Академический Документы
Профессиональный Документы
Культура Документы
Lymphoid Lekemia: DR Budi Enoch SPPD
Загружено:
Lia pramita0 оценок0% нашли этот документ полезным (0 голосов)
13 просмотров32 страницыBhh
Оригинальное название
Lymphoid lekemia
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документBhh
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
13 просмотров32 страницыLymphoid Lekemia: DR Budi Enoch SPPD
Загружено:
Lia pramitaBhh
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 32
LYMPHOID LEKEMIA
DR BUDI ENOCH SPPD
• Malignancies of lymphoid cells range from the most
indolent to the most aggressive human malignancies.
• These cancers arise from cells of the immune system at
different stages of differentiation, resulting in a wide
range of morphologic, immunologic, and clinical
findings. Insights on the normal immune system have
allowed a better understanding of these sometimes
confusing disorders.
• Some malignancies of lymphoid cells almost always
present as leukemia (i.e., primary involvement of bone
marrow and blood), while others almost always present
as lymphomas (i.e., solid tumors of the immune system).
• However, other malignancies of lymphoid cells can
present as either leukemia or lymphoma
WHO CLASSIFICATION
• The classification of lymphoid cancers evolved steadily
throughout the twentieth century. The distinction between
leukemia and lymphoma was made early, and separate
classification systems were developed for each.
• Leukemias were first divided into acute and chronic subtypes
based on average survival. Chronic leukemias were easily
subdivided into those of lymphoid or myeloid origin based on
morphologic characteristics.
• However, a spectrum of diseases that were formerly all called
chronic lymphoid leukemia has become apparent (Table 110–
1). The acute leukemias were usually malignancies of blast
cells with few identifying characteristics. When cytochemical
stains became available, it was possible to divide these
objectively into myeloid malignancies and acute leukemias of
lymphoid cells.
• Acute leukemias of lymphoid cells have been subdivided
based on morphologic characteristics by the French-
American-British (FAB) group (Table 110–2).
• Non-Hodgkin's lymphomas were separated from
Hodgkin's disease by recognition of the Sternberg-Reed
cells early in the twentieth century.
• The histologic classification for non-Hodgkin's lymphomas
has been one of the most contentious issues in oncology.
Imperfect morphologic systems were supplanted by
imperfect immunologic systems, and poor reproducibility
of diagnosis has hampered progress.
• In 1999, the World Health Organization (WHO)
classification of lymphoid malignancies was devised
through a process of consensus development among
international leaders in hematopathology and clinical
oncology. The WHO classification takes into account
morphologic, clinical, immunologic, and genetic
information and attempts to divide non-Hodgkin's
lymphomas and other lymphoid malignancies into
clinical/pathologic entities that have clinical and
therapeutic relevance.
GENERAL ASPECTS OF
LYMPHOID MALIGNANCIES
ETIOLOGY AND EPIDEMIOLOGY
• The relative frequency of the various lymphoid malignancies is shown
in Fig. 110-1.
• Chronic lymphoid leukemia (CLL) is the most prevalent form of
leukemia in Western countries. It occurs most frequently in older adults
and is exceedingly rare in children. In 2010, 14,990 new cases were
diagnosed in the United States, but because of the prolonged survival
associated with this disorder, the total prevalence is many times
higher.
• CLL is more common in men than in women and more common in
whites than in blacks. This is an uncommon malignancy in Asia. The
etiologic factors for typical CLL are unknown.
• In contrast to CLL, acute lymphoid leukemias (ALLs) are predominantly
cancers of children and young adults. The L3 or Burkitt's leukemia
occurring in children in developing countries seems to be associated
with infection by the Epstein-Barr virus (EBV) in infancy. However, the
explanation for the etiology of more common subtypes of ALL is much
less certain. Childhood ALL occurs more often in higher
socioeconomic subgroups. Children with trisomy 21 (Down syndrome)
have an increased risk for childhood ALL as well as acute myeloid
leukemia (AML). Exposure to high-energy radiation in early childhood
increases the risk of developing T cell ALL.
• A number of environmental factors have been implicated in the
occurrence of non-Hodgkin's lymphoma, including infectious
agents, chemical exposures, and medical treatments. Several
studies have demonstrated an association between exposure to
agricultural chemicals and an increased incidence in non-
Hodgkin's lymphoma.
