Академический Документы
Профессиональный Документы
Культура Документы
Congenital Heart Disease
Загружено:
Ethan Marcos GoИсходное описание:
Авторское право
Доступные форматы
Поделиться этим документом
Поделиться или встроить документ
Этот документ был вам полезен?
Это неприемлемый материал?
Пожаловаться на этот документАвторское право:
Доступные форматы
Congenital Heart Disease
Загружено:
Ethan Marcos GoАвторское право:
Доступные форматы
CONGENITAL HEART DISEASE
Prepared by:
Genorga, Christian Marcos NCF-LBSN2A
CONGENITAL HEART DISEASE
Congenital heart defects are abnormalities in the heart's structure that are present at birth. -defect in the structure of the heart and great vessels. -Happens because of incomplete or abnormal development of the fetus' heart during the very early weeks of pregnancy. Some are known to be associated with genetic disorders, such as Down syndrome, but the cause of most congenital heart defects is unknown. -While they can't be prevented, there are many treatments for the defects and any related health problems. -Approximately 8 out of every 1,000 newborns have congenital heart defects, ranging from mild to severe.
How a Healthy Heart Works
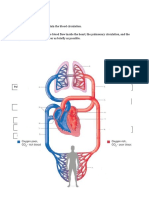
The heart, lungs, and blood vessels make up the circulatory system of the human body. The heart is the central pump of the circulatory system, and consists of four chambers the left atrium and left ventricle and the right atrium and right ventricle.
The heart also has four valves that direct the flow of blood through the heart:
The left atrium of the heart receives oxygen-rich blood from the lungs and then empties into the left ventricle through the mitral valve.
The left ventricle pumps oxygen-rich blood out to the rest of the body. Blood leaves the left ventricle through the aortic valve and enters the aorta, the largest artery (a blood vessel that carries oxygenated blood) in the body. Blood then flows from the aorta into the branches of many smaller arteries, providing the body's organs and tissues with the oxygen and nutrients they need.
After oxygen in the blood is released to the tissues, the now deoxygenated (oxygenpoor) blood returns to the heart through veins, the blood vessels that carry deoxygenated blood. This blood, which appears blue, enters the right atrium of the heart and then travels across the tricuspid valve into the right ventricle.
The right ventricle then pumps deoxygenated blood through the pulmonic valve into the lungs. The oxygen in the air we breathe binds to cells within this blood that is being pumped through the lungs. The oxygen-rich blood, which appears red, then returns to the left atrium and enters the left ventricle, where it is pumped out to the body once again.
This is the normal pathway that blood travels through the heart and the body. However, abnormalities in the heart's structure such as congenital heart defects can affect its ability to function properly.
CONGENITAL HEART DISEASE
Related Factors:
1.Increased or decreased ventricular filling (preload) 2.Alteration in afterload 3.Impaired contractility 4.Alteration in heart rate, rhythm, and conduction 5.Decreased oxygenation 6.Cardiac muscle disease
Types: CONGENITAL HEART DISEASE
1.Aortic Stenosis
2.Atrial Septal Defect (ASD) 3.Atrioventricular Canal Defect 4.Coarctation of the Aorta (COA) 5. Hypoplastic Left Heart Syndrome 6. Patent Ductus Arteriosus (PDA) 7. Pulmonary Atresia
8.Pulmonary Stenosis 9. Tetralogy of Fallot (TOF) 10. Total Anomalous Pulmonary Venous Connection 11. Transposition of the Great Arteries
Types: CONGENITAL HEART DISEASE
Aortic Stenosis
In aortic stenosis, the aortic valve is stiffened and has a narrowed opening (a condition called stenosis). It does not open properly, which increases strain on the heart because the left ventricle has to pump harder to send blood out to the body. Sometimes the aortic valve also does not close properly, causing it to leak, a condition called aortic regurgitation.
Atrial Septal Defect (ASD)
ASD is a hole in the wall (called the septum) that separates the left atrium and the right atrium.
