Академический Документы
Профессиональный Документы
Культура Документы
2 Warthin's Tumor
Загружено:
fado0 оценок0% нашли этот документ полезным (0 голосов)
36 просмотров21 страницаpathology
Авторское право
© © All Rights Reserved
Доступные форматы
PPTX, PDF, TXT или читайте онлайн в Scribd
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документpathology
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
0 оценок0% нашли этот документ полезным (0 голосов)
36 просмотров21 страница2 Warthin's Tumor
Загружено:
fadopathology
Авторское право:
© All Rights Reserved
Доступные форматы
Скачайте в формате PPTX, PDF, TXT или читайте онлайн в Scribd
Вы находитесь на странице: 1из 21
Warthin's Tumor
Warthin�s Tumor (WT) has also been referred to as
cystadenolymphoma, adenolymphoma, and papillary
cystadenoma lymphomatosum.
It is the second most common benign salivary gland
tumor after pleomorphic adenoma. It accounts for 5% to
6% of all neoplasms of salivary glands and up to 12% of
benign parotid tumors.
WT occurs in 3rd to 7th decades of life with a slight male
predominance. Risk factors include smoking (8-fold
higher risk than non-smokers) and radiation exposure.
WT predominantly involves the parotid gland and
presents as a painless mass. Rare cases involving the
submandibular gland and minor salivary glands have been
reported.
Bilateral and multifocal WT are not uncommon. This
gross image of a WT shows solid and cystic components.
The pearly white nodules in the cyst wall are hyperplastic
lymphoid follicles covered by oncocytic epithelium.
Fine needle aspiration of Warthin�s tumor
shows cohesive sheets and clusters of
epithelial cells with oncocytic
features and background of lymphocytes (as
seen here; Diff-Quik stain).
The oncocytic cells are characterized by abundant
granular eosinophilic cytoplasm and round
centrally located nuclei.
The background may show mucus or thick fluid associated
with lymphoid cells.
Fine needle aspirate (FNA) smear of a Warthin�s tumor
(WT) showing cohesive sheets and clusters of oncocytic
cells arranged in a honeycomb pattern.
The background usually shows scattered lymphocytes,
although they are not seen in this image (PAP stain).
Prior manipulation or FNA can cause secondary
changes in WT.
They include cytologic atypia, metaplasia (squamous and
mucous), hemorrhage, infarction, necrosis, acute and
chronic inflammation, fibrosis, granulation tissue formation
and changes of pseudoinvasion.
Grossly Warthin�s tumor (WT) ranges in size from 1.0
� 8.0 cm and has smooth encapsulated outer
surface.
The cut surface is usually shows solid and cystic
areas filled with mucoid, brown material.
The cystic areas may demonstrate papillary
projections.
This low power view of WT shows papillary structures
lined by oncocytic epithelium (left side) and dense
lymphocytic infiltrate with germinal center
formation (right side).
Warthin�s tumor (WT) has a distinct morphologic
appearance composed of papillary structures lined
by bi-layered oncocytic
epithelium forming cystic spaces and the stroma
with lymphoid component (as seen in this low
power micrograph).
Other inflammatory cells such as plasma cells, mast
cells, histiocytes and giant cells can be seen.
Mucous cells and sebaceous glands can also be
seen and their presence may raise the possibility of
mucoepidermoid carcinoma.
This low power micrograph shows Warthin�s Tumor
composed of papillary and tubular
structures lined by bi-layered oncocytic
epithelium and the dense lymphocytic
infiltrate with prominent germinal center
formation.
The eosinophilic granular appearance of the
cytoplasm of oncocytic cells is due to abundant
mitochondriawhich can be demonstrated
by phosohotungstic acid-hematoxylin
stain (PTAH stain; appear as blue-black cytoplasmic
granules).
The epithelial component of Warthin�s tumor
is cytokeratin positive (CK7, 8, 18, and 19) and
the lymphoid stroma consists predominantly of IgA-
producing polyclonal B-cells with a few T-cells,
mast cells, and S-100-positive dendritic cells.
This high magnification view of the previous image shows
dense lymphocytic infiltrate with prominent germinal
center formation.
The epithelial component consists of tubular and papillary
structures lined by bi-layered epithelium composed of tall
columnar luminal cell layer and cuboidal oncocytic cells on
outer side.
High power view of Warthin�s tumor showing papillary
structures lined by bi-layered oncocytic
epitheliumcomposed of tall columnar luminal
cell layer and a discontinuous layer of basally
locatedcuboidal cells.
The stroma shows dense lymphocytic
infiltrate with germinal center formation.
The cystic spaces are filled with eosinophilic granular
material.
Higher magnification image of Warthin�s tumor
demonstrates papillary structures lined by bi-
layered epithelium.
The inner layer (basally located) is discontinuous and
composed cuboidal cells with eosinophilic granular
cytoplasm and vesicular round nuclei.
The columnar cells are located on the luminal aspect. The
stroma is well demarcated and composed of benign
lymphocytic infiltrate.
