Академический Документы
Профессиональный Документы
Культура Документы
Hypo Kale Mia
Загружено:
DareRaymond0 оценок0% нашли этот документ полезным (0 голосов)
15 просмотров14 страницhypokalemia ppt
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документhypokalemia ppt
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
15 просмотров14 страницHypo Kale Mia
Загружено:
DareRaymondhypokalemia ppt
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 14
Low potassium (hypokalemia) refers to a lower
than normal potassium level in your
bloodstream.
Potassium is an important electrolyte for nerve
and muscle cell functioning, especially for
muscle cells in the heart. Your kidneys control
your body’s potassium levels, allowing for
excess potassium to leave the body through
urine or sweat.
A normal level of potassium is 3.6–5.2
millimoles per liter (mmol/L).
Hypokalemia is divided into the following 3
categories:
Mild: K+ 3.0-3.5 mEq/L
Moderate: K+ 2.5-3.0 mEq/L
Severe: K+ < 2.5 mEq/L
Your risks for hypokalemia can increase if you:
take medications, especially diuretics known to
cause potassium loss
have prolonged illness that causes vomiting or
diarrhea
S. Electrolytes / Potassium,
Magnesium, Calcium, Phosphorous,
TSH (thyroid stimulating hormone)
Aldosterone,
ECG,
Urine Potassium.
Low potassium (hypokalemia) has many causes. The most common
cause is excessive potassium loss in urine due to prescription
medications that increase urination. Also known as water pills or
diuretics, these types of medications are often prescribed for people
who have high blood pressure or heart disease.
Vomiting, diarrhea or both also can result in excessive potassium
loss from the digestive tract. Occasionally, low potassium is caused
by not getting enough potassium in your diet.
Causes of potassium loss include:
Chronic kidney disease,
Diabetic ketoacidssis,
Use of diuretics (Water / Fluid pills),
Diarrhea / vomiting,
Excessive sweating due to heat / exercise,
Excessive use of laxative, enema,
Excessive laxative use
Eating disorders (Bulimia)/ low consumption of potassium,
Magnesium Deficiencies,
Antibiotics,
Hyperthyroidism,
Alcoholism,
Coughing syndrome,
Prolonged nasogastric suctioning,
NPO status,
Steroids,
Tissue injury,
Leukemia,
Post ileostomy surgery.
Being aware of hypokalemia symptoms can help. Call your doctor if you are experiencing
these symptoms:
-weakness
-fatigue
-constipation
-muscle cramping
-palpitations
Levels below 3.6 are considered low, and anything below 2.5 mmol/L is life-threateningly
low. At these levels, there may be signs and symptoms of:
-paralysis
-respiratory failure
-breakdown of muscle tissue
-ileus (lazy bowels)
In more severe cases, abnormal rhythms may occur. This is most common in people who take
digitalis medications (digoxin) or have irregular heart rhythm conditions such as:
-fibrillation, atrial or ventricular
-tachycardia (heartbeat too fast)
-bradycardia (heartbeat too slow)
-premature heartbeats
Other symptoms include loss of appetite, nausea, and vomiting.
monitoring serum potassium levels every 1-3 hours and adjusting
supplement doses as necessary.
monitor patients on digoxin or those with digoxin toxicity.
Record fluid intake and output hourly and observe for
dehydration.
Check vitals sign hourly in critical care unit with severe
Hypokalemia.
Continue monitoring ECG and Identify ECG changes such as
depressed T waves, peaking P-waves.
Give mouth care to reduce vomiting tendency.
Give antiemetic drugs as order.
Monitor for any complications such as paralysis, cardiac arrest etc.
Check blood sugar 6 hourly and control by hypoglycemic agent.
Provide oral potassium diluted in 4-8 oz of water or juice
(decreased gastric mucosa irritation).
Dilute IV potassium 20-40mEq in 1L of IV fluids and use
infusion pump (irritating to blood vessels and myocardium).
If central venous line present can be give potassium
supplement through syringe pump 20mEq per hour.
Be careful that never administer bolus IV potassium.
Monitor IV site for phlebitis and infiltration if intravenous
cannula present.
Provide potassium rich diet and consult with dietician.
Check neurological status hourly by GCS scale.
Observe for neuromuscular changes such as fatigue and
muscular weakness.
Teach patient about potassium-rich foods and how to prevent
excessive loss (abuse of laxative and diuretics.
Provide calm and quite environment so that patient can sleep.