Atrioventricular Canal Defect
This defect also known as endocardial cushion defect or atrioventricular septal defect is caused by a poorly formed central area of the heart. Typically there is a large hole between the upper chambers of the heart (the atria) and, often, an additional hole between the lower chambers of the heart (the ventricles). Instead of two separate valves allowing flow into the heart (tricuspid on the right and mitral valve on the left), there is one large common valve, which may be quite malformed. Atrioventricular canal defect is commonly seen in children with Down syndrome.
Types: CONGENITAL HEART DISEASE
Coarctation of the Aorta (COA)
COA is a narrowing of a portion of the aorta, and often seriously decreases the blood flow from the heart out to the lower portion of the body.
Hypoplastic Left Heart Syndrome
When the structures of the left side of the heart (the left ventricle, the mitral valve, and the aortic valve) are underdeveloped, they're unable to pump blood adequately to the entire body. This condition is usually diagnosed within the first few days of life, at which point the baby may be critically ill. Fortunately, many of these infants are recognized to have serious heart disease even before birth on ultrasound tests. A fetal echocardiogram is a specialized ultrasound that allows doctors to see the baby's heart in great detail and plan the best care for the baby while still in utero.
Types: CONGENITAL HEART DISEASE
Patent Ductus Arteriosus (PDA)
The ductus arteriosus (DA) is a normal blood vessel in the developing fetus that diverts circulation away from the lungs and sends it directly to the body. (The lungs are not used while the unborn fetus is in amniotic fluid the fetus gets oxygen directly from the mother's placenta.) The DA usually closes on its own shortly after birth; it is no longer needed once a newborn breathes on his own. If the DA doesn't close, then a condition called patent ductus arteriosus (PDA) results, which can result in too much blood flow to a newborn's lungs. PDA is common in premature babies.
Pulmonary Atresia
In this defect the pulmonic valve does not open at all and may indeed be completely absent. The main blood vessel that runs between the right ventricle and the lungs also may be malformed and the right ventricle can be abnormally small.
Pulmonary Stenosis
In pulmonary stenosis, the pulmonic valve is stiffened and has a narrowed opening (a condition called stenosis). It does not open properly, which increases strain on the right side of the heart because the right ventricle has to pump harder to send blood out to the lungs.
Types: CONGENITAL HEART DISEASE
Tetralogy of Fallot (TOF)
Tetralogy of Fallot is actually a combination of four heart defects. It includes pulmonary stenosis, a thickened right ventricle (known as ventricular hypertrophy), a hole between the lower chambers (known as a ventricular septal defect), and an aorta that can receive blood from both the left and right ventricles, instead of draining just the left. Because deoxygenated (blue) blood can flow out to the body, children with this defect often appear bluish.
Total Anomalous Pulmonary Venous Connection
The pulmonary veins normally are the blood vessels that deliver oxygenated blood from the lungs to the left atrium. Sometimes these vessels don't join the left atrium during development. Instead they deliver blood to the heart by other pathways, which may be narrowed. Pressure builds up in this pathway and in the pulmonary veins, pushing fluid into the lungs, decreasing the amount of oxygenated blood that reaches the body. These infants often have difficulty breathing and appear bluish.
Types: CONGENITAL HEART DISEASE
Transposition of the Great Arteries
In this condition, the pulmonary artery and the aorta (the major blood vessels leaving the heart) are switched so that the aorta arises from the right side of the heart and receives blue blood, which is sent right back out to the body without becoming oxygen-rich. The pulmonary artery arises from the left side of the heart, receives red blood and sends it back to the lungs again. The result is that babies with this condition often appear very blue and have low oxygen levels in the bloodstream. They usually come to medical attention within the first days of life.
Tricuspid Atresia
Blood normally flows from the right atrium to the right ventricle through the tricuspid valve. In tricuspid atresia, the valve is replaced by a plate or membrane that does not open. The right ventricle therefore does not receive blood normally and is often small.
Types: CONGENITAL HEART DISEASE
Truncus Arteriosus
In an embryo, the aorta and the pulmonary artery are initially a single vessel. During normal development, that vessel splits to form the two major arteries. If that split does not occur, the child is born with a single common great blood vessel called the truncus arteriosus. There is usually a hole between the ventricles associated with this defect.
