Академический Документы
Профессиональный Документы
Культура Документы
08&09 Oral Hypoglycemics-Level 11
Загружено:
Usman Ali Akbar0 оценок0% нашли этот документ полезным (0 голосов)
42 просмотров48 страницThis document discusses the classification, mechanisms of action, pharmacokinetics, clinical uses, and side effects of various classes of oral hypoglycemic drugs used to treat type 2 diabetes. It covers insulin secretagogues like sulfonylureas and meglitinides, insulin sensitizers like biguanides and thiazolidinediones, alpha-glucosidase inhibitors, incretin mimetics, and dipeptidyl peptidase-4 inhibitors. The goal is for students to understand how each class of drug works to lower blood glucose levels and their proper uses and adverse effect profiles.
Исходное описание:
ORal
Оригинальное название
08&09 Oral Hypoglycemics-level 11
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документThis document discusses the classification, mechanisms of action, pharmacokinetics, clinical uses, and side effects of various classes of oral hypoglycemic drugs used to treat type 2 diabetes. It covers insulin secretagogues like sulfonylureas and meglitinides, insulin sensitizers like biguanides and thiazolidinediones, alpha-glucosidase inhibitors, incretin mimetics, and dipeptidyl peptidase-4 inhibitors. The goal is for students to understand how each class of drug works to lower blood glucose levels and their proper uses and adverse effect profiles.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
42 просмотров48 страниц08&09 Oral Hypoglycemics-Level 11
Загружено:
Usman Ali AkbarThis document discusses the classification, mechanisms of action, pharmacokinetics, clinical uses, and side effects of various classes of oral hypoglycemic drugs used to treat type 2 diabetes. It covers insulin secretagogues like sulfonylureas and meglitinides, insulin sensitizers like biguanides and thiazolidinediones, alpha-glucosidase inhibitors, incretin mimetics, and dipeptidyl peptidase-4 inhibitors. The goal is for students to understand how each class of drug works to lower blood glucose levels and their proper uses and adverse effect profiles.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 48
Objectives
By the end of this lecture, students should be able to:
Classify different categories of oral hypoglycemic drugs.
Identify mechanism of action, pharmacokinetics and
pharmacodynamics of each class oral hypoglycemic drugs.
Identify the clinical uses of hypoglycemic drugs
Know the side effects, contraindications of each class of
oral hypoglycemic drugs.
Types of diabetes mellitus
Type I
due to autoimmune or viral diseases
Type II
due to obesity, genetic factors
Pts with Type 11 diabetes have
two physiological defects:
1. Abnormal insulin secretion.
2. Resistance to insulin action in target
tissues associated with decreased
number of insulin receptors.
Drugs used for treatment of
Type-2 diabetes
1. Sulfonylurea drugs
2. Meglitinide analogues
3. Biguanides
4. Thiazolidinediones.
5.Alpha-glucosidase inhibitors.
6. Dipeptidyl peptidase-4(DPP-4) inhibitors
Insulin secretagogues
Sulfonylurea drugs
Meglitinide analogues
Insulin sensitizers
Biguanides
Thiazolidinediones
Oral hypoglycemic drugs
Others
Alpha glucosidase inhibitors
Dipeptidyl peptidase-4(DPP-4)
inhibitors
Insulin secretagogues
Are drugs which increase the amount of
insulin secreted by the pancreas
Include:
Sulfonylureas
Meglitinides
Classification of sulfonylureas
Tolbutamide
Acetohexamide
Tolazamide
Chlorpropamide
Glipizide
Glyburide
(Glibenclamide)
Glimepiride
First generation
Long
acting
Short
acting
second generation
Short
acting
Intermediate
acting
Long
acting
Stimulate insulin release from functioning B cells
by blocking of ATP-sensitive K channels resulting
in depolarization and calcium influx(Hence, not
effective in totally insulin-deficient pts type-1).
Potentiation of insulin action on target tissues.
Reduction of serum glucagon concentration.
Mechanism of action of sulfonylureas:
Mechanisms of Insulin Release
Pharmacokinetics of sulfonylureas:
Orally, well absorbed.
