Академический Документы
Профессиональный Документы
Культура Документы
Hypocalcemia & Hypercalcemia
Загружено:
RomMy WiEn MicKho0 оценок0% нашли этот документ полезным (0 голосов)
167 просмотров21 страницаhypo hyper
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документhypo hyper
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
167 просмотров21 страницаHypocalcemia & Hypercalcemia
Загружено:
RomMy WiEn MicKhohypo hyper
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 21
Hypocalcemia & Hypercalcemia
Emergency pediatric PICU division
Pediatric Department
Medical Faculty, University of Sumatera Utara
H. Adam Malik Hospital
1
HYPOCALCEMIA
2
Because of potentially severe symptoms such as
laryngospasm and seizures, hypocalcemia needs to be
identified and treated expeditiously
The ionized calcium concentration is low in true hypocalcemia
The total calcium concentration does not accurately predict
the ionized calcium concentration in the patient with
hypoalbuminemia the ionized calcium concentration
should be determined in patients with suspected
hypocalcemia when the patient is hypoalbuminemic and/or is
critically ill
3
SPECIFIC CAUSES IN THE NEONATE
Early neonatal hypocalcemia
Late neonatal hypocalcemia
Maternal hypercalcemia
HYPOPARATHYROIDISM
DiGeorge syndrome (MIM
*
188400)
X-linked hypoparathyroidism (MIM 307700)
Parathyroid hormone (PTH) gene mutations (MIM 168450)
Calcium-sensing receptor mutation (MIM 601199)
Autosomal recessive hypoparathyroidism with dysmorphic features (MIM 241410)
HDR (or Barakat) syndrome (MIM 146255)
Autoimmune polyglandular syndrome type I (MIM 240300)
Kearns-Sayre syndrome (MIM 530000)
Hemochromatosis
Wilson disease (MIM 277900)
Postsurgical hypoparathyroidism
Radioactive iodine ablation of the thyroid gland
Hypomagnesemia
Causes of hypocalcemia
4
LACK OF RESPONSE TO PTH
Pseudohypoparathyroidism type IA (MIM 103580)
Pseudohypoparathyroidism type IB (MIM 603233)
Pseudohypoparathyroidism type II
Hypomagnesemia
VITAMIN D DEFICIENCY
Poor intake
Lack of sunlight
Malabsorption
Increased metabolism (e.g., anticonvulsants)
Failure to form 25-hydroxyvitamin D in the liver
Vitamin Ddependent rickets type 1 (MIM 264700)
Vitamin Ddependent rickets type 2 (MIM 277420)
Renal insufficiency
Causes...
REDISTRIBUTION OF PLASMA CALCIUM
Hyperphosphatemia
Rhabdomyolysis
Tumor lysis syndrome
Blood transfusions
Hungry bone syndrome
Acute pancreatitis
Osteopetrosis, infantile (MIM 259700)
INADEQUATE CALCIUM INTAKE
Calcium-poor diet or TPN
Dietary calcium chelators
Malabsorption
UNKNOWN
Septic shock
Critical illness
5
Clinical Manifestation
Mild hypocalcemia is usually asymptomatic
The clinical manifestations are mostly due to neuromuscular irritability
Older children: paresthesias, typically perioral or of the hands and feet
Tetany is the classic manifestation of hypocalcemia, and symptoms may
include carpopedal spasm, laryngospasm, and seizures
Seizures may be the first manifestation of hypocalcemia, especially in
infants
Symptoms of tetany may be provoked in patients with hypocalcemia by
hyperventilation, which by raising the pH causes calcium to bind to
albumin, thereby lowering the ionized calcium concentration
6
Newborn infants with hypocalcemia usually do not have carpopedal
spasm. Along with seizures, manifestations in newborns may include
irritability, muscular twitching, jitteriness, and tremors. Alternatively,
newborns with hypocalcemia may have symptoms suggestive of sepsis,
such as poor feeding, vomiting, and lethargy
The consequences of long-standing hypocalcemia depend on the etiology.
