
to the alpha-3 chains of collagen
IV, GBM deposits too!
IDIOPATHIC PULMONARY
HEMOSIDEROSIS, to be
differentiated from chronic CHF
WEGENER GRANULOMATOSIS
CHF, CHRONIC
IDIOPATHIC
PULMONARY
HEMOSIDEROSIS
PNEUMONIA
COMMUNITY-ACQUIRED BACTERIAL ACUTE PNEUMONIAS (BACTERIAL)
Streptococcus Pneumoniae
Haemophilus Influenzae
Moraxella Catarrhalis
Staphylococcus Aureus
Klebsiella Pneumoniae
Pseudomonas Aeruginosa
Legionella Pneumophila
COMMUNITY-ACQUIRED ATYPICAL (VIRAL AND MYCOPLASMAL) PNEUMONIAS
(NON-BACTERIAL)
Influenza Infections
Severe Acute Respiratory Syndrome (SARS)
NOSOCOMIAL PNEUMONIA
ASPIRATION PNEUMONIA
LUNG ABSCESS
Etiology and Pathogenesis.
CHRONIC PNEUMONIA
Histoplasmosis, Morphology
Blastomycosis, Morphology
Coccidioidomycosis, Morphology
PNEUMONIA IN THE IMMUNOCOMPROMISED HOST
PULMONARY DISEASE IN HUMAN IMMUNODEFICIENCY VIRUS INFECTION
PULMONARY INFECTIONS
BASIC CONSIDERATIONS
PNEUMONIA vs. PNEUMONITIS
DIFFERENTIATION from INJURIES, OBSTRUCTIVE
DISEASES, RESTRICTIVE DISEASES, VASCULAR
DISEASES
DIFFERENTIATION FROM NEOPLASMS
CLASSICAL STAGES of INFLAMMATION
LOBAR- vs. BRONCHO-
INTERSTITIAL vs. ALVEOLAR
COMMUNITY vs. NOSOCOMIAL
ETIOLOGIC AGENTS vs. HOST IMMUNITY
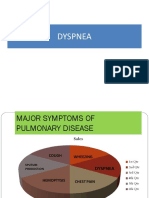
2 PRESENTING SYMPTOMS: What are they?
2 DIAGNOSTIC METHODS: What are they?
ANY ORGANISM CAN CAUSE PNEUMONIA!!!
PREDISPOSING FACTORS
LOSS OF COUGH REFLEX
DIMINISHED MUCIN or CILIA
FUNCTION
ALVEOLAR MACROPHAGE
INTERFERENCE
VASCULAR FLOW IMPAIRMENTS
BRONCHIAL FLOW IMPAIRMENTS
Although pneumonia is
one of the most
common causes of
death, it usually does
NOT occur in healthy
people spontaneously
Classifications of PNEUMONIAS
COMMUNITY ACQUIRED
COMMUNITY ACQUIRED, ATYPICAL
NOSOCOMIAL
ASPIRATION
CHRONIC
NECROTIZING/ABSCESS FORMATION
PNEUMONIAS in
IMMUNOCOMPROMISED HOSTS*
Classifications of PNEUMONIAS
COMMUNITY ACQUIRED
COMMUNITY ACQUIRED, ATYPICAL
NOSOCOMIAL
ASPIRATION
CHRONIC
NECROTIZING/ABSCESS FORMATION
PNEUMONIAS in
IMMUNOCOMPROMISED HOSTS
COMMUNITY ACQUIRED
STREPTOCOCCUS PNEUMONIAE (i.e.,
diplococcus)
HAEMOPHILUS INFLUENZAE (H-Flu)
MORAXELLA
STAPHYLOCOCCUS (STAPH)
KLEBSIELLA PNEUMONIAE
PSEUDOMONAS AERUGINOSA
LEGIONELLA PNEUMOPHILIA
STREPTOCOCCUS
The classic LOBAR pneumonia
Normal flora in 20% of adults
Only 20% of victims have + blood cultures
Penicillins are often 100% curative
Vaccines are often 100% preventive
HAEMOPHILUS PNEUMONIA
Commonest in CHILDREN <2, with
otitis, URI, meningitis, cellulitis,
osteomyelitis
PNEUMONIAS in CHILDREN <2 are
often thought of as being H Flu until
proven otherwise, otitis, meningitis too
Most common pneumonia from COPD
in adults
BACTRIM (Trimethoprim-Sulfa) most
common treatment
MORAXELLA CATARRHALIS
2nd most common COPD pneumonia,
after haemophilus
Gram NEGATIVE coccobacillus, like H.