Reach peak concentration after 2-4 hr.
All are highly bound to plasma proteins.
Duration of action is variable.
Second generation has longer duration than
first generation.
Metabolized in liver
excreted in urine
Cross placenta, stimulate fetal B cells to release
insulin hypoglycemia at birth.
Tolbutamid
short-
acting
Acetohexamide
intermediate-
acting
Tolazamide
intermediate
-acting
Chlorpropa
mide
long- acting
Absorption Well Well Slow Well
Metabolism Yes Yes Yes Yes
Metabolites Inactive Active Active Inactive
Half-life 4 - 5 hrs 6 8 hrs 7 hrs 24 40 hrs
Duration of
action
Short
(6 8 hrs)
Intermediate
(12 20 hrs)
Intermediate
(12 18 hrs)
Long
( 20 60
hrs)
Excretion Urine Urine Urine Urine
First generation sulfonylurea
Tolbutamide:
safe for old diabetic patients or pts with
renal impairment.
First generation sulfonylureas
Glipizide Glibenclamide
(Glyburide)
Glimepiride
Absorption Well Well Well
Metabolism Yes Yes Yes
Metabolites Inactive Moderate activity Moderate activity
Half-life 2 4 hrs Less than 3 hrs 5 - 9 hrs
Duration of 10 16 hrs 12 24 hrs 12 24 hrs
action short long long
Doses Divided doses
30 min before
meals
Single dose Single dose
1 mg
Excretion Urine Urine Urine
SECOND GENERATION SULPHONYLUREA
Type II diabetes:
monotherapy or in combination with other
antidiabetic drugs.
Uses of sulfonylureas
Unwanted Effects:
1. Hyperinsulinemia & Hypoglycemia:
2. Weight gain due to increase in appetite
e.g. Repaglinide
Rapidly acting insulin secretagogues
Meglitinide analogues
Mechanism of Action:
Insulin secretagogue as sulfonylureas.
Pharmacokinetics of Meglitinides
Orally, well absorbed.
Very fast onset of action, peak 1 h.
short duration of action (4 h).
Metabolized in the liver & excreted in
bile.
Type II diabetes:
monotherapy or combined with other
antidiabetic drugs.
Patients allergic to sulfonylurea
Uses of Meglitinides
Hypoglycemia
Weight gain.
Adverse effects of Meglitinides
1. Biguanides, e.g. Metformin
2. Thiazolidinediones, e.g. pioglitazone
Insulin sensitizers
BIGUANIDES
E.g. Metformin
Does not stimulate insulin release.
Increases liver ,muscle &adipose tissues
sensitivity to insulin & increase peripheral
glucose utilization.
Inhibits gluconeogenesis.
Impairs glucose absorption from GIT.
Mechanism of action of metformin
orally.
Not bound to serum protein.
Not metabolized.
t 3 hours.
Excreted unchanged in urine
Pharmacokinetics of metformin
Obese patients with type II diabetes
Monotherapy or in combination.
Advantages:
No risk of hyperinsulinemia or hypoglycemia
or weight gain (anorexia).
Uses of metformin
Metallic taste in the mouth
GIT disturbances: nausea, vomiting, diarrhea
Lactic acidosis
Long term use interferes with vitamin B
12
absorption.
Adverse effects of metformin
Pregnancy.
Renal disease.
Liver disease.
Alcoholism.
Heart failure
Contraindications of metformin
Insulin sensitizers
Thiazolidinediones (glitazones)
Pioglitazone
Mechanism of action
Increase sensitivity of target tissues to insulin.
Increase glucose uptake and utilization in
muscle and adipose tissue.
Pharmacokinetics of pioglitazone
Orally (once daily dose).
Highly bound to plasma albumins (99%)
Slow onset of activity
Half life 3-4 h
Metabolized in the liver
Excreted in urine 64% & bile
Type II diabetes with insulin resistance.
Used either alone or combined with
sulfonylurea, biguanides or insulin.
