Академический Документы
Профессиональный Документы
Культура Документы
Fever in Children and FUO
Загружено:
aldiansyahrauf0 оценок0% нашли этот документ полезным (0 голосов)
58 просмотров61 страницаThis document discusses fever in children. It covers normal body temperature, the definition of fever, pathogenesis and pathophysiology of fever, patterns of fever, fever in clinical settings, and treatment. Fever is an important defense mechanism in children and is usually caused by infections, though sometimes other conditions. The body's temperature is regulated by the hypothalamus and fevers result from the elevation of the thermoregulatory set point. Potential complications include dehydration, febrile seizures, and hyperpyrexia.
Исходное описание:
Оригинальное название
Fever in Children and FUO.pptx
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документThis document discusses fever in children. It covers normal body temperature, the definition of fever, pathogenesis and pathophysiology of fever, patterns of fever, fever in clinical settings, and treatment. Fever is an important defense mechanism in children and is usually caused by infections, though sometimes other conditions. The body's temperature is regulated by the hypothalamus and fevers result from the elevation of the thermoregulatory set point. Potential complications include dehydration, febrile seizures, and hyperpyrexia.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
58 просмотров61 страницаFever in Children and FUO
Загружено:
aldiansyahraufThis document discusses fever in children. It covers normal body temperature, the definition of fever, pathogenesis and pathophysiology of fever, patterns of fever, fever in clinical settings, and treatment. Fever is an important defense mechanism in children and is usually caused by infections, though sometimes other conditions. The body's temperature is regulated by the hypothalamus and fevers result from the elevation of the thermoregulatory set point. Potential complications include dehydration, febrile seizures, and hyperpyrexia.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 61
Fever in Children
Sri Rezeki S Hadinegoro
Dept of Child Health
Faculty of Medicine, University of Indonesia
Lecture
Lecture FKUI 2011
Fever
Normal body temperature
Definition of fever
Pathogenesis & pathophysiology of fever
Pattern of fever
Fever in the clinical setting
Treatment
FUO
Topics
Normal body temperature reached highest level
in early evening (5-7 p.m)
Young children: relatively high rectal temperature
predominate
Diurnal temperature
children have more fluctuated than adult
Gradually decreased towards adult levels beginning
at 2 years of age, trend stabilizes soon after puberty
Normal Body Temperature
Diurnal pattern of body temperature
Diurnal temperature in children more fluctuated
than in adults
Location Thermometer
Normal
temperature
Range, mean (
o
C)
Fever (
o
C)
Axilla Mercury, electronic 34.7 37.3; 36.4 37.4
Sublingual Mercury, electronic 35.5 37.5; 36.6 37,6
Rectal Mercury, electronic 36.6 37.9; 37.0 38.0
Ear Infra red emission 35.7 37.5; 36.6 37.6
Measurement of body temperature
Recommendation site of measurement
Age < 4 weeks: electronic thermometer axilla
Age >4 weeks to 5 years: electronic thermometer axilla,
mercury thermometer axilla, infrared tympanic thermometer
Fever is increased body temperature of 1
0
C or
greater above mean temperature
Clinical setting
Rectal temperature > 38.0 C
Oral temperature > 37.6 C
Axillary temperature > 37.4 C
Tympanic membrane > 37.6 C
Definition
Most common cause of fever in children are
infection, hypersensitivity reaction,
autoimmune diseases, and malignancy
Febrile response is mediated by endogenous
pyrogens (EP, cytokines) in response to
invading exogenous pyrogens, primarily
microorganisms or their product (toxins)
Pathogenesis of Fever
Endogenous pyrogen acts on thermosensitive
neurons in hypothalamus, which upgrade the
set point via prostaglandins
Body reacts by increasing the heat production
and decreasing the heat loss until the body
temperature reaches this elevated set point
Fever will control effectively by hypothalamic
center
Pathogenesis of Fever
Mechanisms of Fever Production
Cytokines play a pivotal role in the immune
response by activation of the B cells and T
cell lymphocytes
Production of fever is strongly evidence as a
defence body mechanism
Fever become harmfull or fatal by
overproduction of cytokines or imbalance
between cytokine & their inhibitors (severe
infection and septic shock)
Pathogenesis of Fever
Fever is an interleukin-1 (IL-1) mediated elevation of the
thermoregulatory set point of the hypothalamic centre.
In response to an upward displacement of the set points,
an active process occurs in order to reach the new set point
minimizing heat loss with vasoconstriction
producing heat with shivering
Pathophysiology of Fever (1)
The regulation of body temperature
Behavioral means of raising body
temperature include seeking
a warmer environment,
adding more clothing,
curling up in bed,
drinking warm liquids.
