Академический Документы
Профессиональный Документы
Культура Документы
PP Dokter Setia Putra Tarigan MASSIVE PLEURAL EFFUSIONS BPLS Maret 2015
Загружено:
zhafran ritonga0 оценок0% нашли этот документ полезным (0 голосов)
68 просмотров19 страницОригинальное название
7. PP dokter setia putra tarigan MASSIVE PLEURAL EFFUSIONS BPLS Maret 2015.ppt
Авторское право
© © All Rights Reserved
Доступные форматы
PPT, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
68 просмотров19 страницPP Dokter Setia Putra Tarigan MASSIVE PLEURAL EFFUSIONS BPLS Maret 2015
Загружено:
zhafran ritongaАвторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPT, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 19
BASIC PULMONARY LIFE SUPPORT
BPLS - 2015
dr. Setia Putra Tarigan, Sp.P (K)
Department of Pulmonology and Respiratory Medicine
Faculty of Medicine University of Sumatera Utara
Adam Malik General Hospital
Medan
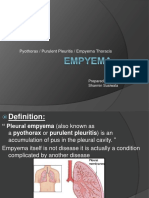
Pleural effusions is an accumulation of pleural
fluid in the pleural space
Massive pleural effusion:
Pleural effusion with opacification on entire
hemithorax
Mediastinum is shifted toward the contralateral side
Dyspnea
Reduction in lung volumes
Ventricular filling may be
impeded leading to decreased
cardiac out put
SYMPTOMS PHYSICAL EXAM
Dyspnea I: Discrepancy in size of
Pleuritic chest pain hemithorax
Non-productive cough P: Decreased tactile
fremitus
P: Dullness to
percussion
A: Decreased breath
sounds
Minimal free pleural effusion Moderate free pleural
effusion
Large free pleural effusion Massive pleural effusion
Thoracocentesis terapeutic
Chest tube insertion
= THORACENTESIS
= PLEURAL ASPIRATION
= PLEURAL TAPPING
Ensure documented
consent is obtained
(encompass common and
serious complications)
Complications:
pneumothorax, procedure
fail, pain, haemorrhage,
visceral injury.
Patient position and site of
insertion: the preferred
site for insertion of the
needle should be the
triangle safety
Equipment:
Skin sterilising fluid: alkohol 70% and povidone
iodine
A clean dressing
A 10 ml syringe
A 50 ml syringe
A three-way tap
Intravenous cannula/abbocath 14
Tubing/syringe
Lidocaine 2%
Sterile gloves
Procedure:
1. Local anaesthetic is infiltrated into the site of
thoracocentesis
2. A 10 ml syringe is used to raise a dermal bleb before
deeper infiltration of the intercostal muscles and
pleural surface (a spinal needle may be required in the
presence of a thick chest wall)
3. Local anaesthetic such as lidocaine (up to 3 mg/kg)
is usually infiltrated. Higher doses may result in
toxic levels
4. The pleural space should be aspirated with the
needle used to administer the local anaesthetic
Procedure (continued…)
5. The aspiration needle or cannula/abbocath 14
should then be advanced into the chest, aspirating
continually until the pleura is breached and fluid are
withdrawn
6. The cannula/abbocath 14 should then be attached to
a three-way tap and fluid withdrawn into the syringe
and expelled via the free port of the three-way tap into
a bag or jug for fluid
7. This process should be repeated and continued until
the procedure is terminated.
8. The cannula/abbocath 14 is then removed and
simple dressing applied
The procedure should be stopped
When no more fluid can be aspirated
The patient develops symptoms of cough or chest
discomfort, or
1.5 l has been withdrawn
Because massive pleural effusion is a sign of
disease and not a diagnosis in itself, after
therapeutic thoracocentesis the patient
should be referred to the pulmonologist for
further management.