Ventricular Septal Defect (VSD)
One of the most common congenital heart defects, VSD is a hole in the wall (septum) between the heart's left and right ventricles. These can occur at different locations and vary in size from very small to very large. Some of the smaller defects may gradually close on their own.
Signs and Symptoms of Heart Defects
Because congenital defects often compromise the heart's ability to pump blood and to deliver oxygen to the tissues of the body, they often produce telltale signs such as:
a bluish tinge or color (cyanosis) to the lips, tongue and/or nailbeds an increased rate of breathing or difficulty breathing poor appetite or difficulty feeding (which may be associated with color change) failure to thrive (failure to gain weight or weight loss) abnormal heart murmur sweating, especially during feedings diminished strength of the baby's pulse
Diagnosing a Heart Defect
An electrocardiogram (EKG) Echocardiogram Cardiac catheterization
CONGENITAL HEART DISEASE
Ongoing Assessment
* Assess mentation.--Restlessness is noted in the early stages; severe anxiety and confusion are seen in later stages. * Assess heart rate and blood pressure.--Sinus tachycardia and increased arterial blood pressure are seen in the early stages; BP drops as the condition deteriorates. Elderly patients have reduced response to catecholamines, thus their response to reduced cardiac output may be blunted, with less rise in heart rate. Pulsus alternans (alternating strongthen-weak pulse) is often seen in heart failure patients. * Assess skin color and temperature.--Cold, clammy skin is secondary to compensatory increase in sympathetic nervous system stimulation and low cardiac output and desaturation. * Assess peripheral pulses.--Pulses are weak with reduced cardiac output.
CONGENITAL HEART DISEASE
Ongoing Assessment: (cont.)
* Assess fluid balance and weight gain.--Compromised regulatory mechanisms may result in fluid and sodium retention. Body weight is a more sensitive indicator of fluid or sodium retention than intake and output. * Assess heart sounds, noting gallops, S3, S4.--S3 denotes reduced left ventricular ejection and is a classic sign of left ventricular failure. S4 occurs with reduced compliance of the left ventricle, which impairs diastolic filling. * Assess lung sounds. Determine any occurrence of paroxysmal nocturnal dyspnea (PND) or orthopnea.--Crackles reflect accumulation of fluid secondary to impaired left ventricular emptying. They are more evident in the dependent areas of the lung. Orthopnea is difficulty breathing when supine. PND is difficulty breathing that occurs at night. * Monitor continuous ECG as appropriate.
CONGENITAL HEART DISEASE
Ongoing Assessment: (cont.)
* Monitor ECG for rate; rhythm; ectopy; and change in PR, QRS, and QT intervals.--Tachycardia, bradycardia, and ectopic beats can compromise cardiac output. Elderly patients are especially sensitive to the loss of atrial kick in atrial fibrillation. * Assess response to increased activity.--Physical activity increases the demands placed on the heart; fatigue and exertional dyspnea are common problems with low cardiac output states. Close monitoring of patients response serves as a guide for optimal progression of activity. * Assess urine output. Determine how often the patient urinates.-Oliguria can reflect decreased renal perfusion. Diuresis is expected with diuretic therapy. * Assess for chest pain.--This indicates an imbalance between oxygen supply and demand. * Assess contributing factors so appropriate plan of care can be initiated.
CONGENITAL HEART DISEASE
Therapeutic Interventions
* Administer medication as prescribed, noting response and watching for side effects and toxicity. Clarify with physician parameters for withholding medications.--Depending on etiological factors, common medications include digitalis therapy, diuretics, vasodilator therapy, antidysrhythmics, ACE inhibitors, and inotropic agents. * Maintain optimal fluid balance. For patients with decreased preload, administer fluid challenge as prescribed, closely monitoring effects.--Administration of fluid increases extracellular fluid volume to raise cardiac output.
CONGENITAL HEART DISEASE
Therapeutic Interventions (cont.)