Give psychological support to reduce anxiety.
oral potassium chloride is administered when
potassium levels need to be replenished, as well as, in
patients with ongoing potassium loss (eg, those on
thiazide diuretics), when it must be maintained.
Potassium-sparing diuretics are generally used only in
patients with normal renal function who are prone to
significant hypokalemia.
Angiotensin-converting enzyme (ACE) inhibitors,
which inhibit renal potassium excretion, can ameliorate
some of the hypokalemia that thiazide and loop
diuretics can cause. However, ACE inhibitors can lead
to lethal hyperkalemia in patients with renal
insufficiency who are taking potassium supplements or
potassium-sparing diuretics.
Eating a diet that is rich in potassium can help prevent and treat low blood
potassium. Discuss your diet with your doctor. You’ll want to avoid
taking too much potassium, especially if you’re taking potassium
supplements. Good sources of potassium include:
avocados
bananas
figs
kiwi
oranges
spinach
tomatoes
milk
peas and beans
peanut butter
bran
While a diet low in potassium is rarely the cause of hypokalemia,
potassium is important for healthy body functions. Unless your doctor
tells you otherwise, eating a diet rich in potassium-containing foods is a
healthy choice.
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- API RP 7C-11F Installation, Maintenance and Operation of Internal Combustion Engines.Документ3 страницыAPI RP 7C-11F Installation, Maintenance and Operation of Internal Combustion Engines.Rashid Ghani100% (1)
- Ob - 1.02 Physiology of Female Reproductive SystemДокумент7 страницOb - 1.02 Physiology of Female Reproductive SystemDareRaymondОценок пока нет
- Pharmacology AntibioticsДокумент91 страницаPharmacology AntibioticsDareRaymond100% (1)
- MedsДокумент2 страницыMedsDareRaymondОценок пока нет
- Nop 0054Документ7 страницNop 0054DareRaymondОценок пока нет
- Ob - 1.02 Physiology of Female Reproductive SystemДокумент7 страницOb - 1.02 Physiology of Female Reproductive SystemDareRaymondОценок пока нет
- TCP Med Ward Mayo Copy 2Документ6 страницTCP Med Ward Mayo Copy 2DareRaymondОценок пока нет
- VREДокумент30 страницVREDareRaymondОценок пока нет
- Pharmacology Cardiovascular DrugsДокумент120 страницPharmacology Cardiovascular DrugsDareRaymond100% (1)
- Analysis ProperДокумент4 страницыAnalysis ProperDareRaymondОценок пока нет
- Gastric Cancer: Calag, Prescilla Tavas, Charme FayeДокумент20 страницGastric Cancer: Calag, Prescilla Tavas, Charme FayeDareRaymond0% (1)
- Respiratory Acidosis: Prepared By: Riezel Umaming Kathleen Testado Hazel AlarillaДокумент16 страницRespiratory Acidosis: Prepared By: Riezel Umaming Kathleen Testado Hazel AlarillaDareRaymond100% (2)
- 2 Systematic ABG AnalysisДокумент31 страница2 Systematic ABG AnalysisDareRaymondОценок пока нет
- 10.1 Water IntoxicationДокумент20 страниц10.1 Water IntoxicationDareRaymond100% (2)
- BCG VaccinatonДокумент11 страницBCG VaccinatonDareRaymondОценок пока нет
- Peptic Ulcer Disease: DR Waseem ChistiДокумент21 страницаPeptic Ulcer Disease: DR Waseem ChistiDarryl AcostaОценок пока нет
- Case Study - Urinary Tract InfectionДокумент10 страницCase Study - Urinary Tract InfectionJiffy198867% (3)
- FeverДокумент2 страницыFeverDareRaymond0% (1)
- Pathophysiology of Pregnancy Induced HypertensionДокумент2 страницыPathophysiology of Pregnancy Induced HypertensionDareRaymondОценок пока нет
- OB Birthing PositionДокумент10 страницOB Birthing PositionDareRaymondОценок пока нет
- Content ServerДокумент9 страницContent ServerDareRaymondОценок пока нет
- Right Sided Congestive Heart FailureДокумент20 страницRight Sided Congestive Heart FailureDareRaymondОценок пока нет
- Philippines EconДокумент16 страницPhilippines EconDareRaymondОценок пока нет
