Академический Документы
Профессиональный Документы
Культура Документы
Midfoot Trauma
Загружено:
Dabessa Mosissa0 оценок0% нашли этот документ полезным (0 голосов)
12 просмотров26 страницdfgj
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документdfgj
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
12 просмотров26 страницMidfoot Trauma
Загружено:
Dabessa Mosissadfgj
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 26
Midfoot trauma
• Tarso-metatarsal dislocation (Lisfranc injury)
• This is an uncommon injury which can be easily overlooked. Thorough
• knowledge of the normal radiographic anatomy and alignment of the
• tarsal bones with the metatarsals is therefore vital.
• Normal dorsi-palmar (DP) view – shows that the medial margin
• of the second metatarsal aligns with the medial margin of the
• middle cuneiform.
• Oblique projection – shows that the medial margin of the third
• metatarsal aligns with the medial margin of the lateral cuneiform.
• The fracture-dislocation (Figures 8.3 and 8.4) is caused by severe
• trauma, usually by forced inversion or eversion of the forefoot when the
• hindfoot is fixed. It can also occasionally be due to a crush injury.
• Common examples of the causes of this injury are a rider falling from
a
• horse, with the foot stuck in the stirrup, and trapping of feet under
pedals
• or seats in head-on road traffic accidents5,6.
• If a bony fragment is detached from the base of any of the four
medial
• metatarsals, a tarso-metatarsal dislocation should be suspected.
Occasionally
• a fracture of the second metatarsal occurs at a more proximal
• level and the base remains in normal alignment. The distal fragment
• then dislocates laterally with the third, fourth and fifth metatarsals.
The
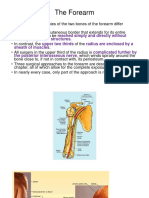
Normal anatomy and alignment of the foot. On
the DP projection (left hand image) the medial
aspect of
the base of the second metatarsal should be
aligned with the medial aspect of the medial
cuneiform. On the DP oblique projection (right
hand image), normal midfoot alignment is
indicated when the medial aspect of the third
metatarsal is aligned with the medial aspect of
the lateral cuneiform. Key = talus (1); navicular
(2); calcaneum (3); cuboid (4); lateral
cuneiform (5); third metatarsal (6); third
proximal phalanx (7); fourth middle phalanx
(8); second distal phalanx (9); lateral (fibular)
sesamoid bone (10); medial cuneiform (11);
middle cuneiform (12); lateral malleolus (fibula)
(13); tibia
Disruption of the tarso-metatarsal joint in the Lisfranc fracture-dislocation on the (a) dorso-palmar (DP) and
(b) DP oblique projections.
• MIDFOOT FRACTURES AND DISLOCATIONS
• Fractures of the tarsal navicular can be divided into four types, and
all can be treated in a cast with protected weight bearing as long as
fracture displacement is minimal. Displaced fractures of the body of
the navicular should be treated with open reduction and internal
fixation, however; the goals are to maintain length of the medial
column and to restore articular congruity. Sangeorzan et al. classified
navicular body fractures into three types and recommended
treatment based on fracture type (Fig. 86-35). In type I fractures, in
which the fracture plane is transverse, a satisfactory reduction
usually was obtainable. In type II and type III fractures, reduction was
more difficult. In each case, an approach was made over the
anteromedial hindfoot in the interval between the anterior and
posterior tibial tendons. The periosteum of the navicular was not
elevated, and the joints were inspected and cleared of debris before
fixation. Fixation usually was obtained with smooth Kirschner wires
and small fragment AO screws when the size of the fragment
permitted
• If collapse of the navicular occurs with medial column
shortening, bone grafting, temporary fixation to the talus or
cuneiforms, or application of a small external fixator is
used for additional fixation. A prolonged recovery and
persistent symptoms are the rule in these injuries.