No risk of hypoglycemia when used alone
Uses of pioglitazone
Hepatotoxicity ?? (liver function tests for
1st year of therapy).
Fluid retention (Edema).
Precipitate congestive heart failure
Mild weight gain.
Adverse effects of pioglitazone
E.g. Acarbose, Meglitol
Reversible inhibitors of intestinal -
glucosidases in intestinal brush border
responsible for degradation of
oligosaccharides to monosaccharides.
-Glucosidase inhibitors
decrease carbohydrate digestion and
absorption in small intestine.
Decrease postprandial hyperglycemia.
Taken just before meals.
No hypoglycemia if used alone.
-Glucosidase inhibitors
37
-GLUCOSIDASE INHIBITORS (Contd.)
MECHANISM OF ACTION
Acarbose
Given orally, poorly absorbed.
Metabolized by intestinal bacteria.
Excreted in stool and urine.
Kinetics of -glucosidase inhibitors
GIT: Flatulence, diarrhea, abdominal
pain.
No hypoglycemia if used alone.
Adverse effects of -glucosidase
inhibitors
Incretin mimetics
e.g. Exenatide(GLP-1)
Incretins are GI hormones secreted in
response to food, carried through circulation
to the beta cells to stimulate insulin secretion
& decrease glucagon secretion.
Incretins
Two main Incretin hormones:
GLP-1 (glucagon-like peptide-1)
GIP (gastric inhibitory peptide or glucose-
dependent insulinotropic peptide)
Both are inactivated by dipeptidyl peptidase-4
(DPP-4).
Incretin mimetics
Exenatide
is glucagon-like peptide-1 (GLP-1) agonist.
given s.c. once or twice daily
Therapy of patients with type 2 diabetes
who are not controlled with oral medicine.
Adverse efects
Nausea & vomiting(most common)
Dipeptidyl peptidase-4 (DPP- 4 )
inhibitors
e.g. Sitagliptin
Orally
Given once daily
half life 8-14 h
Dose is reduced in pts with renal
impairment
Mechanism of action of sitagliptin
Inhibit DPP-4 enzyme and leads to an
increase in incretin hormones level.
This results in an increase in insulin
secretion & decrease in glucagon secretion.
Mechanism of
action
Clinical uses
Type 2 DM as an adjunct to diet &
exercise as a monotherapy or in
combination with other antidiabetic drugs.
Adverse effects
Nausea, abdominal pain, diarrhea
Nasopharyngitis
Вам также может понравиться
- Drug Doses Frank Shann - PDFДокумент49 страницDrug Doses Frank Shann - PDFAgustina Permata Sari100% (1)
- 58 Cases History and Physical Exam BookДокумент102 страницы58 Cases History and Physical Exam BookeleazarmdОценок пока нет
- UTI On A Background of Obstructive NephropathyДокумент26 страницUTI On A Background of Obstructive NephropathyAminath MeesanОценок пока нет
- Adult Electrolyte Replacement Protocol - MCLN 0006 J PDFДокумент1 страницаAdult Electrolyte Replacement Protocol - MCLN 0006 J PDFCraigОценок пока нет
- SMART Asthma TherapyДокумент4 страницыSMART Asthma TherapyKen Won100% (1)
- Mefenamic Acid Drug StudyДокумент1 страницаMefenamic Acid Drug StudyBer AnneОценок пока нет
- Year 6 Clerkship - Welcome & Curriculum Class 2020 (Revised 25.04.2019)Документ190 страницYear 6 Clerkship - Welcome & Curriculum Class 2020 (Revised 25.04.2019)Ali SemajОценок пока нет
- Final GIT Case PresentationДокумент53 страницыFinal GIT Case PresentationRovan100% (1)
- Nephrology: Omar K MRCP IrelandДокумент54 страницыNephrology: Omar K MRCP IrelandManmeet SОценок пока нет