In children with inadequate vitamin D, there is concomitant
hypophosphatemia and secondary hyperparathyroidism. These patients
have inadequate bone mineralization, and consequently develop rickets
Rickets may also occur with severe dietary calcium deficiency
7
Chvostek and Trousseau signs
may be elicited in patients with
hypocalcemia
A positive Chvostek sign occurs
if tapping the facial nerve anterior
to the external auditory meatus
elicits a twitch of the upper lip or
entire mouth. This is not a very
specific sign because it is
positive in about 10% of patients
without hypocalcemia
8
9
http://www.wrongdiagnosis.com/bookimages/14/4721.1.png
10
Trousseau sign is more specific, but
quite uncomfortable to elicit and
generally not an appropriate test in
a child
A blood pressure cuff is inflated
slightly above the systolic blood
pressure for more than 3 min;
carpopedal spasm occurs if
hypocalcemia is present as a result
of the ischemia of the motor nerves
11
http://www.dinf.ne.jp/doc/english/global/david/dwe002/dwe002g/dwe00215g01.gif
Diagnosis & Treatment
Diagnosis of the patient with hypocalcemia
should begin with a thorough history of dietary
intake.
It should also include an investigation of family
history of rickets, hypocalcemia and endocrine
disorders. Physical examination should include
a close evaluation of the bones and joints
12
A primary tenet in the treatment of hypocalcemia is to tailor the therapy to
the cause of hypocalcemia
Calcium may be given IV or orally
Acute symptomatic hypocalcemia: a bolus dose of Ca gluconate (100-
200mg/kg or 9-18 mg/kg elemental Ca to a maximum of 1-3 g in adults)
should be administered over 10-20 mins. A continuous infusion of Ca
gluconate inf may be administered at starting dose of 10-30 mg/kg/hr, the
rate can then be titrated based on serial Ca measurement
All patients receiving IV Ca require close monitoring of total or ionized Ca
levels and cardiac ECG
13
Rogers textbook of pediatric intensive care, 4
th
ed, 2008
For symptomatic hypocalcemia in neonates, calcium gluconate is given
at a dose of 100200 mg/kg (12 mL/kg of a 10% solution; 918 mg of
elemental Ca/kg)
This dose may be repeated every 68 hr until the calcium level
stabilizes
Alternatively, calcium gluconate may be given as a constant
intravenous infusion, with neonates typically requiring 500
750 mg/kg/24 hr of calcium gluconate
14
Nelson Textbook of pediatrics, 17
th
ed, 2004
HYPERCALCEMIA
15
Hypercalcemia is frequently discovered incidentally on a routine
chemistry profile
This is because hypercalcemia is an uncommon electrolyte disorder, and
its clinical manifestations are fairly nonspecific
There are, however, some clinical situations in which hypercalcemia
should be suspected
16
17
EXCESS PARATHYROID HORMONE
Primary hyperparathyroidism
Sporadic adenoma
Familial isolated hyperparathyroidism (MIM
*
145000)
Multiple endocrine neoplasia type I (MIM 131100)
Multiple endocrine neoplasia type II (MIM 171400)
Hyperparathyroidismjaw tumor syndrome (MIM 145001)
Calcium-sensing receptor mutation (MIM 239200)
Transient secondary neonatal hyperparathyroidism
Tertiary hyperparathyroidism
EXCESS VITAMIN D
Hypervitaminosis D
Subcutaneous fat necrosis
Sarcoidosis
Granulomatous diseases
Lymphomas
EXCESS CALCIUM INTAKE