* Maintain adequate ventilation and perfusion, as in the following: o Place patient in semi- to high-Fowlers position. This reduces preload and ventricular filling. o Place in supine position. This increases venous return, promotes diuresis. o Administer humidified oxygen as ordered. The failing heart may not be able to respond to increased oxygen demands. * Maintain physical and emotional rest, as in the following: o Restrict activity. This reduces oxygen demands. o Provide quiet, relaxed environment. Emotional stress increases cardiac demands. o Organize nursing and medical care. This allows rest periods. - Monitor progressive activity within limits of cardiac function.
CONGENITAL HEART DISEASE
Therapeutic Interventions (cont.)
* Administer stool softeners as needed.--Straining for a bowel movement further impairs cardiac output. * Monitor sleep patterns; administer sedative.--Rest is important for conserving energy. * If arrhythmia occurs, determine patient response, document, and report if significant or symptomatic. o Have antiarrhythmic drugs readily available. o Treat arrhythmias according to medical orders or protocol and evaluate response.--Both tachyarrhythmias and bradyarrhythmias can reduce cardiac output and myocardial tissue perfusion.
CONGENITAL HEART DISEASE
Education/Continuity of Care
* Explain drug regimen, purpose, dose, and side effects.
* Explain symptoms and interventions for decreased cardiac output related to etiological factors.
* Explain progressive activity schedule and signs of overexertion.
* Explain diet restrictions (fluid, sodium).
Fin..
Вам также может понравиться
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeОт EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeРейтинг: 4 из 5 звезд4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreОт EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreРейтинг: 4 из 5 звезд4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItОт EverandNever Split the Difference: Negotiating As If Your Life Depended On ItРейтинг: 4.5 из 5 звезд4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceОт EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceРейтинг: 4 из 5 звезд4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersОт EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersРейтинг: 4.5 из 5 звезд4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureОт EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureРейтинг: 4.5 из 5 звезд4.5/5 (474)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)От EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Рейтинг: 4.5 из 5 звезд4.5/5 (120)
- The Emperor of All Maladies: A Biography of CancerОт EverandThe Emperor of All Maladies: A Biography of CancerРейтинг: 4.5 из 5 звезд4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingОт EverandThe Little Book of Hygge: Danish Secrets to Happy LivingРейтинг: 3.5 из 5 звезд3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyОт EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyРейтинг: 3.5 из 5 звезд3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)От EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Рейтинг: 4 из 5 звезд4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaОт EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaРейтинг: 4.5 из 5 звезд4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryОт EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryРейтинг: 3.5 из 5 звезд3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnОт EverandTeam of Rivals: The Political Genius of Abraham LincolnРейтинг: 4.5 из 5 звезд4.5/5 (234)
- DOH Ambulatory Surgical Clinic LTO at 1262015rev1Документ12 страницDOH Ambulatory Surgical Clinic LTO at 1262015rev1al gul50% (2)
- The Unwinding: An Inner History of the New AmericaОт EverandThe Unwinding: An Inner History of the New AmericaРейтинг: 4 из 5 звезд4/5 (45)