- Clinical CasesДокумент12 страницClinical CasesAndreea HanuОценок пока нет
- Insulin and Oral Hypoglycemic DrugsДокумент30 страницInsulin and Oral Hypoglycemic DrugsAngga NugrahaОценок пока нет
- Treatment of Resistant and Refractory HypertensionДокумент21 страницаTreatment of Resistant and Refractory HypertensionLuis Rodriguez100% (1)
- Practical Guidance On The Use of Premix Insulin - FinalДокумент14 страницPractical Guidance On The Use of Premix Insulin - FinalJonesius Eden ManoppoОценок пока нет
- Article - Medical ErrorsДокумент4 страницыArticle - Medical ErrorsDavid S. ChouОценок пока нет
- Nutritionalanemia25thmarch2021 210403063057Документ29 страницNutritionalanemia25thmarch2021 210403063057najeebОценок пока нет
- Peadiatric Guildlines For Malaysian House OfficerДокумент44 страницыPeadiatric Guildlines For Malaysian House OfficerAlex MatthewОценок пока нет
- Mock Record B-1-2-Well Child VisitsДокумент4 страницыMock Record B-1-2-Well Child VisitsaelteeОценок пока нет
- Read MeДокумент1 страницаRead MeJack GuccioneОценок пока нет
- Ectopic PregnancyДокумент76 страницEctopic PregnancyVivian Jean TapayaОценок пока нет
- Aquifer InternalMedicine11 - 45Документ8 страницAquifer InternalMedicine11 - 45JulieОценок пока нет
- Alarm Symptoms of Hematoonco in Pediatrics: Dr. Cece Alfalah, M.Biomed, Sp.A (K) Pediatric Hematology and OncologyДокумент22 страницыAlarm Symptoms of Hematoonco in Pediatrics: Dr. Cece Alfalah, M.Biomed, Sp.A (K) Pediatric Hematology and OncologyMuhammad ArifОценок пока нет
- Pass 2010 ScheduleДокумент1 страницаPass 2010 SchedulewldcrdОценок пока нет
- Gastroenterology AscitesДокумент2 страницыGastroenterology AscitesNour SamadОценок пока нет
- Family Medicine PresentationДокумент53 страницыFamily Medicine PresentationNancy BaggaОценок пока нет
- Approach: A. How The Kidney Handle The Proteins?Документ9 страницApproach: A. How The Kidney Handle The Proteins?Rashed ShatnawiОценок пока нет
- Diabetes and Complications: When Documenting Diabetes, It's Important To Note The FollowingДокумент2 страницыDiabetes and Complications: When Documenting Diabetes, It's Important To Note The Followingmeikaizen100% (1)
- Gyne Case COCДокумент37 страницGyne Case COCLian BaylosisОценок пока нет
- Third-Year OSCE Manual 2019-2020Документ17 страницThird-Year OSCE Manual 2019-2020Agleema AhmedОценок пока нет
- Pharmacology Exam4 ReviewДокумент8 страницPharmacology Exam4 ReviewNatalia BortellОценок пока нет
- Reye's SyndromeДокумент11 страницReye's SyndromeChristine Go100% (1)
- General Population (No Diabetes or CKD) Diabetes or CKD PresentДокумент1 страницаGeneral Population (No Diabetes or CKD) Diabetes or CKD PresentMuthia ArsilОценок пока нет
- Step 1 REVIEWДокумент140 страницStep 1 REVIEWRima HajjarОценок пока нет
- DiabeticcasestudyДокумент7 страницDiabeticcasestudyapi-272773859Оценок пока нет
- Newborn NotesДокумент44 страницыNewborn NotesHaziq KamardinОценок пока нет
- New Guidelines For The Diagnosis of Paediatric Coeliac DiseaseДокумент3 страницыNew Guidelines For The Diagnosis of Paediatric Coeliac DiseaseDiana NicaОценок пока нет
- DiabetesMellitusMasterclass MedmasteryHandbookДокумент88 страницDiabetesMellitusMasterclass MedmasteryHandbookDeenissa Van GawaranОценок пока нет