• Patients treated for Hodgkin's disease can develop non-
Hodgkin's lymphoma; it is unclear whether this is a consequence
of the Hodgkin's disease or its treatment. However, a number of
non-Hodgkin's lymphomas are associated with infectious agents
(Table 110–4). HTLV-I infects T cells and leads directly to the
development of adult T cell lymphoma (ATL) in a small
percentage of infected patients.
• The cumulative lifetime risk of developing lymphoma in an
infected patient is 2.5%. The virus is transmitted by infected
lymphocytes ingested by nursing babies of infected mothers,
bloodborne transmission, or sexually. The median age of patients
with ATL is 56 years, emphasizing the long latency. HTLV-I is also
the cause of tropical spastic paraparesis—a neurologic disorder
that occurs somewhat more frequently than lymphoma and with
shorter latency and usually from transfusion-transmitted virus
IMMUNOLOGY
• All lymphoid cells are derived from a common hematopoietic
progenitor that gives rise to lymphoid, myeloid, erythroid,
monocyte, and megakaryocyte lineages.
• Through the ordered and sequential activation of a series of
transcription factors, the cell first becomes committed to the
lymphoid lineage and then gives rise to B and T cells.
• About 75% of all lymphoid leukemias and 90% of all
lymphomas are of B cell origin. A cell becomes committed to
B cell development when it begins to rearrange its
immunoglobulin genes. The sequence of cellular changes,
including changes in cell-surface phenotype, that
characterizes normal B cell development is shown in Fig. 110-2.
• A cell becomes committed to T cell differentiation upon
migration to the thymus and rearrangement of T cell antigen
receptor genes
Pathway of normal B cell differentiation and
relationship to B cell lymphomas. HLA-DR, CD10,
CD19, CD20, CD21, CD22, CD5, and CD38 are cell
markers used to distinguish stages of development.
Terminal transferase (TdT) is a cellular enzyme.
Immunoglobulin heavy chain gene rearrangement
(HCR) and light chain gene rearrangement or
deletion (R or D, R or D) occur early in B cell
development. The approximate normal stage of
differentiation associated with particular
lymphomas is shown. ALL, acute lymphoid
leukemia; CLL, chronic lymphoid leukemia; SL, small
lymphocytic lymphoma.
• Malignancies of lymphoid cells are associated with recurring
genetic abnormalities. While specific genetic abnormalities
have not been identified for all subtypes of lymphoid
malignancies, it is presumed that they exist.
• Genetic abnormalities can be identified at a variety of levels
including gross chromosomal changes (i.e., translocations,
additions, or deletions); rearrangement of specific genes that
may or may not be apparent from cytogenetic studies; and
overexpression, underexpression, or mutation of specific
oncogenes. Altered expression or mutation of specific proteins
is particularly important.
• Many lymphomas contain balanced chromosomal
translocations involving the antigen receptor genes;
immunoglobulin genes on chromosomes 2, 14, and 22 in B
cells; and T cell antigen receptor genes on chromosomes 7
and 14 in T cells.
• The rearrangement of chromosome segments to generate
mature antigen receptors must create a site of vulnerability to
aberrant recombination. B cells are even more susceptible to
acquiring mutations during their maturation in germinal
centers; the generation of antibody of higher affinity requires
the introduction of mutations into the variable region genes in
the germinal centers. Other nonimmunoglobulin genes, e.g.,
bcl-6, may acquire mutations as well.
APPROACH TO THE PATIENT:
LYMPHOID CELL
MALIGNANCIES
• Regardless of the type of lymphoid malignancy, the initial
evaluation of the patient should include performance of a
careful history and physical examination. These will help confirm
the diagnosis, identify those manifestations of the disease that
might require prompt attention, and aid in the selection of
further studies to optimally characterize the patient's status to
allow the best choice of therapy. It is difficult to overemphasize
the importance of a carefully done history and physical
examination. They might provide observations that lead to
reconsidering the diagnosis, provide hints at etiology, clarify the
stage, and allow the physician to establish rapport with the
patient that will make it possible to develop and carry out a
therapeutic plan.
• For patients with ALL, evaluation is usually completed after a
complete blood count, chemistry studies reflecting major organ
function, a bone marrow biopsy with genetic and immunologic
studies, and a lumbar puncture. The latter is necessary to rule out
occult CNS involvement. At this point, most patients would be
ready to begin therapy. In ALL, prognosis is dependent upon the
genetic characteristics of the tumor, the patient's age, the white
cell count, and the patient's overall clinical status and major
organ function.