- Community Junk Food PDFДокумент5 страницCommunity Junk Food PDFDareRaymondОценок пока нет
- Ah 1 N 1Документ9 страницAh 1 N 1DareRaymondОценок пока нет
- DiabetesДокумент11 страницDiabetesDareRaymondОценок пока нет
- Req Equip Material Devlopment Power SectorДокумент57 страницReq Equip Material Devlopment Power Sectorayadav_196953Оценок пока нет
- Overlay Control PlansДокумент1 страницаOverlay Control PlansSTS-SPARK GAMINGОценок пока нет
- ABBindustrialdrives Modules en RevBДокумент2 страницыABBindustrialdrives Modules en RevBMaitry ShahОценок пока нет
- Celula de CargaДокумент2 страницыCelula de CargaDavid PaezОценок пока нет
- 16 - Ocean Currents & Salinity Interactive NotebookДокумент23 страницы16 - Ocean Currents & Salinity Interactive NotebookRaven BraymanОценок пока нет
- Learning English Through The Educational Games of Wordwall Website For Elementary Students by Group 1 (R4E)Документ6 страницLearning English Through The Educational Games of Wordwall Website For Elementary Students by Group 1 (R4E)NurulОценок пока нет
- Review of LiteratureДокумент3 страницыReview of LiteratureAbhimanyu Narayan RaiОценок пока нет
- Docket - CDB Batu GajahДокумент1 страницаDocket - CDB Batu Gajahfatin rabiatul adawiyahОценок пока нет
- Makalah Bahasa Inggris TranslateДокумент14 страницMakalah Bahasa Inggris TranslatevikaseptideyaniОценок пока нет
- How To Change Front Suspension Strut On Citroen Xsara Coupe n0 Replacement GuideДокумент25 страницHow To Change Front Suspension Strut On Citroen Xsara Coupe n0 Replacement Guidematej89Оценок пока нет
- Fce Use of English 1 Teacher S Book PDFДокумент2 страницыFce Use of English 1 Teacher S Book PDFOrestis GkaloОценок пока нет
- Fortnite Task Courier Pack 1500 V Bucks - BuscarДокумент1 страницаFortnite Task Courier Pack 1500 V Bucks - Buscariancard321Оценок пока нет
- What Is The PCB Shelf Life Extending The Life of PCBsДокумент9 страницWhat Is The PCB Shelf Life Extending The Life of PCBsjackОценок пока нет
- Prediction of CBR From Index Properties of Cohesive Soils: Magdi ZumrawiДокумент1 страницаPrediction of CBR From Index Properties of Cohesive Soils: Magdi Zumrawidruwid6Оценок пока нет
- Study and Interpretation of The ScoreДокумент10 страницStudy and Interpretation of The ScoreDwightPile-GrayОценок пока нет
- The One With The ThumbДокумент4 страницыThe One With The Thumbnoelia20_09Оценок пока нет
- PDF BrochureДокумент50 страницPDF BrochureAnees RanaОценок пока нет
- Current Harmonics: Electric Power System Power QualityДокумент3 страницыCurrent Harmonics: Electric Power System Power QualityAlliver SapitulaОценок пока нет
- Clinical Skills TrainingДокумент12 страницClinical Skills TrainingSri Wahyuni SahirОценок пока нет
- Kootenay Lake Pennywise April 26, 2016Документ48 страницKootenay Lake Pennywise April 26, 2016Pennywise PublishingОценок пока нет
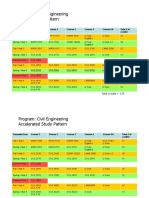
- HKUST 4Y Curriculum Diagram CIVLДокумент4 страницыHKUST 4Y Curriculum Diagram CIVLfrevОценок пока нет
- CandyДокумент24 страницыCandySjdb FjfbОценок пока нет
- 2.ed - Eng6 - q1 - Mod3 - Make Connections Between Information Viewed and Personal ExpiriencesДокумент32 страницы2.ed - Eng6 - q1 - Mod3 - Make Connections Between Information Viewed and Personal ExpiriencesToni Marie Atienza Besa100% (3)
- Visi RuleДокумент6 страницVisi RuleBruce HerreraОценок пока нет
- CHN Nutri LabДокумент4 страницыCHN Nutri LabMushy_ayaОценок пока нет
- Vest3000mkii TurntableДокумент16 страницVest3000mkii TurntableElkin BabiloniaОценок пока нет
- Final SEC Judgment As To Defendant Michael Brauser 3.6.20Документ14 страницFinal SEC Judgment As To Defendant Michael Brauser 3.6.20Teri BuhlОценок пока нет
- Vendor Registration FormДокумент4 страницыVendor Registration FormhiringОценок пока нет
- Previews 1633186 PreДокумент11 страницPreviews 1633186 PreDavid MorenoОценок пока нет