http://www.nejm.org/doi/full/10.1056/NEJMvc
m053812
JUAH
Вам также может понравиться
- Pleural Effusion, A Simple Guide To The Condition, Treatment And Related ConditionsОт EverandPleural Effusion, A Simple Guide To The Condition, Treatment And Related ConditionsОценок пока нет
- Bronchopleural Fistula 1frankДокумент105 страницBronchopleural Fistula 1frankroshjamesОценок пока нет
- Pleural Effusion: PathophysiologyДокумент6 страницPleural Effusion: PathophysiologyNyamburaОценок пока нет
- THORACENTESISДокумент11 страницTHORACENTESISJeann sumbillaОценок пока нет
- Tube Thoracostomy GuideДокумент47 страницTube Thoracostomy GuideleizelgalvezОценок пока нет
- EmpyemaДокумент1 страницаEmpyemaMicah MagallanoОценок пока нет
- Chest PhysiotherapyДокумент2 страницыChest PhysiotherapyCarmela Dawn MarcoОценок пока нет
- NursingBulletin Notes On PneumothoraxДокумент27 страницNursingBulletin Notes On Pneumothoraxseigelystic100% (11)
- Brief Description: Pleural EffusionДокумент3 страницыBrief Description: Pleural EffusionJessica CatacutanОценок пока нет
- ThoracentesisДокумент9 страницThoracentesisPatricia G ChiuОценок пока нет
- Pleural Conditions: Pleurisy (Pleuritis)Документ10 страницPleural Conditions: Pleurisy (Pleuritis)merin sunilОценок пока нет
- Therapeutic and Diagnostic ProceduresДокумент27 страницTherapeutic and Diagnostic Proceduresamare mitkuОценок пока нет
- ThoracentesisДокумент36 страницThoracentesisMarivic DianoОценок пока нет
- Surgical InstrumentsДокумент28 страницSurgical InstrumentsNama Best100% (1)
- Advanced Airway Care: Intensive Care Unit PerspectiveДокумент42 страницыAdvanced Airway Care: Intensive Care Unit PerspectiveJeffery Samuel100% (1)
- Assisting in Patients Undergoing A ThoracentesisДокумент7 страницAssisting in Patients Undergoing A Thoracentesiscoosa liquorsОценок пока нет
- Suctioning Techniques and ProceduresДокумент24 страницыSuctioning Techniques and Proceduresluis_chubee100% (1)
- EmpyemaДокумент107 страницEmpyemaNITHA KОценок пока нет
- How to Perform Suctioning for an Intubated PatientДокумент24 страницыHow to Perform Suctioning for an Intubated PatientLanz LlnsОценок пока нет
- Chest Tube ThoracostomyДокумент5 страницChest Tube ThoracostomyChristine AduvisoОценок пока нет
- Chest Tube TherapyДокумент5 страницChest Tube Therapye항해Оценок пока нет
- Bronchial Hygiene Therapy ElectiveДокумент20 страницBronchial Hygiene Therapy ElectiveHelen Grace Dela Cruz0% (1)
- Chest Tubes, Pneumonectomy, Lobectomy, PleuralДокумент40 страницChest Tubes, Pneumonectomy, Lobectomy, PleuralMuhammad AliОценок пока нет
- Thoracocentes IS: (Pleural Tap)Документ9 страницThoracocentes IS: (Pleural Tap)Farhan AfzalОценок пока нет
- MX of Pleural DisorderДокумент17 страницMX of Pleural DisorderKun KandaОценок пока нет
- CHEST PROCEDURESДокумент10 страницCHEST PROCEDURESSilinna May Lee SanicoОценок пока нет
- Essential Tracheostomy Suctioning TechniquesДокумент33 страницыEssential Tracheostomy Suctioning TechniquesSuchit Kumar50% (2)
- Thoracentesis IntroductionДокумент8 страницThoracentesis Introductionjyoti singhОценок пока нет
- Thoracentesis Is Also Known As Pleural Fluid AnalysisДокумент3 страницыThoracentesis Is Also Known As Pleural Fluid AnalysisJ.r. MercadoОценок пока нет
- PneumothoraxДокумент6 страницPneumothoraxmengjapson123Оценок пока нет