Pathophysiology of Fever (2)
Fever is not dangerous
Fever is a body defence mechanism
Morbidity & mortality due to underlying disease
Fever does not damage the central nervous system
Controlled by a hypothalamic centre
Phase of Fever
Phase of temperature
raise
Phase of temperature
stabilization (fastigium)
Characterized by
discomfort
Result of decreased
heat loss through
vasoconstriction &
increased heat
production through
shivering
Child feels cool, skin
feels cold to the
touch
New level of
thermoregulatoy set
point
Balance heat
production & heat loss,
at a higher
hypothalamic set point
Flushed or pink face
appearance signifies
that fever has peaked
Child feels comfort
without shivering
Phase of falling temperature
or defervescence
Occur either by lysis
(falling gradulally
within 2-3 days to a
normal level) or crisis
(falling within a few
hours to normal level)
Pattern Diseases
Continuous Typhoid fever, malignant malaria falciparum
Remittent Most viral or bacterial diseases
Intermittent Malaria, lymphoma, endocarditis
Septic or hectic Kawasaki disease, pyogenic infection
Quotidian Malaria (P.vivax)
Double quotidian Juvenile rheumatoid arthritis, some drug fever
(carbamazepine), Kalaazar, gonococcal
arthritis
Relapsing/periodic Quartana & tertiana malaria, brucellosis
Recurrent fever Familial Mediterranean fever
Pattern of Fever
Continuous Fever (sustained fever)
Typhoid fever, malignant malaria falciparum
Sustained increased body temperature with maximal
fluctuation 0,4
0
C for 24 hours periode
Diurnal body temperature does not significance appear
N
o
r
m
a
l
l
e
v
e
l
3
7
.
5
0
C
Remittent Fever
Most viral or bacterial diseases
Temperature decreased every day but never reach normal level with fluctuation
more than 0.5
0
C per 24 hours
The most frequent fever pattern in pediatric practice, no spesific for certain diseases
Diurnal variation showed particularly if fever due to infection process
N
o
r
m
a
l
l
e
v
e
l
3
7
.
5
0
C
Intermitent Fever
Malaria, lymphoma, endocarditis
Every day body temperature reached normal level at the
morning and highest level at noon
This pattern is the second most frequent found in pediatric
practices
at noon
morning
Quotidian Fever
Malaria (P.vivax)
Body temperature
increased gradually within every four days
Periodic Fever
Pattern of Fever in Malaria
Recurrent fever
Borrelia (louse borne), ticks borne disease
Normal level of body temperature
Biphasic Fever
Dengue fever, poliomyelitis, leptospirosis, yellow fever, Colorado tick fever,
spirillary rat-bite fever, African hemorrhagic fever (Marburg, Ebola, Lassa)
Camelback fever pattern or saddleback fever
Showed two fever episodes in one disease
T
e
m
p
e
r
a
t
u
r
e
0
C
Time of fever defervescence
Measles, Rubeola
Skin rash (maculopapular rash) appeared when body
temperature reached the highest level
11/1/2014
Natural history of diseases
11/1/2014
Rash distribution
Exanthemas
11/1/2014
11/1/2014
Varicella Zoster Infection
Presence of all stages of lesions in one area
Differential diagnosis Acute Exanthema
Maculopapular eruptions
Measles
Rubella
Scarlet fever
Meningococcemia
Toxoplasmosis
Cytomegalovirus infecton
Roseola infantum
Enteroviral infection
Drug eruptions
Miliaria
Kawasaki disease
others
11/1/2014
Differential diagnosis of Acute Exanthema
Papulovesicular eruptions
Varicella-zoster infection
Smallpox
Excema herpeticum
Coxsackie virus infection
Rickettsial pox
Impetigo
Insect bites
Drug eruptions
Molluscum contagiosum
Papular urticaria
others
11/1/2014
37
0
C
40
0
C
Complications
Day -15 Day 0 Day 7 Day 21
Incubation
period
Asymtomatic
Invasive phase
Intermitent fever
Headache
Fatique
Abdominal discomfort
Constipation
Diarrhoea
Toxic phase
Continuous fever
Bradycardia
Hepatomegaly
Splenomegaly
Constipation
Diarrhoea
Rose spot
Convalescence
period
Typhoid Fever, Typhus Abdominalis
History of illness
Symptoms
Chills (rigor), myalgia, headaches, anorexia, excessive
sleep, fatigue, thirst, delirium, scanty urine (oliguria)
Signs