• In CLL, the patient evaluation should include a complete blood
count, chemistry tests to measure major organ function, serum
protein electrophoresis, and a bone marrow biopsy.
CLINICAL FEATURES,
TREATMENT, AND
PROGNOSIS OF SPECIFIC
LYMPHOID MALIGNANCIES
PRECURSOR B CELL LYMPHOBLASTIC
LEUKEMIA/LYMPHOMA
• The most common cancer in childhood is B cell ALL. Although this
disorder can also present as a lymphoma in either adults or
children, presentation as lymphoma is rare.
• The malignant cells in patients with precursor B cell lymphoblastic
leukemia are most commonly of pre–B cell origin.
• Patients typically present with signs of bone marrow failure such
as pallor, fatigue, bleeding, fever, and infection related to
peripheral blood cytopenias.
• Peripheral blood counts regularly show anemia and
thrombocytopenia but might show leukopenia, a normal
leukocyte count, or leukocytosis based largely on the number of
circulating malignant cells.
• Extramedullary sites of disease are frequently involved in patients
who present with leukemia, including lymphadenopathy,
hepato- or splenomegaly, CNS disease, testicular enlargement,
and/or cutaneous infiltration.
• The diagnosis is usually made by bone marrow biopsy, which
shows infiltration by malignant lymphoblasts
TREATMENT: PRECURSOR B CELL
LYMPHOBLASTIC LEUKEMIA
• The treatment of patients with precursor B cell ALL
involves remission induction with combination
chemotherapy, a consolidation phase that includes
administration of high-dose systemic therapy and
treatment to eliminate disease in the CNS, and a period
of continuing therapy to prevent relapse and effect
cure. The overall cure rate in children is 90%, while 50% of
adults are long-term disease-free survivors. This reflects
the high proportion of adverse cytogenetic
abnormalities seen in adults with precursor B cell ALL.
• Precursor B cell lymphoblastic lymphoma is a rare
presentation of precursor B cell lymphoblastic
malignancy. These patients often have a rapid
transformation to leukemia and should be treated as
though they had presented with leukemia. The few
patients who present with the disease confined to lymph
nodes have a high cure rate.
B CELL CHRONIC LYMPHOID
LEUKEMIA/SMALL LYMPHOCYTIC
LYMPHOMA
• B cell CLL/small lymphocytic lymphoma represents the most
common lymphoid leukemia, and when presenting as a
lymphoma, it accounts for 7% of non-Hodgkin's lymphomas.
• Presentation can be as either leukemia or lymphoma. The major
clinical characteristics of B cell CLL/small lymphocytic lymphoma
are presented in Table 110–10.
• The diagnosis of typical B cell CLL is made when an increased
number of circulating lymphocytes (i.e., >4 x 109/L and usually
>10 x 109/L) is found (Fig. 110-6) that are monoclonal B cells
expressing the CD5 antigen. Finding bone marrow infiltration by
the same cells confirms the diagnosis.
• The peripheral blood smear in such patients typically shows
many "smudge" or "basket" cells, nuclear remnants of cells
damaged by the physical shear stress of making the blood
smear. If cytogenetic studies are performed, trisomy 12 is found
in 25–30% of patients.
• Abnormalities in chromosome 13 are also seen
TREATMENT: B CELL CHRONIC
LYMPHOID LEUKEMIA/SMALL
LYMPHOCYTIC LYMPHOMA
• Patients whose presentation is typical B cell CLL with no manifestations of the
disease other than bone marrow involvement and lymphocytosis (i.e., Rai
stage 0 and Binet stage A; Table 110–7) can be followed without specific
therapy for their malignancy. These patients have a median survival >10 years,
and some will never require therapy for this disorder. If the patient has an
adequate number of circulating normal blood cells and is asymptomatic,
many physicians would not initiate therapy for patients in the intermediate
stage of the disease manifested by lymphadenopathy and/or
hepatosplenomegaly. However, the median survival for these patients is 7
years, and most will require treatment in the first few years of follow-up.
