Академический Документы
Профессиональный Документы
Культура Документы
Hormone Replacement Therapy For Menopause
Загружено:
doctorsinternational0 оценок0% нашли этот документ полезным (0 голосов)
52 просмотров90 страницhormone replacement therapy for menopause, Natasha Cinta Vinski.
Preventive Medicine
Оригинальное название
Hormone Replacement Therapy for Menopause
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документhormone replacement therapy for menopause, Natasha Cinta Vinski.
Preventive Medicine
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
52 просмотров90 страницHormone Replacement Therapy For Menopause
Загружено:
doctorsinternationalhormone replacement therapy for menopause, Natasha Cinta Vinski.
Preventive Medicine
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 90
HORMONE REPLACEMENT
by Natasha Cinta Vinski
THERAPY FOR
MENOPAUSE
The 2012 hormone therapy position statement of the
North American Menopause Society
Objective
to update the evidence based position statement by
NAMS in 2010
regards recommendation on use of HT for post
menopause women.
further distinguishes the emerging difference in
therapeutic benefit-risk ratio between ET & EPT
at various ages & time intervals since menopause
onset
Method
expert clinicians and researchers of womens health
review the 2010 NAMS position statement, evaluate
new evidence and reach consensus
Then, reviewed and approved by NAMS
Then made an official statement.
Result
use of HT for peri- & post- menopause is supported
when the balance when the balance of potential
benefits and risk ratio is favorable for the individual.
Conclusion
Initiation of HT is supported at the time of
menopause to treat symptoms of menopause & to
prevent osteoporosis in women with high-risk of
fracture
ET has greater flexibility for duration of use than
EPT , especially if there are early signs of breast
cancer prevents the use of EPT beyond 3-5 years
physiology of
female hormones
Female Hormones
Estrogen:
Progesterone:
Luteal Phase : the earlier phase of the estrous
cycle menstrual cycle). It begins with the formation
of the corpus luteum and ends in either pregnancy
or luteolysis. The main hormone associated with this
stage is progesterone, which is significantly higher
during the luteal phase than other phases of the
cycle.[1] The opposite of the luteal phase, the rest of
the four weeks, is called the follicular phase.
follicular phase is the phase of the menstrual cycle.
during which follicles in the ovary mature. It ends
with ovulation. The main hormone controlling this
stage is estradiol.
Menopause
Perimenopause :
Menopause :
Postmenopause :
Perimenopause
Menopause
Postmenopause
symptoms
Perimenopause means around menopause. The
time period where a womans body makes its natural
transition toward permanent infertility.
can occur as long as 10 years before menopause,
where less oestrogen is produced.
Menopause symptoms may start to arise starting
from this phase; such as hot flushes, decreased
sexual arousal (lowering of libido)
Menopause is the time when a woman stops having
her monthly menstrual period which signals that her
ovaries no longer produces ovum. It is usually
defined by the time where a womans period
ceases, but some anovulatory bleeding may occur
afterwards.
But is corrected; Menopause is for sure menopause
if the woman has not had her period for at least 12
months.
Postmenopause is the time period after menopause.
ovaries degenerate causing less hormone production
hormones beneficial for human health.
Anovulatoir Bleeding
normal menses have intervals of 4 weeks or 28 days (but
21-35 days is still normal, if regular)
anovulatoir : >35 - 180 days interval = oligomenorhea
or even amenorrhea = menses stop
mennorhagia: abnormally heavy and prolonged
menstrual period at regular intervals.
metrorrhagia: uterine bleeding at irregular intervals,
particularly between the expected menstrual periods.
Normal menstrual bleeding in ovulatory cycle is a result of
decline in progesterone due to the demise of corpus luteum =
progesterone withdrawal bleeding.
no progesterone in anovulatory cycle =bleeding is caused by
the inability of estrogen - that needs to be present to stimulate
the endometrium in the first place - to support a growing
endometrium.
Anovulatory bleeding is hence termed estrogen
breakthrough bleeding.