Drowsiness, irritability, tachycardia, tachypnoea,
increased BP, flushed face, grunting, decrease in GFR<
proteinuria. Appearance of an innocent (functional)
murmur & third heart sound
ECG changes
Shortening QT-interval, increased in supraventricular
ectopic beats
Clinical changes noted during fever
Dehydration
Result of increased body temperature & therapeutic effect of drugs
that promoting sweating
Fever & infection increase the metabolic rate to >1.5 time the basal
metabolic rate (1 degree C = 10% increase of insensible water loss)
Prevent & treated by providing extra fluid to the
Febrile convulsion
Mostly has a familial history of febrile convulsion
Genetically hypothalamic center susceptible to high body
temperature (imbalance of thermoregulator)
Incidence in 6 months to 4 years of ages
Prevent & treated by antipyretic & anticonvulsion drug
Potential Complication (1)
Hyperpyrexia (by Dubois)
Imbalance between heat production and loss
, not controlled centrally
Rectal temp 41.1
0
C or higher or axillary/
tympanic temp >40
0
C
Young infants with hyperpirexia suggested to
have severe infection (serious bacterial
infection)
Potential Complication (2)
Classification
Definition
Most frequent
etiology
Duration of
fever
Fever with
localizing signs
Acute febrile illness with focus
infection which could be
diagnosed by anamnesis &
physical examination
Upper respiratory
tract infection (URTI)
< 1 week
Fever without
localizing signs
Acute febrile illness without
focus infection diagnosed after
anamnesis & physical
examination
Viral infection,
urinary tract infection
(UTI)
< 1 week
Fever of
unknown origin
Fever occured minimal 3 weeks,
no established diagnosis yet after
1 week investigation at hospital
Infection, juvenile
idiopathic arthritis
> 1 week
Classification of Fever
Organ system Diseases
Upper airway infections Viral URTI, otitis media,tonsillitis,
laryngitis, herpetic stomatitis
Pulmonary Bronkhiolitis, pneumonia
Gastrointestinal Gastroenteritis, hepatitis, appendicitis
CNS Meningitis, encephalitis
Exanthems Campak, chicken pox
Collagen Rheumathoid arthritis, Kawasaki disease
Neoplasma Leukemia, lymphoma
Tropics Kala azar, cickle cell anemia
Main causes of
fever due to disease of localized signs
Acute febrile illness with focus of infection, which can be diagnosed
after history & physical examination
About 20% all febrile episodes demonstrate no localizing signs
Most common cause is a viral infection
Most occuring during the first few years of life
Fever without localizing signs
Serious infections occured in 1% cases:
serious bacteriemic infections (SBIs)
Children 3-24 months have the highest incidence (3-4%),
aged 7-12 months demonstrating twice incidence
association with high fever >39.5
0
C
Etiology Causes Diagnostic tools
Infections Bacteremia/sepsis
Most virus (HH-6)
UTI
Malaria
Ill looking, high CRP, leukocytosis
Well appearing, nomal CRP, WBC
Urine dipsticks
In malarial area
FUO
Juvenile idiopathic
arthritis
Pre-articular, rash, splenomegaly, high
antinuclear factor, CRP
Post vaccination DTwP, measles Time of fever onset in relation to the time
of vaccination
Drug fever Most drug History of drug intake, diagnosis of
exclusion
Usual causes of fever without localized signs
Definition of Fever of Unknown Origin
(Unknown Source)
FUO defined when fever without localizing signs
persists
for one week during which evaluation in hospital
fails to
detect the cause
Cause of FUO
Infection 60%-70%
Localized infections
Systemic infections
Collagen diseases 20%
Neoplasma 2%
Miscellenous 5%-10%
Lack of laboratory facilities
No experience to certain cases (rare case)
Not do the history on travel abroad, animal exposure,
prior use antibiotics
Repeated physical examinations are more helpful
Causes Diseases Reasons of being a case of FUO
Infection (60%-70%)
Repeated history taking & repeated
physical examination
Localized
Sinusitis
Endocarditis
Occult abscess
Sinus radiograph not performed or
negative