• Patients who present with bone marrow failure (i.e., Rai stage III or IV or Binet
stage C) will require initial therapy in almost all cases. These patients have a
serious disorder with a median survival of only 1.5 years. It must be
remembered that immune manifestations of typical B cell CLL should be
managed independently of specific antileukemia therapy. For example,
glucocorticoid therapy for autoimmune cytopenias and globulin
replacement for patients with hypogammaglobulinemia should be used
whether or not antileukemia therapy is given.
• Patients who present primarily with lymphoma and have a low IPI score have
a 5-year survival of 75%, but those with a high IPI score have a 5-year survival
of <40% and are more likely to require early therapy.
• The most common treatments for patients with typical B
cell CLL/small lymphocytic lymphoma have been
chlorambucil or fludarabine, alone or in combination.
• Chlorambucil can be administered orally with few
immediate side effects, while fludarabine is administered IV
and is associated with significant immune suppression.
• However, fludarabine is by far the more active agent and is
the only drug associated with a significant incidence of
complete remission.
• The combination of rituximab (375–500 mg/m2 day 1),
fludarabine (25 mg/m2 days 2–4 on cycle 1 and 1–3 in
subsequent cycles), and cyclophosphamide (250 mg/m2
with fludarabine) achieves complete responses in 69% of
patients, and those responses are associated with
molecular remissions in half of the cases. Half the patients
experience grade III or IV neutropenia.
• For young patients presenting with leukemia requiring
therapy, regimens containing fludarabine are the
treatment of choice. Because fludarabine is an effective
second-line agent in patients with tumors unresponsive to
chlorambucil, the latter agent is often chosen in elderly
patients who require therapy.
DIFFUSE LARGE B CELL LYMPHOMA
• Diffuse large B cell lymphoma is the most common type of non-Hodgkin's
lymphoma, representing approximately one-third of all cases. This
lymphoma makes up the majority of cases in previous clinical trials of
"aggressive" or "intermediate-grade" lymphoma. Table 110–10 shows the
clinical characteristics of diffuse large B cell lymphoma.
• The diagnosis of diffuse large B cell lymphoma can be made accurately
by an expert hematopathologist. Cytogenetic and molecular genetic
studies are not necessary for diagnosis, but some evidence has
accumulated that patients whose tumors overexpress the BCL-2 protein
might be more likely to relapse than others. Patients with prominent
mediastinal involvement are sometimes diagnosed as a separate
subgroup having primary mediastinal diffuse large B cell lymphoma. This
latter group of patients has a younger median age (i.e., 37 years) and a
female predominance (66%). Subtypes of diffuse large B cell lymphoma,
including those with an immunoblastic subtype and tumors with extensive
fibrosis, are recognized by pathologists but do not appear to have
important independent prognostic significance.
Вам также может понравиться
- Overview of LymphomaДокумент42 страницыOverview of Lymphomaadamu mohammadОценок пока нет
- Chronic Lymphocytic LeukemiaОт EverandChronic Lymphocytic LeukemiaMichael HallekОценок пока нет
- Non Hodgkin LymphomaДокумент9 страницNon Hodgkin LymphomaAhmad SaifulОценок пока нет
- Lymphoma HerfindalДокумент56 страницLymphoma HerfindalAanshi ShahОценок пока нет
