Академический Документы
Профессиональный Документы
Культура Документы
Congenital Heart Defect-Vsd
Загружено:
Auni Akif Aleesa0 оценок0% нашли этот документ полезным (0 голосов)
142 просмотров53 страницыVentricular septal defect (VSD) is a congenital heart defect that causes a hole in the wall separating the left and right ventricles of the heart. There are several types of VSD depending on the location of the hole. VSDs are usually caused by abnormal formation of the heart during fetal development. Untreated VSDs can cause lung and heart complications due to abnormal blood flow. Surgical repair is often needed to close large VSDs. Nursing care focuses on pre-and post-operative care and patient/family education about VSD management and signs of complications.
Исходное описание:
Congenital Heart Defect-Vsd
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документVentricular septal defect (VSD) is a congenital heart defect that causes a hole in the wall separating the left and right ventricles of the heart. There are several types of VSD depending on the location of the hole. VSDs are usually caused by abnormal formation of the heart during fetal development. Untreated VSDs can cause lung and heart complications due to abnormal blood flow. Surgical repair is often needed to close large VSDs. Nursing care focuses on pre-and post-operative care and patient/family education about VSD management and signs of complications.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
142 просмотров53 страницыCongenital Heart Defect-Vsd
Загружено:
Auni Akif AleesaVentricular septal defect (VSD) is a congenital heart defect that causes a hole in the wall separating the left and right ventricles of the heart. There are several types of VSD depending on the location of the hole. VSDs are usually caused by abnormal formation of the heart during fetal development. Untreated VSDs can cause lung and heart complications due to abnormal blood flow. Surgical repair is often needed to close large VSDs. Nursing care focuses on pre-and post-operative care and patient/family education about VSD management and signs of complications.
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 53
ARTRIAL SEPTAL DEFECT
VENTRICULAR SEPTAL DEFECT
PBP SAKINAH BINTI SHAFFAI
1/2017
OBJECTIVE
Introduction of congenital heart defect
Definition of ventricular septal defect
(VSD)
Type of ventricular septal defect
Etiology (cause) of VSD
Pathophysiology of VSD
OBJECTIVE
Manifestion clinical of VSD
Investigation of VSD
Management of VSD
Nursing care plan & health educations
INTRODUCTIONS
CONGENITAL HEART DEFECT
Congenital heart defects have been
classified into several categories. It divided
into acynotic and cynotic defects.
Children with acynotic defect may
develop cynocis
CONGENITAL HEART DEFECT
Children with cynotic defect may be pink
and have more clinical signs of heart
failure
More than 35 types of congenital heart
defect have been identified, and some
patient have multiple defects
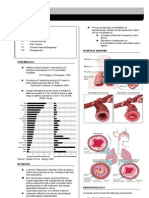
CONGENITAL HEART DEFECTS
ACYNOTIC CYNOTIC
↑ Pulmonary Obstruction to ↓Pulmonary Mixed
blood flow blood flow blood flow blood flow
from ventricles
Coartation of aorta Transposition of great
Aortic stenosis arteries
Pulmonic stenosis Total anomalous pulmonary
venous return
Atrial septal defect Truncus arteriosus
Ventricular septal defect
Patent ductus arteriosus Tetralogy of Fallot Hypoplastic left heart
Atrioventricular canal Tricuspid atresia syndrome
VENTRICULAR
SEPTAL DEFECT
DESCRIPTION
Abnormal opening between the right and
left ventricles, (hole in the part of dividing
wall - septum) classified according to
location. Membranous (80%) or
muscular
DESCRIPTION
VSD are frequently assosiated with other
defect such as pulmonaric stenosis,
transposition of the great vessels, ductus
arterious, atrial defects and coarctation
of the aorta.
DESCRIPTION
Many VSDs (20% - 60%) close
spontaneously. (1st year of life in children
having small or moderate defect)
DESCRIPTION
A ventricular septal defect allows
oxygen-rich (red) blood to pass from the
left ventricle, through the opening in the
septum, and then mix with oxygen-poor
(blue) blood in the right ventricle
Common type of congenital heart defect
(25%)
There are basic types of ventricular
septal defect (VSD)
Conal septal VSD
Muscular VSD
The most common type of VSD
It is an opening in the muscular portion
of the lower section of the ventricular
septum
Usually close spontaneously and do not
require surgery
Perimembranous VSD
Opening in an area of the upper section
of the ventricular septum (membranous
septum), located near the valves
Require surgery because most do not
close on their own
Atrioventricular canal type VSD
Associated with atrioventricular canal
defect. This VSD located underneath the
tricuspid and mitral valves
Conal septal defect.