- CD Im PrimerДокумент28 страницCD Im PrimerTiagogiesteiraОценок пока нет
- Stroke - Final ReportДокумент16 страницStroke - Final ReportgolokipokОценок пока нет
- From This Age in What Patient Group? Start Screening For With Test FrequencyДокумент7 страницFrom This Age in What Patient Group? Start Screening For With Test Frequencyphoenix24601Оценок пока нет
- Personal Statement - FinalДокумент2 страницыPersonal Statement - Finalapi-383932502Оценок пока нет
- Turkey Book 03 Internal Medicine PDFДокумент47 страницTurkey Book 03 Internal Medicine PDFPreaisОценок пока нет
- USMLE Step 3 ER PDFДокумент12 страницUSMLE Step 3 ER PDFlalaОценок пока нет
- Victorias New ResumeДокумент2 страницыVictorias New Resumeapi-513192361Оценок пока нет
- 7.8 Collect Data & Come Up With Plan For Day & Nursing Diagnosis Pre-Conference 8-9 Vitals Then Chart, AM Care, StartДокумент2 страницы7.8 Collect Data & Come Up With Plan For Day & Nursing Diagnosis Pre-Conference 8-9 Vitals Then Chart, AM Care, StartSade' CovingtonОценок пока нет
- National Leaflet About CKD and eGFR For GPs (Updated September 2007)Документ2 страницыNational Leaflet About CKD and eGFR For GPs (Updated September 2007)Dhika ArdiansyahОценок пока нет
- Nausea VomitingДокумент36 страницNausea VomitingDian Fitri100% (1)
- Preventive Health: Based On The USPSTF 2014Документ42 страницыPreventive Health: Based On The USPSTF 2014Louella CarpioОценок пока нет
- Akd & CKDДокумент44 страницыAkd & CKDﻣﻠﻚ عيسىОценок пока нет
- Mo Intern Handbook - FinalДокумент37 страницMo Intern Handbook - FinalGideon K. MutaiОценок пока нет
- The Stages of Prevention - Primer On Public Health PopulationДокумент2 страницыThe Stages of Prevention - Primer On Public Health PopulationBSN 201450% (2)
- Grand Rounds - Pulmonary EmbolismДокумент25 страницGrand Rounds - Pulmonary EmbolismAdrian CastroОценок пока нет
- MGH/HMS Internal Medicine Comprehensive Review and Update Renal Cases - June 2021Документ49 страницMGH/HMS Internal Medicine Comprehensive Review and Update Renal Cases - June 2021Churschmann SpiralОценок пока нет
- Inborn Errors of Metabolism - Basics For Students (Iver Andreas Norbergs Kopi Som Er I Konflikt 2016-01-24)Документ4 страницыInborn Errors of Metabolism - Basics For Students (Iver Andreas Norbergs Kopi Som Er I Konflikt 2016-01-24)Wen Jie LauОценок пока нет
- Introduction To Internal Medicine - PPTMДокумент30 страницIntroduction To Internal Medicine - PPTMAddyОценок пока нет
- Mood Disorders: Advanced Practice Education AssociatesДокумент11 страницMood Disorders: Advanced Practice Education AssociatesAndrea100% (1)
- Breaking Bad News 1 PDFДокумент5 страницBreaking Bad News 1 PDFSaeed HasanОценок пока нет
- CCT - CCI Code of EthicsДокумент2 страницыCCT - CCI Code of EthicsAvanca LouisОценок пока нет
- Problem-based Approach to Gastroenterology and HepatologyОт EverandProblem-based Approach to Gastroenterology and HepatologyJohn N. PlevrisОценок пока нет
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsОт EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsОценок пока нет
- Practical Gastroenterology and Hepatology Board Review ToolkitОт EverandPractical Gastroenterology and Hepatology Board Review ToolkitKenneth R. DeVaultОценок пока нет