• Navicular stress fractures are frequent causes of arch pain in athletes. Because many of these fractures are not clearly
identified on routine radiographs, a high index of suspicion is necessary for accurate diagnosis. Torg et al. reported 21
patients with this injury. Most patients have increasing arch pain with activity. Track athletes seem to be particularly
vulnerable. The midfoot may be tender over the navicular, and the foot may be irritable with eversion and inversion
stress. Radiographs may be normal initially, but a bone scan frequently is positive, and tomograms, CT, or MRI may
confirm the diagnosis. In an extensive review of 86 proven cases of navicular stress fractures, Khan et al. found that
with two exceptions the fractures were located in the sagittal plane, involving the central third of the navicular bone.
There were 83 partial fractures and three complete fractures. In their series, non–weight bearing cast immobilization for
6 weeks initially was successful in 86%. Limitation of activity resulted in only a 38% success rate, whereas surgical
management with bone grafting and internal fixation resulted in a 67% success rate. Based largely on their work, Quirk
recommended the following treatment:
• 1. At the time of initial diagnosis, all patients should be placed in a below-knee, non–weight bearing cast for 6 weeks.
• 2. If tenderness is still located over the navicular after 6 weeks of non–weight bearing immobilization, another cast
is applied for 2 weeks.
• 3. If treatment is successful, the patient is allowed to return to previous activity gradually under supervision.
• Quirk also suggested that if open reduction, internal fixation, and bone grafting are required, a CT scan should be made
preoperatively with a marker placed over the fracture line to help identify the area intraoperatively.
• Cuboid and cuneiform fractures are rare as isolated injuries.
These bones frequently are injured as part of a wider injury
pattern involving the Lisfranc (most common) or Chopart joint.
Cuboid fractures can be classified into avulsion or compression
types. Small avulsions may occur with inversion-type ankle
sprains and generally respond to conservative treatment.
Compression, or “nutcracker,” fractures of the cuboid are
associated with Lisfranc and midtarsal disruptions. Most are
minimally displaced and can be treated in a non–weight bearing
cast for 4 weeks followed by weight bearing casts for 4 weeks.
A well-molded arch support often is used afterward. For severe
displacement with shortening of the lateral column,
consideration should be given to open reduction and internal
fixation with bone grafting.
• Richter et al., in their evaluation of 155 patients with midfoot fractures and
dislocations, found a relative incidence of isolated midfoot fractures of
35.5%; Lisfranc fracture-dislocations, 31%; Chopart-Lisfranc fracture-
dislocations, 16.8%; and pure Chopart fracture-dislocations, 16%.
Dislocations and fracture-dislocations at the Chopart joint are frequent and
are associated with high-energy injuries, such as traffic accidents. The
incidence of this injury at our institution has been markedly higher,
especially since the introduction and routine use of airbags in motor
vehicles. Patients who may not previously have survived injuries now
sustain severe blunt force trauma to the feet often resulting in dislocations
of the Chopart and Lisfranc joints in addition to other injuries. In this study
and a similar study from the same authors, there seemed to be significant
improvement in the scores in patients who were treated with early operative
intervention and anatomical or near-anatomical alignment and reduction of
the joints. The lowest scoring results occurred in patients who had
combined Chopart and Lisfranc fracture-dislocations. Most often, the
exposure of the Chopart joint is a combination of that described for
subtalar dislocation with an anterolateral incision as described for the
Lisfranc fracture-dislocation and a dorsomedial incision.
A, Type I fracture. Dorsal fragment usually consists of
less than 50% of body of tarsal navicular.
Anteroposterior radiographs show only subtle double
cortical shadow at joint line. B, Type II fracture.
Talonavicular joint is most often subluxated dorsally
and medially with adduction of forepart of foot. C,
Type III fracture. Comminuted fracture of body of
navicular is associated with disruption of cuneiform-
navicular joint, lateral deviation of forepart of foot,
and injuries to cuboid or anterior process of
calcaneus.
Open reduction and internal fixation of type III
navicular fracture. A and B, Preoperative radiographs.