Previously unsuspected of having cardiac
defect
Absence of clinical signs
Systemic
Viral
TB
Kawasaki disease
Fever is the only sign of disease
Extrapulmonary, tuberculin test negative
Incomplete presentation, diagnosis not
considered
Principles causes of FUO
Causes Diseases Reasons of being a case of FUO
Collagen
(about 20%)
JIA
SLE
Prearthritis presentation
Atypical manifestation
Neoplasma
Leukemia
Lymphoma
Neuroblastoma
Atypical presentation, blood tests neg
Unusual localization
Disseminated
Miscellaneous
(5%-10%)
Drug fever
Factitious fever
Diagnosis not considered, suspected drug
not stopped
Diagnosis not considered, thermometer
left to patient
Principles causes of FUO
Algorithmic approach to FUO
Step 1
Repeated anamnesis, physical examination &
laboratory examination
Evaluation: is there any specific signs & symptoms
Step 2
Option 1: found the specific signs & symptom
examination additional specific lab
Option 2: no any specific signs & symptom repeated
FBC
Evaluation option 1 & 2, go to step 3
Step 3
More comprehensive examination, consultation to
other specialist, including invasive procedure
Anamnesis
Age
Age < 6 years: UTI, local infection (abcess, osteomyelitis), JRA
Children > 6 years: TB, collitis, autoimmune disease, neoplasma
Characteristic of fever
When, duration, and type of fever
Non-specific symptoms (fatique, headache, stomac-ache, chill)
Epidemiological data
Animal exposure
Travel aboard
Genetic
Drugs used
Physical examinations
Detail physical examinations are needed
Special attention to certain part
Heart sound (endocarditis)
Joint, lymph nodes, muscle (myalgia),
Pain of extrimities (SLE)
Icterus (hepatitis)
Skin rash (vascular-collagen disease, Kawasaki disease)
Peritonsillar abscess
Mass intra abdominal
Blood stool
Green low risk Yellow-intermediate Red high risk
Colour Normal colour of skin, lips,
tounge
Pallor reported parents Pale, mottled, blue
Activity Respond normal to social
cues, smiles, stay awake or
awakens quiclky
Stronge normal crying
Not responding normal
social cues, wakes with
prolonged stimulation
Decreased activity, no smile
No respond to social cues
Appear ill to health care
professional
Does not wake
Weak, high-piched crying
Respiratory Normal respiratory rate Nasal flaring, tachypnoea
Oxygen saturation <95%
Crackles
Grunting
Tachypnoea
Moderate or severe chest
indrawing
Hydration Normal skin & eyes
Moist mucous membranes
Dry mucous membrane
Poor feeding in infants
CRT 3 seconds
Reduced urine output
Reduced skin turgor
Temperature:
0-3 mos 38
0
C
3-6 mos 39
0
C
Other None yellow or red signs Fever 5 days Bulging of fontanel
Neck stiffness
Swelling limb or joint Local seizure
Neurological signs
Bile stained vomiting
Clinical illness severity in children
The Yale Observation Scale (YOS)
The Yale Observation Scale
National Collaborating Centre for Womens and Childrens
Health:
Skor YOS + anamnesis + pemeriksaan fisik: sensitifitas 89%-93%
dan NPV 96%-98%.
Nilai total skor 6 pada kelompok umur 3 bulan-3 tahun, dapat
mendeteksi occult bacteriemia dengan NPV 97,4%.
Pratiwi , Tumbelaka AR. dkk. dalam penelitiannya di
Departemen IKA FKUI/RSCM, RS Fatmawati, dan RS
Harapan Kita di Jakarta, 2010
256 kasus demam dengan skor 8 : sensitivitas 69,35%,
spesifisitas 90,2%, PPV 69,35%, NPV 90,2%, rasio kemungkinan
positif 7,08, dan rasio kemungkinan negative 0,34.
Laboratory examination
Laboratorium examination as a tools for
looking to the cause
An important part to established the
diagnosis
Recommend done gradually, not at the
same time for many examinations
Depend on severity of the disease
Step 1
FBC, blood smear, blood cell morphology
Chest x-ray
Tick blood smear
BSR, CRP
Urine analysis
LCS, other body fluid depend on indication
Blood, urine, stool, nasopharyngeal swab culture
Tuberculin test
Liver function test
Laboratory examination
* Note: in serious case, lab procedure should be performed more rapidly
Step 2
Serological test: Salmonella, toxoplasma, leptospira,
mononucleosis, CMV, histoplasma