Flu
STAPH aureus
Most common pneumonia
following viral pneumonias
M.R.S.A., of course, is usually
NOT community acquired
KLEBSIELLA PNEUMONIAE
DEBILITATED
MALNOURISHED PEOPLE
ALCOHOLICS with
pneumonia are often thought
of as having Klebsiella until
proven otherwise
PSEUDOMONAS Aeruginosa
Usually NOT community acquired
but nosocomial
CYSTIC FIBROSIS patients with
pneumonia are presumed to have
PSEUDOMONAS until proven
otherwise
LEGIONELLA (pneumophila)
Often in OUTBREAKS
Often LOBAR
Spread by water droplets
Often immunosuppressed patients,
but remember..*
Although pneumonia is
one of the most
common causes of
death, it usually does
NOT occur in healthy
people spontaneously
MORPHOLOGY
ACUTE
ORGANIZING
CHRONIC
FIBROSIS vs. FULL RESOLUTION
HEPATIZATION, RED vs. GREY
CONSOLIDATION
INFILTRATE, XRAY vs. HISTOPATH
Loss of CREPITANCE
Classifications of PNEUMONIAS
COMMUNITY ACQUIRED
COMMUNITY ACQUIRED,
ATYPICAL
NOSOCOMIAL
ASPIRATION
CHRONIC
NECROTIZING/ABSCESS FORMATION
PNEUMONIAS in IMMUNOCOMPROMISED
HOSTS
COMMUNITY ACQUIRED, (atypical)
VIRAL (INFLUENZA)
MYCOPLASMAL (MYCOPLASMA
PNEUMONIAE (obligate intracellular))
NOT BACTERIAL
CULTURES NOT HELPFUL
VIRAL PNEUMONIAS
Frequently interstitial, NOT alveolar
INFLUENZA VIRUS
A,B,C
1915, 1918, PAN-demics, type A
Has MUTATED throughout history,
many STRAINS, avian swine, etc.
B and C in children
Exact strains can be IDs by PCR
SARS
(Severe Acute Respiratry Syndrome)
CORONA-VIRUS
2002 China outbreak
Spread CHIEFLY in Asia
Like most other NON-bacterial
pneumonias confirmed by PCR
Like most viral pneumonias,
interstitium infiltrated, some giant
cells often present
S
A
R
S
Classifications of PNEUMONIAS
COMMUNITY ACQUIRED
COMMUNITY ACQUIRED, ATYPICAL
NOSOCOMIAL
ASPIRATION
CHRONIC
NECROTIZING/ABSCESS FORMATION
PNEUMONIAS in
IMMUNOCOMPROMISED HOSTS
NOSOCOMIAL
Acquired in HOSPITALS, also called hospital acquired,
versus community acquired pneumonias.
DEBILITATION
CATHETERS, VENTILATORS
ENTEROBACTER, PSEUDOMONAS
STAPH (MRSA)
MRSA (MR=Methicillin Resistant)
OTHER Common causes of Noso. Pneum.