Perimenopause symptoms
Some of the most common :
Fatigue
Loss of libido
Weight gain
Depression
Hot flashes
Night sweats
Mood swings
Vaginal dryness
Irritability
androsteneidone: Androstenedione is a hormone that is produced in the gonads of men, the ovaries of women, and the
adrenal glands of both genders. It is produced in people before the appearance of either testosterone or estrogen. In males,
androstenedione is converted to testosterone using the enzyme 17-hydroxysteroid dehydrogenase. For females, the enzyme
aromatase is used to covert this hormone into estrogen. This compound is also known as a prohormone, which is a precursor
substance that leads to hormone production, but lacks many of the functional qualities of a true hormone.
conversion of cholesterol
Aldosterone: steroid hormone (mineralocorticoid
family) produced by the outer section (zona
glomerulosa) of the adrenal cortex in the adrenal
gland.[1][2] It plays a central role in the regulation of
blood pressure mainly by acting on the distal tubules
and collecting ducts of the nephron, increasing
reabsorption of ions and water in the kidney, to
cause the conservation of sodium, secretion of
potassium, increased water retention, and increased
blood pressure
Cortisone : It is one of the main hormones released by the
adrenal gland in response to stress. They elevate blood
pressure and prepare the body for a fight or flight response.
Also used to reduce pain.
types of HT
ET
EPT
Estradiol can oppose ageing of
organs by:
opposing age-related increase
of free radicals thanks to potent
antioxidant activity.
preventing unwanted cross-
linking of protein.
reducing damage and
accelerating repair of tissues.
stimulating the immune system.
increasing number of viable
fibroblast.
opposing telomere shortening.
Progesterone can oppose
senescent processes by:
improving immune resistance
in certain conditions.
by increasing the number of
viable fibroblast.
BENEFITS & RISKS
of hormone replacement
therapy
Why bad effects?
Imbalance, High Dosage, Synthetic and wrong
administration.
Vasomotor Symptoms
ET with or without progesterone is the most effective
treatment of menopause-related vasomotor symptoms
& their potential consequences.
All ET and EPT Hormone Therapy have government
approval for treating moderate to severe vasomotor
symptoms except for low-dose transdermal estradiol
progesterone also reduces vasomotor symptoms but not
as effectively as estrogen.
Vaginal Symptoms
ET is the most effective treatment for moderate-
severe vaginal symptoms of vulvar and vaginal
atrophy.
many systemic HT products and local ET have
government approval.
low dose systemic regimens may be inadequate,
and needs addition of low dose vaginal ET to meet
requirements
Progestogen is not indicated when ET at
recommended low doses is administered locally.
Though clinical trial data supporting endometrial
safety beyond 1 year is lacking.
endometrial hyperplasia increases with increasing
dose and duration of oestrogen.
thorough evaluation of women using low-dose ET is
advised
Sexual Function
Current evidence does not support ET giving a
significant effect on sexual interest, arousal &
orgasmic response
Independent from its role in treating menopausal
symptoms
Low dose local ET may improve sexual satisfaction
by increasing lubrication and increasing blood flow
and sensation in vaginal tissue.
according to WHI, HT was not correlated with longer
persistence of sexual activity.
Libido treatment might be recommended better to
solve this case.
Urinary Tract Health
Local ET may benefit some women with overactive bladder.
An RCT found that an estradiol ring had a clinical benefit
equivalent to oxybutin in this case.
SYSTEMIC HT may prove or worsen stress incontinence.
Ultra-low dose of transdermal estradiol therapy gives no effect.
1 RCT found that HT may increase risk of kidney stones.
2 studies have found that decreased risk of UTI with intra-
vaginal oestrogen.
Only intra-vaginal ET has been shown to be
effective.
No HT product has government approval for this.
Quality of Life
Can be affected by other menopausal symptoms such
as Vasomotor Symptoms.
No HT has government approval for enhancing QOL but
there is an improvement for health-related QOL in
women through alleviation symptoms.
No HT has been proved to improve HQOL in
asymptomatic women.
WHI found no benefit of HT in women >65 years when
measured for grip strength, chair standing and walking.
Osteoporosis
RCT evidence states that standard-dose HT reduces post-
menopausal osteoporotic fractures; hip, spine and all non-spine.
low dose > effective in maintaining/improving bone density. WHY?
No HT product has government approval for osteoporosis.
Many Systemic HT products have government approval for
prevention of postmenopausal osteoporosis.