Calcium supplements
Iatrogenic (e.g., total parenteral nutrition)
EXCESS RENAL REABSORPTION OF CALCIUM
Familial benign hypocalciuric hypercalcemia (MIM 145980)
Thiazide diuretics
RELEASE FROM BONE
Thyrotoxicosis
Hypervitaminosis A
Malignancy associated
Ectopic parathyroid hormone (PTH)
PTH-related peptide
Bone metastasis
Other factors
Immobilization
Renal osteodystrophy
Low turnover disease
Aluminum deposition
MISCELLANEOUS
Williams syndrome (MIM 194050)
Hypophosphatemia
Pheochromocytoma
Adrenal insufficiency
Recovery phase of rhabdomyolysis
Jansen metaphyseal chondrodysplasia
(MIM 156400)
Hypophosphatasia (MIM 241500)
Causes of hypercalcemia
Clinical Manifestation
The signs and symptoms of hypercalcemia are related to the magnitude of
the problem
Hypercalcemia is conventionally classified as mild (<12 mg/dL), moderate
(1215 mg/dL), or severe (>15 mg/dL)
Many patients with mild or moderate hypercalcemia are asymptomatic,
with the diagnosis resulting from an incidental laboratory test
18
19
GASTROINTESTINAL
Nausea and vomiting
Poor feeding
Failure to thrive
Constipation
Abdominal pain
Pancreatitis
Peptic ulcer
CARDIAC
Hypertension
Decreased QT interval
Arrhythmias
CENTRAL NERVOUS SYSTEM
Lethargy
Hypotonia
Psychiatric disturbances
Coma
KIDNEY
Polyuria and dehydration
Hypernatremia
Renal failure
Nephrolithiasis
Clinical manifestations of hypercalcemia
Treatment
Dependent on its severity
The initial basic tenets of therapy are to restore intravascular volume and to
enhance renal excretion, which can be accomplished by administration of
normal saline at 2 or 3 times maintenance fluid rate
If the patient is adequately rehydrated and Ca levels do not decrease, loop
diuretics may be administered, but should be done judiciously
Calcitonin and biphosponate are useful adjuncts in hypercalcemia
In severe cases in which hydration and medications fail to reduce serum Ca
levels, hemodialysis using a low Ca dialysate can be performed
Glucocorticoids have been useful in treating hypercalcemia secondary to
sarcoidosis and vit D deficiency
20
Rogers textbook of pediatric intensive care, 4
th
ed, 2008
21
Вам также может понравиться
- Anesthesia For Open Abdominal Aortic SurgeryДокумент18 страницAnesthesia For Open Abdominal Aortic SurgeryAurora TrifaОценок пока нет
- AKI in SepsisДокумент45 страницAKI in SepsisIkeBundaAdellulaОценок пока нет
- Chronic Kidney DiseaseДокумент40 страницChronic Kidney DiseasePaul SinsОценок пока нет
- Nephrology Best RДокумент6 страницNephrology Best Rfrabzi100% (1)
- Prostrolane Intra Articular en INGLESДокумент6 страницProstrolane Intra Articular en INGLESjuanОценок пока нет
- Disorder of Potassium MetabolismДокумент28 страницDisorder of Potassium MetabolismSaif AliОценок пока нет
- Fluid Therapy and ElectroliteДокумент36 страницFluid Therapy and ElectroliteAriefBudimanHidayatОценок пока нет
- FIXED PPT Case Report EsterДокумент39 страницFIXED PPT Case Report Esterririn esterinaОценок пока нет
- Acid Base Disorders - Lecture 45Документ14 страницAcid Base Disorders - Lecture 45yassin mostafaОценок пока нет
- Acute Treatment of Hypocalcaemia (Adults)Документ2 страницыAcute Treatment of Hypocalcaemia (Adults)Ahed WarwarОценок пока нет
- Approach To Etiology of HypokalemiaДокумент97 страницApproach To Etiology of Hypokalemiadrbhaskar100% (2)