- Case StudyДокумент10 страницCase Studysabrown109Оценок пока нет
- LymphomaДокумент69 страницLymphomaDawit g/kidanОценок пока нет
- Lymphoma Shofik EDITED BY SAYAM 8.53PMДокумент35 страницLymphoma Shofik EDITED BY SAYAM 8.53PMRAGHU NATH KARMAKERОценок пока нет
- Leukemia Research Paper Thesis StatementДокумент9 страницLeukemia Research Paper Thesis Statementaparnaharrisonstamford100% (1)
- Non - Hodgkin LymphomaДокумент25 страницNon - Hodgkin LymphomaRo RyОценок пока нет
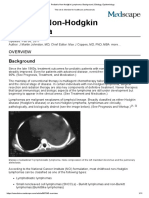
- Pediatric Non-Hodgkin Lymphoma - Background, Etiology, EpidemiologyДокумент11 страницPediatric Non-Hodgkin Lymphoma - Background, Etiology, EpidemiologytopОценок пока нет
- Acute Leukemia: Thirunavukkarasu MurugappanДокумент22 страницыAcute Leukemia: Thirunavukkarasu MurugappanFelix Allen100% (1)
- Acute Leukemia HerfindalДокумент35 страницAcute Leukemia HerfindalAanshi ShahОценок пока нет
- 1) Explain The Risk Factors For CLL, Including The Relevance of Monoclonal B Cell Lymphocytosis (MBL)Документ6 страниц1) Explain The Risk Factors For CLL, Including The Relevance of Monoclonal B Cell Lymphocytosis (MBL)Fahim MahmudОценок пока нет
- Pediatrik LeukemiasДокумент14 страницPediatrik LeukemiasLefrina GusrianiiОценок пока нет
- Non-Hodgkin's LymphomasДокумент23 страницыNon-Hodgkin's LymphomasshevmyrОценок пока нет
- Acute Myeloid Leukemia-BookДокумент15 страницAcute Myeloid Leukemia-BookRhoda Lom-ocОценок пока нет
- Acute Leukemia RodaksДокумент14 страницAcute Leukemia RodaksLoiLoiChanОценок пока нет
- Nk-Cell Lymphomas of The Head and Neck: AuthorДокумент8 страницNk-Cell Lymphomas of The Head and Neck: AuthorCharmila SariОценок пока нет
- Medicine Seminar Combined-1Документ30 страницMedicine Seminar Combined-1Deepanshu KumarОценок пока нет
- The Role of Immunophenotyping in The Diagnosis of Acute Leukemia. A Narrative Literature ReviewДокумент6 страницThe Role of Immunophenotyping in The Diagnosis of Acute Leukemia. A Narrative Literature ReviewmyhalfsmileОценок пока нет
- Acute Lymphoblastic LeukemiaДокумент80 страницAcute Lymphoblastic LeukemiaGizo YitayewОценок пока нет
- Childhood LeukemiaДокумент10 страницChildhood LeukemiafrancyriveraОценок пока нет
- Non-Hodgkin's Lymphoma: A Histopathologic and Prognostic EvaluationДокумент12 страницNon-Hodgkin's Lymphoma: A Histopathologic and Prognostic Evaluationchimbimb100% (2)
- Hodgkein and Nonhodgkein LymphomaДокумент57 страницHodgkein and Nonhodgkein Lymphomasamar yousif mohamedОценок пока нет
- Hutter2010 LeucemiaДокумент10 страницHutter2010 LeucemiasarabisimonaОценок пока нет
- Acuteleukemia: Hayley Rose-Inman,, Damon KuehlДокумент18 страницAcuteleukemia: Hayley Rose-Inman,, Damon KuehlJorge Tovar AvilaОценок пока нет
- L-3 Introduction To LeukemiaДокумент26 страницL-3 Introduction To LeukemiaAbood dot netОценок пока нет
- Wall 2016Документ15 страницWall 2016Jose AbadiaОценок пока нет
- Background: Pediatric Acute Lymphoblastic LeukemiaДокумент3 страницыBackground: Pediatric Acute Lymphoblastic LeukemiaNitin KumarОценок пока нет
- Acute Lymphoblastic LeukemiaДокумент30 страницAcute Lymphoblastic LeukemiaHarancang Kahayana0% (1)
- PATHO LEC WBC Lymph Nodes Spleen Thymus Part1 CompressedДокумент84 страницыPATHO LEC WBC Lymph Nodes Spleen Thymus Part1 CompressedAngelo HinonОценок пока нет
- Shan Shal 2012Документ15 страницShan Shal 2012Jose AbadiaОценок пока нет
- Leukemia Myeloproliferation, Myelodysplasia: Lita Septina Peyakit Dalam FK UMSUДокумент47 страницLeukemia Myeloproliferation, Myelodysplasia: Lita Septina Peyakit Dalam FK UMSUJr SparkОценок пока нет