Mostly used when alternate osteoporosis therapies are inappropriate
and cause adverse effects.
extended use of HT is an option for women with high risk of
osteoporotic fractures.
Cardiovascular disease
Coronary Heart Disease
Stroke
Venous Thromboembolism
Coronary Heart Disease
Most observed studies support the use of HT for
CHD. But most RCTs do not.
Stroke
WHI trials on ET and EPT increased risk of ischemic
stroke and no effect on haemmoraghic stroke.
8 additional strokes per 10000 women per year of EPT
11 additional strokes per 10000 women per year of ET
But in younger women (50-59 years) sowed no effect
on stroke.
But inaccurate because the exact age of menopause
onset was unclear
Venous Thromboembolism
increased risk with oral HT
For obese women even higher risk (3x)
With BMI increase , risk of use of HT increase
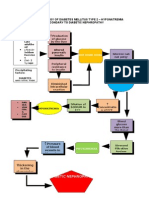
Diabetes Mellitus
Reduces risk of type 2 diabetes
21% reduction with combined HT
but the studies dont include oral glucose tolerance
Endometrial Cancer
systemic ET in postmenopausal women with intact
uterus shows increased risk of Endometrial cancer.
especially in use >10 years
risk still increases after a few years after
discontinuation of use.
Breast Cancer
Estrogen-Progesterone Therapy
Estrogen Therapy
HT after breast cancer
Estrogen-Progesterone Therapy
increase risk with use of HT for 3-5 years
Studies do not differ between continuous and
sequential use of progesterone.
increase breast cancer proliferation, pain and
mammography density
caused by promotion of preexisting cancer cells that
are too small to be diagnosed by clinical
examination.
Estrogen Therapy
No increased risk of breaast cancer in average of
7,1 years of use
A decreased risk in women 50-79 years old
the longer breast cells are oestrogen deprived, the
more probable physiologic-estrogen will cause
turmeric effects
But use >15 years showed increase risk
HT after breast cancer
Reccurence may occur
Ovarian Cancer
No elevated risk
Lung Cancer
Increased in past and current smokers
no change in non-smokers
Mood & Depression
women with past PMS using HT may cause
decrease in mood
But ET and EPT may cause increase in mood if
balanced
Cognitive Aging & Dementia
No substantial effect on memory
Nation wide WHI research states that there is a
significant role when ET is combined with GH and
pregnenolone.
Premature Menopause &
Primary Ovarian Insufficiency
ET and EPT can help balance the female body by
manually replacing the ovarian function.
Because ET and EPT functions to rid of the post-
menopausal symptoms.
Total Mortality
HT may reduce total mortality due to well-being of
patients and well functioning of organs (just like
during the reproductive age)
Practical therapeutic
issues
CLASS vs. SPECIFIC PRODUCT
EFFECTS
all estrogens have some common features and
effects as well as potentially different properties, as
is progesterone
because its difficult to research specific oestrogen
products, this research is just based on any kind of
oestrogen therapy.
there are likely to be differences on their relative
potency, androgenicity, glucocorticoid effects,
bioavailability and route of administration.
Progesterone Indication
mainly used to negate Endometrial Cancer from
systemic ET use
any woman with a intact uterus should get
progesterone with ET
postmenopause women without a uterus should
Dose & Route of
Administration
lower doses typically used when initiating systemic
ET are 0,3 - 0,45mg oral CE.
0,5mg oral micronized 17-beta estradiol and 0,014 -
0,0375 mg transdermal 17-beta estradiol patch.
Estrogen less than the traditional prescription
(<0,625mg) often require longer duration of
treatment upon initiation to achieve maximal
efficacy.
Bioidentical Hormones
These hormones are better because they are identical to
hormones produced by the ovaries. So it is non-synthetic, thus
better accepted and metabolised correctly by our body.
Bioidentical Hormones
custom made HT formulations.
there is lack of research evidence on wether this is
safe. But most clinical trials does state so.
Why this is better than regular HT is that it is specific
for each Woman, based on their bodily needs that
are encountered by sputum tests.
But now hormone-blood tests are better at
determining a womans hormonal levels.
1. Preventive Medicine :
Vitamin : A, C , D, E, Vitamin B, Vit K and other micronutritions such as selenium, co Q10,
Chromium.