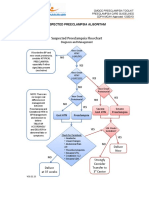
- Suspected Preeclampsia AlgorithmДокумент1 страницаSuspected Preeclampsia Algorithmmisstina.19876007100% (1)
- Surfactant PresentationДокумент18 страницSurfactant PresentationMaadaОценок пока нет
- Fluid N Electrolyte BalanceДокумент60 страницFluid N Electrolyte BalanceAnusha Verghese67% (3)
- Hormonal Control of Calcium and Phosphate MetabolismДокумент50 страницHormonal Control of Calcium and Phosphate MetabolismhamidОценок пока нет
- Acid-Base BalanceДокумент28 страницAcid-Base Balanceps4only100% (1)
- Potassium Homeostasis and Causes of Hypo/HyperkalemiaДокумент47 страницPotassium Homeostasis and Causes of Hypo/HyperkalemiaMayuresh ChaudhariОценок пока нет
- Anaesthetic management of TURPДокумент39 страницAnaesthetic management of TURPanon_727764033Оценок пока нет
- ECG in Electrolyte AbnormalitiesДокумент26 страницECG in Electrolyte AbnormalitiessmoggindakrakОценок пока нет
- HYPOCALCEMIAДокумент27 страницHYPOCALCEMIAJeffri SetiawanОценок пока нет
- Assessing Endocrine Function and Diabetes ComplicationsДокумент14 страницAssessing Endocrine Function and Diabetes ComplicationsSarahMelissaОценок пока нет
- Isotonic Saline (0.9%Nacl-Normal Saline) IndicationДокумент3 страницыIsotonic Saline (0.9%Nacl-Normal Saline) IndicationJared AllenОценок пока нет
- Regional AnesthesiaДокумент54 страницыRegional AnesthesiaIdza Fariha AfriОценок пока нет
- Potassium ParticipantsДокумент21 страницаPotassium ParticipantsSkylar IvyОценок пока нет
- Manajemen Anestesi Pada Uremic SyndromeДокумент27 страницManajemen Anestesi Pada Uremic SyndromeAdi Nugroho MelyanaОценок пока нет
- Preoperative Assessment ChecklistДокумент27 страницPreoperative Assessment ChecklistHairina MazlanОценок пока нет
- Disorders of Calcium, Phosphate and Magnesium MetabolismДокумент89 страницDisorders of Calcium, Phosphate and Magnesium MetabolismJuhiJahan AmanullahОценок пока нет
- Chronic Kidney Disease Stages, Risk Factors, and TreatmentДокумент45 страницChronic Kidney Disease Stages, Risk Factors, and Treatmentnaro ayosОценок пока нет
- Nephrotic SyndromeДокумент24 страницыNephrotic SyndromeJawad SaleemОценок пока нет
- Tubulointerstitial Diseases: Dr. Raid JastaniaДокумент48 страницTubulointerstitial Diseases: Dr. Raid JastaniaThomas McconnellОценок пока нет
- Thromboprophylaxis in The ICUДокумент31 страницаThromboprophylaxis in The ICUdocansh100% (1)
- Management of Acute Glomerulonephritis in Children: Children's Services Medical GuidelinesДокумент7 страницManagement of Acute Glomerulonephritis in Children: Children's Services Medical GuidelinesdaypranitaОценок пока нет
- DR Aida Lombok 3 Mei 2017 - HisfarsiДокумент39 страницDR Aida Lombok 3 Mei 2017 - HisfarsiBasri BaslamОценок пока нет
- Acute Renal FailureДокумент6 страницAcute Renal Failurearif kurnia timurОценок пока нет
- HypothyroidismДокумент54 страницыHypothyroidismagakshat23Оценок пока нет
- Hypovolemic ShockДокумент21 страницаHypovolemic ShockOlga GoryachevaОценок пока нет
- Diabetic Nephropathy: Assisstant Professor Dr. Mihaela-Dora DonciuДокумент65 страницDiabetic Nephropathy: Assisstant Professor Dr. Mihaela-Dora DonciuFloreaAndreiОценок пока нет
- Cme Acs 2. Stemi (Izzah)Документ36 страницCme Acs 2. Stemi (Izzah)Hakimah K. SuhaimiОценок пока нет