- Chronic Renal Failure: Concise Long Case ApproachДокумент3 страницыChronic Renal Failure: Concise Long Case ApproachUsman Ali AkbarОценок пока нет
- GI Bleeding Team Work - 2nd EditionДокумент9 страницGI Bleeding Team Work - 2nd EditionUsman Ali AkbarОценок пока нет
- Polycystic Kidneys: Adult PKD: ComplicationsДокумент1 страницаPolycystic Kidneys: Adult PKD: ComplicationsUsman Ali AkbarОценок пока нет
- Renal Tubular Acidosis Summary - AdjДокумент1 страницаRenal Tubular Acidosis Summary - AdjUsman Ali AkbarОценок пока нет
- Urinary Tract Infection & PyelonephritisДокумент3 страницыUrinary Tract Infection & PyelonephritisUsman Ali AkbarОценок пока нет
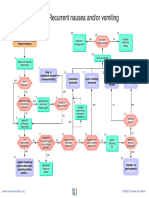
- Recurrent Nausea Andor VomitingДокумент8 страницRecurrent Nausea Andor VomitingUsman Ali AkbarОценок пока нет
- King Khalid University Hospital Department of Obstetrics & Gyncology Course 481Документ40 страницKing Khalid University Hospital Department of Obstetrics & Gyncology Course 481Usman Ali AkbarОценок пока нет
- DialysisДокумент2 страницыDialysisUsman Ali AkbarОценок пока нет
- Obstructive Airway Disease: Dr. Khalid Al-Mobaireek King Khalid University HospitalДокумент53 страницыObstructive Airway Disease: Dr. Khalid Al-Mobaireek King Khalid University HospitalUsman Ali AkbarОценок пока нет
- Anaemia in PregnancyДокумент13 страницAnaemia in PregnancyUsman Ali AkbarОценок пока нет
- Through The Strange WindsДокумент5 страницThrough The Strange WindsUsman Ali AkbarОценок пока нет
- Subject: Permission For Badminton Court NID, Multan: TH THДокумент1 страницаSubject: Permission For Badminton Court NID, Multan: TH THUsman Ali AkbarОценок пока нет
- DR Othman Alharbi, MBBS FRCPC Assistance Professor & Consultant Gastroenterology College of Medicine King Saud UniversityДокумент18 страницDR Othman Alharbi, MBBS FRCPC Assistance Professor & Consultant Gastroenterology College of Medicine King Saud UniversityUsman Ali AkbarОценок пока нет
- Recurrent VomitingДокумент16 страницRecurrent VomitingUsman Ali AkbarОценок пока нет
- GRAM NEGATIVE RODS (5) Fastidious Organisms From Animal Sources (A)Документ1 страницаGRAM NEGATIVE RODS (5) Fastidious Organisms From Animal Sources (A)Usman Ali AkbarОценок пока нет
- Cord ProlapseДокумент2 страницыCord ProlapseUsman Ali AkbarОценок пока нет
- Organophosphate PoisoningДокумент23 страницыOrganophosphate PoisoningUsman Ali AkbarОценок пока нет
- Alas!! EmpytinessДокумент2 страницыAlas!! EmpytinessUsman Ali AkbarОценок пока нет
- When Hope DiesДокумент2 страницыWhen Hope DiesUsman Ali AkbarОценок пока нет
- Untold Stanza... : - Nasim Alam (N-61)Документ1 страницаUntold Stanza... : - Nasim Alam (N-61)Usman Ali AkbarОценок пока нет
- Lect 1:: M2Pasysl21 Urinary SystemДокумент4 страницыLect 1:: M2Pasysl21 Urinary SystemUsman Ali AkbarОценок пока нет
- Death and The Mother For MergeДокумент4 страницыDeath and The Mother For MergeUsman Ali AkbarОценок пока нет
- Miconazole Oral Gel and Drug InteractionsДокумент4 страницыMiconazole Oral Gel and Drug InteractionsWeng AceОценок пока нет
- Invitro Toxicity Assay MethodsДокумент11 страницInvitro Toxicity Assay MethodsShubham RastogiОценок пока нет
- Ascorbic Acid Tablets 500mg Label LeafletДокумент4 страницыAscorbic Acid Tablets 500mg Label LeafletmostofarubalОценок пока нет