The rarest of VSD
It occurs in the ventricular septum just
below the pulmonary valve
ETIOLOGY
8weeks of gestation (formation of the
heart)
begins as a hollow tube
it partitions into two sides
creating a wall (septum)
the partitioning process are not complete
leaving an opening in the ventricular
septum
Ventricular septal defect
ETIOLOGY
Genetic link
Gene defects : chromosome
abnormalities
Environmental exposure
Occur sporadically by chance with no
clear cause
PATHOPHYSIOLOGY
Higher pressure within the left
ventricles
Blood flow through the defect into the
pulmonary artery
Increased blood volume pumped into
the lungs
Increase pulmonary vascular
resistence
Increased pressure in the in the right
ventricle
Left to right shunting and pulmonary
resistent
Right atrium also enlarge
Incomplete right ventricular emptying
CLINICAL MANIFESTATION
Fatigue
Sweating
Rapid breathing
Heavy breathing
Congested breathing
Disinterest in feeding or tiring while feeding
Poor WT gain
INVESTIGATIONS
Auscaltion – heart murmur (basis of
pitch, loudness and duration)
Chest Xray – enlarged
ECG or EKG – arrhythmias or
dysrhythmias
Echocardiogram – show the pattern of
blood flow through the septal opening
MANAGEMENT
Surgical management
• Palliative – pulmonary artery banding
(placement of a band around the main
pulmonary artery to decrease pulmonary
blood flow ) – multiple muscular VSDs or
complex anatomy
Surgical management
• Complete repair –
o small defects are repaired with
sutures
o Larged defect : sewing a knitted
Darcon patch over the opening require.
o Cardiopulmonay bypass is used both
procedures
NonSurgical management
• Catheter closure of muscular
COMPLICATIONS
Lung disease – extra blood passes
through the pulmonary artery into
the lungs causing higher than
normal pressure in the lung’s blood
vessel
NURSING CARE PLAN
Tanggungjawab jururawat sebelum
pembedahan
1. Beri penerangan kepada ibubapa /
penjaga berkaitan pembedahan yang
akan dilakukan dengan bahasa yang
mudah untuk mendapatkan kerjasama
dan mengurangkan kebimbangan
ibubapa.
2. Pastikan consent telah ditandatangani
oleh ibu atau bapa pesakit selepas
penerangan oleh doctor sebagai
persetujuan pembedahan dan juga
sebagai medicol legal
3. Puasakan pesakit sekurang –
kurangnya 6 jam sebagai persediaan
bowel dan untuk mengelak risiko
aspiration pneumonia.
4. Berikan terapi Interavena seperti ½
saline dextrose 5% per body weight per
hour atas arahan doktor untuk
memgekalkan status hydration serta
monitor intake output pesakit untuk
mengenalpasti kesimbangan intake dan
out put pesakit
5. Bantu doctor dalam pengambilan blood
investigation seperti FBC, BUSE,
PT/APPT sebagai baseline dan Group
Cross Match (GXM) persedia jika
berlaku pendarahan
6. Ambil vital sign seperti tekanan darah,
pulse, respiratorion, SPO2 dan
temperatue sebagai baseline dan
mengesan sebarang keabnormalan
7. Lakukan persediaan pesakit untuk ke
bilik pembedahan seperti menukar
pampers, tukar gown bedah, dan
tanggalkan barang – barang perhiasan
jika ada untuk mengurangkan risiko
infeksi
8. Berikan antibiotic prophylasis atas
arahan doktor seperti IV cefuroxime
25mg/kg prior operation untuk
mengurang risiko infeksi
Tanggungjawab jururawat selepas
pembedahan
1. Rehatkan pesakit dalam posisi lateral –
supine dengan kepala mengiring ke sisi
untuk mengelak aspirasi pneumonia
(muntah)
2. Lakukan pemerhatian keatas pesakit
dari segi
- Keadaan am dengan memerhati keadaan
pesakit, memek muka dan
- Tanda vital untuk mengesan pendarahan
seperti tekanan darah yang rendah,
tachycardia, tachypnea untuk tindakan
awal
- Luka pembedahan : pemerhati juga
pada luka pembedahan seperti ada
pendarah atau dressing soaked untuk
mengesan active bleeding
3. Pastikan keseimbangan cecair dan
elektrolite diteruskan dengan
memastikan patensi infusi interavena
mengalir dengan baik, merekod intake
Dan output pesakit
4. Kekalkan saluran pernafasan dengan
memerhati corak pernafasan, posisi
pesakit dalam posisi yang selesa jika
bukan kontraindikasi dan lakukan
sedutan kahak jika sekresi berlebihan
untuk melancarkan salur pernafasan.