- Dr. Sunatrio - Management Hypovolemic ShockДокумент59 страницDr. Sunatrio - Management Hypovolemic ShockArga Putra SaboeОценок пока нет
- Secondary Arterial HypertensionДокумент32 страницыSecondary Arterial HypertensionAndi SusiloОценок пока нет
- Anticoagulation Guidelines JMДокумент32 страницыAnticoagulation Guidelines JMMichael HuntОценок пока нет
- January-2016 Papers (1071 MCQS) by Amlodipine BesylateДокумент95 страницJanuary-2016 Papers (1071 MCQS) by Amlodipine BesylateAmlodipine Besylate100% (1)
- COPD: Chronic Obstructive Pulmonary Disease ExplainedДокумент52 страницыCOPD: Chronic Obstructive Pulmonary Disease ExplainedErik II100% (1)
- ERAS Guidelines PDFДокумент8 страницERAS Guidelines PDFWadezigОценок пока нет
- Dexmedetomidine Expanding Role in AnesthesiaДокумент9 страницDexmedetomidine Expanding Role in AnesthesiaUnggul Yudha100% (1)
- Patient Controlled AnalgesiaДокумент35 страницPatient Controlled AnalgesiamochkurniawanОценок пока нет
- 2 Renal PhysiologyДокумент56 страниц2 Renal PhysiologyNoraine Princess TabangcoraОценок пока нет
- Platelet, FFP and Cryoprecipitate Transfusion in Emergency Room by DR Riaz AhamedДокумент31 страницаPlatelet, FFP and Cryoprecipitate Transfusion in Emergency Room by DR Riaz AhamedAETCM Emergency medicineОценок пока нет
- Intravenous Fluid Therapy For Adults in Hospital Clinical GuidelineДокумент10 страницIntravenous Fluid Therapy For Adults in Hospital Clinical GuidelinePremaKurniaОценок пока нет
- GlomerulonephritisДокумент59 страницGlomerulonephritistressОценок пока нет
- Anaesthesia For Endovascular Surgery (Tevar and EvarДокумент18 страницAnaesthesia For Endovascular Surgery (Tevar and EvaranaeshklОценок пока нет
- Renal Transplant: 1) Steps Involved in Kidney TransplantationДокумент4 страницыRenal Transplant: 1) Steps Involved in Kidney TransplantationNadia SalwaniОценок пока нет
- Pneumocystis Carinii PneumoniaДокумент16 страницPneumocystis Carinii PneumoniaHera HeraОценок пока нет
- Embryology and Development of KidneyДокумент75 страницEmbryology and Development of Kidneyranjitha sraateОценок пока нет
- Anemia in CKD: Ppds Sp1 Divisi Ginjal Hipertensi Bagian Ilmu Penyakit Dalam Rsup Dr. Mohammad Hoesin Palembang 2021Документ31 страницаAnemia in CKD: Ppds Sp1 Divisi Ginjal Hipertensi Bagian Ilmu Penyakit Dalam Rsup Dr. Mohammad Hoesin Palembang 2021Richard 151289Оценок пока нет
- Hyperkalemia Approach AND Management: Dr. Renuka RayanaДокумент38 страницHyperkalemia Approach AND Management: Dr. Renuka RayanaSap ModulesОценок пока нет
- Hemophilia: Factor IX (Hemophilia B)Документ38 страницHemophilia: Factor IX (Hemophilia B)Jhvhjgj JhhgtyОценок пока нет
- Diabetes and NephrologyДокумент36 страницDiabetes and NephrologydrpbendreОценок пока нет
- On Admission:: STROKE MANAGEMENT (Beaumont Hospital)Документ3 страницыOn Admission:: STROKE MANAGEMENT (Beaumont Hospital)Nadia SalwaniОценок пока нет
- Controlled Hypotension: Moderator: DR V. Y. Srinivas Presenter: Dr. Ann Susan MathewДокумент49 страницControlled Hypotension: Moderator: DR V. Y. Srinivas Presenter: Dr. Ann Susan MathewAnn Susan MathewОценок пока нет