P. aeruginosa
Klebsiella
E. coli
S. pneumoniae
H. influenzae
Classifications of PNEUMONIAS
COMMUNITY ACQUIRED
COMMUNITY ACQUIRED, ATYPICAL
NOSOCOMIAL
ASPIRATION
CHRONIC (often granulomatous)
NECROTIZING/ABSCESS FORMATION
PNEUMONIAS in
IMMUNOCOMPROMISED HOSTS
ASPIRATION PNEUMONIAS
UNCONSCIOUS PATIENTS
PATIENTS IN PROLONGED BEDREST
LACK OF ABILITY TO SWALLOW OR GAG
USUALLY CAUSED BY ASPIRATION OF
GASTRIC CONTENTS
POSTERIOR LOBES (gravity dependent)
MOST COMMONLY INVOLVED,
ESPECIALLY THE SUPERIOR SEGMENTS of
the LOWER LOBES
Often lead to ABSCESSES
LUNG ABSCESSES
ASPIRATION
SEPTIC EMBOLIZATION
NEOPLASIA
From NEIGHBORING structures:
ESOPHAGUS
SPINE
PLEURA
DIAPHRAGM
ANY pneumonia which is severe and
destructive, and UN-treated enough
Classifications of PNEUMONIAS
COMMUNITY ACQUIRED
COMMUNITY ACQUIRED, ATYPICAL
NOSOCOMIAL
ASPIRATION
CHRONIC
NECROTIZING/ABSCESS FORMATION
PNEUMONIAS in
IMMUNOCOMPROMISED HOSTS
CHRONIC Pneumonias
USUALLY NOT persistences of the
community or nosocomial bacterial
infections, but CAN BE, at least
histologically
Often SYNONYMOUS with the 4 classic
systemic fungal or granulomatous
pulmonary infections infections, i.e., TB,
Histo-, Blasto-, Coccidio-
If you see pulmonary granulomas, think of a
CHRONIC process, often years
CHRONIC Pneumonias
TB
HISTO-PLASMOSIS
BLASTO-MYCOSIS
COCCIDIO-MYCOSIS
HISTOPLASMOSIS
Spores in bird or bat droppings
Mimics TB
Histoplasma CAPSULATUM
Pulmonary granulomas, often large and
calcified
Tiny organisms live in macrophages
Ohio, Mississippi valley
MANY other organs
can be affected
BLASTOMYCOSIS
Spores in soil
Mimics TB, like ALL the granulomatous lung
dideases do.
Blastomyces DERMATIDIS
Pulmonary granulomas, often large and
calcified
Large distinct SPHERULES (larger than
coccidio)
Ohio, Mississippi valley, Great Lakes,
WORLDWIDE
MANY other organs can be affected,
especially SKIN
COCCIDIOMYCOSIS
Spores in soil
Mimics TB
Coccidioides IMMITIS
Pulmonary granulomas, often large and
calcified
Smaller spherules than blasto.
Tiny organisms live in macrophages
American SOUTHWEST
MANY other organs can be affected
GRANULOMA
COMPROMISED HOSTS
PNEUMOCYSTIS CARINII*
CYTOMEGALOVIRUS (CMV)
FUNGI
PCP
Methenamine SILVER
stain for
Pneumocystis carinii*
WOOLY?
LUNG TRANSPLANTATION
EMPHYSEMA
Pulmonary Fibrosis
Cystic Fibrosis
Pulmonary Hypertension
Any end-stage lung disease in which the patient can tolerate
long term immunosuppression, and often just ONE lung is
enough, donors very SCARCE!
Lung Transplant Pathology
Infections (patients are on
immunosuppressives )
Bacterial
Viral (CMV)
Fungal
PCP
ACUTE rejection, pneumonias, usually
weeks to months
CHRONIC rejection, HALF of all patients by
3-5 years, bronchiolitis obliterans (COP)
LUNG TUMORS
Benign, malignant, epithelial, mesenchymal,
but 90% are CARCINOMAS
BIGGEST USA killer. Why? Ans: Prevalence
not as high as prostate or breast but
mortality higher. Only 15% 5 year survival.