Beri terapi oksigen jika perlu
5. Berikan pesakit patent controlled
analgesia continuous setiap 2 jam
hingga 6 jam untuk mengurangkan rasa
sakit
6. Rancang perawatan untuk
mengurangkan gangguan keatas
pesakit bagi memastikan pesakit
mendapat rehat secukupnya
Pendidikan kesihatan penjagaan
kanak – kanak congenital heart
disease
1. Beri penerangan kepada ibubapa
berkaitan penyakit menggunakan
diagram, picture, model supaya ibubapa
faham dengan jelas berkaitan proses
penyakit
2. Galak ibubapa pesakit menyertai
persatuan seperti Yayasan Jantung
Malaysia untuk sokongan moral
3. Terangkan kepada ibubapa tentang sign
and symptom of worsening clinical
status seperti tanda – tanda heart failure
(cynosis and hypercynotic spell)
2. Galak ibubapa pesakit menyertai
persatuan seperti Yayasan Jantung
Malaysia untuk sokongan moral
3. Terangkan kepada ibubapa tentang sign
and symptom of worsening clinical
status seperti tanda – tanda heart failure
(cynosis and hypercynotic spell) supaya
perawatan segera dapat dilakukan
5. Terangkan kepada ibubapa kepentingan
pengambilan ubatan untuk mengelak
risiko severe heart failure dan
arrhytmias
6. Terangkan kepada ibubapa kepentingan
pengambilan makan kaya zat nutrient
seperti high calorie sebagai membekal
tenaga dan high vitamin untuk
meningkatkan daya pertahanan badan
7. Nasihat ibubapa elak membawa kanak
– kanak ke tempat yang sesak dan
hadkan pelawat untuk mengurangkan
risiko infeksi kerana kanak – kanak CHD
mempunyai daya imuniti yang rendah
8. Nasihat ibubapa melengkapkan
suntikan immunisasi yang dijadualkan
dan galakkan pegambilan suntikan
immunisasi palizumab untuk mencegah
respiratory syncytial virus (RSV)
sebagai pelindungan tambahan badan
9. Terangkan kepada ibubapa berkaitan
perkembangan kanak – kanak tersebut.
Kanak – kanak yang serious heart
disease berisiko untuk developmental
delay
10.Beritahu ibubapa tentang kepentingan
meneruskan temujanji dengan doktor
untuk menilai perkembangan
Вам также может понравиться
- Congenital Heart DiseaseДокумент77 страницCongenital Heart DiseaseMalueth Angui100% (1)
- Congenital Heart Disease - ASDДокумент36 страницCongenital Heart Disease - ASDAuni Akif Aleesa100% (1)
- Congenital Heart Disease - Cynotic AcynoticДокумент34 страницыCongenital Heart Disease - Cynotic Acynoticvruttika parmarОценок пока нет
- Nursing the NeonateОт EverandNursing the NeonateMaggie MeeksОценок пока нет
- Hemophilia in ChildrenДокумент16 страницHemophilia in ChildrenVinay Sahu100% (1)
- Ventricular Septal DefectДокумент55 страницVentricular Septal DefecthoneyworksОценок пока нет
- NeonatalresuscitationДокумент67 страницNeonatalresuscitationfidaОценок пока нет
- Transposition of Great ArteriesДокумент18 страницTransposition of Great Arteriesparmeshori100% (2)
- Neonatal SeizuresДокумент4 страницыNeonatal SeizuresSerag EdeenОценок пока нет
- Neonatal SeizuresДокумент13 страницNeonatal SeizuresLuis Daniel Bernal CondeОценок пока нет
- Brain DeathДокумент12 страницBrain DeathAbdallahMousaОценок пока нет
- Meconium Aspiration SyndromeДокумент7 страницMeconium Aspiration SyndromeAi Niech Inoel100% (1)
- Hepatitis in ChildrenДокумент2 страницыHepatitis in ChildrenShilpi SinghОценок пока нет
- Neonatal HypocalcemiaДокумент8 страницNeonatal HypocalcemiaCristina Fernández ValenciaОценок пока нет