- Lung Metabolism: Proteolysis and Antioproteolysis Biochemical Pharmacology Handling of Bioactive SubstancesОт EverandLung Metabolism: Proteolysis and Antioproteolysis Biochemical Pharmacology Handling of Bioactive SubstancesAlain JunodОценок пока нет
- DermatomycosesДокумент34 страницыDermatomycosesRomMy WiEn MicKhoОценок пока нет
- ThalassemiaДокумент24 страницыThalassemiaRomMy WiEn MicKhoОценок пока нет
- Johannes H. SaingДокумент67 страницJohannes H. SaingRomMy WiEn MicKhoОценок пока нет
- Kul RadioДокумент87 страницKul RadioRomMy WiEn MicKhoОценок пока нет
- RD (Respirasi)Документ14 страницRD (Respirasi)RomMy WiEn MicKhoОценок пока нет
- Otitis MediaДокумент8 страницOtitis MediaRomMy WiEn MicKhoОценок пока нет
- Kul RadioДокумент87 страницKul RadioRomMy WiEn MicKhoОценок пока нет
- Anemia Post HemorrageДокумент26 страницAnemia Post HemorrageRomMy WiEn MicKhoОценок пока нет
- Pediatrics Neuromuscular Disorders: Lower Motor Neuron, GBS, Muscular DystrophiesДокумент49 страницPediatrics Neuromuscular Disorders: Lower Motor Neuron, GBS, Muscular DystrophiesRomMy WiEn MicKhoОценок пока нет
- Johannes H. SaingДокумент67 страницJohannes H. SaingRomMy WiEn MicKhoОценок пока нет
- Pediatric TuberculosisДокумент112 страницPediatric TuberculosisRomMy WiEn MicKhoОценок пока нет
- RD (Respirasi)Документ14 страницRD (Respirasi)RomMy WiEn MicKhoОценок пока нет
- AtelectasisДокумент8 страницAtelectasisRomMy WiEn MicKhoОценок пока нет
- Treating Bacterial Pleural EffusionsДокумент18 страницTreating Bacterial Pleural EffusionsRomMy WiEn MicKhoОценок пока нет
- EnsefalopatiДокумент13 страницEnsefalopatieby_3tamaОценок пока нет
- GI BleedingДокумент32 страницыGI BleedingRomMy WiEn MicKhoОценок пока нет
- RhinitisДокумент11 страницRhinitisRomMy WiEn MicKhoОценок пока нет
- Konsti Pas IДокумент15 страницKonsti Pas IRomMy WiEn MicKhoОценок пока нет
- SinusitisДокумент10 страницSinusitisRomMy WiEn MicKhoОценок пока нет
- Hyperglycemia in Critically Ill Children, Should It Be Treat AgressivelyДокумент30 страницHyperglycemia in Critically Ill Children, Should It Be Treat AgressivelyRomMy WiEn MicKho0% (1)
- Cell Injury Apoptosis.Документ78 страницCell Injury Apoptosis.RomMy WiEn MicKhoОценок пока нет
- Solute HypertonicityДокумент9 страницSolute HypertonicityRomMy WiEn MicKhoОценок пока нет
- Neonatal SepsisДокумент65 страницNeonatal SepsisRomMy WiEn MicKhoОценок пока нет
- Gangguan Plasental1Документ81 страницаGangguan Plasental1RomMy WiEn MicKhoОценок пока нет
- PPTДокумент19 страницPPTAhmad RamadhanОценок пока нет
- Bakteri Penyebab Infeksi Saluran KemihДокумент7 страницBakteri Penyebab Infeksi Saluran KemihRomMy WiEn MicKhoОценок пока нет
- Reading TextДокумент5 страницReading TextRomMy WiEn MicKhoОценок пока нет
- Obstetrics OverviewДокумент91 страницаObstetrics OverviewAbi TudОценок пока нет
- Eight Hallmarks of Cancer ExplainedДокумент40 страницEight Hallmarks of Cancer ExplainedArnab KalitaОценок пока нет
- LUMENIS Laser Article on Keloid and Scar Treatment GuidelinesДокумент8 страницLUMENIS Laser Article on Keloid and Scar Treatment GuidelinesAuroraОценок пока нет
- Study DesignДокумент130 страницStudy Designephremtigabie7Оценок пока нет
- AGada TantraДокумент3 страницыAGada TantraGuru Prasad100% (1)
- Clinical Profile of Indian Children With Down SyndromeДокумент5 страницClinical Profile of Indian Children With Down SyndromeRicky Wahyu setiawanОценок пока нет