TOBACCO has polycyclic aromatic
hydrocarbons, such as benzopyrene,
anthracenes, radioactive isotopes
Radiation, asbestos, radon
C-MYC, K-RAS, EGFR, HER-2/neu
PATHOGENESIS
NORMAL BRONCHIAL
MUCOSA
METAPLASTIC/DYSPLASTIC
MUCOSA
CARCINOMA-IN-SITU
(squamous, adeno)
INFILTRATING (i.e.,
INVASIVE) cancer
TWO TYPES
NON-SMALL CELL
SQUAMOUS CELL CARCINOMA
ADENOCARCINOMA
LARGE CELL CARCINOMA
SMALL CELL CARCINOMA
The BIG list
Squamous cell carcinoma
Small cell carcinoma
Combined small cell carcinoma
Adenocarcinoma: Acinar, papillary,
bronchioloalveolar, solid, mixed subtypes
Large cell carcinoma
Large cell neuroendocrine carcinoma
Adenosquamous carcinoma
Carcinomas with pleomorphic, sarcomatoid, or
sarcomatous elements
Carcinoid tumor: Typical, atypical
Carcinomas of salivary gland type
Unclassified carcinoma
OTHER TUMORS
T1
Tumor <3 cm without pleural or main stem bronchus involvement
T2
Tumor >3 cm or involvement of main stem bronchus 2 cm from carina,
visceral pleural involvement, or lobar atelectasis
T3
Tumor with involvement of chest wall (including superior sulcus tumors),
diaphragm, mediastinal pleura, pericardium, main stem bronchus 2 cm from
carina, or entire lung atelectasis
T4
Tumor with invasion of mediastinum, heart, great vessels, trachea,
esophagus, vertebral body, or carina or with a malignant pleural
effusion
N0 No demonstrable metastasis to regional lymph nodes
N1
Ipsi-lateral hilar or peribronchial nodal involvement
N2
Metastasis to ipsilateral mediastinal or subcarinal lymph nodes
N3
Metastasis to contra-lateral mediastinal or hilar lymph nodes, ipsilateral
or contralateral scalene, or supraclavicular lymph nodes
M0 No (known) distant metastasis
M1 Distant metastasis present
TNM, Lung
Clinical Feature Pathologic Basis
Pneumonia, abscess, lobar
collapse
Tumor obstruction of airway
Lipid pneumonia Tumor obstruction; accumulation of cellular
lipid in foamy macrophages
Pleural effusion Tumor spread into pleura
Hoarseness Recurrent laryngeal nerve invasion
Dysphagia Esophageal invasion
Diaphragm paralysis Phrenic nerve invasion
Rib destruction Chest wall invasion
SVC syndrome SVC compression by tumor
Horner syndrome Sympathetic ganglia invasion
Pericarditis, tamponade Pericardial involvement
LOCAL effects of LUNG CANCER
SYSTEMIC effects of LUNG CANCER
(PARA-NEOPLASTIC SYNDROMES)~ 5%
ADH (hyponatremia)
ACTH (Cushing)
PTH (Hyper-CA)
CALCITONIN (Hypo-CA)
GONADOTROPINS
SEROTONIN/BRADYKININ
OTHER TUMORS
METASTATIC TUMORS
LUNG is the MOST COMMON
site for all metastatic tumors,
regardless of site of origin
It is the site of FIRST CHOICE
for metastatic sarcomas for
purely anatomic reasons!
PLEURA
PLEURITIS (pleurisy)
PNEUMOTHORAX
EFFUSIONS
HYDRO-THORAX (Peric-, Perito-)
HEMO-THORAX (Peric-, Perito-)
CHYLO-THORAX (Peric-, Perito-)
MESOTHELIOMAS
PLEURITIS
Usual bacteria, viruses, etc.
Infarcts
Lung abscesses, empyema
TB
Collagen diseases, e.g., RA, SLE
Uremia
Metastatic
PNEUMOTHORAX
SPONTANEOUS, TRAUMATIC,
THERAPEUTIC
OPEN or CLOSED
TENSION pneumothorax,
valvular effect
Bleb (bulla) rupture
Perforating injuries
Post needle biopsy
EFFUSIONS
TRANSUDATE (HYDROTHORAX)
EXUDATE (HYDROTHORAX)
BLOOD (HEMOTHORAX)
LYMPH (CHYLOTHORAX)
MESOTHELIOMAS
Benign vs. Malignant
differentiation does not matter, but a
self limited localized nodule can be
regarded as benign, and a spreading
tumor can be regarded as malignant
Visceral or parietal pleura, pericardium,
or peritoneum
Most are regarded as asbestos caused
or asbestos related
EM
H&E,
IMMUNOCHEMISTRY
(CALRETININ)
Вам также может понравиться
- Pathological Optic Disc CuppingДокумент1 страницаPathological Optic Disc CuppingazmifalahОценок пока нет
- HemianopiaДокумент5 страницHemianopiaazmifalahОценок пока нет