C, Semicoronal CT scan showing comminution of
body of navicular. D and E, Postoperative
radiographs.
• Fracture-Dislocations of the Tarsometatarsal Articulation
(Lisfranc Joint)
• Injuries of the tarsometatarsal articulation encompass a wide
spectrum ranging from mild sprains or subtle subluxations to
widely displaced debilitating injuries (Fig. 86-37). Myerson
reported a 4% incidence per year of tarsometatarsal injuries in
collegiate football players. Players with medial or global
tenderness had longer periods of disability than players with
isolated lateral tenderness. Aitken and Poulson; Hardcastle et
al.; Arntz and Hansen; Sangeorzan, Veith, and Hansen; and
Adelaar have published excellent reviews on this subject. In
1986, Myerson et al. published a study of 76 high-velocity
tarsometatarsal injuries, noting a direct correlation between
better results and anatomical reduction of the fracture-
dislocation.
Dorsal view of foot showing contour of tarsometatarsal joints.
• study by Petje et al. found statistically significant anatomical abnormalities in the
normal foot of patients with contralateral Lisfranc fracture-dislocations. This
abnormality is best described as a shallow recessed mortise in the second
metatarsal, which suggests that patients who do have a Lisfranc fracture-
dislocation may have underlying anatomical abnormalities in the feet that might
predispose them to contralateral injury.
• Teng et al. reported less than satisfactory outcomes in 11 patients with excellent
anatomical alignment 41 months after surgical treatment of closed Lisfranc
fracture-dislocations. Although objective measures of gait analysis had returned to
normal, the investigators concluded that even with seemingly anatomical
restoration of normal alignment, many patients did poorly subjectively. Many
patients, even with degenerative posttraumatic changes in the joints, have a
satisfactory result, however.
• Classification
• Classification of this injury is useful for communication between orthopaedists and
for determining the plane of displacement and magnitude of soft-tissue injury. The
classification is not prognostic for the result, however. Myerson's modification of
the original classification of Quénu and Küss and Hardcastle et al. is presented
because it incorporates more proximal injuries to the medial column of the foot
(Fig. 86-38). Subtle injuries through the intercuneiform region and the
naviculocuneiform joint probably are more common than previously thought.
Classification of tarsometatarsal fracture-
dislocations.
• Type A Injuries
• Type A injuries involve displacement of all five metatarsals with or without fracture of the base of the second
metatarsal. The usual displacement is lateral or dorsolateral, and the metatarsals move as a unit. These injuries
are referred to as homolateral.
• Type B Injuries
• In type B injuries, one or more articulations remain intact. Type B1 injuries are medially displaced, sometimes
involving the intercuneiform or naviculocuneiform joint. Type B2 injuries are laterally displaced and may
involve the first metatarsal–cuneiform joint.
• Type C Injuries
• Type C injuries are divergent injuries and can be partial (C1) or complete (C2). These generally are high-energy
injuries, associated with significant swelling, and prone to complications, especially compartment syndrome.
• Evaluation and Treatment
• Any injury resulting in midfoot tenderness and swelling merits a careful physical and radiographic
examination. Although grossly displaced fracture-dislocations are obvious on examination, care should be
taken with subtle injuries to palpate each articulation for tenderness and swelling, especially the medial
cuneiform–first metatarsal joint, which often appears nondisplaced on radiographs. Trevino and Kodros
described a “rotation test,” in which stressing the second tarsometatarsal joint by elevating and depressing the
second metatarsal head relative to the first metatarsal head elicits pain at the Lisfranc joint. Careful
observation of the plantar aspect of the foot may reveal a small ecchymosis indicating a significant injury. The
inability to bear weight on the foot is another sign of potential instability.
• Radiographs must be obtained with the patient bearing weight. If the radiograph reveals no displacement, and the
patient cannot bear weight, a short leg cast should be used for 2 weeks, and the radiographs should be repeated with
weight bearing. Evaluation should be directed to the following areas: 1. The medial shaft of the second metatarsal
should be aligned with the medial aspect of the middle cuneiform on the anteroposterior view.