- Blockxiv Neoplasms Lymphoid 2006Документ54 страницыBlockxiv Neoplasms Lymphoid 2006Ryo RyozОценок пока нет
- Childhood Malignancies - LeukaemiasДокумент4 страницыChildhood Malignancies - Leukaemiasvictortayor_26105009Оценок пока нет
- The Qualitative Estimation of BCR-ABL Transcript: An In-Lab Procedural Study on Leukemia PatientsОт EverandThe Qualitative Estimation of BCR-ABL Transcript: An In-Lab Procedural Study on Leukemia PatientsОценок пока нет
- Opeyemi IdaeworДокумент66 страницOpeyemi IdaeworOpeyemi IdaeworОценок пока нет
- Review of Related LiteratureДокумент11 страницReview of Related LiteratureJanОценок пока нет
- Hodgkin Lymphoma 2023 Update On Diagnosis, Risk-Stratification, and ManagementДокумент24 страницыHodgkin Lymphoma 2023 Update On Diagnosis, Risk-Stratification, and ManagementZuri100% (1)
- Chronic Lymphocytic Leukaemia: Key PointsДокумент5 страницChronic Lymphocytic Leukaemia: Key PointsJorge Tovar AvilaОценок пока нет
- Disorders of White Blood Cells and Lymphoid TissuesДокумент30 страницDisorders of White Blood Cells and Lymphoid Tissuesammar amerОценок пока нет
- Group 1 Apolonio, Leizel, R. Corpuz Rolyn Mañalac Joelle Anne Señeres Loui AnneДокумент33 страницыGroup 1 Apolonio, Leizel, R. Corpuz Rolyn Mañalac Joelle Anne Señeres Loui AnneLeizel ApolonioОценок пока нет
- LymphomasДокумент51 страницаLymphomasYousef IbrahimОценок пока нет
- Diseases and Tumors of Lymphoid SystemДокумент97 страницDiseases and Tumors of Lymphoid SystemamyОценок пока нет
- Thesis On Hodgkin LymphomaДокумент5 страницThesis On Hodgkin Lymphomafjm38xf3100% (2)
- An Sell 2005Документ11 страницAn Sell 2005Rachel AutranОценок пока нет
- Week 15-Mature-Lymphoid-Neoplasms-SCДокумент65 страницWeek 15-Mature-Lymphoid-Neoplasms-SCKyle CollladoОценок пока нет
- Hodgkin's DiseaseДокумент11 страницHodgkin's DiseaseReiswandhika Intan PermatasariОценок пока нет
- Acute Leukaemias Lecture-1Документ39 страницAcute Leukaemias Lecture-1MarvellousОценок пока нет
- Clinical Presentation, Pathologic Features, Diagnosis, and Differential Diagnosis of Chronic Lymphocytic Leukemia - UpToDateДокумент23 страницыClinical Presentation, Pathologic Features, Diagnosis, and Differential Diagnosis of Chronic Lymphocytic Leukemia - UpToDateJosé Martínez100% (1)
- LLC 2006Документ11 страницLLC 2006claudia8a_ulamedОценок пока нет
- Paediatric Acute Lymphoblastic LeukemiaДокумент49 страницPaediatric Acute Lymphoblastic LeukemiaKishoreChandraKoradaОценок пока нет
- Fast Facts: Blastic Plasmacytoid Dendritic Cell Neoplasm: Shedding light on a rare diseaseОт EverandFast Facts: Blastic Plasmacytoid Dendritic Cell Neoplasm: Shedding light on a rare diseaseОценок пока нет
- Reviews: Chronic Lymphocytic Leukaemia: From Genetics To TreatmentДокумент18 страницReviews: Chronic Lymphocytic Leukaemia: From Genetics To Treatmentlengers poworОценок пока нет
- Bosch2019 PDFДокумент18 страницBosch2019 PDFlengers poworОценок пока нет
- Leukaemia Lecture 01 - Aml - DRДокумент69 страницLeukaemia Lecture 01 - Aml - DRapi-273068056100% (1)
- Acute Lymphoblastic LeukemiaДокумент34 страницыAcute Lymphoblastic LeukemiamtyboyОценок пока нет
- K3. Penatalaksanaan Kasus Neurologi Di FKTP - Dr. Achmad Faqih, SP.SДокумент30 страницK3. Penatalaksanaan Kasus Neurologi Di FKTP - Dr. Achmad Faqih, SP.SLia pramitaОценок пока нет
- 388tetanus For Website PDFДокумент52 страницы388tetanus For Website PDFLia pramitaОценок пока нет