Warthin�s tumor (WT) is believed to develop
from neoplastic transformation of salivary
duct epithelium that is entrapped in intra-
parotid lymph nodes during embryonic
development.
The presence of subcapsular sinuses in some cases of
WT, the occurrence of WT in periparotid lymph nodes, and
the presence of B- and T-cells in the lymphoid component
of WT appear to support this theory.
This high power image of WT shows bi-layered oncocytic
epithelium and the stroma composed of dense
lymphocytic infiltrate with prominent germinal center
formation.
This image of Warthin�s Tumor shows tubular structures
composed of bi-layered oncocytic epithelium surrounded
by stroma with dense lymphocytic infiltrate.
The diagnosis of Warthin�s tumor (WT) is straight-
forward in most cases.
Cases with a predominant oncocytic cell component may
raise suspicion for oncocytoma, mucoepidermoid
carcinoma, oncocytosis or acinic cell
carcinoma.
When squamous and mucinous cell metaplasia is present
in WT, its distinction from mucoepidermoid carcinoma may
be challenging.
Mucoepidermoid carcinomas often
carry translocations
t(11;19) and t(11;15)resulting in CRTC1-
MAML2 and CRTC3-MAML2 fusion genes � a
finding not seen in Warthin�s tumor.
This image shows classic appearance of Warthin�s
tumor with oncocytic epithelium arranged in tubules and
nests with associated lymphoid infiltrate.
Higher magnification image of Warthin�s tumor showing
oncocytic cells with eosinophilic granular cytoplasm and
vesicular round nuclei with prominent nucleoli.
The background shows benign lymphocytes and a few
plasma cells.
The tumor has multicystic appearance here
with oncocytic epithelium lining fluid-filled
spaces.
The cystic areas may contain cholesterol crystals,
cellular debris, or laminated bodies.
The lymphoid stroma is deficient in this focus.
Complete surgical excision with adequate surgical
margins is usually curative.
Local recurrence may follow an incomplete excision of
Warthin�s tumor.
Malignant transformation is seen in less than
0.1% cases and can occur in either epithelial
component (squamous cell carcinoma, oncocytic
carcinoma, adenocarcinoma NOS, mucoepidermoid
carcinoma) or lymphoid component (Non-Hodgkin�s
lymphoma).
The image shows papillary structures lined by bi-layered
oncocytic epithelium and enclosing scant amount of
lymphocytic infiltrate.
Higher magnification image of the previous image showing
papillary structures lined by bi-layered oncocytic
epithelium and enclosing scant amount of lymphocytic
infiltrate.
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- A Clinician's Guide To Gender-Affirming Care Working With Transgender and Gender Nonconforming Clients by Sand C. Chang PHD 2018 PDFДокумент314 страницA Clinician's Guide To Gender-Affirming Care Working With Transgender and Gender Nonconforming Clients by Sand C. Chang PHD 2018 PDFmaquis87100% (6)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Miller Trailblazer 280 NT ManualДокумент50 страницMiller Trailblazer 280 NT ManualGary Condict67% (3)
- 15-Item DMSES UKДокумент2 страницы15-Item DMSES UKkumalaselvia49Оценок пока нет
- Pathology of Breast CancerДокумент22 страницыPathology of Breast CancerfadoОценок пока нет
- RCPCH Progress Level 1 Paediatrics and Child Health CurriculumДокумент16 страницRCPCH Progress Level 1 Paediatrics and Child Health CurriculumSabera KapasiОценок пока нет
- FNA Soft TX TuДокумент74 страницыFNA Soft TX TufadoОценок пока нет
- ThyroidДокумент102 страницыThyroidfadoОценок пока нет
- Tissue Pathways For Breast Pathology: September 2010Документ9 страницTissue Pathways For Breast Pathology: September 2010fadoОценок пока нет
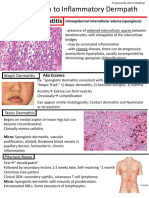
- Spongiotic Dermatitis: Aka EczemaДокумент8 страницSpongiotic Dermatitis: Aka EczemafadoОценок пока нет
- Breast: Kurt'S NotesДокумент4 страницыBreast: Kurt'S NotesfadoОценок пока нет
- Thyroid AspirationДокумент23 страницыThyroid AspirationfadoОценок пока нет
- Pancreas: Kurt'S NotesДокумент3 страницыPancreas: Kurt'S NotesfadoОценок пока нет
- Benign and Malignant Lesions in Respiratory CytologyДокумент43 страницыBenign and Malignant Lesions in Respiratory CytologyfadoОценок пока нет