- Forensic Investigation Tool For Volatility FrameworkДокумент4 страницыForensic Investigation Tool For Volatility FrameworkInternational Journal of Innovative Science and Research TechnologyОценок пока нет
- Treatment For My Patient: Drug Dose Route Action Indication Side Effect Nurse's ResponsibilityДокумент2 страницыTreatment For My Patient: Drug Dose Route Action Indication Side Effect Nurse's ResponsibilityValarmathiОценок пока нет
- General PharmacologyДокумент60 страницGeneral PharmacologyHAMMADОценок пока нет
- Defekta PEMDA 13 09 2021Документ13 страницDefekta PEMDA 13 09 2021k24 bambukuningОценок пока нет
- SakajayaДокумент36 страницSakajayates sajaОценок пока нет
- Obat Pagi: No Generik Paten Sediaan Harga/tab Antibiotik, Antivirus, AntijamurДокумент2 страницыObat Pagi: No Generik Paten Sediaan Harga/tab Antibiotik, Antivirus, Antijamursatria12Оценок пока нет
- Psyc Un 2460Документ11 страницPsyc Un 2460Robyn AnОценок пока нет
- Biostar Pharmaceuticals PVTДокумент36 страницBiostar Pharmaceuticals PVTBobby GolaОценок пока нет
- Drug StudyДокумент3 страницыDrug StudyTarquin Tomada100% (2)
- Pharmacist (Haad/Doh) : Mahboob AliДокумент4 страницыPharmacist (Haad/Doh) : Mahboob AliMahboob AliОценок пока нет
- Pharmaceutical Care PlaneДокумент28 страницPharmaceutical Care PlaneMUGHALОценок пока нет
- Kava and Kratom Guide Shot of JoyДокумент3 страницыKava and Kratom Guide Shot of JoyRick BulowОценок пока нет
- Aesthetic Trends and Technologies Formula 82M Special Report (Sept 2010)Документ4 страницыAesthetic Trends and Technologies Formula 82M Special Report (Sept 2010)nuno costeОценок пока нет
- Research and Development FinalДокумент17 страницResearch and Development FinalChaОценок пока нет
- Low-Cumulative Dose Isotretinoin Treatment in Mild-To Moderate AcneДокумент5 страницLow-Cumulative Dose Isotretinoin Treatment in Mild-To Moderate Acneseptian88_cahyoОценок пока нет
- Industrial Chemicals by W L Faith Donald B Keyes and Ronald L Clark John Wiley and Sons New York 1950 Xi 652 PP Illustrated 15 235 CM Price 8 CompressДокумент1 страницаIndustrial Chemicals by W L Faith Donald B Keyes and Ronald L Clark John Wiley and Sons New York 1950 Xi 652 PP Illustrated 15 235 CM Price 8 CompressKejora PitalokaОценок пока нет
- Steel Specification PDFДокумент8 страницSteel Specification PDFPeter AntonyОценок пока нет
- Hal 38-47 46 Herline 12-1 Rev2Документ10 страницHal 38-47 46 Herline 12-1 Rev2Facebook VionyОценок пока нет
- Key Topics - Bioequivalence - 13-April-2017.ppt'Документ36 страницKey Topics - Bioequivalence - 13-April-2017.ppt'Md TayfuzzamanОценок пока нет
- Info Foriegn Grad Reg Intern ManualДокумент25 страницInfo Foriegn Grad Reg Intern ManualYamchi Arnavaz0% (1)
- Indomethacin From Anti-Inflammatory To Anticancer AgentДокумент26 страницIndomethacin From Anti-Inflammatory To Anticancer AgentYaqeen Alhaqq F. GhaziОценок пока нет
- 04 - Extravascular Administration (Oral)Документ41 страница04 - Extravascular Administration (Oral)Prasanna PappuОценок пока нет
- Abbreviation Meaning Notes: Cibo ("With Food")Документ4 страницыAbbreviation Meaning Notes: Cibo ("With Food")TantriОценок пока нет
- Medication Deferral ListДокумент2 страницыMedication Deferral ListNatasha MendozaОценок пока нет