Ultrasonography: abdominal, skull
Step 3
Bone marrow puncture
Intravenous pyelography
Paranasal sinus photography
Antinuclear antibody (ANA)
Barium enema examination
Scanning examination
Liver biopsy
Laparatomy diagnostic
Laboratory examination
Ill-looking or <1 month
Outpatient clinic
Option 1
CBC , blood culture
Urine exam & culture
Chest x-ray
Stool micros & culture
(if indicated)
Abnormal labs or x-ray
Antibiotic
Option 2
As in option 1
+ CSF
Hospital addmission
Blood culture
Urine examination
Complete blood count
Chest x-ray
CSF
IV antibiotic
Management of child aged
0-< 3months without a focus of infection
No
Yes
Management of child aged 3-36 months
without a focus of infection
Ill-looking
child
Hospitalization
administer
antibiotic
Not ill-looking
body temperature
<39
0
C
Urine
dipstick,
review if
condition
worsen
Body temperature > 39
0
C
Evaluate for SBIs
Option 1
Urine dipstick, CBC, blood
culture, CXR, consider
antibiotic
Option 2
Urine, no blood test,
evaluation if the condition
worsen
Option 3
CBC, if WBC > 15.000/mm
3,
blood culture, consider
antibiotic
ICU
FUO case clinical
setting
Antipyretic act centrally by lowering the
thermoregulatory set point of the hypothatalamic
center
Inhibition of cyclooxygenase, the enzyme responsible
for the conversion of arachidonic acid to prostaglandin
Antipyretic
The main indication for prescribing an antipyretic is not
to reduce body temperature but to relieve the childs
discomfort & reduced parents anxiety
Give rapid result and be effective in reducing fever by
at least 1
0
C
Be available in liquid and suppository form
Have low rate of side effect in theurapeutic doses
Have low incidence of interaction with other
medications and rarely contraindication in pediatric
doses
Be safe
Be cost effective
Characteristic of an ideal antipyretic
Medications & Physical Measures
Para-aminophenols
Paracetamol
Propionic acid derivates
Ibuprofen
Naproxen
Salicylates
Aspirin
Other NSAIDs
Diclofenac
Endogenous antipyretic
Arganine vasopressin
Physical measures
Bed rest
Tepid sponging
Antipyretic Oral Rectal Intravenous
Paracetamol Tablet
500 mg
Liquid
120mg/5ml or
250mg/5ml
Suppository
60, 125, 500mg
Infusion 10mg
Children
10-15 mg/kg at 4-6 hrs or
60-75mg/kg per day
Same as oral 15mg/kg
Ibuprofen Tablet
500 mg
Liquid
120mg/5ml or
250mg/5ml
Suppository
60, 125, 500mg
Children
5mg/kg at 3-4 hrs, dose 10mg/kb more potent
& has longer lasting fever suppression than PCT
Same as oral
Doses of antipyretics
58
Spektrum
sempit atau
luas
Bakterisidal
atau
bakteriostatik
Mono atau
kombinasi
Intravena
atau oral
Empiris atau
definitif
Kriteria
pemilihan
antibiotik
Alur pengobatan
infeksi bakteri
59
Infeksi
bakteri
Biakan
(Gram stain)
Identifikasi
patogen
Terapi
definitif
Antibiotik
spektrum
sempit
Sembuh
Terapi empiris
Diduga
Fever is a body defence mechanism, controlled by a
hypothalamic centre
Fever does not damage the central nervous system
Morbidity & mortality due to underlying disease
Fever become harmful by overproduction of cytokines or
imbalance between cytokine & their inhibitors (hyperthermia)
The main indication of giving antipyretic is not to reduce body
temperature but to relieve the childs discomfort & reduced
parents anxiety
Conclusions
Conclusions
FUO defined when fever without localizing signs persists
for one week during which evaluation in hospital fails to
detect the cause
60%-70% cause of FUO is infection
Reasons of being a case of FUO
Lack of laboratory facilities
No experience to certain cases (rare case)
Not do the history on travel abroad, animal exposure,
prior use antibiotics
Repeated physical examinations are more helpful
Вам также может понравиться
- Phlebotomy Course OutlineДокумент7 страницPhlebotomy Course OutlineDegee GonzalesОценок пока нет
- Position Statements of The PSAAI On COVID19 Vaccines and Their Adverse Reactions August 5 2021 ClickableДокумент25 страницPosition Statements of The PSAAI On COVID19 Vaccines and Their Adverse Reactions August 5 2021 ClickableMonica LowinskiОценок пока нет