- Neonatal Golden HourДокумент28 страницNeonatal Golden HourGendis Ayu ArdiasОценок пока нет
- Neonatal Sepsis LectureДокумент142 страницыNeonatal Sepsis Lectureokwadha simion0% (1)
- Transient Tachypnea of The Newborn (TTN)Документ6 страницTransient Tachypnea of The Newborn (TTN)Wivan Havilian DjohanОценок пока нет
- National Control of Dirrheal Diseases (CDD) Program ObjectivesДокумент6 страницNational Control of Dirrheal Diseases (CDD) Program ObjectivesJoy FucananОценок пока нет
- Pediatrics: by DR - Mohammad Z. Abu Sheikha@Документ101 страницаPediatrics: by DR - Mohammad Z. Abu Sheikha@صقر حوران100% (1)
- BSC Nursing: Medical Surgical Nursing Unit V - Disorders of The Cardio Vascular SystemДокумент34 страницыBSC Nursing: Medical Surgical Nursing Unit V - Disorders of The Cardio Vascular SystemPoova Ragavan100% (1)
- Rheumatic Fever and RHDДокумент49 страницRheumatic Fever and RHDbereket gashuОценок пока нет
- 05 Polycythemia in The NewbornДокумент11 страниц05 Polycythemia in The NewbornMorales Eli PediatraОценок пока нет
- Congenital SyphilisДокумент6 страницCongenital SyphilisFrozen Pandora MahayaОценок пока нет
- HypothermiaДокумент5 страницHypothermiaMRS CHAKRAPANIОценок пока нет
- Non Hodgkin Lymphoma in ChildrenДокумент4 страницыNon Hodgkin Lymphoma in ChildrenMilzan MurtadhaОценок пока нет
- Neonatal Hypoglycemia: 1.transient (Most Common) 2.persistenet (Less Common)Документ8 страницNeonatal Hypoglycemia: 1.transient (Most Common) 2.persistenet (Less Common)mohammadОценок пока нет
- Appproach To A Case of Status Epilepticus in PaediatricsДокумент45 страницAppproach To A Case of Status Epilepticus in PaediatricsChin NamОценок пока нет
- Patent Ductus Arteriosus (PDA)Документ6 страницPatent Ductus Arteriosus (PDA)Sintia MardhaОценок пока нет
- Allergic Rhinitis in ChildrenДокумент7 страницAllergic Rhinitis in ChildrenTina MorleyОценок пока нет
- ALLERGIC RHINITIS IN CHILDREN RinaДокумент39 страницALLERGIC RHINITIS IN CHILDREN Rinarinajacky100% (2)
- Hematological Alterations: Disseminated Intravascular Coagulation (DIC)Документ16 страницHematological Alterations: Disseminated Intravascular Coagulation (DIC)jhommmmmОценок пока нет
- Persistent Newborn Pulmonary HypertensionДокумент10 страницPersistent Newborn Pulmonary HypertensionWali MoralesОценок пока нет
- Neonatal BLSДокумент18 страницNeonatal BLSPatrickNichols0% (1)
- Lec 2, Congenital Heart DiseasesДокумент61 страницаLec 2, Congenital Heart DiseasesAlexandrescuОценок пока нет
- Neonatal ExaminationДокумент50 страницNeonatal ExaminationCLEMENT50% (2)
- Approach To Bleeding NeonateДокумент20 страницApproach To Bleeding NeonateIndranil DuttaОценок пока нет
- Respiratory DistressДокумент11 страницRespiratory DistressHina MasoodОценок пока нет
- Hypoxic Ischemic EncephalopathyДокумент7 страницHypoxic Ischemic EncephalopathyJennesse May Guiao IbayОценок пока нет
- Congenital SyphilisДокумент3 страницыCongenital SyphilisadmusОценок пока нет
- Neonatal SepsisДокумент53 страницыNeonatal SepsisFrancis AmuzuОценок пока нет
- MECONIUM Aspiration SyndromeДокумент37 страницMECONIUM Aspiration SyndromekamalaОценок пока нет
- Idiopathic Thrombocytopenic PurpuraДокумент8 страницIdiopathic Thrombocytopenic PurpuraMonette Abalos MendovaОценок пока нет
- Renal Failure in ChildrenДокумент43 страницыRenal Failure in Childrendennyyy175Оценок пока нет
