Академический Документы
Профессиональный Документы
Культура Документы
ARDS
Загружено:
Martoyo Ichwan0 оценок0% нашли этот документ полезным (0 голосов)
68 просмотров18 страницAcute respiratory distress syndrome (ARDS) is a life-threatening lung condition caused by injury to the lungs. It is characterized by inflammation and fluid in the lungs, preventing enough oxygen from entering the bloodstream. The Berlin Definition provides criteria for diagnosing ARDS based on timing of symptoms, chest imaging findings, origin of edema, and level of hypoxemia. Treatment involves supportive care in an intensive care unit, including mechanical ventilation, maintaining fluid balance, antibiotics, and sometimes corticosteroids. The goal is to keep oxygen levels in an adequate range using the lowest possible pressures and oxygen levels.
Исходное описание:
Оригинальное название
ARDS.pptx
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документAcute respiratory distress syndrome (ARDS) is a life-threatening lung condition caused by injury to the lungs. It is characterized by inflammation and fluid in the lungs, preventing enough oxygen from entering the bloodstream. The Berlin Definition provides criteria for diagnosing ARDS based on timing of symptoms, chest imaging findings, origin of edema, and level of hypoxemia. Treatment involves supportive care in an intensive care unit, including mechanical ventilation, maintaining fluid balance, antibiotics, and sometimes corticosteroids. The goal is to keep oxygen levels in an adequate range using the lowest possible pressures and oxygen levels.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
68 просмотров18 страницARDS
Загружено:
Martoyo IchwanAcute respiratory distress syndrome (ARDS) is a life-threatening lung condition caused by injury to the lungs. It is characterized by inflammation and fluid in the lungs, preventing enough oxygen from entering the bloodstream. The Berlin Definition provides criteria for diagnosing ARDS based on timing of symptoms, chest imaging findings, origin of edema, and level of hypoxemia. Treatment involves supportive care in an intensive care unit, including mechanical ventilation, maintaining fluid balance, antibiotics, and sometimes corticosteroids. The goal is to keep oxygen levels in an adequate range using the lowest possible pressures and oxygen levels.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 18
ACUTE RESPIRATORY DISTRESS SYNDROME
Taufan Arif, S.Kep., Ns., M.Kep
Description
• Acute respiratory distress syndrome (ARDS) is a
systemic process that is considered to be the
pulmonary manifestation of multiple organ
dysfunction syndrome.
• It is characterized by noncardiac pulmonary edema
and disruption of the alveolarcapillary membrane as
a result of injury to either the pulmonary vasculature
or the airways
The Berlin Definition of ARDS is as follows
• Timing—within 1 week of known clinical insult or new or worsening respiratory
symptoms
• Chest imaging—bilateral opacities not fully explained by effusions, lobar/lung
collapse or nodules
• Origin of edema—respiratory failure not fully explained by heart failure or fluid
overload; need objective assessment to exclude hydrostatic edema if no risk
factor present
• Oxygenation—mild (200 mg Hg less than Pao2/Fio2 less than or equal to 300 mm
Hg with positive end-respiratory airway pressure [PEEP] or constant positive
airway pressure [CPAP] greater than or equal to 5 cm H2O); Moderate (100 mg
Hg less than Pao2/Fio2 less than or equal to 200 mm Hg with PEEP greater than
or equal to 5 cm H2O); or Severe (Pao2/Fio2 less than or equal to 100 mm Hg
with PEEP greater than or equal to 5 cm H2O)
Etiology
• These are categorized as direct or indirect, depending on
the primary site of injury (Box 20-5).
• Direct injuries are those in which the lung epithelium
sustains a direct insult. Indirect injuries are those in which
the insult occurs elsewhere in the body and mediators are
transmitted via the bloodstream to the lungs.
• Sepsis, aspiration of gastric contents, diffuse pneumonia,
and trauma were found to be major risk factors for the
development of ARDS
Pathophysiology
• Activation of inflammatory mediators and cellular
components resulting in damage to capillary endothelial
and alveolar epithelial cells
• Increased permeability of alveolar capillary membrane
• Influx of protein rich edema fluid,blood cells, inflammatory
cells into alveoli
• Dysfunction of surfactant
• Alveoli collapse(atelektasis) fibrotic
• Lungs become stiff, less compliant, very hard to inspire
• Decrease in gas exchange /shunted Hypoxia
STAGES
1. Exudative (acute) phase - 0- 4 days
2. Proliferative phase - 4- 8 days
3. Fibrotic phase - >8 days
4. Recovery
Clinical Manifestation
• Rapid onset of severe dyspnea • ABG’s
• with in 12-48 hours PaO2 < 70mmHg
• Intercostal and suprasternal PaCO2 > 45
retractions HCO3
• Increased resp rate • Normal
• Hypoxemia that does not respond to • < 22
O2 pH
• Confusion anxiety • low
• Restlessness Analysis
• Cyanosis • Resp. and met. Acidosis
• Fever
Complication
• Lung damage (such as pneumothorax) due to
use of high settings on the breathing machine
needed to treat the disease
• Multiple organ system failure
• Pulmonary fibrosis
• Ventilator-associated pneumonia
Diagnostic Test
• Arterial blood gas analysis reveals hypoxemia (reduced
levels of oxygen in the blood)
• A complete blood count may be taken. The number of
white blood cells is increased in sepsis
• Chest x-ray will show the presence of fluid in the lungs
• CT scan of the chest may be required only in some
situations (routine chest x-ray is sufficient in most cases)
• Echocardiogram (an ultrasound of the heart) may help
exclude any heart problems that can cause fluid build-up in
the lung
Diagnostic Test
• Monitoring with a pulmonary artery catheter may be
done to exclude a cardiac cause for the difficulty in
breathing.