- NCP Sexual DisfunctionДокумент10 страницNCP Sexual DisfunctionDeca Tan50% (6)
- Bells Palsy or Stroke 02.06.2019Документ19 страницBells Palsy or Stroke 02.06.2019Emily EresumaОценок пока нет
- TularemiaДокумент19 страницTularemiaEmily EresumaОценок пока нет
- CHCECE002 Theory Tasks v8Документ46 страницCHCECE002 Theory Tasks v8Palvi Sharma100% (1)
- MSF HIV-TB Clinical Guide EnglishДокумент365 страницMSF HIV-TB Clinical Guide EnglishAhmed Dbb100% (2)
- Fever in Children and FUOДокумент62 страницыFever in Children and FUOAmbartyas Niken WОценок пока нет
- Approach To FeverДокумент80 страницApproach To FeverRaditia AbrahamОценок пока нет
- Fever in Children: Dept of Child Health Faculty of Medicine, University of IndonesiaДокумент40 страницFever in Children: Dept of Child Health Faculty of Medicine, University of IndonesiaMahesa RamadhiantoОценок пока нет
- Effect of Ursodeoxycholic Acid On Indirect Hyperbilirubinemia in Neonates Treated With PhototherapyДокумент4 страницыEffect of Ursodeoxycholic Acid On Indirect Hyperbilirubinemia in Neonates Treated With PhototherapyEka Satria AnanditaОценок пока нет
- Infective Endocarditis IeДокумент26 страницInfective Endocarditis IeAnthie FitriОценок пока нет
- Botulism 08.16.2013Документ12 страницBotulism 08.16.2013Emily EresumaОценок пока нет
- Approach To Child With WheezingpediatricsДокумент25 страницApproach To Child With WheezingpediatricsshahinaОценок пока нет
- Morning Report 9/5/18: Adam Cardullo, MD Pgy - 2Документ22 страницыMorning Report 9/5/18: Adam Cardullo, MD Pgy - 2Emily EresumaОценок пока нет
- Approach To Ill Looking ChildДокумент66 страницApproach To Ill Looking ChildUzair MuhdОценок пока нет
- 1 RicketsДокумент32 страницы1 RicketsDarina Ismakaieva100% (1)
- Surfactant ReplacementДокумент40 страницSurfactant ReplacementDr.Sushree Smita BehuraОценок пока нет
- Referat HDKДокумент29 страницReferat HDKAga Haris100% (1)
- Hyperinsulinisminthe Neonate: Katherine Lord,, Diva D. de LeónДокумент14 страницHyperinsulinisminthe Neonate: Katherine Lord,, Diva D. de LeónMaría Paula Sarmiento RamónОценок пока нет
- Pediatric Urology Topics Relating To Infants & Toddlers: Danielle Brady, Pgy-2Документ35 страницPediatric Urology Topics Relating To Infants & Toddlers: Danielle Brady, Pgy-2Emily EresumaОценок пока нет
- Perinatal Asphyxia: Walter Otieno Consultant PaediatricianДокумент25 страницPerinatal Asphyxia: Walter Otieno Consultant PaediatricianMalueth AnguiОценок пока нет
- Graves' Disease & PregnancyДокумент19 страницGraves' Disease & Pregnancyrajan kumar100% (1)
- KEPILEPSY PresentationДокумент39 страницKEPILEPSY PresentationalotfyaОценок пока нет
- FEVER Approach (Paeds)Документ3 страницыFEVER Approach (Paeds)NorFarah Fatin AnuarОценок пока нет
- Special Sense System Group 6Документ24 страницыSpecial Sense System Group 6RushdaОценок пока нет
- Larsen Syndrome: - Dr. Kapil R JagtapДокумент23 страницыLarsen Syndrome: - Dr. Kapil R JagtapKapil JagtapОценок пока нет
- Neonatal Hyperbilirubinemia: Presenter: DR Rakesh Dey DM Resident Dept of NeonatologyДокумент70 страницNeonatal Hyperbilirubinemia: Presenter: DR Rakesh Dey DM Resident Dept of Neonatologyrakesh deyОценок пока нет
- Practice Based Learning (Grand Round)Документ48 страницPractice Based Learning (Grand Round)AnnumОценок пока нет
- Respiratory Distress Syndrome: Islamic University Nursing CollegeДокумент21 страницаRespiratory Distress Syndrome: Islamic University Nursing Collegeyaumil agisnaОценок пока нет
- Neonatal Hepatitis SyndromeДокумент18 страницNeonatal Hepatitis Syndromeenny_rommyОценок пока нет
- Drugs in The Neonatal Unit: 1 Julia PettyДокумент5 страницDrugs in The Neonatal Unit: 1 Julia PettyMarjoОценок пока нет
- Cerebral Palsy (CP)Документ16 страницCerebral Palsy (CP)Divija ChowdaryОценок пока нет
- Febrile SeizuresДокумент11 страницFebrile SeizuresLita Al AmudiОценок пока нет