- THORACENTESISДокумент14 страницTHORACENTESISKatherine Jeanne RosalОценок пока нет
- Tracheostomy EmergenciesДокумент32 страницыTracheostomy EmergenciesDr-Firas Nayf Al-Thawabia100% (1)
- Chest Tubes: Indications, Placement and CareДокумент76 страницChest Tubes: Indications, Placement and CareMarites Santos AquinoОценок пока нет
- Macro PneumohemoДокумент28 страницMacro PneumohemoSiti AishahОценок пока нет
- Abdominal ParacentesisДокумент5 страницAbdominal ParacentesisSivaprasad S100% (1)
- Seminar On ETДокумент10 страницSeminar On ETISLAMIC KNOWLEDGE BASED ON TRULY HADISОценок пока нет
- Intercostal Drain Chest Drain Pleural Drain InsertionДокумент5 страницIntercostal Drain Chest Drain Pleural Drain InsertionDr. rohith JaiswalОценок пока нет
- Abdominal ParacentesisДокумент4 страницыAbdominal ParacentesisRashmi C S100% (1)
- THORACENTESIS pdfДокумент5 страницTHORACENTESIS pdfjinsi georgeОценок пока нет
- ThoracentesisДокумент10 страницThoracentesisGabriel Friedman100% (1)
- Alternative Airway Management TechniquesДокумент13 страницAlternative Airway Management TechniquesAlaa DaoudОценок пока нет
- Jurnal Abses PeritonsilarДокумент12 страницJurnal Abses PeritonsilarGita KurniasariОценок пока нет
- Chest TubeДокумент18 страницChest TubeAyu MasturaОценок пока нет
- Pyothorax Treatment & StagesДокумент22 страницыPyothorax Treatment & StagesAnkan Dey100% (1)
- Chest Tube DrainageДокумент3 страницыChest Tube DrainageCyndi Jane Bandin Cruzata100% (1)
- Et CareДокумент15 страницEt CarePaulo GarciaОценок пока нет
- SP42 Thoracentesis (Adult)Документ7 страницSP42 Thoracentesis (Adult)Adam HuzaibyОценок пока нет
- Chest TubesДокумент27 страницChest TubesJerson EdilloОценок пока нет
- NCP PneumothoraxДокумент3 страницыNCP Pneumothorax'Harold Mark Borja100% (2)
- 7.2 IV InjectionДокумент4 страницы7.2 IV InjectionManisa ParidaОценок пока нет
- ThoracentesisДокумент20 страницThoracentesislovelots1234100% (2)
- Respiratory Care ModalitiesДокумент5 страницRespiratory Care ModalitiesWendy EscalanteОценок пока нет
- BronchiectasisДокумент40 страницBronchiectasisyana jaeОценок пока нет
- Safe SuctioningДокумент31 страницаSafe SuctioningKatrina Ponce100% (2)
- Chest Tubes and ThoracentesisДокумент18 страницChest Tubes and ThoracentesisecleptosОценок пока нет
- Basic Nursing ProceduresДокумент9 страницBasic Nursing Proceduresbernadette_olaveОценок пока нет
- TreatmentДокумент1 страницаTreatmentScheibe VanityОценок пока нет
- PNEUMOTHORAX - ManuscriptДокумент6 страницPNEUMOTHORAX - ManuscriptPrincess Quennie Pardo GuroОценок пока нет
- Physiotherapy in Respiratory MedicineДокумент8 страницPhysiotherapy in Respiratory MedicineHAMMYER ALROKHAMIОценок пока нет
- BHTДокумент18 страницBHTNitesh KumawatОценок пока нет
- GAIN-SS Manual PDFДокумент32 страницыGAIN-SS Manual PDFAmethyst CareyОценок пока нет
- Comparison of Bupivacaine-Dexmedetomidine VS Bupivacaine-Fentanyl VS Bupivacaine - Saline For Unilateral Spinal Anaesthesia in Lower Limb SurgeryДокумент9 страницComparison of Bupivacaine-Dexmedetomidine VS Bupivacaine-Fentanyl VS Bupivacaine - Saline For Unilateral Spinal Anaesthesia in Lower Limb SurgeryIJAR JOURNALОценок пока нет
- EVRMC 1st EndorsementДокумент4 страницыEVRMC 1st EndorsementPatrick DycocoОценок пока нет
- 7 - Nursing Service Floating and Pull OutДокумент4 страницы7 - Nursing Service Floating and Pull Outakositabon100% (3)