Hormones like Estradiol, progesterone, testosterone low dose
Other Hormones like ; Melatonin, it D3< Hormone of the brain, HGH and IGF-1 is essential to
reverse aging of many target organs in the body like including increase fat loss, increase lean
body silhouette, improve emotional and good mood and physical aging of the patient.
Increasing Oxytocin and testosterone liposome gel therapy improves patient social life, makes
patients more understanding and loving with their partner and makes them become friendlier. It
also boosts sexuality and promotes multiple orgasms in women.
from :dr. Deby Vinski speaker at WOSAAM Anti Aging Seminar, Monaco 2014
Additionally.
2. Aesthetics therapy
by lipolaser, liposuction, nanotechnology or mesolipolysis for slimming
and shapely body silhouette.
Plastic surgery : Tummy tuck, liposuction, blepharoplasty, breast
augmentation
Treatment issues
Duration of Use
use of EPT at the time of menopause and at a later
onset after a hiatus in oestrogen exposure increase
risk of breast cancer.
ET = no increase in Breast Cancer incidence in
early use.
decrease CHD and MI.
longer the duration, earlier onset the better.
But
Discontinuation of HT
Stopping ET and EPT = increased risk of
osteoporosis, cardiovascular disease, vasomotor
symptoms.
Stop previous use of EPT = higher risk of all cancer
CONCLUSION &
RECOMMENDATION
individualization
duration of use, ET is more flexible due to breast cancer risks.
ET is most effective for vulvar + vaginal atrophy. local vaginal is
recommended for this only.
women with premature or early menopause may use HT for at
least until the median age of menopause (51 years old). Longer
duration may be considered
although ET does not increase breast cancer rates, there are lack
of safety-data, and there are reports of recurrent BC with ET.
Both transdermal and low dose ET have been associated with
lower risk of VTE and stroke than standard doses. (no evidence)
Summary
Anti-aging Preventive medicine :
Anti-Oxidants, Hormonal correction, Stem cells and etc., the
important:the patient wants to feel is wellness,healthy and FEEL OPTIMAL HEALTH
so the point of HRT is not to make the patient have menstrual periods again, but to rid of the symptoms of menopause.
HT formulation, route of administration, and timing of
therapy gives different effects.
Individual benefit-risk ratio should be largely taken into
consideration from age to severity of menopausal
symptoms.
long term HT or HT initiation in older women have greater
risks.
ET is more favourable than EPT.
Women with premature menopause are at greater risk of
osteoporosis and CVD, and have more intense menopausal
symptoms.
Additional research is required to prove safety
and know the combinations for each individual
woman to know the best for aesthetic and anti
ageing benefits and lower risks.
1. Barnabei VM, Cochrane BB, Aragaki AK, et al, for the Womens Health Initiative
Investigators. Menopausal symptoms and treatment- related effects of estrogen
and progestin in the Womens Health Ini- tiative. Obstet Gynecol 2005;105:1063-
1073.
2. National Institutes of Health. State-of-the-Science Panel. National Insti- tutes of
Health State-of-the-Science Conference statement: management of menopause-
related symptoms. Ann Intern Med 2005;142:1003-1013.
3. Maclennan A, Broadbent J, Lester S, Moore V. Oral oestrogen and combined
oestrogen/progestogen therapy versus placebo for hot flushes. Cochrane
Database Sys Rev 2004;4:CD002978.
4. Schiff I, Tulchinsky D, Cramer D, Ryan KJ. Oral medroxyprogester- one in the
treatment of postmenopausal symptoms. JAMA 1980;244: 1443-1445.
5. Suckling J, Kennedy R, Lethaby A, Roberts H. Local oestrogen for vaginal
atrophy in postmenopausal women. Cochrane Database Sys Rev
2006;4:CD001500.