- Pneumonia: Past and Present: Dr. Pushpa Raj Sharma Professor of Child Health Institute of MedicineДокумент41 страницаPneumonia: Past and Present: Dr. Pushpa Raj Sharma Professor of Child Health Institute of MedicineKartika RezkyОценок пока нет
- Neonatal Jaundice Prolonged Jaundice: by Mohd Zamir GhouseДокумент18 страницNeonatal Jaundice Prolonged Jaundice: by Mohd Zamir GhousezamirsgОценок пока нет
- 12 Neonatal Hypocalcemia, Glycemia and MagnesemiaДокумент55 страниц12 Neonatal Hypocalcemia, Glycemia and MagnesemiaRana Vandana100% (1)
- Protein Calorie MalnutritionДокумент97 страницProtein Calorie Malnutritionnshaikh56Оценок пока нет
- Hypo ToniaДокумент56 страницHypo ToniaKRITHIKA A/P PALANNY MoeОценок пока нет
- DR Supriyanto Spa SMF Kes Anak Rsms PurwokertoДокумент62 страницыDR Supriyanto Spa SMF Kes Anak Rsms PurwokertoSylvia Delti ElviraОценок пока нет
- Neonatal Jaundice DR - MaslianiДокумент58 страницNeonatal Jaundice DR - MaslianiHengky HanggaraОценок пока нет
- Anaphylaxis Case PedsCasesДокумент5 страницAnaphylaxis Case PedsCasesSara Ilyas KhanОценок пока нет
- Hypothyroidism in PregnancyДокумент29 страницHypothyroidism in PregnancyhanaddulОценок пока нет
- Sepsis PowerPointДокумент49 страницSepsis PowerPointWonyenghitari GeorgeОценок пока нет
- Congenital Adrenal HyperplasiaДокумент29 страницCongenital Adrenal HyperplasiaMohan RaoОценок пока нет
- Hypocalcemia - Endocrinology AdvisorДокумент14 страницHypocalcemia - Endocrinology AdvisorAliHussainОценок пока нет
- Kole StasisДокумент16 страницKole StasisAlia SalviraОценок пока нет
- Neonatal CholestasisДокумент13 страницNeonatal Cholestasisgts999Оценок пока нет
- Follow-upoftheNICUPatient Medscape FormatДокумент65 страницFollow-upoftheNICUPatient Medscape FormatJohn ParudaОценок пока нет
- Celiac Disease in ChildrenДокумент59 страницCeliac Disease in Childrend-fbuser-57045067Оценок пока нет
- Nephrotic SyndromeДокумент40 страницNephrotic SyndromesangheetaОценок пока нет
- Understanding Epilepsy and Its Homeopathic AnswerДокумент21 страницаUnderstanding Epilepsy and Its Homeopathic AnswerDr. Sandeep Anwane100% (3)
- Normal NewbornДокумент127 страницNormal Newbornjanetwillams100% (3)
- Primary Adrenal InsufficiencyДокумент26 страницPrimary Adrenal InsufficiencyEmily EresumaОценок пока нет
- Neonatal Seizures: Dr. Venkatesh Postgraduate Dept of Pediatrics S V Medical CollegeДокумент43 страницыNeonatal Seizures: Dr. Venkatesh Postgraduate Dept of Pediatrics S V Medical CollegeManju ManjunathОценок пока нет
- Newborn Screening: Alyssa Nicole B. ReyesДокумент12 страницNewborn Screening: Alyssa Nicole B. ReyesJohn Christian LasalitaОценок пока нет
- Central Nervous System AbnormalitiesДокумент56 страницCentral Nervous System AbnormalitiesApin PokhrelОценок пока нет
- Febrile Seizure Case FileДокумент4 страницыFebrile Seizure Case Filehttps://medical-phd.blogspot.comОценок пока нет
- Neonatal JaundiceДокумент23 страницыNeonatal JaundiceAsad M AminОценок пока нет
- 4 EpilepsyДокумент25 страниц4 EpilepsymuhammadridhwanОценок пока нет
- Masalah Gastrointestinal KolestasisДокумент21 страницаMasalah Gastrointestinal KolestasisMuthi'ah Ramadhani AgusОценок пока нет
- GuidelineДокумент3 страницыGuidelinebelvacuteОценок пока нет
- Hypoglycaemia FinalДокумент31 страницаHypoglycaemia FinalJian Han LiewОценок пока нет
- Fanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandFanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- Hereditary Spherocytosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОт EverandHereditary Spherocytosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsОценок пока нет
- ECG InterpretationДокумент81 страницаECG InterpretationaldiansyahraufОценок пока нет
- Appendix 5. Melbourne Ambulance Stroke Screen (MASS) : Clinical History ElementsДокумент1 страницаAppendix 5. Melbourne Ambulance Stroke Screen (MASS) : Clinical History ElementsaldiansyahraufОценок пока нет
- Absorpsi Makromolekuler Oleh Usus Atan Baas Sinuhaji Bika Fk-Usu/Rs HamДокумент22 страницыAbsorpsi Makromolekuler Oleh Usus Atan Baas Sinuhaji Bika Fk-Usu/Rs HamaldiansyahraufОценок пока нет