- AsphyxiaДокумент35 страницAsphyxiaAna Cristina Montillano100% (1)
- Newborn Respiratory Distress 11.28.2011Документ41 страницаNewborn Respiratory Distress 11.28.2011Emily EresumaОценок пока нет
- Hirschsprung DiseaseДокумент19 страницHirschsprung DiseaseUgi Rahul100% (1)
- DR Varsha Atul Shah Senior Consultant Dept of Neonatal and Devt Medicine, SGH Visiting Consultant Dept of Child Devt, KKHДокумент47 страницDR Varsha Atul Shah Senior Consultant Dept of Neonatal and Devt Medicine, SGH Visiting Consultant Dept of Child Devt, KKHJennifer MrjОценок пока нет
- Final Exam NotesДокумент24 страницыFinal Exam NotesNicholeGarcesCisnerosОценок пока нет
- OS 213 Pediatric AsthmaДокумент8 страницOS 213 Pediatric Asthma2012Оценок пока нет
- Laryngomalacia - PPTX Dr. FeriДокумент114 страницLaryngomalacia - PPTX Dr. FeriAldy BimaОценок пока нет
- Neonatal Seizures: Bhavith Ravi Medical StudentДокумент16 страницNeonatal Seizures: Bhavith Ravi Medical StudentkakuОценок пока нет
- Anatomic Disorders of Female Reproductive SystemДокумент42 страницыAnatomic Disorders of Female Reproductive SystemNelly AstikaОценок пока нет
- Atrial Septal Defect: by DR - AnandДокумент21 страницаAtrial Septal Defect: by DR - AnandJaya PrabhaОценок пока нет
- Status EpilepticusДокумент28 страницStatus EpilepticusDaniel AlfredОценок пока нет
- Pathophysiology of Birth AsphyxiaДокумент14 страницPathophysiology of Birth AsphyxiaEduardo Rios DuboisОценок пока нет
- A Neonate With Acute Kidney Injury: Case PresentationДокумент4 страницыA Neonate With Acute Kidney Injury: Case PresentationSahil DhamijaОценок пока нет
- Congenital Cyanotic Heart DiseaseДокумент26 страницCongenital Cyanotic Heart DiseaseAlokh Saha Raj100% (1)
- Etiology PPPДокумент24 страницыEtiology PPPCresty Estalilla100% (1)
- Perioperative Fluid Management in ChildrenДокумент31 страницаPerioperative Fluid Management in ChildrenRashmi SahaОценок пока нет
- Conginital Heart DiseaseДокумент19 страницConginital Heart DiseaseSanthosh.S.UОценок пока нет
- Soalan MEQ Head InjuryДокумент7 страницSoalan MEQ Head InjuryAuni Akif Aleesa100% (1)
- Table 2 of TMC501 Lesson 3 Go On Holiday (Prepared by Dr. Neo Kian Sen)Документ4 страницыTable 2 of TMC501 Lesson 3 Go On Holiday (Prepared by Dr. Neo Kian Sen)Auni Akif AleesaОценок пока нет
- Febrile FitДокумент3 страницыFebrile FitAuni Akif AleesaОценок пока нет
- Table 1 of TMC501 Lesson 2 Kampung Life (Prepared by Dr. Neo Kian Sen)Документ2 страницыTable 1 of TMC501 Lesson 2 Kampung Life (Prepared by Dr. Neo Kian Sen)Auni Akif AleesaОценок пока нет
- RainДокумент1 страницаRainAuni Akif Aleesa50% (2)
- Cell, TissueДокумент8 страницCell, TissueAuni Akif AleesaОценок пока нет
- Heart Failure - Nursing ManagementДокумент9 страницHeart Failure - Nursing ManagementAuni Akif Aleesa100% (1)
- Quick NOteДокумент7 страницQuick NOteAuni Akif Aleesa100% (1)
- Ebook Concepts of Fitness and Wellness A Comprehensive Lifestyle Approach 10Th Edition Corbin Test Bank Full Chapter PDFДокумент30 страницEbook Concepts of Fitness and Wellness A Comprehensive Lifestyle Approach 10Th Edition Corbin Test Bank Full Chapter PDFkaylinque98y2100% (11)
- April 2021 - Pediatric Emergency CareДокумент128 страницApril 2021 - Pediatric Emergency CareEdison Junior Juarez LaricoОценок пока нет