- KEILMUAN DAN SENI DALM KEBIDANANДокумент18 страницKEILMUAN DAN SENI DALM KEBIDANANRizky Putri AndriantiОценок пока нет
- What Are The Different Types of Stress?Документ2 страницыWhat Are The Different Types of Stress?Полина КосьминаОценок пока нет
- Greater Political ParticipationДокумент12 страницGreater Political ParticipationBe-COOL State Of MindОценок пока нет
- J Paediatrics Child Health - 2017 - Halliday - The Fascinating Story of SurfactantДокумент6 страницJ Paediatrics Child Health - 2017 - Halliday - The Fascinating Story of SurfactantTin TomašićОценок пока нет
- Vet Histology Lecture Notes on Digestive System IДокумент62 страницыVet Histology Lecture Notes on Digestive System IDEV3LLS100% (3)
- Pharmacology Lab (1) : Routes of Drug AdministrationДокумент14 страницPharmacology Lab (1) : Routes of Drug AdministrationBotan AbdullahОценок пока нет
- Pflipsen Anaphylaxis Recognition and ManagementДокумент10 страницPflipsen Anaphylaxis Recognition and ManagementOlivia McCuskerОценок пока нет
- Cardiac Case Study NDДокумент11 страницCardiac Case Study NDapi-313165458Оценок пока нет
- Review Article: Guided Bone Regeneration: A Literature ReviewДокумент16 страницReview Article: Guided Bone Regeneration: A Literature ReviewGonçalo Gomes SanchesОценок пока нет
- A Prospective Study On Acute Limb Ischemia - Presentation, Management, Outcome - Our Institutional ExperienceДокумент6 страницA Prospective Study On Acute Limb Ischemia - Presentation, Management, Outcome - Our Institutional ExperienceIJAR JOURNALОценок пока нет
- Bailey 5th Ed. 2014 (1125-1318) - TraumaДокумент194 страницыBailey 5th Ed. 2014 (1125-1318) - TraumaelFadhlyОценок пока нет
- Expanding Consensus in Portal HypertensionДокумент29 страницExpanding Consensus in Portal HypertensionJosé Pepo Apey Reinoso100% (1)
- Fixed Prosthodontic Ii: Department of Fixed ProsthodonticsДокумент70 страницFixed Prosthodontic Ii: Department of Fixed Prosthodonticsعبد الرحمن خالد الزميليОценок пока нет
- The Impact of Good HealthДокумент5 страницThe Impact of Good HealthavasiОценок пока нет
- Treatment of Endometriosis in Women Desiring FertilityДокумент23 страницыTreatment of Endometriosis in Women Desiring FertilityVaisnavi Muthoovaloo67% (3)
- 2015parathyroid Carcinoma Challenges in Diagnosis and TreatmentДокумент9 страниц2015parathyroid Carcinoma Challenges in Diagnosis and TreatmentCharley WangОценок пока нет
- Rubrics Normal DeliveryДокумент3 страницыRubrics Normal DeliveryKYLE MITZIE SENGCOОценок пока нет
- 3.2. The Hospital Medical VocabularyДокумент7 страниц3.2. The Hospital Medical VocabularyMarkus ZahndОценок пока нет
- ImmunosuppressionДокумент1 страницаImmunosuppressionabc007200Оценок пока нет
- Chapter 24 - Arthritis - Osteoarthritis, Gout, & Amp Rheumatoid ArthritisДокумент23 страницыChapter 24 - Arthritis - Osteoarthritis, Gout, & Amp Rheumatoid ArthritisHarris GhifaryОценок пока нет
- 9 Amazing Eucalyptus Oil Benefits You Need To KnowДокумент1 страница9 Amazing Eucalyptus Oil Benefits You Need To KnowBabalwa JaliОценок пока нет
- Anomalies of ConvergenceДокумент12 страницAnomalies of ConvergenceDaniDenzongpaSulaemanОценок пока нет
- Journal TetanusДокумент10 страницJournal TetanusWinariieeyy NayyОценок пока нет