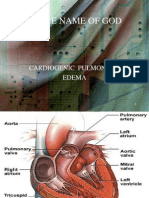
- In The Name of God: Cardiogenic Pulmonary EdemaДокумент51 страницаIn The Name of God: Cardiogenic Pulmonary EdemaaldiansyahraufОценок пока нет
- Hyponatremia in Neurological Diseases in ICU: Review ArticleДокумент5 страницHyponatremia in Neurological Diseases in ICU: Review ArticlealdiansyahraufОценок пока нет
- Tugas Dr. ATJSДокумент7 страницTugas Dr. ATJSaldiansyahraufОценок пока нет
- Best Practice & Research Clinical Endocrinology & MetabolismДокумент9 страницBest Practice & Research Clinical Endocrinology & MetabolismaldiansyahraufОценок пока нет
- Sabiston Textbook of Surgery, 19th Ed: VGHTCДокумент85 страницSabiston Textbook of Surgery, 19th Ed: VGHTCaldiansyahraufОценок пока нет
- Lymphangitis & LymphadenitisДокумент6 страницLymphangitis & LymphadenitisaldiansyahraufОценок пока нет
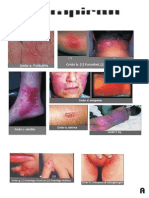
- Lampiran: GMBR B. (1) Furunkel, (2) Karbunkel GMBR B. (1) Furunkel, (2) Karbunkel GMBR A. Folikulitis GMBR A. FolikulitisДокумент4 страницыLampiran: GMBR B. (1) Furunkel, (2) Karbunkel GMBR B. (1) Furunkel, (2) Karbunkel GMBR A. Folikulitis GMBR A. FolikulitisaldiansyahraufОценок пока нет
- New Classification and Colour Code Development For An Efficient Medical Waste SegregationДокумент12 страницNew Classification and Colour Code Development For An Efficient Medical Waste SegregationGlobal Research and Development ServicesОценок пока нет
- Journal Pre-ProofДокумент58 страницJournal Pre-Proof묭Оценок пока нет
- Practical Guide - LymeherbsДокумент56 страницPractical Guide - Lymeherbsalba lopezОценок пока нет
- Hygienic Condition InspectionДокумент14 страницHygienic Condition InspectionjoechengshОценок пока нет
- Diagnostic Report: Patient Name: Ritesh Sharma RITSF30101992 0202UB003850Документ2 страницыDiagnostic Report: Patient Name: Ritesh Sharma RITSF30101992 0202UB003850Dhyan VigyanОценок пока нет
- أسئلة مايكروДокумент7 страницأسئلة مايكروazoz254Оценок пока нет
- Group 2 SIGNIFICANCE OF THE STUDYДокумент1 страницаGroup 2 SIGNIFICANCE OF THE STUDYMara CabreraОценок пока нет
- Prevention of PneumoniaДокумент2 страницыPrevention of Pneumoniaella19inaОценок пока нет
- Unit 5: Education, Health and Land TransportДокумент56 страницUnit 5: Education, Health and Land TransporthabtamuОценок пока нет
- Nursing Practice 1 QuestionДокумент12 страницNursing Practice 1 QuestiongranfrancoОценок пока нет
- Disease and First AidДокумент4 страницыDisease and First AidPriyadharsini BalasubramanianОценок пока нет
- HSE National Cleaning Standards ManualДокумент149 страницHSE National Cleaning Standards ManualNemer MansourОценок пока нет
- Infection Control Manual 1Документ54 страницыInfection Control Manual 1Botanic Hair Oil100% (1)
- Clove Magic WorkshopДокумент13 страницClove Magic Workshoppriyanka100% (1)
- Questions:: Reading Comprehension PracticeДокумент44 страницыQuestions:: Reading Comprehension PracticeAmmar QureshiОценок пока нет
- Copy (2) of ThesisДокумент20 страницCopy (2) of Thesiscaridadlintao100% (1)
- PinwormsДокумент2 страницыPinwormsPieck FingerОценок пока нет
- Food Borne Diseases - 0Документ131 страницаFood Borne Diseases - 0Nur FithriahОценок пока нет
- 1.1 Identify The Differences Between Bacteria, Viruses, Fungi and ParasitesДокумент4 страницы1.1 Identify The Differences Between Bacteria, Viruses, Fungi and ParasitesgemmaОценок пока нет
- M10 FundaДокумент6 страницM10 FundaAl-Khan HadjailОценок пока нет
- English10 Q3 LC3Документ12 страницEnglish10 Q3 LC3Ivy SalazarОценок пока нет
- Staphylococcus AureusДокумент3 страницыStaphylococcus AureusDenisse Watt CuarterosОценок пока нет
- Become Healthy or Extinct by Darryl D'Souza-1Документ288 страницBecome Healthy or Extinct by Darryl D'Souza-1Asha ShivaramОценок пока нет
- What Causes Malaria?Документ8 страницWhat Causes Malaria?Dulce M. LupaseОценок пока нет
- Sepup - Cell BiologyДокумент104 страницыSepup - Cell BiologyOmar YahiaОценок пока нет