•
• 2. The medial shaft of the fourth metatarsal should be aligned with the medial aspect of the cuboid on the oblique
view.
•
• 3. The first metatarsal–cuneiform articulation should have no incongruency.
•
• 4. A “fleck sign” should be sought in the medial cuneiform–second metatarsal space. This represents an avulsion of
the Lisfranc ligament.
•
• 5. The naviculocuneiform articulation should be evaluated for subluxation.
•
• 6. A compression fracture of the cuboid should be sought.
•
• Compartment syndrome, although rare and usually seen
only with higher energy fracture-dislocations, can cause
severe, difficult-to-treat clawing of the toes and chronic
pain. We routinely obtain compartmental pressures in
patients who have severe swelling, but individual
compartments can be difficult to assess, and clinical
suspicion alone is enough to warrant decompression. We
prefer a long medial incision to decompress the abductor
hallucis and deep compartments of the foot, including the
calcaneal compartment, as described by Manoli (Fig. 86-
39A). In addition, two incisions—one between the second
and third and one between the fourth and fifth
metatarsals—are used for the dorsal intrinsic
Cross section of foot showing release of four fascial
compartments of forefoot through medial approach
(top). Single medial incision for decompression of
fascial compartments of foot (bottom). Proximal
extension used for decompression of calcaneal
compartment and tarsi tunnel. B, Double dorsal
longitudinal incisions (left) are used to decompress
all four compartments (right).
• The key to successful outcome in Lisfranc injuries is anatomical
alignment of the involved joints. Closed, nondisplaced (<2 mm)
injuries can be treated with a non–weight bearing cast for 6 weeks
followed by a weight bearing cast for an additional 4 to 6 weeks.
Repeat radiographs should be obtained to ensure that no
displacement is occurring in the cast. Displaced fractures should be
treated operatively (Fig. 86-40). Closed reduction, using finger traps
and countertraction, can be successful if displacement is not severe.
Fixation should be used to maintain the reduction. Steinmann pins
(3/32-inch) can be used, especially for the lateral two joints; however,
4-mm cannulated or 4-mm standard, partially threaded cancellous
screws provide excellent fixation and can be inserted under image
control. Using cannulated screws makes removal easier by
employing a guide pin to find the screw head and ultimately to seat
with the screwdriver. If the reduction is inadequate, or significant
comminution is present, open reduction is preferred, especially in
partial (type B) or divergent (type C) patterns.
Subtle Lisfranc instability. A, Intraoperative
fluoroscopic radiograph showing fleck sign at medial
cuneiform–second metatarsal articulation. Patient
was taken to operating room because standing
radiographs in office showed subtle subluxation,
swelling, and tenderness and pointed to more serious
instability. B, Intraoperative stress radiographs
showing subluxation of first through third
tarsometatarsal articulations. C, Provisional
stabilization with guidewires inserted under
fluoroscopic control. D, Final fixation with cannulated
screws.
• The literature confirms that the ability to obtain and maintain an anatomical
reduction of a fracture-dislocation is associated with improved outcome over
nonanatomical reduction. Kuo et al., in their evaluation of open reduction and
internal fixation in 48 patients with Lisfranc injuries with an average follow-up of 52
months, found that nonanatomical reduction was associated with the presence of
posttraumatic arthrosis in 60%. In patients with anatomical reduction,
posttraumatic arthrosis occurred in only 16%. No statistical significance was
shown in their series regardless of whether the injury was open or closed, whether
all five tarsometatarsals or fewer were injured, whether a cuneiform or cuboid was
injured, whether the Lisfranc injury was isolated or associated with multiple
injuries, whether the diagnosis was made acutely or delayed, or whether it was a
work-related injury.