- Actinic Keratosis: (Aka Bowen's Disease)Документ5 страницActinic Keratosis: (Aka Bowen's Disease)fadoОценок пока нет
- Presentation by - Dr. Monika NemaДокумент118 страницPresentation by - Dr. Monika NemafadoОценок пока нет
- Pap Smear: Dr. Monika NemaДокумент114 страницPap Smear: Dr. Monika NemafadoОценок пока нет
- Small Intestine 01 PDFДокумент9 страницSmall Intestine 01 PDFfadoОценок пока нет
- Dermatofibroma: Aka Benign Fibrous HistiocytomaДокумент4 страницыDermatofibroma: Aka Benign Fibrous HistiocytomafadoОценок пока нет
- Cytopathology of Cerebrospinal FluidДокумент44 страницыCytopathology of Cerebrospinal FluidfadoОценок пока нет
- 1 Soft TissueДокумент41 страница1 Soft TissuefadoОценок пока нет
- Myxoid STTДокумент37 страницMyxoid STTfadoОценок пока нет
- Non Gynae CytologyДокумент32 страницыNon Gynae CytologyfadoОценок пока нет
- CytologyДокумент7 страницCytologyfadoОценок пока нет
- Pathology 2 PDFДокумент18 страницPathology 2 PDFfadoОценок пока нет
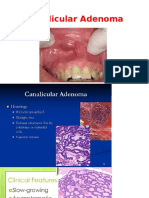
- 4 Canalicular AdenomaДокумент9 страниц4 Canalicular AdenomafadoОценок пока нет
- GyncomastiaДокумент3 страницыGyncomastiafadoОценок пока нет
- Pathology 5 B PDFДокумент14 страницPathology 5 B PDFfadoОценок пока нет
- Heat Stress CardДокумент2 страницыHeat Stress CardAshish TelangОценок пока нет
- Maternal Mortality Rates Report For 2022Документ5 страницMaternal Mortality Rates Report For 2022ABC Action NewsОценок пока нет
- Tubal Patency TestДокумент3 страницыTubal Patency TestLovely SarangiОценок пока нет
- Effect of Liquid Smoke As An Ingredient in FrankfuДокумент11 страницEffect of Liquid Smoke As An Ingredient in FrankfuLuciano EscobarОценок пока нет
- Total Solids and Total Dissolved Solids in WaterДокумент14 страницTotal Solids and Total Dissolved Solids in WaterGeorge Ataher100% (1)
- Msds AntracolДокумент9 страницMsds AntracolLidya Nathalia Patandung100% (1)
- Internship ReportДокумент52 страницыInternship ReportVaidurya KeerthiОценок пока нет
- 02 CY 2023 Query of PDMPДокумент3 страницы02 CY 2023 Query of PDMPPartha Sarathi DasОценок пока нет
- Homeopathic Facial Analysis Grant Bentley.03455 1contentsДокумент7 страницHomeopathic Facial Analysis Grant Bentley.03455 1contentsab moonОценок пока нет
- Jha - Dismantle Scaffolding Activity and Housekeeping Scaffolding MaterialДокумент13 страницJha - Dismantle Scaffolding Activity and Housekeeping Scaffolding MaterialAliff ApamОценок пока нет
- Bed MakingДокумент36 страницBed MakingGlaiza Mae TuralbaОценок пока нет
- Attitudes of Young Adults Towards MarriageДокумент12 страницAttitudes of Young Adults Towards MarriageMehzabin DishaОценок пока нет
- Teacher-Made-Test BEVДокумент3 страницыTeacher-Made-Test BEVMaureen Madriaga100% (1)
- Epos Hip UltrasoundДокумент20 страницEpos Hip UltrasoundBogdan Popescu100% (1)
- Potencial Uso de Ivermectina en Tratamiento y Profilaxis de Covid19Документ18 страницPotencial Uso de Ivermectina en Tratamiento y Profilaxis de Covid19Andrimar Del Carmen Torres MuñozОценок пока нет
- Respiratory System QuizДокумент2 страницыRespiratory System Quizapi-281108263100% (1)
- BEAUTY-CARE-9 Q1 W7 Mod7Документ14 страницBEAUTY-CARE-9 Q1 W7 Mod7Kc PitacioОценок пока нет
- Idexx Sdma Test Algorithm PDFДокумент2 страницыIdexx Sdma Test Algorithm PDFblueice999Оценок пока нет
- Kelompok 1Документ22 страницыKelompok 1teguhОценок пока нет
- 173 301 1 SM PDFДокумент7 страниц173 301 1 SM PDFAnggista MayangОценок пока нет
- Who Are Eligible For This Exam?: Where Can I Book/register For Examination?Документ4 страницыWho Are Eligible For This Exam?: Where Can I Book/register For Examination?Bhargav Krsna GayanОценок пока нет
- Antiseptics & DisinfectantsДокумент53 страницыAntiseptics & DisinfectantselanthamizhmaranОценок пока нет
- Fix 4Документ20 страницFix 4asep bensinОценок пока нет
- Kode Barang Nama Barang Qty Sat3 Qty Sat2 Sat Jual Unit Sat JL Unit Sat3 Unit Sat2Документ34 страницыKode Barang Nama Barang Qty Sat3 Qty Sat2 Sat Jual Unit Sat JL Unit Sat3 Unit Sat2Gigih Kenanga SariОценок пока нет
- Grade 9 - Health - LC 3Документ6 страницGrade 9 - Health - LC 3Leah Casano100% (1)
- Health Risk Assessment: Practical Steps To Conduct HraДокумент14 страницHealth Risk Assessment: Practical Steps To Conduct HraPris RodriguezОценок пока нет