- Virus Hepatitis: Enny Suswati, Dr. Mkes. Lab. Mikrobiologi Fakultas Kedokteran UnejДокумент71 страницаVirus Hepatitis: Enny Suswati, Dr. Mkes. Lab. Mikrobiologi Fakultas Kedokteran UnejazmifalahОценок пока нет
- Enterobacteriaceae Biokimia TestДокумент20 страницEnterobacteriaceae Biokimia TestazmifalahОценок пока нет
- Sistem Respirasi: Muh. Ihwan NarwantoДокумент50 страницSistem Respirasi: Muh. Ihwan NarwantoazmifalahОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Oxygenation NCM 103Документ10 страницOxygenation NCM 103Marti GregorioОценок пока нет
- NP 1Документ73 страницыNP 1Aldous SerranoОценок пока нет
- SGFP Common Fee Codes 09 6REVДокумент4 страницыSGFP Common Fee Codes 09 6REVeschiuОценок пока нет
- Med Surg QuizДокумент91 страницаMed Surg QuizCharles Gerard B. Beluan0% (1)
- TB Nursing CareplanДокумент14 страницTB Nursing CareplanEstherThompson100% (1)
- Clinical Case Scenario 6Документ17 страницClinical Case Scenario 6Sean Menard Flores100% (1)
- Nursing Care Plan For Ineffective Airway ClearanceДокумент6 страницNursing Care Plan For Ineffective Airway ClearanceCaroline ChaОценок пока нет
- COPD DOH GuidelinesДокумент20 страницCOPD DOH Guidelinesqariasif1900Оценок пока нет
- Shortness of BreathДокумент17 страницShortness of BreathChingHuaОценок пока нет
- OSCE NotesДокумент4 страницыOSCE NotesHighschool AudiobooksОценок пока нет
- SJDH Chester Kyle Fernandez Risk AssessmentДокумент8 страницSJDH Chester Kyle Fernandez Risk AssessmentChester KyleОценок пока нет
- Buku SDKIДокумент246 страницBuku SDKIAdi Pramono100% (1)
- July PNLE 2011 PreBoard ExamДокумент9 страницJuly PNLE 2011 PreBoard ExamRon KimОценок пока нет
- 2nd Problem Emergency Medicine Block KEL 1Документ141 страница2nd Problem Emergency Medicine Block KEL 1Jonathan TandajuОценок пока нет
- Medical Revision PaperДокумент106 страницMedical Revision PaperDavin SugumarОценок пока нет
- Case Study of AsthmaДокумент6 страницCase Study of Asthmabuzz Q100% (4)
- BRONCHIAL ASTHMA Case Presentation. EditedДокумент37 страницBRONCHIAL ASTHMA Case Presentation. Edited92006770% (10)
- Test Bank For Respiratory Disease A Case Study Approach To Patient Care 3rd Edition by WilkinsДокумент10 страницTest Bank For Respiratory Disease A Case Study Approach To Patient Care 3rd Edition by Wilkinsa498226706Оценок пока нет
- Pals CasesДокумент24 страницыPals CasesPaíto San Martín100% (16)
- Pneumonia Careplan MedДокумент17 страницPneumonia Careplan MedGayatri MudliyarОценок пока нет
- The ABCDE ApproachДокумент4 страницыThe ABCDE Approachazmar3Оценок пока нет
- CDHO Factsheet AsthmaДокумент4 страницыCDHO Factsheet AsthmaIlse AnzuresОценок пока нет
- H&P TemplateДокумент6 страницH&P TemplateRicardoMelendezОценок пока нет
- PneumothoraxДокумент2 страницыPneumothoraxAfif MansorОценок пока нет
- Prenatal Care Common Discomforts During PregnancyДокумент5 страницPrenatal Care Common Discomforts During PregnancyKarina MadriagaОценок пока нет
- Health Teaching Plan DyspneaДокумент3 страницыHealth Teaching Plan DyspneaMae JavierОценок пока нет
- Nursing Care Plan Preoperative Cues Nursing Diagnosis Objectives Nursing Interventions Rationale Evaluation SubjectiveДокумент5 страницNursing Care Plan Preoperative Cues Nursing Diagnosis Objectives Nursing Interventions Rationale Evaluation SubjectiveShamsa AfdalОценок пока нет
- Mana-Ay, Virginitaagumeno: (Claim Form 4) Series # August 2018Документ2 страницыMana-Ay, Virginitaagumeno: (Claim Form 4) Series # August 2018CARES Martin Federic PalcoОценок пока нет
- RLE - Reviewer - OxygenationДокумент14 страницRLE - Reviewer - OxygenationVinzii DrtОценок пока нет
- Neoflo 1 58 bản tiếng anhДокумент17 страницNeoflo 1 58 bản tiếng anhLê CôngОценок пока нет