Thank you
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Module 12 - Human Reproduction Health PDFДокумент137 страницModule 12 - Human Reproduction Health PDFvarunОценок пока нет
- Anatomy & Physiology (Chapter 10 - Endocrine System)Документ23 страницыAnatomy & Physiology (Chapter 10 - Endocrine System)Kate Nicole EjercitoОценок пока нет
- Usmle World Step 1 Physiology: Question ListДокумент70 страницUsmle World Step 1 Physiology: Question ListNick JacobОценок пока нет
- Endocrinology Part 1Документ131 страницаEndocrinology Part 1LucjaОценок пока нет
- Anatomy and Physiology of LactationДокумент29 страницAnatomy and Physiology of LactationGayli De Lima BongyadОценок пока нет
- Pathophysiology of Diabetes Mellitus Type 2Документ1 страницаPathophysiology of Diabetes Mellitus Type 2faula rocamora100% (3)
- The Steroidogenic PathwayДокумент47 страницThe Steroidogenic Pathwaysusan64Оценок пока нет
- Hypothyroidism and InfertilityДокумент19 страницHypothyroidism and Infertilitysandeepdogra5357Оценок пока нет
- Hypoglycemia - 2014 Morales N DoronДокумент8 страницHypoglycemia - 2014 Morales N DoronDian Eka RamadhaniОценок пока нет
- Chapter 45 Endocrine DosordersДокумент50 страницChapter 45 Endocrine DosordersShaun Gabriel AmpoОценок пока нет
- Jurnal CKDДокумент9 страницJurnal CKDwiwik suprihatinОценок пока нет
- PMNP 2023 Paloyon ProperДокумент6 574 страницыPMNP 2023 Paloyon ProperJeckay P. OidaОценок пока нет
- Dermatology Lecture 5-21-09: by Ma. Socorro W. Toledo, MD, FPDSДокумент17 страницDermatology Lecture 5-21-09: by Ma. Socorro W. Toledo, MD, FPDSapi-25914483Оценок пока нет
- Adrenal GlandДокумент15 страницAdrenal GlandUnggul YudhaОценок пока нет
- Physiology of The Normal Menstrual Cycle - UpToDateДокумент14 страницPhysiology of The Normal Menstrual Cycle - UpToDatefranciscaОценок пока нет
- Polycystic Kidney DiseaseДокумент15 страницPolycystic Kidney DiseaseSabita TripathiОценок пока нет
- Unit Seven: The Endocrine SystemДокумент8 страницUnit Seven: The Endocrine SystemTofik MohammedОценок пока нет
- Patients With G-Tubes Other Types of Tubes (I.e., NG, Dobhoff, J-Tubes) Should Not Be Used For Hypoglycemia TreatmentДокумент1 страницаPatients With G-Tubes Other Types of Tubes (I.e., NG, Dobhoff, J-Tubes) Should Not Be Used For Hypoglycemia Treatmentdelapan is bakirОценок пока нет
- A Patient With Neck Swelling Moving With SwallowingДокумент40 страницA Patient With Neck Swelling Moving With SwallowingzaminazzОценок пока нет
- Endocrine and Reproductive Pharmacology-By:Dr. DHIREN BHOIДокумент77 страницEndocrine and Reproductive Pharmacology-By:Dr. DHIREN BHOIdrdhirenvet100% (9)
- Case Study On Endocrine and Metabolic Disorders PDFДокумент3 страницыCase Study On Endocrine and Metabolic Disorders PDFJude Micko Bunyi AlipitОценок пока нет
- Hyper Pro Lac Tine MiaДокумент47 страницHyper Pro Lac Tine Miakharbosham100% (3)
- Diabetes Mellitus An OverviewДокумент4 страницыDiabetes Mellitus An OverviewALОценок пока нет
- Chronic Kidney Disease LIFA FixxxДокумент19 страницChronic Kidney Disease LIFA FixxxMuzdalifa MohamadОценок пока нет
- Skin Histology 1Документ72 страницыSkin Histology 1ace danielОценок пока нет
- A Sample Research Information-Sheet With Consent FormДокумент5 страницA Sample Research Information-Sheet With Consent FormnomoredocОценок пока нет
- Endocrin E Diseases: by Group 3Документ53 страницыEndocrin E Diseases: by Group 3Ash AshОценок пока нет
- Ganirelix Drug StudyДокумент2 страницыGanirelix Drug Studyhappymee927Оценок пока нет
- Addison'sДокумент4 страницыAddison'sKoRnflakesОценок пока нет
- Activity #11 Urogenital SystemДокумент4 страницыActivity #11 Urogenital SystemNathaniel FelicianoОценок пока нет