• Degenerative posttraumatic arthrosis can be managed successfully with
tarsometatarsal and intermetatarsal arthrodesis as necessary for stabilization of
the arthritic joints and reduction of posttraumatic flatfoot deformity. In a review of
32 patients who had arthrodesis of the tarsometatarsal joints for intractable pain
after traumatic injury of the midfoot, Komenda, Myerson, and Biddinger noted
significant improvement in the AOFAS score for the midfoot from 44 points
preoperatively to 78 points postoperatively. Mann, Prieskorn, and Sobel reported
long-term results of arthrodesis of the midtarsal and tarsometatarsal joints in 40
patients, of whom 17 had posttraumatic arthritis. In their series, 93% of patients
were satisfied with the results at an average follow-up of 6 years
• With the patient under a regional or general anesthetic, make a dorsal incision lateral to the extensor hallucis longus tendon over the interval between the base of the first and second metatarsals. At
the distal extent of the excision, preserve the most medial branch of the dorsal medial cutaneous nerve.
•
• • Locate and incise the inferior extensor retinaculum.
•
• • Isolate the dorsalis pedis artery and deep peroneal nerve, and use a vessel loop for retraction of these structures medially or laterally to allow inspection of different areas of the Lisfranc joint
(Fig. 86-41A).
•
• • Remove any debris from the Lisfranc region between the base of the second metatarsal and the medial cuneiform to allow the space to be reduced. If an intercuneiform screw is needed, insert it
under fluoroscopic guidance from the medial side of the medial cuneiform into the middle cuneiform (Fig. 86-41B).
•
• • Under fluoroscopic guidance, pass a guidewire from the medial cuneiform into the base of the second metatarsal while holding the reduction with a towel clip.
•
• • Pass a 4-mm cancellous cannulated screw over the guidewire. Reduce any injury and instability to the first tarsometatarsal joint, and hold similarly with a screw from the dorsal aspect of the first
metatarsal into the medial cuneiform (Fig. 86-41C). The third metatarsal-cuneiform joint usually is visible through this dorsal incision and can be reduced and fixed similarly.
•
• • Reduce lateral metatarsocuboid disruptions either closed with smooth 3/32-inch Steinmann pins or open through a parallel incision centered dorsolaterally over the articulations (Fig. 86-41D).
•
• • Close the dorsal skin with interrupted nylon sutures.
•
A, Extensile dorsomedial approach to midfoot.
Dorsolateral approach to second and third
metatarsals (left). Dorsomedial approach to first and
second metatarsals (right). B, Medial and middle
column fixation. C, Temporary lateral column fixation.
D, Permanent lateral column fixation.
• AFTERTREATMENT
• A bulky dressing and posterior splint are applied postoperatively.
These are converted to a short leg, non–weight bearing cast at 7 to
10 days postoperatively. Partial weight bearing may be allowed at 6 to
8 weeks. Laterally placed Steinmann pins are removed at 8 weeks.
Medial screws are removed at 4 months. A prefabricated walker is
used until the medial screws are removed.
• Because many of these injuries are initially missed, the question is at
what point should open reduction and internal fixation without
arthrodesis still be attempted. We attempt open reduction and
internal fixation without arthrodesis 8 weeks after injury in a patient
weighing less than 150 to 160 lb and having little or no comminution.
Patients who weigh more are treated earlier with arthrodesis of the
medial three joints and rarely, if ever, with arthrodesis of the lateral
two joints (Fig. 86-42). Mobility is important in the fourth and fifth
metatarsal–cuboid articulation, and posttraumatic arthrosis may
cause only mild symptoms in this region.
Divergent Lisfranc fracture-dislocation. A and B,
Preoperative radiographs. Note intercuneiform and
naviculocuneiform disruption. C and D, Postoperative
radiographs. Intracuneiform arthrodesis was
performed for stabilization. Patient's weight was 250
lb.