• Bronchoscopy (a procedure used to look large airways
of the lung) may be considered to evaluate the
possibility of lung infection
• Sputum cultures and analysis
MANAGEMENT
INTENSIVE CARE UNIT
• O2 Intubation and mechanical vent
• Give lowest possible level of O2 to prevent toxicity
• Higher airway pressures usually necessary
• PEEP may be indicated
• Maintain PaO2 at > 60mm Hg
• Potitioning and chest fisioterapi
• Increase cardiac output and maintain blood pressure
• Fluid therapy
• Dobutrex, dobutamine
• Maintenance of fluid balance
• Diuretics may be indicated Diuretics may be indicated
MANAGEMENT
• Surfactant replacement
• Corticosteroids
• Antibiotis
• Sedatives
• Diuretics
SELECT PEEP
• PEEP/FiO2 relationship to maintain adequate
PaO2/SpO2
• PaO2 goal: 55-80mmHg or SpO2 88-95% use
FiO2/PEEP combination to achieve oxygenation goal
Fio2 0.3 0.4 0.4 0.5 0.5 0.6 0.7 0.7 0.7 0.8 0.9 0.9 0.9 1.0
PEEP 5 5 8 8 10 10 10 12 14 14 14 16 18 20-24
Вам также может понравиться
- Test Your Knowledge About Pneumonia - ProProfs QuizДокумент8 страницTest Your Knowledge About Pneumonia - ProProfs QuizNaresh Kumar SoniОценок пока нет
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- SA Anesthesia Drug Dosages 2022Документ3 страницыSA Anesthesia Drug Dosages 2022KRLITHIU Borja100% (1)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5795)
- Xerostomia As A Potential Condition in PДокумент4 страницыXerostomia As A Potential Condition in PAlamsyah PiliangОценок пока нет
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- ENT Summery TABLEДокумент19 страницENT Summery TABLEtaliya. shvetzОценок пока нет
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- Sexual Behaviors in Autism: Problems of Definition and ManagementДокумент7 страницSexual Behaviors in Autism: Problems of Definition and ManagementPaula MarcuОценок пока нет
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Morning Report: Supervisor: Dr. Rusdhy A.H., SP - OG Medical StudentsДокумент8 страницMorning Report: Supervisor: Dr. Rusdhy A.H., SP - OG Medical StudentsEra MoetzОценок пока нет
- Medical Decision MakingДокумент14 страницMedical Decision MakingwbothaОценок пока нет
- Dermocalm LotionДокумент5 страницDermocalm LotionSai KrishnaОценок пока нет
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- RetailerPriceList OHДокумент1 страницаRetailerPriceList OHMuhammad Samiur RahmanОценок пока нет
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- Basics of Pharmacology: Speaker - DR - SantoshДокумент76 страницBasics of Pharmacology: Speaker - DR - SantoshRamya ChallaОценок пока нет
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- iHFG Part C Space Standards DimensionsДокумент7 страницiHFG Part C Space Standards DimensionsShalini MinnaОценок пока нет
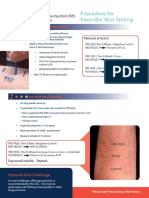
- Procedure For Penicillin Skin TestingДокумент4 страницыProcedure For Penicillin Skin TestingHarshan Isuru KumaraОценок пока нет
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- MCQ Pead MockДокумент8 страницMCQ Pead MocknoblefxОценок пока нет
- ARI Company Catalogue PDFДокумент29 страницARI Company Catalogue PDFEd Gar YundaОценок пока нет
- Do You Know Me Flyer-Teacher VersionДокумент1 страницаDo You Know Me Flyer-Teacher VersionMaria Guy Del DucaОценок пока нет
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- QUIZ Classification of Surgery in TableДокумент1 страницаQUIZ Classification of Surgery in TableMaria Sheila BelzaОценок пока нет
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Trends of Violence Against Healthcare by ShaheerДокумент9 страницTrends of Violence Against Healthcare by ShaheerShaheer zia100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- Behavioral TherapyДокумент35 страницBehavioral TherapyLouriel NopalОценок пока нет
- What Causes A Urinary Tract InfectionДокумент6 страницWhat Causes A Urinary Tract InfectionStepyn SalvadorОценок пока нет
- Nursing Group Research PaperДокумент16 страницNursing Group Research Paperapi-368267454Оценок пока нет
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- Final Resume Package Douglas ShawДокумент3 страницыFinal Resume Package Douglas Shawapi-347691125Оценок пока нет
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Gingival Tissue ManagementДокумент8 страницGingival Tissue ManagementJoshua RosalОценок пока нет
- National Quality Assurance Standards: Mandatory Requirements PHC/CHCДокумент14 страницNational Quality Assurance Standards: Mandatory Requirements PHC/CHCSathish KumaarОценок пока нет
- Bruxism-An Unsolved Problem in Dental MedicineДокумент4 страницыBruxism-An Unsolved Problem in Dental Medicinedentace1Оценок пока нет
- Daftar PustakaДокумент2 страницыDaftar PustakarisdaauliaputriОценок пока нет
- Meditation Its EffectДокумент11 страницMeditation Its Effectmanisami7036Оценок пока нет
- Eye Test For Alp Post Imp PDFДокумент1 страницаEye Test For Alp Post Imp PDFGyg GtgОценок пока нет
- Jsa Assembly The Chimney (Not Finish)Документ3 страницыJsa Assembly The Chimney (Not Finish)putrasejahtraОценок пока нет
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- OT HoppysAppReviewДокумент1 страницаOT HoppysAppReviewIris De La CalzadaОценок пока нет
- Stem Cell Research PaperДокумент3 страницыStem Cell Research Papermyrentistoodamnhigh100% (1)