- Time Table-1-1Документ3 страницыTime Table-1-1Lia pramitaОценок пока нет
- Jadwal 1 Februari FixДокумент4 страницыJadwal 1 Februari FixLia pramitaОценок пока нет
- K28. Malpraktek - Dr. Monang, SP.FДокумент18 страницK28. Malpraktek - Dr. Monang, SP.FLia pramitaОценок пока нет
- Journal AppraisalДокумент1 страницаJournal AppraisalNur Vicka VickaОценок пока нет
- ESC Guidelines For DX and TX of Acute and Chronic HF (2016)Документ85 страницESC Guidelines For DX and TX of Acute and Chronic HF (2016)Imja94Оценок пока нет
- Ehz 467Документ65 страницEhz 467Coy Calapatia-TorresОценок пока нет
- K20. DNA Forensik - Dr. Virhan, M.BiomedДокумент20 страницK20. DNA Forensik - Dr. Virhan, M.BiomedLia pramitaОценок пока нет
- Prevention Guidelines Made SimpleДокумент17 страницPrevention Guidelines Made SimplearseniosilvaОценок пока нет
- Lung Abscess: DR Budi Enoch SPPDДокумент14 страницLung Abscess: DR Budi Enoch SPPDLia pramitaОценок пока нет
- Systrmic Lupus Erythematosus (Sle)Документ62 страницыSystrmic Lupus Erythematosus (Sle)Dedy Santoso ChouОценок пока нет
- Steno Ciii StenoДокумент21 страницаSteno Ciii StenoLia pramitaОценок пока нет
- Atherosklerosis: DR Budi Enoch SPPDДокумент56 страницAtherosklerosis: DR Budi Enoch SPPDLia pramitaОценок пока нет
- Myeloid LeukemiaДокумент36 страницMyeloid LeukemiaLia pramitaОценок пока нет
- ReferatДокумент53 страницыReferatLia pramitaОценок пока нет
- Gout and Othercrystal-Associated ArthropathiesДокумент31 страницаGout and Othercrystal-Associated ArthropathiesLia pramitaОценок пока нет
- Systemic Lupus Erythematosus (SLE)Документ62 страницыSystemic Lupus Erythematosus (SLE)Lia pramitaОценок пока нет
- Atherosklerosis: DR Budi Enoch SPPDДокумент56 страницAtherosklerosis: DR Budi Enoch SPPDLia pramitaОценок пока нет
- Coagulation DisordersДокумент26 страницCoagulation DisordersLia pramita0% (1)
- Hemoglobinopathy Dan Sindroma ThalasemiaДокумент62 страницыHemoglobinopathy Dan Sindroma ThalasemiaLia pramitaОценок пока нет
- Coagulation DisordersДокумент26 страницCoagulation DisordersLia pramitaОценок пока нет
- Periarticular Disorders of The ExtremitiesДокумент20 страницPeriarticular Disorders of The ExtremitiesLia pramitaОценок пока нет
- Gout and Othercrystal-Associated ArthropathiesДокумент31 страницаGout and Othercrystal-Associated ArthropathiesLia pramitaОценок пока нет
- 5 Pain Management in The Elderly PopulationДокумент26 страниц5 Pain Management in The Elderly PopulationLia pramitaОценок пока нет
- Gout and Othercrystal-Associated ArthropathiesДокумент31 страницаGout and Othercrystal-Associated ArthropathiesLia pramitaОценок пока нет
- 4 Palliative CareДокумент35 страниц4 Palliative CareLia pramitaОценок пока нет
- Glucose and Dementia - Geriatri JurnalДокумент20 страницGlucose and Dementia - Geriatri JurnalLia pramitaОценок пока нет
- Geriatric Medicine KuliahДокумент38 страницGeriatric Medicine KuliahLia pramitaОценок пока нет
- AsthmaICS PDFДокумент7 страницAsthmaICS PDFCARES Martin Federic PalcoОценок пока нет
- Procedures in OBGДокумент8 страницProcedures in OBGKanak Soni100% (1)
- Modul Praktikum Patologi Anatomi Fakultas Kedokteran Universitas Muhammadiyah Palembang Tahun 2015Документ23 страницыModul Praktikum Patologi Anatomi Fakultas Kedokteran Universitas Muhammadiyah Palembang Tahun 2015TasyaОценок пока нет
- DataДокумент207 страницDatamikhael muaneoОценок пока нет
- Assessment, Traumatic Grief, TahomaДокумент3 страницыAssessment, Traumatic Grief, TahomaJesus Carrillo Raymond100% (2)