Вам также может понравиться
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Electrical Safety Awareness TrainingДокумент45 страницElectrical Safety Awareness TrainingManish Deswal50% (2)
- Errors of Eye Refraction and HomoeopathyДокумент11 страницErrors of Eye Refraction and HomoeopathyDr. Rajneesh Kumar Sharma MD HomОценок пока нет
- Complete Guide To Pediatric NusringДокумент135 страницComplete Guide To Pediatric NusringSANKARОценок пока нет
- LUS HSE FM4 455 005.01 Audit Gap Analysis ChecklistДокумент10 страницLUS HSE FM4 455 005.01 Audit Gap Analysis ChecklistRichu PaliОценок пока нет
- Blood Cells MorphologyДокумент20 страницBlood Cells MorphologyKevin MikeОценок пока нет
- Hand IncisionsДокумент55 страницHand IncisionsDabessa Mosissa100% (2)
- Work Experience SheetДокумент2 страницыWork Experience SheetAko Si Gilsboy100% (1)
- External FixatorДокумент19 страницExternal FixatorDabessa MosissaОценок пока нет
- ACTIVITY DESIGN-first AidДокумент4 страницыACTIVITY DESIGN-first AidShyr R Palm0% (1)
- MNT CancerДокумент62 страницыMNT CancerSaufi ZakariaОценок пока нет
- Management of Hepatic CystsДокумент12 страницManagement of Hepatic CystsDabessa MosissaОценок пока нет
- Common FractureДокумент314 страницCommon FractureDabessa MosissaОценок пока нет
- Techniques of Exposure, Hilar DissectionДокумент20 страницTechniques of Exposure, Hilar DissectionDabessa MosissaОценок пока нет
- Open Radical Cholecystectomy With Partial Hepatectomy For Gallbladder CancerДокумент2 страницыOpen Radical Cholecystectomy With Partial Hepatectomy For Gallbladder CancerDabessa MosissaОценок пока нет
- Esophageal Perforation TreatmentДокумент4 страницыEsophageal Perforation TreatmentDabessa MosissaОценок пока нет
- General Consideration in EsophagectomyДокумент4 страницыGeneral Consideration in EsophagectomyDabessa MosissaОценок пока нет
- Whipple ProcedureДокумент16 страницWhipple ProcedureDabessa MosissaОценок пока нет
- Trauma RadiologyДокумент9 страницTrauma RadiologyDabessa MosissaОценок пока нет
- Fractures of The Femoral NeckДокумент37 страницFractures of The Femoral NeckDabessa MosissaОценок пока нет
- 2.supracondylar Humerus FracturesДокумент26 страниц2.supracondylar Humerus FracturesDabessa MosissaОценок пока нет
- Soft Tissue TumorДокумент248 страницSoft Tissue TumorDabessa MosissaОценок пока нет
- Flexor Tendon AnatomyДокумент29 страницFlexor Tendon AnatomyDabessa MosissaОценок пока нет
- Surgical Approaches and Applied AnatomyДокумент44 страницыSurgical Approaches and Applied AnatomyDabessa MosissaОценок пока нет
- The ForearmДокумент49 страницThe ForearmDabessa MosissaОценок пока нет
- Humerous Fxs With Radial Nerve PalsyДокумент26 страницHumerous Fxs With Radial Nerve PalsyDabessa MosissaОценок пока нет
- Trauma RadiologyДокумент9 страницTrauma RadiologyDabessa MosissaОценок пока нет
- Bone and Joint InfectionsДокумент153 страницыBone and Joint InfectionsDabessa MosissaОценок пока нет
- Fingertip AmputationДокумент41 страницаFingertip AmputationDabessa MosissaОценок пока нет
- Distal Phalanx (45%) - Metacarpal (30%) - Proximal Phalanx (15%) - Middle Phalanx (10%)Документ40 страницDistal Phalanx (45%) - Metacarpal (30%) - Proximal Phalanx (15%) - Middle Phalanx (10%)Dabessa MosissaОценок пока нет