- Bir Form 2307Документ2 страницыBir Form 2307devine peraltaОценок пока нет
- 365 Daily QuotesДокумент32 страницы365 Daily QuotesAna SilivestruОценок пока нет
- ViewДокумент3 страницыViewEthan Marcos GoОценок пока нет
- Community NursingДокумент3 страницыCommunity NursingEthan Marcos GoОценок пока нет
- Fecal IncontinenceДокумент7 страницFecal IncontinenceEthan Marcos GoОценок пока нет
- CC SholehДокумент2 страницыCC SholehWulan Ervinna SimanjuntakОценок пока нет
- Thorax RadiologyДокумент31 страницаThorax Radiologyshanti kiranaОценок пока нет
- Exercise 1: Label and Explain The Blood CirculationДокумент2 страницыExercise 1: Label and Explain The Blood CirculationKiana Ramosa100% (1)
- Cardiac Resynchronization Therapy (Sep 19 2007) - (1841846376) - (CRC Press)Документ337 страницCardiac Resynchronization Therapy (Sep 19 2007) - (1841846376) - (CRC Press)Morozovschi VitalieОценок пока нет
- THE CARDIOVASCULAR SYSTEM ReviewДокумент34 страницыTHE CARDIOVASCULAR SYSTEM ReviewEndahОценок пока нет
- Determinari Pulmonare in Boli Ale Tesutului Conjunctiv Si VasculiteДокумент4 страницыDeterminari Pulmonare in Boli Ale Tesutului Conjunctiv Si VasculiteAna-Maria PopaОценок пока нет
- Cardiac CycleДокумент2 страницыCardiac CycleU Than HanОценок пока нет
- Veteriner Anatomi Dolaşım Sistemi by VETSДокумент54 страницыVeteriner Anatomi Dolaşım Sistemi by VETSalparslanhocaoglu60Оценок пока нет
- Chest X-Ray Fundamentals: Dr. Emad EfatДокумент241 страницаChest X-Ray Fundamentals: Dr. Emad EfatRutvik Shah100% (1)
- Cardiology Procedures 2017 - HendelДокумент339 страницCardiology Procedures 2017 - HendelGian Carlo Chalarca LondoñoОценок пока нет
- Buku Bantu ICD 9CM (Tindakan)Документ2 страницыBuku Bantu ICD 9CM (Tindakan)muhammad aldafikinОценок пока нет
- TOPIC 12 The Cardiovascular SystemДокумент27 страницTOPIC 12 The Cardiovascular SystemLorraine RiegoОценок пока нет
- L A S - S Ci: Science Activity Sheet Quarter 1-MELC 1 Week 1Документ15 страницL A S - S Ci: Science Activity Sheet Quarter 1-MELC 1 Week 1Benedick Zorilla ZaspaОценок пока нет
- The Circulatory SystemДокумент67 страницThe Circulatory Systemapi-263357086Оценок пока нет
- L2 PericardiumДокумент36 страницL2 PericardiumElisaОценок пока нет
- Science: Mahay Integrated Secondary SchoolДокумент10 страницScience: Mahay Integrated Secondary Schoollavenia acdalОценок пока нет
- Note Making and Note TakingДокумент33 страницыNote Making and Note TakingManisha SalikarОценок пока нет
- PeriCardio SintesisДокумент34 страницыPeriCardio SintesisAnonymous Tq6ui0t8LОценок пока нет
- 8 Coronary CirculationДокумент31 страница8 Coronary CirculationAhmed AliОценок пока нет
- Basics of Chest X-RayДокумент44 страницыBasics of Chest X-RayMelissa Aina Mohd YusofОценок пока нет
- Heart Structure and Cardiac Cycle Questions: Bournemouth School 1Документ9 страницHeart Structure and Cardiac Cycle Questions: Bournemouth School 1Shermer100% (1)
- Heart and Blood VesselsДокумент15 страницHeart and Blood VesselsIDKОценок пока нет
- Ebstein Anomaly in The Adult PatientДокумент11 страницEbstein Anomaly in The Adult PatientRJMОценок пока нет
- The Skeleton Vertebral Column 26 BonesДокумент3 страницыThe Skeleton Vertebral Column 26 BonesJingle Capistrano TarucОценок пока нет
- Nuclear CaseДокумент106 страницNuclear CaseAkramОценок пока нет
- Electrical Axis of HeartДокумент19 страницElectrical Axis of Heartrera_avisОценок пока нет
- DETAILED LESSON PLAN GRADE 6 BIOLOGY ExpirementДокумент10 страницDETAILED LESSON PLAN GRADE 6 BIOLOGY ExpirementLoiweza Abaga100% (1)
- Bates Test Questions The Cardiovascular System Bates Test Questions The Cardiovascular SystemДокумент16 страницBates Test Questions The Cardiovascular System Bates Test Questions The Cardiovascular SystemmuranОценок пока нет
- Congenital Heart DiseaseДокумент120 страницCongenital Heart Diseasemerin sunilОценок пока нет