- Pathology of Blood VesselsДокумент80 страницPathology of Blood VesselsiqiqiqiqiqОценок пока нет
- Na Hypo PotomaniaДокумент7 страницNa Hypo Potomaniaanderson roberto oliveira de sousaОценок пока нет
- Physiology Mid Q Part 3 VIPДокумент16 страницPhysiology Mid Q Part 3 VIPDanah AlhusainiОценок пока нет
- Jalil 2017Документ24 страницыJalil 2017Karel ZertucheОценок пока нет
- Byrd PDFДокумент16 страницByrd PDFEghet SilviuОценок пока нет
- Uia 10 CARDIOVASCULAR PHYSIOLOGYДокумент7 страницUia 10 CARDIOVASCULAR PHYSIOLOGYLiliesther Erminda Hernandez VallecilloОценок пока нет
- Rendam Kaki Dengan Rebusan Jahe Merah Dapat Mencegah Terjadinya EklamsiaДокумент8 страницRendam Kaki Dengan Rebusan Jahe Merah Dapat Mencegah Terjadinya EklamsiaMellwandariskОценок пока нет
- Contemporary Outcomes of Percutaneous Closure of Patent Ductus Arteriosus in Adolescents and Adults PDFДокумент8 страницContemporary Outcomes of Percutaneous Closure of Patent Ductus Arteriosus in Adolescents and Adults PDFMuhammad IrfanОценок пока нет
- Pericardial Effusion and Cardiac TamponadeДокумент18 страницPericardial Effusion and Cardiac TamponadeSiti Hamidah Abd Aziz100% (1)
- Basic ECG InterpretationДокумент16 страницBasic ECG InterpretationKim BadillesОценок пока нет
- Anatomy of Mitral ValveДокумент6 страницAnatomy of Mitral ValvesrhubanbabuОценок пока нет
- Fundamentals of CT PDFДокумент415 страницFundamentals of CT PDFAl Marchese100% (1)
- Antihypertensive DrugsДокумент62 страницыAntihypertensive DrugsYeshaa MiraniОценок пока нет
- Pacemaker Timing & IntervalsДокумент124 страницыPacemaker Timing & IntervalsNiranjan Reddy100% (1)
- 1 Tolerancia Al Esfuerzo MyersДокумент9 страниц1 Tolerancia Al Esfuerzo MyersAMALIAОценок пока нет
- Anph121lb CardiovascularДокумент28 страницAnph121lb CardiovascularDANIELA PEREZОценок пока нет
- Heart Failure: Christian Rey Cayabyab Y3 Medical Student University of LimerickДокумент16 страницHeart Failure: Christian Rey Cayabyab Y3 Medical Student University of LimerickChristian CayabyabОценок пока нет
- Carto3 Fact SheetДокумент3 страницыCarto3 Fact SheetVimal NishadОценок пока нет
- Guidelines and Standards: KeywordsДокумент18 страницGuidelines and Standards: KeywordsTuan HaiОценок пока нет
- ACC-AHA Guidelines Heart FailureДокумент56 страницACC-AHA Guidelines Heart FailureUswatul HasanahОценок пока нет
- Diagnosis and Management of Myocardial InfarctionДокумент69 страницDiagnosis and Management of Myocardial InfarctionSanjana GkОценок пока нет
- Ananya Basu Internal Medicine Clinical CaseДокумент4 страницыAnanya Basu Internal Medicine Clinical Caseavnikasharma4889Оценок пока нет
- 2018CV03Документ22 страницы2018CV03Cheng-Ting WuОценок пока нет
- Divine Intervention Step 2CK Podcasts Notes - Read Only File - Docx (Dragged) 4Документ3 страницыDivine Intervention Step 2CK Podcasts Notes - Read Only File - Docx (Dragged) 4winston1234Оценок пока нет
- Circulatory SystemДокумент21 страницаCirculatory SystemKumar Sujeet100% (1)
- Regulation of Coronary Blood Flow PDFДокумент330 страницRegulation of Coronary Blood Flow PDFAlin-Octavian BorinaОценок пока нет
- The Transport System IB Qq'sДокумент12 страницThe Transport System IB Qq'sJohn OsborneОценок пока нет
- Unicare Product List (Oct. 2023)Документ3 страницыUnicare Product List (Oct. 2023)rizaie.azizuddin2022Оценок пока нет