- Sample Questions 2Документ6 страницSample Questions 2Filipino Nurses CentralОценок пока нет
- Bowel Nosode MatrixДокумент3 страницыBowel Nosode MatrixAndrea Middleton92% (13)
- Hiking and TrekkingДокумент11 страницHiking and TrekkingDavidОценок пока нет
- 5 - Cell Division - Notes 1Документ68 страниц5 - Cell Division - Notes 1Cole HarrisОценок пока нет
- Abstracts 8th Congress CSMBLM Rijeka Korekcija N.nikolac 5.11.2015. BO2Документ101 страницаAbstracts 8th Congress CSMBLM Rijeka Korekcija N.nikolac 5.11.2015. BO2BoyITBОценок пока нет
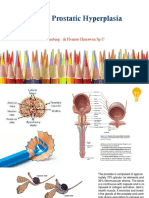
- Benign Prostatic Hyperplasia: Pembimbing: DR Herinto Himawan Sp.UДокумент42 страницыBenign Prostatic Hyperplasia: Pembimbing: DR Herinto Himawan Sp.Uilma aulia zahraОценок пока нет
- Dentassure Gano Toothpaste Launch PDFДокумент14 страницDentassure Gano Toothpaste Launch PDFnitesh sharma100% (1)
- Surgical Endoscopy Journal 1Документ86 страницSurgical Endoscopy Journal 1Saibo BoldsaikhanОценок пока нет
- Worry More Live Longer American English Student Ver2 BWДокумент5 страницWorry More Live Longer American English Student Ver2 BWLanting LeeОценок пока нет
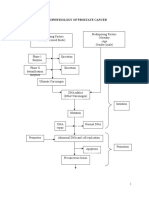
- Pathophysiology of Prostate CancerДокумент3 страницыPathophysiology of Prostate Cancermkho100% (1)
- Nej Mo A 1905287Документ12 страницNej Mo A 1905287Ari KurniawanОценок пока нет
- Opioid-Induced Androgen Deficiency in Males (OPIAD Syndrome) : Medicinski Casopis January 2015Документ7 страницOpioid-Induced Androgen Deficiency in Males (OPIAD Syndrome) : Medicinski Casopis January 2015Lilamala LilavelikaОценок пока нет
- Periodontal Risk Assessment, Diagnosis and Treatment PlanningДокумент22 страницыPeriodontal Risk Assessment, Diagnosis and Treatment PlanningHenry E. CoaquiraОценок пока нет
- KalojiraДокумент2 страницыKalojiralutfurrahman35Оценок пока нет
- Material Safety Data Sheet: 1. Chemical Product and Company IdentificationДокумент7 страницMaterial Safety Data Sheet: 1. Chemical Product and Company IdentificationKun Adi ReksatamaОценок пока нет
- PMP Pancreas 2014Документ5 страницPMP Pancreas 2014Lyna PangaribuanОценок пока нет
- Chapter 6 - Inflammation, Tissue Repair & FeverДокумент8 страницChapter 6 - Inflammation, Tissue Repair & FeverChrista CastorОценок пока нет
- GuidelinesДокумент4 страницыGuidelinesChidambaram SeevakanОценок пока нет
- HDFC Life Click 2 Protect Life - Product Brochure PDFДокумент24 страницыHDFC Life Click 2 Protect Life - Product Brochure PDFvaibhav kumar KhokharОценок пока нет
- BIOGENДокумент71 страницаBIOGENPamela GabrielОценок пока нет
- UPTODATE - MIOMA - Epidemiology, Clinical Manifestations, Diagnosis, and Natural History of Uterine Leiomyomas (Fibroids)Документ20 страницUPTODATE - MIOMA - Epidemiology, Clinical Manifestations, Diagnosis, and Natural History of Uterine Leiomyomas (Fibroids)Gaby FloresОценок пока нет
- Functions of The Respiratory PassagewaysДокумент2 страницыFunctions of The Respiratory PassagewaysAdnin ShereenОценок пока нет
- Functional Dyspepsia: Recent Advances in Pathophysiology: Update ArticleДокумент5 страницFunctional Dyspepsia: Recent Advances in Pathophysiology: Update ArticleDen BollongОценок пока нет
- Building An NCD-ready Workforce: Technical Meeting ReportДокумент48 страницBuilding An NCD-ready Workforce: Technical Meeting ReportnavenОценок пока нет
- GYNE 9 1 Breast Diseases PDFДокумент19 страницGYNE 9 1 Breast Diseases PDFColeen NeyraОценок пока нет