- Chapter 026 CoagulationДокумент7 страницChapter 026 Coagulationthubtendrolma100% (3)
- Maternal & Child Care Nursing Table of ContentsДокумент2 страницыMaternal & Child Care Nursing Table of Contentsɹǝʍdןnos100% (4)
- Use of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFДокумент9 страницUse of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFJose Luis Granados SolerОценок пока нет
- Effectiveness of Structured Teaching Program On Knowledge and Practice-FormatДокумент7 страницEffectiveness of Structured Teaching Program On Knowledge and Practice-FormatAtul PrabhuОценок пока нет
- Rebekah Wilson PT ResumeДокумент3 страницыRebekah Wilson PT Resumeapi-487211279Оценок пока нет
- 4 - Tracheostomy Care and SuctioningДокумент4 страницы4 - Tracheostomy Care and SuctioningABEGAIL BALLORANОценок пока нет
- Roleplay Procedure Nasogastric Incubation (NGT)Документ3 страницыRoleplay Procedure Nasogastric Incubation (NGT)naimathur rodiyahОценок пока нет
- SRJI 4-3-2015 Historical Roots of Acupressure Pillows PatentsДокумент4 страницыSRJI 4-3-2015 Historical Roots of Acupressure Pillows PatentsDr. Krishna N. SharmaОценок пока нет
- Cover Letter To The EditorДокумент2 страницыCover Letter To The EditorMohamed GhaliОценок пока нет
- Efficacy and Safety of Rabeprazole in Children.20Документ10 страницEfficacy and Safety of Rabeprazole in Children.20Ismy HoiriyahОценок пока нет
- Unconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationДокумент4 страницыUnconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationAdvanced Research PublicationsОценок пока нет
- Competitor AnalysisДокумент30 страницCompetitor AnalysisMukulОценок пока нет
- Inguinal LAPДокумент12 страницInguinal LAPDarawan MirzaОценок пока нет
- Greater Political ParticipationДокумент12 страницGreater Political ParticipationBe-COOL State Of MindОценок пока нет
- LPS AnnouncementsДокумент124 страницыLPS AnnouncementsNEWS CENTER MaineОценок пока нет
- MOH, DHA and HAAD recalls from 2017 WhatsApp groupДокумент32 страницыMOH, DHA and HAAD recalls from 2017 WhatsApp groupshahzadОценок пока нет
- Pantoea Agglomerans - AДокумент9 страницPantoea Agglomerans - AmadelaineОценок пока нет
- Bharat India: Extremely Bad Status of Testing & VaccinationДокумент308 страницBharat India: Extremely Bad Status of Testing & VaccinationP Eng Suraj SinghОценок пока нет
- Comparing Phenol and Apamarg Kshar for Sclerotherapy in Bleeding PilesДокумент8 страницComparing Phenol and Apamarg Kshar for Sclerotherapy in Bleeding PilesNishant SainiОценок пока нет
- Private Practice and Public School Speech Therapy Options in AustinДокумент2 страницыPrivate Practice and Public School Speech Therapy Options in Austiniese027Оценок пока нет
- FNDRC Vol 2 AppendicesДокумент43 страницыFNDRC Vol 2 AppendicesJohn Michael Macabenta100% (1)
- Assessment of The Thorax and LungsДокумент108 страницAssessment of The Thorax and LungsJohn Martin Casihan100% (3)
- Hematology - Oncology - PREP 2021Документ46 страницHematology - Oncology - PREP 2021drthanalla100% (1)
- Clinical Profile of Indian Children With Down SyndromeДокумент5 страницClinical Profile of Indian Children With Down SyndromeRicky Wahyu setiawanОценок пока нет
- IMCI - For PakistanДокумент35 страницIMCI - For Pakistanerajkhan100% (1)
- First Aid - CPR ProjectДокумент13 страницFirst Aid - CPR ProjectJade MorrisОценок пока нет