- Trigger Finger (TF)Документ59 страницTrigger Finger (TF)Dabessa MosissaОценок пока нет
- The ForearmДокумент49 страницThe ForearmDabessa MosissaОценок пока нет
- EsophagusДокумент24 страницыEsophagusDabessa MosissaОценок пока нет
- Pediatric Surgical ThemesДокумент32 страницыPediatric Surgical ThemesDabessa MosissaОценок пока нет
- Congenital Diaphragmatic HerniaДокумент45 страницCongenital Diaphragmatic HerniaDabessa MosissaОценок пока нет
- JaundiceДокумент12 страницJaundiceDabessa MosissaОценок пока нет
- Discribd DocumentДокумент1 страницаDiscribd DocumentDabessa MosissaОценок пока нет
- Discribd DocumentДокумент1 страницаDiscribd DocumentDabessa MosissaОценок пока нет
- Patient Care Management Human Anatomy With Answer KeyДокумент7 страницPatient Care Management Human Anatomy With Answer KeyMarylyn Grass RootОценок пока нет
- Coron School of FisheriesДокумент3 страницыCoron School of FisheriesRafael DacullaОценок пока нет
- Httpsjkbopee Gov InPdfDownloader Ashxnid 13580&type NДокумент221 страницаHttpsjkbopee Gov InPdfDownloader Ashxnid 13580&type NMONISОценок пока нет
- Stress MGMT in Call CentersДокумент70 страницStress MGMT in Call CentersJayesh Kambli100% (1)
- BaliДокумент206 страницBaliErick JordisonОценок пока нет
- 03 - Hazards Identification, Risk Assessment and ControlДокумент39 страниц03 - Hazards Identification, Risk Assessment and ControlDEO SALVACIONОценок пока нет
- Periodontal Probing and Techniques JCДокумент58 страницPeriodontal Probing and Techniques JCAbhay TandonОценок пока нет
- GRP 3 - Galatians - Borgia Et1Документ3 страницыGRP 3 - Galatians - Borgia Et1Kyle BARRIOSОценок пока нет
- Impact of COVID19 To CommunityДокумент3 страницыImpact of COVID19 To CommunitySheila Mae AramanОценок пока нет
- Mental Practice in Chronic StrokeДокумент6 страницMental Practice in Chronic StrokeIsa AbdantauhidОценок пока нет
- Pinnacle Tecnica Quirurgica 2Документ49 страницPinnacle Tecnica Quirurgica 2Saenz Guzman LauraОценок пока нет
- Perdev Week 5Документ3 страницыPerdev Week 5AdiraОценок пока нет
- American Architecture Began With Frank Lloyd WrightДокумент8 страницAmerican Architecture Began With Frank Lloyd WrightAdheith South NgalamОценок пока нет
- Biology Class 10 Syllabus Break Up AY 2022-23Документ8 страницBiology Class 10 Syllabus Break Up AY 2022-23alfredo pastaОценок пока нет
- AK Vegan Animals Lifescape 2008 (May) 74-6Документ3 страницыAK Vegan Animals Lifescape 2008 (May) 74-6Pepa GarcíaОценок пока нет
- Family Nursing Care Plan Group 1talisay Del CarmenДокумент8 страницFamily Nursing Care Plan Group 1talisay Del CarmenMarla GanalОценок пока нет
- Takaful MaybankДокумент4 страницыTakaful MaybankSHAОценок пока нет
- Gn-31 Qms Cad (Dec 2012) FinalДокумент19 страницGn-31 Qms Cad (Dec 2012) FinalSeanОценок пока нет
- Industrial Counseling HWДокумент3 страницыIndustrial Counseling HWJoyce SisonОценок пока нет
- PoemДокумент8 страницPoemJeevitraОценок пока нет
- Wiri 08 - Zambia Trip Application FormДокумент11 страницWiri 08 - Zambia Trip Application Forminfo@zcfcanada.orgОценок пока нет
- Ofw Child Experience: An Analysis PaperДокумент2 страницыOfw Child Experience: An Analysis PaperClark AbonadoОценок пока нет